PAEDIATRICS FOR GPS Dr Laura Weidner MBCh B

PAEDIATRICS FOR GPS Dr Laura Weidner MBCh. B MRCGP PGCMDE GP partner / new trainer at Southmead Surgery

Introduction • Who am I & who are you? • Plan for the afternoon: Quiz, Cases, Rashes • Please share you own cases / experience • Resources

How are GPs unique? • Gatekeepers to hospital – know when to refer • Deal with all the minor childhood illnesses • Supporting parents in caring for their children day-to-day Practicalities of life as a GP – top things I think you need to know

WHAT DOES A GP HAVE TO KNOW ABOUT PAEDIATRICS? Team quiz…

Common GP Problems Case stories…

My child is constipated… Red flags – blood, faltering growth, meconium Think coeliac / hypothyroidism NICE - Movicol 1 st line +/- stimulant Movicol –licensed >5 faecal impaction and >2 chronic constipation • Maintenance = half dis-impaction dose • Ask diet / fluids / behavioural rewards / regular toileting • • NICE guidelines [CG 99] Published date: May 2010

My son’s foreskin doesn’t retract…. • By 3 y 90% have retractile foreskins • Of those that are not, 90% improve by age 15 y • Diprosone od 4 -6 w 70% success

My babies eyes are always sticky… • • • Imperforate valve of Muller 90% clear spontaneously Try lacrimal massage tds 20 squeezes for 3 m Refer 12 m for probing (success greatest <2 y) Sooner if >3 conjunctivitis

My daughter has sore bits… • • Worms? Thrush? Contact dermatitis - Bubble baths? Tights? Think child protection

My baby cries a lot… • Physical exam to exclude organic cause • Growth chart • Screen for maternal depression • Colic? = Paroxysmal uncontrollable crying in an otherwise healthy baby <3 m age with >3 h crying / day in >3 d / wk for >3 w

My baby vomits a lot… • Think about organic causes e. g. pyloric stenosis, volvulus • Behavioural measures – feed propped up, feed volumes, winding • Trial gaviscon / ranitidine • Refer if failing to thrive despite simple measures • Reassure and review

I think my baby has a food allergy… • Top food allergens – milk (CMP 2 -7% children), eggs, nuts, wheat • Consider if multi-system sx or dose dependent sx or failure to respond to rx for eczema / GORD / constipation • Ig. E within 20 m – urticaria / angiooedema • Non Ig. E – eczema / GORD / diarrhoea • Rx – elimination (4 -6 w), dietician • Refer if – Ig. E mediated, severe, failure to thrive, atopic, multiple food allergies, diagnostic uncertainty, nonresolution • Most outgrow – 3 y for non Ig. E and 5 y for Ig. E • 1° lactose intolerance rare (except after gastroenteritis) NICE guidelines [CG 116] Published date: February 2011

My child ‘just isn’t right’ doc… E. g. headache, tummy aches • • Try to pin them down Acute or chronic Ask about red flags eg sweats, failure to thrive Examine – glands, organomegaly Height / Weight Document Review

