Pain Inflammation NSAIDs and Analgesics BY DR KAUKAB

Pain, Inflammation, NSAIDs and Analgesics BY DR KAUKAB AZIM

Learning Outcomes By the end of the lecture the student should be able to • Define and discuss the pathobiology of pain pathways • Explain the molecular mechanism of action common to all nonsteroidal antiinflammatory drugs (NSAIDs) • Describe the pharmacological effects of each drug in each class. • Describe the pharmacokinetics of salicylates. • Describe the main adverse effects of the drugs of each class. • Describe the clinically important drug interactions of the drugs of each class. • Describe the principal contraindications of the drugs of each class. • Describe the main therapeutic uses of NSAIDs and acetaminophen.

What is inflammation? • INFLAMMATION – is a reaction to tissue injury caused by the release of chemical mediators that cause both vascular response and the migration of fluids and cells to the injured site. • It is a protective mechanism in which the body attempts to neutralize and destroy harmful agents at the site of tissue injury and establish condition for tissue repair.

What is Pain: An unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage Hyperaesthesia (hypersensitivity): Increased sensitivity to stimulation, excluding the special senses Hyperalgesia: Increased pain in response to a noxious stimulus Allodynia: Pain due to a stimulus that does not normally produce pain From the International Association for the Study of Pain (IASP) definitions (Merskey, and Bogduk 1994)

Physicians Have a Moral Obligation to Provide Comfort and Pain Management Especially for those near the end of life! • Pain is the most feared complication of illness • Pain is the second leading complaint in physicians’ offices • Often under-diagnosed and under-treated • Effects on mood, functional status, and quality of life • Associated with increased health service use

18% of Elderly Persons Take Analgesic Medications Regularly (daily or more than 3 times a week) • 71 % take prescription analgesics – 63% for more than 6 months • 72% take OTC analgesics – Median duration more than 5 years • 26% report side-effects – 10% were hospitalized – 41% take medications for side-effects

