Outcomes of Bariatric Surgery Majid Valizadeh MD Obesity

Outcomes of Bariatric Surgery Majid Valizadeh, MD Obesity Prevention and Treatment Research Center Research Institute for Endocrine Sciences Shahid Beheshti University of Medical Sciences 16 Nov. 2018 1397. 08. 25 Tehran, Iran

Agenda: § Introduction § Effects of the bariatric surgery on: § § § § Weight Glycemic control (DM remission & Improvement) Lipids Blood pressure Prevention of Diabetes Microvascular & Macrovascular complications Cardiovascular disease and mortality § Conclusions § Tehran Obesity Treatment Study (TOTS) 2
![Introduction: The world epidemic of overweight [BMI] > 25 and obesity ≥ (BMI 30) Introduction: The world epidemic of overweight [BMI] > 25 and obesity ≥ (BMI 30)](http://slidetodoc.com/presentation_image/24dd8f71773043087e80d6a6b269b0ea/image-3.jpg)
Introduction: The world epidemic of overweight [BMI] > 25 and obesity ≥ (BMI 30) is estimated about 1. 7 billion individuals. In US approximately two thirds of individuals are overweight, and of those, almost half are obese. The BMI subgroups experiencing the most rapid growth are: 35 or higher (23 million) and 40 or higher (8 million). In Iran: the prevalence of obesity in populations > the age of 18 was 21. 7% and in populations < 18 was 6. 1%. An ascending trend in the prevalence of obesity in Iran. 3

4

Overweight and Obesity: Findings from 20 Years of the Tehran Lipid and Glucose Study Prevalence of excess weight, including overweight and obesity were 20. 8 and 63. 6% among those aged below and above 20 years, respectively. TLGS found a high incidence of obesity with higher incidence in women among Tehranian adults; Prevalence of abdominal obesity in men and women were 52. 8% and 44. 4% respectively. 5
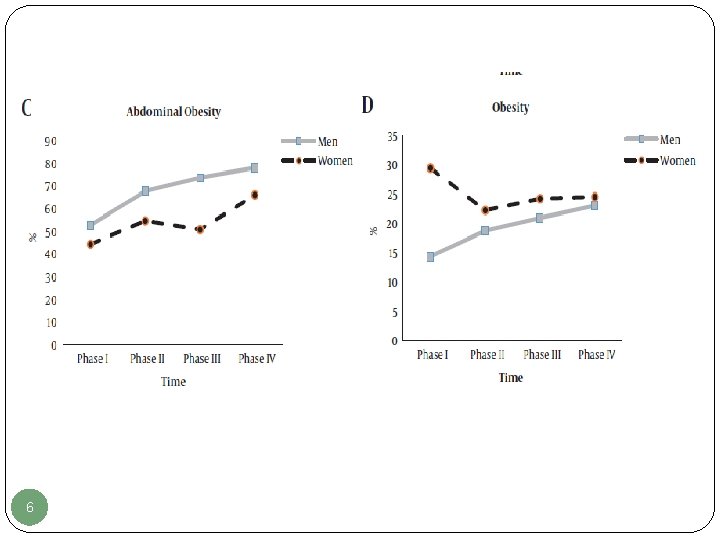
6

The rise in the prevalence of obesity is associated with increases in the prevalence of obesity comorbidities: (eg, type 2 diabetes, hyperlipidemia, hypertension, obstructive sleep apnea, heart disease, stroke, asthma, back and lower extremity weight-bearing degenerative problems, several forms of cancer, depression, etc). These comorbidities are responsible for more than 2. 5 million deaths/year worldwide. The loss of life expectancy due to obesity is profound—in comparison with a normal-weight individual, a 25 -year-old morbidly obese man has a 22% reduction in expected remaininglifespan, representing an approximate loss of 12 years of life. 7

Efficacy of Life style ± Drugs Unfortunately, diet therapy, ± support organizations, is relatively ineffective in treating obesity in the long term. (Modest and nondurable- high failure rate) There are currently no truly effective pharmaceutical agents to treat obesity, especially morbid obesity. 8

