Overview n n The complement system is part








- Slides: 14

Overview n n The complement system is part of the innate immune system (vs adaptive) It is named “complement system” because it was first identified as a heat-labile component of serum that “complemented” antibodies in the killing of bacteria n It is now known that it consists of over 30 proteins.

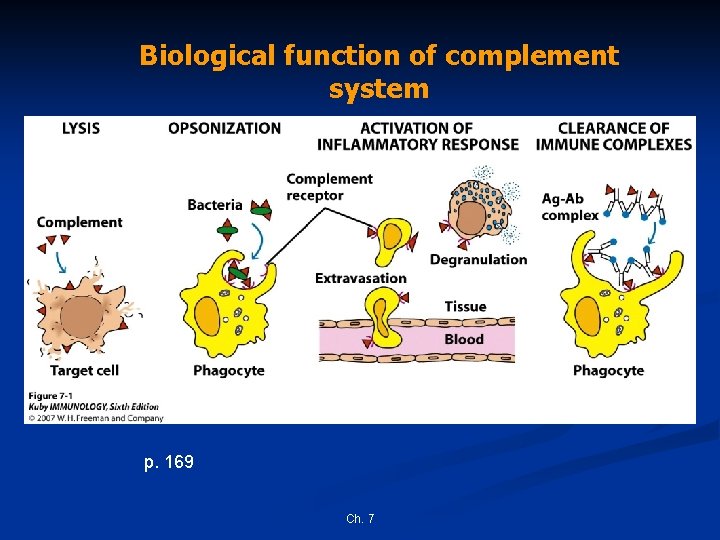
Biological function of complement system p. 169 Ch. 7

“Classical” Pathway n n n Begins with antibody binding to a cell surface and ends with the lysis of the cell The proteins in this pathway are named C 1 -C 9 When complement is activated it is split into two parts – a – smaller part – B – larger part and usually the active part (except with factor 2)

“Classical Pathway” n ACTIVATION – C 1 q portion of C 1 attaches to the Fc portion of an antibody – Only Ig. G and Ig. M can activate complement – Once activated C 1 s is eventually cleaved which activates C 4 and C 2 – C 4 b & C 2 a come together to form the C 4 b 2 a which is the C 3 convertase – C 3 convertase activates C 3 to C 3 a and C 3 b

“Classical Pathway” n ACTIVATION – C 3 a binds to receptors on basophils and mast cells triggering them to release there vasoactive compounds (enhances vasodilation and vasopermeability) – C 3 a is called an anaphylatoxin – C 3 b serves as an opsonin which facilitates immune complex clearance – C 3 b binds to C 4 b. C 2 a to form the C 5 convertase C 4 b. C 2 a. C 3 b – C 5 convertase cleaves C 5 leading to the formation of the Membrane attack Complex (C 5 -C 6 -C 7 -C 8 -C 9) – The MAC “punches holes” in cell walls resulting in lysis

C 5 a is a: C 2 C 4 C 1 q C 3 1. Potent anaphylatoxin 2. Chemoattractant for neutrophils 2 a 4 a 2 b 4 b C 3 a binds to receptors on basophils and mast cells triggering them to release there vasoactive compounds (enhances vasodilation and vasopermeability) ANAPHYLATOXIN C 3 a C 3 b C 5 b. C 5 a C 3 -convertase C 5 -Convertase C 7 C 9 Classical Pathway C 8 C 6

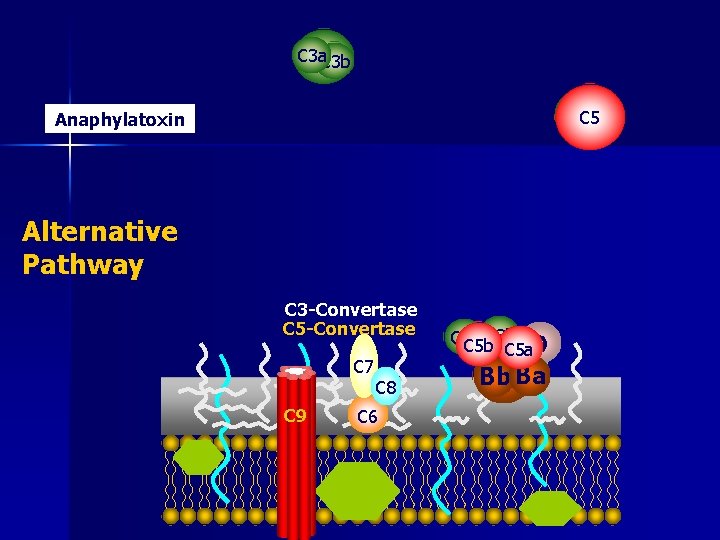
“Alternative Pathway” n Requires no specific recognition of antigen in order to cause activation n ACTIVATION – Spontaneous conversion from C 3 to C 3 b occurs in body – Normally, C 3 b is very short lived and quickly inactivated by proteins on the surface of the body’s own cell walls (DAF) – However, bacteria or other foreign material may lack these surface proteins allowing C 3 b to bind and stay active

“Alternative Pathway” – Factor B binds to C 3 b – Factor B is then cleaved by factor D into Ba and Bb – C 3 b. Bb remains which acts as a C 3 convertase (C 3 C 3 a and C 3 b) – C 3 b. Bb. C 3 b is formed which acts as a C 5 convertase – C 5 is cleaved to C 5 a and C 5 b – C 5 b then starts the assembly of the Membrane Attack Complex