SPOT DIAGNOSIS My picture quiz…
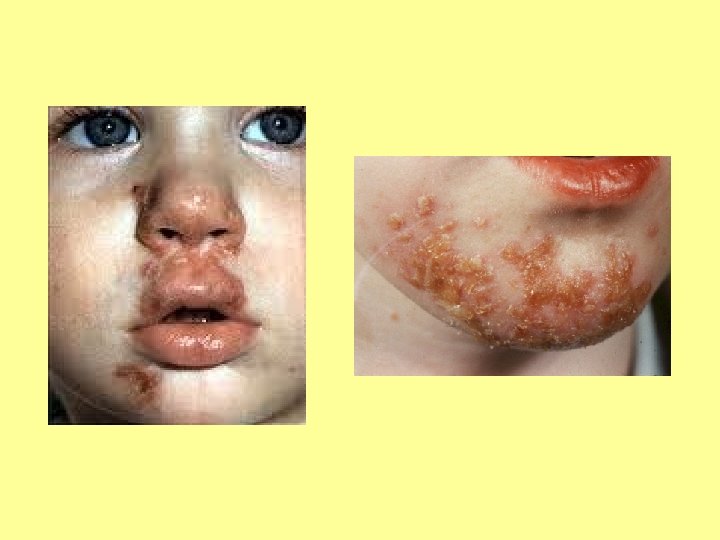
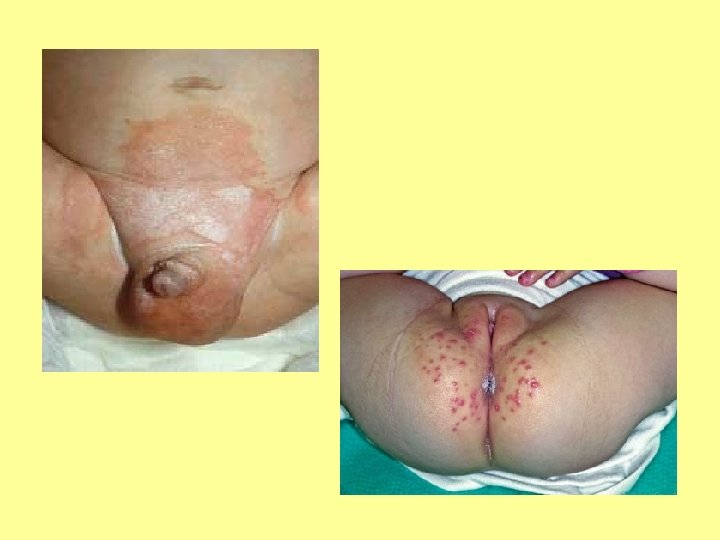