Surgical Treatment Bariatric or Metabolic Surgery is one of the best way of obesity treatment, effective (more weight loss) and durable. The literature with respect to Weight loss and Co morbidity outcomes of bariatric surgery is extensive. 9
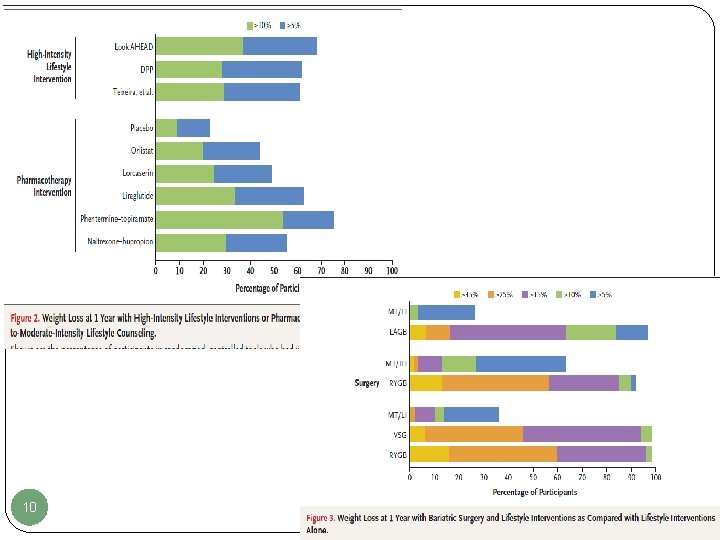
10
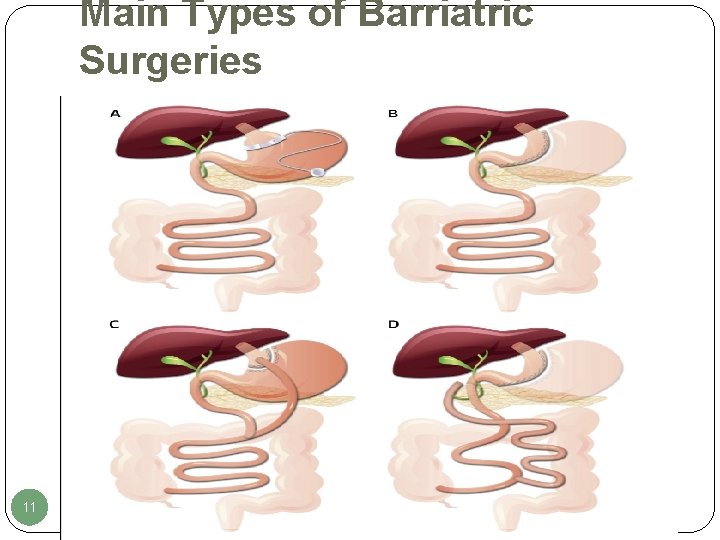
Main Types of Barriatric Surgeries 11
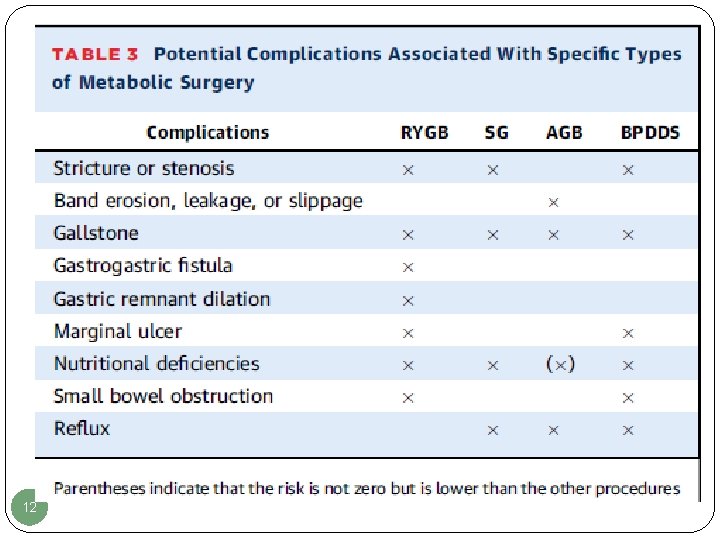
12
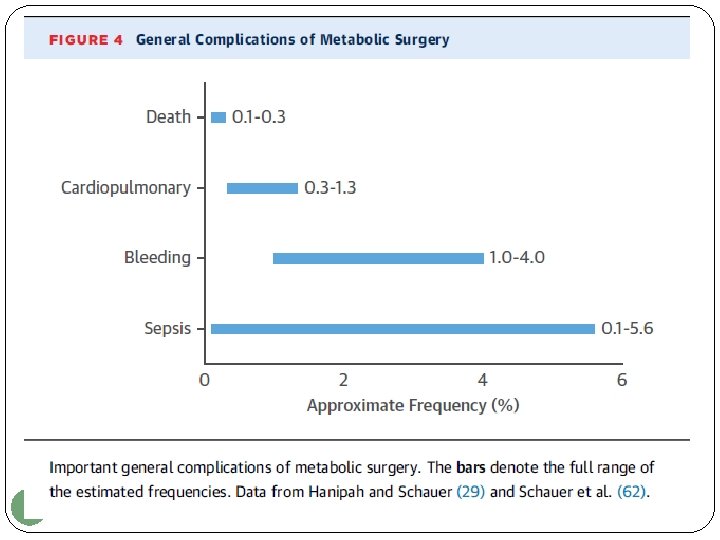
13

Obesity complications Mechanical : Osteoarthritis Sleep Apnea Gastroesophageal reflux Metabolic T 2 DM HTN Dyslipidemia Fatty liver 14 Hard Outcomes: CVD § Coronary heart disease § Heart failure § Atrial fibrillation § Stroke Mortality Cancer
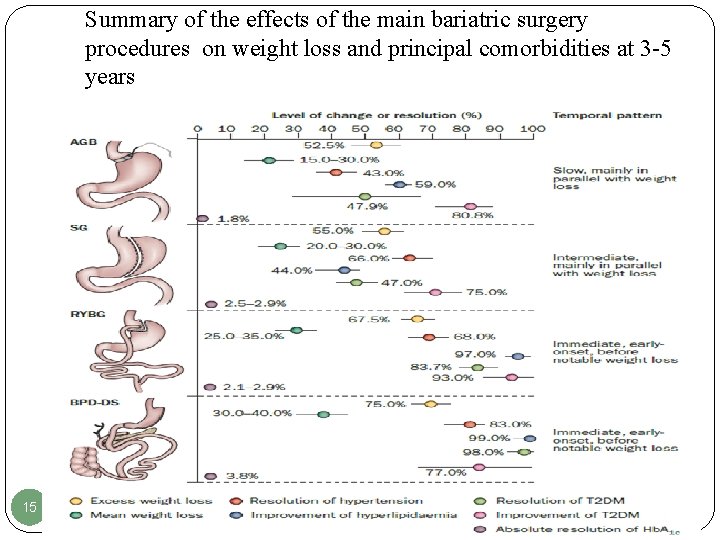
Summary of the effects of the main bariatric surgery procedures on weight loss and principal comorbidities at 3 -5 years 15
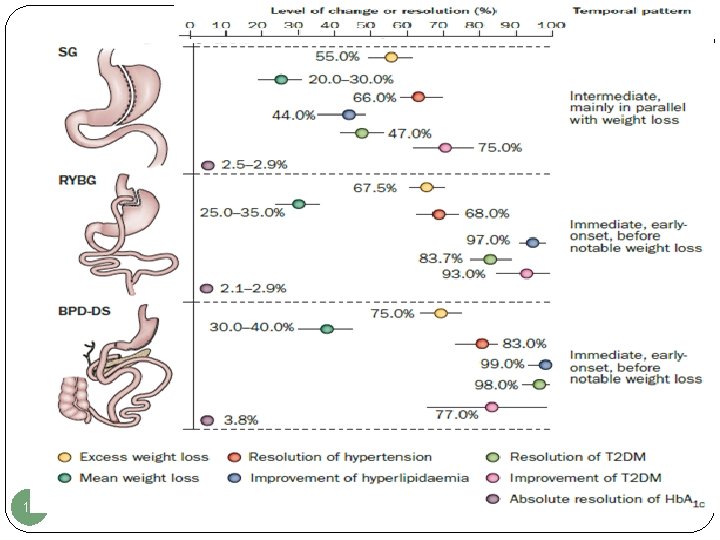
16
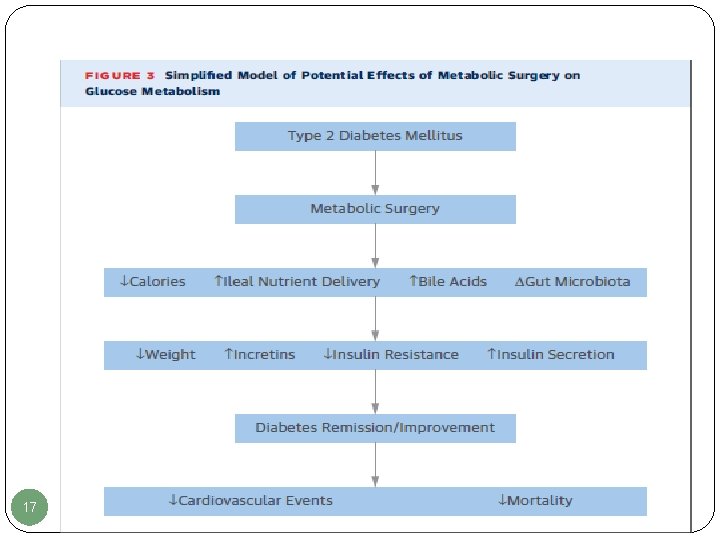
17

