Pain Dr H N Sarker MBBS FCPSMedicine MACPUSA

Pain Dr. H. N. Sarker MBBS, FCPS(Medicine), MACP(USA), MRCP(UK). Associate professor Medicine

Pain is an unpleasant sensation localised to a part of the body. It is often described in terms of a penetrating or tissue -destructive process (e. g. stabbing, burning, twisting, tearing, squeezing) and/or of a bodily or emotional reaction (e. g. , terrifying, nauseating, sickening).

Any pain of moderate or severe intensity is accompanied by anxiety and the urge to escape or terminate the feeling. These properties illustrate the duality of pain: it is both sensation and emotion.

Pain is perceived by pain receptors and is carried by A -delta (small myelinated) and C (unmyelinated) fibres, called Primary afferent nociceptors (pain receptors).

Pain pathway The cell bodies of primary sensory afferents are located in the dorsal root ganglia in the vertebral foramina. The primary afferent axon has two branches: one projects centrally into the spinal cord and the other projects peripherally to innervate tissues.

The axons of primary afferent nociceptors enter the spinal cord via the dorsal root. They terminate in the dorsal horn of the spinal gray matter A majority of spinal neurons contacted by primary afferent nociceptors send their axons to the contralateral thalamus.

These axons form the contralateral spinothalamic tract, which lies in the anterolateral white matter of the spinal cord, the lateral edge of the medulla, and the lateral pons and midbrain.
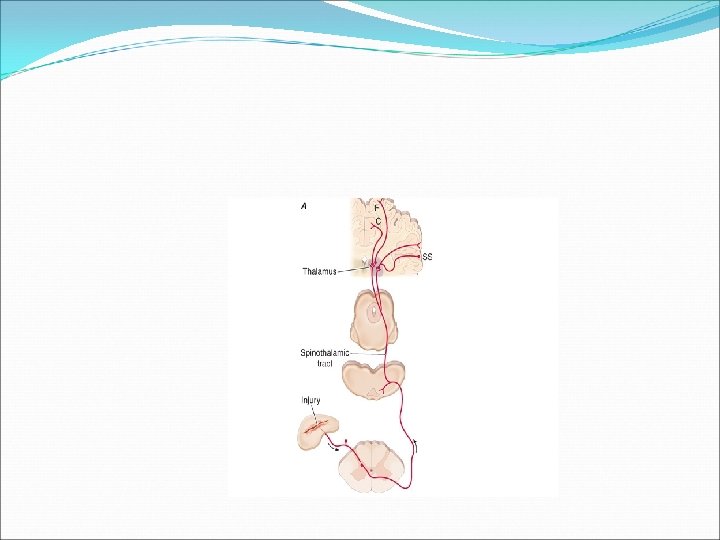

Spinothalamic tract axons ascend to several regions of the thalamus. There is tremendous divergence of the pain signal from these thalamic sites to broad areas of the cerebral cortex that subserve different aspects of the pain experience

The spinothalamic pathway is crucial for pain sensation in humans. Interruption of this pathway produces permanent deficits in pain and temperature discrimination.

Assessment of pain Pain history is very important because it may occur at any site of the body and its variable characterstics. Pain is assessed by analysing its following characterstics.

Characteristics of pain (SOCRATES) Site Somatic pain often well localized, e. g. costochondritis Visceral pain more diffuse, e. g. angina pectoris Onset Speed of onset and any associated circumstances, e. g. acute, subacute and chronic

Character Described by adjectives, e. g. sharp/dull, burning/tingling, boring/stabbing, crushing/tugging, preferably using the patient's own description rather than offering suggestions
Radiation Through local extension Referred by a shared neuronal pathway to a distant unaffected site, having same segmental innervation e. g. diaphragmatic pain at the shoulder tip via the phrenic nerve (C 3, C 4) Associated symptoms Visual aura accompanying migraine with aura Numbness in the leg with back pain suggesting nerve root irritation

Timing (duration, course, pattern) Since onset Episodic or continuous If episodic, duration and frequency of attacks If continuous, any changes in severity

Exacerbating and relieving factors Circumstances in which pain is provoked or exacerbated, e. g. food in gastric ulcer and pancreatitis. Specific activities or postures, and any avoidance measures that have been taken to prevent onset Effects of specific activities or postures, including effects of medication and alternative medical approaches

Severity Difficult to assess, as so subjective Sometimes helpful to compare with other common pains, e. g. toothache Variation by day or night, during the week or month, e. g. relating to the menstrual cycle

Common pain Chest Pain Chest pain may be due to any of the following conditions. Cardiac Causes Angina pectoris Myocardial infarction Pericarditis Acute dissection of aorta.