Common Causes of Pain In Elderly Persons • Osteoarthritis – back, knee, hip • Night-time leg cramps • Claudication • Neuropathies – idiopathic, traumatic, diabetic, herpetic • Cancer
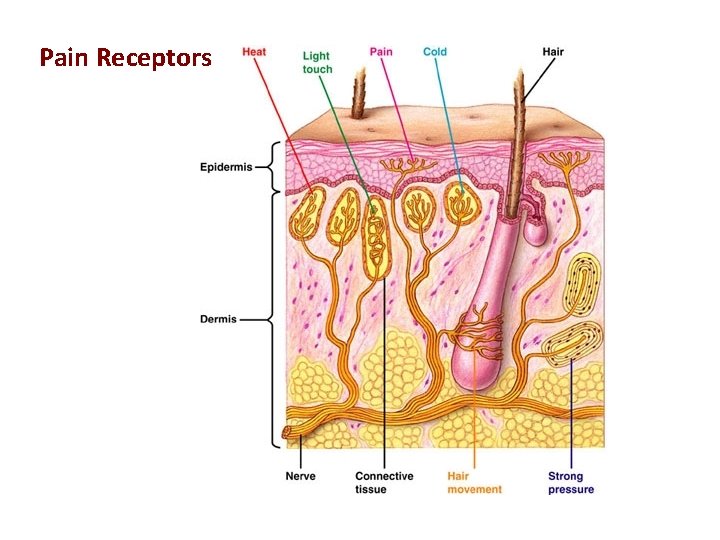
Pain Receptors
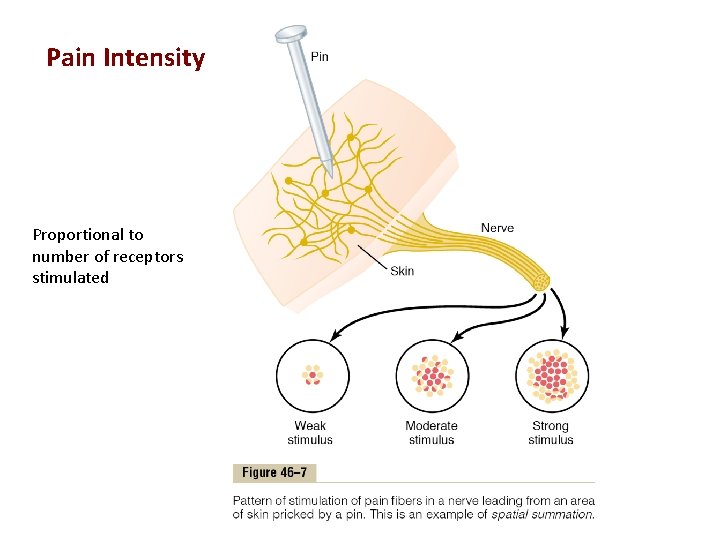
Pain Intensity Proportional to number of receptors stimulated
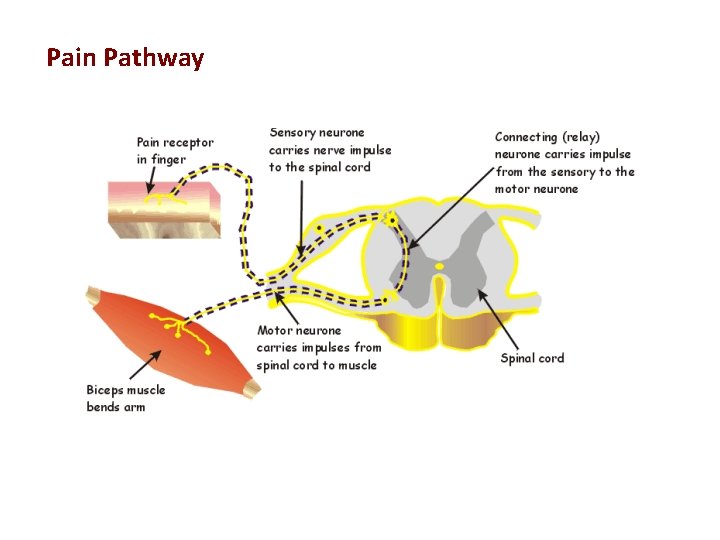
Pain Pathway
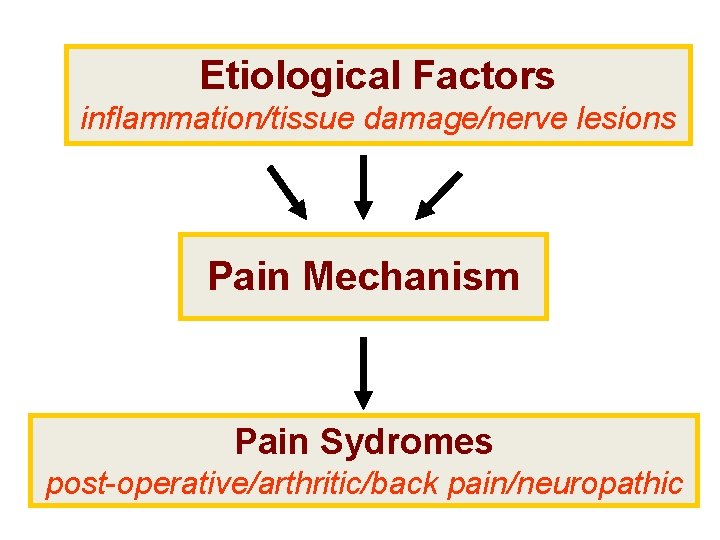
Etiological Factors inflammation/tissue damage/nerve lesions Pain Mechanism Pain Sydromes post-operative/arthritic/back pain/neuropathic
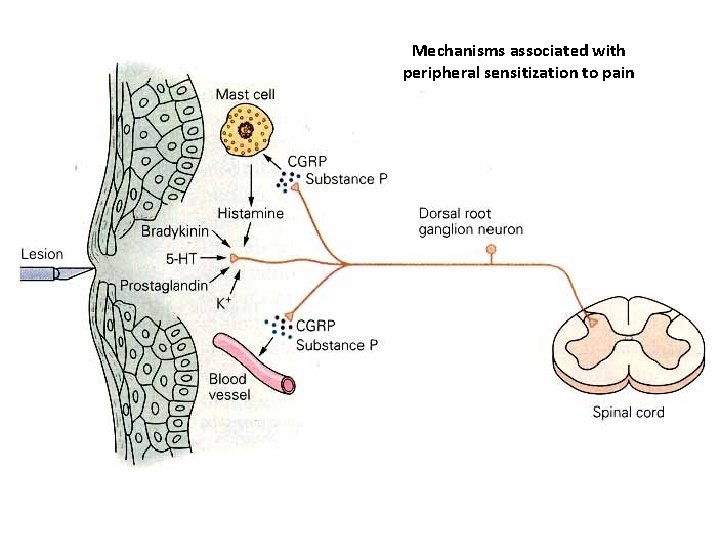
Mechanisms associated with peripheral sensitization to pain
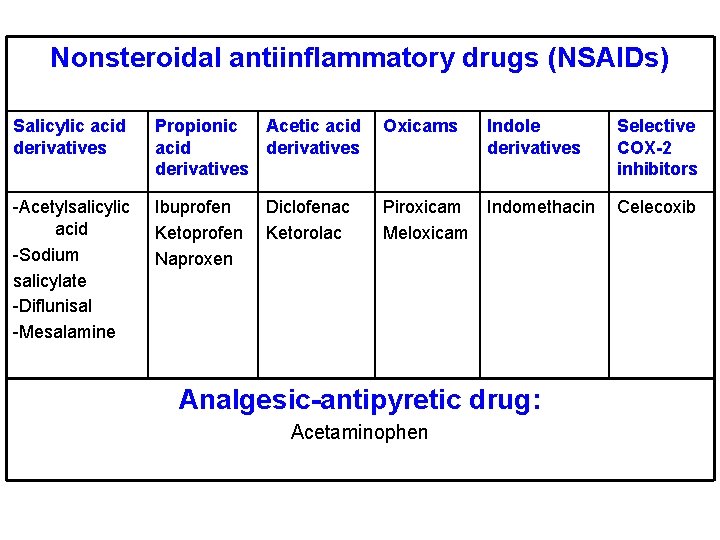