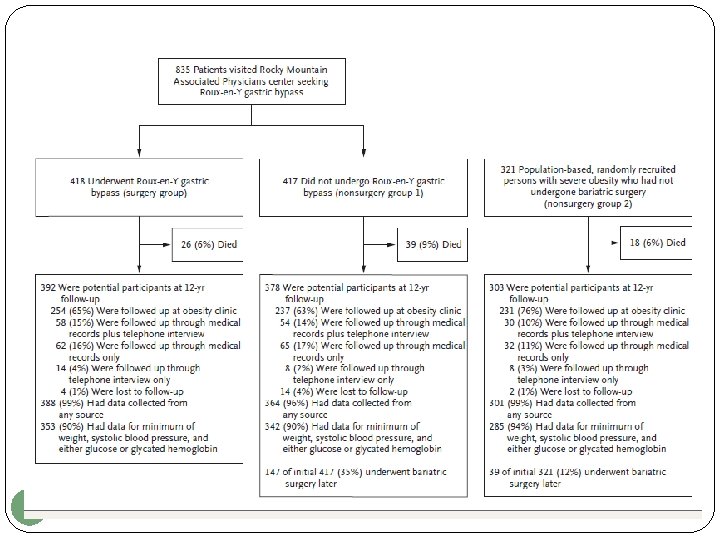
Design: An observational, prospective study in the US. Population: 1156 patients with severe obesity comprised three groups: 418 patients who sought and underwent Roux-en-Y gastric bypass (surgery group), 417 patients who sought but did not undergo surgery (primarily for insurance reasons) (nonsurgery group 1), and 321 patients who did not seek surgery (nonsurgery group 2). Primary end points: The percentage of original weight lost and the incidence and remission rates of type 2 diabetes, hypertension, and dyslipidemia among the survivors at 12 years. 18 Adams TD, et al. N Engl J Med 2017; 377: 1143 -55.
19
20
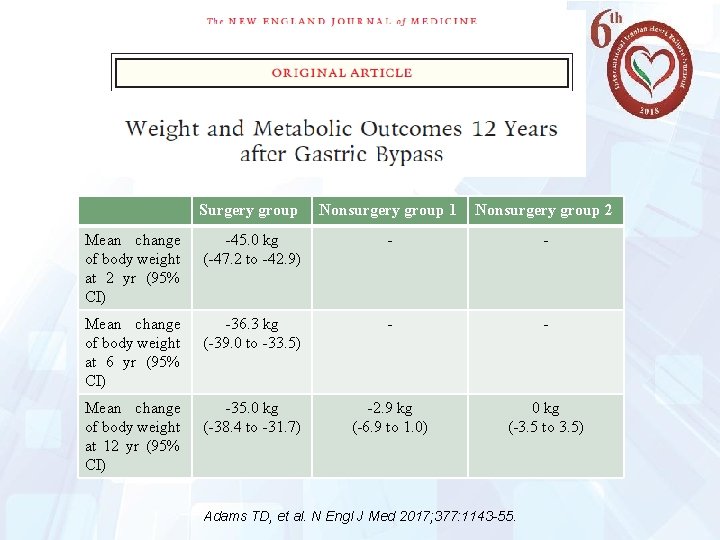

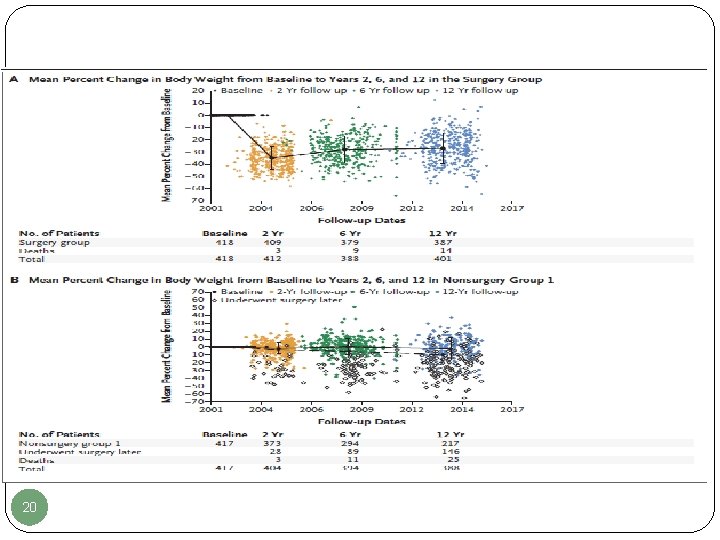
21 Surgery group Nonsurgery group 1 Nonsurgery group 2 Mean change of body weight at 2 yr (95% CI) -45. 0 kg (-47. 2 to -42. 9) - - Mean change of body weight at 6 yr (95% CI) -36. 3 kg (-39. 0 to -33. 5) - - Mean change of body weight at 12 yr (95% CI) -35. 0 kg (-38. 4 to -31. 7) -2. 9 kg (-6. 9 to 1. 0) 0 kg (-3. 5 to 3. 5) Adams TD, et al. N Engl J Med 2017; 377: 1143 -55.
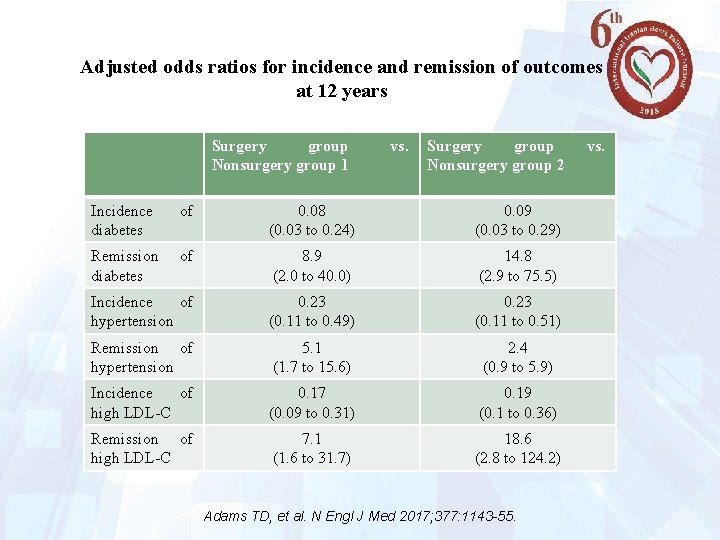
Adjusted odds ratios for incidence and remission of outcomes at 12 years 22 Surgery group Nonsurgery group 1 vs. Surgery group Nonsurgery group 2 Incidence diabetes of 0. 08 (0. 03 to 0. 24) 0. 09 (0. 03 to 0. 29) Remission diabetes of 8. 9 (2. 0 to 40. 0) 14. 8 (2. 9 to 75. 5) Incidence of hypertension 0. 23 (0. 11 to 0. 49) 0. 23 (0. 11 to 0. 51) Remission of hypertension 5. 1 (1. 7 to 15. 6) 2. 4 (0. 9 to 5. 9) Incidence of high LDL-C 0. 17 (0. 09 to 0. 31) 0. 19 (0. 1 to 0. 36) Remission of high LDL-C 7. 1 (1. 6 to 31. 7) 18. 6 (2. 8 to 124. 2) Adams TD, et al. N Engl J Med 2017; 377: 1143 -55. vs.

