Oxford Inflammatory Bowel Disease Master Class Understanding Pouch

Oxford Inflammatory Bowel Disease Master. Class Understanding Pouch Problems (in context) Kangaroo Club Dr Oliver Brain DPhil Consultant Gastroenterologist 7 th Oct 2017

Overview · Normal pouch function · Pouchitis · Structured approach to pouch dysfunction
‘Normal’ pouch function? · 6 -8 bowel movements per 24 h · 1 -2 bowel movements per night (approx 50% of patients) · Lack of urgency / able to defer for 1 h · Loose or semi-formed · Occasional seepage at night · Pouch function stabilises 1 year post surgery Fazio V etal Ann Surg 1995; 222: 120 -127 Sagar PM, Pemberton JH Dig Dis 1997; 15: 172 -188
What is normal?
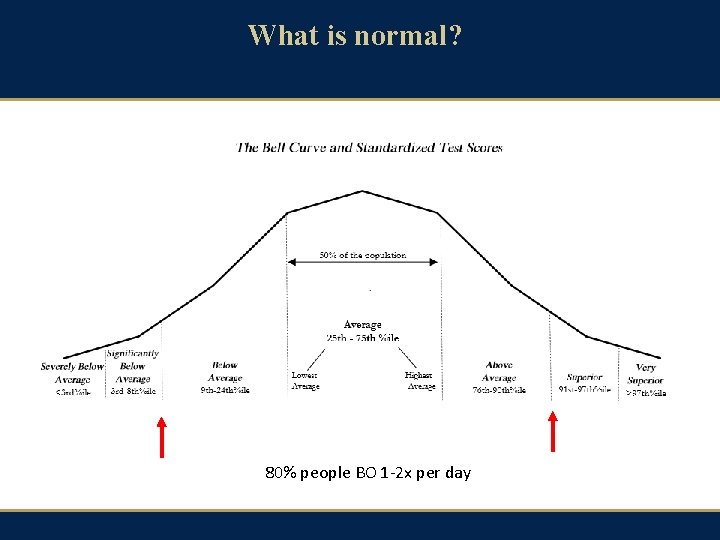
What is normal? 80% people BO 1 -2 x per day

What is normal?
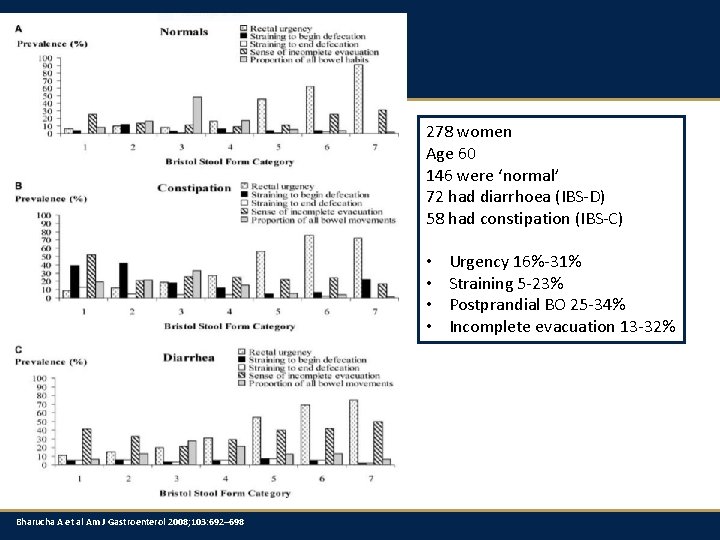
278 women Age 60 146 were ‘normal’ 72 had diarrhoea (IBS-D) 58 had constipation (IBS-C) • • Bharucha A et al Am J Gastroenterol 2008; 103: 692– 698 Urgency 16%-31% Straining 5 -23% Postprandial BO 25 -34% Incomplete evacuation 13 -32%
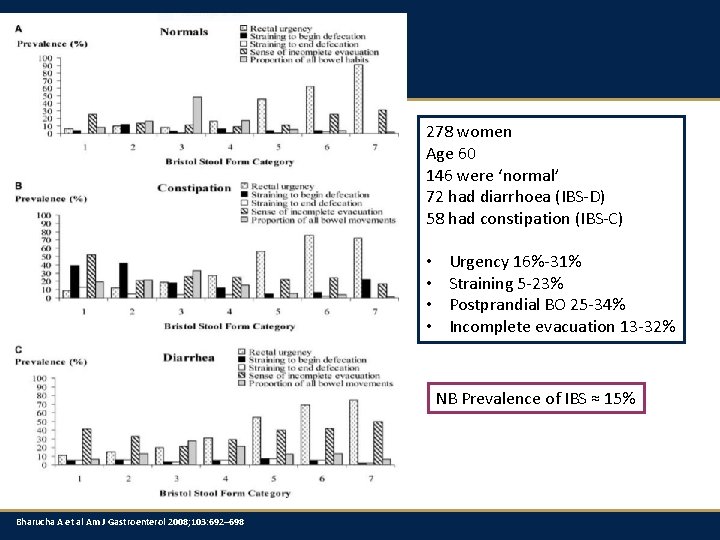
278 women Age 60 146 were ‘normal’ 72 had diarrhoea (IBS-D) 58 had constipation (IBS-C) • • Urgency 16%-31% Straining 5 -23% Postprandial BO 25 -34% Incomplete evacuation 13 -32% NB Prevalence of IBS ≈ 15% Bharucha A et al Am J Gastroenterol 2008; 103: 692– 698

