Pain Disability Management Consultants P C Directions in

Pain & Disability Management Consultants, P. C. “Directions in Healing” Stephen M. Thomas, M. D. , MBA 105 Braunlich Drive Suite 410 Pittsburgh, PA 15237 412 -635 -2920 Fax 412 -635 -9677

Narcotics and the Injured Worker Opioid Therapy: Wishes meet Reality

Disclosures � This is a program length commercial for the services of PDMC. � IME, Record Review, UR, case consultation and excellent patient care. � “If you tell the truth, you don't have to remember anything. ” --Mark Twain

Objectives of this presentation � How did the pain medicine business currently plaguing the U. S. develop? � What are the systemic and societal aspects of the problem of which you should be aware? � How can one recognize appropriate opioid prescribing? � How do all of the above uniquely impact the injured worker? � Is there any hope?

Give Up All Hope… � V. B. was injured in 1997 at the age of 35 years, falling from a ladder, sustaining a lumbar injury. Early opioid therapy. Two years until first operation: lumbar fusion in the absence of instability. Two additional lumbar operations. � IME 2007: lack of analgesia and loss of control despite liberal prescribing. Smoker. Discharged from pain management practice. (continued)

Give Up All Hope… Ø IME 2011: Untrained Pain Doctor. Oxy. Contin 80 mg, 2 three times daily, Opana ER 40 mg twice daily, Oxycodone 30 mg six times daily, Skelaxin 800 mg three times daily, Valium 10 mg three times daily, Neurontin 300 mg nightly, Seroquel, Wellbutrin, and Voltaren gel. Ø Serum levels obtained: 3 X therapeutic level Ø Doctor thought the levels were too low!

Give Up All Hope… R. I. P. --2012

FYI: I shouldn’t be doing this! “…to give share of precepts and oral instruction and all other learning to my sons and to the sons of him who has instructed me and to pupils who have signed the covenant and have taken an oath according to the medical law, but to no one else. ---Hippocrates, the Oath
PAIN “An unpleasant sensory experience associated with or described in terms of tissue damage. ” --IASP

Patient Selection “Some things work for some people some times. ” --Thomas

Plight of the Medical Profession “In the middle of the road of my life, I awoke in a dark wood and the true way was wholly lost. ” --Dante, La Comedia

The Road…

A Little History � Opium extracted from the poppy by the Sumerians for the treatment of dysentery, 3400 BCE. � Morphine extracted from opium by Serturner (1806) � Oxycodone synthesized from thebaine in ~1917. � Purdue Pharma has been extracting money from everybody since the introduction of Oxy. Contin in 1995.

Narcotics � Harrison Narcotics Act of 1914 "An Act to provide for the registration of, with collectors of internal revenue, and to impose a special tax on all persons who produce, import, manufacture, compound, deal in, dispense, sell, distribute, or give away opium or coca leaves, their salts, derivatives, or preparations, and for other purposes. " The courts interpreted this to mean that physicians could prescribe narcotics to patients in the course of normal treatment, but not for the treatment of addiction.

1965 Methadone Maintenance Dole and Nyswander

1996 “Consensus Statement on the Use of Opioids in the Treatment of Chronic Pain” APS and AAPM

Joint Commission on the Accreditation of Hospital Organizations (JCAHO) May 1999 “Pain: The 5 th Vital Sign”

Verbal Digital Pain Score 0_1___2____3_____4___5_6_7_8910 (Calculus with an imaginary ruler)

Visual Analogue Scale (VAS) No pain______________________Worst pain (Every picture tells a story, don’t it…? )

