Paediatric A llergy in West Ess ex Sue

























































- Slides: 76

Paediatric A llergy in West Ess ex Sue Clarke, Dr Liz Owen and Dr Neh a Khanna

Learning Outcomes 0 Appreciate the differences between Ig. E mediated and non Ig. E mediated reactions 0 Understand the importance of taking an allergy focussed clinical history to form a diagnosis 0 Appreciating when infants need referral and when they can be managed in Primary care 0 Update on West Essex Services and from April 2017 0 Secondary care in West Essex: testing, treating and other allergies

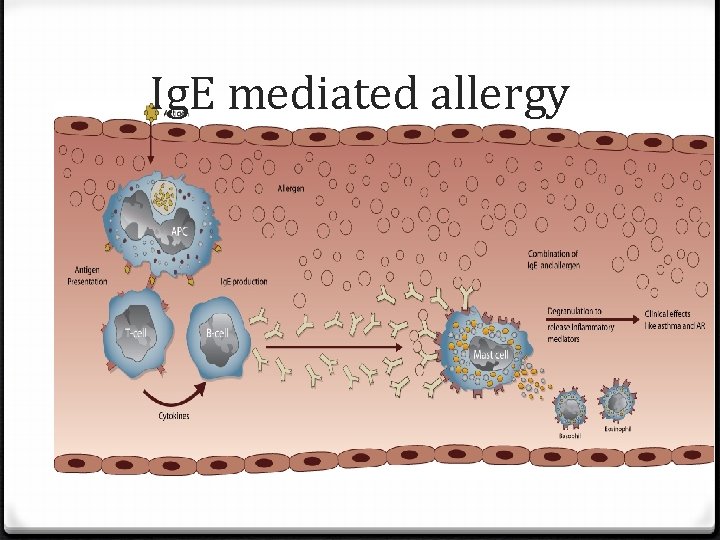
Ig. E mediated allergy

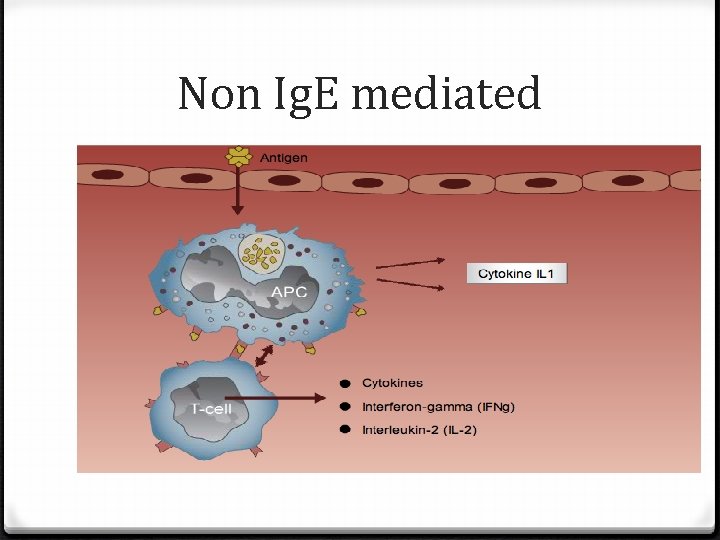
Non Ig. E mediated

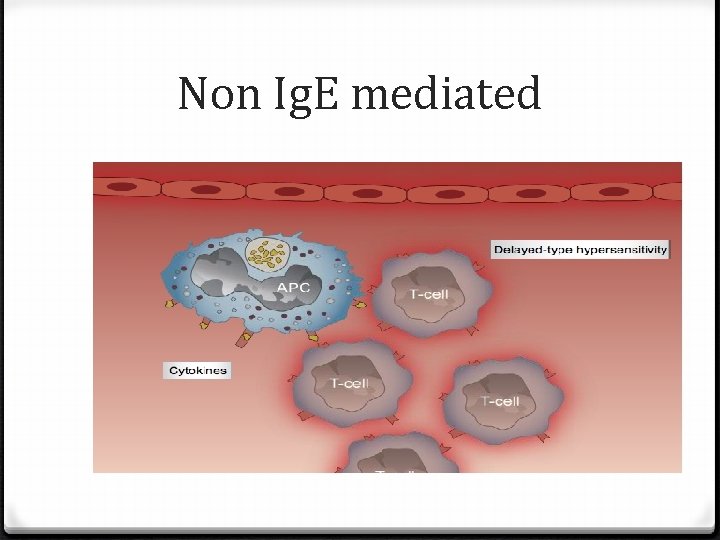
Non Ig. E mediated

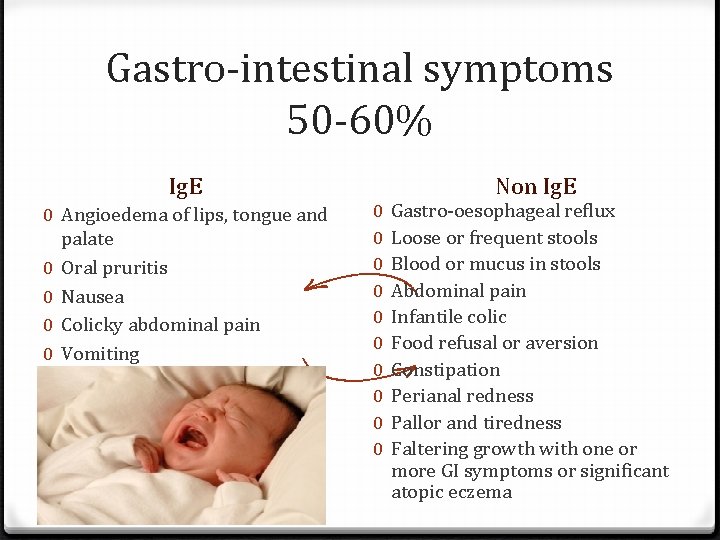
Gastro-intestinal symptoms 50 -60% Non Ig. E 0 Angioedema of lips, tongue and palate 0 Oral pruritis 0 Nausea 0 Colicky abdominal pain 0 Vomiting 0 Diarrhoea 0 0 0 0 0 Gastro-oesophageal reflux Loose or frequent stools Blood or mucus in stools Abdominal pain Infantile colic Food refusal or aversion Constipation Perianal redness Pallor and tiredness Faltering growth with one or more GI symptoms or significant atopic eczema

