Overview of the Management of Vulnerable and Underserved

Overview of the Management of Vulnerable and Underserved Populations N 530, 535

Cost, Quality, Access to Care

Introduction • Certain populations in the United States face greater challenges in accessing timely and needed health care services • They are at risk for poor physical, psychological and/or social health
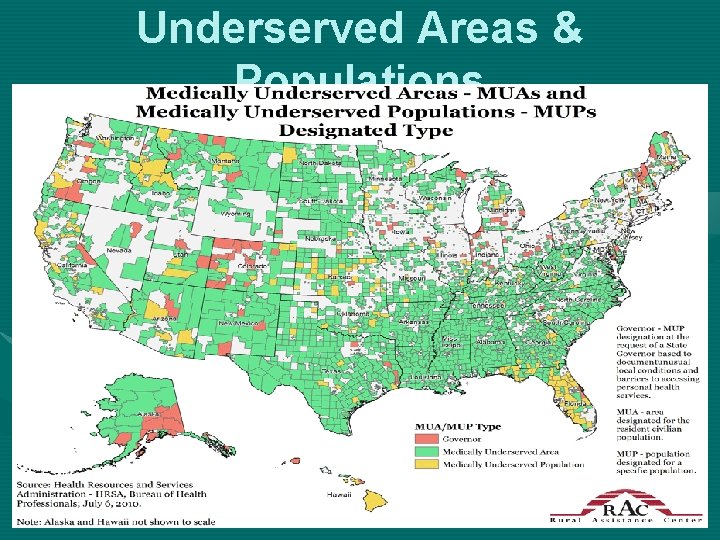
Underserved Areas & Populations
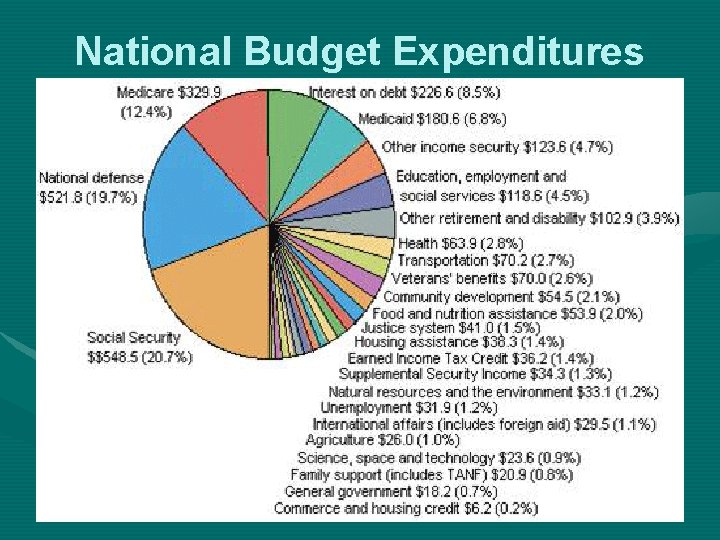
National Budget Expenditures

Terminology These populations are called: • Underserved populations • Medically underserved • Medically disadvantaged • Underprivileged • American under classes

Population Health Issues

Introduction Their vulnerability is due to: • Unequal social, economic, health and geographic conditions They consist of: • Racial and ethnic minorities • Uninsured children • Women • Those living in rural areas • Homeless • Mentally Ill • Chronically ill and disabled • HIV/AIDS patients

Framework to Study Vulnerable Populations • Racial/Ethnic Minorities • Women and Children • Geographical Distribution: Rural Health

Framework to Study Vulnerable Populations • Vulnerability Model: an integrated approach to studying vulnerability • Vulnerability: denotes susceptibility to negative events • In health care, vulnerability is the likelihood of experiencing poor health or illness

Framework to Study Vulnerable Populations • Poor health is compounded for problems along multiple dimensions • Vulnerability represents the interaction effects of multiple factors over which many do not have control

Framework to Study Vulnerable Populations Vulnerability is determined by a convergence of: • Predisposing • Enabling • Need • Characteristics at both the individual and ecological level • They converge and determine access to care and influence individuals’ risk of contracting illness

Framework to Study Vulnerable Populations • Understanding vulnerability as a combination or convergence of disparate factors is preferred over studying individual factors separately

Framework to Study Vulnerable Populations The Vulnerability Model has distinctive characteristics: • It is comprehensive, including individual and ecological attributes of risk • It focuses on the attributes of vulnerability for the total population rather than on vulnerable traits of subpopulations

Framework to Study Vulnerable Populations • It emphasizes the convergence of vulnerability • Multiple vulnerable traits may lead to cumulative vulnerability that is additive or multiplicative

Framework to Study Vulnerable Populations Attributes that predispose vulnerability include: • Demographic characteristics • Belief Systems • Social Structures variables • These attributes influence vulnerability status • They are associated with social position, status, access to resources, health behaviors and variations in health status

Race/Ethnic Minorities • In 1997 The U. S. Office of Management and Budget (OMB) included race and ethnicity to reflect diversity • Minimum categories of race include: Black, Asian, American Indian or Alaska Native, Native Hawaiian or Other Pacific Islander and White • OMB included 2 ethnicities: Hispanic and Latino

Racial/Ethnic Minorities

Racial/Ethnic Minorities • Significant differences exist across the various racial/ethnic groups on health • Minority race and ethnicity usually serves as a proxy for factors such as: socioeconomic status, language ability, or cultural behaviors that are correlated with health status and health care experiences • Racial/ethnic minorities have poorer access, receive poorer-quality care and greater deficits in health status.

