Pacemaker vs CRTP vs CRTD Evidencebased medicine Randomized


Pacemaker vs CRT-P vs CRT-D


Evidence-based medicine Randomized controlled trials Consensus guidelines Clinical practice

Pacemaker vs CRT-P

Patients with conventional pacemaker indications and heart failure q q q Previous studies have clearly shown that RV apical pacing might have deleterious effects on cardiac structure and function. Moreover, different clinical trials have shown that there was a positive correlation between the rate of RV pacing and the occurrence of adverse events. For patients with conventional pacemaker who develop HF, upgrading from VVI or DDD to CRT devices represents an important part of the patient population implanted with a CRT device, being 23– 28% of the CRT implantations in different registries. Leclercq C, Cazeau S, Lellouche D, Fossati F, Anselme F, Davy JM, Sadoul N, Klug D, Mollo L, Daubert JC. Upgrading from single chamber right ventricular to biventricular pacing in permanently paced patients with worsening heart failure: The RD-CHF Study. Pacing Clin Electrophysiol 2007; 30 Suppl 1: S 23– 30.
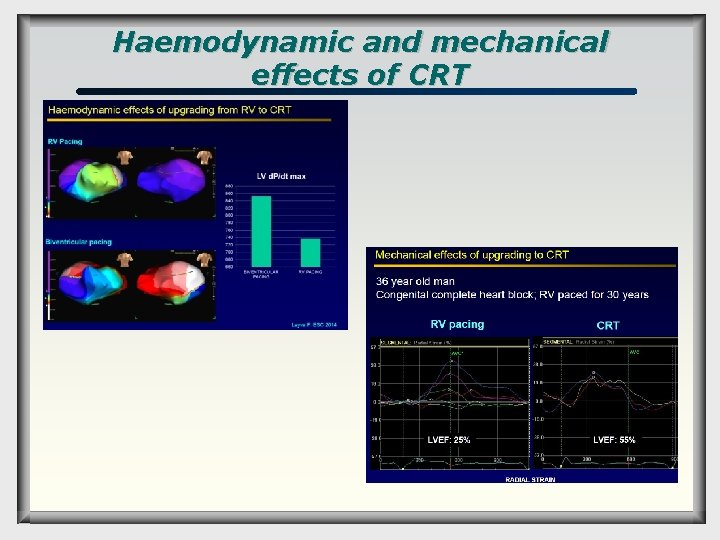
Haemodynamic and mechanical effects of CRT