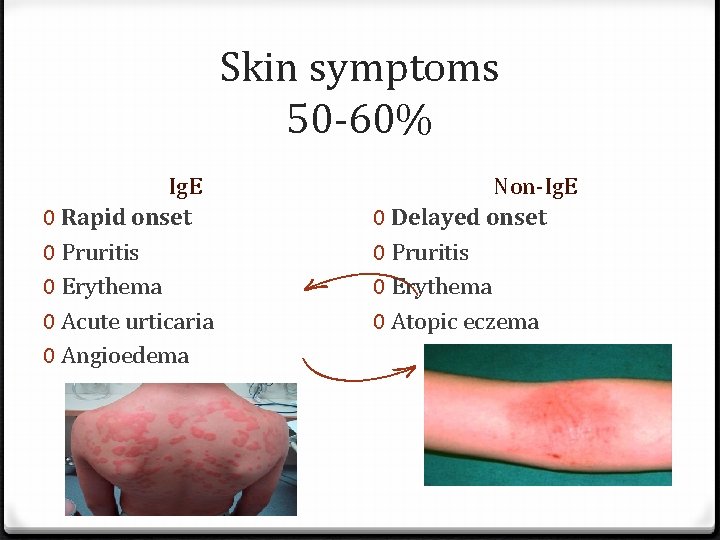
Skin symptoms 50 -60% Ig. E 0 Rapid onset 0 Pruritis 0 Erythema 0 Acute urticaria 0 Angioedema Non-Ig. E 0 Delayed onset 0 Pruritis 0 Erythema 0 Atopic eczema

Respiratory symptoms 20 -30% Ig. E 0 Nasal itching, sneezing, rhinorrhoea or congestion (with or without conjunctivitis) 0 Cough, chest tightness, wheeze and shortness of breath 0 Anaphylaxis and systemic allergic reactions Non Ig. E 0 Cough, chest tightness, wheeze and shortness of breathe 0 Congestion, catarral.

Assessment and allergy-focused clinical history 0 Consider the possibility of food allergy when symptoms of atopic eczema, gastro-oesophageal reflux disease or chronic gastrointestinal symptoms do not respond adequately to treatment 0 If food allergy is suspected, a healthcare professional should take an allergy-focused clinical history, and physically examine the child based on the findings. (NICE CG 116, 2011)

Allergy focussed clinical 0 Past medical history? 0 Family history? 0 Timing of the symptoms – immediate or delayed? 0 What symptoms experienced? 0 What quantity consumed? 0 Physical examination

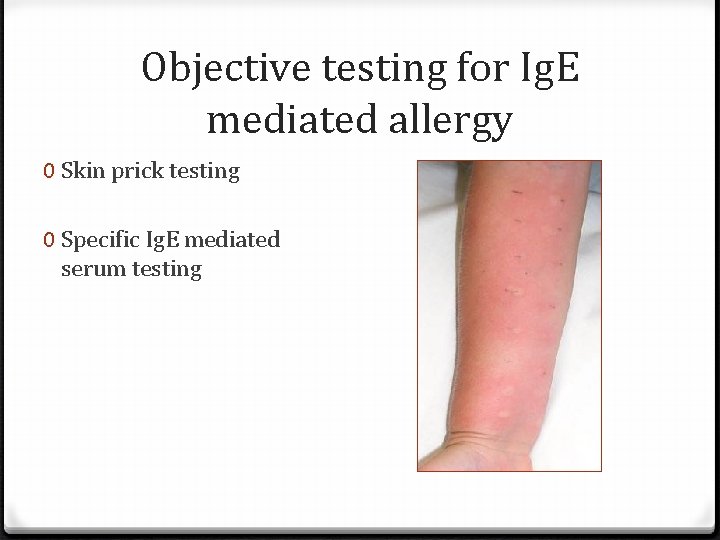
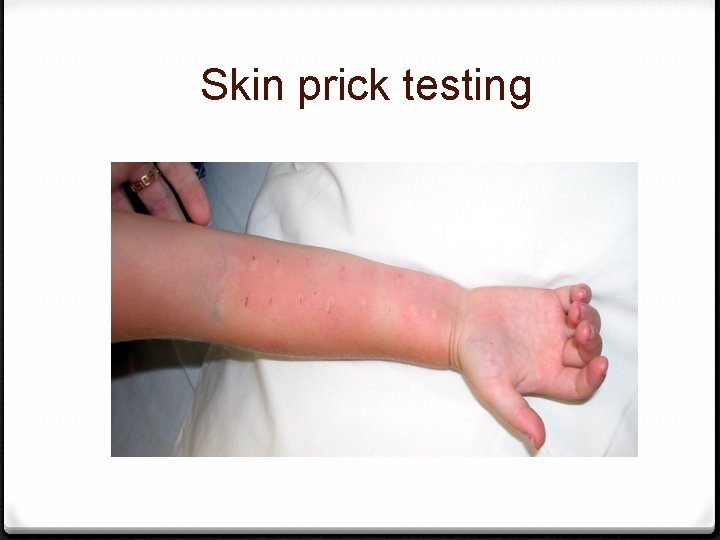
Objective testing for Ig. E mediated allergy 0 Skin prick testing 0 Specific Ig. E mediated serum testing

