Oxygen Therapy British Thoracic Society Guideline for oxygen

Oxygen Therapy British Thoracic Society Guideline for oxygen use in healthcare and emergency settings 12/05/2017 (update) Key messages for nurses and PAMs (Professions Allied to Medicine)

Important Points to Consider about Oxygen Therapy • Oxygen is a life saving drug for hypoxaemic patients. (Patients whose oxygen levels are low) • Giving too much oxygen is unnecessary as oxygen cannot be stored in the body • COPD patients (and some other patients) may be harmed by too much oxygen as this can lead to increased carbon dioxide (CO 2) levels • Other patients (e. g. myocardial infarction) may also be harmed by too much oxygen • Only give as much as needed– no need for extra!

Oxygen (O 2) What’s the problem? Published audits have shown: • Doctors and nurses have a poor understanding of how oxygen should be used • Oxygen is often given without a prescription (In the 2015 BTS audit, 42% of hospital patients using oxygen had no prescription) • If there is a prescription, patients do not always receive what is specified on the prescription • Where there is a prescription with target range, almost one third of patients are outside the range (9. 5% of Sp. O 2 results below target range and 21. 5% above target range in 2015 BTS audit)

Oxygen is a DRUG and should be prescribed (except in emergencies) • Oxygen should be regarded as a drug (BNF 78 Sept 19 – Mar 2020) • Oxygen must be prescribed in all situations (except for the immediate management of critical illness in accordance with BTS guidelines) (NPSA Oct 2009) • Oxygen should be prescribed to achieve a target saturation (Sp. O 2) which should be written on the drug chart or electronic prescription

Aims of Emergency Oxygen Therapy • To correct potentially harmful hypoxaemia • To alleviate breathlessness (only if hypoxaemic) Oxygen has not been proven to have any consistent effect on the sensation of breathlessness in non-hypoxaemic patients. Benefit has been found with use of a hand-held fan and consider use of opioids for patients with malignancy or other causes of chronic severe breathlessness.

Oxygen therapy by first responders in critical illness • Patients must not go without O 2 therapy while waiting a medical review • Initial O 2 therapy is a high concentration reservoir mask at 15 litres/minute • Once stable aim for Sp. O 2 94 -98% OR patient specific target range • COPD patients who are critically ill should have the same oxygen therapy until blood gases have been obtained and may then need controlled oxygen therapy or Non Invasive or Invasive Ventilation

Prescribing to a target saturation range • It is recommended that all patients are routinely prescribed a target saturation on admission to hospital • This is so that the right target range will be used if the patient deteriorates and used in conjunction with the NEWS 2 • Patients will only receive O 2 therapy if the saturation falls below the target
Normal oxygen saturation range in healthy adults HEALTHY ADULTS Daytime Sp. O 2 96 -98% *Transient dip in saturation are common during sleep (˜ 84%)

Patients will initially be prescribed a target saturation • 94– 98% Most patients (Those not risk at risk of CO 2 retention) • 88– 92% COPD or CO 2 retaining patients: Chronic hypoxic lung disease COPD Severe Chronic Asthma Bronchiectasis Chest Wall Disease Kypho-scoliosis Neuromuscular disease Obesity hypoventilation • Other Some patients with oxygen sensitivity may require a different lower target range such as 85 – 90% Target saturations should be reviewed and changed if required This guideline recommends an upper limit of 98% for most patients Combination of what is normal and safe

Safeguarding patients at risk of Type 2 Respiratory Failure • • Lower target saturation range for these patients (usually 88 -92%) Education of patients and health care workers Use of oxygen alert cards Issue of personal oxygen mask/nasal to high risk patients

