Paarl Hospital Safety Protocol 2020 Current Situation COVID19


























- Slides: 31

Paarl Hospital Safety Protocol 2020

Current Situation

COVID-19 stats to date - Patients • 5081 tested • 1331 Positive in total • 424 Positive Admissions (cumulative) • 115 COVID-19 Deaths in total

COVID-19 stats to date - Staff • 451 tested • 160 Positive in total • 288 Negative in total • 157 Successfully returned to work • 0 Deaths

Clinical Services Safety Protocol

Patient flow • Patients arriving at Emergency Centre are screened for COVID at entrance and streaming to appropriate clinical areas for interventions. • Viral testing unit was established as a designated area to review high risk patients and test them prior to entry into hospital • Depending on screening initially, when at peak of infections, divided into two patient streams, one high risk COVID stream and one low risk COVID stream to lower risk of patients infecting each other. Different areas and staff were utilized for this. • Patients are seen and placed in allocated areas and overcrowding is prevented as far as possible.

Patient flow • Only a limited number of patients are allowed into the EC evaluation area and patients on trolleys/beds are spaced to prevent cross infection. • Curtains are drawn to prevent droplet spread between patients. • Where required specific areas have been designated and used to perform aerosolizing procedures (isolation/decontamination room). • Specialist disciplines has designated a specific doctor on call to ensure expedited consultation and treatment with disposal or admission of patients to reduce waiting times in emergency centre.

Wards • Specific and designated high risk COVID ward have been identified and deployed to manage patients under investigation (PUI) and COVID + patients to ensure a lower risk of infecting other patients. • Patients are further cohorted and risk stratified and shifted as their COVID status is known as infrastructure allows to protect vulnerable patients (placed in isolation or single rooms) and cohort confirmed positive patients or negative patients • Dedicated staff and clinicians to ensure there is lower risk of cross contamination. • Patients in low risk/non covid areas actively monitored for symptoms development and tested immediately if any NICD criteria present • All psychiatric admission are tested for COVID and placed in isolation until proven negative, since coughing behavior and mask etiquette is challenge with these patients.

Outpatients • All patients arriving for OPD visit are screened for COVID and if screening positive, examined or tested and a new appointment provided if the visit can wait, if not patient are seen in a separate designated area. • OPD number have been reduce to prevent crowding of patients and risk of contamination. a • Seating arrangements at Clinics ensure social distancing and preventing cross infections. • Patients receive extended and repeat scripts and chronic medication is issued and delivered to prevent them from coming into hospital and risk of being infected.

Theatres & Critical Care • All elective procedures have been stopped • Clinicians review all surgical cases to only do emergencies and urgent operations where the risk of delay outweigh the possible risk of COVID infection. • Specific operational procedures have been developed to manage COVID + and PUI theatre cases and dedicated theatres identified during the peak. • Theatre air exchange norms adhere/exceeds the requirements • Thorough cleaning of theatres between cases. • Designated critical care facilities with isolation facilities • Closed suction systems installed reducing the risk of aerosolizing the and infecting other patients during suction. virus

Occupational Health Safety Protocol

Safety measures in place - OHS • • • Individual Risk Assessment for each staff member Covid-19 workplace risk assessment All staff self-screen every day for any Covid-19 symptoms Screened every body entering the facility Training to all staff re: Ø What is Covid? Ø PPE: donning and doffing Ø Waste management Ø Linen management Ø Social distance Ø Hand hygiene Ø What PPE to wear in what area

Safety measures in place - OHS • Social distance enforced in tea rooms, meetings, lifts, offices as well as beds in the wards. • Masks are compulsory for any body entering the facility • Broadcasting reminders 3 x day • Installation of foot operated doors mechanisms • Flu vaccination for all staff • New SOP written: staff member screened positive • EAP in place – Metropolitan Life • Testing of health care workers – Pathcare • Covid 19 posters in all three languages

Safety measures in place - OHS • Surveillance: daily reporting of all positive staff members • All positive staff members are followed up by OHS practitioner on a daily basis • Donning and doffing video’s • PPE: gloves, goggles/visor, gown, scrubs, surgical masks/N 95, disposable apron • All patients wearing cloth of surgical masks • All agency staff members self-screen daily and individual risk assessment done

