PACEMAKER IMPLANTATION Alpay Celiker M D Acbadem University

PACEMAKER IMPLANTATION Alpay Celiker M. D. Acıbadem University

Pacing in Pediatric & Congenital Heart Disease Advances in lead and device technology allow pacemaker system implantation in children and even in neonates Specific problems in children such as small vessel size, cardiovascular abnormalities often lead to implant problems. Physical activity and somatic growth may affect lead longevity in young patients
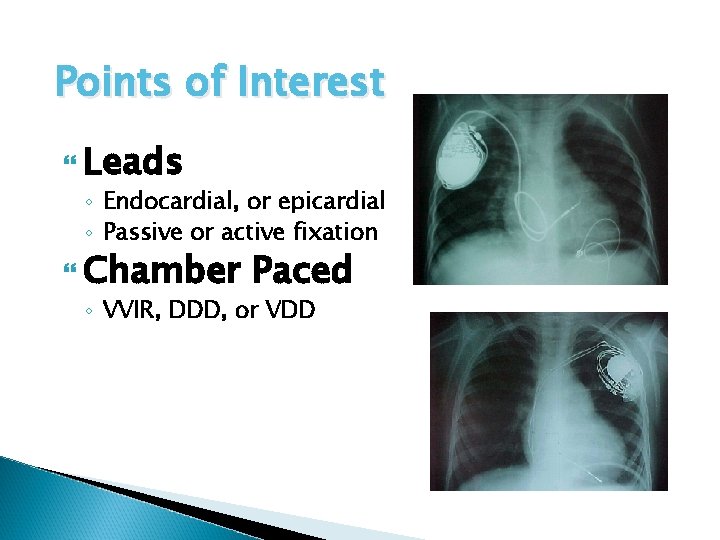
Points of Interest Leads ◦ Endocardial, or epicardial ◦ Passive or active fixation Chamber Paced ◦ VVIR, DDD, or VDD

Pros and Cons of Transvenous Leads • Venous obstructions Leads generally more reliable than epicardial • Pace related impaired ventricular function. implants • Lead infections Procedure more easy • Lead extraction Less thresholds necessity Fast adaptation to new • Interaction with cardiac pacemaker systems valves • Impossible in some patients
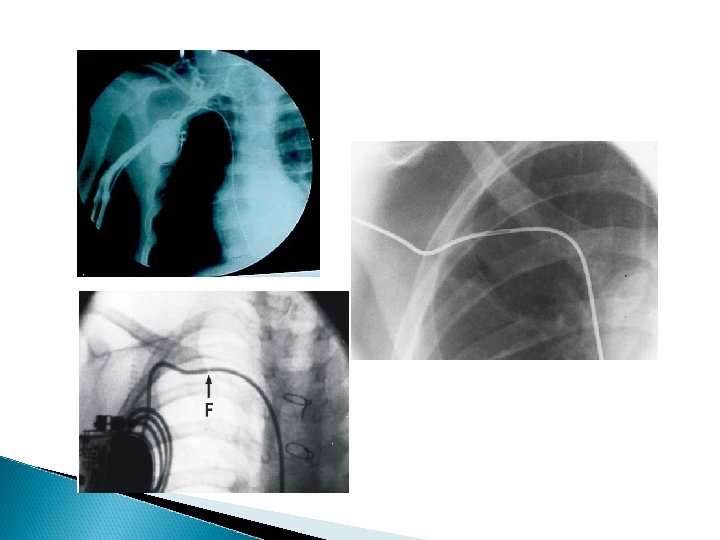
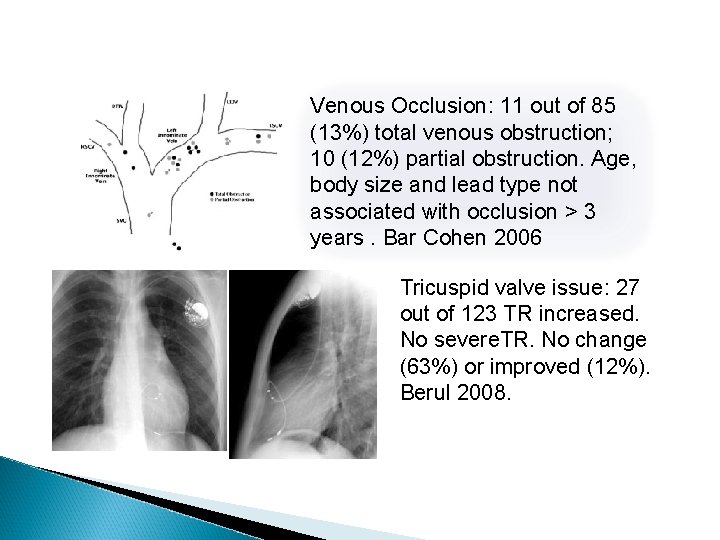
Venous Occlusion: 11 out of 85 (13%) total venous obstruction; 10 (12%) partial obstruction. Age, body size and lead type not associated with occlusion > 3 years. Bar Cohen 2006 Tricuspid valve issue: 27 out of 123 TR increased. No severe. TR. No change (63%) or improved (12%). Berul 2008.