Problems Specific to the Pouch · Pouchitis
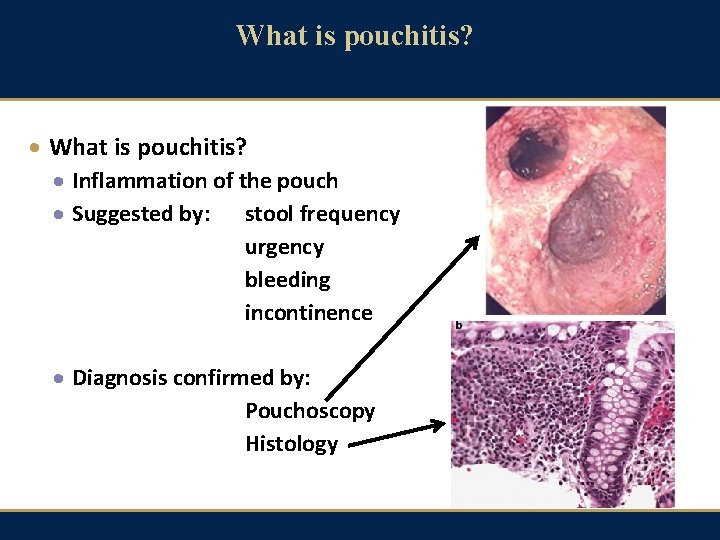
What is pouchitis? · What is pouchitis? · Inflammation of the pouch · Suggested by: stool frequency urgency bleeding incontinence · Diagnosis confirmed by: Pouchoscopy Histology
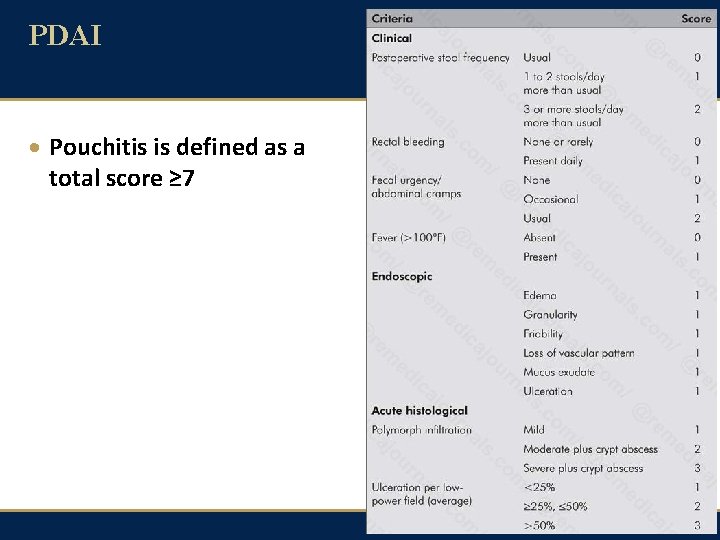
PDAI · Pouchitis is defined as a total score ≥ 7