Chest pain Respiratory Causes Pleurisy. Chest Wall Causes Musculoskeletal pain Neuropathic pain

GI Causes Reflux oesophagitis Hiathus hernia Oesophageal spasm.

Angina pectoris It is a midline retrosternal constrictive, compressive or squeezing diffuse pain lasting for 3 -15 minutes. It may radiate to either arm, either shoulder, jaw, back and upper abdomen. It is aggravated by exertion, heavy meal, emotion.

It is relieved by rest or nitrates. Usually the patient lies still. When there are no risk factors for ischaemic heart disease, precordial pain in a young individual or a fertile female is mostly non-ischaemic.

Myocardial infarction (MI) Pain in MI is a similar anginal pain of spontaneous origin lasting for more than 30 minutes, but the intensity is very severe. In contrast to angina, this pain is not rapidly relieved by rest or coronary dilators.

Myocardial infarction (MI) It may be accompanied by autonomic distrubances like diapho- resis, nausea, hypotension and a feeling to defacate. Patient is usually restless.

Pericardial Pain It is a steady substernal discomfort that mimics the pain of MI, it is worsened by lying down and is relieved by sitting and leaning forward. Often pain may be pleuritic, consequent to accompanying pleural inflammation.

Pain in Acute aortic Dissection The pain is of abrupt onset, tearing in nature, reaches a peak rapidly and is felt in the centre of the chest and/or the back between shoulder blades depending on the site of aneurysm.

Pain in Acute aortic Dissection This pain lasts for many hours and is not aggravated by changes in position or respiration. It is associated with unequal or absent pulses.

Pleural pain It is a sharp, knife like, localised superfical pain. aggravated by deep inspiration and coughing due to stretching of the inflamed parietal pleura and is relieved by lying down on the affected side due to restricted movement of chest on the same side.
Pleural pain In diaphragmatic pleurisy, pain arising from central tendinous portion of the diaphragm is felt characteristically at the tip of the shoulder, trapezius ridge and the neck since the central part of diaphragm receives sensory supply from phrenic nerve (C 3, 4, 5).

Pleural pain Pain may radiate down to upper abdomen when peripheral part of diaphragmatic pleura (supplied by 6 th to 12 th intercostal nerves) is involved simulating acute abdomen
Musculoskeletal pain Costo-chondral and chondro-sternal articulations are most commn sites of anterior chest pain may be darting and lasts for a few seconds or it may be a dull ache lasting for hours or days.

Musculoskeletal pain Tiezte’s Syndrome Painful swelling fo one or more costo-chondral articulations, usually second or third.

Neuropathic pains have an unusual buring, thingling or electric shock like quality. Pain is triggered by very light touch and on examination.

Neuropathic pain sensory deficit is characteristically present in the corresponding dermatome, e. g. damage to peripheral nerves as in diabetic polyneuropathy or peripheral afferents as in herpes zoster.

Abdominal pain results from GI disease and extraintestinal conditions involving the genitourinary tract, abdominal wall, thorax, or spine. There are four types of abdominal pain: Visceral, Parietal, Referred pain and Psychogenic.

Visceral- Gut organs are insensitive to stimuli such as burning and cutting but are sensitive to distension, contraction, twisting and stretching. Pain from unpaired structures, such as the pancreas, is usually but not always felt in the midline. Pain from paired structures is felt on and radiates to the affected side, e. g. renal colic.

