Pain Management Copyright 2010 Wolters Kluwer Health Lippincott


































- Slides: 41

Pain Management Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Pain • Unpleasant sensory, emotional experience with actual or potential tissue damage • Most common reason for seeking health care • “The fifth vital sign” • Joint Commission (2005) standards: “pain is assessed in all patients, ” “patients have the right to appropriate assessment and management of pain. ” • “Pain is whatever a person says it is, existing whenever the experiencing person says it does” (Mc. Caffery & Pasero, 1999) Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

• https: //www. youtube. com/watch? v=I 7 wf. Denj 6 CQ Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

• Pain related to cancer may be caused by direct tumor infiltration of bones, nerves, viscera, or soft tissue or by prior therapeutic measures (surgery, radiation). Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Types of Pain • Acute pain: usually of recent onset and associated with specific injuries (last from seconds-6 weeks) • Chronic pain: is constant or intermittent that persists beyond the expected healing time. It has poorly defined onset and often difficult to treat (last for 6 months) • Cancer-related pain(acute or chronic) • May be classified by location (e. g. pelvic pain, headach) or etiology (burn pain) Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

1. Somatic pain—caused • by direct tumor involvement of sensory receptors in cutaneous and deep tissues. • a. Usually described as dull, sharp, aching, and throbbing; usually constant and localized. • b. Most common somatic pain is bone pain caused by metastasis. • c. Can usually be controlled with NSAIDs or oral opioids Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

2 - Neuropathic pain. • a. Results from nerve injury or compression. • b. Includes phantom pain. • c. Described as burning, shooting, electric, and lancinating. (It can be constant or sporadic. ) • d. Usually associated with paresthesia. • e. Treatment usually includes combinations of antidepressants, anticonvulsants, and opioids. Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

3. Visceral pain. • a. Usually described as deep, dull, aching, squeezing, or pressure sensation. It can be vague or ill-defined and can be referred to cutaneous sites, making it difficult to differentiate from somatic pain. • b. Usually caused by abnormal stretching of smooth muscle walls, ischemia of visceral muscle, and serosal irritation. • c. Can be treated with oral opioids or surgery to remove the cause. Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Effects of Pain • Sleep deprivation • Acute pain – Can affect respiratory, cardiovascular, endocrine, immune systems – Stress response increases metabolic rate, cardiac output, risk for physiologic disorders Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Effects of Pain (cont’d) • Chronic pain – Depression – Increased disability – Suppression of immune function Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Question • What is the time frame for pain that can be classified as chronic? A. 1 month B. 2 to 3 months C. 4 to 5 months D. Longer than 6 months Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Answer • D. Longer than 6 months • Rationale: Chronic pain is constant or intermittent pain that persists beyond the expected healing time and that can seldom be attributed to a specific cause or injury. Chronic pain may be defined as pain that lasts for 6 month or longer, although 6 months is an arbitrary period for differentiating between acute and chronic pain. Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Pathophysiology of Pain • Nociceptors (pain receptors) • Transmission of pain (nocicetion) • Chemical substances – Prostaglandins (increase sensitivity of pain receptors) – Endorphins, enkephalins (suppress pain reception) Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

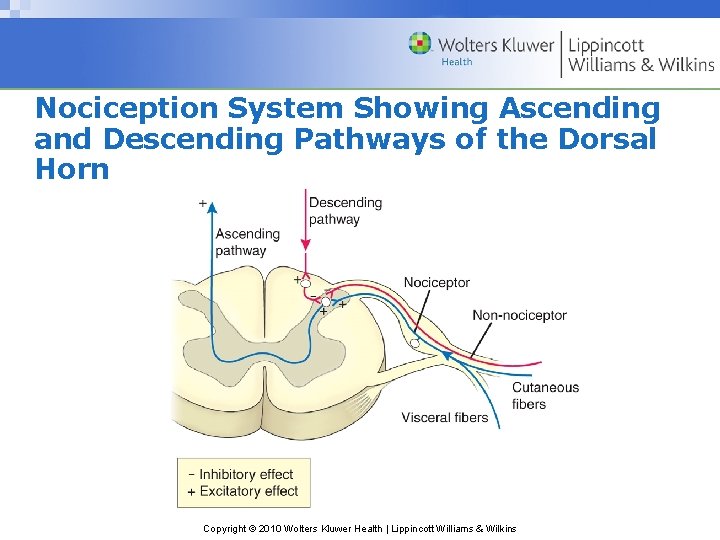
Nociception System Showing Ascending and Descending Pathways of the Dorsal Horn Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