What do the guidelines say ? ESC ACC/AHA

Patients with conventional pacemaker indications and heart failure q q q The additional benefit of biventricular pacing should be considered in patients requiring permanent or frequent RV pacing for bradycardia, who have symptomatic HF and low LVEF. The patients had conventional bradycardia indications (mostly permanent AV block), severe symptoms of HF (mostly NYHA class III or IV) and depressed EF mostly <35 -40%. During the CRT study phase, the pts consistently showed clinical subjective improvement, less hospitalization and improved cardiac function, compared with the RV study phase.
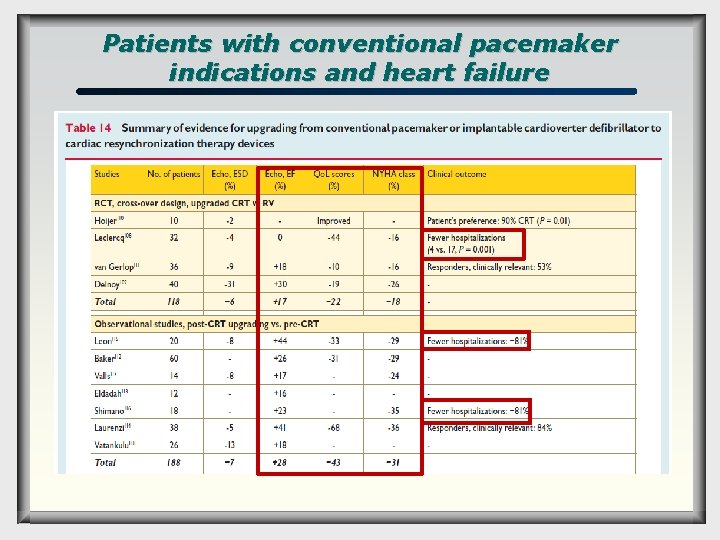
Patients with conventional pacemaker indications and heart failure
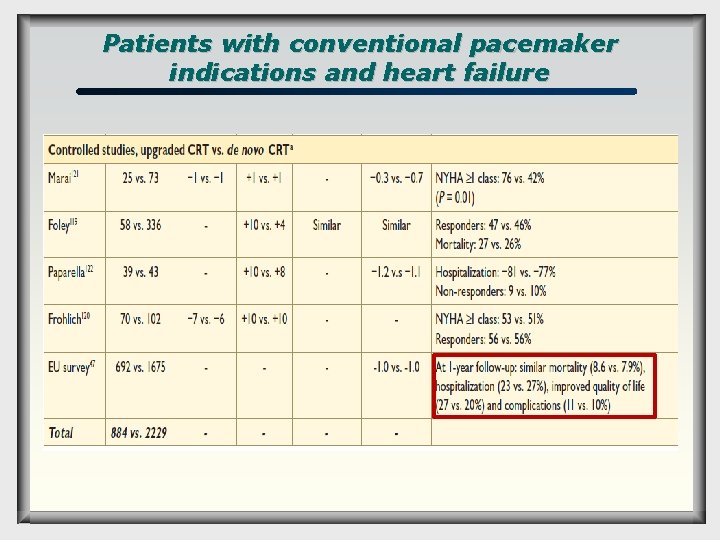
Patients with conventional pacemaker indications and heart failure
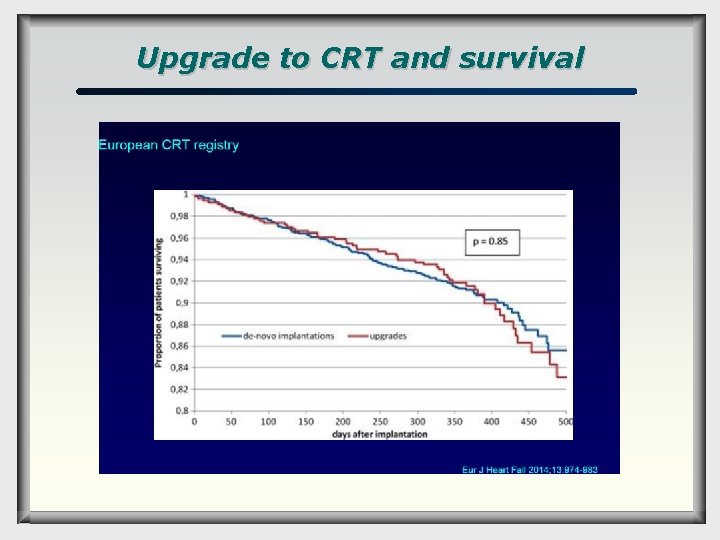
Upgrade to CRT and survival

Upgrade to CRT is associated with a high complication rate, which ranges 11 - 18. 7% in prospective trials. The decision to upgrade should therefore be made after careful assessment of the risk–benefit ratio.
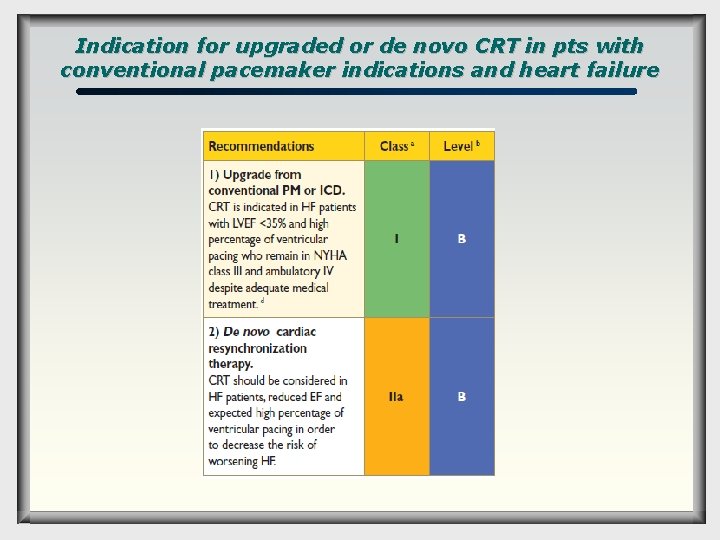