Who does What? Doctors (and other prescribers) • • • Prescribe O 2 target range for ALL patients Registered Nurses/Midwives/AHP/NA • Assess patient • Monitor patient • If indicated start O 2 and ensure target achieved • Observation and NEWS 2 completion • Titrate O 2 to keep in range • Record Sp. O 2 and delivery device • Monitor O 2 minimum 4 hourly. • Inform nurses when Sp. O 2 outside target range – urgency? • Liaise with Registered Staff regarding care and safety of patient receiving oxygen therapy Usually 94 -98% or 88 -92% May specify starting device Review patient accordingly/diagnostics Provide advice to nurses if the clinical condition of the patient changes Adjust the target range if the patient’s condition alters (e. g. new hypercapnia) HCA / Student nurses / TNA • Follow guidance • Complete documentation • Record Sp. O 2 & delivery device/ NEWS 2 • Wean off O 2 if clinically stable • Inform and educate patient
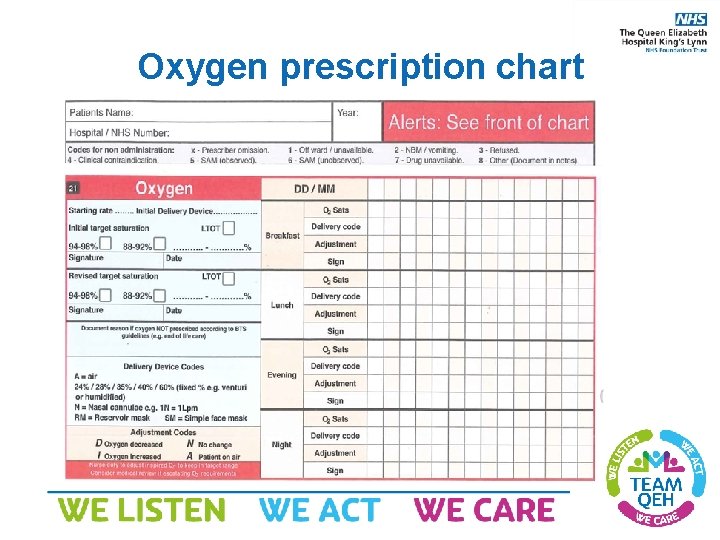
Oxygen prescription chart

Monitoring and Starting Oxygen Therapy Record Sp. O 2 before starting oxygen therapy where possible. (Do NOT take oxygen off an acutely unwell patient to obtain a reading on air) If target saturation is 94 -98% • Choose mask and/or flow rate to achieve target saturation • Repeat blood gases are not needed for these patients if within target range If target saturation is 88 -92% • Start with nasal cannula at 1 -2 l/minute or 28% Venturi mask then titrate to achieve the target saturation • Blood gases are needed after 30 -60 mins If ‘Other’ Sp. O 2 prescribed - start as directed by doctor Monitor Sp. O 2 for first 5 minutes and then monitor patient Sp. O 2 minimum 4 hourly. Record delivery device and flow on observations chart.

Maintaining the target saturation • Nurses may use the oxygen escalator (next slide) • Masks and flow rate should be changed up or down to ensure target saturation range is met as quickly as possible • Nurses do not need to use each step of the escalator and can change devices and/or flow rate to ensure target Sp. O 2 is achieved Always monitor Sp. O 2 for 5 minutes after any change in oxygen therapy to ensure target saturation is achieved.

Titrating Oxygen up and down using the mask escalator This table below shows APPROXIMATE conversion values. Venturi 24% (BLUE) 2 -3 L/M OR Nasal Cannulae 1 L OR Nasal Cannulae 2 L OR Nasal Cannulae 4 L Venturi 40% (RED) 10 -15 L/M OR Simple face mask Venturi 60% (GREEN) 15 L/M OR Simple face mask 7 -10 L/min Venturi 28% (WHITE) 4 -6 L/M Venturi 35% (YELLOW) 8 -12 L/M Reservoir mask at 15 L oxygen flow If reservoir mask is required, seek senior medical input immediately

Titrating oxygen up or down in a target saturation range 94 -98% Increase oxygen if Sp. O 2 is lower than target range Decrease oxygen if Sp. O 2 is higher than target range • Monitor Sp. O 2 for 5 mins at every change • Document Sp. O 2 on chart after 5 mins If oxygen therapy is increased, medical assessment is needed and blood gases may be required If oxygen therapy is decreased for a stable patient, blood gases are NOT needed - No need to inform doctor if clinically stable - Ensure change is documented in patient record

