Overview of Carcinoma Buccal Mucosa with Practical Experience

Overview of Carcinoma Buccal Mucosa with Practical Experience Dr Tanzina Hossain MD Thesis (3 rd part) NICRH
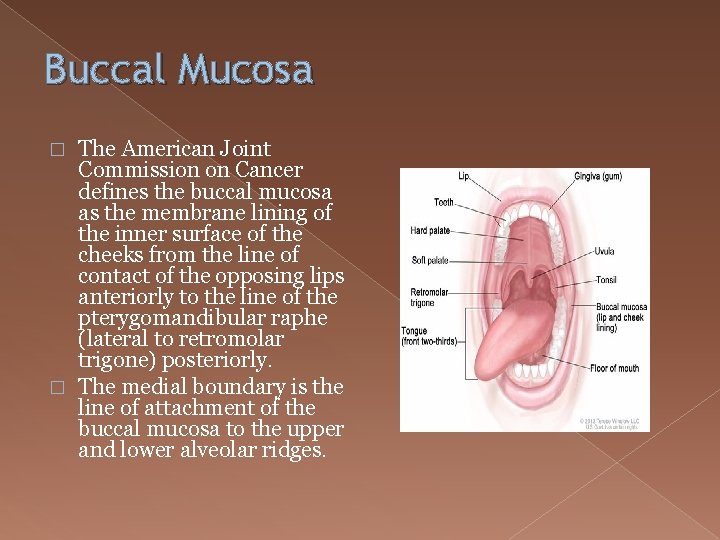
Buccal Mucosa The American Joint Commission on Cancer defines the buccal mucosa as the membrane lining of the inner surface of the cheeks from the line of contact of the opposing lips anteriorly to the line of the pterygomandibular raphe (lateral to retromolar trigone) posteriorly. � The medial boundary is the line of attachment of the buccal mucosa to the upper and lower alveolar ridges. �
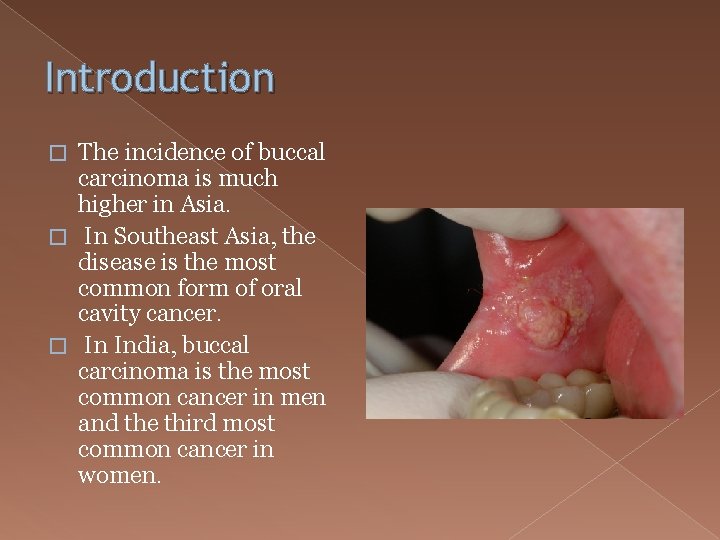
Introduction The incidence of buccal carcinoma is much higher in Asia. � In Southeast Asia, the disease is the most common form of oral cavity cancer. � In India, buccal carcinoma is the most common cancer in men and the third most common cancer in women. �

� Buccal carcinoma has the propensity to become aggressive, with high rates of locoregional recurrence. � Diagnosis and treatment at an early stage leads to significantly improved prognosis and function over advanced disease. � It occurs more often in men, with a male: female ratio of 3 -4: 1, � And most commonly in the 7 th or 8 th decade of life.

Squamous cell carcinoma is by far the most important and the most common malignant mucosal neoplasm of the head and neck accounting for over 90% of all malignancies. Conventional oral squamous cell carcinoma can present as several variants that include : � verrucous carcinoma , � adenoid/acantholytic/pseudoglandular SCC , � spindle cell/sarcomatoid carcinoma , � adenosquamous carcinoma , � basaloid SCC and � papillary SCC.