An inhomogeneous and dyssynchronous electrical activation of ventricles, leading to changes in myocardial architecture and left ventricular mechanical contractions. This problem is secondary to right ventricle apical pacing via transvenous pacing. Karpawich P. Pace 2008

Pediatric Pacemaker Infections* Perioperative Infections (before discharge): Staphylococcus ◦Superficial 1, 2 % ◦Deep 0, 2 % Early Pacemaker Infections (< 60 days) ◦Superficial 3, 1 % ◦Deep 1, 2 % species were isolated in 44 % Increased Risks ◦Reintervention ◦Down syndrome ◦Subcutaneous preperitoneal pocket Late Pacemaker Infections ◦Superficial 0, 5 % ◦Deep 0, 7 % * Cohen et al J Thorac Cardiovasc Surg 2002; 124.

Lead Extraction in Children. Why? Remove the intravascular and intracardiac lead material Relieve and reconstruct the venous access for the new leads Prevent lead related infection

Indications Class I: a: sepsis b: life-threatening arrhythmia c: life threatening condition d: thromboembolic event caused by retained lead ◦ Obliteration of all useable veins ◦ Lead interfereres with the operation of another device ◦ ◦
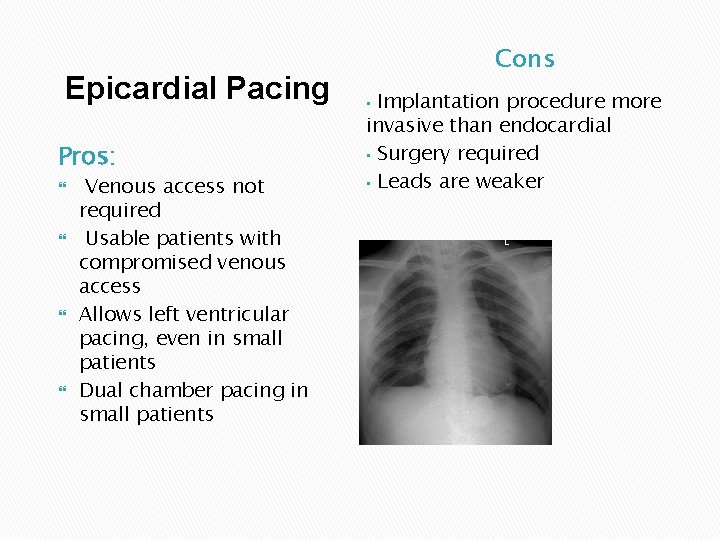
Epicardial Pacing Pros: Venous access not required Usable patients with compromised venous access Allows left ventricular pacing, even in small patients Dual chamber pacing in small patients Cons Implantation procedure more invasive than endocardial • Surgery required • Leads are weaker •