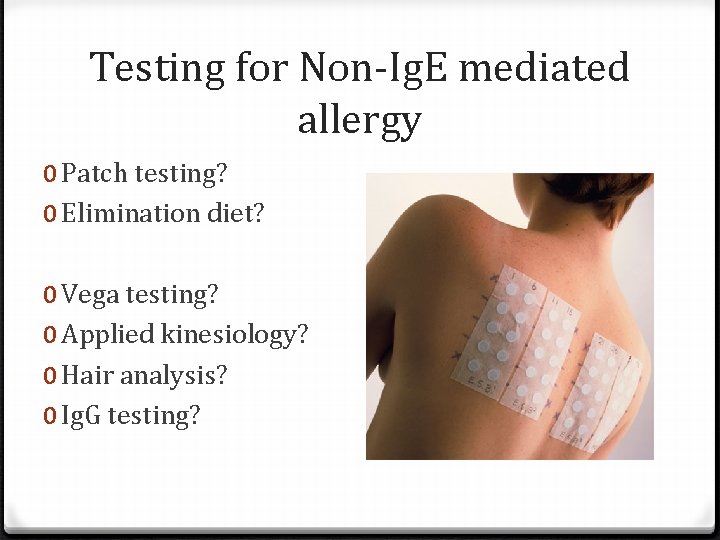
Testing for Non-Ig. E mediated allergy 0 Patch testing? 0 Elimination diet? 0 Vega testing? 0 Applied kinesiology? 0 Hair analysis? 0 Ig. G testing?

Management - MAP guidelines Milk Allergy in Primary care Guidelines help to guide management

Management of Ig. E mediated allergy 0 Allergy clinic referral 0 Allergen avoidance 0 Risk assessment for future reactions 0 Emergency treatment for accidental exposure-AAI 0 Training package 0 On going education and support

Management of Non Ig. E mediated allergy 0 Trial elimination diet for 26 weeks, then challenge 0 Extensive education about avoidance 0 Avoidance advice for breastfeeding mothers 0 Hypoallergenic formulas 0 Referral to dietitian

Specialist formulas 0 Breastfeeding is the preferred way to feed an allergic baby 0 Partially hydrolysed 0 Extensively hydrolysed 0 Amino acid formulas 0 Soya 0 Lactose free

What baby milk?

Case studie s

Emily 1 0 5 month old with persistent colic, gastro-eosophageal reflux and constipation 0 Taking Gaviscon and Lactulose daily. 0 Normal weight gain (on 75 th percentile) 0 Has been on cow’s milk formula from birth

Emily 2 0 Mum suspects cows milk allergy, she’s keen to try goats milk to see if this would help? 0 Father had a milk allergy as a baby, now hayfever 0 Examination showed mild eczema and dry skin 0 No immediate type symptoms

Emily 3 0 ? Non Ig. E mediated CMPA 0 How would you proceed? 0 Goats milk? 0 Soya milk? 0 EHF Formula 0 AA formula 0 Lactulose/Gaviscon?

Emily 4 0 Commenced on e. HF 0 Mum started weaning, advised dairy free. (Dietetic referral) 0 Within 4 weeks symptoms much better. Challenge confirmed diagnosis. 0 Continued on an extensively hydrolysed formula until 12 months when tolerated cow’s milk without symptoms.

Henry 1 0 Henry is 4 months old. 0 He‘s exclusively breastfed, but dropping through the centiles from 50 th to 9 th. 0 He has excessive colic, abdominal pain, severe congestion and reflux. 0 He cries for long periods and Mum has noticed mucus in his stools

Henry 2 Mum had a milk allergy when she was a child and Dad has eczema. Mum keen to try a dairy free diet. How would you advise her?

Henry 3 0 Advice on strict exclusion for up to 6 weeks. 0 Maternal supplements of calcium and vitamin D. 0 Rapid improvement in Henry’s symptoms. Mum maintained dairy free diet until 12 months old when Henry tolerated milk in his diet

Matthew 1 0 13 month old baby with moderate to severe eczema since 2 months of age. 0 Recently developed wheezy episode with a cold virus. 0 Coughing at night 0 Acute urticaria, lip swelling and projectile vomiting after cow’s milk. Tolerating formula.

Matthew 2 0 Matthew is very miserable with eczema and requiring frequent ABs for recurrent infections 0 FH of allergy- Dad hay fever, cousin has peanut allergy 0 Becoming a very fussy eater.

Matthew 3 0 SIg. E testing shows ++ to milk. 0 How would you manage Matthew now? 0 In Primary care? 0 Treatment options?

Matthew 4 0 Specialist allergy clinic 0 Allergen avoidance advice 0 Management plan 0 Adrenaline injector? 0 Allergy education 0 Dietetic advice 0 Support groups

Grace 1 0 Grace is 11 weeks old. She has severe colic, reflux and constipation from 2 weeks old. 0 Commenced on Similac Alimentum at 4 weeks and improved.

Grace 2 0 Some of Grace’s gastrointestinal symptoms improved but she developed eczema and a very sore bottom. 0 Eczema failed to respond to emollients and hydrocortisone. 0 Sore bottom was raw and not responding to any creams

Grace 3 0 Grace was referred to a Paediatric allergist who prescribed an amino acid based formula. 0 Skin and sore bottom improved within a week. 0 Referred to a dietitian 0 Remained on AA formula until 12 months. 0 Audit at 12 months showed Grace eating cheese and yoghurts. Milk challenge tolerated and started on Cow’s milk.