Indication for upgraded or de novo CRT in pts with conventional pacemaker indications and heart failure

CRT-P vs CRT-D

Benefit of adding ICD in patients with indications for CRT q q Even though theoretical reason for adding an ICD to CRT is clear —to reduce of the risk of arrhythmic death— the survival benefit of CRT-D over CRT-P is still a matter of debate, mainly because no RCT has been designed to compare these treatments. The evidence from RCTs is insufficient to show the superiority of combined CRT and ICD over CRT alone. Nevertheless the Bayesian analysis, based on an extrapolated analysis, suggests that it is probable that combined therapy is the best option (probability of 75% in analysis).
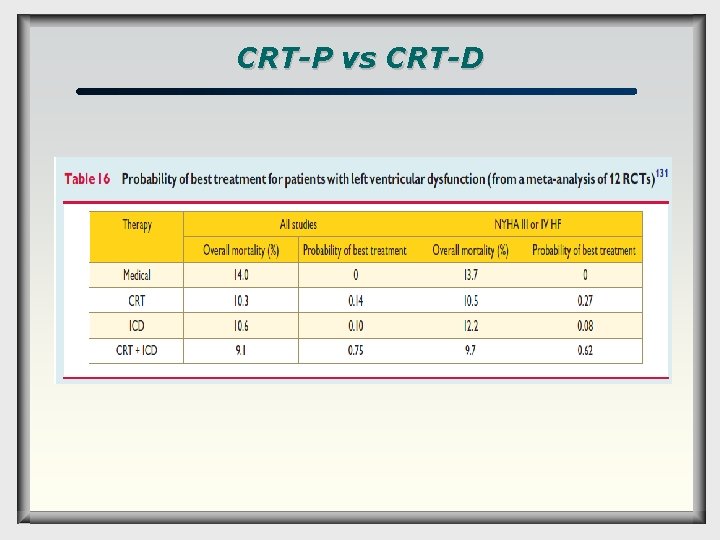
CRT-P vs CRT-D