Effect on T 2 DM Incidence Roux-en-Y gastric bypass resulted in a 91 to 92% lower incidence of new onset type 2 diabetes at 12 years than that among patients in the non-surgery groups. After a median follow-up of 10 years in the SOS study, the incidence of type 2 diabetes was 83% lower among all the patients who underwent surgery and 88% lower among patients who underwent Roux-en-Y gastric bypass than among patients in the control group. 23

Conclusions: This study showed long-term durability of weight loss and effective remission and prevention of type 2 diabetes, hypertension, and dyslipidemia after Roux-en-Y gastric bypass. 24 Adams TD, et al. N Engl J Med 2017; 377: 1143 -55.
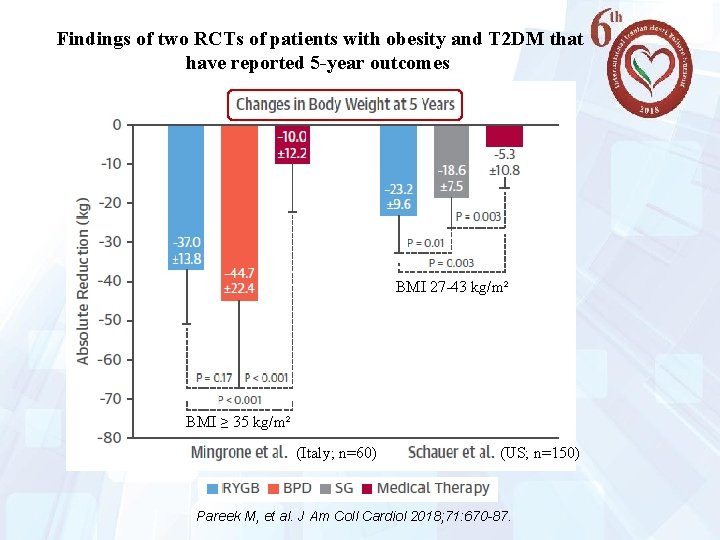
Findings of two RCTs of patients with obesity and T 2 DM that have reported 5 -year outcomes BMI 27 -43 kg/m² BMI ≥ 35 kg/m² (Italy; n=60) 25 (US; n=150) Pareek M, et al. J Am Coll Cardiol 2018; 71: 670 -87.
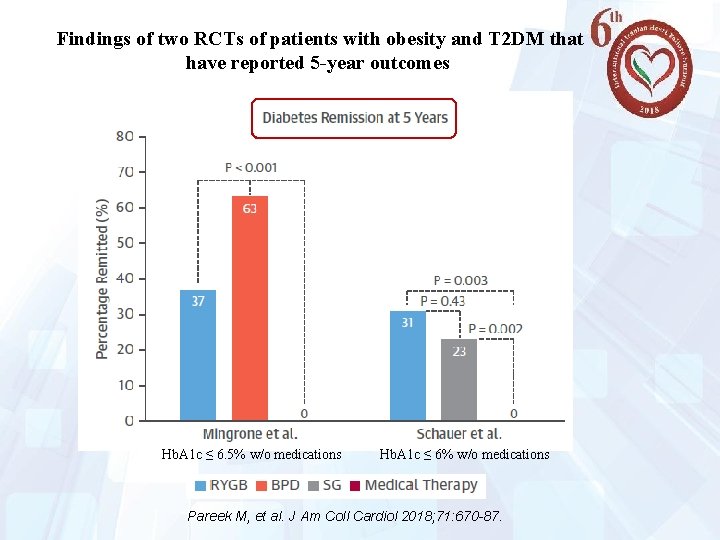
Findings of two RCTs of patients with obesity and T 2 DM that have reported 5 -year outcomes Hb. A 1 c ≤ 6. 5% w/o medications 26 Hb. A 1 c ≤ 6% w/o medications Pareek M, et al. J Am Coll Cardiol 2018; 71: 670 -87.

