Pain control and controlled drug prescribing Gayle Munro

Pain control and controlled drug prescribing Gayle Munro Specialist Pharmacist 22. 03. 10

Types of pain Somatic Activation of pain receptors in either cutaneous or deep tissues (muscoloskeletal) Cutaneous – sharp, burning, pricking Deep – dull, aching (eg. bone mets)
Types of pain Visceral Internal areas of the body enclosed within Cavity. Pain caused by infiltration, compression, extension or stretching of the thoracic, abdominal or pelvic viscera eg. liver capsule pain.
Types of pain Neuropathic Damage to the nervous system: Compression of nerves/spinal cord Infiltration of nerves/spinal cord Chemical damage – chemotherapy/XRT Burning/tingling

Types of pain All 3 types of pain can be acute or chronic Acute: short-lived Chronic: at least 3 month duration Other factors affect the perception of pain: Mood – depression, anxiety Context – expectation, pain beliefs, placebo

Treatment Pain can adversely affect a patient’s life in many ways: Personality Quality of life Ability to function Good pain control is important
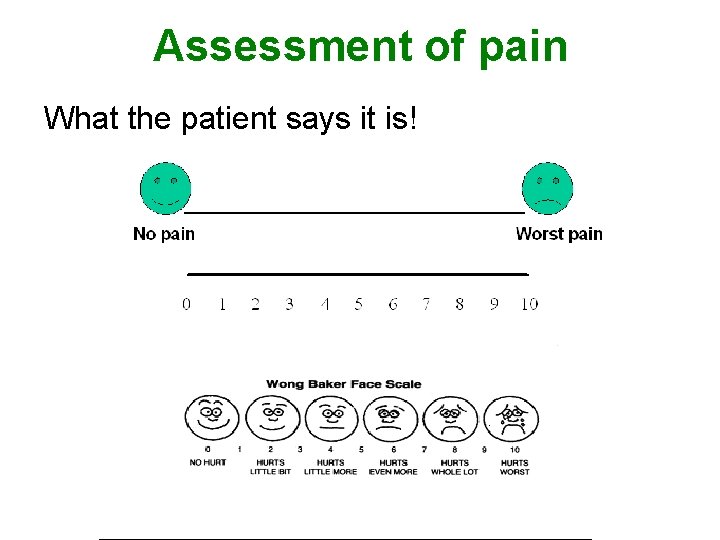
Assessment of pain What the patient says it is!

Treatment Assess cause of pain Review current medication Initiate treatment or Step up the pain ladder or Add adjuvant drug

WHO Pain Ladder MILD: Paracetamol MILD to MODERATE: Co-codamol 30/500, dihydrocodeine, tramadol MODERATE to SEVERE: Morphine, diamorphine, oxycodone, hydromorphone, Methadone ADJUVANT: NSAID’s, TCA’s, anticonvulsants, corticosteroids, anxiolytics, muscle relaxants, antimuscarinics

Controlled Drug Prescribing • Patient’s name and address • Name of drug and the FORM eg. tablet, patch • Dose and frequency of administration • Strength to be supplied • Total quantity in words and figures e. g. for MST 40 mg bd 7 day supply 14 (fourteen) 10 mg tablets and 14 (fourteen) 30 mg tablets

Opioids Act on opiod receptors: Mu, kappa Initial side-effects N&V, drowsiness, unsteadiness, confusion On-going side-effects Constipation Occasional side-effects Dry mouth, sweating, pruritus, hallucinations, myoclonus Rare Respiratory depression, psychological dependence
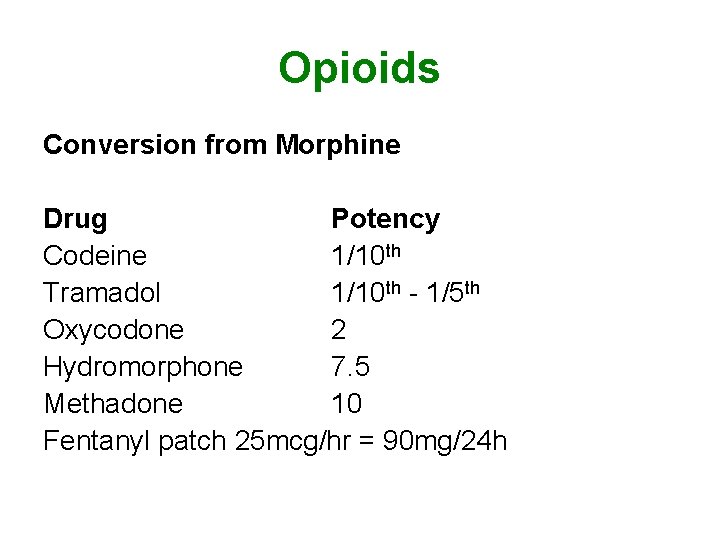

Opioids Conversion from Morphine Drug Potency Codeine 1/10 th Tramadol 1/10 th - 1/5 th Oxycodone 2 Hydromorphone 7. 5 Methadone 10 Fentanyl patch 25 mcg/hr = 90 mg/24 h

Opioids Convert co-codamol 30/500, 2 tabs qds to MST in a patient who has used 4 breakthrough doses of oramorph 10 mg in 24 hours.