Nonsteroidal antiinflammatory drugs (NSAIDs) Salicylic acid derivatives Propionic Acetic acid derivatives Oxicams Indole derivatives Selective COX-2 inhibitors -Acetylsalicylic acid -Sodium salicylate -Diflunisal -Mesalamine Ibuprofen Ketoprofen Naproxen Piroxicam Meloxicam Indomethacin Celecoxib Diclofenac Ketorolac Analgesic-antipyretic drug: Acetaminophen
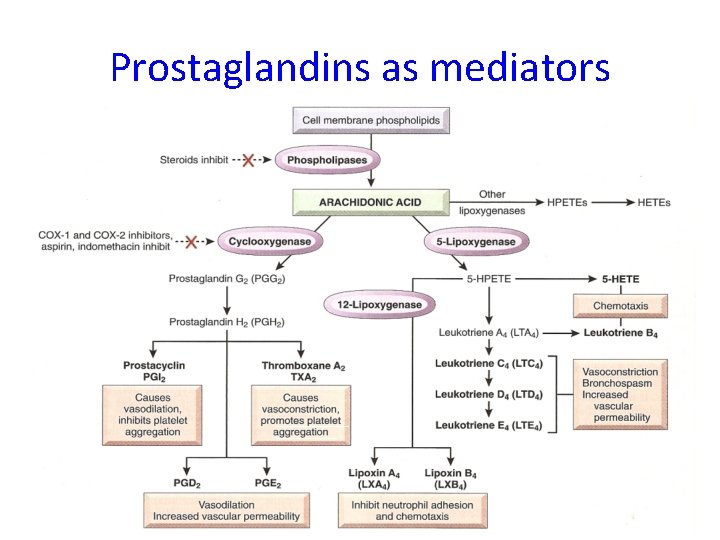
Prostaglandins as mediators √ 14
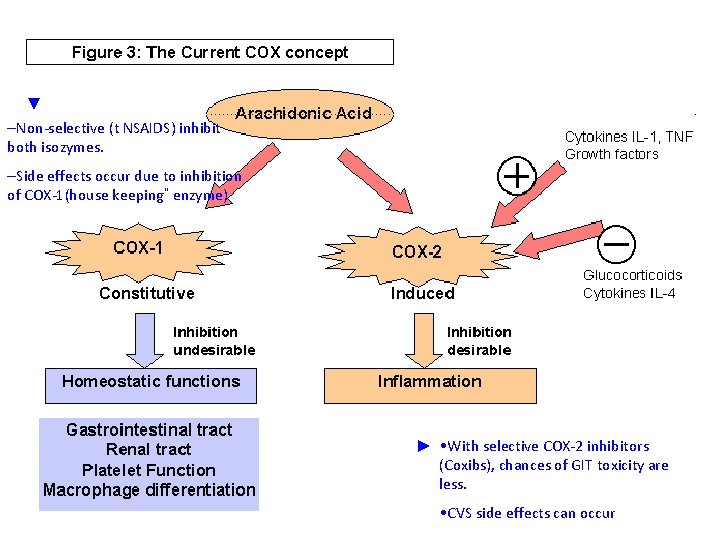
▼ –Non-selective (t NSAIDS) inhibit both isozymes. –Side effects occur due to inhibition of COX-1(house keeping” enzyme) ► • With selective COX-2 inhibitors (Coxibs), chances of GIT toxicity are less. • CVS side effects can occur