CRT-P vs CRT-D Task Force is of the opinion that no strict recommendations can be made, and prefers to merely offer guidance regarding the selection of patients for CRT-D or CRT-P, based on overall clinical condition, device-related complications and cost. CRT-D is beneficial in all disease states, but the benefit appears relatively small in end-stage HF, in which the main reason for choice of device is related to improvement of quality of life and reduction of HFrelated hospitalizations and death.
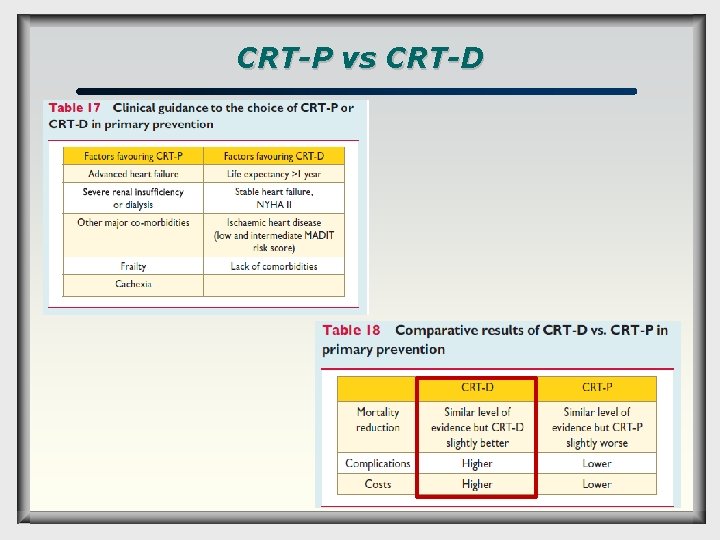
CRT-P vs CRT-D
CRT-D vs CRT-P
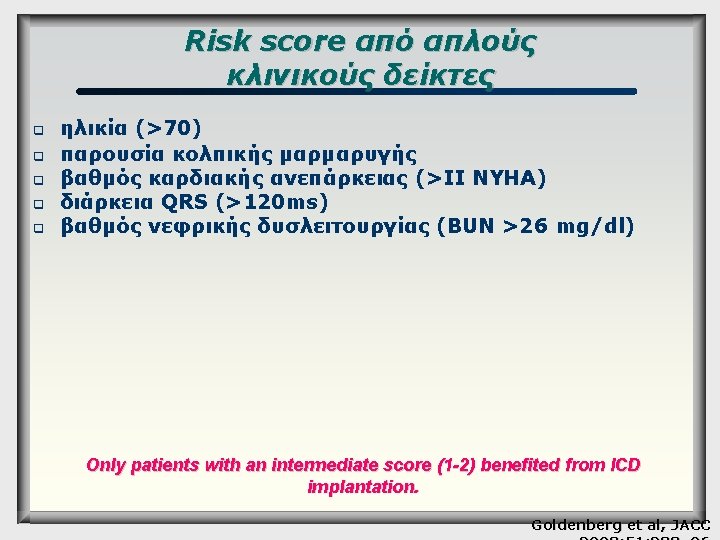
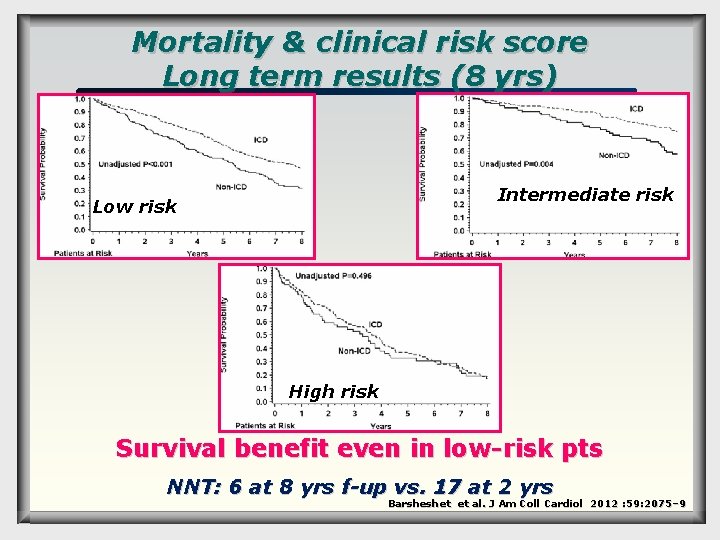
Mortality & clinical risk score Long term results (8 yrs) Intermediate risk Low risk High risk Survival benefit even in low-risk pts NNT: 6 at 8 yrs f-up vs. 17 at 2 yrs Barsheshet et al. J Am Coll Cardiol 2012 : 59: 2075– 9

