Outcomes of shoulder replacement in humeral head avascular












- Slides: 19

Outcomes of shoulder replacement in humeral head avascular necrosis Jacob J Ristow MD, Ciani M Ellison BS, Dara J Mickschl PA-C, Kenneth C Berg MD, Kirk C Haidet MD, Jason R Gray MD, Steven I Grindel MD Department of Orthopaedic Surgery, Froedtert and the Medical College of Wisconsin, Milwaukee, WI

No disclosures

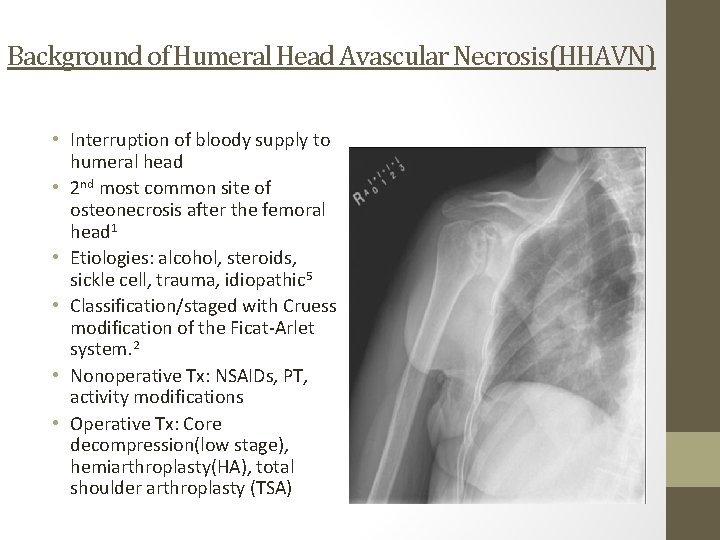
Background of Humeral Head Avascular Necrosis(HHAVN) • Interruption of bloody supply to humeral head • 2 nd most common site of osteonecrosis after the femoral head 1 • Etiologies: alcohol, steroids, sickle cell, trauma, idiopathic 5 • Classification/staged with Cruess modification of the Ficat-Arlet system. 2 • Nonoperative Tx: NSAIDs, PT, activity modifications • Operative Tx: Core decompression(low stage), hemiarthroplasty(HA), total shoulder arthroplasty (TSA)

Cruess Classification • Stage 1+2 nonoperative, core decompression 4 • Stage 3 -5 Nonoperative, hemiarthroplasty, total shoulder arthroplasty

Background • Direct relationships between the increase in necrotic stage and the percent of patients who needed shoulder arthroplasty have been described • Outcomes of total shoulder arthroplasty (TSA) and hemiarthroplasty (HA) in patients with HHAVN of different etiologies individually have been documented • Reduction in pain and an increase in range of motion (ROM) • Studies few and small in sample size with exception of a limited number • Fail to compare surgical outcomes between differing etiologic groups • Sickle cell disease population in particular being underrepresented

Aim of study • Goal of this study was to evaluate clinical outcomes of surgical intervention for HHAVN and identify any influencing factors on outcomes including: etiology, stage, implant choice • Hypothesis: Regardless of implant choice, disease stage and etiology of osteonecrosis, patients would appreciate significant improvement in functional outcome scores postoperatively

Methods • Retrospective review of senior author’s patients 2004 -2015 • Inclusion criteria: • • Diagnosis of HHAVN complete pre-operative functionality assessments +imaging surgical treatment with HA or TSA Minimum 1 -year follow up. • Study patients: • 41 cases identified • 25 patients with 29 arthroplasty procedures (19 HA, 10 TSA) who met criteria • Outcomes: Baseline functionality scores: • Pre-op shoulder strength and range of motion and completed questionnaires • • Simple Shoulder Test Constant Score modified for age and sex UCLA Shoulder Score ASES Shoulder Score • Radiographic anaylsis: Stage of necrosis determined by senior author • Surgical Technique/Implants: Deltopectoral approach for all patients. Tornier and Depuy implants and all humeral implants were press-fit. In TSA, allpolyethylene glenoids with peripheral cement inserted