Resources 0 MAP Guidelines 0 http: //www. ctajournal. com/content/3/1/23 0 NICE CG 116 0 https: //www. nice. org. uk/guidance/cg 116 0 http: //cks. nice. org. uk/cows-milk-protein-allergy-inchildren 0 RCPCH Care pathways for children with allergic conditions. 0 http: //www. rcpch. ac. uk/allergy/foodallergy

GP perspect ive Dr Liz Owen GP

Reflux and CMPA 0 Feeding difficulties make a high proportion of GP time/appointments 0 Frequently accompanied by repeat visits to A+E as well as GP and HV 0 Parents and families in distress with constantly crying baby 0 Traditionally symptoms of pain and vomiting addressed as GOR to varying degrees of intervention 0 CMPA as a cause for the symptoms fairly new concept 0 CMPA an expensive condition to treat

Flow chart introduced 0 To try to distinguish the children with GOR and those with GOR caused by milk allergy 0 40% with GOR will have CMPA as a cause 0 Get them on the right treatment and resolve symptoms asap 0 MAP guidance consulted and attempted to condense 0 Adaptation of previous document from medicine’s management 0 Explaining the roles of the HV and the GP

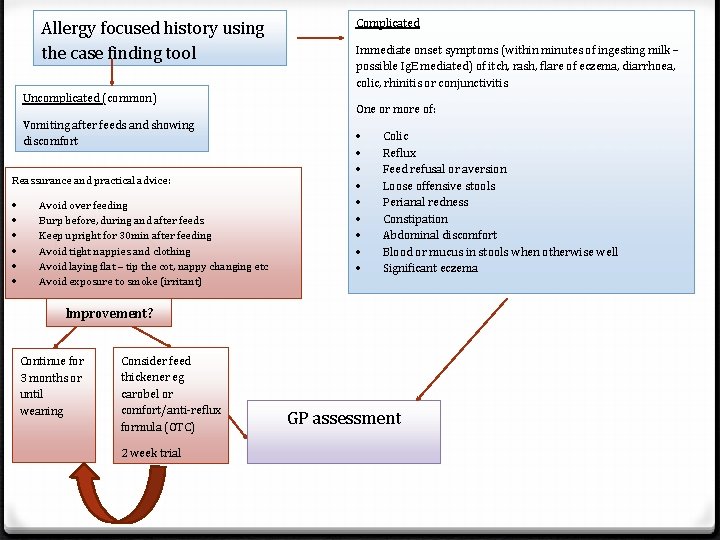
Allergy focused history using the case finding tool Uncomplicated (common) Vomiting after feeds and showing discomfort Reassurance and practical advice: Avoid over feeding Burp before, during and after feeds Keep upright for 30 min after feeding Avoid tight nappies and clothing Avoid laying flat – tip the cot, nappy changing etc Avoid exposure to smoke (irritant) Complicated Immediate onset symptoms (within minutes of ingesting milk – possible Ig. E mediated) of itch, rash, flare of eczema, diarrhoea, colic, rhinitis or conjunctivitis One or more of: Colic Reflux Feed refusal or aversion Loose offensive stools Perianal redness Constipation Abdominal discomfort Blood or mucus in stools when otherwise well Significant eczema Improvement? Continue for 3 months or until weaning Consider feed thickener eg carobel or comfort/anti-reflux formula (OTC) 2 week trial GP assessment

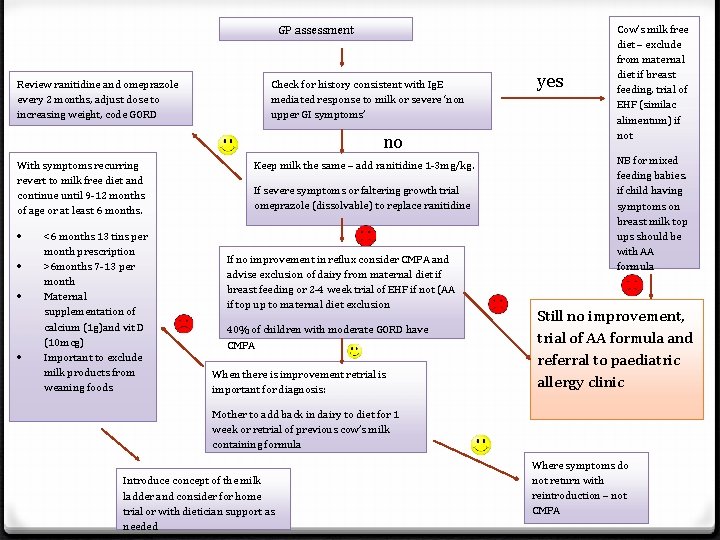
GP assessment Review ranitidine and omeprazole every 2 months, adjust dose to increasing weight, code GORD Check for history consistent with Ig. E mediated response to milk or severe ‘non upper GI symptoms’ yes no With symptoms recurring revert to milk free diet and continue until 9 -12 months of age or at least 6 months. <6 months 13 tins per month prescription >6 months 7 -13 per month Maternal supplementation of calcium (1 g)and vit D (10 mcg) Important to exclude milk products from weaning foods NB for mixed feeding babies. if child having symptoms on breast milk top ups should be with AA formula Keep milk the same – add ranitidine 1 -3 mg/kg. If severe symptoms or faltering growth trial omeprazole (dissolvable) to replace ranitidine If no improvement in reflux consider CMPA and advise exclusion of dairy from maternal diet if breast feeding or 2 -4 week trial of EHF if not (AA if top up to maternal diet exclusion 40% of children with moderate GORD have CMPA When there is improvement retrial is important for diagnosis: Mother to add back in dairy to diet for 1 week or retrial of previous cow’s milk containing formula Introduce concept of the milk ladder and consider for home trial or with dietician support as needed Cow’s milk free diet – exclude from maternal diet if breast feeding, trial of EHF (similac alimentum) if not Still no improvement, trial of AA formula and referral to paediatric allergy clinic Where symptoms do not return with reintroduction – not CMPA