Pain arising from foregut structures (stomach, pancreas, liver and biliary system) is localized above the umbilicus. Pain arising from midgut structures(small intestine and colon upto right two-third of transverse colon) is felt around the umbilicus (periumbilical).
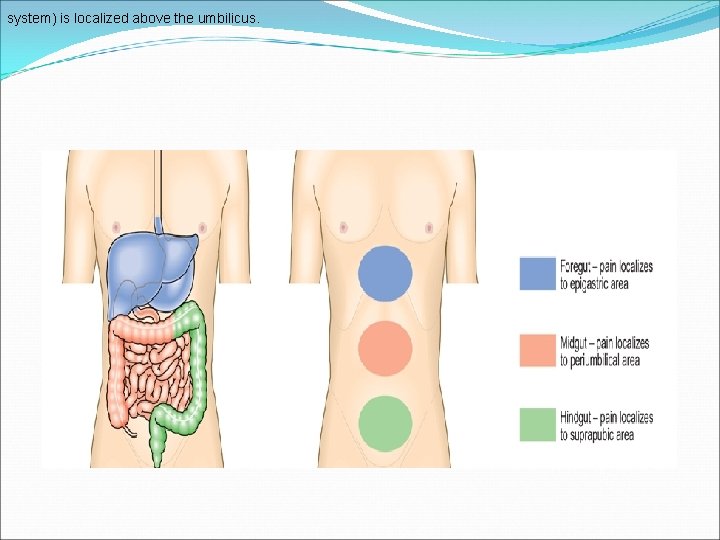
system) is localized above the umbilicus.

If the parietal peritoneum is involved, the pain will localize to that area, e. g. right iliac fossa pain in acute appendicitis and in Crohn's disease of the terminal ileum. Pain arising from hindgut structures (distal 1/3 rd of transverse colon and rest of the colon) is localized below the umbilicus (suprapubic region).

Parietal- The parietal peritoneum is innervated by somatic nerves, and its involvement by inflammation, infection or neoplasia causes sharp, well localised and lateralised pain.

Referred pain. Pain referred to the abdomen from the thorax, spine, or genitalia may prove a deficult diagnostic problem, because diseases of the upper part of the abdominal cavity such as acute cholecystitis or perforated ulcer are frequently associated with intrathoracic complications.

To evaluate abdominal pain, the possibility of intrathoracic disease must be considered in every patient with abdominal pain, especially if the pain is in the upper part of the abdomen.

Systematic questioning and examination directed toward detecting myocardial or pulmonary infarction, pneumonia, pericarditis, or esophageal disease (the intrathoracic diseases that most often masquerade as abdominal emergencies) will often provide sufficient clues to establish the proper diagnosis

In contrast to this, abdominal pain may refer to other part of the body (For example, gallbladder pain is referred to the back or shoulder tip. ).
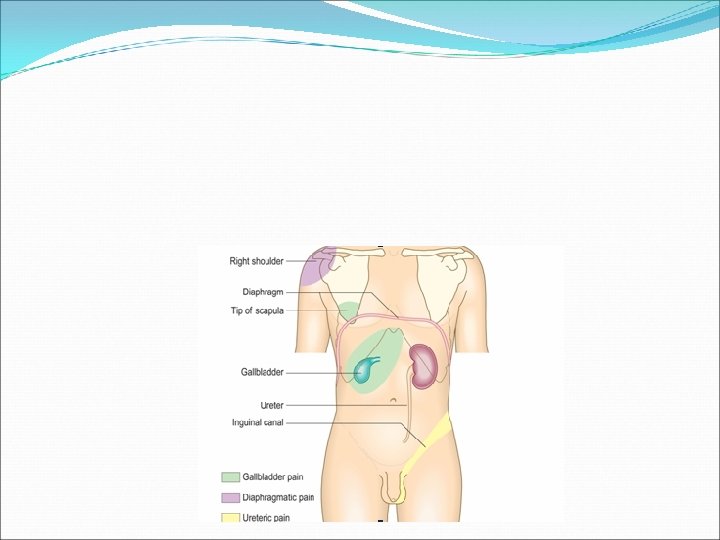

Psychogenic- Cultural, emotional and psychosocial factors influence everyone's experience of pain. In some patients, no organic cause can be found despite investigation, and psychogenic causes (depression or somatisation disorder) may be responsible.