NSAIDS: Mechanism of action • Main mechanism: Inhibition of COX – Reversible (competitive) inhibitors – Irreversible inactivation (by Aspirin) – Nonselective COX inhibitors (traditional NSAIDS) – Selective COX-2 inhibitors (Celecoxib)

NSAIDS: Effects • Anti-inflammatory effect – reverses vasodilation, edema, tenderness • Analgesic effect – By preventing PG mediated sensitization of nerve endings • Antipyretic effect – Resets the hypothalamic thermostat by decreasing PG synthesis – Vasodilation and heat loss – Do not cause hypothermia

• Antiplatelet aggregation effect – Platelets have COX-1 – Aspirin acetylates COX-1 to inhibit its activity in an “irreversible manner”. – All other t. NSAIDS- reversible inhibitors – Selective COX-2 inhibitors do not disturb platelet aggregation at therapeutic doses – Acetaminophen do not inhibit platelet aggregation

Common side effects of NSAIDS • Gastrointestinal: Nonselective NSAIDS COX-1 inhibition ↓ gastroprotective PGs – Gastric irritation, erosions, ulcers, gastric bleeding – Misoprostol (PGE 1) can be used to prevent gastric ulcers caused by t. NSAIDS. – Selective COX-2 inhibitors are safer.

• Renal: Sodium water retention, Papillary necrosis • CVS: ↑ Na and water retention • Platelet inhibition : bleeding – Selective COX-2 inhibitors and acetaminophen do not disturb platelet function. • CNS: Headache, confusion, seizures • Hypersensitivity: “Pseudoallergic reaction” (due to increased leukotrienes)

Salicylates • Acetylated salicylate: Aspirin (Acetylsalicylic acid) • Non-acetylated salicylates: sodium salicylate, diflunisal, mesalamine (5 -ASA) ►Mechanism of action: – Aspirin: non-selective COX inhibitor; “Irreversible inhibition” by acetylation. – Other salicylates: weak COX inhibitors; other mechanisms are involved.
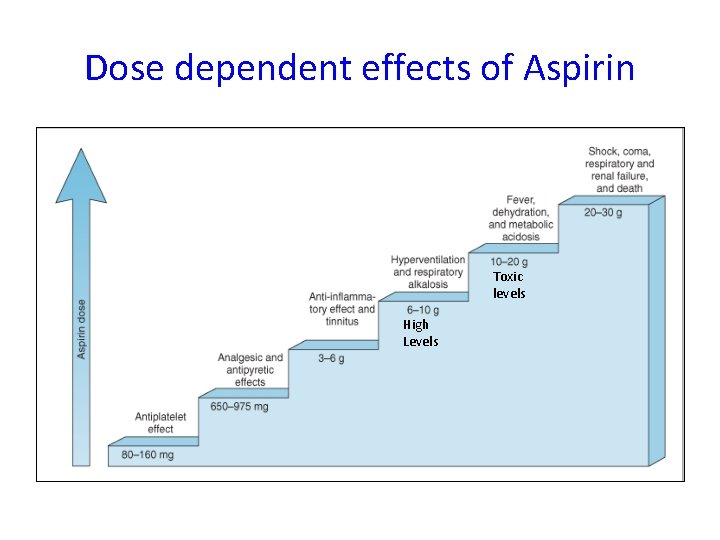
Dose dependent effects of Aspirin Toxic levels High Levels

