PAIN ASSESSMENT Ayesha Palihawadana Nursing Officer Colombo North

PAIN ASSESSMENT Ayesha Palihawadana Nursing Officer – Colombo North Teaching Hospital Batch No: 9 th OUM

Objectives • Understand how the assessment of pain affects the quality of life of a patient. • Understand the pain assessment goals • Recognize different types of pain that patient can experince • To identify the barriers when assess the pain. • Recognize different types of pain. • Understand that all team members have a role in assessment and treatment of pain.

Pain Assessment Goals • Characterize the pain- Temporal features, Intensity, location, quality, alleviating factors • Infer Pathophysiology • Evaluate physical & psychological factors • Assess degree and nature of disability • Develop a therapeutic strategey stimulation
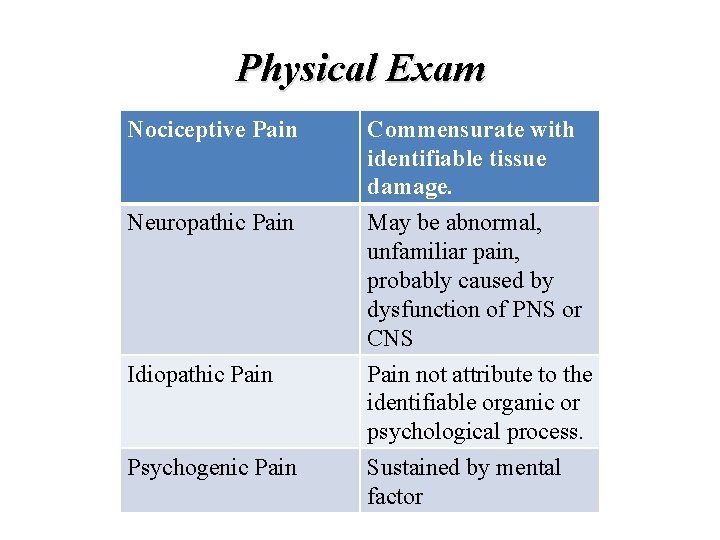
Physical Exam Nociceptive Pain Neuropathic Pain Idiopathic Pain Psychogenic Pain Commensurate with identifiable tissue damage. May be abnormal, unfamiliar pain, probably caused by dysfunction of PNS or CNS Pain not attribute to the identifiable organic or psychological process. Sustained by mental factor

Nociceptive Pain • • Pain is consistent with the degree of tissue injury Sub types Somatic – Well localized, described as sharp, aching, throbbing Visceral- More diffuse, described as growing cramping

Nursing Assessment & Interventions • To provide effective pain management, nursing assessment, physical examination, and review of laboratory values are very important. See standards of care guidelines. 1. Screen for pain at each visit. Evaluate objectively the nature of the patient’s pain, including, • • . Location / Distrubuting or etiology of pain, if identifiable Duration, Quality Impact on daily activities.

Con. . • Chronicity • Severity • Contributing associated factors • Barriers to pain assessment There are two thresholds-Pain perception & Pain tolerance • Pain self assessment is the most reliable guide to both cause of the pain & the effectiveness of pain treatment

Nursing Interventions… • Assess patient history and physical examination findings and laboratory values to differentiate expected pain from pain due to a new problem, an oncologic complication, or worsening of the underlying process. • Use a pain intensity scale of 0 (no pain) to 10 (worst possible pain) or other pain scale as appropriate. • Take careful history of prior and present medications, response, and adverse effects. • Assess relief from medications and duration of relief. • Base the initial analgesic choice on the patient’s report of pain.

Con. . • Administer drugs orally whenever possible, avoid I. M. injection. • Administer analgesia “around the clock” rather than as needed. • Convey the impression that the patient’s pain is understood and that the pain can be controlled. • Take a careful pain history. Explore pain interventions that have been used and their effectiveness. Determine whether the intensity of the pain correlates with the prescribed analgesic. • Reevaluate the pain frequently. The requirement for analgesia should decrease if other treatment is given, including radiation or chemotherapy.

