Outofthe Operating Room Pediatric Anesthesia Updated 82019 Fiona
















































- Slides: 53

Out-of-the Operating Room Pediatric Anesthesia Updated 8/2019 Fiona Patrao, MBBS, MD Corrie Anderson, MD, FAAP Seattle Children’s Hospital Seattle, Washington, USA

Disclosures No relevant financial relationships

Learning Objectives Describe levels of sedation/anesthesia Risk assess patients Define the challenges of different environments Be prepared for a crisis

Goals of Care for Out-of-OR Anesthesia • Achieve immobility • Avoid patient discomfort and injury • Provide anxiolysis, safe sedation and analgesia • Support patients as they transition from one level of sedation through another

Why sedate for out of OR procedures? • Ensures a cooperative and still patient - Especially consider sedation in children < 6 years old or developmentally delayed • Reduces a child’s anxiety and stress

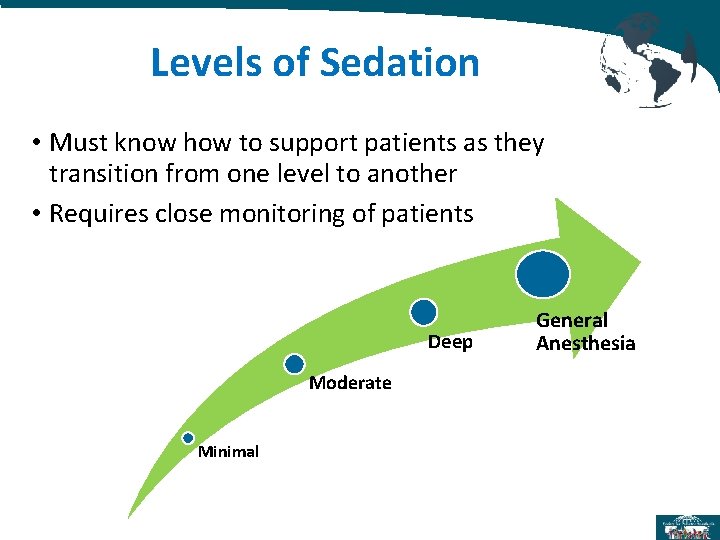
Levels of Sedation • Must know how to support patients as they transition from one level to another • Requires close monitoring of patients Deep Moderate Minimal General Anesthesia

MINIMAL SEDATION (previously “anxiolysis”) • • Minimally depressed level of consciousness Respond to tactile stimulation and verbal command. MODERATE SEDATION (previously “conscious sedation”) • Further depression - respond purposefully to verbal commands alone or with light tactile stimulation Patients independently and continuously maintain airway and ventilation

DEEP SEDATION • NOT easily aroused but respond purposefully following repeated or painful stimulation. • Cardiovascular function is usually maintained. GENERAL ANESTHESIA • NOT arousable • Cardiovascular function may be impaired. Deep sedation may require airway support, and GA probably will require positive pressure ventilation

What is MAC? Monitored Anesthesia Care • Anesthesia resources utilized to support life and provide patient comfort and safety during diagnostic/therapeutic procedures Can range from only monitoring, to monitoring with sedation and can progress to GA and to resuscitation