Pain Medications Aspirin Acetaminophen Morphine

Papaver somniferum

The “Morphines” Ø Morphine (MSContin) Ø Hydrocodone (Vicodin) Ø Oxycodone (Oxy. Contin) Ø Methadone (Dolophine) Ø Fentanyl (Duragesic, Actiq, Fentora) Ø Oxymorphone (Opana) Ø Hydromorphone (Dilaudid, Exalgo) Levorphanol, Meperidine, Heroin, et al.
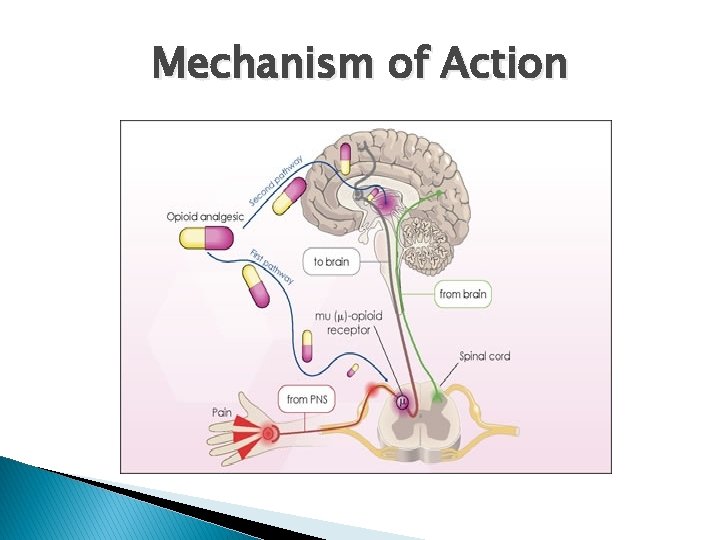
Mechanism of Action

Potency Fentanyl (70) Hydromorphone (5) Oxymorphone (4) Oxycodone (2) Methadone (1. 5) Morphine (1) Hydrocodone (0. 8)

Opioid Effects Analgesia Sedation Euphoria Blunting of airway reflexes Constipation

Acute Opioid (Side) Effects ØRespiratory depression ØNausea / vomiting ØSedation ØEuphoria / dysphoria ØConfusion ØBlunting of airway reflexes ØUrinary retention ØPoikilothermia (temperature dysregulation) ØPruritis (itching)

Chronic Opioid (Side) Effects � Secondary hypogonadism � Adrenal suppression � Sleep disturbance � Depression/anhedonia
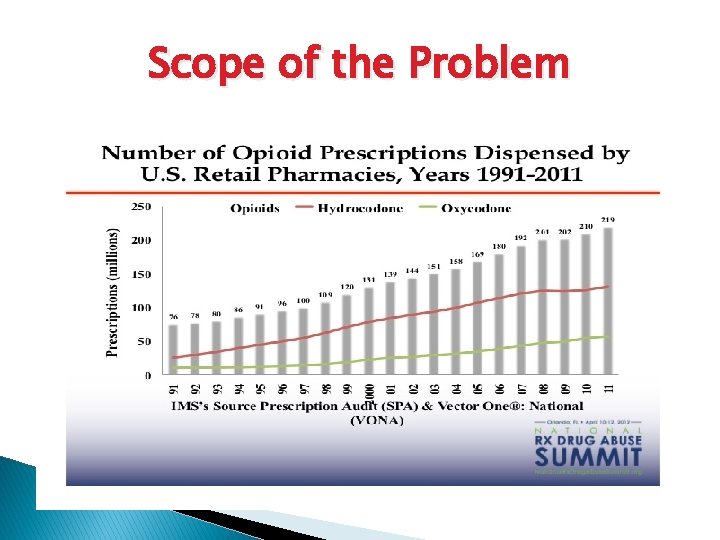
Scope of the Problem

How much? !! 1997 – 96 mg Morphine equivalence person 2007 – 700 mg Morphine equivalence person ~ 300, 000 people taking 5 mg Hydrocodone every 4 hours for 3 weeks!

Doctors are the problem. �In California Workers’ Compensation system, 3% of the physicians prescribe 65% of the Schedule II analgesics. � (Well, maybe not all of us, not the entire problem. )

Opioids How can we distinguish appropriate from inappropriate use? What does it mean for these drugs to “work”?