Patterns of pouchitis · Acute: ≤ 4 weeks · Chronic: > 4 weeks · Infrequent · Treatment responsive · Relapsing · Treatment refractory · Continuous

Pouchitis prevalence · 50% of UC patients will have ≥ 1 acute episode 1 · Up to 60% suffer recurrent episodes pouchitis · Prevalence of chronic pouchitis is 5 -10%1 · Pouch failure · At 20 years pouch failure rates are 10 -15%2 · Pouchitis accounts for 10% of pouch failure 3 1. Simchul et al World J Surg 2000. Stahlberg et al Dis Colon Rectum 1996. Lohmuller et al Ann Surg 1990. Salemans et al Dig Dis Sci 1992. Dis 2010. Hahnloser et al Br J Surg 2007. Leowardi et al Lengenbecks Arch Surg 2010 3. Tulchinsky et al Ann Surg 2003 2. Tekkis et al Colorectal
Why does pouchitis occur? · Idiopathic · Occurs in up to 50% of UC patients · Rarely seen in FAP patients · Genetic risk? · Microbial risk / dysbiosis?

Genetics of pouchitis · Small, underpowered studies. · IL 1 RA 1 · NOD 22 · TLR 93 · CD 143 } Chronic relapsing pouchitis 1. Brett et al EJGH 1996; Carter et al Gastroenterology 2001. 2. Seghal et al Dis Colon Rectum 2010; Tyler et al Gastroenterology 2011 3. Lammers et al World J Gastroenterol 2005

Other Risk Factors · Extensive / severe UC } } · Pre-colectomy thrombocytosis · Backwash ileitis · Extra-intestinal manifestations · p. ANCA positivity · Non-smokers · NSAID use Reviewed in Landy J et al Inflamm Bowel Dis 2012 Reflection of disease severity Reflect PSC association

Risk Factors · PSC · Associated with a 2 -fold increase in risk of pouchitis 1 · Also associated with pre-pouch ileitis · Ig. G 4 may be associated with a subset of chronic pouchitis patients 2 1. Zins BJ et al Am J Gastroetnerol 1995. Penna C et al Gut 1996. 2. Navaneethan U et al Gastrointestin Surg 2011

Aetiology · Pouch mucosal adaptation and colonic metaplasia · Part of a normal adaptive response · Altered short chain fatty acid metabolism · Anaerobic fermentation of PSAs · Bile acids · Conflicting data · Microbiome

Microbiome · Pouchitis only occurs once ileostomy closed · Pouch is exposed to concentrations >106 times the TI 1, 2 · Evidence of an altered microbial signature in pouchitis 3, but there is significant study heterogeneity · Antibiotics · Probiotics 1. Nicholls et al Gut 1981. 2. Santavirta et al Int J Colorectal Dis 1991 3. Landy J et al Inflamm Bowel Dis 2012
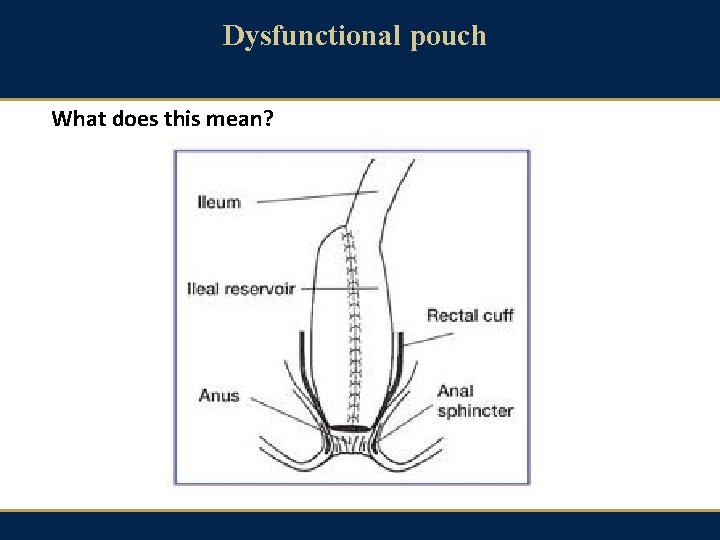
Dysfunctional pouch What does this mean?