Titrating oxygen up or down in a target saturation range 88 -92% or other Increase oxygen if Sp. O 2 is lower than target range Decrease oxygen if Sp. O 2 is higher than target range • Monitor Sp. O 2 for 5 mins at every change • Document Sp. O 2 on chart after 5 mins If oxygen therapy is increased, take blood gases after 30 -60 minutes (show doctor results) If oxygen therapy is decreased for a stable patient, blood gases are NOT needed - No need to inform doctor if clinically stable - Ensure change is documented in patients record

Checks prior to increasing oxygen • • • Airway Patient position Check device, check tubing, check flow rate Is oxygen piped? Is there piped air? Is oxygen cylinder empty or integral valve in open position • Drug therapies (e. g nebuliser) • Check oxygen saturation monitor working / used correctly

Stopping oxygen therapy for stable patients Stop 02 if patient stable and Sp. O 2 is within range on 2 consecutive observations • Patient will usually be weaned to low dose oxygen by this time • Stop supplemental oxygen & monitor Sp. O 2 for 5 mins & document this in the chart • If Sp. O 2 remains stable, continue on air for 1 hour monitoring Sp 02 • Document Sp. O 2 on chart at end of hour • If stable at one hour, the patient is weaned off oxygen and continues regular observations If saturation falls on stopping oxygen, then re-start the previous dose In cases of acute deterioration or if Sp. O 2 fall outside of the target range despite re-starting oxygen therapy, the patient should have an immediate medical review
Devices to use

High concentration reservoir mask • • Non re-breathing Reservoir Mask Critical illness / Trauma patients Post-cardiac or respiratory arrest Delivers O 2 concentrations between 60 & 80% or above Effective for short term treatment Has your patient been reviewed by Medical team? Check frequency of observations

Nasal Cannula • • • Recommended for most patients. 1 -6 L/min gives approx 24 -50% FIO 2 4 L/min max recommended FIO 2 depends on oxygen flow rate and patient’s minute volume and inspiratory flow and pattern of breathing. Comfortable and easily tolerated No re-breathing Patient can eat and drink Preferred by patients Low cost product Check pressure areas Two lengths
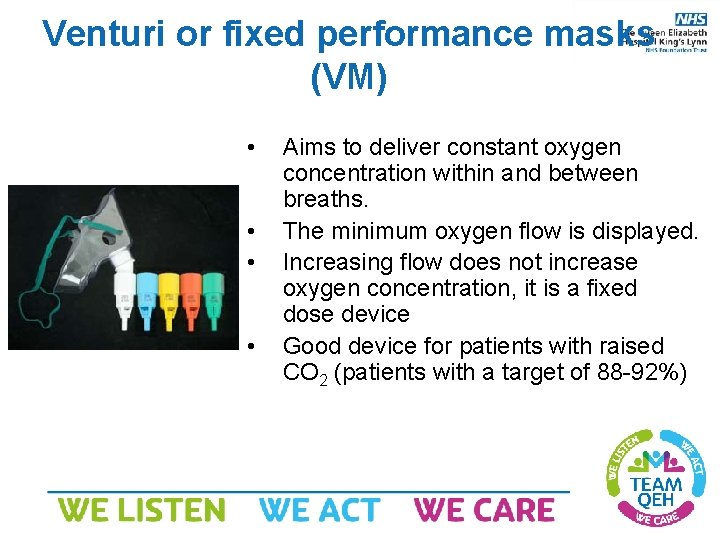
Venturi or fixed performance masks (VM) • • Aims to deliver constant oxygen concentration within and between breaths. The minimum oxygen flow is displayed. Increasing flow does not increase oxygen concentration, it is a fixed dose device Good device for patients with raised CO 2 (patients with a target of 88 -92%)
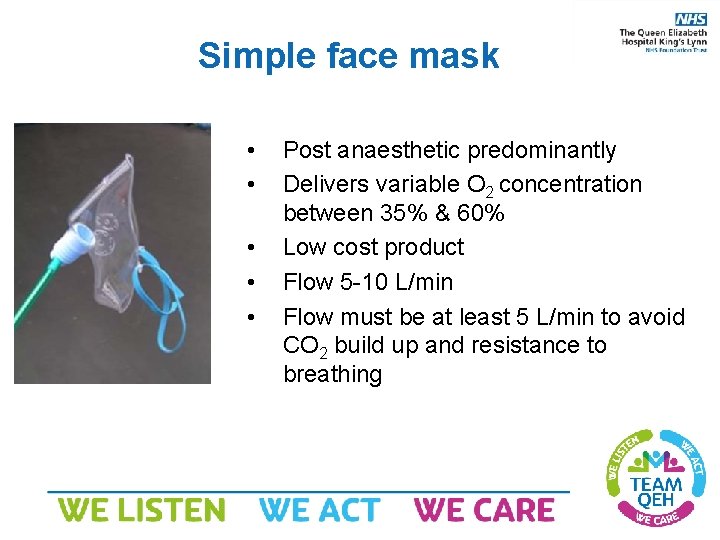
Simple face mask • • • Post anaesthetic predominantly Delivers variable O 2 concentration between 35% & 60% Low cost product Flow 5 -10 L/min Flow must be at least 5 L/min to avoid CO 2 build up and resistance to breathing