Analysis • 3 comparison groups were evaluated for complication rates, need for additional treatment, and functionality scores: • HA v TSA • Low stage (Cruess 1 -3) v High Stage (Cruess 4 -5) • Underlying Etiology • Statistics (IBM SPSS predictive analytics software): • Fischer’s Exact test was used to compare two groups of binomial data • Pearson’s Chi-Squared used for three or more groups of binomial data • Wilcoxon Sign Ranked test was used to compare two groups of paired scale variables • The Mann-Whitney test was used to compare two unpaired groups of scale variables • Kruskal-Wallis test used for three or more unpaired scale variables

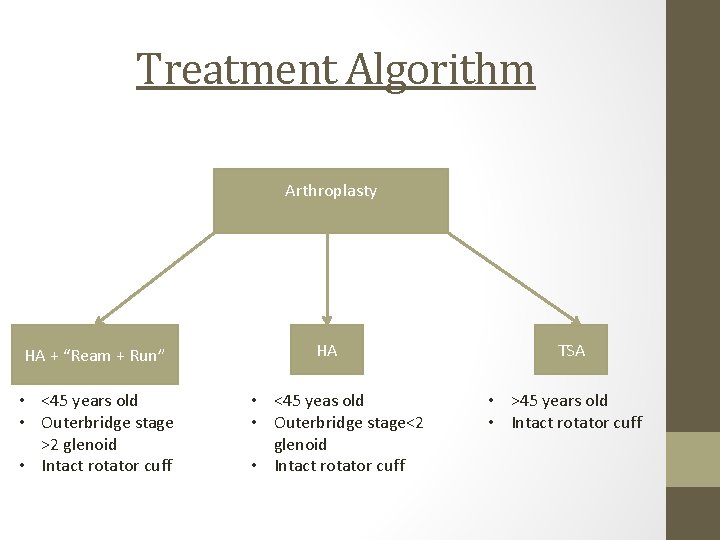
Treatment Algorithm Arthroplasty HA + “Ream + Run” • <45 years old • Outerbridge stage >2 glenoid • Intact rotator cuff HA • <45 yeas old • Outerbridge stage<2 glenoid • Intact rotator cuff TSA • >45 years old • Intact rotator cuff

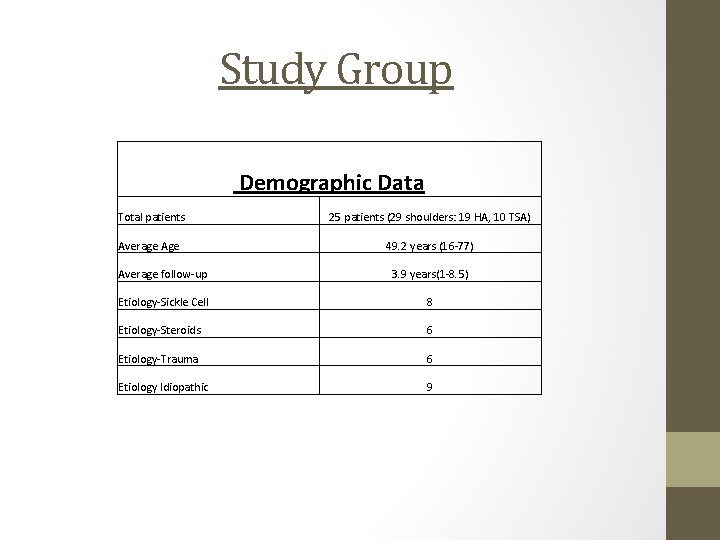
Study Group Demographic Data Total patients 25 patients (29 shoulders: 19 HA, 10 TSA) Average Age 49. 2 years (16 -77) Average follow-up 3. 9 years(1 -8. 5) Etiology-Sickle Cell 8 Etiology-Steroids 6 Etiology-Trauma 6 Etiology Idiopathic 9