Effects of aspirin • Antiplatelet effect: – Irreversible inactivation of COX-1 in platelets causes decreased production of TXA 2 (aggregation promoter) • Platelets (enucleated) cannot regenerate COX; effect lasts for 7 -8 days. – Irreversible inactivation of COX in endothelial cells causes decreased production of PGI 2 (aggregation inhibitor) • Endothelial cells can regenerate cyclooxygenase in a matter of hrs. – Net effect is decreased platelet aggregation and increase in bleeding time. – Low doses (80 -160 mg) are enough to inhibit aggregation without anti-inflammatory effects.
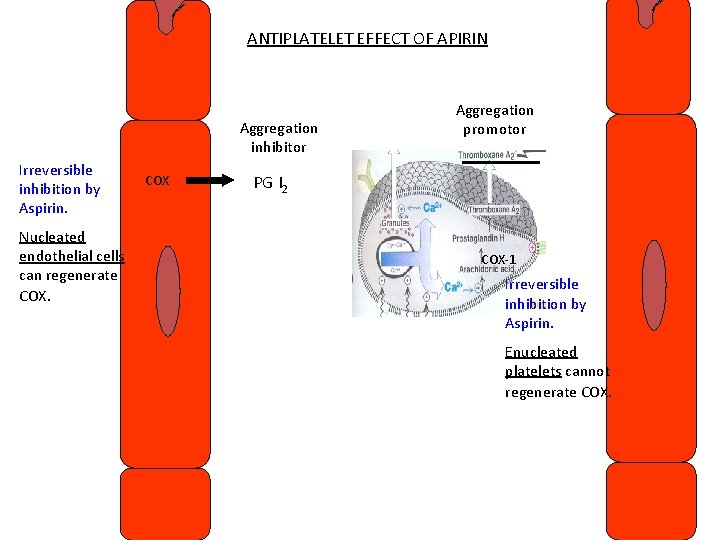
ANTIPLATELET EFFECT OF APIRIN Aggregation inhibitor Irreversible inhibition by Aspirin. Nucleated endothelial cells can regenerate COX Aggregation promotor PG I 2 COX-1 Irreversible inhibition by Aspirin. Enucleated platelets cannot regenerate COX. 24

• ↑ Plasma uric acid levels (at low dose) • ↓ Plasma uric acid levels (at high dose) • Hyperventilation and compensated alkalosis (At high levels) – stimulates respiratory center, ↓ p. CO 2, Increased bicarbonate in urine • Metabolic acidosis: (At toxic levels) – Accumulation of salicylic acid due to zero order kinetics at high levels. – Respiratory center depression; ↑ p. CO 2

Salicylates: Adverse effects • Hypersensitivity reactions – Pts with asthma, nasal polyps, chronic urticaria are more susceptible – Pseudoallergic reaction – Cross reactivity with other NSAIDS • Reye’s syndrome: Encephalopathy, hepatotoxicity. – Do not use aspirin in children with viral fever. • Salicylism: Tinnitus, dimness of vision, mental confusion, sweating, hyperventilation, nausea and vomiting, diarrhea

Salicylate intoxication – – – Tinnitus, Nausea and vomiting, abdominal cramps, gastric bleeding. Respiratory depression, Acidosis, generalized convulsions. marked hyperthermia, dehydration. Skin eruptions, petechial hemorrhages coma and death (due to respiratory failure) Treatment: Symptomatic and supportive. – – – External cooling and I. V. fluids with Na, K, and glucose. Gastric lavage to remove unabsorbed drug Forced alkaline diuresis to remove absorbed drug

Salicylates: Therapeutic uses • Keratolytic: salicylic acid • Counterirritant: Methylsalicylate • Antiinflammatory, analgesic, antipyretic – Diflunisal: does not enter CNS; no antipyretic effect Mesalamine (5 -ASA): – inflammatory bowel diseases Aspirin (Low doses): – MI, Angina – Atrial flutter/fibrillation – Transient ischemic attacks

Other t. NSAIDS Ibuprofen, Naproxen: – Widely used NSAID for pain and inflammation – GIT and CNS side effects are less Diclofenec – Inhibits COX and lipooxygenase (to minor extent) – Decreases free radical production – Accumulates in synovial fluid Ketorolac – Can be administered IV, IM – Used in postoperative pain

Indomethacin • One of the most potent COX inhibitor – – Inhibits COX Inhibits Phospholipase A 2 Reduces neutrophil migration Reduces T and B cell proliferation • Severe side effects (in 1/3 rd pts) – Abdominal pain, diarrhea, GI bleeding – Frontal headache – Dizziness, confusion, depression, hallucinations • Therapeutic Uses: – Arthritis (osteoarthritis, rheumatoid arthritis, Ankylosing spondylitis, Gout) – Closure of ductus arteriosus

Selective Cox-2 inhibitors “Coxibs” • Celecoxib: first selective COX-2 inhibitor • Potent antiinflammatory, analgesic and antipyretic activity • Incidence of GI bleeding and peptic ulcers is lower than t. NSAIDS • Does not inhibit platelet aggregation • Increased risk of cardiovascular side effects: Hypertension, Thrombotic events