Humidified Oxygen • Tracheostomy • Bronchiectasis • Cystic Fibrosis patients • Physiotherapists may advise humidification • Humidification may be provided by cold or warm humidifiers • ( H 24, H 28, H 35 etc. ) The illustration shows a cold humidifier delivering 28% oxygen at 5 l/min flow. N. B. There is little evidence for humidification in routine oxygen therapy
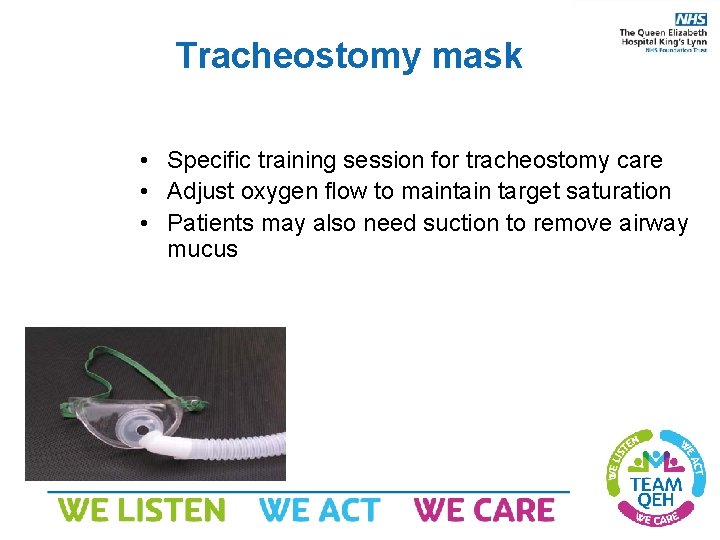
Tracheostomy mask • Specific training session for tracheostomy care • Adjust oxygen flow to maintain target saturation • Patients may also need suction to remove airway mucus
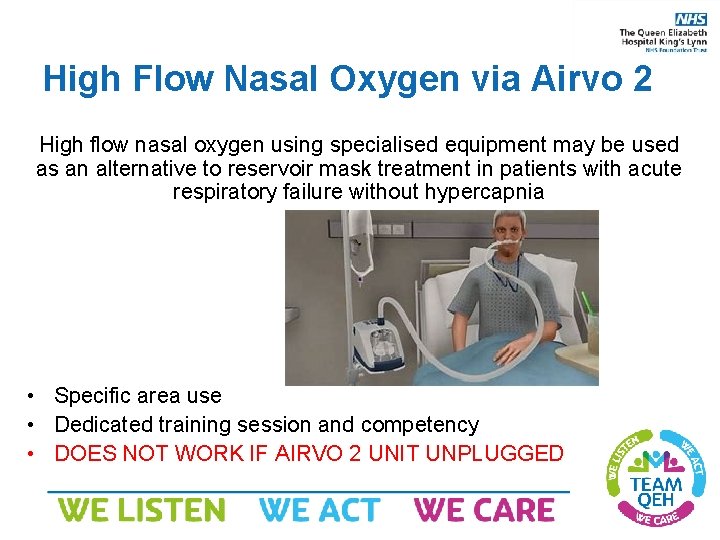
High Flow Nasal Oxygen via Airvo 2 High flow nasal oxygen using specialised equipment may be used as an alternative to reservoir mask treatment in patients with acute respiratory failure without hypercapnia • Specific area use • Dedicated training session and competency • DOES NOT WORK IF AIRVO 2 UNIT UNPLUGGED