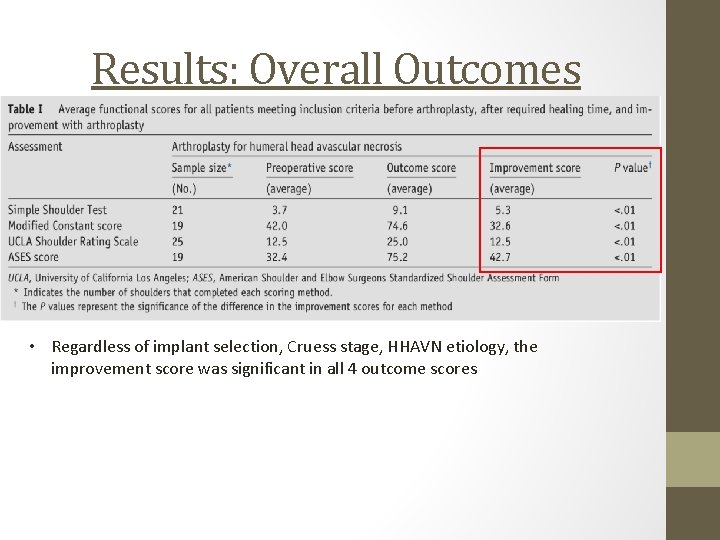
Results: Overall Outcomes • Regardless of implant selection, Cruess stage, HHAVN etiology, the improvement score was significant in all 4 outcome scores

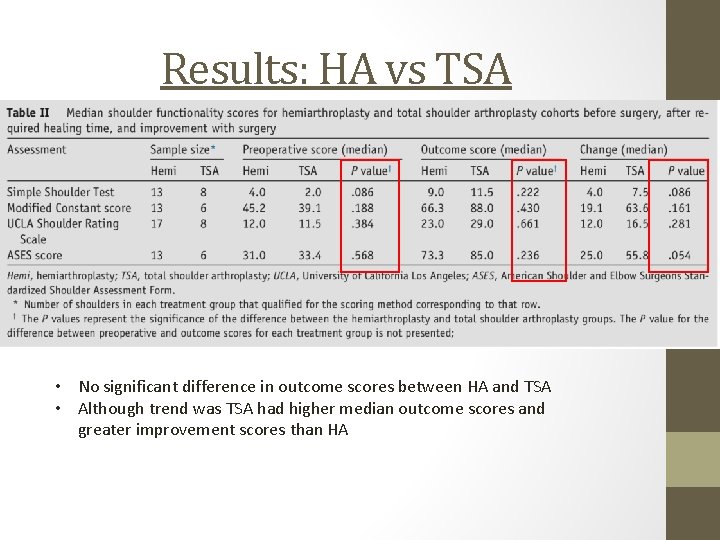
Results: HA vs TSA • No significant difference in outcome scores between HA and TSA • Although trend was TSA had higher median outcome scores and greater improvement scores than HA

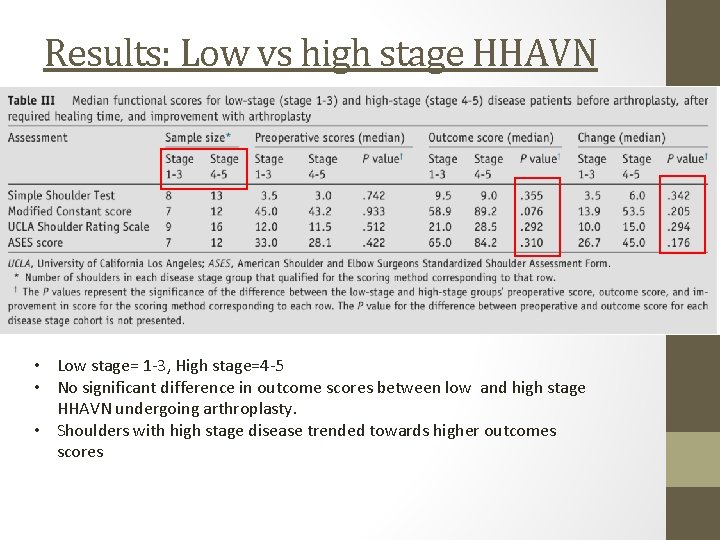
Results: Low vs high stage HHAVN • Low stage= 1 -3, High stage=4 -5 • No significant difference in outcome scores between low and high stage HHAVN undergoing arthroplasty. • Shoulders with high stage disease trended towards higher outcomes scores