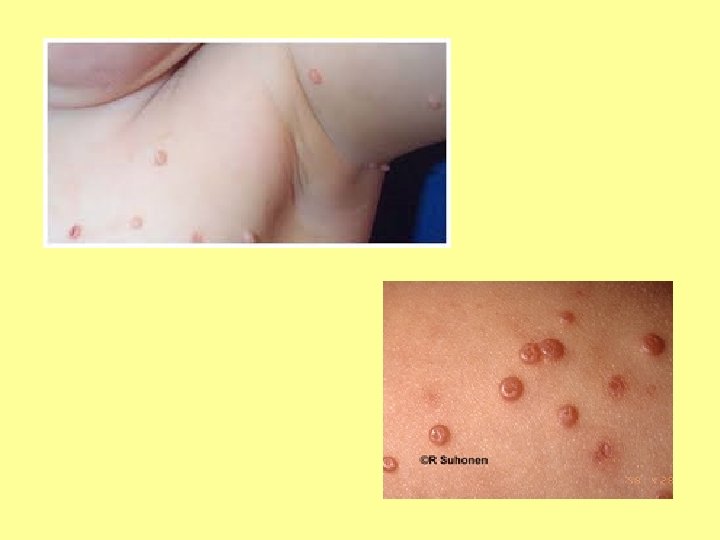
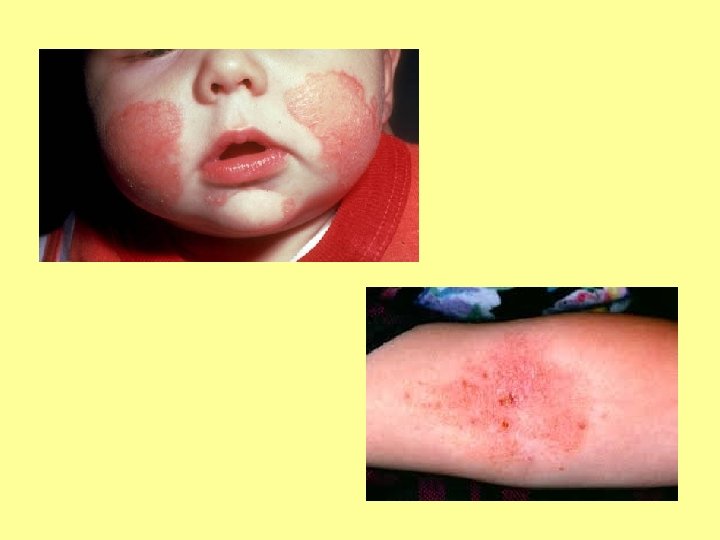
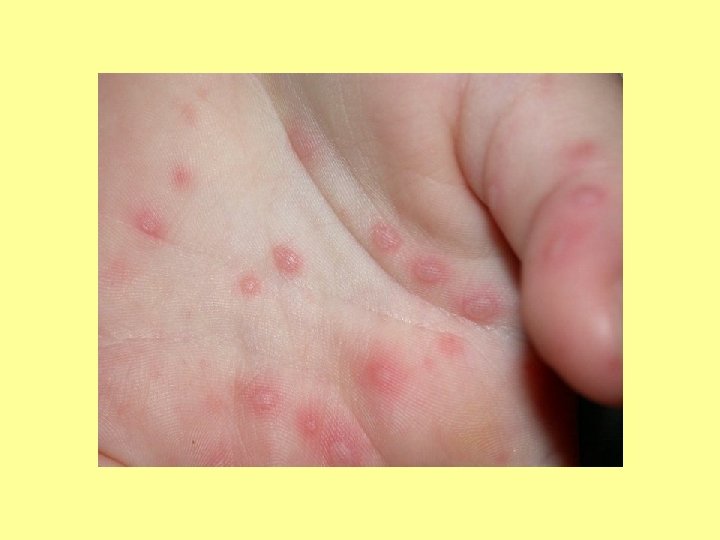
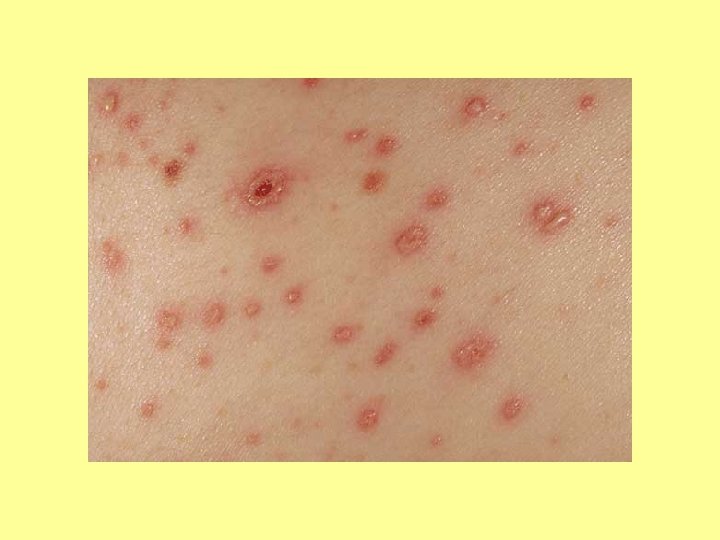