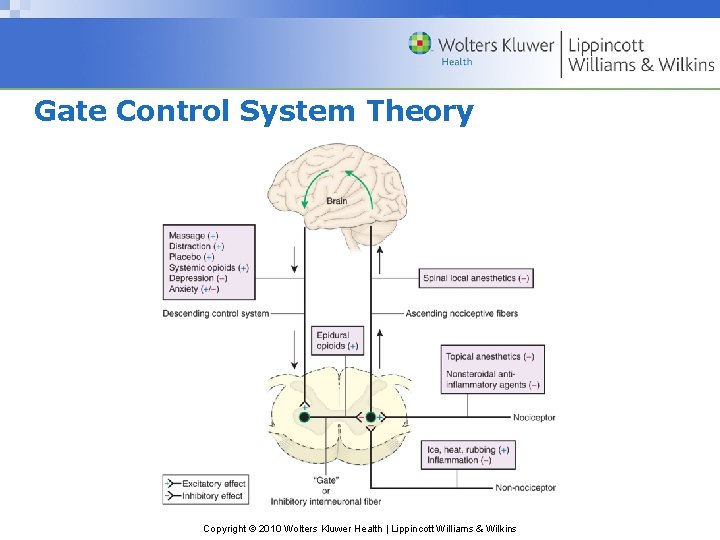
Gate Control System Theory Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Question • Tell whether the following statement is true or false: • Endorphins represent the same mechanism of pain relief as nonnarcotic analgesics. Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Answer • False. • Rationale: Endorphins do not represent the same mechanism of pain relief as nonnarcotic analgesics. Endorphins release inhibits the transmission of painful impulses. They are endogenous neurotransmitters structurally similar to opioids. They are found in heavy concentration in the central nervous system. Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Factors that Influence Pain Response • Past experience • Anxiety • Depression • Culture • Age • Gender Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

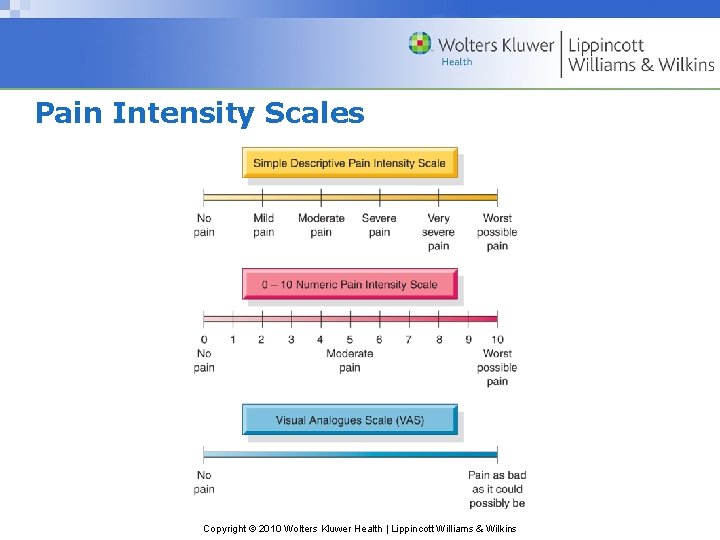
Characteristics of Pain • Intensity • Timing • Location • Quality • Personal meaning • Aggravating, alleviating factors • Pain behaviors Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Pain Intensity Scales Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Faces Pain Scale Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Question • The RN asks a patient to describe the quality of pain. Which of the following is a descriptive term for the quality of pain? A. Burning B. Chronic C. Intermittent D. Severe Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Answer • A. Burning • Rationale: A descriptive term for the quality of pain is burning. Chronic and intermittent pain are examples of types of pain. Severe is a descriptive term for the intensity of pain. Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Principles of Pain Management • 1. The goal of pain management is complete relief of pain. • 2. Placebos are never indicated for the treatment of pain. • 3. Physical dependence and tolerance commonly occur; patient may require escalating doses of medications to control pain. • 4. It is essential that physicians and nurses do not confuse addiction with tolerance. Addiction is an unrelated medical disorder with behavioral components. These facts must also be stressed with patients who are reluctant to take medications. Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Physiologic Basis for Pain Relief Pharmacologic Interventions • Opioid analgesics act on CNS to inhibit activity of ascending nocioceptive pathways • NSAIDS decrease pain by inhibiting cyclo-oxygenase (enzyme involved in production of prostaglandin) • Local anesthetics block nerve conduction when applied to nerve fibers Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Nonopioid analgesics • 1. Acetaminophen—a centrally acting analgesic; does not have anti-inflammatory or antiplatelet activities. • 2. NSAIDs. • a. Produce analgesia by decreasing levels of inflammatory mediators such as prostaglandins at the site of tissue injury. • b. Suppress platelet function, decrease creatinine clearance, and interfere with the protective effect of prostaglandins on the gastric mucosa. • c. Used to treat mild to moderate pain; examples include ibuprofen, 400 to 800 mg P. O. t. i. d. ; nabumetone, 500 to 1000 mg P. O. b. i. d. ; indomethacin, 25 to 50 mg P. O. t. i. d. Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