Acetaminophen • Analgesic and antipyretic agent – Inhibits COX-3 in CNS… ? • Lacks significant anti-inflammatory and antiplatelet activity: very weak COX 1& 2 inhibitor • Metabolized in the liver • Toxic doses deplete glutathione – A metabolite, N-acetyl-p-benzoquinoneimine accumulates and causes hepatic necrosis. – Acetylcysteine administered as antidote.
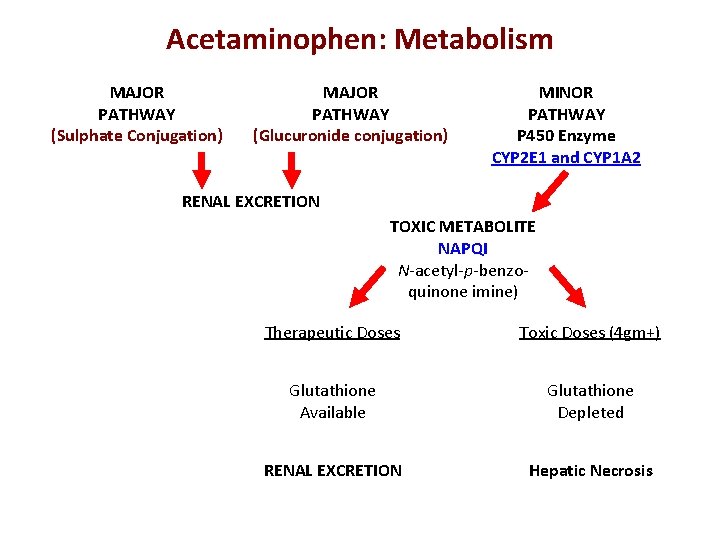
Acetaminophen: Metabolism MAJOR PATHWAY (Sulphate Conjugation) MAJOR PATHWAY (Glucuronide conjugation) MINOR PATHWAY P 450 Enzyme CYP 2 E 1 and CYP 1 A 2 RENAL EXCRETION TOXIC METABOLITE NAPQI N-acetyl-p-benzoquinone imine) Therapeutic Doses Toxic Doses (4 gm+) Glutathione Available Glutathione Depleted RENAL EXCRETION Hepatic Necrosis

Antiinflammatory agents: Steroids
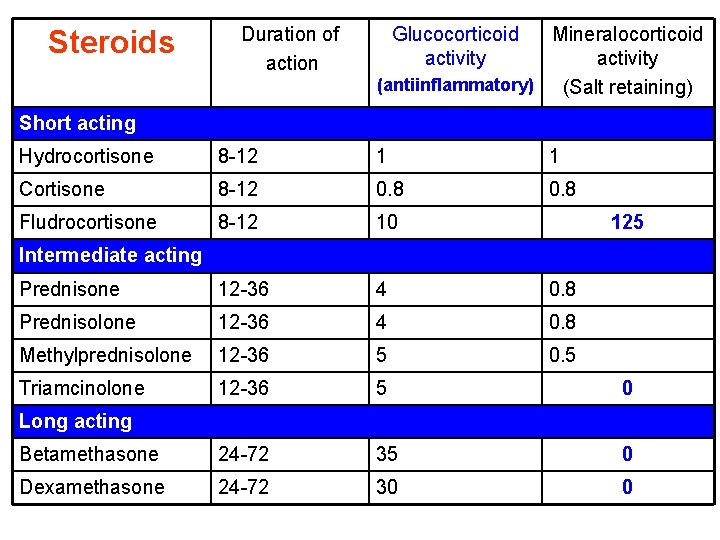
Steroids Duration of action Glucocorticoid activity Mineralocorticoid activity (antiinflammatory) (Salt retaining) Short acting Hydrocortisone 8 -12 1 1 Cortisone 8 -12 0. 8 Fludrocortisone 8 -12 10 Prednisone 12 -36 4 0. 8 Prednisolone 12 -36 4 0. 8 Methylprednisolone 12 -36 5 0. 5 Triamcinolone 12 -36 5 0 Betamethasone 24 -72 35 0 Dexamethasone 24 -72 30 0 125 Intermediate acting Long acting
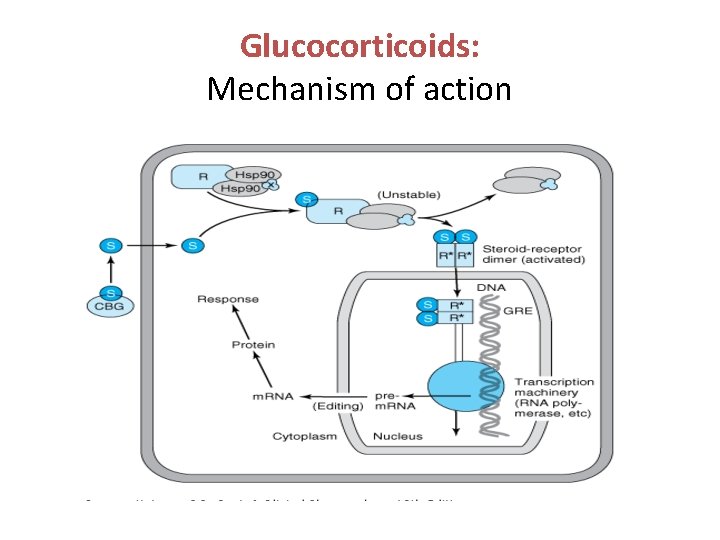
Glucocorticoids: Mechanism of action
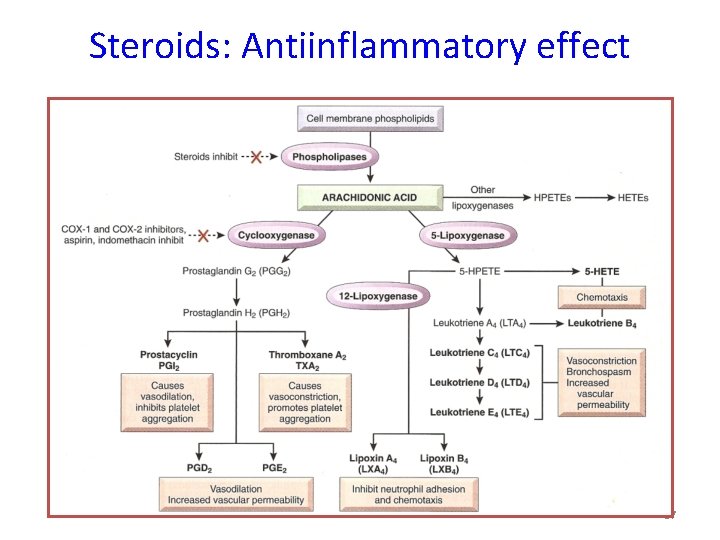
Steroids: Antiinflammatory effect 37

