Overtraining Syndrome Dr Isstelle Joubert 2 nd year

Overtraining Syndrome Dr Isstelle Joubert 2 nd year M Sports Medicine 2012

Patient History. . . v 15 yo blonde girl v 3 week history of being tired (Nov 2011) v poor sport performance v Level of participation: § youngest in school’s u/19 netball team § chosen to go to Mauritius in April 2012 v Academically: top 3 in her class

Patient History. . . Presenting Sx: v tired v poor sport performance v mood swings

Patient History. . . Other history: v No menarche v Exercise programme v Sleep pattern v Diet v Drugs / supplements

Exercise Programme
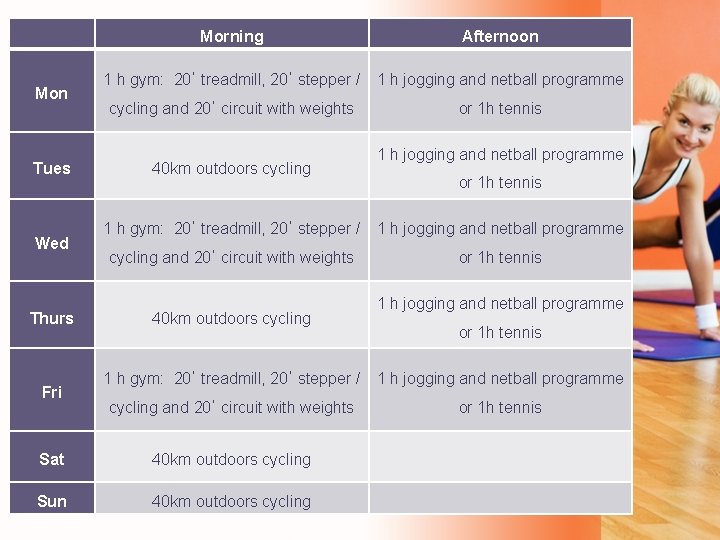
Mon Tues Wed Thurs Fri Morning Afternoon 1 h gym: 20ˈ treadmill, 20ˈ stepper / 1 h jogging and netball programme cycling and 20ˈ circuit with weights 40 km outdoors cycling or 1 h tennis 1 h jogging and netball programme or 1 h tennis 1 h gym: 20ˈ treadmill, 20ˈ stepper / 1 h jogging and netball programme cycling and 20ˈ circuit with weights or 1 h tennis Sat 40 km outdoors cycling Sun 40 km outdoors cycling

Sleep Pattern

v Sleep pattern: § getting up at 04: 30 every morning (except Saturday and Sunday) § going to bed as 21: 30 or 22: 00

Diet

v Breakfast: § muesli, all bran and full cream milk v Midmorning snack: apple v Noon: chicken / red meat Total daily k. J intake: 3913. 4 v Mid afternoon snack: 1 x fruit v Supper: jogurt or carrots with 3 provitas v Fluids: 8 x 500 ml water a day, fusion shake 200 ml sometimes after cycling

Drugs & Supplements

Medication: § Caltrate plus i tab daily § Vitamine C and Spirulina § Fusion shake sometimes after cycling § No anabolic steroids

Examination. . . On examination: v Weight 45 kg v Height 158 cm v BMI 18. 0 v Vitals within normal limits

Special Investigations. . . Blood Tests: • Urea 7. 3 (1. 8 -6. 4 mmol/L) • cholesterol 3. 9 (mmol/L) • Creatinine 67 (53 -97 umol/L) • trigliserides 0. 5 (mmol/L) • Glucose 3. 55 (mmol/L) • HDL Cholesterol 1. 45 (0. 75 -2. 30 mmol/L) • Insulien 2. 2 (2. 6 -11. 1 ul/ml) • LDL Cholesterol 2. 2 mmol/L • total iron 11. 0 (9. 0 -30. 4 umol/L) • Transferrin 2. 41 (2. 03 -3. 60 g/L) • Ferritin 50. 26 (7 -140 ng/ml) • % saturation 20. 4 (20 -55%)

Three Stage Assessment. . . v Biological § re-evaluate health status as BMI is low, diet changes § risk for osteoporosis v Personal / Psychological § fear of making mistakes and letting down the team § feeling anxious and jittery one month before competitions v Social / contextual § family disrupted due to strict diet and ex programme

Differential Diagnosis. . . v OTS v Female athlete triad v Iron deficiency

Management Plan. . . v Dietician – 9920 k. J !! (3914 k. J) v Exercise programme v Psychologist – athlete and family

DISCUSSION ON. . . q Overtraining Syndrome q Female Triad

Terminology. . . OVERTRAINING q process of excessive training in high performance athletes – lead to persistent fatigue q performance decrements q neuro-endocrine changes q alterations in mood states q frequent illnesses (especially URTI) q months to years to recover

OVERTRAINING SYNDROME. . . q failed adaptation to overload training q (inadequate regeneration) q = neuro-endocrine disorder - ? result from process of overtraining q reflects accumulated fatigue during periods of excessive training with inadequate recovery q inappropriate training loads and recovery periods depression of performance capacity and maladaptation Polman RCJ and Houlahan KA. Sports Med: Int J 2004

OVERREACHING. . . q same Sx q more transitory in nature q resolved with short periods of rest or recovery (2 w) q associated with poor performance Budgett R. 1994.
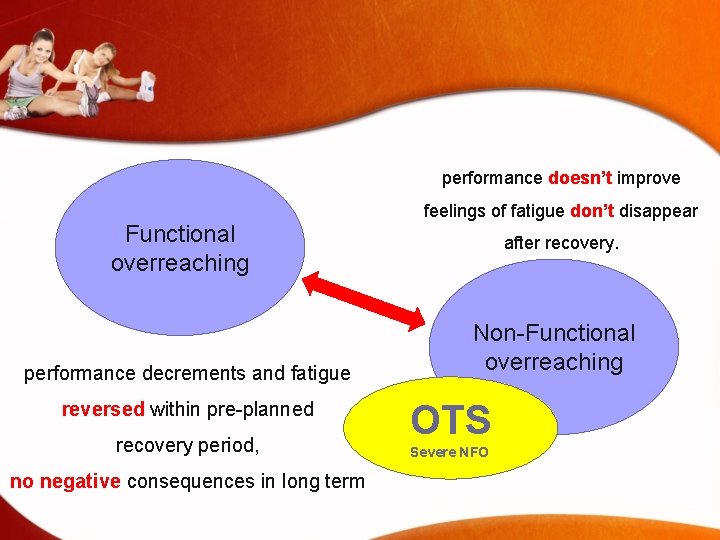
performance doesn’t improve Functional overreaching performance decrements and fatigue reversed within pre-planned recovery period, no negative consequences in long term feelings of fatigue don’t disappear after recovery. Non-Functional overreaching OTS Severe NFO

Complaining of. . . ü disturbed mood profile ü decreased physical performance Exclusion of. . . ü organic disease or infections ü dietary caloric restriction (negative energy balance) ü insufficient CH / protein intake ü iron / magnesium deficiency ü allergies Prevention, diagnosis and treatment of OTS. ECSS position statement “task force”. European Journal of Sport Science. 2006

DIAGNOSIS OF OTS. . .

INCIDENCE. . . 7 – 20% § highest incidence § endurance sport § high volume intense training 4 -6 h per day 6/7 a week § swimming § triathlon § road cycling § power sports - weight lifting judo

PARAMETERS ASSOCIATED WITH OTS

Parameters scientifically shown to be associated with OTS ü Performance decrements ü Persistent high fatigue ratings ü Reduced maximal heart rate by 5 -10 beats per minute ü ∆ in blood lactate threshold, lactate concentration at a given work rate or maximal blood lactate level ü Neuro-endocrine changes: ↑resting p-NA-levels and ↓resting p-NA-excretion ü High self-reported stress levels and sleep disturbances

CHANGES IN OTS. . .

CHANGES IN OTS. . . Hormonal: ü ↓NA excretion, ↑ p-NA levels ü cortisol - resting levels unchanged, reduced maximal response ü ↓testosterone: cortisol ratio by ≥ 30% - followed over time in individual athletes to establish baseline values Blood lactate: ü onset of blood lactate accumulation reflects ↑ in lactate output from skeletal muscle ü ↑lactate levels in muscle - ↓p. H - inducing fatigue ü via inhibition of metabolic pathways ü ( esp anaerobic glycolysis, ↓ ATP production)

CHANGES IN OTS. . . Immunological: ü ↓ salivary Ig. A levels in OTS ü ↓ glutamine plasma levels ü (= substrate for cells of immune systems, esp lymphocytes, macrophage and NK cells) Psychological: ü POMS = profile of mood states scores ↑in OTS ü (? predictor of onset) ü anxiety, depression, apathy, lack of motivation, irritability, inability to relax, lack of self confidence

CHANGES IN OTS. . . Central fatigue and depression: ü alterations in neurotransmitters (serotonin) ü chronically diminished BCAA and ↑p-tryptophan (metabolic precursor of serotonin) ü peripherally released inflammatory mediators ü NB in development of OTS

CHANGES IN OTS. . . Central fatigue and depression: ü 2 hormonal axes ü HPA-axis (catecholamines) and ü SAM-axis (glucocorticoids) ü both implicated in OTS ü ↓TSH, corticotropin releasing hormone response and GH, circulating cytokines released ü in association with state of chronic systemic inflammation induced by overtraining ü Rx: SSRI (Fluoxetine)

MONITORING

q simplest and most effective q self analysis by athletes: ü daily documentation & ratings of ü stress ü fatigue ü muscle soreness ü quality of sleep ü irritability ü perceived exertion during training q perceived exertion during standardized exercise test q changes in blood lactate concentration (threshold and during exercise) q POMS (predictor, not reliable as diagnostic tool)

PREVENTION OF OTS. . .

ü good periodization with active recovery ü regenerative techniques - massage, hydrotherapy, relaxation ü increased fluid and carbohydrate intake ü complete rest ü as much sleep as possible over next 48 hours ü ? contributing factors →

CONTRIBUTING FACTORS. . . ü physical and psychological problems ü too high volume of training or too intense (follow 10% rule) ü too little sleep ü travel & jet lag ü dehydration ü poor eating habits ü injuries, surgery or medication ü family responsibilities / problems ü financial problems

TREATMENT. . .

§ rest and recover § hydration § recognise risk / problem § cut back on exercise § counselling § hydration § muscle fuelling and repair § promote recovery – meditation, relaxation exercises, sports massage - (mentally and physically relaxing) stretching, cold baths, sauna / steam room, electric muscle stimulation

HYDRATION TIPS. . .

q part of game plan • always fluid available, not restricting of amount q start hydrated: 480 ml 2 -3 h before onset of exercise q teach how to monitor own hydration status: • urine volume and color, normal = large amounts, light yellow or clear q sports bottle - required equipment q call frequent water breaks q drink it, don’t splash it q what to hydrate with and when: • water for short practices and mild temperatures • energade / powerade for longer practices, humid and very hot temp q active rehydration post-exercise: 2 -3 cups after exercise

WHAT IS NEW IN OTS?

WHAT IS NEW? § early morning heart rate (EMHR) as indicator of OTS – § empirical evidence failed to find changes § good evidence for max heart rate that ↓with 5 -10 bpm § ↓in blood lactate concentration accompanies OTS § urinary catecholamine output: ü good indicator ü not cost-effective ü inconvenient for routine testing Overtraining effects on immunity and performance in athletes. Laurel T Mackinnon. 2000.

WHAT IS NEW? § hypothesis: psychomotor speed decreased in OTS § similarities with chronic fatigue syndrome and with major depression two meta-analyses - psychomotor slowness consistently present in both syndromes. Nederhof E. et al. Psychomotor speed: Possibly a new marker for overtraining syndrome. Sports Medicine. 2006

FEMALE TRIAD
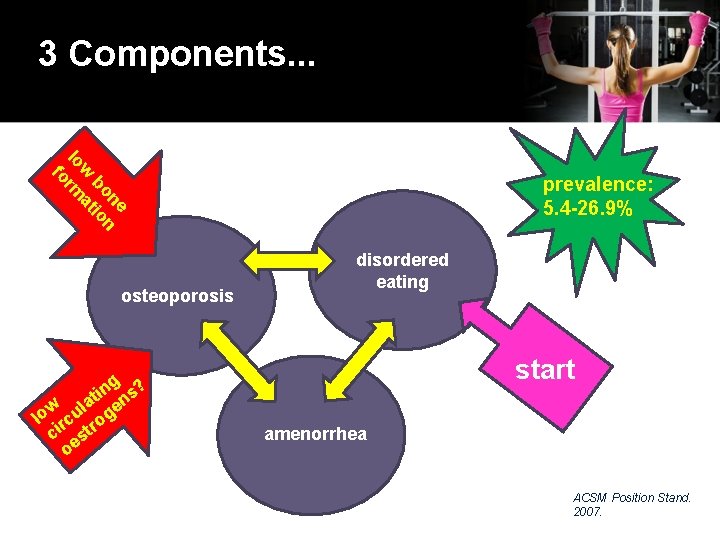
3 Components. . . e on n b io w at lo rm fo osteoporosis g ? n lati ens w lo rcu rog ci st oe prevalence: 5. 4 -26. 9% disordered eating start amenorrhea ACSM Position Stand. 2007.

Prevention. Recognition. Treatment. disordered eating § referred to mental health practitioner , dietician: § evaluation, diagnosis and recommendations for treatment, nutritional counselling BMD assessed § stress / low impact # § total of 6 months of amenorrhea, oligomenorrhea, disordered eating amenorrhea § >16 yo, if BMD is ↓with non-pharmacological management § despite adequate nutrition and body weight - OCP

Take Home Message. . . If you don’t look for something, you will not find it. . . Do not get one-track-minded on the complaint – see the bigger picture. . .

REFERENCES. . .

Budgett R. The overtraining syndrome. Br J Sport Med 1994; 309: 65 -68 Brukner & Khan, 2006 Mackinnon LT. Special feature for the Olympics: Effects of Exercise on the Immune System. Immunology and cell Biology. 2000; 78: 502 -509. Overtraining effects on immunity and performance in athletes. Nederhof E, et al. Psychomotor speed: Possibly a new marker for overtraining syndrome. Sports Medicine. 2006. 36; 10(12)817828 Polman RCJ, Houlahan KA. Cumulative stress and training continuum model: a multidisciplinary approach to unexplained underperformance syndrome. Res Sports Med: Int J 2004; 12: 301 -316 Prevention, diagnosis and treatment of OTS. ECSS position statement “task force”. European Journal of Sport Science. 2006; 6: 1(11 -14)
- Slides: 50