Etiology � Tobacco and alcohol use are the main etiologic agents associated with the development of buccal carcinoma.

Etiology � In Asia, betel nut is a significant etiologic agent, in addition to tobacco and alcohol. In India, over 90% of patients with buccal carcinoma have a history of using betel nut.

Etiology � Other suspected but not confirmed etiologic agents include human papilloma virus, poor oral hygiene, and chronic irritation. � Premalignant conditions include submucosal fibrosis and lichen planus.

Symptoms � � � No symptoms in the early stage White or red lump in the mouth that does not go away after two weeks A red, raised patch in the mouth that bleeds easily A lump or thickening in the mouth Pain increases when eating or drinking Soreness or a feeling that something is caught in the throat Difficulty chewing or swallowing Severe ear pain Difficulty moving the jaw or tongue Hoarseness Numbness of the tongue or other areas of the mouth Dentures fit poorly or become uncomfortable because the jaw is swollen

Morphological Types The lesion often has 1 of 3 morphologic types: 1)exophytic, 2) ulceroinfiltrative, or 3)verrucous. � The exophytic type is the most common, appearing as a papillary mass that becomes ulcerated when large. � The ulceroinfiltrative variety appears as an ulcer that penetrates deep into the underlying structures, with surrounding induration. � Verrucous carcinomas are uncommon variants of oral-cavity carcinomas; among these, the buccal mucosa is the most common site. These lesions appear as papillary masses, and keratinization gives them a whitish appearance.

Diagnosis � A detailed medical history is important to determine the patient's candidacy for surgery or radiation therapy. � The person often has a history of tobacco and alcohol use. � A history of previous malignancies of the upper aerodigestive tract should be ascertained.

� � � Comprehensive examination of the head and neck should be conducted with a focus on the oral cavity. Palpation is important to determine the depth of invasion. Mandibular or maxillary alveolar invasion should be noted on inspection and palpation. Dentition must also be assessed, especially if irradiation is part of the planned management. The larynx and hypopharynx should be assessed by means of examination with a mirror or flexible endoscopy to rule out a second primary tumor of the upper aerodigestive tract.

The ears should be examined in those patients with a history of otalgia because a lack of evidence of ear disease suggests referred pain due to malignancy. � The neck and parotid gland should be carefully examined for adenopathy. � Signs of advanced disease on physical examination include bleeding, skin ulceration, facial swelling, neck mass, trismus, facial numbness, and paralysis of the facial musculature. �

Diagnostic workup Evaluation of a patient presenting with a lesion in the Buccal Mucosa should be aimed at pathological confirmation and staging of the disease Essential: 1. History and physical examination 2. Biopsy of the primary lesion 3. Complete Blood counts, Renal Function Tests including Creatinine clearance & Liver Function Tests. 4. Chest X-Ray 5. Ultra Sonogram of the neck in patients with no clinically enlarged neck nodes. 6. Dental evaluation 7. CT scan except in patients with early lesions and clinically and USG proven N 0 neck �

� Ideal 1. Ortho Pantomogram (OPG) or plain radiograph of mandible if the lesion extends to lower GB sulcus or lower alveolus. 2. CT Scan / MRI 3. PET-CT where indicated 4. Evaluation under anesthesia when clinical examination is not feasible. 5. Human Papilloma Virus (HPV)

Once a malignant diagnosis is established, treatment options include 1)surgery, 2)irradiation or 3) combined-modality therapy. Treatment recommendations should be based upon multiple factors, including the stage of the tumor, the patient's general health, and patient desires. �

Staging Buccal carcinoma is staged using the American Joint Commission on Cancer (AJCC) Staging System for the oral cavity. Primary tumor (T) � Tx - Primary tumor cannot be assessed � T 0 - No evidence of primary tumor � Tis - Carcinoma in situ � T 1 - Tumor no larger than 2 cm in greatest dimension � T 2 – Tumor larger than 2 cm but smaller than 4 cm in greatest dimension � T 3 - Tumor larger than 4 cm in greatest dimension � T 4 a - Tumor invading adjacent structures (eg, through cortical bone, into the deep [extrinsic] muscles of the tongue, maxillary sinus, or skin of the face) � T 4 b - Tumor invades masticator space, pterygoid plates, or skull base and/or encases internal carotid artery

