Overview Digestion process of breaking down food into

Overview • Digestion- process of breaking down food into molecules small enough for cells • Absorption-passage of these molecules through the plasma membrane of the stomach and small intestine into the blood and lymph

Medical terminology Gastroenterology- the specialty dealing with the stomach and intestine Proctology- specialty dealing with the rectum and anus

Digestive process • • Ingestion-taking in food into the mouth Mixing/movement-muscles and secretions Mechanical Digestion- chew, peristalsis Chemical Digestion-break down carbs, lipids, and proteins • Absorption-see above • Defecation-elimination of indigestible substances
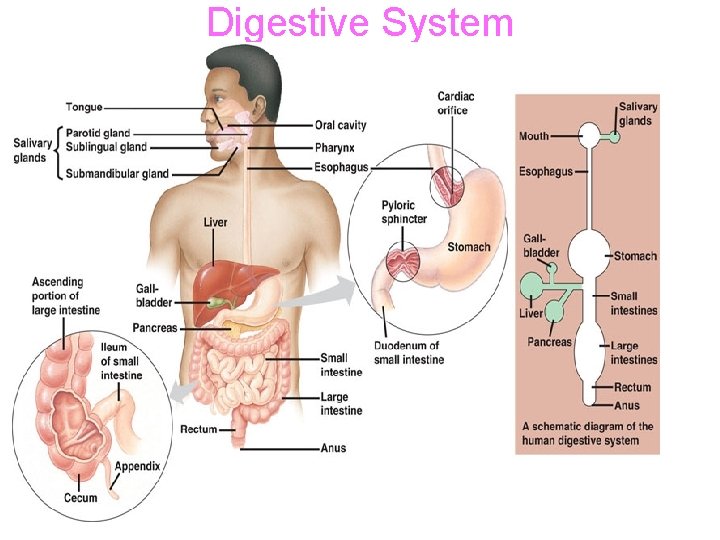
Digestive System
Alimentary Canal Mouth Pharynx Cardiac Sphincter Pyloric Sphincter Jejunum Ileum Ascending Colon Descending Colon Esophagus Stomach Duodenum Ileocecal Valve Transverse Colon Rectum Anus

General Histology • • • GI Tract has 4 layers Mucosa Subcosa Muscularis Serosa and Peritoneum

MUCOSA • Made of : epithelial---areolar---thin layer of smooth muscle (muscularis mucosae) • Epithelium: Mouth, pharynx, esophagus, and anal canal is mostly nonkeratinized stratified squamous for protection. Stomach and Intestines has simple columnar for secretion and absorption. Last 5 -7 days.

AREOLAR • Lamina Propria: Areolar tissue containing many blood and lymph vessels. • Binds the layers. Contains Mucosa Associated Lymphatic Tissue (MALT): lymph nodules that hold immune system cells, especially in the tonsils, intestines and appendix. • MALT: Mucosa Associated Lymphatic Tissue

MUSCULARIS MUCOSAE • Throws the mucous membrane of the stomach and small intestine into many folds to increase surface area.

SUBMUCOSA • Composed of areolar tissue that binds mucosa to the muscularis. • Contains the submucosal plexus or plexus of Meissner, an extensive network of neurons. Part of the Enteric Nervous System or ENS. The brains of the gut.

MUSCULARIS • Thick muscle layer • Voluntary/skeletal in the mouth, pharynx, and upper esophagus • Involuntary/smooth in the rest if the GI tract. • Inner is circular muscle • Outer is longitudinal muscle • Contains the mysenteric plexus or plexus of Auerbach which controls motility.

SEROSA • Simple squamous and connective tissue • Secretes serous fluid that allows the tract to glide against other organs. • Parietal peritoneum lines the wall of the abdominal cavity. • Visceral peritoneum covers the organs on the cavity. • Mesentery is fan shaped and binds the sm. intestine to the posterial abdominal wall. • Falciform ligament attaches the liver to to the anterior abdominal wall. • Greater omentum the largest peritoneal fold, drapes over the transverse colon. “fatty apron”.