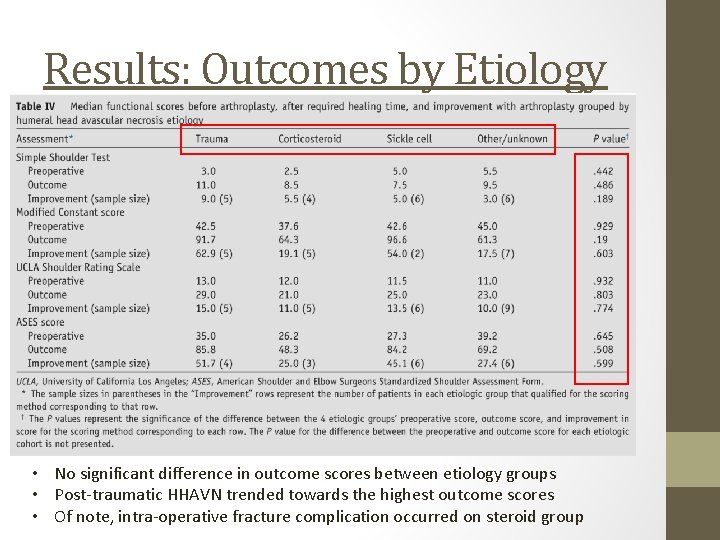
Results: Outcomes by Etiology • No significant difference in outcome scores between etiology groups • Post-traumatic HHAVN trended towards the highest outcome scores • Of note, intra-operative fracture complication occurred on steroid group

Complications • Suture abscess • In TSA patient • Treated conservatively with oral antibiotics/local wound cares • Intra-operative fracture to the medial calcar during the implantation of a press fit humeral component in TSA patient • Immediate placement of a cable for support • Uneventful healing without change in post-operative protocol • Occurred in the corticosteroid subgroup with high stage necrosis. • None of the arthroplasties required a revision surgery.

Conclusions • Efficacy and safety of arthroplasty procedures in HHAVN • Patient factors (stage and etiology) do not appear to have a significant effect on surgical outcomes • Improvements in pain, range of motion, and functionality can be achieved with either TSA or HA with low risk of complications or need for additional procedures. • Statistically significant difference of both the HA and TSA postoperative outcome scores when compared to their preoperative scoring (P<0. 05). • Caution in corticosteroid induced HHAVN. Noted higher complication rates in other studies and 1 complication in this study. 9

Limitations • Trends towards greater improvements in functionality scores in the shoulders that underwent TSA and patients who’s etiology was post-traumatic, as well as higher outcome scores in shoulders with high stage disease but not statistically significant • A larger sample size may have provided the power necessary to prove these trends to be statistically significant • Longer term follow-up necessary to follow up on revision rates and long term outcomes. • Lack of randomization to HA versus TSA as decision-making was made based on intra-operative findings as mentioned before.