Telling the Difference � Dose and frequency (lower and less often) � Route of Administration � Expectation euphoria) � Context of Drug Effect (analgesia versus of Use (home, work, bar, scheduled)

“Model Policy for the Use of Controlled Substances for the Treatment of Pain” Federation of State Medical Boards of the United States, Inc. , 2004 Evaluation of the Patient Ø Treatment Plan Ø Informed Consent and Agreement for Treatment Ø Periodic Review Ø Consultation Ø Medical Records Ø Compliance with Controlled Substances Laws and Ø Regulations

Guidelines � � � “Clinical Guidelines in the Use of Chronic Opioid Therapy in Chronic Noncancer Pain, ” Chou, et al. , J of Pain, 2009. (APS/AAPM) “Management of Opioid Therapy for Chronic Pain, ” VA/Do. D Evidence Based Practice, 2010 “Canadian Guideline for Safe and Effective Use of Opioids for Chronic Noncancer Pain, ” Federation of Medical Regulatory Authorities of Canada, 2010 “Interagency Guideline on Opioid Dosing for Chronic Noncancer Pain, ” Washington State Agency Medical Directors, 2010 ASIPP Guidelines for Responsible Opioid Prescribing in Chronic Noncancer Pain, Part 1 and Part 2, Pain Physician, 2012 --My i. Pad

And now the bad news…

The Evidence � Opioid prescribing has increased dramatically over the last 20 years. � Non-medical use of opioids has increased dramatically over the last 20 years. � Short-term effectiveness of opioids is fair (50%). � Long-term (> 16 weeks) effectiveness is unknown --Pain Physician, 2012

Studies showing long-term opioid effectiveness

Oops…! People are dying. --CDC, 2010
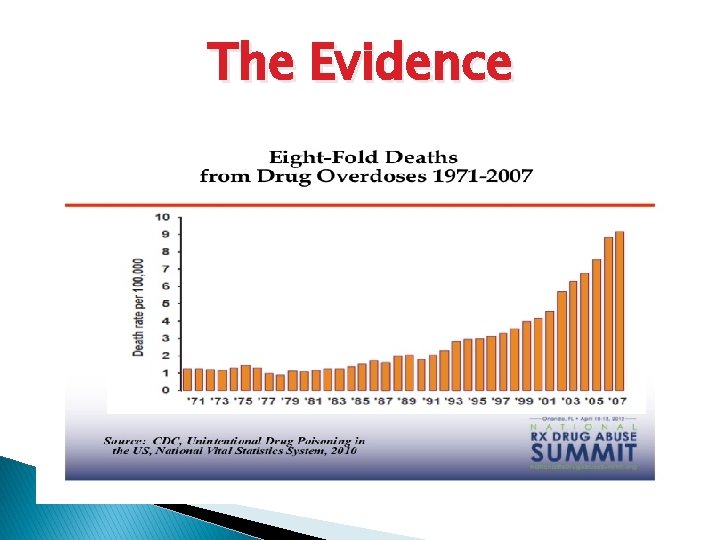
The Evidence

27, 000 Deaths due to overdose --CDC, 2007
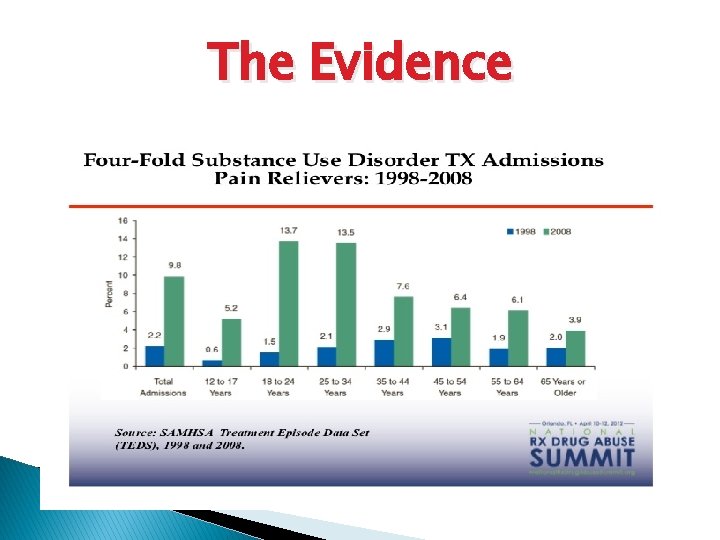
The Evidence
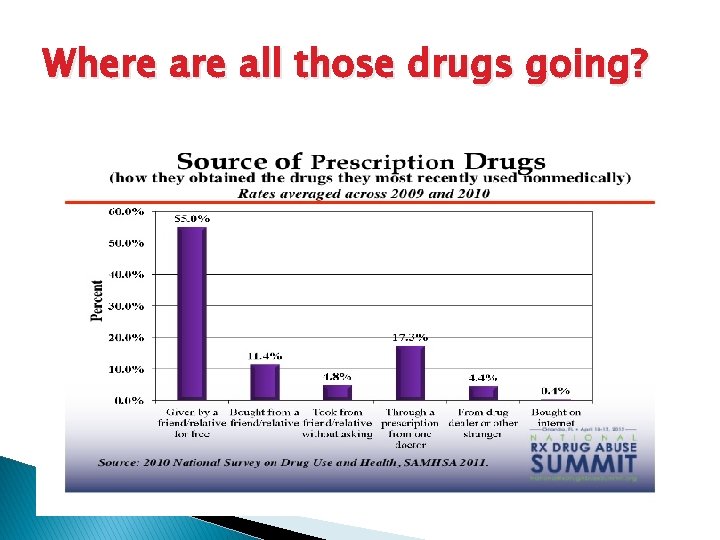
Where all those drugs going?