Epicardial versus Endocardial Pacing: Conclusion Epicardial: <15 kg Compromised venous access or a univentricular heart Pace the left ventricle Endocardial Possible implant <15 kg Venous occlusion Risks of future lead extraction Beware of pacing induced heart failure
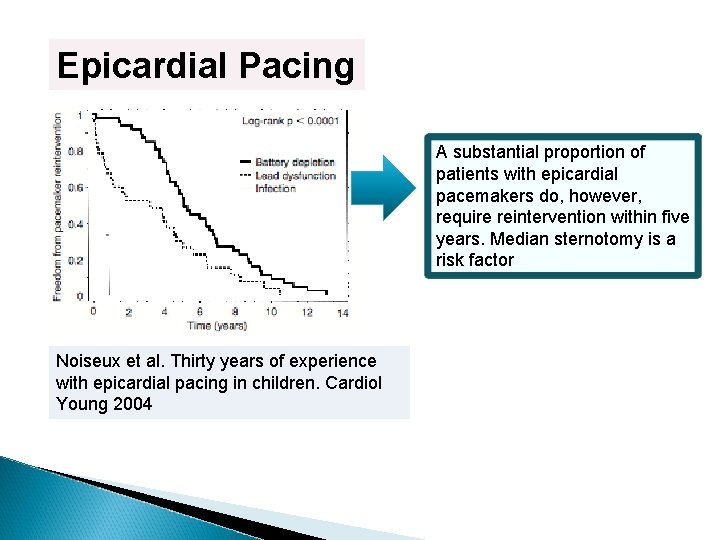
Epicardial Pacing A substantial proportion of patients with epicardial pacemakers do, however, require reintervention within five years. Median sternotomy is a risk factor Noiseux et al. Thirty years of experience with epicardial pacing in children. Cardiol Young 2004
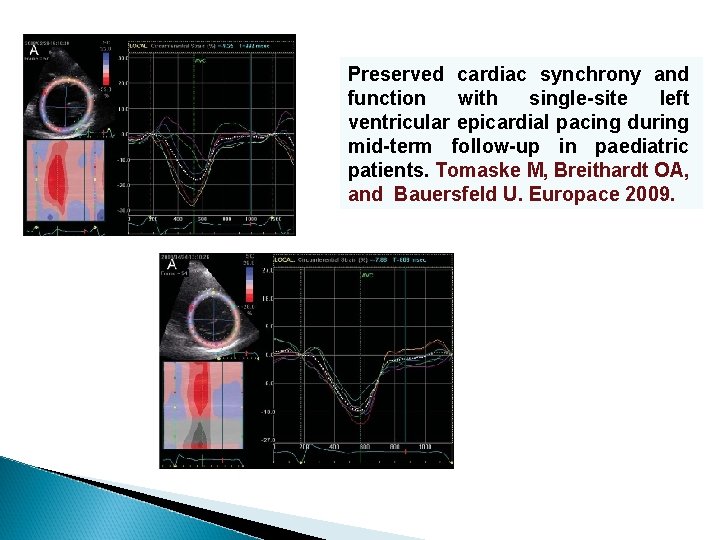
Preserved cardiac synchrony and function with single-site left ventricular epicardial pacing during mid-term follow-up in paediatric patients. Tomaske M, Breithardt OA, and Bauersfeld U. Europace 2009.
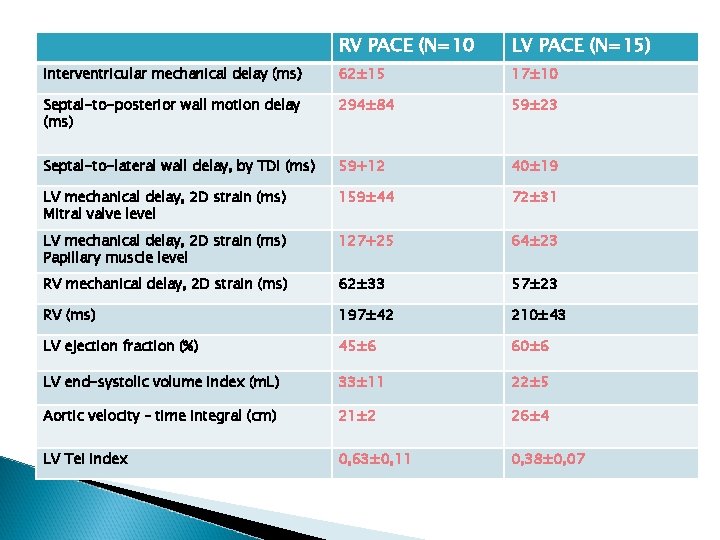
RV PACE (N=10 LV PACE (N=15) Interventricular mechanical delay (ms) 62± 15 17± 10 Septal-to-posterior wall motion delay (ms) 294± 84 59± 23 Septal-to-lateral wall delay, by TDI (ms) 59+12 40± 19 LV mechanical delay, 2 D strain (ms) Mitral valve level 159± 44 72± 31 LV mechanical delay, 2 D strain (ms) Papillary muscle level 127+25 64± 23 RV mechanical delay, 2 D strain (ms) 62± 33 57± 23 RV (ms) 197± 42 210± 43 LV ejection fraction (%) 45± 6 60± 6 LV end-systolic volume index (m. L) 33± 11 22± 5 Aortic velocity – time integral (cm) 21± 2 26± 4 LV Tei index 0, 63± 0, 11 0, 38± 0, 07