Pharmacologic Interventions Sedatives Analgesics Anxiolysis

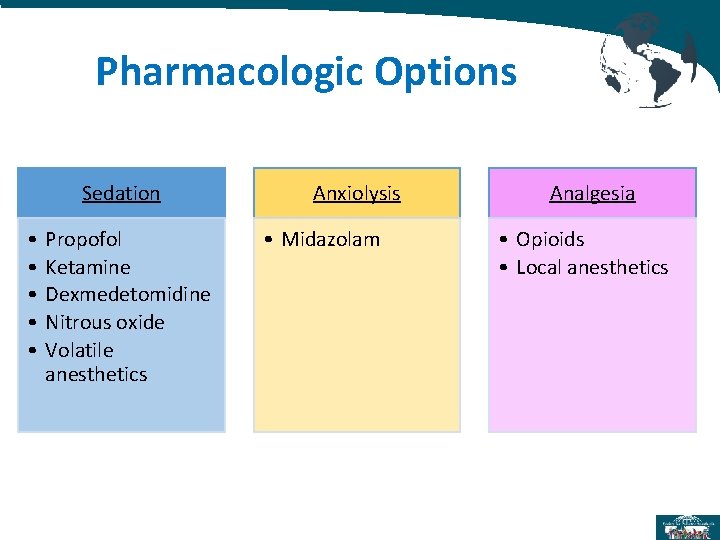
Pharmacologic Options Sedation • • • Propofol Ketamine Dexmedetomidine Nitrous oxide Volatile anesthetics Anxiolysis • Midazolam Analgesia • Opioids • Local anesthetics

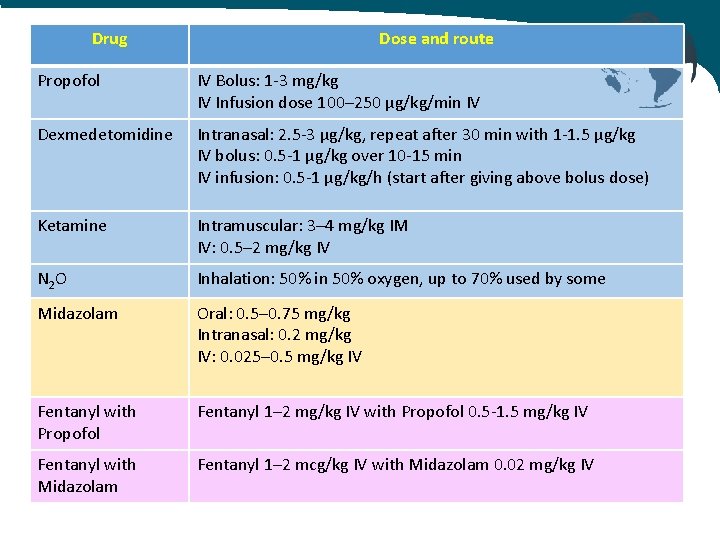
Drug Dose and route Propofol IV Bolus: 1 -3 mg/kg IV Infusion dose 100– 250 µg/kg/min IV Dexmedetomidine Intranasal: 2. 5 -3 µg/kg, repeat after 30 min with 1 -1. 5 µg/kg IV bolus: 0. 5 -1 µg/kg over 10 -15 min IV infusion: 0. 5 -1 µg/kg/h (start after giving above bolus dose) Ketamine Intramuscular: 3– 4 mg/kg IM IV: 0. 5– 2 mg/kg IV N 2 O Inhalation: 50% in 50% oxygen, up to 70% used by some Midazolam Oral: 0. 5– 0. 75 mg/kg Intranasal: 0. 2 mg/kg IV: 0. 025– 0. 5 mg/kg IV Fentanyl with Propofol Fentanyl 1– 2 mg/kg IV with Propofol 0. 5 -1. 5 mg/kg IV Fentanyl with Midazolam Fentanyl 1– 2 mcg/kg IV with Midazolam 0. 02 mg/kg IV

Pharmacologic Options Combined sedative + analgesics Ketamine Dexmedetomidine N 2 O

Non-pharmacologic Options Applicable for short, minimally invasive procedures • Calming and reassurance by parents • • For older kids - Distraction techniques: - TV, video games or other devices Play hypnosis

Non-pharmacologic Options For babies: • • Swaddling, sugar drops For infants < 6 months: keep baby fasted for 4 hours, swaddle and then feed right before procedure - “Feed and sleep” “Fast and feed”

Dose of ”sugar drops” • Administer 2 m. L of 25% sucrose/dextrose solution by syringe into the infant’s mouth (1 m. L in each cheek) • Or infant may suck solution from nipple (pacifier) 1 -2 min before the start of the procedure