27
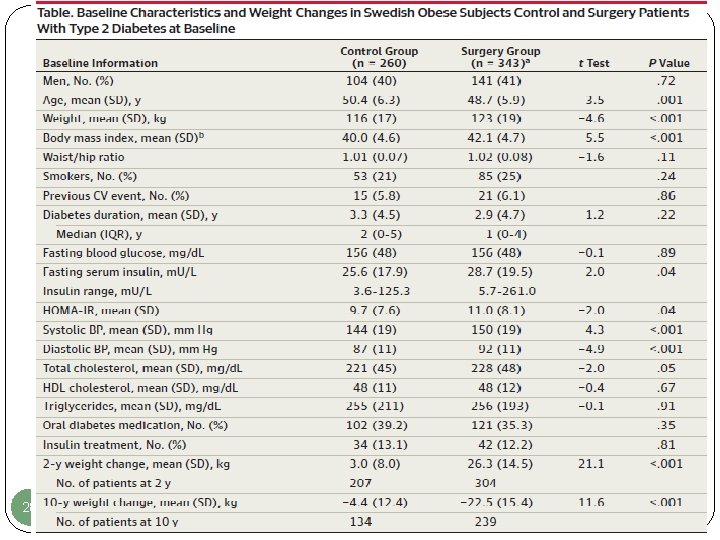
28
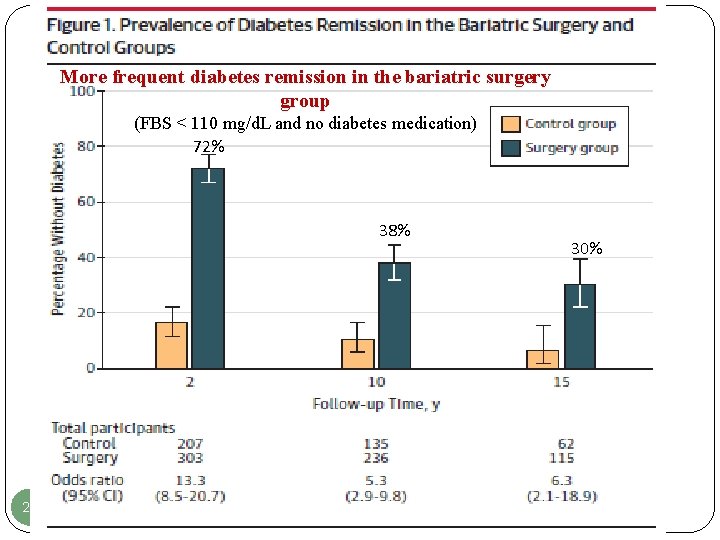
More frequent diabetes remission in the bariatric surgery group (FBS < 110 mg/d. L and no diabetes medication) 72% 38% 29 30%
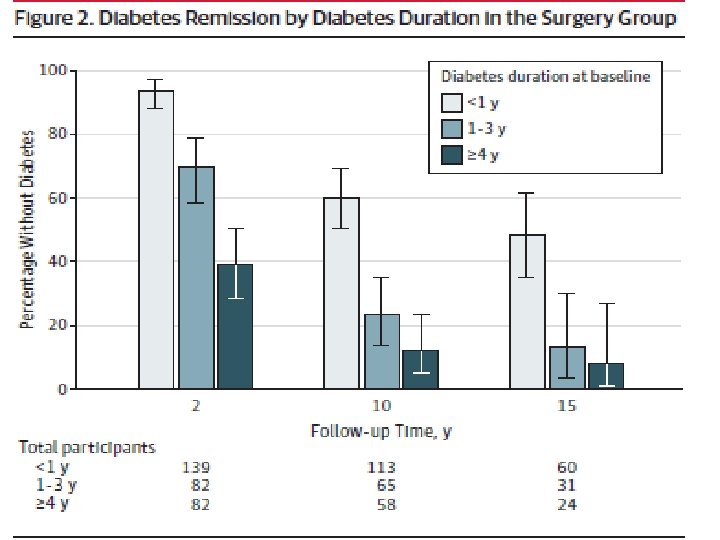
30
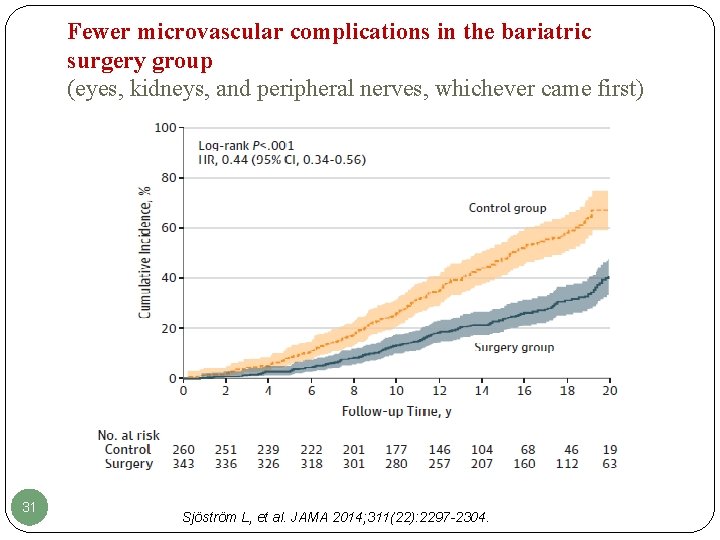
Fewer microvascular complications in the bariatric surgery group (eyes, kidneys, and peripheral nerves, whichever came first) 31 Sjöström L, et al. JAMA 2014; 311(22): 2297 -2304.
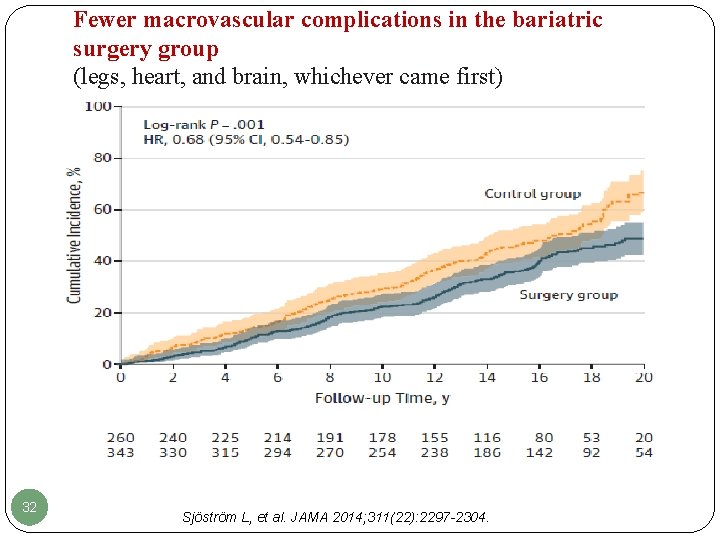
Fewer macrovascular complications in the bariatric surgery group (legs, heart, and brain, whichever came first) 32 Sjöström L, et al. JAMA 2014; 311(22): 2297 -2304.
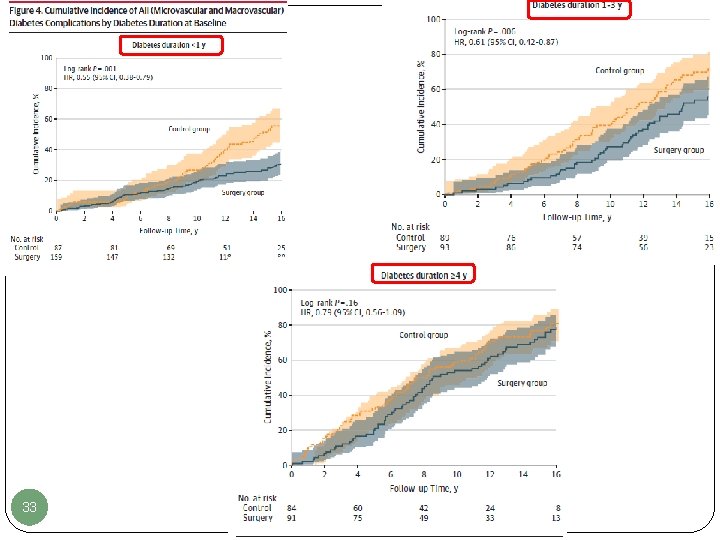
33
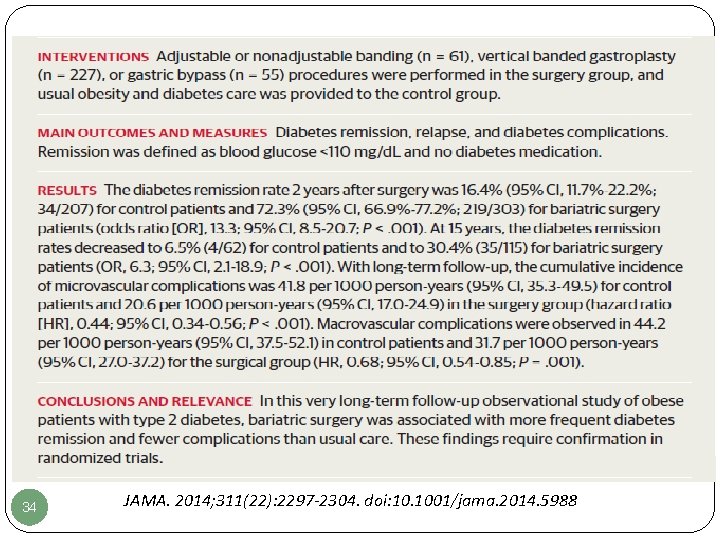
34 JAMA. 2014; 311(22): 2297 -2304. doi: 10. 1001/jama. 2014. 5988
35 JAMA, January 4, 2012—Vol 307, No. 1
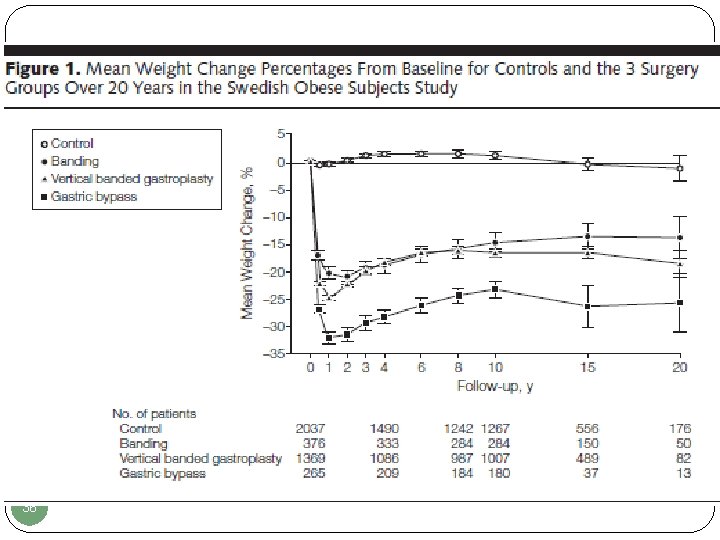
36
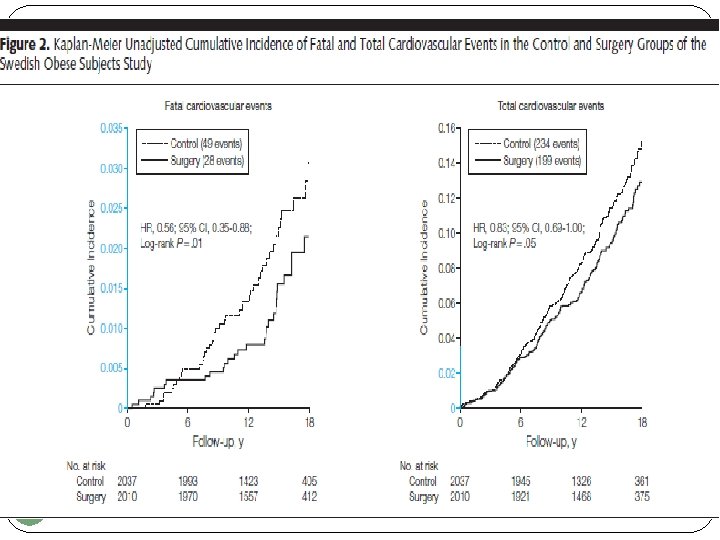
37
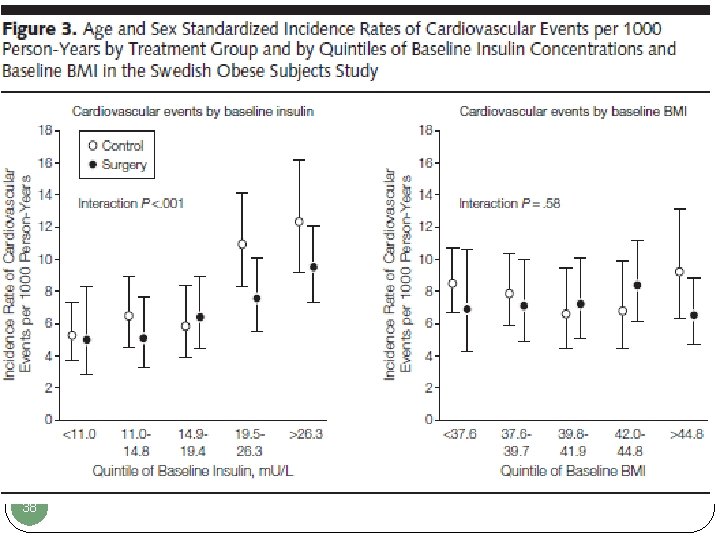
38
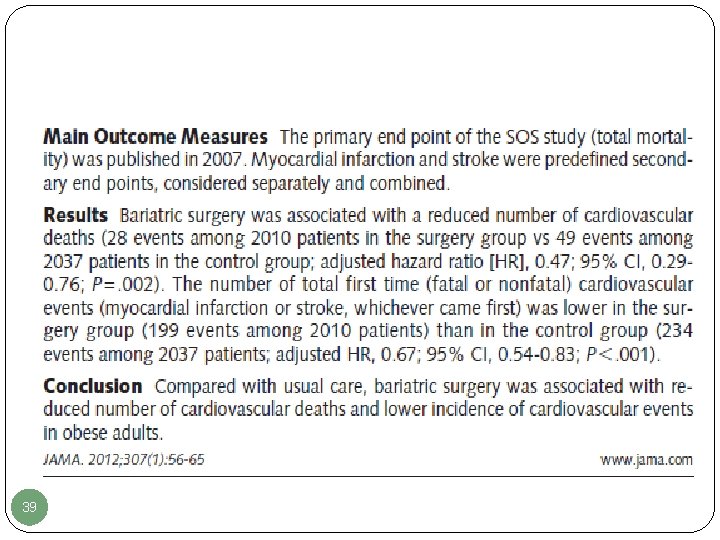
39