Opioids Convert 60 mg bd of MST to Oxycodone Hydromorphone What would the breakthrough dose be? What other regular medication should be prescribed?

Opioids Oral to subcutaneous route Oral Morphine Oxycodone Hydromorphone Morphine Subcutaneous Morphine ÷ 2 Diamorphine ÷ 3 Oxycodone ÷ 2 Hydromorphone ÷ 2* Fentanyl ÷ 200** Alfentanil ÷ 30** *Different ranges quoted in the literature **Seek advice from HPCT

Opioids Convert a fentanyl 50 mcg/hr patch to a diamorphine syringe driver. The patient is stabilised on diamorphine 90 mg/24 hrs after titration of the dose. Convert back to a fentanyl patch. What issues do you need to consider?

Opioid Choice Morphine most commonly used Oxycodone/Hydromorphone – less CNS side-effects Fentanyl – less constipation Fentanyl/Alfentanil – good in renal Impairment (shorter half-life)

Opioids Management of side-effects Initiation of opioid – antiemetic for first few days Regular laxative Hallucinations – haloperidol (nausea) or switch Myoclonus – reduce dose, switch or benzodiazepine Drowsiness – reduce dose or switch Pruritus – antihistamine or switch if does not settle Respiratory depression - naloxone

Adjuvant Drugs Can be used at any point in the pain ladder NSAID’s bone pain (watch renal function, other medicines, platelet count) Diclofenac 50 mg tds (rectal route available) Corticosteroids Reduce inflammation (cerebral mets, spinal cord compression, liver capsule pain), stimulate appetite, antitumour effect (lymphoma etc)

Adjuvant Drugs Neuropathic pain TCA’s amitriptyline (small doses may suffice) Anti-convulsants Carbamazepine 100 -200 mg tds Na Valproate 200 mg tds Gabapentin titrate dose gradually 300 mg nocte day 1, 300 mg bd day 2, 300 mg tds day 3 then increase up to 900 mg tds. Elderly patients, start with a 100 mg dose and titrate. Watch renal function.

Adjuvant Drugs Anxiolytics (agitation, dyspnoea) Agitation, dyspnoea Diazepam 2 mg tds Lorazepam 0. 5 -1 mg Sub-lingual 8 -12 hrly Midazolam 2. 5 mg s/c or 10 -30 mg via syringe driver Muscle Relaxants (muscle spasm pain) Diazepam 2 mg tds prn Baclofen 5 mg tds increased every 3 days to 20 mg tds Antimuscarinics (colic) Hyoscine Butylbromide 20 mg qds

Adjuvant Drugs Ketamine Reduces opioid requirement Neuropathic pain – HPCT advice Oral 50 mg in 5 ml – titrate dose usually start 10 mg (1 ml) qds Subcut – usually start 50 mg/24 hrs and titrate Side-effects - hallucinations

Adjuvant Treatment • A single fraction of radiotherapy can be used for pain control

Answers Co-codamol 30/500 2 tabs qds = 240 mg codeine ÷ 10 = 24 mg morphine + 40 mg from breakthrough = 64 mg morphine Give MST 30 mg bd + 10 mg oramorph hourly as required for breakthrough pain (1/6 th total daily dose)

Answers Oxycodone is twice as potent as morphine therefore divide morphine dose by 2 Give oxycodone sustained release tablets (oxycontin) 30 mg bd with oxycodone normal release (oxynorm) 10 mg hourly as required for breakthrough pain Hydromorphone is 7. 5 times more potent therefore divide morphine dose by 7. 5 Give hydromorphone sustained release capsules 8 mg bd with hydromorphone normal release capsules 2. 6 mg hourly as required for breakthrough pain Always prescribe a laxative

Answers Fentanyl 50 mc/hr patch is equivalent to oral morphine 180 mg in 24 hours. Divide oral morphine dose by 3 to get diamorphine dose. Give 60 mg diamorphine subcutaneously via syringe driver over 24 hours To convert subcutaneous diamorphine back to oral morphine multiply by 3 = 270 mg morphine which is equivalent to a 75 mcg/hr fentanyl patch. It takes 12 -24 hours after a fentanyl patch is started to reach steady state and 12 -24 hours after a patch is removed for the reservoir of drug in the skin to be depleted. When changing from a syringe driver to a patch, keep the driver going for approx 12 hours after the patch has been applied.

Questions ?
- Slides: 27