What does ‘dysfunctional pouch’ mean? · Answers: · a) Dysfunctional pouch = poorly functioning pouch from any cause · b) Dysfunctional pouch = poor pouch function in absence of demonstrable pouchitis / inflammation · c) Dysfunctional pouch = irritable pouch
Dysfunctional Pouch · Obstruction: Stricture Functional obstruction · Peri-pouch sepsis: Acute or historic · Small volume pouch · Irritable pouch – symptoms with a PDAI <7

Risk Factors for Pouch Dysfunction · Patient-dependent · IBS · Weak sphincters · Disease-dependent · PSC · Surgery-dependent · Peri-pouch sepsis / anastomotic leak · Anastomosis formation · Small pouch volume

Patient · 28 year old man · Background UC and PSC diagnosed 6 years ago · Colectomy for refractory colitis 3 years ago · Post-operative anastomotic leak · Best pouch function: · 6 x per day, 2 x nocte · Minimal urgency, occasional nocturnal accidents · Currently · · · 12 x per day, 3 x nocte Severe urgency, incontinence every other day Minimal response to antibiotics
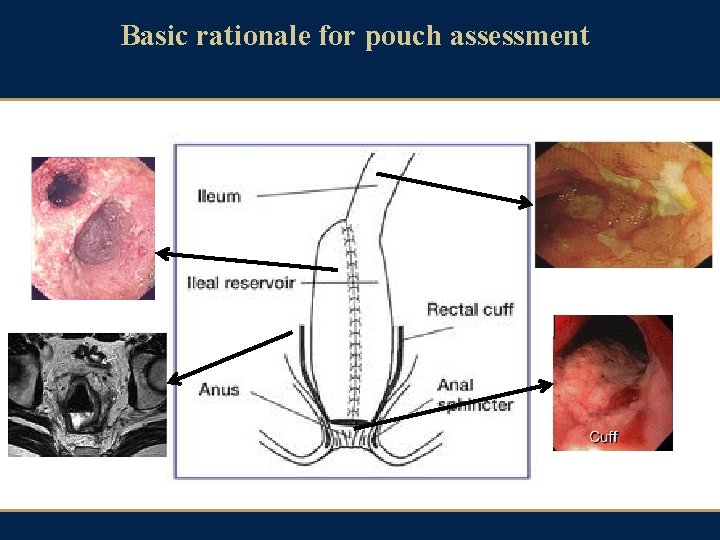
Basic rationale for pouch assessment
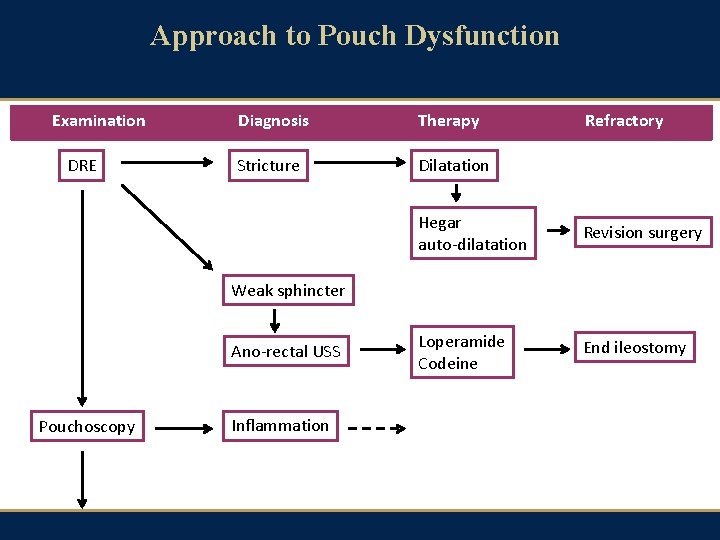