40
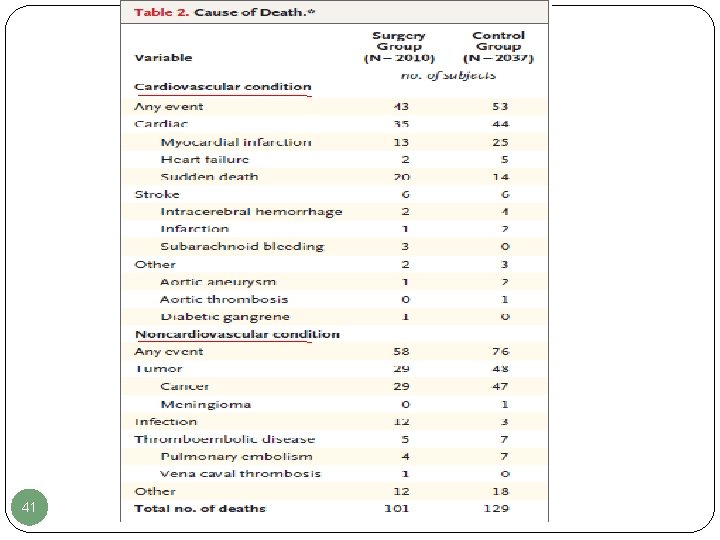
41
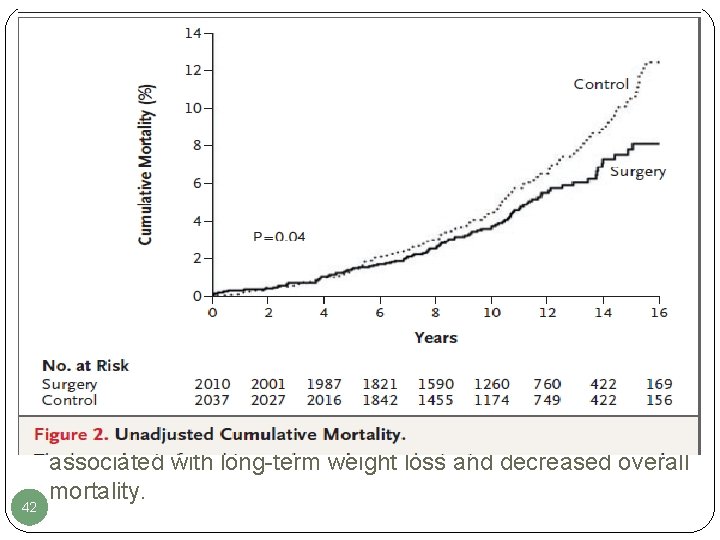
42 Conclusions: Bariatric surgery for severe obesity is associated with long-term weight loss and decreased overall mortality.