References • • • • . Cruess RL. "Steroid-Induced Avascular Necrosis of the Head of the Humerus: Natural History and Management. " J Bone Joint Surg Br; 58 B. 3 (August 1976): 313 -17. 2. Feeley BT, Fealy S, Dines DM, Warren RF, Craig EV. “Hemiarthroplasty and total shoulder arthroplasty for avascular necrosis of the humeral head. ” J Shoulder and Elbow Surg: 7 (September/October 2008): 689 -94. doi: 10. 1016/j. jse. 2008. 03. 009 3. Franceschi F, Fracneschetti E, Paciotti M, Torre G, Samuelsson K, Papalia R, Karlsson J, Denaro V. “Surgical management of osteonecrosis of the humeral head: a systematic review. ” Knee Surg Sports Traumatol Arthrosc. 25 (2017): 3270 -3278. 4. Hattrup SJ, Cofield RH. “Osteonecrosis of the humeral head: Relationship of disease stage, extent, and etiology to natural history. " J Shoulder and Elbow Surg; 8. 6 (1999): 559 -64. 5. Hattrup SJ, Cofield RH. “Osteonecrosis of the humeral head: Results of replacement. ” J Shoulder and Elbow Surg: 9. 3 (May/June 2000): 177 -82. 6. Lau MW, Blinder MA, Williams K, Galatz LM. “Shoulder Arthroplasty in Sickle Cell Patients with Humeral Head Avascular Necrosis. " J Shoulder and Elbow Surg: 16. 2 (2007): 129 -34. doi: 10. 1016/j. jse. 2006. 05. 012. 7. Mansat P, Huser L, Mansat M, Bellumore Y, Rongières M, Bonnevialle P. “Shoulder Arthroplasty for Atraumatic Avascular Necrosis of the Humeral Head: Nineteen Shoulders Followed Up for a Mean of Seven Years. " J Shoulder and Elbow Surg: 14. 2 (2005): 114 -20. doi: 10. 1016/j. jse. 2004. 06. 019 8. Orfaly RM, Rockwood Jr. CA, Esenyel CZ, Wirth MA. “Shoulder arthroplasty in cases with avascular necrosis of the humeral head. " J Shoulder and Elbow Surg: 16. 3 Suppl (2007): S 27 -32. doi: 10. 1016/j. jse. 2006. 005 9. Parsch D, Lehner B, Loew M. “Shoulder arthroplasty in nontraumatic osteonecrosis of the humeral head. ” J Shoulder and Elbow Surg: 12. 3 (May/June 2003): 226 -30. doi: 10. 1016/S 1058 -2746(02)00040 -X 10. Schoch BS, Barlow JD, Schleck C, Cofield RH, Sperling JW. “Shoulder arthroplasty for atraumatic osteonecrosis of the humeral head. ” J Shoulder Elbow Surg. 25. 2 (February 2016): 238 -45. doi: 10. 1016/j. jse. 2015. 07. 019 11. Schoch BS, Barlow JD, Schleck C, Cofield RH, Sperling JW. “Shoulder arthroplasty for post-traumatic osteonecrosis of the humeral head. ” J Shoulder Elbow Surg. 25. 3 (March 2016) : 406 -12. doi: 10. 1016/j. jse. 2015. 08. 041 12. Smith RG, Sperling JW, Cofield RH, Hattrup SJ, Schleck CD. “Shoulder hemiarthroplasty for steroid-associated osteonecrosis. ” J Shoulder and Elbow Surg. 17. 5 (September/October 2008): 685 -88. doi: 10. 1016/j. jse. 2008. 01. 149 13. Raiss P, Kasten P, Baumann F, Moser M, Rickert M, Loew M. “Treatment of osteonecrosis of the humeral head with cementless surface replacement arthroplasty. ” J Bone Joint Surg Am. 91. 2 (February 2009): 340 -9. doi: 10. 2106/JBJS. H. 00560 14. Tyrrell Burrus M, Cancienne JM, Boatright JD, Yang S, Brockmeier SF, Werner BC. “Shoulder arthroplasty for humeral head avascular necrosis is associated with increased postoperative complications. ” HSS J. 14(1) February 2018: 2 -8. Doi: 10. 1007/s 11420 -017 -9562 -8

Thank you