Case finding tool for HV 0 Condensed form of focused allergy history 0 To be conducted with a health professional – ideally the health visitor for the child 0 Main point to decrease history taking time 0 From these descriptions should be able to distinguish Ig. E symptoms from non-Ig. E and likelihood of CMPA

What to do when presented with the info/case finding tool 0 Long winded guidance for GPs available 0 Salient points: 0 ‘Stay down’ milks can be brought and very similar cost to normal so should ideally not be prescribed 0 If prescribing EHF milk please use most cost effective ie similac alimentum 0 Lactose free milks should not be recommended or prescribed 0 Soya milk not suitable for <6 months old 0 ‘Other’ mammal milks also not recommended 0 Other EHFs same but may have different tastes – possible to trial another EHF if taste not tolerated but symptoms improve on similac alimentum 0 Review appointments important – child will improve in 2 weeks if going to respond

Prepare for milk ladder 0 Prepare for weaning at the time of diagnosis 0 Milk free weaning and check labels 0 If gets symptoms on weaning when excluding milk also exclude soya. 0 Prepare for stopping the milk at start of treatment. 0 Life-long treatment not needed for most 0 Prescribed milks can usually be changed to alternatives at age 1. 0 Locally training up HV to be CMPA champions and to run special weaning groups

Milk ladder

Milks to substitute after 1 yr 0 Must be calcium fortified milks ie not organic 0 Soya, Oat, hemp, coconut or almond milk can be trialled 0 Rice milk should not be a main drink until 4. 5 yrs 0 All these milks can be used in cooking from 6 months

Myth busting 0 All children on prescribed milks need to be referred to allergy clinic or dietician for approval 0 Refer to allergy clinic if Ig. E symptoms or FTT or symptoms do not resolve with treatment. 0 Refer to allergy clinic if prescribing AA formula due to non response to EHF 0 Refer to dietician if parents struggling with milk free diet, weaning, how to exclude, use of milk ladder.

Myth busting 0 Testing needed for non Ig. E - CMPA 0 Clinical dx with the re-trial of CMP after exclusion to confirm dx 0 Pre-weaning allergy testing needed for other foods as allergic to milk 0 No benefit unless child has shown other reactions at weaning 0 Possible exception with severe eczema

Allergy service from April 2017 0 Central referral form 0 Triaged by allergy clinic team 0 Assigned to community allergy clinic or secondary care team 0 At community clinic to be seen by specialist nurse, skin prick testing as needed and see dietician same day 0 Secondary care clinic – to see allergy specialist, skin prick testing as needed and access to dietician 0 Refer back to primary care with diagnosis and plan +/= direct dietician follow up.

Websites and resources 0 Flow chart for ref or MAP guideline 0 Milk ladder 0 www. livingwithreflux. org 0 www. allergy. uk 0 www. godairyfree. org – recipes for breast feeding mums

Basics of Paediatric Allergy 1 st November 2016 DR Neha Khanna Consultant Paediatrician Princess Alexandra Hospital NHS Trust

Intend to cover 0 Basics of food allergy 0 Understanding tests and diagnosis 0 When to prescribe Adrenaline auto injector 0 When to refer to Allergy clinic

Atopy 0 A genetic predisposition to producing Ig. E antibodies to common environmental antigens 0 Associated with a constellation of common conditions: 0 Asthma, eczema, rhinitis, conjunctivitis, urticaria, anaphylaxis.