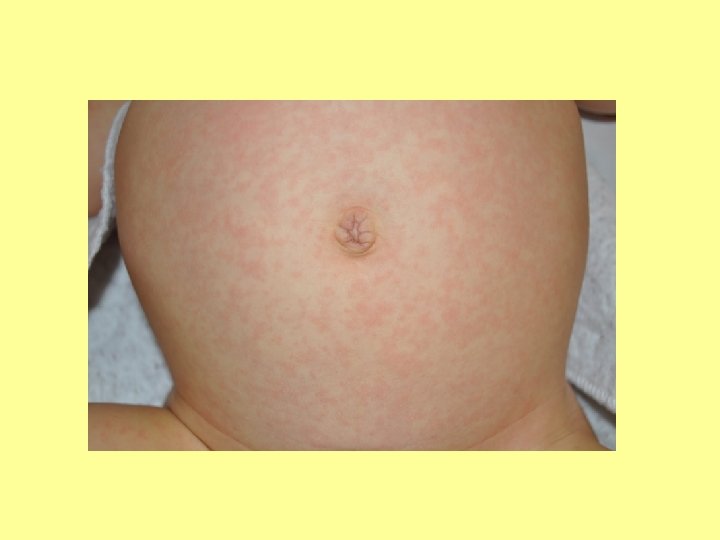
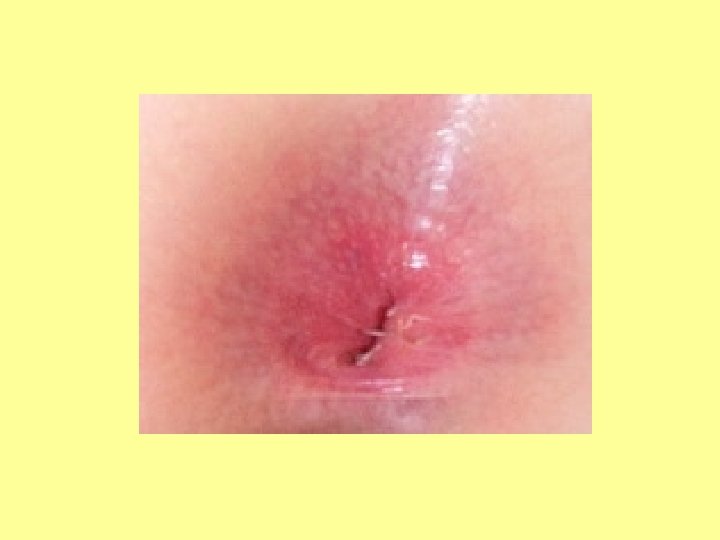
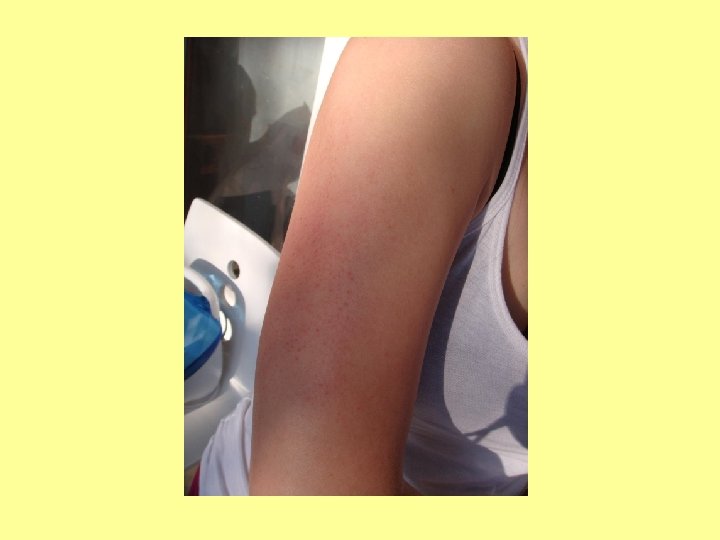