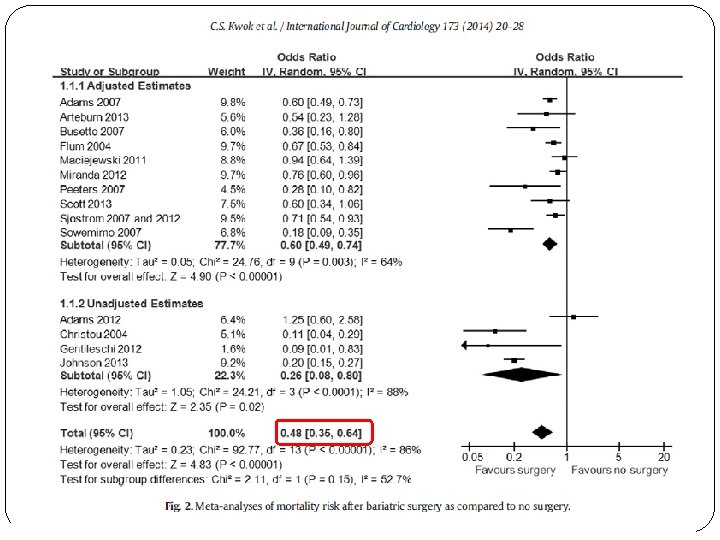
§ 43 Characteristics of included studies: § 14 cohort studies including 29, 208 patients who underwent bariatric surgery and 166, 200 nonsurgical controls. § Mean age: 48 years, 30% male § Follow up period: 2 -14. 7 years § Four studies were considered at moderate-high risk of bias, whilst ten studies were at moderate or lower risk of bias. Kwok CS, et al. Int J Cardiol 2014; 173: 20 -28.
44
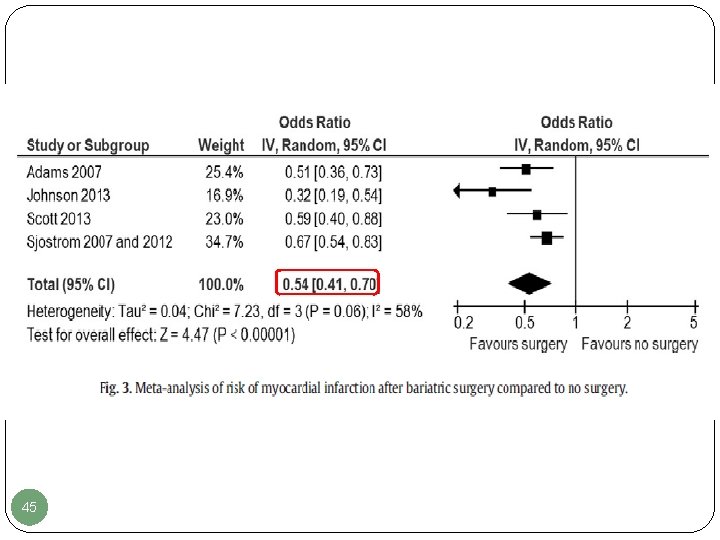
45
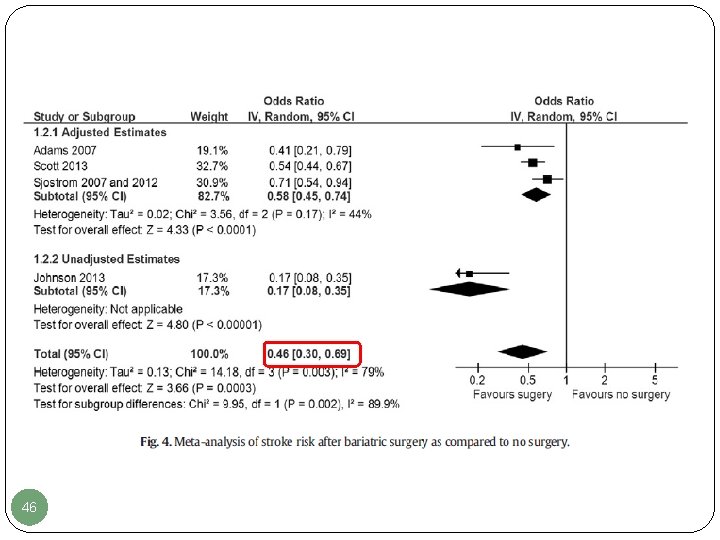
46
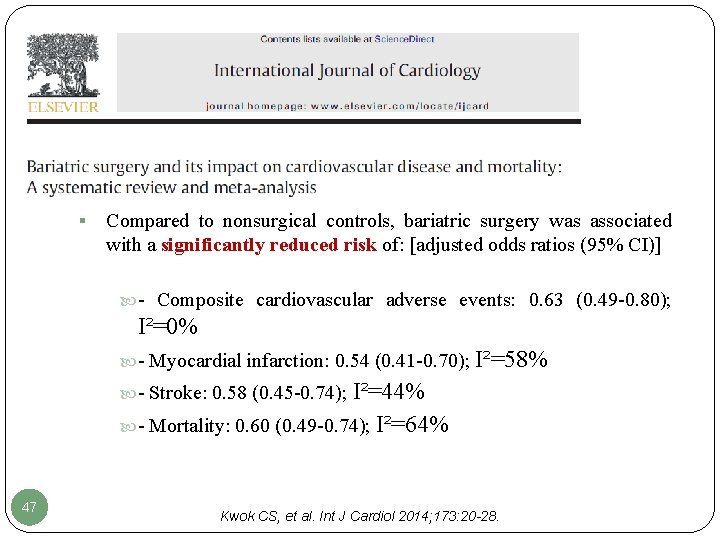
§ Compared to nonsurgical controls, bariatric surgery was associated with a significantly reduced risk of: [adjusted odds ratios (95% CI)] - Composite cardiovascular adverse events: 0. 63 (0. 49 -0. 80); I²=0% - Myocardial infarction: 0. 54 (0. 41 -0. 70); I²=58% - Stroke: 0. 58 (0. 45 -0. 74); I²=44% - Mortality: 0. 60 (0. 49 -0. 74); I²=64% 47 Kwok CS, et al. Int J Cardiol 2014; 173: 20 -28.