Abdominal pain may present as acute abdominal pain or chronic/recurrent abdominal pain. Acute abdominal pain (The acute abdomen) is a consequence of one or more pathological processes : Inflammation, Perforation and Obstruction

Some important causes of abdominal pain: Inflammation of peritoneum Mechanical obstruction to hollow viscera Vascular disturbances Abdominal wall causes (trauma or infection of muscles)

Some important causes of abdominal pain: Distention of visceral surfaces (hepatic or renal capsules) Referred pain from extra-abdominal sources (pneumonia, IHD, spine, genitalia) Metabolic causes (DKA, porphyria, uraemia, etc. ) Neurogenic causes.

Pain due to Disorders of GIT Oesophagal pain This may be either due to oesophageal spasm or due to reflux oesophagitis. In case of oesophageal spasm, the pain is retrosternal and mimics anginal pain. In case of reflux oesophagitis, the pain is retrosternal and has a burning character, usually occurring about 1 hour after a meal.

Peptic Ulcer pain Duodenal ulcer: It is often an episodic, recurrent epigastric pain described as sharp, burning or illdefined. It characteristically occurs from 90 minutes to 3 hours after eating and awakens the patients from sleep. Pain is relieved by food, antacids or H 2 blockers.

Changes in character of pain suggests development of complications: pain radiating to back- penetration of ulcer Pain aggravated by food and accumpanied by vomiting - Gastric outlet obstruction

Changes in character of pain suggests development of complications: abrupt, severe abdominal pain- perforation of ulcer When accompanied by coffee ground vomitus and melena- Ulcer bleed Some patients with duodenal ulcer have no symptoms.

Gastric ulcer: Epigastric pain, which is worsened by taking food and is relieved by vomiting. Relief with antacids is less consistent than that of duodenal ulcer pain.

Mechanical small bowel obstruction In this condition, the colicky pain is mid abdominal which tends to be more severe in case of high obstruction. pain occurs in paroxysms and the patient is comfortable in between the pains. Borborygmi is heard during episodes of pain.

Later, pain becomes less severe as the motility is impaired in the oedematous intestine. If there is strangulation of gut, pain is steady, severe, localised, without colicky nature. Pain of small bowel obstruction is accompanied by faeculent vomiting, and obstipatin (No passage of faces or gas)

Colonic Obstruction Colicky abdominal pain is of much less intensity, felt at any site over abdomen depending on the part of colon involved, e. g. hypogastric pain in sigmoid colonic involvement. Faeculent vomiting is rare, Constipation progresses to obstipation,

Pain in Acute Appendicitis In the initial stages, pain is poorly localised in the periumbilical or epigastric region. As inflammation spreads, pain becomes somatic, more severe and is localised to right lower quadrant.

Pain in Acute Appendicitis Pain is accompanied by anorexia, nausea, vomiting and fever. Tenderness at Mc. Burneys point (junction of medial 2/3 and lateral 1/3 of spinoumbilical line) is elicited later.

Acute Pancreatitis In acute pancreatitis, there is a severe, constant epigastric pain radiating to the back, lasting for 24 hours. pain is aggravated by taking alcohol or fatty food and is relieved by sitting upright or mohmadan’s prayer position.

Acute Pancreatitis pain may by associated with vomiting, jaundice, paralyti ileus, and shock. there is profound elevation of amylase levels.

Biliary Colic Acute distention of gallbladder causes pain in the right hypochondrium with radiation to the right posterior region of thorax or to the tip of right scapula. Distention of common bile duct (CBD) causes pain in the epigastrium radiating to upper part of lumbar region.

Biliary Colic Murphys sign: In acute cholecystitis, the patient is asked to breathe in deeply and galbladder is palpated in the usual way, At the height of inspiration, the breath is arrested with a gasp as the mass is felt.

Pain of peritonitis It is a steady and aching pain located directly over inflammed area. The pain is accentuated by pressure or changes in tension of the peritoneum and hence the patient lies still. There is associated tonic muscle spasm.

Pain of peritonitis The intensity of pain is dependent on the type and amount of foreign substance to which the peritoneal surfaces are exposed. If the peritonitis is due to perforeation of a hollow abdominal viscera, liver dullness is obliterated.