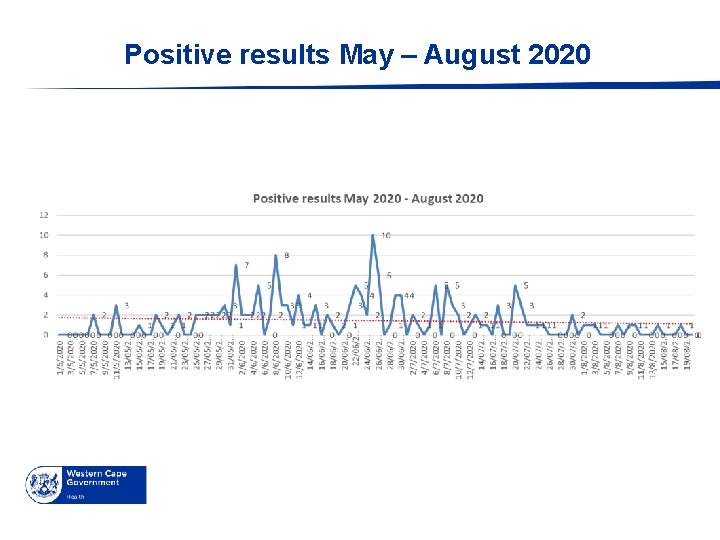
Positive results May – August 2020

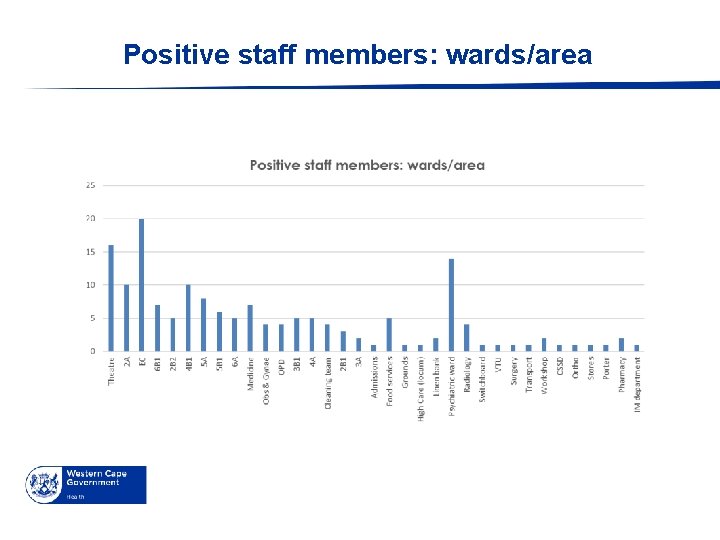
Positive staff members: wards/area

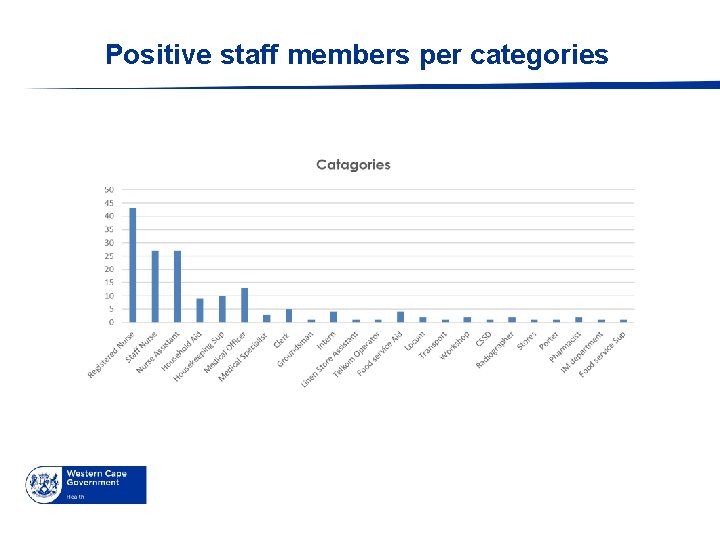
Positive staff members per categories

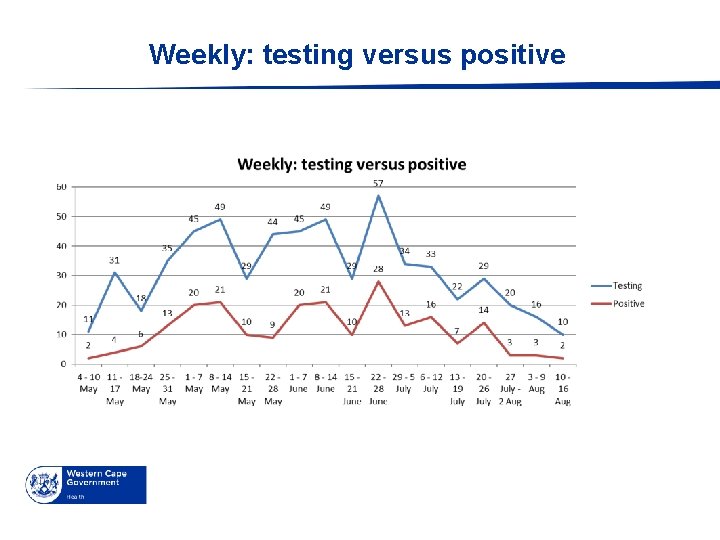
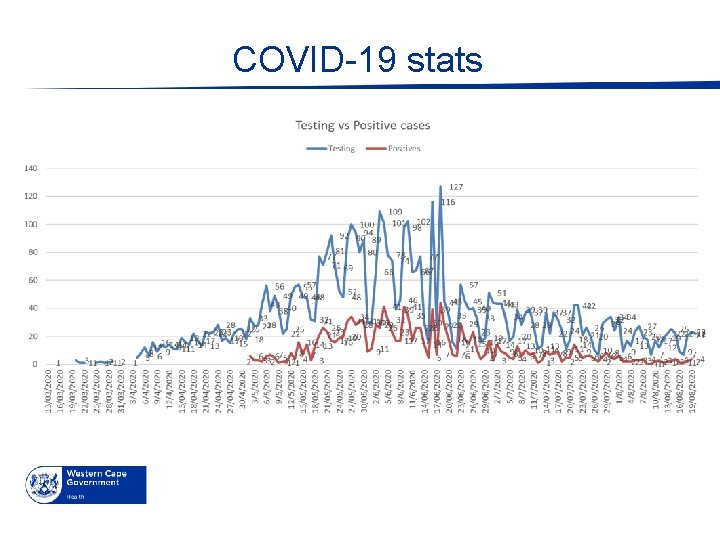
Weekly: testing versus positive