Regional lymph nodes NX - Regional lymph nodes cannot be assessed � N 0 - No regional lymph node metastasis � N 1 - Metastasis in a single ipsilateral lymph node, 3 cm or less in greatest dimension � N 2 a - Metastasis in a single ipsilateral lymph node larger than 3 cm but smaller than 6 cm in greatest dimension � N 2 b - Metastases in multiple ipsilateral lymph nodes, none larger than 6 cm in greatest dimension � N 2 c - Metastases in bilateral or contralateral lymph nodes, none larger than 6 cm in greatest dimension � N 3 - Metastases in a lymph node larger than 6 cm in greatest dimension Distant metastases › MX - Distant metastasis not assessable › M 0 - No distant metastasis › M 1 - Distant metastasis

Stages are defined as follows: � Stage 0 - Tis N 0 M 0 � Stage 1 - T 1 N 0 M 0 � Stage 2 - T 2 N 0 M 0 � Stage 3 - T 3 N 0 M 0; T 1, T 2, or T 3 N 1 M 0 � Stage 4 a - T 4 a N 0 M 0; T 4 a N 1 M 0; T 1, T 2, T 3 or T 4 a N 2 M 0 � Stage 4 b – Any T N 3 M 0; T 4 b any N M 0 � Stage 4 c - Any T any N M 1

Treatment � The aim of treatment is “curative” for patients with Stage I to IVA and � “palliative” for patients with Stage IVB (locoregionally advanced disease), & IV C (metastatic disease)

Early Stage (Stage I and II) Disease Options: (Both Essential) � (i) Surgery (adjuvant treatment to be decided after histopathology report) � (ii) Radical Radiotherapy (a) Brachytherapy (b) External Beam Radiotherapy (EBRT)+/- Brachytherapy boost

Indications for adjuvant treatment • Margin status: All patients with close/ positive margin should be considered for re-excision. If not a candidate for the same, PORT should be considered. • Nodal status: Multiple nodes positive disease requires post operative treatment (CT+RT) as for stage IV A disease. In single node positive disease (Stage III) the role of RT is controversial. • Extra capsular spread: Post operative chemoradiation should be given.

Chemotherapy in chemoradiation: • Cisplatin is the preferred agent. • Weekly cisplatin 30 mg/m 2 is practiced at many centers. • In three weekly regimen, the dose of cisplatin recommended is 100 mg/m 2 every three weekly i. e on day 1, 22, and 43 of radiotherapy. • Monoclonal antibody therapy directed against EGFR (cetuximab and nimotuzumab) added to radiation therapy improves outcome • In patients who are not candidates for cisplatin, carboplatin and paclitaxel is the regime of choice for chemoradiation. • Feeding through nasogastric tube, gastrostomy or jejunostomy is strongly recommended during chemoradiation
Locally Advanced (Stage III & IV A) Disease: (T 3, T 4 a or any node positive (except N 3) disease). Such patients should always be offered radical combined modality treatment. Options (All Essential) � (i) Surgery ----- RT+/-CT � (ii) CT+RT � (iii) Induction chemotherapy + surgery + RT

� Advanced Stage IV B & IV C : • Intention of treatment is only palliation with maintenance of quality of life. Options � (i) Radiotherapy (ii) Chemotherapy

Radiotherapy � If patient is symptomatic +/- nodal , consider palliative EBRT. Chemotherapy � Systemic disease or progressive local disease after RT could be treated with chemotherapy. Agents Used: 1. Single agent Methotrexate 2. Single agent Cisplatin 3. cisplatin+ 5 -Flurouracil 4. Cisplatin + Docetaxel 5. Cisplatin + Paclitaxel 6. Cisplatin + Cetuximab