Challenges of Remote Locations Patient challenges • Procedure challenges • - • Shared airway: GI, Dental clinic Painful: burns, bone marrow aspirate Immobility: MRI, Proton therapy Environmental challenges - Lack of equipment Metal free zones: MRI Crowded spaces and difficulty to access patient Lack of electrical/gas outlets Remote location of hospital

Staffing • Fully trained anesthesiologist • Trainees should be closely supervised • Additional staff to support anesthesiologist: nurses, technicians

Evaluate Your Patient Assess risk • ASA Status and Risk: - • Airway assessment - - • Organ systems Development and maturity Review: past anesthetics, labs, imaging Assess and plan appropriate size airway equipment Difficult airway? Physical exam

Prepare Your Patient • • Informed consent Ensure adequate fasting IV vs Inhalational induction If need/prefer IV first, consider: - - Sedation with oral/nasal midazolam or dexmedetomidine, or IM ketamine EMLA cream (safe from 37 weeks of infancy onwards)

Prepare Your Patient Prepare your anesthesia plan based on your risk assessment and YOUR skill set

Prepare the Environment Visit the location in advance • Assess space and dimensions: Can anesthesia equipment pass through the door? - • Layout of room: How will you access patient and equipment efficiently? - • Ensure necessities: - Location of O 2 outlets Suction: central or need independent machines? Piped vs cylinder gases Electric outlets? Adequate battery charge?

Prepare for a Crisis • Establish Space: - • for induction, emergence, management of crisis Be prepared: - - Identify location of defibrillator and emergency drugs Battery powered source of light- flashlight Communication- telephone, extra people

Anesthesia Equipment Set Up Airway support CHECK and ENSURE a reliable O 2 source Have FULL O 2 cylinder available as backup Self inflating bag or Mapleson circuit Suction Face mask, oral/nasal airway, supraglottic airway, ETT, laryngoscope, difficult airway tools • Anesthesia machine if possible • • •

Anesthesia Set Up… Anesthesia delivery • • Monitors: ECG, BP, Sp. O 2, ETCO 2, temperature Drugs IV access Airway and ventilation Safe positioning Temperature regulation Documentation

Post Anesthesia Care • Staff to monitor patient - nurse or anesthesiologist • • Safe transport Resources - • O 2, airway equipment Suction Emergency drugs Monitors Prepare for unexpected admissions

Location Specific Discussions

Bedside Procedures Examples: Burns or wound dressings, line placements, chest tubes • Assess patient’s suitability. • May be suitable for older children (> 10 to 12 years) • Monitors: ECG, NIBP, SPO 2, ETCO 2 • Airway and suction equipment • Consider PO, nasal or IM sedation prior to placing IV

Bedside Procedures… • Minimum to moderate sedation only - ketamine, midazolam, dexmedetomidine • Provide analgesia - opioids, NSAIDS, local anesthesia • • Airway and O 2 support as needed Distraction techniques - Music, cartoons, play therapy, parental presence Repetitive procedures? Consider neuraxial or regional nerve catheters

GI Suite Special considerations: • Shared airway: for EGD (esophagogastro-duodenoscopy), ERCP • Short procedures: not usually painful. Use short acting drugs • Full stomach risks

GI Suite… Examples: EGD, Colonoscopy, Liver Biopsy • Options range from minimum sedation to GA: - Spontaneous breathing with boluses of propofol +/short acting opioids - Spontaneous breathing with TIVA: propofol +/dexmedetomidine infusions - GA with LMA or ETT • midazolam as needed for anxiety • Consider lidocaine gargles, swish and swallow for less sedated patients.

GI Suite… GA with ETT for: • ERCP • Gastro-jejunostomy • Any concern for full stomach or unstable airway?