Approach to Pouch Dysfunction Examination DRE Diagnosis Therapy Stricture Dilatation Refractory Hegar auto-dilatation Revision surgery Loperamide Codeine End ileostomy Weak sphincter Ano-rectal USS Pouchoscopy Inflammation
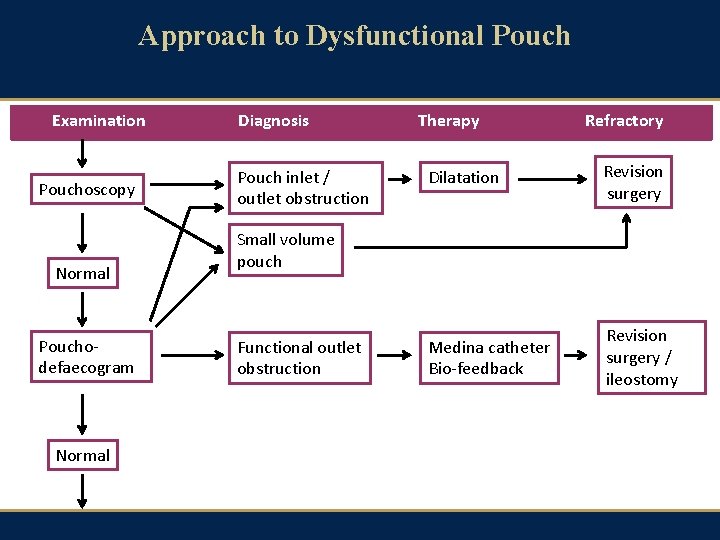
Approach to Dysfunctional Pouch Examination Pouchoscopy Normal Pouchodefaecogram Normal Diagnosis Pouch inlet / outlet obstruction Therapy Refractory Dilatation Revision surgery Medina catheter Bio-feedback Revision surgery / ileostomy Small volume pouch Functional outlet obstruction
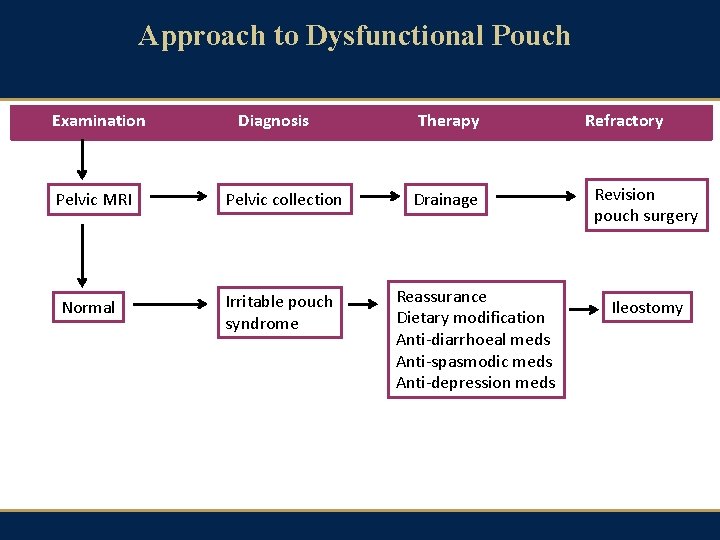
Approach to Dysfunctional Pouch Examination Diagnosis Pelvic MRI Pelvic collection Normal Irritable pouch syndrome Therapy Drainage Reassurance Dietary modification Anti-diarrhoeal meds Anti-spasmodic meds Anti-depression meds Refractory Revision pouch surgery Ileostomy

Patient · Pouch-anal anastomotic stricture (moderate) àDilated endoscopically · MRI peri-pouch fibrosis · Recovery of reasonable pouch function

Summary · Many people with and without pouches have GI symptoms when surveyed. · Pouch dysfunction can be due to both pouch-related and unrelated causes · A structured approach to investigation and management is required
- Slides: 30