Principles of treatment of recurrent disease: � If recurrence is small, revision surgery or radiotherapy are the treatment options. • If recurrence is operable and patient is radiotherapy naïve : Surgery + PORT ± chemotherapy or Radical radiotherapy alone (lesion is r. T 1 N 0 or r. T 2 N 0) • If surgery is not medically feasible or patient is not willing, radiotherapy naïve and good performance status: Concurrent CT+RT or radiotherapy alone to be considered.
If surgery is not feasible, and poor performance status the treatment should be individualized employing appropriate measures such as: • If Radiotherapy naïve: Palliative radiotherapy - 30 Gy/10 Fr or weekly RT 7 -8 Gy/2 -3 fr. • Palliative chemotherapy (as for stage IV B & IV C disease) • Best supportive care

Study on Polychemotherapy in squamous cell carcinoma of the buccal mucosa Thirty-nine patients with previously untreated squamous cell carcinoma of the buccal mucosa were treated by two polychemotherapeutic regimens. � The first regimen consisted of bleomycin and methotrexate (BLM-MTX): bleomycin 30 mg was given intravenously twice weekly, and methotrexate 25 mg intravenously twice weekly for 2 1/2 and two weeks, respectively. � The second program consisted of Cytoxan (cyclophosphamide), methotrexate and 5 -FU (CMF): methotrexate 25 mg twice weekly for two weeks, Cytoxan 100 mg/day for two weeks, and 5 -FU 500 mg twice weekly for 1 1/2 weeks. � All of the patients were evaluated one week after completion of their chemotherapy regimen. They matched in age and extent of disease. �

� High response rates (88. 9%) were noted with the BLM-MTX combination, which is comparable to the best responses reported previously using cisplatinum, vincristine, and methotrexate. This may suggest that buccal cancers are highly sensitive to an initial treatment by BLM-MTX, and therefore the authors highly recommend its use as preoperative adjuvant therapy in patients who present with Stage III and IV (Mo) disease.

Case Scenario A 48 year old female patient reported with a chief complain of pain in the left side of mouth since 7 days. The patient has H/O dental procedure 1 year back. 1 month later Patient noticed a small, painless growth over the left buccal mucosa , which gradually grew to the present size. Patient developed pain 3 months back which was initially mild and intermittent but has aggravated since 7 days.

On local examination, on inspection - intraorally there was presence of solitary proliferative growth over the left buccal mucosa. � The lesion was approximately 7 x 5 cm in size, well defined with irregular margins. Surface of the lesion was irregular at the periphery with finger like projections in the centre. Color of the lesion varied from pink in periphery to frank white in the centre. � On palpation, size, site, surface, shape were confirmed. Lesion was tender and elevated from adjacent mucosa with irregular and firm margins �

� The patient was diagnosed as a case of squamous cell cancer of buccal mucosa. She was treated with 4 cycles of paclitaxel, CPL, 5 FU but no improvement was noted. Then changed schedule with weekly MTX and Bleomycin 6 cycles were given and the patient was responding well.
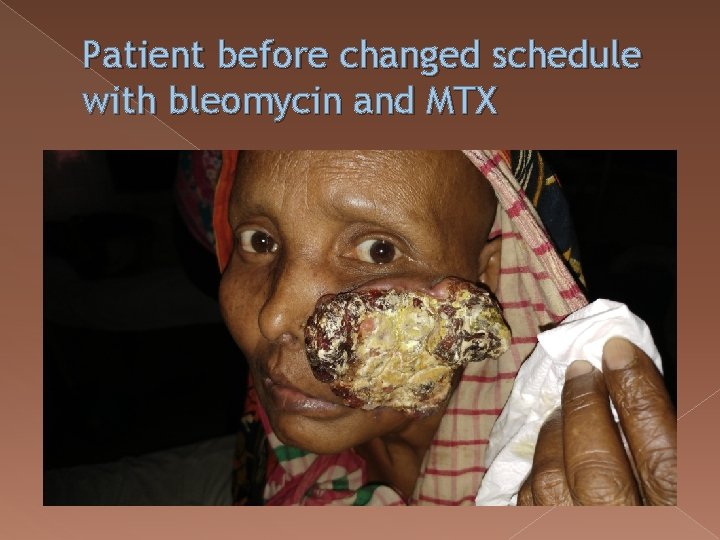
Patient before changed schedule with bleomycin and MTX
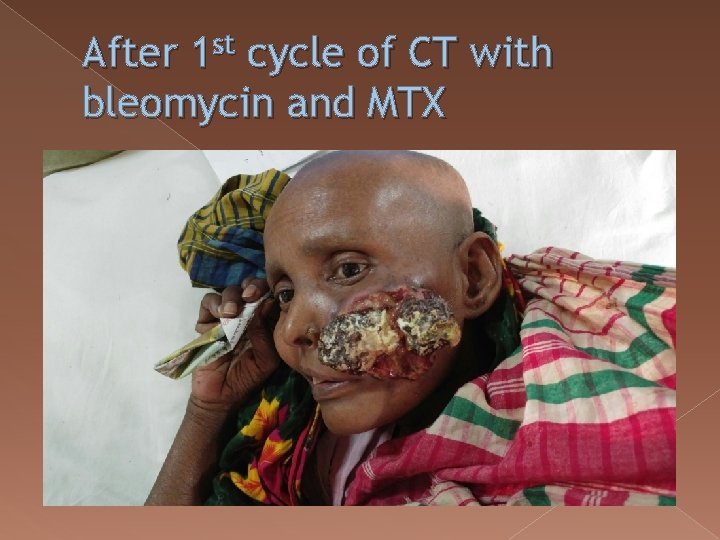
After 1 st cycle of CT with bleomycin and MTX
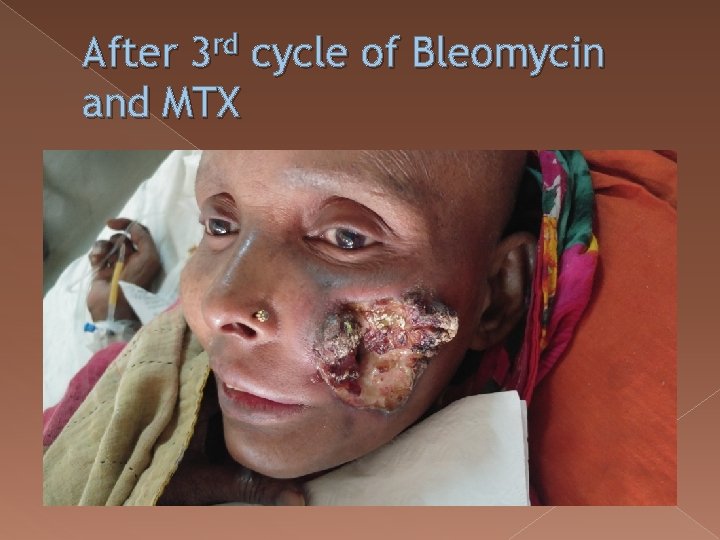
After 3 rd cycle of Bleomycin and MTX
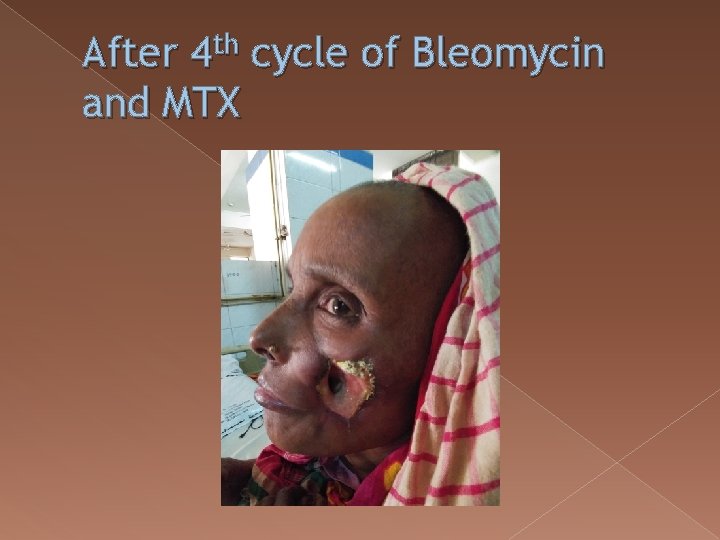
After 4 th cycle of Bleomycin and MTX

After 6 th cycle of Bleomycin and MTX

� After completing 6 th cycle of chemotheray overall condition of the patient was improved. Afterwards patient was referred to Plastic surgery department for reconstruction.

- Slides: 40