Superior Mesenteric Artery Occlusion It is a mild, continuous, diffuse pain present for 2 to 3 days before vascular collapse or peritonits sets in, There is no tenderness or rigidity. Bloody diarrhoea may be present. In chronic mesenteric artery insufficiency, abdominal pain occurs after intake of food (abdominal angina).

Pain Referred to Abdomen Possibility of intrathoracic disease must be considered in every patinet with abdominal pain. Apparent abdominal muscle spasm caused by referred pain will diminish during inspiration whereas it is persistent throughout respiratory phases, if it is of abdominal origin.

Pain Referred to Abdomen Pain of diaphragmatic pleuritis is felt at right upper quadrant of abdomen. Referred pain from spine is characteristically intensified by certain motions like coughing, sneezing or straining and is associated with hyperaesthesia over involved dermatomes.

Pain Referred to Abdomen Pain referred from testicles or seminal vesicles is accentuated by slightest pressure on either of these organs. The abdominal discomfort is of dull aching character and is poorly localised.

Abdominal Wall Pain It is a constant, aching pain aggravated by movement, Prolonged standing and pressure. When muscles of other parts of the body are also involved, myositis should be considered.

Metabolic Causes of Abdominal Pain. Whenever the cause of abdominal pain is obscure, one of the following metabolic causes must be considered. Diabetic ketoacidois Porphyria

Metabolic Causes of Abdominal Pain Uraemia Lead colic Hyperlipidaemia C 1 esterase deficiency(angioedema).

Neurogenic Abdominal Pain Causalgic pain is of burning character and is limited to the distribution of peripheral nerve. Normal stimuli like touch can evoke this type of pain. There is no muscle spasm or change with respiration or food intake.

Neurogenic Abdominal Pain from spinal nerves or roots is of lancinating type. It may be caused by herpes zoster, arthritis, tumours, herniated nucleus pulposus, diabetes, syphilis. Pain is aggravated by movement of spine and is usually confined to a few dermatomes. Hyperasthesia is common.

Psychogenic Abdominal Pain There is no relation to meals. Onset is usually at nights. There is no nausea or vomiting. There is no abdominal muscle spasm, even if present does not persist. There is no change with respiration. But restriction of depth of respiration occurs as a part of anxiety state.

Renal Pain due to obstruction of urinary bladder causes a dull suprapubic pain of low intensity. Pain due to ureteric obstruction (intravesical portion) is characterised by severe suprapubic and flank pain which radiates to genitalia and upper part of thigh.

Renal Pain Obstruction of pelviureteric junction causes pain at costovertebral angle. whereas obstruction of the remainder of the ureter is associated with flank pain which radiates from loin to groin.
Peripheral Vascular Pain Arterial Occlusion Intermittent Claudication Patient often complains that after walking a distance (claudication distance) the pain starts in calf muscles and on continued walking the pain is aggravated and compels the patient to take rest. Pain disappears when the patient stops walking.

Rest Pain This pain is continuous and aching in nature. This is due to ischaemic changes in the somatic nerves (cry of the dying nerves). Venous Pain Venous pain may be due to: Varicose Veins, Venous Thrombosis

Varicose Veins Pain felt in lower leg or whole of the leg according to the site of varicosities. Pain gets worse when the patient stands on the site of varicosities and for a long time and is relieved when he lies down. Pain of varicocele of testes is of similar character.

Venous Thrombosis Patient may have pain and swelling of leg. Homan’s sign: Dorsiflexion of foot elicits pain in the calf. The above maneuver may dislodge thrombus resulting in pulmonary embolism. In superficial thrombophlebitis, there is pain and tenderness over superficial inflamed veins.

Neurogenic Claudication Symptoms of dysfunction of cauda equina appear on walking or prolonged standing and are relieved by rest. This is due to lumbar canal stenosis which is made worse in middle age due to degenerative change especially between L 4 and L 5 vertebrae.

There is march of pain with paraesthesia and absent ankle jerk after exercise. Symptoms take 5 -10 minutes to fade.

Headache Pain in and around vault of the head is called headache.

THANK YOU
- Slides: 85