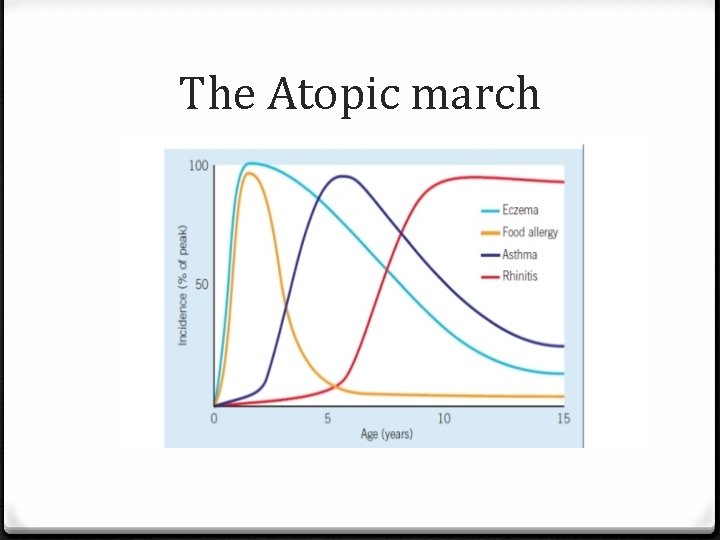
The Atopic march

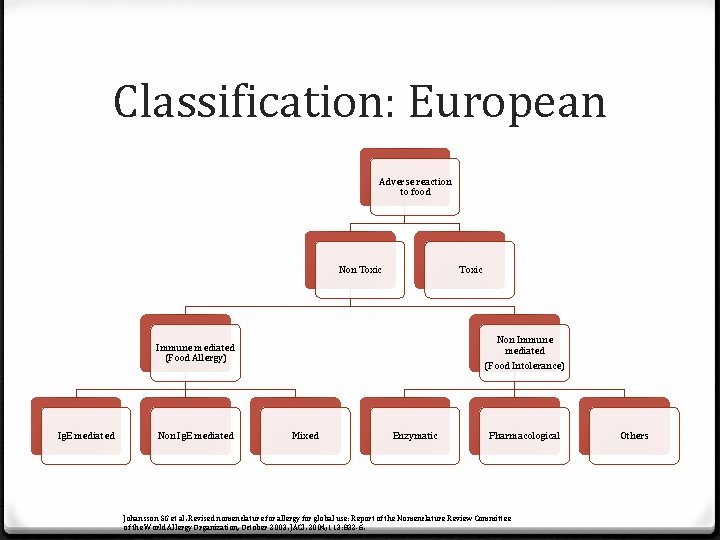
Classification: European Adverse reaction to food Non Toxic Non Immune mediated (Food Allergy) Ig. E mediated Non Ig. E mediated (Food Intolerance) Mixed Enzymatic Pharmacological Johansson SG et al. Revised nomenclature for allergy for global use: Report of the Nomenclature Review Committee of the World Allergy Organization, October 2003. JACI. 2004; 113: 832 -6. Others

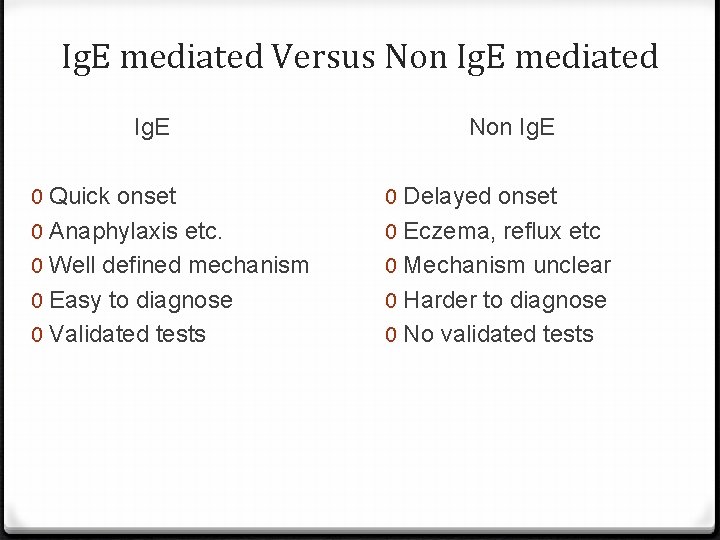
Ig. E mediated Versus Non Ig. E mediated Ig. E Non Ig. E 0 Quick onset 0 Anaphylaxis etc. 0 Well defined mechanism 0 Easy to diagnose 0 Validated tests 0 Delayed onset 0 Eczema, reflux etc 0 Mechanism unclear 0 Harder to diagnose 0 No validated tests

Diagnosis: Ig. E mediated 0 History 0 Allergy tests 0 Food challenges

Skin prick testing

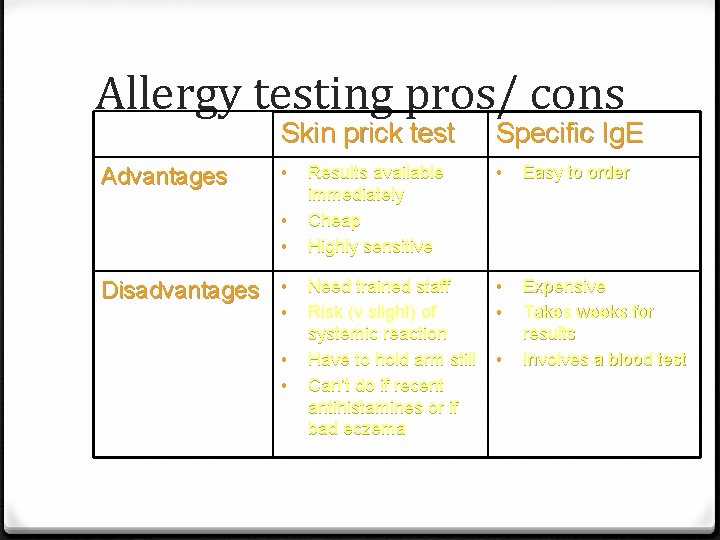
Allergy testing pros/ cons Advantages Skin prick test Specific Ig. E • Results available immediately Cheap Highly sensitive • Easy to order Need trained staff Risk (v slight) of systemic reaction Have to hold arm still Can’t do if recent antihistamines or if bad eczema • • Expensive Takes weeks for results Involves a blood test • • Disadvantages • • •

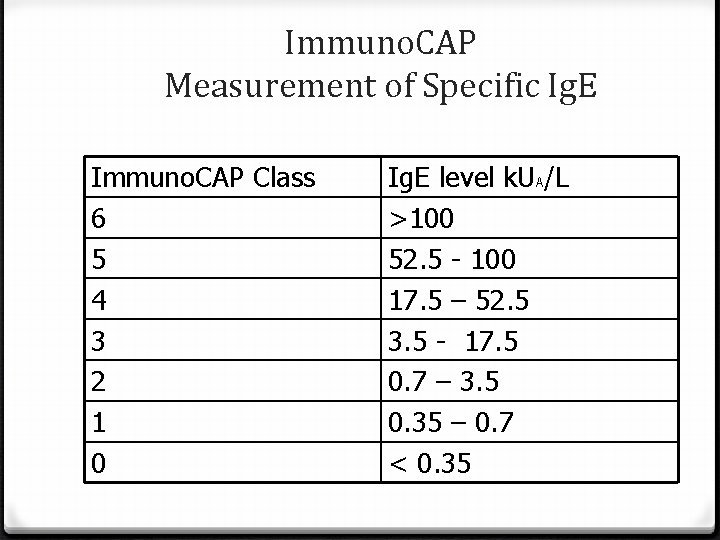
Immuno. CAP Measurement of Specific Ig. E Immuno. CAP Class 6 5 4 3 2 1 0 Ig. E level k. UA/L >100 52. 5 - 100 17. 5 – 52. 5 3. 5 - 17. 5 0. 7 – 3. 5 0. 35 – 0. 7 < 0. 35