Con. . • Use alternative measures to relieve pain such as guided imagery, relaxation, & biofeedback. • Provide ongoing support & open communication. • Assess bowel function & institute bowel regimen immediately. • Consider referral to a pain specialist for interactable pain. • Instruct patients that there is no benefit to suffering and that addiction is not a problem. a. Instruct patients that taking these medications now does not mean that they will not work later. b. Encourage patients to talk to their physician or nurse about their pain & effectiveness of treatment plan.

Con. . • Establish supportive relationship with the patient. • Respect patient’s response to pain & management. • Educate the patient regarding methods of pain relief, preventive measures, and expectations. • Monitor patient’s response to and effectiveness of treatment. • Assure patients that there are other options if the medications prescribed do not work.

Comprehensive Pain Assessment • Pain intensity (Numerical scale) “On a scale of 0 to 10, what would be your pain rating if 0 means no pain & 10 means the worst pain you can imagine” - At rest -With movement • Location, referral pattern, radiation of pain • History -Onset -Duration -Course -Aggravating or associated symptoms

Con. . • a. b. c. Quality Persistent, intermittent Aching, stabbing, throbbing, pressure somatic pain Cramping, aching, sharp-visceral pain Sharp, tingling, burning, shooting-neuropathic pain Psychosocial Family & other support Cultural/spiritual beliefs about pain & pain management. Response to pain relief and adverse effects.

Barriers To Pain Assessment • Clinician related barriers • Patient related barriers

Patient Related Barriers • • • Reluctance to report pain Reluctance to take opiods drugs Poor adherence Reluctance to ask drugs Inappropriate fear of addiction

Clinician Related Barriers • • • Lack of pain management in training Insufficient knowledge Lack of pain assessment skills Rigidity or timidity in prescribing practices Fear of regulating oversight.

Characterize the Pain • • • Temporal features-Onset, duration Intensity – average, current pain Location-focal, multifocal, generalized Quality- aching, throbbing, stabbing Alleviating factors- Positions, activity, weight bearing

Pain Assessment Tools • The presently available pain measures fall into two categories: single-dimensional scales and multidimensional scales The results obtained from these instruments must be viewed as guides and not absolutes.

Pain Assessment in Elderly • Pain assessment can be particularly difficult in elderly patients for the following reason: • Underreporting of undiscomfort because the patient does not want to complain. • Decrease in hearing and visual acuity so that pain assessment tools that require extensive explanation or visualization to perform will be more difficult and possibly less reliable.

Pain Assessment in Infants • The following tools use a combination of behavioral physiologic measurements to assess pain in infants. a) § § § a) CRIES C- CRYING R-REQUIRE OXYGEN I-INCREASED VITAL SIGNS E-EXPRESSIONS S-SLEEPINESS Modified Behavioral Pain Scale. - Positions and Activities

References 1. Pain Assessment: Practice Essentials, Overview Technique. (Online). http: //emedicine. medscape. com/article 2. Sandra, M. et al. (2010). Pain in Cancer Patient. Lippincott Manual of Nursing. Volume(9), pp: 258 -259.

Questions On Pain Assessment. .

1. A patient in pain may • • a. Moan and groan b. Be depressed c. Be angry e. All of the above • The answer is “e”

2. Any patient in pain is suffering? • True or False • The answer is True

3. Patients may sleep in spite of severe pain? • True or False • The answer is False

4. The most accurate way to measure a patient’s pain is? • a. for the nurse and physician to observe the patient together • b. monitor vital signs for any changes • c. patient’s self-report • “C”

5. What factors about the patient’s pain must you know to develop a pain management plan? • • • a. description of the pain and its intensity b. location of the pain and when it started c. aggravating factors and previous treatments d. a and b e. a and b and c • “e”

6. Dull and aching commonly describe which type of pain? • • • a. visceral b. somatic c. Neuropathic d. nociceptive e. all of the above f. none of the above • “d”

7. Shooting, burning and tingling describe which type of pain? • • • a. visceral b. somatic c. Neuropathic d. nociceptive e. all of the above f. none of the above • “c”

8. Severe usually describes which type of pain? • • • a. visceral b. somatic c. Neuropathic d. nociceptive e. all of the above f. none of the above • “e”

9. Pain reported as “cramping, all over my lower stomach” usually describes which type of pain? • • • a. visceral b. somatic c. Neuropathic d. nociceptive e. all of the above f. none of the above • “a”

THANK YOU …
- Slides: 32