Therapeutic uses • Adrenal Uses • Non-adrenal uses: – Inflammatory disorders • Asthma • Allergies: Allergic rhinitis, Acute allergic reactions • Autoimmune disorders: RA, SLE, glomerulonephritis – Carcinomas – For immunosuppression
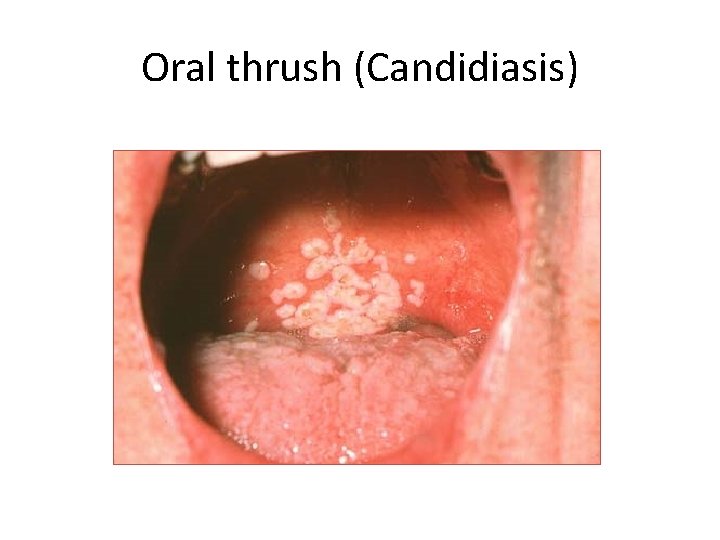
Oral thrush (Candidiasis)

Other Adverse effects of Glucocorticoids • • • Cushing like syndrome Psychosis Peptic ulcers Osteoporosis Aseptic necrosis of hip Easy bruisability, Purple striae on skin Visceral fat deposition Posterior subcapsular cataract, glaucoma Hirsutism Increased appetite Growth retardation in children

OPIOID ANALGESICS

History of Opioids • Opium is extracted from poppy seeds • Used for thousands of years to produce: – Euphoria – Analgesia – Sedation – Relief from diarrhea – Cough suppression