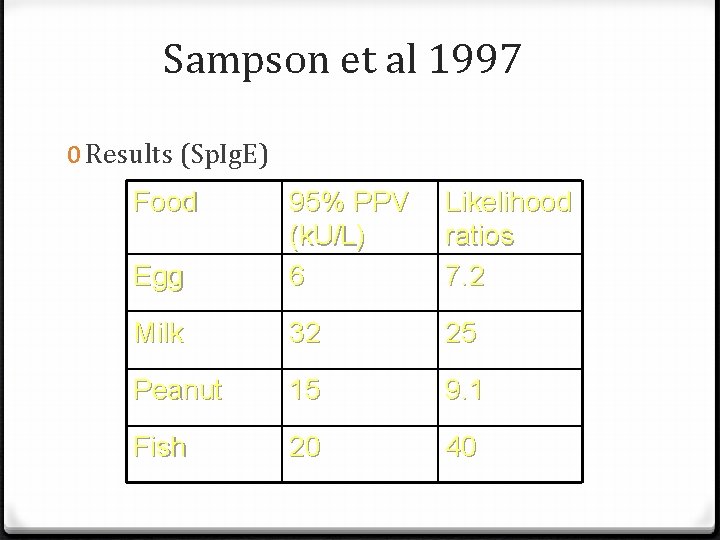
Sampson et al 1997 0 Results (Sp. Ig. E) Food Egg 95% PPV (k. U/L) 6 Likelihood ratios 7. 2 Milk 32 25 Peanut 15 9. 1 Fish 20 40

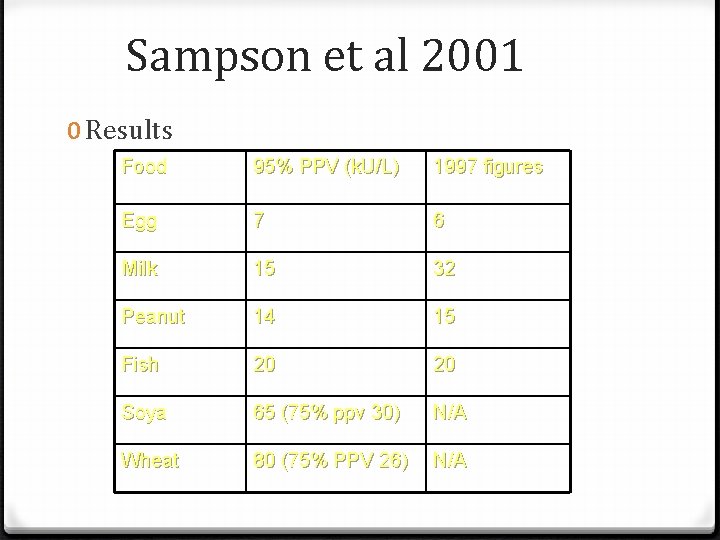
Sampson et al 2001 0 Results Food 95% PPV (k. U/L) 1997 figures Egg 7 6 Milk 15 32 Peanut 14 15 Fish 20 20 Soya 65 (75% ppv 30) N/A Wheat 80 (75% PPV 26) N/A

Diagnosis 0 Consider Ig. E as giving 3 possible results 0 low 0 specific Ig. E <0. 7 k. U/l 0 medium 0 specific Ig. E Grade 2 to 95% PPV published by Sampson 0 high 0 specific Ig. E > 95% PPV published by Sampson

Value of Allergy testing 0 Does a positive test imply allergy? 0 No, but makes it more likely 0 Can be sensitised but not allergic 0 Does a negative test exclude allergy? 0 No, but makes it less likely 0 Size predicts for likelihood of allergy 0 Size of wheal does NOT relate to severity of reaction 0 Negative tests are strongly predictive

Gold standard: Food challenge 0 0 DBPCFC Open Food challenge: objective, reproducible symptoms Child given graded doses of food Final dose is a portion of the food 0 0 Challenge stopped if there is a reaction If tolerates top dose not allergic If reacts allergic If unable to eat all doses inconclusive 0 NOT first line test!