• d. COX-2 inhibitors are NSAIDs that are somewhat selective for cyclooxygenase 2 (COX-2) compounds, present in most tissues but less present than COX-1 in gastric mucosa. • COX-2 is induced in response to inflammation and converts arachidonic acid to prostaglandin. COX-2 inhibitors inhibit prostaglandins at the site of inflammation but cause less GI irritation and bleeding. Examples include celecoxib, Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

• Corticosteroids—may decrease edema associated with tumor invasion of neural tissue or bone. • a. Typically used for headache associated with brain tumors. • b. Examples include dexamethasone • 4. Bisphonates—used for lytic bone lesions to prevent fractures and may help control bone pain. Examples include zoledronic acid, • 5. Anticonvulsants and antidepressants for neuropathic pain— used to enhance the effect of opioids. Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Opioid Tolerance and Addiction • Maximum safe opioid dosage must be individually assessed • Tolerance develops in all patients who take opioids for prolonged periods • With tolerance, increased usage needed to effect pain relief Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Opioid Tolerance and Addiction (cont’d) • Dependence occurs with tolerance, physical symptoms occur when opioid is discontinued • Addiction: behavioral pattern characterized by need to take drug for psychic effects • Addiction from therapeutic use of opioid is negligible Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Pain Relief Interventions-Pharmacologic • Opioid and NSAID • Balanced anesthesia • “PRN” medications • Routine administration: around the clock (ATC) or preventive approach • PCA: patient-controlled analgesia • Local anesthetics • Topicals, patches • Intraspinal administration Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Nonpharmacologic Interventions • Cutaneous stimulation (massage): Stimulation of gfibers that transmit non-painful sensation can block or decrease the transmission of pain impulses • Thermal therapies (Ice or heat) • Transcutaneous electrical nerve stimulation: uses battery operated unit with electrodes applied to the skin to produce tingling, vibrating, or buzzing sensation in the area of pain • Distraction: focusing patient attention on something other than pain • Relaxation techniques( e. g. abdominal breathing) Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Nonpharmacologic Interventions (cont’d) • Guided imagery is a mind-body intervention by which a trained practitioner or teacher helps a participant or patient to evoke and generate mental images that simulate or re-create the sensory perception of sights, sounds, tastes, smells, movements, and images associated with touch, such as texture, temperature… https: //www. youtube. com/watch? v=Bg. OKKjgqq. Mc • Hypnosis is a state of human consciousness involving focused attention and reduced peripheral awareness and an enhanced capacity to respond to suggestion • Music therapy Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