CT Scans (Computed Tomography) Special considerations: Short procedures • Contrast injections - Requires IV placement - Allergic reactions • Exposure to radiation •

CT Scans… Anesthetic options: • If anesthesia machine available: Can consider using volatile agent for induction and maintenance • Other options: propofol, midazolam, ketamine, dexmedetomidine boluses

CT Scans… Other considerations • Babies: - Soothing: swaddling, sugar on pacifier - ”Fast and Feed” • Some scans require breath holds, prone positioning - May require ETT/ LMA - Inspiratory breath hold- with positive pressure ventilation (PPV) - Expiratory hold or apneic pause: following hyperventilation +/- propofol bolus

MRI Special considerations • • • Immobility Confined space No ferromagnetic materials Programmable VP shunts-reprogram after MRI Noise protection Contrast injections

MRI… Anesthesia set up: • Monitors - Do not use regular monitors. ALL wires can cause burns - Use only MRI compatible ECG, NIBP, SPO 2 and ETCO 2 • No monitors? - Proceed with caution - Visual inspection of patient and “HAND on PULSE” • Some “MRI-compatible” equipment cannot be taken too close to the scanner.

MRI… • • Infusions managed and patient monitored from control room. Infusions tunneled through copper channel in wall of control room • Small copper channel on side of door to allow long infusion tubing of critical medications 0 Other options include running tubing under the door, or MRI compatible pumps.

MRI… Anesthetic techniques: • Sedation vs GA - Sedation with midazolam, propofol or ketamine boluses - GA with LMA/ETT with volatile gent - GA with TIVA (Propofol): nasal cannula vs LMA/ETT • Infants - Swaddle - “Fast and Feed”

Oncology Patients Example: Bone marrow aspirate, lumbar puncture, line or drain placement • • • Using central lines -> ensure strict asepsis Check anticoagulation status Minimum to moderate sedation only with spontaneous ventilation - Midazolam, propofol or ketamine will lead to deeper level of sedation and require airway support. - Analgesia with opioids - Liberal local anesthesia infiltration

Oncology Patients For radiation and gamma knife therapy • • Frequent treatments – Long procedures that require immobility and stereotactic head frames Anesthetic risks and considerations vary

Dental Clinics Special considerations: • Shared airway • Often anxious/phobic or developmentally delayed patients • If considering sedation -> MAINTAIN airway reflexes to protect from aspiration of blood/oral secretions

Dental Clinics… Anesthetic techniques: • Oral/ Nasal • Intramuscular • Inhalational • Intravenous • GA with ETT - Midazolam, ketamine, dexmedetomidine - Ketamine - With N 2 O nasal mask – titrated mixture of up to 70% - Titrating dose of midazolam and/or propofol - Preferably in hospital with adequate resources - Oral vs nasal ETT with throat pack

Other considerations…

Crisis Management • Identify how to activate emergency system - Support staff, phones • • Identify location of defibrillator and emergency drugs Ensure defibrillator working - Battery charged, plugged in and routine testing • • Transfer patient to safe location during crisis Crowd control

Complications • Hypoxic episodes: - Laryngospasm - Bronchospasm • • Aspiration Failed sedation Prolonged recovery Allergic reactions and anaphylaxis

Management of anaphylaxis Severity of symptoms Intervention MILD (Urticaria, flushing) • Remove offending agent • Consider oral dose of diphenhydramine MODERATE to SEVERE (Bronchospasm, facial or laryngeal edema, hypotension with tachycardia/bradycardia) • Remove offending agent • 100 % high flow O 2 • IM Epinephrine (10 µg/kg) – repeat 10 to 15 mins as needed • IV hydrocortisone • 2 agonist for bronchospasm • Antihistamine: IV diphenhydramine (H 1 blocker), IV ranitidine (H 2 blocker) • Intubate for stridor/airway compromise • Treat hypotension - Supine as tolerated, legs elevated - 20 ml/kg isotonic fluid bolus, repeat as needed

Occupational Hazards • Exposure to radiation: use lead aprons, thyroid lead shields, lead screens • Noise damage: use ear plugs in MRI • Tripping • Inadequate lighting • Accidental injuries to self

Safety and Improvement • Posters with checklists and reminders • Protocols for using checklists before start of procedure • Emergency phone numbers should be easily visible