CRT-P vs CRT-D q q q In the extension of CARE-HF study with a 37. 4 month follow-up time, there was a significant 5. 6% reduction in the absolute risk of dying suddenly. The results imply that, although the risk of dying from HF is immediately lowered by CRT, the reduction of risk of sudden cardiac death evolves at a much slower rate. It is very probable that reduction in risk of sudden cardiac death by CRT is related to the extent of reverse remodelling.
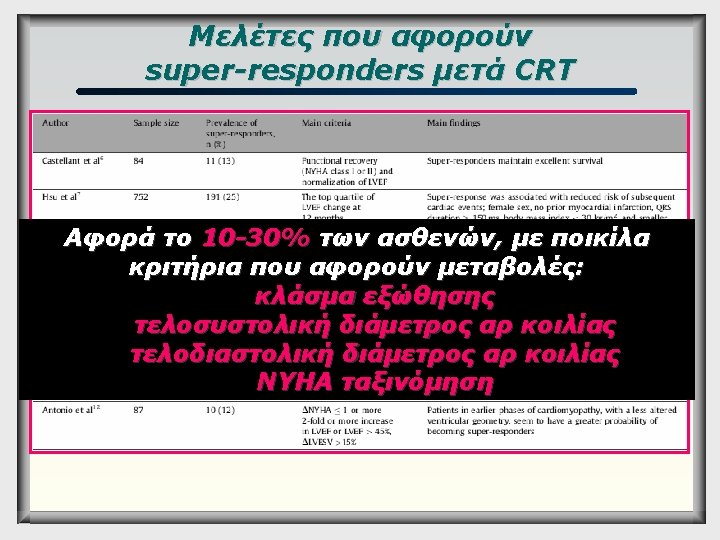


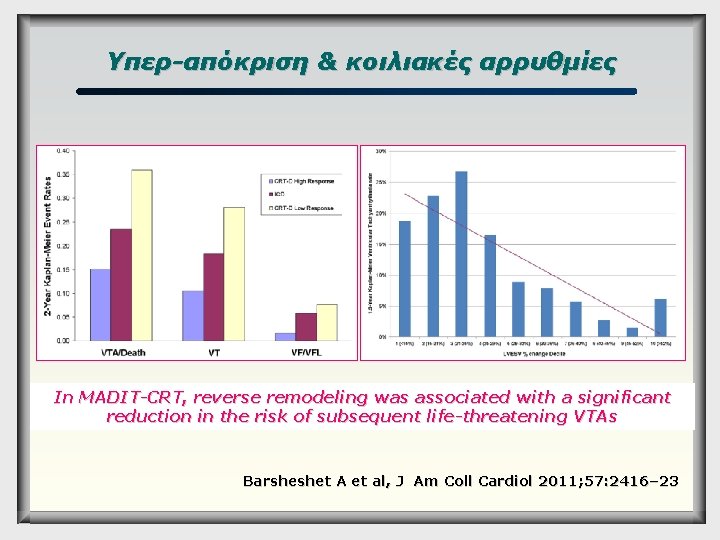
Υπερ-απόκριση & κοιλιακές αρρυθμίες In MADIT-CRT, reverse remodeling was associated with a significant reduction in the risk of subsequent life-threatening VTAs Barsheshet A et al, J Am Coll Cardiol 2011; 57: 2416– 23
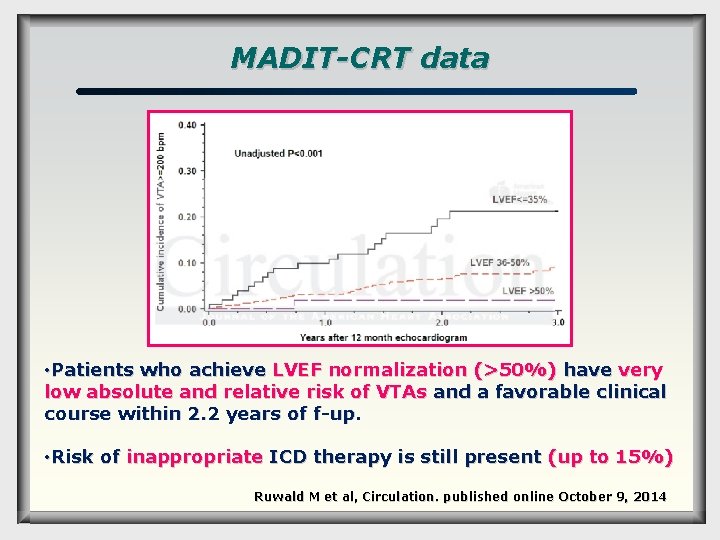
MADIT-CRT data • Patients who achieve LVEF normalization (>50%) have very low absolute and relative risk of VTAs and a favorable clinical course within 2. 2 years of f-up. • Risk of inappropriate ICD therapy is still present (up to 15%) Ruwald M et al, Circulation. published online October 9, 2014