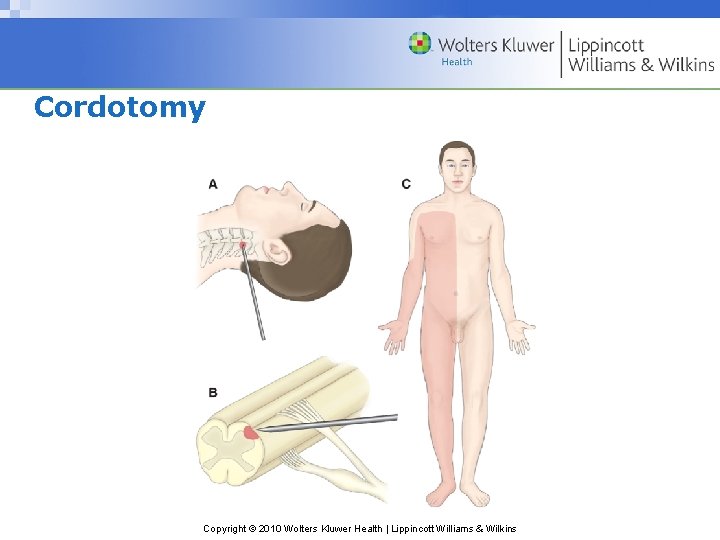
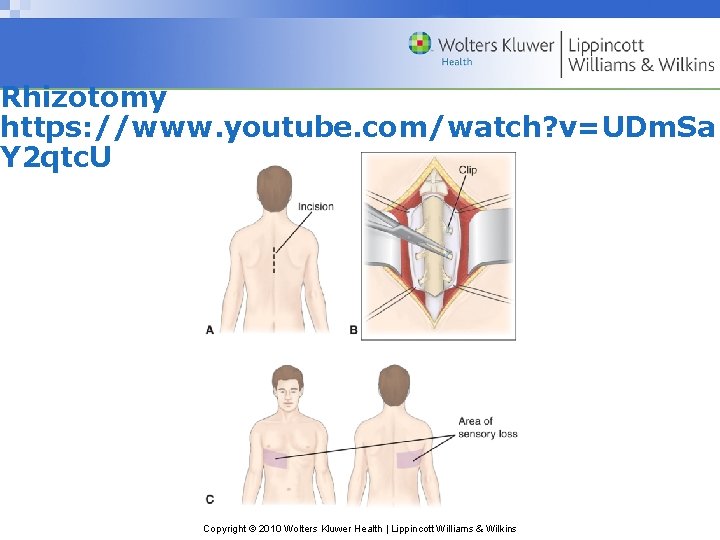
Neurologic and Neurosurgical Methods for Pain Control • Stimulation procedures: applying controlled low voltage electrical impulses to the different part of the nervous system • Interruption of pain pathways – Cordotomy: division of certain tract of spinal cord – Rhizotomy: sensory nerve roots destroyed where they enter the spinal cord – Nursing intervention: education, monitor SE Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

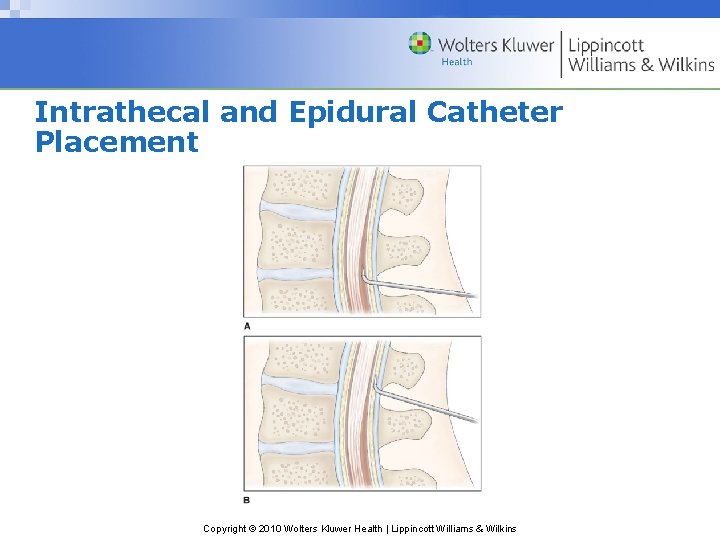
Intrathecal and Epidural Catheter Placement • 3 -5 cm of the catheter is in the subarachnoid space Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Intrathecal and Epidural Catheter Placement Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Cordotomy Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Rhizotomy https: //www. youtube. com/watch? v=UDm. Sa Y 2 qtc. U Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Adverse Effects of Analgesic Agents • Respiratory depression • Sedation • Nausea, vomiting • Constipation • Pruritis Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Nursing Process Framework for Pain Management • Identify goals for pain management • Establish nurse-patient relationship, teaching • Provide physical care • Manage anxiety related to pain • Evaluate pain-management strategies Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins