OVERCOMING VACCINE HESITANCY Lisa Barker MD St Lukes

OVERCOMING VACCINE HESITANCY Lisa Barker, MD St. Luke’s Treasure Valley Pediatrics
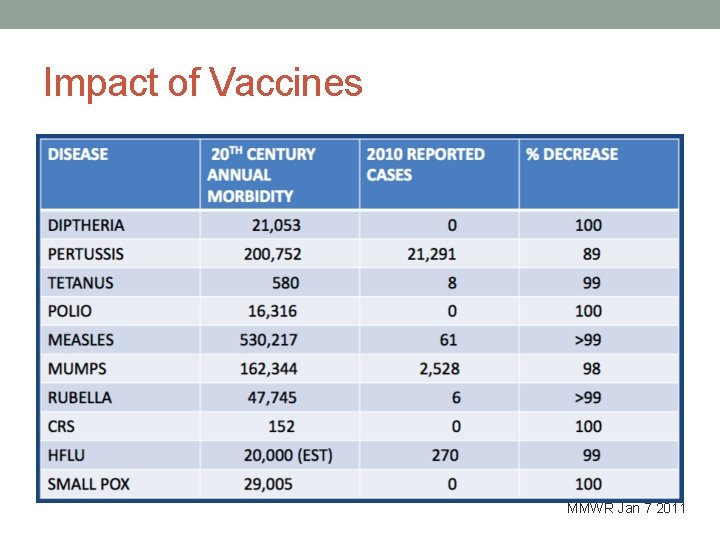
Impact of Vaccines MMWR Jan 7 2011

The Good Old Days • “Vaccines save lives, therefore your child needs to be vaccinated. ” …. Easy, right? No Longer Enough!

What are we up against?

Barriers for Providers • Not enough time (no reimbursement) • The media captures public attention • Parents come in with bad information from the internet • Anecdotes are powerful

Objectives • Define vaccine hesitancy • Understand characteristics of vaccine-hesitant parents • Develop communication strategies to respond to vaccine hesitancy • Identify and respond to the most common concerns raised by vaccine-hesitant parents
What is Vaccine Hesitancy? • A delay in acceptance or refusal of vaccines despite the availability of vaccination services

How Big is the Problem? • 2009 Survey of Parents • >50% of parents expressed concerns about serious adverse effects • 11. 5% had refused at least 1 recommended vaccine • HPV was the most common • Then, varicella, meningococcal conjugate, MMR • 25% believed vaccines cause autism • 90% believe that vaccines are a good way to protect children from disease • 88% do what their doctor recommends • 2012 Survey • 93% of doctors had been asked to delay vaccines Freed 2009, Kemp 2015

Categorizing Parental Attitudes • Unquestioning acceptor – 30 -40% • Cautious acceptor – 25 -35% • Hesitant “fence-sitter” – 20 -30% • Late/selective vaccinator – 2 -27% • Refuser - <2% Leask 2012

Contributing Factors • Personal experience • Media/social networks • Distrust in government, science, big pharma • Decrease in vaccine-preventable diseases • Interactions with healthcare providers • Historical vaccination scares • Grassroots movements • Moral/religious convictions • School entry requirements

RESPONDING TO VACCINE HESITANCY

Communication Strategies Figure 3. Main reasons parents who planned to delay or not to get a vaccine for their child changed their minds Gust 2008

Communication Strategies 1) Initiate the Conversation • “presumptive” vs. “participatory” format • Presumptive: “well, we have to do some shots today” • Participatory: “what do you want to do about shots today? ” • Try to stick with your original recommendation Opel 2013

Communication Strategies 2) Establish Honest Dialogue • Avoid making assumptions • Ask questions • “Do you have cultural or religious beliefs regarding immunization? ” • “Do you know anyone who has had a serious adverse event after an immunization? ” • “Do you have vaccine safety concerns? ” • Listen to concerns Healy 2011

Communication Strategies 3) Acknowledge Risk (corroborate) • Promote partnerships • Be open and honest • Put adverse events into context • Stress the positive benefits of vaccines 4) Discuss the science • Direct, unambiguous language 5) Offer personal experiences/stories Healy 2011

Communication Strategies 6) Provide Information Sources • Ask, “What sources are most influential for you? ” • Ask, “Are you interested in more information? ” (be prepared) • Offer information relevant to specific concerns • Consider offering personal stories www. cdc. gov/vaccines/hcp/patient-ed/conversations

Communication Strategies 7) Other Suggestions • Discuss state laws around childcare and school entry • Make it easy to schedule a vaccination appointment • Ensure ongoing communication

Things to avoid… • Missing cues • Using medical jargon • Patronizing • Discrediting information sources • Overstating vaccine safety • Being confrontational • Using scare tactics

CASE Framework • Corroborate • Acknowledge the concern • Find a point on which you can agree • Set the tone for a respectful conversation • About me • Talk about what you’ve done to enhance your vaccine knowledge • Science • Describe what science has to say • Explain and advise • Offer your recommendation, based on science Singer 2011

Categorizing Parental Attitudes • Unquestioning acceptor – 30 -40% • Cautious acceptor – 25 -35% • Hesitant “fence-sitter” – 20 -30% • Late/selective vaccinator – 2 -27% • Refuser - <2% Leask 2012

ADDRESSING SPECIFIC CONCERNS

Top Vaccine Concerns of Parents/Families • Overwhelming the immune system • “Risk of infection is low” • MMR and autism • Desire for an alternative schedule • Distrust of vaccine additives (preservatives, heavy metals) • HPV vaccine?

“DO IMMUNIZATIONS OVERWHELM THE IMMUNE SYSTEM? ”

The number of vaccinations has steadily increased over the last century… 2015: 14 total vaccines, up to 29 injections by age 2 Offit 2002
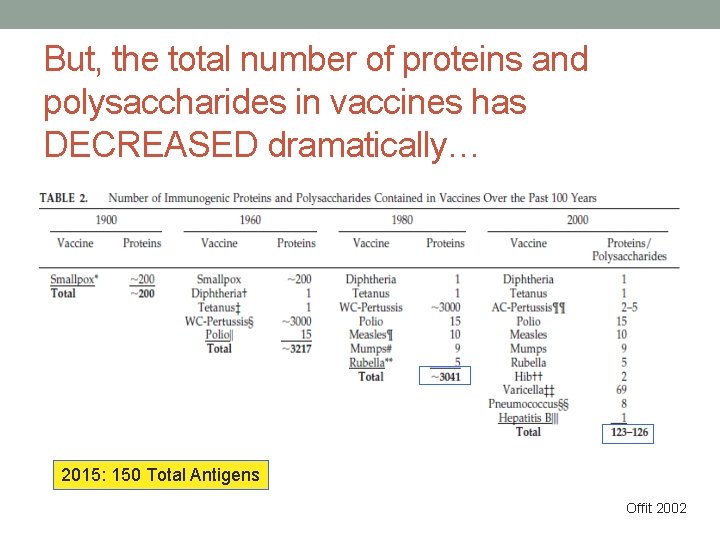
But, the total number of proteins and polysaccharides in vaccines has DECREASED dramatically… 2015: 150 Total Antigens Offit 2002

Important Points • Infants today get more vaccines but fewer antigens to challenge their immune system • “We are giving smarter, safer shots” • The immune system has the capacity to respond to multiple antigens simultaneously • Vaccines do not increase the risk of other infections • Vaccines actually prevent the “weakening” of the immune system

“I’m worried about giving my baby too many shots at one time” • Corroborate: “Kids today certainly get more shots than kids did years ago. ” • About Me: “Our practice follows the CDC schedule because it is carefully designed to protect children at the time they are most vulnerable to disease. ” “I recently returned from a meeting, ” or “I served on a committee that reviewed the schedule. ” • Science: “Although kids get more shots today, they actually receive fewer antigens than when they got fewer shots, because technology has enabled us to make vaccines that have only the part of the cell that induces immune response. Plus, the immunological challenge from a vaccine is nothing compared to what kids fight off every day. An ear infection is a bigger immunological challenge. ” • Explain: “We want all the kids in our practice to be immunized so that they have the greatest chance for a long, healthy life. My own children are fully vaccinated. ” Singer 2011

“HAVEN’T THE DISEASES BEEN ELIMINATED? ”

Herd Immunity • When a critical portion of the population is immunized against a contagious disease, most members of that community are protected against that disease • No single vaccine is 100% effective • Important for protection of immunosuppressed children and children too young to be immunized • Vaccination only works (and continues to work) when a HIGH PERCENTAGE of the population remains vaccinated
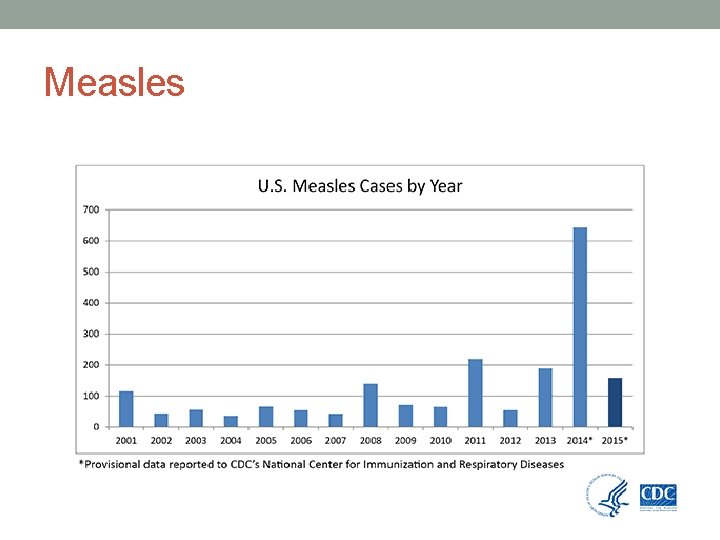
Measles
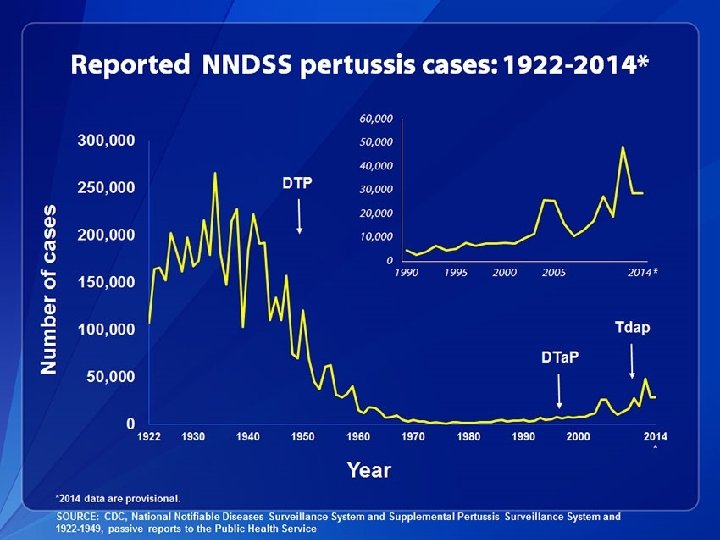
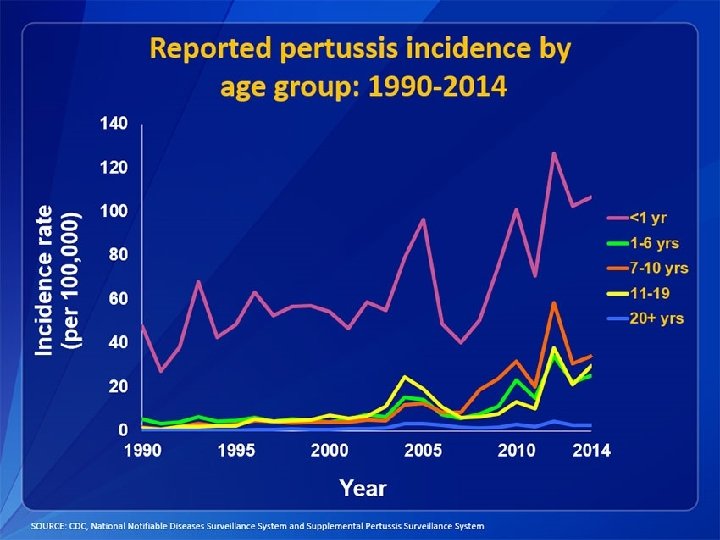
In the news: Whooping cough • Caused by the bacterium Bordatella pertussis • Uncontrollable violent coughing • Most often affects infants and young children • Prior to vaccination, ~200, 000 cases per year • Now, ~10, 000 -40, 000 cases per year

“I had chicken pox and I was fine” • Corroborate: “I can understand why you might feel that way. Hey, I had chicken pox myself. ” • About Me: “The vaccine program has been so successful and a lot of the diseases that we feared, like polio, are no longer a concern. Until last year, I had never seen a case of HIB or measles, but now these diseases are making a comeback. My colleague in San Diego was telling me about what’s going on in CA regarding the whooping cough epidemic. In my practice…” • Science: “These diseases have come back in areas where vaccination rates are low. We have seen measles outbreaks in several states surrounding Idaho. Last year we saw an outbreak of mumps in Idaho…” • Explain: “We care about our patients and don’t want to practice substandard care. All of our patients need to be vaccinated. My children are fully vaccinated. ” Singer 2011

“DO VACCINES CAUSE AUTISM? ”

Autism • Neurodevelopmental disorder • In the 1980’s – 1/10, 000 kids diagnosed with autism • Now, 1/150 American 8 -year-olds has some form of autism • Causes • Genetics • Abnormal brain growth • Environmental triggers • Prematurity • Older parents • Closely spaced pregnancies

“I heard that vaccines cause autism” • Corroborate: “There’s certainly been a lot of coverage on television about vaccines and autism so I can understand why you have questions. ” • About Me: “I always want to make sure I’m up to date on the latest information so that I can do what’s best for my patients, so I’ve researched this thoroughly. In fact, I just returned from a professional conference…” or “I just read nother study looking at this. . . ” • Science: “The scientific evidence does not support a causal link. The CDC, the AAP, the NIH, the IOM (etc) all reviewed the data and all reached the same conclusion. Dozens of studies have been done. None show a link. In fact, the latest autism science indicates…” • Explain/Advise: “Vaccines are critical to maintaining health and wellbeing. They prevent diseases that cause real harm. Choosing not to vaccinate does not protect children from autism, but does leave them open to diseases. ” Singer 2011

“I HEARD IT WOULD BE SAFER TO SPACE OUT THE VACCINES”

Why is the schedule like that? • The ACIP reevaluates the immunization schedule yearly • Each vaccine dose is scheduled using two factors: • Age when the body is most responsive • Goal of protecting children at the earliest possible age Offit 2002

Dangers of an Alternative Schedule • Not founded in science • Cumbersome = more room for error • Increased number of office visits = increased noncompliance • ACIP schedule is based on optimizing the body’s response to a vaccine • Leaves children vulnerable to acquiring serious, potentially fatal diseases

“WHAT ABOUT ALL THAT OTHER STUFF THAT’S IN VACCINES? ”

Other vaccine components • Aluminum • Added to help the vaccine stimulate a better response • Present in higher levels in food, air, water, breast milk, formula • Monosodium glutamate (MSG) • Used as a stabilizer in a few vaccines • Antibiotics • Added to some vaccines to prevent the growth of bacteria during production and storage

Other vaccine components • Formaldehyde • Used to inactivate bacterial toxins (diphtheria, tetanus) • Thimerosal • Mercury-containing preservative used in multi-dose vials • Ethyl mercury – processed easily in the body, not harmful

HPV VACCINATION

HPV • Human Papillomavirus (HPV) • Most common sexually transmitted virus in the U. S. • >50% of sexually active adults are infected with HPV at some point • Causes cancers of the cervix, vagina, vulva, penis, anus, mouth, throat • 26, 000 cancer cases each year

HPV Vaccination • Most recent HPV vaccine = Gardasil 9 • 3 -dose series • Recommended for boys and girls • First dose at age 11 -12

Parent Concerns • “Why should I vaccinate my child at such a young age? ” • “Will my child perceive this as permission to have sex? ” • “My child will not be exposed to HPV because they are going to wait until marriage to have sex. ” • “I’ve heard terrible stories about the side effects of HPV vaccine. ” • “I see this as a moral issue. ”

SUMMARY

Summary • Vaccine hesitancy is on the rise • Vaccine hesitant parents fall along a spectrum of opinion • There are many powerful influences guiding today’s parents – internet, social media, etc. • But, a child’s healthcare provider has the most impact on a parent’s final decision on immunization • Parents ask tough vaccine questions – now you have the tools to answer • With careful conversation and partnership, we can guide and educate hesitant parents

Resources for Families • Healthcare Provider • Websites • American Academy of Pediatrics www. aap. org • American Nurses Association www. nursingworld. org • CDC www. cdc. gov/vaccines • Every Child by Two www. ecbt. org • Vaccine Education Center (CHOP) www. vaccine. chop. edu • CDC: “Provider Resources for Vaccine Conversations With Parents” • Books • Vaccines and Your Child by Paul Offit, MD • Do Vaccines Cause That? By M. Myers, MD • Mama Doc Medicine, by Wendy Sue Swanson, MD • On Immunity, by Eula Biss

References • Gust et al. Immunization attitudes and beliefs among parents: beyond a • • dichotomous perspective. Am J Health Behav 2005; 29(1): 81 -92 Gust et al. Parents with doubts about vaccines: which vaccines and reasons why. Pediatrics 2008; 122: 718 -725 Healy et al. How to Communicate with Vaccine-Hesitant Parents. Pediatrics 2011; 127: S 127 -133 Kempe et al. Physician response to parental requests to spread out the recommended vaccine schedule. Pediatrics 2015; 135 Leask et at. Communicating with parents about vaccination: a framework for healthcare professionals. BMC Pediatrics 2012; 12: 154 Offit et al. Addressing parents’ concerns: do multiple vaccines overwhelm or weaken the infant’s immune system? Pediatrics 2002; 109: 124 -129 Singer A. Making the CASE for vaccine communication: a new model for talking to parents about vaccines. November 2011. http: //bit. ly/14 l. Klh 4. Accessed June 7, 2016 http: //www 2. aap. org/immunization/ http: //www. cdc. gov/vaccines/

Questions
- Slides: 51