Oxygen Flow Meter The ball must be centred on the line. This diagram illustrates the correct setting of the flow meter to deliver a flow of 2 litres per minute.

Check your medical gas

TRANSFER OF PATIENT RECEIVING OXYGEN THERAPY ADDRESSOGRAPH LABEL WARD……………. . . DESTINATION………………. . . . . OXYGEN FLOW RATE …………L/M OXYGEN DEVICE ……………… You are signing this form to confirm that you have assessed the above named patient and that they are safe for transfer without a Registered Nurse escort. You have transferred your patient’s oxygen supply to a CD cylinder and ensured flow and capacity for duration of the transfer. DATE ………… TIME………… SIGNATURE OF REGISTERED NURSE………. . . . . PRINT NAME ………………………………. . An assessed as competent SHCA or Porter can escort a patient receiving oxygen with a flow rate ≤ 35% O 2 via venturi or ≤ 4 L/M via nasal specs or simple face mask ONLY if patient is stable as assessed by the Registered Nurse. A Registered Nurse must escort a patient who requires additional monitoring/intervention on any flow rate of oxygen OR receiving oxygen with a flow rate of 40% or more via venturi or ≥ 5 L/M via simple face mask. (MR V 3 02/19) Signature of RN on return to Ward…………DATE/TIME……………………………….

Safety • • Oxygen supply Nebuliser therapy (40% oxygen drive via O 2) Explain/educate your patient and carer(s) Be aware of oil based creams/lotions/alcohol hand gel Store cylinders in designated holder Smoking/naked flames Too little or too much oxygen cause harm Incident reporting
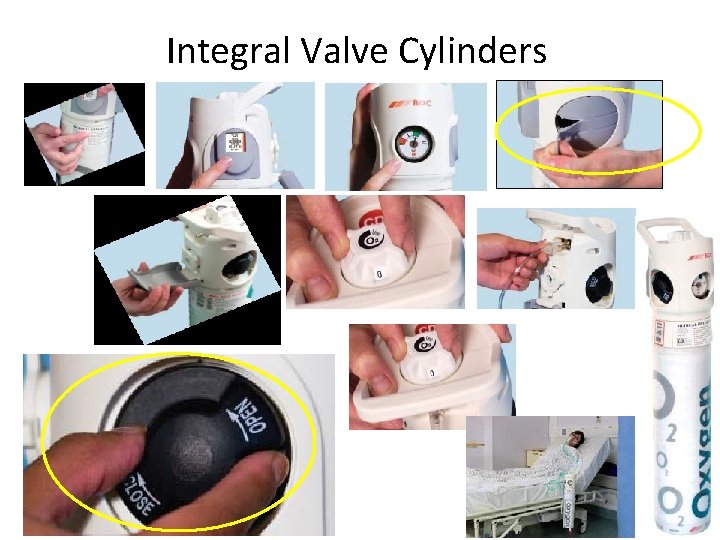
Integral Valve Cylinders

Additional Support Mandy Rye Respiratory Nurse Specialist Ext 4645 Bleep 2460
- Slides: 33