C 3 a C 3 b C 3 C 5 Anaphylatoxin Alternative Pathway C 3 -Convertase C 5 -Convertase C 7 C 9 C 8 C 6 C 3 b C 3 a C 5 b C 5 a. D Bb B Ba

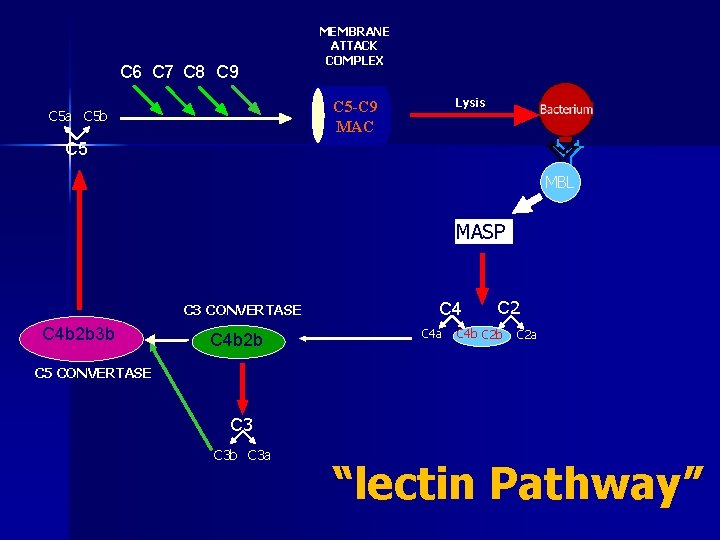
C 6 C 7 C 8 C 9 MEMBRANE ATTACK COMPLEX Lysis C 5 -C 9 MAC C 5 a C 5 b C 5 MBL MASP C 3 CONVERTASE C 4 b 2 b 3 b C 4 b 2 b C 4 a C 2 C 4 b C 2 a C 5 CONVERTASE C 3 b C 3 a “lectin Pathway”

Complement Regulation n n C 1 inhibitor (C 1 INH) bind to and inactivate the serine protease activity of C 1 r, and C 1 s Factor I cleave C 3 b and C 4 b thereby reducing amount of C 5 convertase available Factor H enhance activity of factor I on C 3 b As spontaneously produced C 3 b binds to autologous host membranes it interacts with DAF (decay accelerating factor), a membrane bound protein which can act to accelerate dissociation of C 3 convertase of both pathways.

Summary - Activation n Complement can be activated by the binding of antibody (Classical) or by the adherance of C 3 b to foreign material (Alternative) The two pathways converge at the formation of the C 5 convertase (C 4 b 2 a 3 b or C 3 b. Bb. C 3 b) The final common pathway is the formation of the membrane attack complex

Summary - Function Opsonization – C 3 b n Chemotaxis – C 5 a (attracts neutrophils) n Increases vasodilation & permeability of capillary beds via mast cell and basophil activation – C 3 a & C 5 a (Anaphylatoxins) n Cellular Lysis via the MAC n

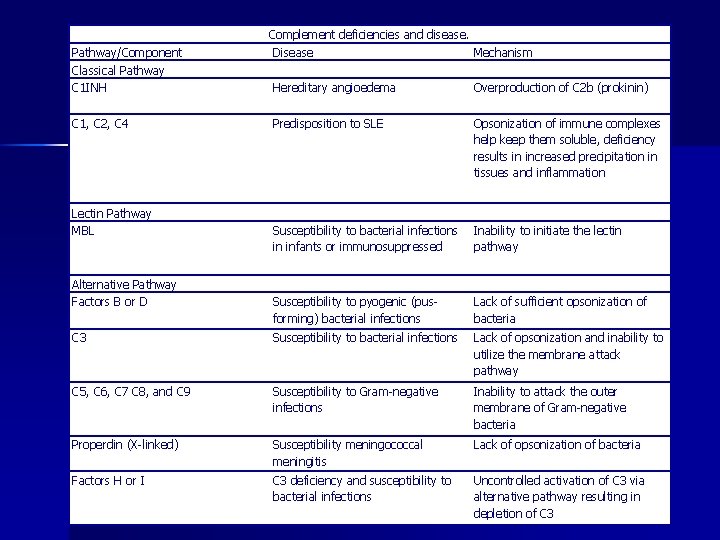
Pathway/Component Classical Pathway C 1 INH Complement deficiencies and disease. Disease Mechanism Hereditary angioedema Overproduction of C 2 b (prokinin) Predisposition to SLE Opsonization of immune complexes help keep them soluble, deficiency results in increased precipitation in tissues and inflammation Susceptibility to bacterial infections in infants or immunosuppressed Inability to initiate the lectin pathway Susceptibility to pyogenic (pusforming) bacterial infections Lack of sufficient opsonization of bacteria C 3 Susceptibility to bacterial infections Lack of opsonization and inability to utilize the membrane attack pathway C 5, C 6, C 7 C 8, and C 9 Susceptibility to Gram-negative infections Inability to attack the outer membrane of Gram-negative bacteria Properdin (X-linked) Susceptibility meningococcal meningitis Lack of opsonization of bacteria Factors H or I C 3 deficiency and susceptibility to bacterial infections Uncontrolled activation of C 3 via alternative pathway resulting in depletion of C 3 C 1, C 2, C 4 Lectin Pathway MBL Alternative Pathway Factors B or D