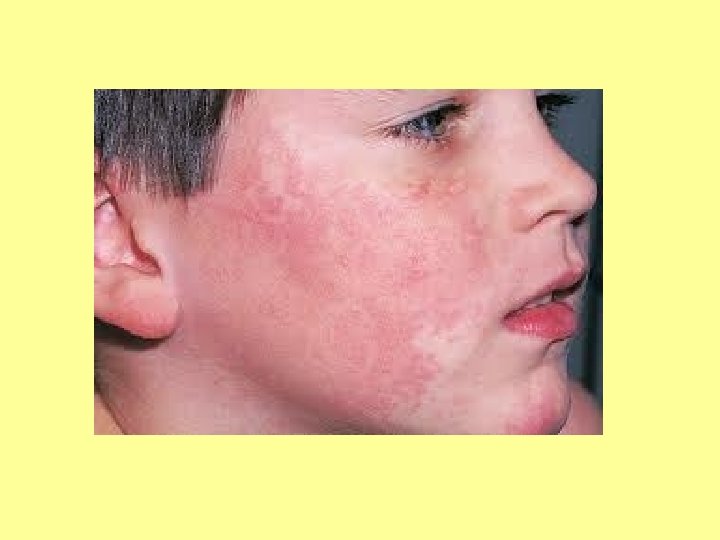
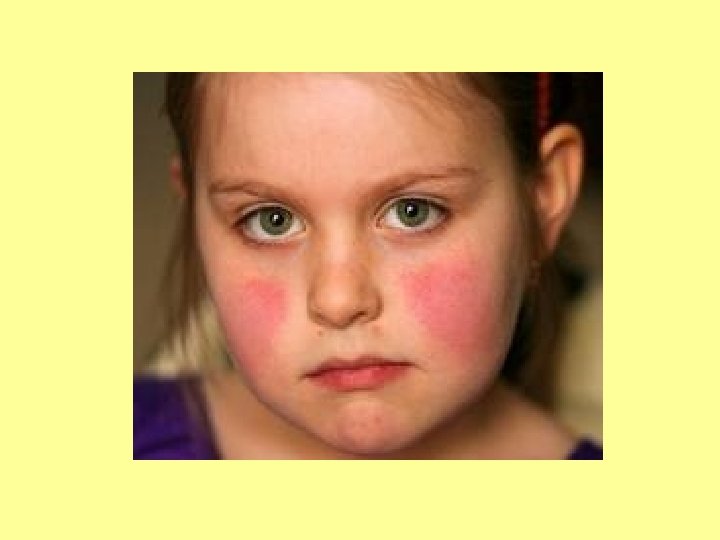
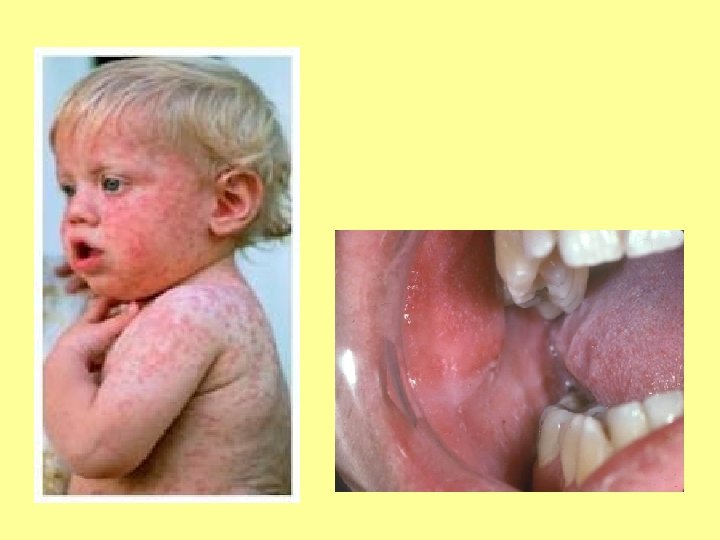
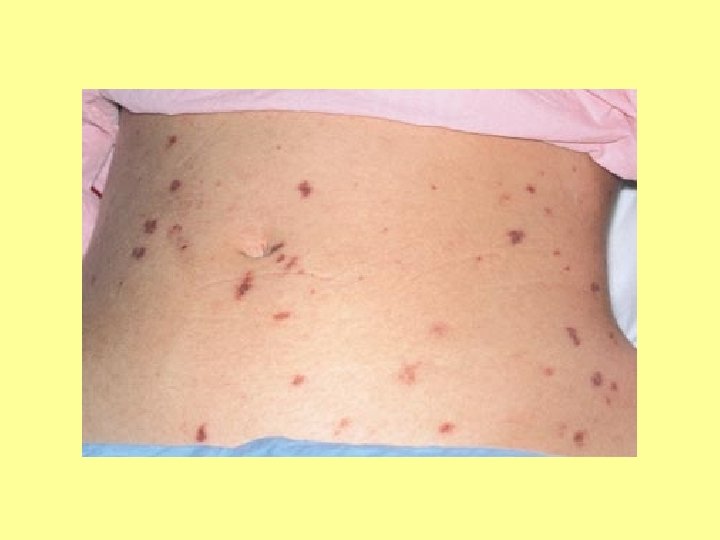

Anyone share any stories… What’s the oddest thing you’ve ever been asked?

Survival tips… • How do you deal with all the odd questions you are asked – paeds, colleagues, personal experience, friends, super nanny! • Be aware of local funding priorities e. g. tonsillectomy

Resources • NICE: febrile child, UTI in children, food allergy in children • Local hospital or CCG guidelines • Local support: – Colleagues – GPw. SI? – Paeds line Mon-Fri 1 -2 pm 07919 -175643

References • Google images • Dr Martin Kittel (Forest End Medical Centre – Bracknell)
- Slides: 32