DDD vs VDD pacing may be an alternative for DDD pacing in children with normal sinus node function. Ovsyshcher, Rosenthal and Seiden et al. have been showed good results with this mode of pacing. Late results of this mode of pacing seems to encourage Atrial electrogram amplitude was decreased in children without any atrial sensing problem. Loss of atrial sensing can be a problem in children with operated congenital heart diseases. It may be first choice older children with congenital AV block and normal sinus node dysfunction.

VVIR versus DDD Pacing VVIR Pros and Cons ◦ Pros: One lead required, Smaller generator, gives satisfactory exercise tolerance, slower heart rates than DDD ◦ Cons: Heart rate response is not physiological, loss of AVsynchrony, DDD Pros and Cons Pros: Physiological heart rate response, AV synchrony maintained, reduced risk of atrial fibrillation Cons: Two leads required, larger generator, faster heart rates than VVIR, pacemaker mediated tachycardia

VDD Pacing Advantages ◦ Single lead dual chamber sensing ◦ Avoid of many electrodes ◦ Provide AV Synchrony ◦ Avoid of venous thrombosis? ? Disadvantages ◦ Atrial sensing problems in postop. cases ◦ Relative change of atrial dipole with the growth ◦ Decrease of AV synchrony with time ◦ Lack of active fixation ◦ Large electrodes ◦ No indication in SSS ◦ Lack of epicardial use

Site Selective Pacing • Pioneereed by Karpawich. • Implant possible to desired place • Less material at venous system and heart • Similar results compared to conventional systems • Lead extraction issue? • Long-term results? Select Secure system: steroid eluting, bipolar, lumenless, non-retractable screw-in 4, 1 F lead (model 3830, Medtronic, Inc. ), delivered through a 8 F steerable catheter (Select Site) Karpawich et al. Altered cardiac histology following apical right ventricular pacing in patients with congenital atrioventricular block. Pacing Clin Electrophysiol 1999

Conclusion Long term complications of pacing in childhood include venous occlusion, impaired ventricular function, lead failure, and risks of multiple implants and explants. Right ventricular apical pacing should be minimised where possible. In small infants epicardial pacing should be encouraged. Long term complications largely relate to problems with the leads.
- Slides: 21