SVT Responses to Adenosine

Complications

Complications q q Device upgrade or revision is associated with a complication risk ranging from 4% of patients who had a generator replacement only, to 15. 3% of patients who had a generator replacement or upgrade combined with one or more transvenous lead insertions. Major complications were higher with CRT-D, compared with PM replacements. Complications were highest in patients who had an upgrade to - or a revised CRT device (18. 7%). These data support careful decision-making before device replacement and when considering upgrades to more complex systems.
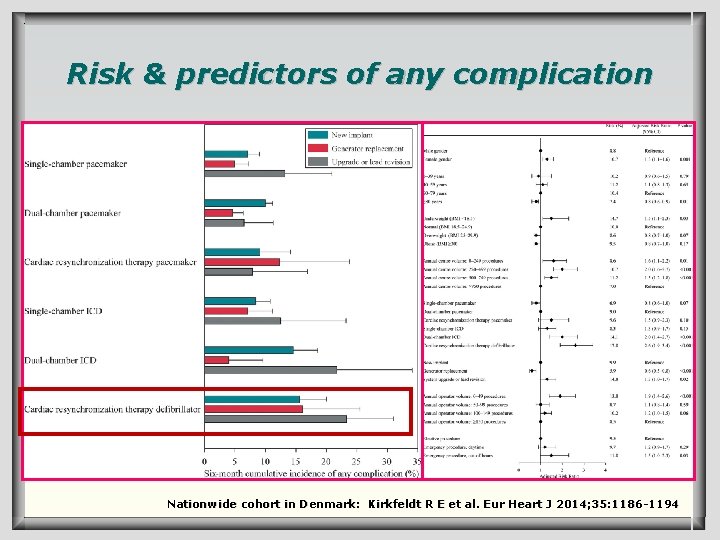
Risk & predictors of any complication Nationwide cohort in Denmark: Kirkfeldt R E et al. Eur Heart J 2014; 35: 1186 -1194