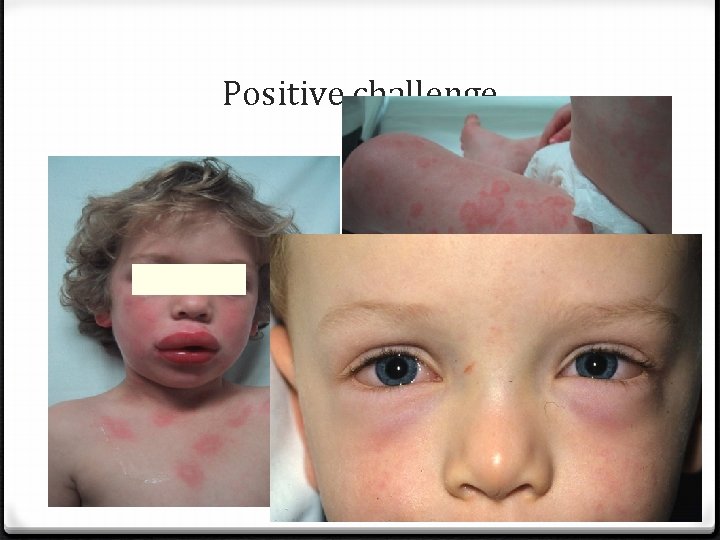
Positive challenge

Food Allergy

Co-morbidities 0 0 Children with one food allergy often have others Eczema more likely to be severe in food allergic children Food allergy predicts for later respiratory allergy Managing one allergic condition will impact on others 0 Active asthma is the major risk factor for severe allergic reactions 0 Nearly all recorded child death from food allergy also had poorly controlled asthma. 0 Some severe asthma attacks are actually anaphylaxis 0 0 Sampson HA et al. Fatal and near-fatal anaphylactic reactions to food in children and adolescents. N Engl J Med. 1992 Aug 6; 327(6): 380 -4. Roberts et al. Food allergy as a risk factor for life-threatening asthma in childhood: a case-controlled study. J Allergy Clin Immunol. 2003 Jul; 112(1): 168 -74.

Egg allergy 0 Peanut allergy (1: 5) 0 Increased risk of asthma, 50 - 80% of egg allergic asthmatic by age 7 Ø Egg Allergy in infancy predicts sensitisation to inhalant allergies , Nickel et al. JACI 1997 Ø Egg Allergy in infancy predicts childhood wheeze at age 4 yr. Tariq SM et al. Pediatr Allergy Immunol 2000 0 Dietary baked egg in children accelerates resolution of egg allergy. Leonard et all JACI 2012

Management: Ig. E mediated 0 BSACI action plans 0 Antihistamine for mild reactions 0 Adrenaline for anaphylaxis

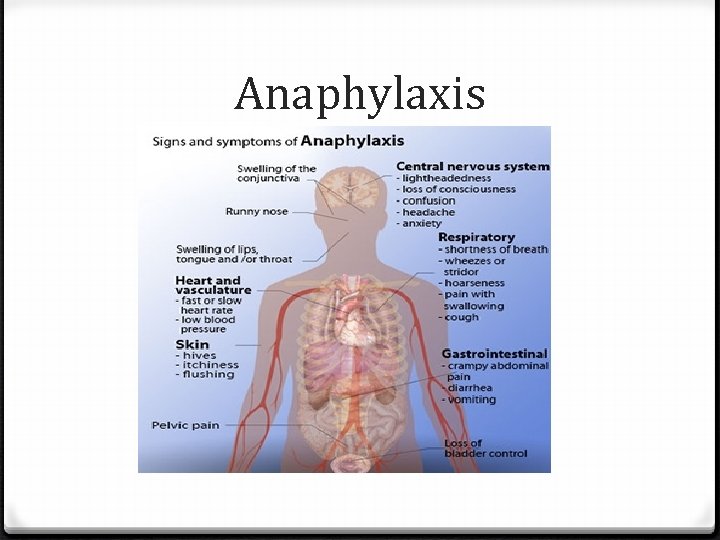
Anaphylaxis

Adrenaline Absolute: 0 Previous Cardiovascular or respiratory reactions 0 Food allergy and co- existent persistent asthma Relative 0 Reaction to small amounts of food (air borne, skin) 0 Remoteness from medical facilities 0 Teenagers

Egg allergy and Vaccines 0 MMR 0 Influenza 0 Yellow fever

MMR and Yellow Fever MMR 0 Amount of egg protein negligible 0 Children with egg allergy, give MMR as normal 0 Documented anaphylaxis to MMR: assess by allergist Yellow Fever 0 Refer to specialist centres

Influenza vaccine 0 Nasal flu vaccine (Fluenz tetra): safe in any setting in children with egg allergy including children with previous anaphylaxis to egg 0 SNIFFLE studies: 887 egg allergic children safely received nasal flu vaccine, only exclusion children with anaphylaxis to egg so severe requiring ventilation/PICU 0 Inactivated (injected) influenza vaccines that are egg free or have an ovalbumin content < 0. 12 μg/ml may be used safely in primary care.

Refer to Allergy Clinic 0 0 0 0 0 Food allergies: History of Ig. E mediated food allergy needing SPT Fish and nut allergy Persistent milk and egg allergy beyond 4 years of age Multiple food allergies History of Anaphylaxis Food allergy and concomitant uncontrolled asthma Reactions to unidentified food allergen along with asthma Reaction to a minute or trace amount of allergen Multiple non Ig. E mediated food allergies (restricted diet) 0 0 0 Urticaria: Angioedema only with no urticarial lesions Chronic urticaria (lasting more than 6 weeks) not responding to regular antihistamines 0 0 Eczema: Severe eczema not responding to treatment, needing exclusion of food allergies 0 0 Hay fever: Allergic rhinitis not responding to antihistamines/nasal steroids, or needs SPT 0 0 0 Others: Wasp and bee sting generalised reactions History of Immediate reactions to drugs (antibiotic reactions when no alternative class of drugs available, or requiring recurrent courses of antibiotics)

Please DO NOT REFER 0 Uncomplicated non Ig. E mediated cow’s milk allergy 0 Parents asking for blanket allergy tests with no clear history of allergic reaction 0 Isolated Urticaria with no trigger (unless chronic and no response to regular anti histamines) 0 Children with mild or moderate eczema and not having any direct flare ups related to specific triggers. 0 All asthmatics and wheezers to look for aero allergen trigger 0 Children with egg allergy for vaccinations unless previous egg anaphylaxis required PICU admission 0 Single class antibiotic allergy in otherwise well child 0 We are happy to offer advice on Specific Ig. E blood tests requested by individual clinicians.

Discussion