Infection Prevention Safety Protocol

IPC Safety measures Training of all staff regarding: o COVID: What is COVID-19, Transmission routes, Isolation precautions o PPE: Donning & Doffing, What PPE to wear in what area o Hand Hygiene: Correct Alcohol -based hand rub technique, hand washing with soap and water o Waste management: Appropriate PPE to wear, Double bagging, close with cable tie, sealing box with tape, marking box “COVID-19” o Linen Management: Appropriate PPE to wear when handling linen, clear soluble bag o Videos: Donning and Doffing, general information

IPC Safety measures Social distancing enforced: Tearooms, Lifts, offices, all meetings done via MS Teams Masks: Compulsory for anyone entering the facility (staff, public, patients, contractors) Broadcasting reminders 3 x day re hand hygiene, social distancing, surface disinfection, wearing mask COVID-19 posters and reminders throughout the facility Environmental cleaning (Surface disinfection): Checklist implemented for 2 -4 hourly cleaning of all high-touch surfaces for example: doorknobs, desks etc. Installation of foot operated door mechanisms to prevent cross-infection (removed doorknobs) COVID-19 positive bodies: Shroud and waterproof closed body bag Changed method of testing to a mid-nose swab to prevent aerolization of the virus

IPC Safety measures • • New IPC related SOP’s written (all based on provincial and national guidelines) o Environmental cleaning & schedule in high and low risk areas o PPE for all categories of staff o Donning & Doffing o Correct use of chemicals o Cleaning & Disinfection of goggles/visors Hand Hygiene: o Battery operated alcohol-based hand rub (ABHR) dispenser at staff entrance/exit o 50 ml ABHR carry-on bottles for staff o Re-use 500 ml ABHR bottles, decanted in pharmacy to prevent shortage of ABHR Surveillance: Daily reporting of all positive cases

COVID-19 stats

Corporate Governance Safety Protocol

Recruiting Staff • Appointed 6 medical officers on 6 month contract • Appointed 21 Nurses on 6 month contract • Bolstered admin, clerical and support service support through agency

Purchasing Equipment • Medical equipment such as ventilators, high flow oxygen meters, syringe drivers, infusion pumps, monitors, Video Laringoscope, ECG, feeding pumps, cardiotocographs, defibrillator etc… • Other equipment such as beds, mattresses, over-bed tables drip stands, patient and medicine trolleys, flow meters, Oxygen regulators, wall-mounted suction units, drug cabinet, emergency and Food Trolleys, linen carts etc…

Purchasing Services • Environmental cleaning: Extra cleaners used from agency to enhance cleaning • External contractors for high risk areas and also assist with deep cleaning • Rent and erect a viral testing unit • External contractors for securing the viral testing unit • Ambulance services to support transfer between Paarl and Sonstraal • Extra containers to create storage space • Installation of extra wall mounted oxygen points

Increasing medical supplies • Scrubs, Gowns, Occlusive Goggles, Visors, 50 ml carry-on hand sanitizer bottles • Procured Disposable suctioning bottles and closed suctioning system to protect staff • Massive increase in stock levels of all PPE • Masks, hand sanitizers and surface disinfectant for non-clinical staff • Doors to key areas received footpods so they could be opened without touching door handles

What we learned thus far

Lessons learned Without staff you have nothing • Keep them safe, listen to them, keep them informed, find ways to appreciate them and involve them in the planning Staff will get infected • Adjust your capacity planning to accommodate staff absenteeism • Highest risk for staff is colleagues and community, not patients You don’t have time • Plan immediately and act quickly there is far more to do than time allows Be flexible • Your best laid plans will change as you implement and new information emerge You can’t do this alone • Whole of society approach - link with wider health platform, private hospitals, municipality, infrastructure, engineering, NGO, facility board, local business Look after yourself • This is not a sprint but a marathon, personal resilience and mental health should be focused on from the start. Its OK to take some time out © Western Cape Government 2012 | Hospital SOP 30

Thank you