Racial/Ethnic Minorities • Consistently over decades of research: • Minorities have poor access to health services compared with white counterparts even after considering insurance, socioeconomics, and health status • The most commonly used measure of access is whether or not a person has a regular or usual source of care

Vulnerable Women and Children

Women and Children • Women in the U. S. enjoy a life expectancy almost eight years longer than that of men, but they: • -Have a higher prevalence of health problems over their lifetime • -Develop more acute and chronic illnesses resulting in more short and long term disabilities

Women and Children • Have a higher percentage of deaths at all ages for heart disease and stroke • Have the highest growing population diagnosed with AIDS • Suffer greater morbidity and poorer health outcomes • Differences between men and women are equally pronounced for mental illness

Women and Children • Children’s health has unique aspects of delivery such as: developmental vulnerability, dependency, and patterns of morbidity and mortality • Developmental vulnerability refers to: the rapid and cumulative physical and emotional changes that characterize childhood and the effects that illness, injury or untoward family and social circumstances can have on a child’s life.

Women and Children • Dependency means: the special circumstances children face where others have to recognize and respond to their health needs. • Children are increasingly affected by “new morbidities” such as: • -Drug and alcohol abuse • -Family and neighborhood violence • -Emotional disorders • -Learning problems

Rural Health Care

Geographic Distribution: Rural Health • Poverty: is consistent in rural areas and affects access • Geographic mal-distribution creates a shortage of health care professionals in rural settings which is another dimension of poor health care delivery • Rural populations face greater barriers in access to care

Geographic Distribution: Rural Health To improve access in rural America there is: • The National Health Service Corps • Health Manpower Shortage Areas • Medically Underserved Areas • Community and Migrant Health Centers • Rural Health Clinics Acts

Enabling Characteristics • • These include: Socioeconomic status Individual assets Mediating factors

Enabling Characteristics • Socioeconomic status is associated with social position, access to resources, variations in health status, income, education, employment status and occupation • Individual assets (human capital) contributes to one’s ability to be selfsufficient • Mediating factors are associated with the use of health care services (e. g. health

Enabling Characteristics Uninsured tend to: • Be poor and less educated • Work in part-time jobs and/or are employed by small firms • Be younger (25 -40) • Be ethnic minorities

Enabling Characteristics Homelessness • The homeless face several barriers to adequate and appropriate health care: • Financial barriers • Problems in satisfying eligibility requirements for health insurance • Transportation • Lack of sanitation, a stable place to store medicines • Inability to buy/get nutritious food

Enabling Characteristics • Federal Initiatives to Eliminate Socioeconomic disparities • Programs that have helped eliminate socioeconomic differences: -Community Health Center Program -National Health Service Corps -Public Housing Primary Care Program -Health Schools, Health Communities Program -Health Care for the Homeless Program

Need Characteristics • Mental Health • Chronic Illness/Disability • HIV/AIDS

Need Characteristics • Self-perceived or professionally-evaluated health status refers to: -self-perceived physical and mental health status and diagnoses of disease and illness from a health professional

Mental Health

Mental Health • Mental illness ranks second, after ischemic heart disease, as a burden on health and productivity • Mental illness is a risk factor for death from suicide, cardiovascular disease and cancer.

Mental Health • Most mental health services are provided in the general medicine sector, rather than through formal mental health specialist services • This is a concept first described by Regier and colleagues as the de facto mental health service system

Mental Health • The nation’s mental health system is composed of two subsystems: • One, primarily for individuals with insurance coverage or private funds and • The other for those without private means of coverage.

Chronic Illness/Disability

Chronic Illness/Disability • Chronic conditions are characterized by persistent and reoccurring health consequences lasting over a long period, which are generally irreversible • Chronic illness and disability pose unique challenges to a health car m m l; e system that is primarily oriented towards treating acute illness.
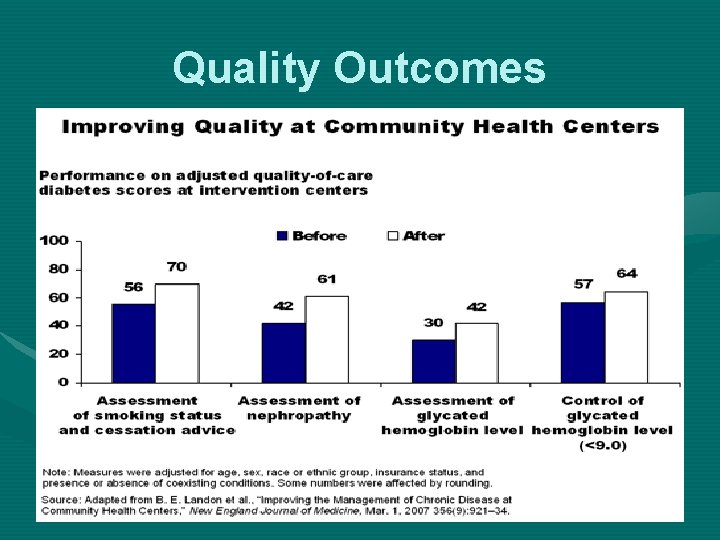
Quality Outcomes

References • Benson, K (2010). Winthrop University • King & Wheeler (2007). Medical Management of Vulnerable and Underserved Patients. Mc. Graw Hill.
- Slides: 43