Mechanism of action • Activation of peripheral nociceptive fibers causes release of substance P and other pain-signaling neurotransmitters from nerve terminals in the dorsal horn of the spinal cord • Release of pain-signaling neurotransmitters is regulated by opioid agonists by acting presynaptically to inhibit substance P release, causing analgesia

Molecular Effect of Opioid Receptor Activation • Reduction or inhibition of neurotransmission, due largely to opioid-induced presynaptic inhibition of neurotransmitter release • Involves changes in transmembrane ion conductance – Increase potassium conductance (hyperpolarization) – Inactivation of calcium channels

Pharmacological Effects • Sedation and anxiolysis – Drowsiness and lethargy – Apathy – Cognitive impairment • Depression of respiration – Main cause of death from opioid overdose – Combination of opioids and alcohol is especially dangerous • Cough suppression – Opioids suppress the “cough center” in the brain • Pupillary constriction – pupillary constriction in the presence of analgesics is characteristic of opioid use

Pharmacological effects • Nausea and vomiting – Stimulation of receptors in an area of the medulla called the chemoreceptor trigger zone causes nausea and vomiting – Unpleasant side effect, but not life threatening • Gastrointestinal symptoms – Opioids relieve diarrhea as a result of their direct actions on the intestines • Other effects – Opioids can release histamines causing itching or more severe allergic reactions including bronchoconstriction – Opioids can affect white blood cell function and immune function

Three Opioid Receptors • Mu • Kappa • Delta

Delta Receptor • It is unclear what delta’s responsible for. • Delta agonists show poor analgesia and little addictive potential • May regulate mu receptor activity

Mu-Receptor: Two Types • Mu-1 – Located outside spinal cord – Responsible for central interpretation of pain • Mu-2 – Located throughout CNS – Responsible for respiratory depression, spinal analgesia, physical dependence, and euphoria

Kappa Receptor • Only modest analgesia • Little or no respiratory depression • Little or no dependence • Dysphoric effects

Mu and Kappa Receptor Activation Response Mu-1 Mu-2 Kappa Analgesia ✓ ✓ ✓ Respiratory Depression ✓ Euphoria ✓ Dysphoria ✓ Decrease GI motility ✓ Physical Dependence ✓

AGONISTS Morphine Heroin Hydromorphone Fentanyl Codeine

Morphine • PHARMACOKINETICS • Routes of administration (preferred) *Oral latency to onset –(15 – 60 minutes ) • * it is also sniffed, swallowed and injected. • * duration of action – ( 3 – 6 hours) • * First-pass metabolism results in poor • availability from oral dosing. • * 30% is plasma protein bound • EFFECTS AND MEDICAL USES • *symptomatic relief of moderate to severe pain • *relief of certain types of labored breathing • *suppression of severe cough (rarely) • *suppression of severe diarrhea • *AGONIST for mu, kappa, and delta receptors.

Hydromorphone • PHARMACOKINETICS • *Routes of administration (Preferred) • *Oral • *latency to onset (15 – 30 minutes) • *Intravenous • *Duration of Action (3 -4 hours) • *Peak effect (30 -60 minutes) • PROPERTIES AND EFFECTS • * potent analgesic like morphine but is 7 -10 • times as potent in this capacity. • *used fequently in surgical settings for moderate to • severe pain. (cancer, bone trauma, burns, renal colic. )

Fentanyl Pharmacokinetics Routes of Administration * Oral, and transdermal (possibly intravenous) *Highly lipophilic *latency to onset (7 -15 minutes oral; 12 -17 hours transdermal *duration of action ( 1 -2 hours oral; 72 transdermal) *80 – 85% plasma protein bound *90 % metabolized in the liver to inactive metabolites Other properties * 80 times the analgesic potency of morphine and 10 times the analgesic potency of hydromorphone. *high efficacy for mu 1 receptors. *most effective opiate analgesic • •

Antagonists Naloxone Naltrexone

Naltrexone • PHARMACOKINETICS • *latency to onset (oral tablet 15 -30 min. ) • *duration of action 24 -72 hours • *peak effect (6 -12 hours) • STRUCTURAL DISTINCTION • *Differs from naloxone insofar as the • allyl group on the nitrogen atom is supplanted • by a cyclopromethyl group. • EFFECTS • *Reverses the psychotomimetic effects of opiate • agonists. • * Reverses hypotension and cardiovascular instability • secondary to endogeneous endorphins (potent vasodilators) • *inhibits Mu, Delta, and Kappa receptors.

THANK YOU
- Slides: 58