Complications q A meta-analysis of 9082 patients in 25 CRT trials showed that the implantation success rate was 94. 4%: § § peri-implantation deaths occurred in 0. 3% of trial participants, mechanical complications (including coronary sinus dissection or perforation, pericardial effusion or tamponade, pneumothorax and haemothorax) in 3. 2%, § lead problems in 6. 2% § and infections in 1. 4%. Al-Majed NS et al. Meta-analysis: cardiac resynchronization therapy for patients with less symptomatic heart failure. Ann Intern Med 2011
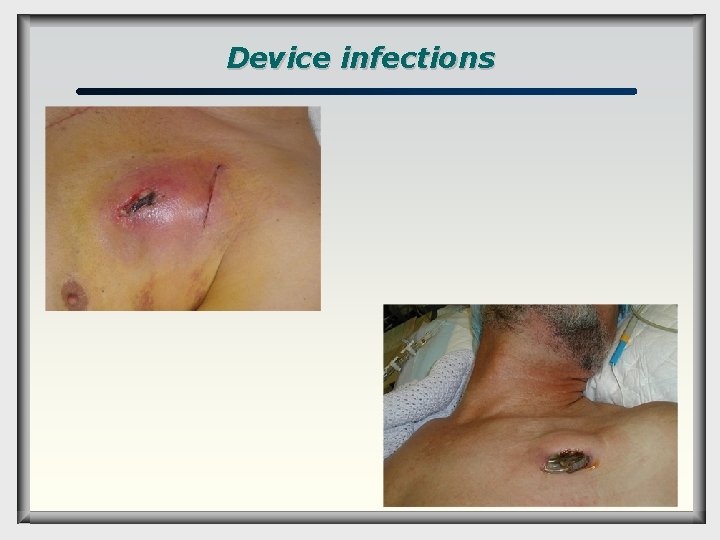
Device infections
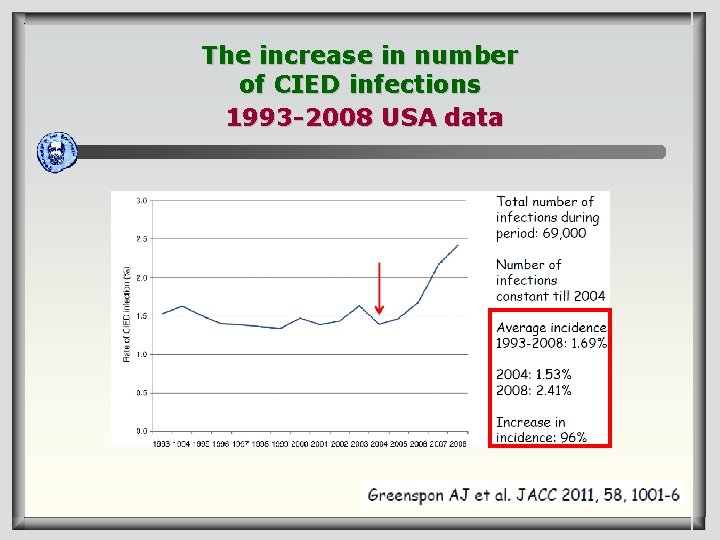
The increase in number of CIED infections 1993 -2008 USA data

Risk factors - Procedure q Operator experience q No antibiotic prophylaxis q Long procedure duration q Device revision /replacement q Fever 24 hrs before implantation q Complexity of procedure /Hardware items q Temporary pacemaker Baddour LM et al, Circulation 2010

Incidence of pacemaker infections

Incidence of pacemaker infections


Clinical factors influencing the likehood to respond to CRT




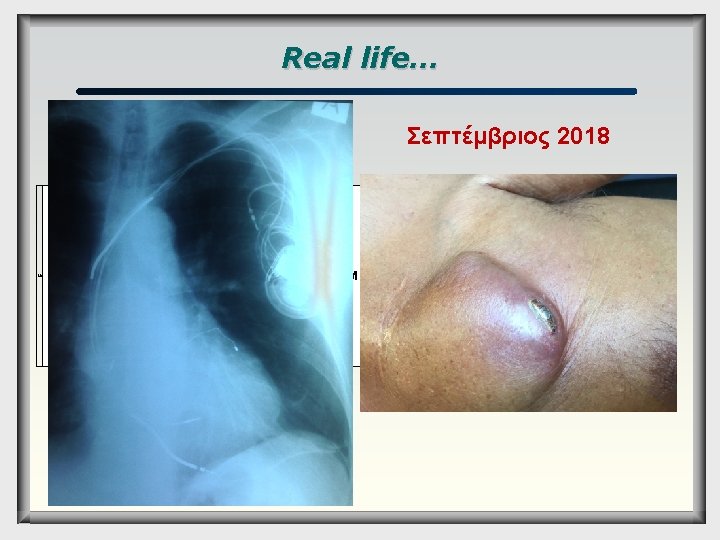
Real life… Σεπτέμβριος 2018 80 Α. Τ. 10/3/2011 1 Medtron Maximo II 9 ic CRT 24/5/2007 In. Sync 4 21/10/2015 Sentry 7 Maximo II CRT sprint 1 DCM fidelis AV block non inducible 15/2/18 replacement with pacesense due to SF (μακρύ θηκάρι)
- Slides: 45