Scope of the problem � Employers and insurers spent an estimated $1. 4 billion on narcotics in Worker’s Compensation claims in 2012. � Oxy. Contin is the most prescribed drug in Worker’s Compensation. � After opioid treatment likelihood of return to work falls.

Death Among Injured Workers � 2, 378 injured workers underwent lumbar fusion surgery 1994 to 2001. � 103 (1. 9%) died by 2004. � Twenty-one (21%) percent of the deaths were analgesic-related. Associated with reoperation, instrumentation and DDD as the diagnosis for fusion. � Age 45 -54 years. --Spine, 2009, 34(7): 740 -747

Exclusion Criteria � A history of alcohol abuse and/or dependence. � Any history of illicit drug use (cannabinoids, cocaine, etc. ) � Any history of unauthorized escalation of therapeutic drugs such as benzodiazepines, e. g. , Valium, Xanax. � Any history of other addictive behaviors. � Heavy smokers with inability to quit. � First-degree relatives of addicted individuals.

Drug Screening � Urine, saliva, sweat, blood and hair can all be tested for the presence or absence of drugs. � Urine is the standard fluid with the greatest amount of data. Saliva is favored by the entrepreneurial tester. � Screening shows the presence or absence of the drug not the manner in which it was taken. This is its major limitation.

Urine Drug Screening � No established standards. 2 -4 times per year. � Screening is best in the presence of a high pretest probability of disorder, e. g. , initial presentation, randomly and for cause. � Cross-reactivity can result in false positives. Confirmatory testing is necessary. � Negative may not be negative. Cutoff values are important. � Costs rising. Benefits unclear. Sound familiar?

Pill Counts �While not foolproof, when added to urine drug screening pill counting gives an integral view (use over time) of the patient’s medication-taking behavior.

How did we get here and why stay? “Why Doctors Prescribe Opioids to Known Opioid Abusers” � Primacy --Lemke, NEJM, 2012; 367: 1580 -1581 of self-report. � Fear of poor patient evaluation. � Fear of litigation. � A society where the belief exists that “all suffering is avoidable. ” � Pain pays. Addiction does not.

“The world we have made as a result of the level of thinking we have done thus far creates problems we cannot solve at the same level of thinking at which we created them. ” --Einstein

AEQUIP SM Analgesic Effectiveness Quality Improvement Program A unique cooperative, incentivized approach in a two-sided network of physicians and insurers to assure the safest, simplest and most effective drug therapy for injured Pennsylvania workers.

What if…? �Six out of ten (60%) of physicians surveyed would agree to prescribing safely, simply and effectively for an incentive payment. �How much would you pay in year one to forgo $100 in ongoing prescription costs?

Thank you! sthomas@pdmconsultants. info jwade@pdmconsultants. info
- Slides: 53