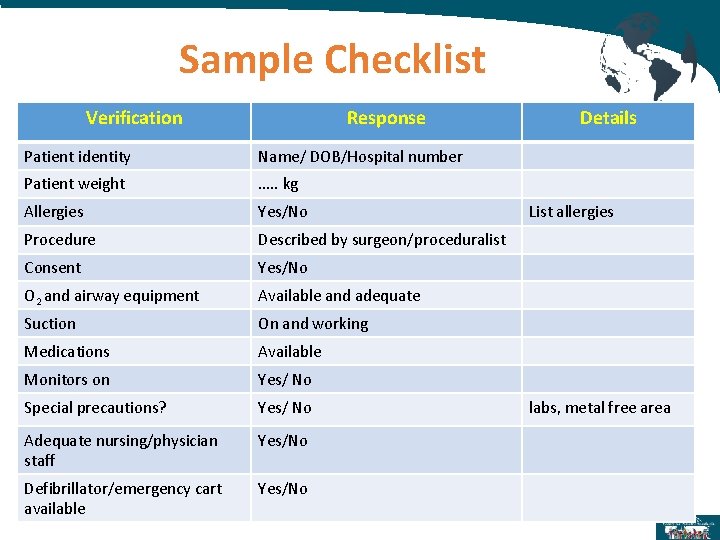
Sample Checklist Verification Response Patient identity Name/ DOB/Hospital number Patient weight …. . kg Allergies Yes/No Procedure Described by surgeon/proceduralist Consent Yes/No O 2 and airway equipment Available and adequate Suction On and working Medications Available Monitors on Yes/ No Special precautions? Yes/ No Adequate nursing/physician staff Yes/No Defibrillator/emergency cart available Yes/No Details List allergies labs, metal free area

Safety and Improvement • Consider QI (Quality Improvement) projects to test and improve protocols • Simulation sessions - Simulate crises in remote locations to identify weaknesses and improve awareness

Conclusion • Evaluate, assess and prepare the patient • Plan an anesthetic based on patient, location, procedure, available equipment and YOUR skill set • Prepare for: - Changing levels of sedation - Critical events

References 1. Practice Guidelines for Moderate Procedural Sedation and Analgesia 2018: A Report by the American Society of Anesthesiologists Task Force on Moderate Procedural Sedation and Analgesia, the American Association of Oral and Maxillofacial Surgeons, American College of Radiology, American Dental Association, American Society of Dentist Anesthesiologists, and Society of Interventional Radiology. Anesthesiology 2018; 128: 437– 79 2. Coté CJ, Wilson S. Guidelines for Monitoring and Management of Pediatric Patients Before, During, and After Sedation for Diagnostic and Therapeutic Procedures: Update 2016. Pediatrics. July 2016; Vol 138: e 20161212 -2 3. Metzner J, Domino KB. Risks of anesthesia or sedation outside the operating room: the role of the anesthesia care provider. Curr Opin Anaesthesiol. 2010; 23: 523 -31 4. Cravero JP et al and the Pediatric Sedation Research Consortium. Incidence and nature of adverse events during pediatric sedation/anesthesia for procedures outside the operating room: report from the Pediatric Sedation Research Consortium. Pediatrics 2006; 118: 1087– 96 5. 6. Cantlay K, Williamson S, Hawkings J. Anaesthesia for Dentistry. Br J Anaesth. 2005; 5: 71 -5 7. 8. Cravero JP, George TB. Review of Pediatric Sedation. Anesth Analg 2004; 99: 1355– 64 9. Sottas CE, Anderson B. Dexmedetomidine: the new all-in-one drug in paediatric anaesthesia? Curr Opin Anaesthesiol 2017; 30: 441 -51 Bell C, Sequeira PM. Nonoperating room anesthesia for children. Curr Opin Anaesthesiol 2005, 18: 271 -6 Fein JA, Zempsky WT, Cravero JP and the Committee on Pediatric Emergency Medicine and Section on Anesthesiology and Pain Medicine. Relief of Pan and Anxiety in Pediatric Patients in Emergency Medical Systems. Pediatrics 2012; 130; e 1391