Oral or Buccal Cavity • Formed by the cheeks, hard and soft palate, and tongue • Cheeks or bucca form the lateral wall, made of nonkeratinized stratified squamous • Lips or labia (fleshy borders) • Orbicularis oris muscle- between the skin and the mucous membrane in the lips keeps food in the right place while chewing

Salivary Glands • Any cell or organ that releases a secretion called saliva into the oral cavity. • Mucous membrane of the mouth and tongue have many small salivary glands ie… labial, buccal, palatal, and lingual. • Most saliva comes from the major salivary glands.

3 Major Salivary Glands • Parotid- inferior and anterior to the ear, between the skin and masseter. • Submandibular- beneath the base of the tongue. • Sublingual- superior to the submandibular gland.
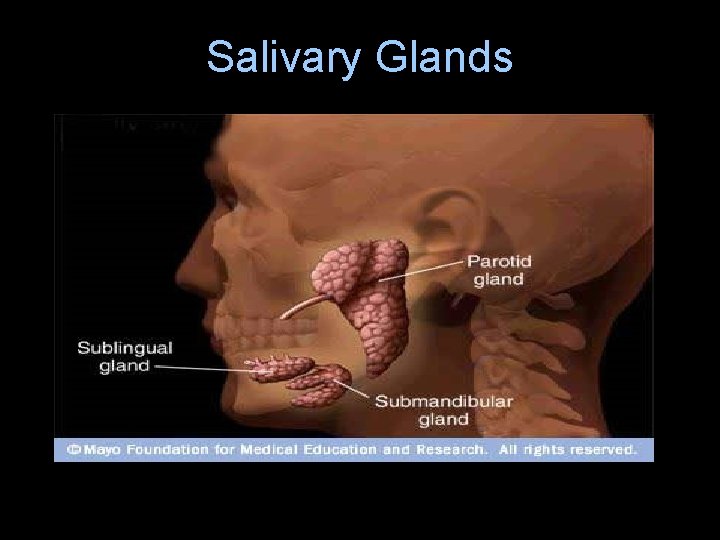
Salivary Glands

Saliva 1. Saliva is 99. 5% water and. 05% solutes 2. Solutes are ions. Dissolved gasses, and organic substances. a. urea and uric acid b. immunoglobulin A ( bacteria killing enzyme ) c. salivary amylase ( enzyme that acts on starch )
Salivation • Controlled by the autonomic nervous system • The Parasympathetic Facial nerve (VII) and Glossopharyngeal nerve (IX) promotes continuous secretion • The Sympathetic nerves during stress will turn this secretion off. • Can be stimulated by smell, sight, sound, or thought of food. • Daily 1000 -1500 m. L/day= 1 -1. 6 quarts

Tongue • An Accessory organ • lingual frenulum is a fold in the mucous membrane in the midline of the undersurface. • Ankyloglossia- “tongue tied” frenulum is too short. • Papillae- most contain taste buds, some contain receptors for touch. • Lingual lipase- enzyme for tryglycerides.

Teeth or Dentes • Accesory digestive organs located in the sockets of the alveolar processes of the mandible and maxillae. • Gingivae or gums cover these processes. • Periodontal ligament- dense fibrous connective tissue keeps teeth in position and serves a shock absorber.

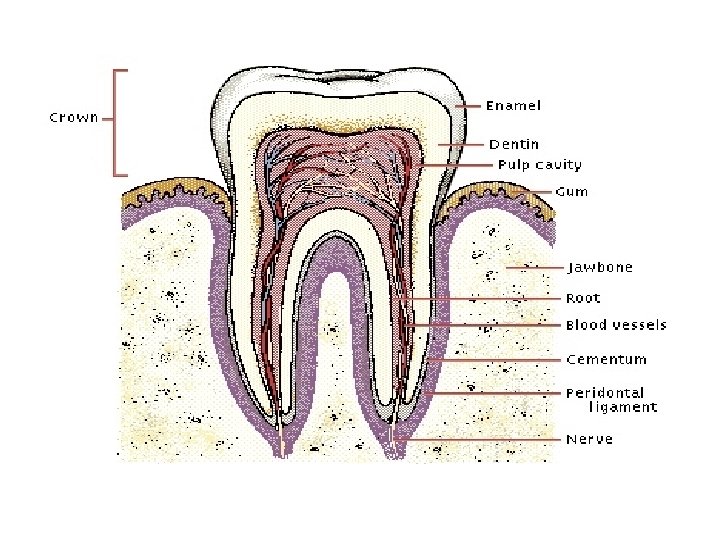
3 basic parts of a tooth 1. Crown- exposed portion. 2. Root- one to three projections inbedded in the socket. 3. Neck- the junction line between the crown and the root.
Tooth composition and design • Dentin-calcified connective tissue. Harder than bone due to more calcium salts. • Pulp cavity- lies within the crown filled with pulpconnective tissue containing blood vessels , nerves, and lymphatic vessels. • Root canals- narrow extensions of the pulp cavity. • Apical foramen- opening at the base of the root canal for vessels. • Enamel- hardest substance in the body, calcium phosphate and calcium carbonate. • Cementum- bonelike substance that covers the root, and attaches it to the peiodontal ligament.

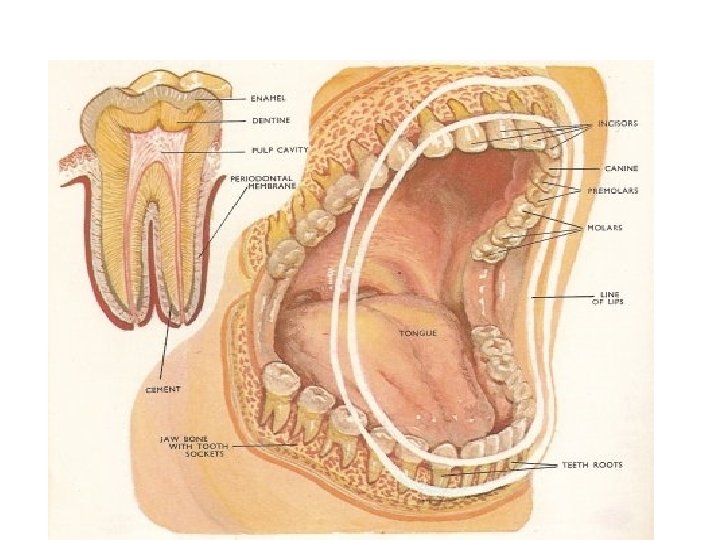
Types of Teeth • Deciduous- baby teeth, 20 total • Permanent teeth, 32 totoal – 16 on top, 16 on bottom – 8 incisors – 4 cuspids – 8 premolars – 12 molars

Deglutition • • Swallowing from mouth to stomach 3 stages 1. Voluntary 2. Pharyngeal 3. Esophageal- peristalsis controlled by the medulla oblongota Epiglottis closes pharynx and vocal cords for about 1 -2 seconds while swallowing
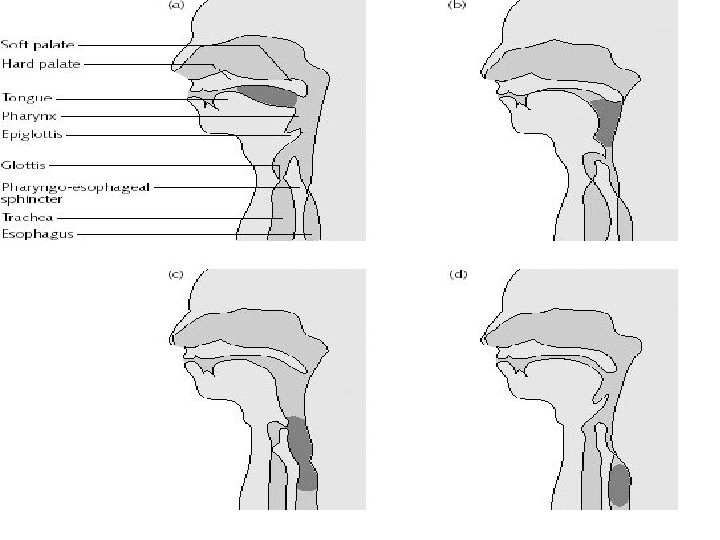

Esophagus • Collapsible tube • 25 cm or 10 inches in length • Connects the inferior laryngopharynx to the stomach • No absorption or secretion of enzymes • Passes thru the esophageal hiatus (opening in the diaphragm)

Stomach • Connects the esophagus to the duodenum • 5 major functions: 1. Mixes saliva, food, and gastric juice(20003000 m. L/DAY) to form chyme. 2. Reservoir for the small intestine. 3. Secretes gastric juice which contains HCl, pepsin, intrinsic factor, and gastric lipase. 4. HCl kills bacteria and denatures protein, pepsin begins to digest proteins, intrinsic factor aids in absorption of vitamin B-12, gastric lipase aids in digesting triglycerides. 5. Secretes gastrin into blood.
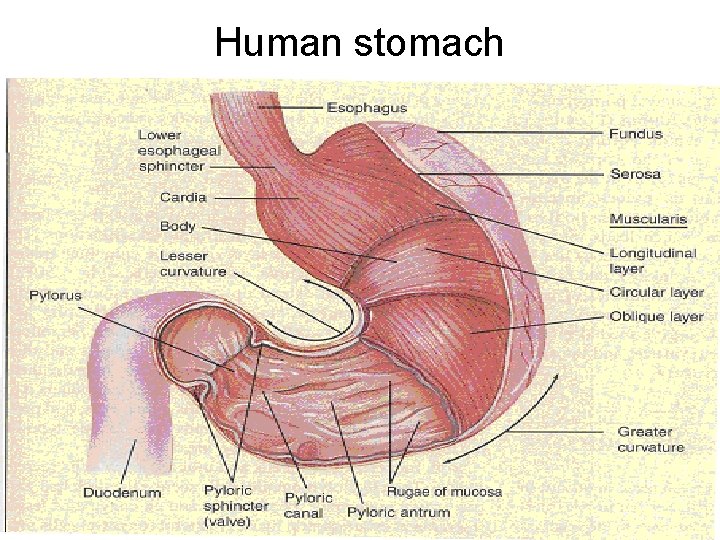
Human stomach
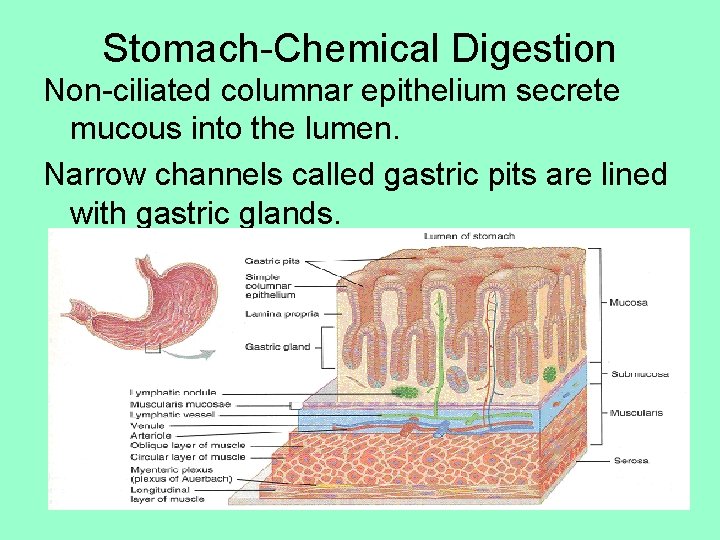
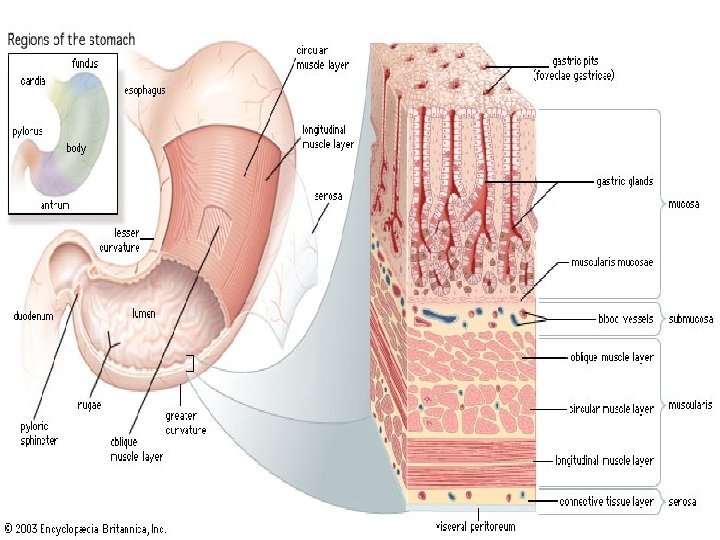
Stomach-Chemical Digestion Non-ciliated columnar epithelium secrete mucous into the lumen. Narrow channels called gastric pits are lined with gastric glands.

3 types of exocrine cells • Mucous neck cells- secrete mucous • Chief cells- secrete pepsinogen • Parietal cells- secrete HCl which converts pepsinogen into pepsin, and secretes intrinsic factor • The secretions of these 3 types of cells make up the gastric juice. • G cells- also secrete a hormone gastrin into the bloodstream, which increases motility, production of gastric juice, and relaxes the pyloric sphincter.

Stomach Physiology-Mechanical Digestion • Rugae-visible folds in the mucosa • Mixing waves pass over the stomach every 15 -25 seconds. • Macerates the food and adds it to gastric juice forming chyme. • Each wave forces 10 -15 Ml of chyme into the duodenum thru alomost completely closed pyloric sphincter.

Regulation • Stimulation from parasympathetic nervous system. Impulses from the medulla oblongata via the vagus nerves (X). • Inhibition. Sympathetic nervous system. by: food in small intestine negative emotions Hormones GIP Gastric Inhibitory Peptide – stops gastric secretions and mobility. Secretin- decreases gastric secretions. Cholecystokinin or CCK – inhibits gastric emptying. Absorption- water, electrolytes, drugs like aspirin, and alcohol

Pancreas • About 12 -15 cm (6 inches) in length. • 3 portions- head, body, and tail • Made up of 2 types of cells: 1. Pancreatic islets (islets of Langerhans)- endocrine glands which produce insulin and glucagon. About 1% 2. Acini- exocrine glands which secrete pancreatic juice. About 99% Pancreatic duct or duct of Wirsung combines with common bile duct and enters the duodenum at the hepatopancreatic ampulla or (ampulla of Vater)
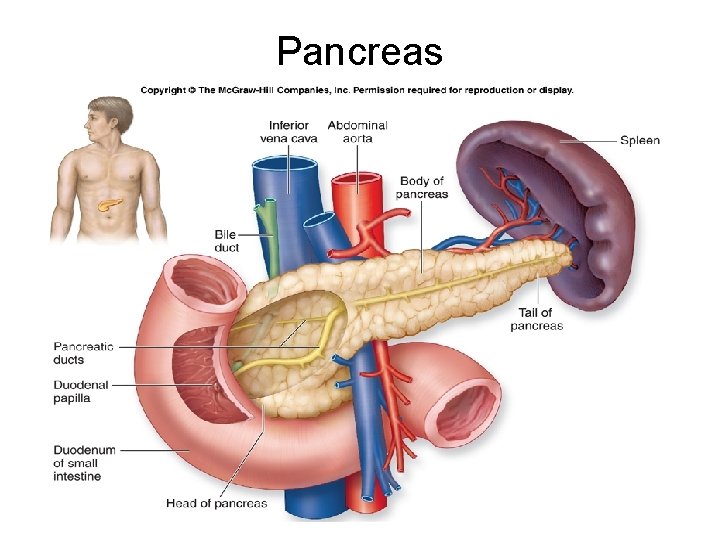
Pancreas

Pancreatic Juice • Mostly water, salt, sodium bicarbonate (alkaline), and enzymes. • Enzymes: Pancreatic amylase-carbs Trypsin, chymotrypsin, and carboxypeptidaseproteins. Pancreatic Lipase-triglycerides Ribonuclease, and Deoxyribonuclease- nucleic acids

Pancreas Regulation • Just like the stomach: Nervous system- parasympathetic vagus (x) Hormones- secretin, and cholecystokinin
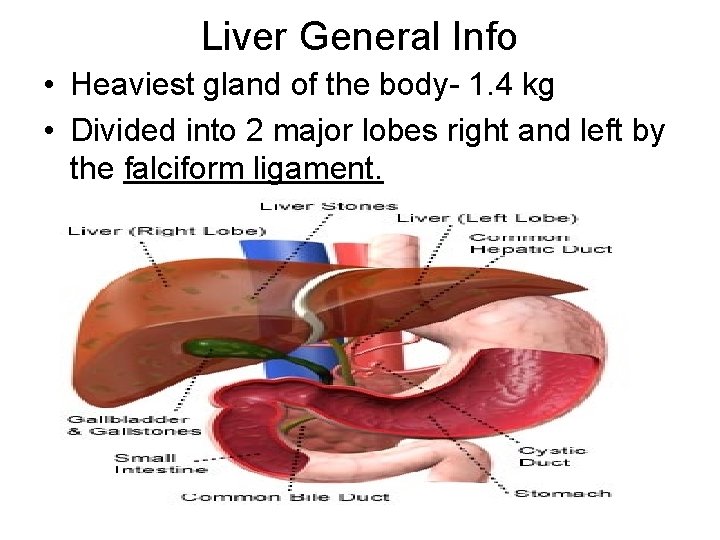
Liver General Info • Heaviest gland of the body- 1. 4 kg • Divided into 2 major lobes right and left by the falciform ligament.
Liver lobules • Hepatocytes-bile producing cells around a central vein. • Sinusoids-large capillaries • Stellate reticuloendothelial or Kupffer’s cellsphagocytic cells that destroy worn out blood cells , bacteria, and toxins. • Rt+Lt hepatic duct merge into and leave the liver as the common hepatic duct. • Common hepatic joins the cystic duct from the Gall Bladder to form the common bile duct
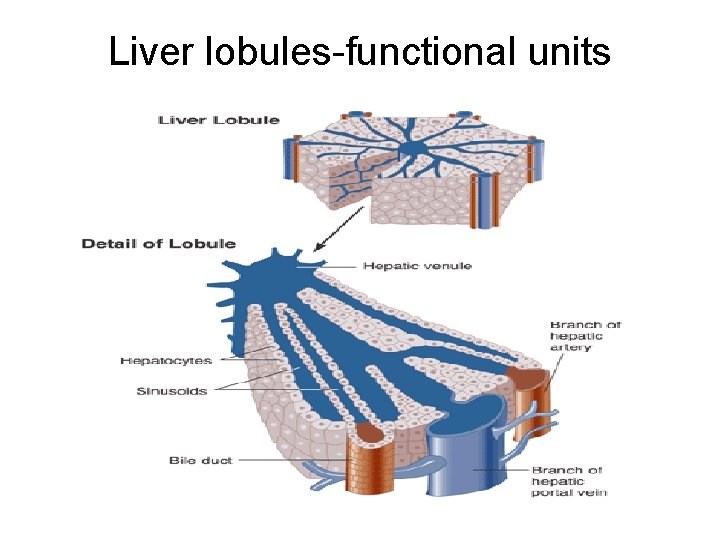
Liver lobules-functional units
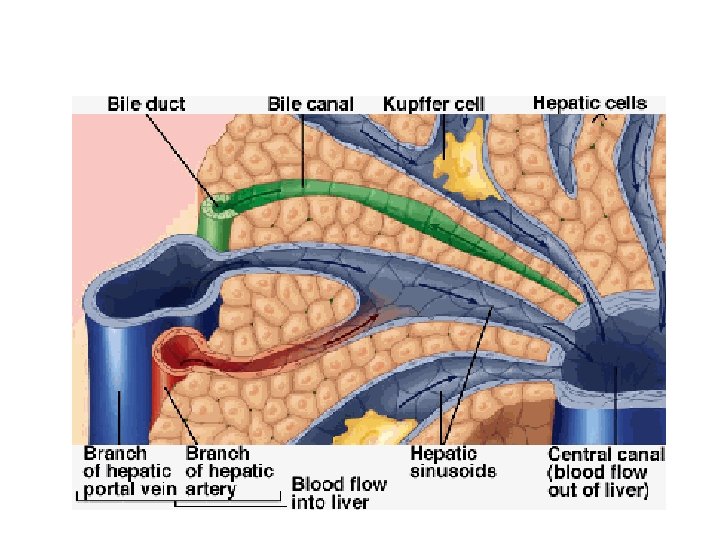

Bile • Ph of 7. 6 -8. 6 • Secreted by hepatocytes but stored in the gall bladder • Emulsifies triglycerides which increases the surface area for enzymes like lipase that digest them • Pigment-bilirubin • Parasymathetic vagus(x) increase secretion. • Secretin stimulates secretion. • CCK causes ejection from the gall bladder.
Liver Function • • • Carb + Lipid + Protein metabolism Removal of drugs and hormones (detoxify) Excretion of bile Synthesis of bile salts Storage of glycogen, vitamins, and minerals • Phagocytosis-function of Kupffer’s cells • Activation of vitamin D

Gall Bladder • • Galla –bile Found under the liver Function-concentrate and store bile When triglycerides enter the small intestine CCK stimulates muscle contraction in the Gall Bladder and bile is emptied into the common bile duct to flow into the small intestine.
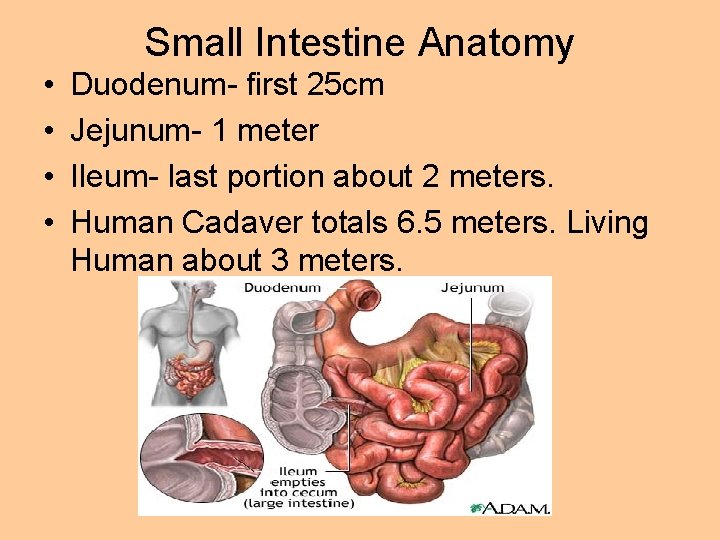
Small Intestine Anatomy • • Duodenum- first 25 cm Jejunum- 1 meter Ileum- last portion about 2 meters. Human Cadaver totals 6. 5 meters. Living Human about 3 meters.

Small Intestine- Anatomy Cont. • Villi- Projections of the mucosa to increase surface area for absorption. • Lacteal- Lymphatic capillary • Epithelium- Mostly simple columnar containing: 1. absorptive cells with microvilli, 2. goblet cells-secrete mucus 3. hormone producing cellssecretin, CCK, gastric inhibitory peptide 4. Paneth cells-secrete lysozyme

Mechanical Digestion • Segmentation- moves chyme back and forth without advancing it thru the lumen of the sm. intestine. • Peristalsis- propels the chyme thru the intestine. • Both are stimulated by the parasymathetic nervous system • It takes about 4 hours for a meal to get to arrive at the large intestine

Chemical Digestion • Intestinal enzymes include: Maltase, sucrase, and lactase for carbs. Peptidase which completes protein digestion. Nucleases for nucleic acid digestion.

Absorption • 90% takes place in the small intestine. • Thru diffusion, osmosis, facilitated diffusion, and active transport. • Misc: LDL or low density lipoproteins are the considered the “bad” cholesterol, because it can contribute to Atherosclerosis. • HDL or high density cholesterol is considered “good” cholesterol because it takes cholesterol away from the arterial walls. • Below 200 mg/dl total blood cholesterol is recommended

Absorption cont. • Of the over 9 liters of fluid that enters the small intestine almost all is absorbed thru osmosis. • Most electrolytes are absorbed thru active transport. • Fat soluble vitamins (A, D, E. and K) are absorbed with dietary triglycerides. • Most water soluble vitamins like B’s and C’s diffuse. • B 12 needs intrinsic factor present to be absorbed thru active transport.
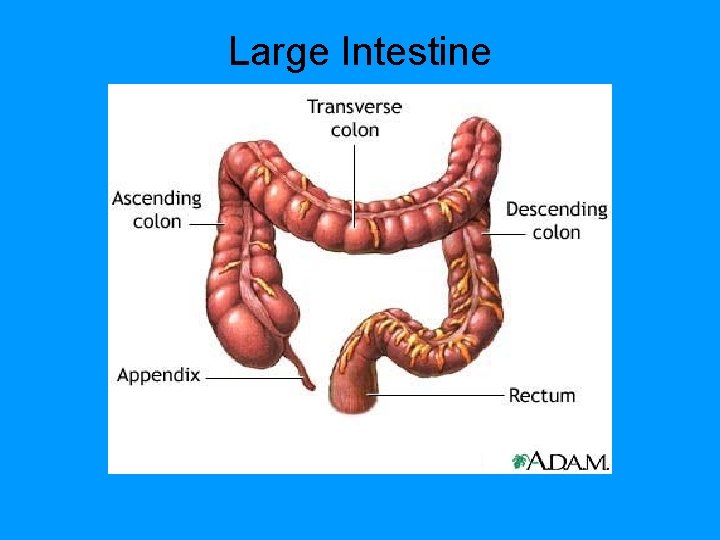
Large Intestine

Large Intestine • Haustra-pouches in the large int. • Ileocecal sphincter regultes movement of chyme from the sm-large intestine. After a meal this increases. • Haustral Churning- chambers in the l. int relax and fill, when they become distended the squeeze the contents to the next haustra • Peristalsis-slower than the rest of the track. • Mass Peristalsis- starts at the transverse colon and drives the colonic contents into the rectum. Increases right after a meal.

Large Intestine Chemical digestion • • • 3 -10 hours in the large intestine. After this time it is called feces. 40% Bacteria Absorption of vitamin K, and B. water. Defecation-emptying of feces via the anus.







- Slides: 63