Conclusions: Data from different studies indicates that patients undergoing bariatric surgery have a reduced risk of CV risk factors (DM, HTN, HLP ) also hard outcomes such as MI, stroke, other cardiovascular events and mortality compared to non-surgical controls. This intervention also reduced incidence of T 2 DM, HLP and HTN. Future randomized studies should investigate whether 48 these observations are reproduced in a clinical trials

What is TOTS (Tehran Obesity Treatment Study) ? TOTS is an ongoing, single-institution, prospective study commencing March 2013. The TOTS enrolls patients to undergo a bariatric procedure based on an individualized clinical decision plan. It is organized into 4 phases: Øpreoperative evaluation Øoperation Øshort-term follow-up 49 Ølong-term follow-up

Inclusion criteria: Age 15 -75 years BMI levels ≥ 40 kg/m 2 35<BMI<40 kg/m 2 with a medical comorbidity Failure of intensive medical treatment for at least 1 year Acceptable surgical risk Able and willing to provide informed consent and assure regular follow-up. 50

Exclusion criteria: Obesity due to a treatable medical disease (eg, endocrine abnormality) High operative risk Contraindication to bariatric surgery or weight loss Active drug addiction Nursing, pregnant, or intending to become pregnant in the following year 51
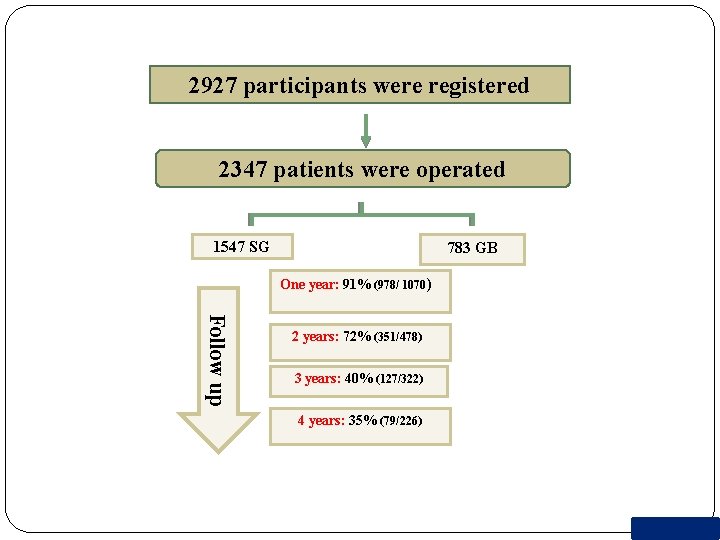
2927 participants were registered 2347 patients were operated 1547 SG 783 GB One year: 91% (978/ 1070) Follow up 2 years: 72% (351/478) 3 years: 40% (127/322) 4 years: 35% (79/226)

Published data: 1. Bariatric Surgery for Morbid Obesity: Tehran Obesity Treatment Study (TOTS) Rationale and Study Design. JMIR Res Protoc. 2016 Jan 20; 5(1) 2. Safety and effectiveness of sleeve gastrectomy versus gastric bypass: one-year results of Tehran Obesity Treatment Study (TOTS). Gastroenterol Hepatol Bed to Bench. 2016 Dec; 9(Suppl 1) 3. Comparison of the Effect of Gastric Bypass and Sleeve Gastrectomy on Metabolic Syndrome and its Components in a Cohort: Tehran Obesity Treatment Study (TOTS). Obes Surg. 2017 Jul; 27(7) 4. Severe fatal protein malnutrition and liver failure in a morbidly obese patient after mini-gastric bypass surgery: Case report. Int J Surg Case Rep. 2017; 33: 71. 5. Biopsy-proven progressive fatty liver disease nine months post mini-gastric bypass surgery: A case study. Int J Surg Case Rep. 2017 Aug 18; 39: 168 6. Nonalcoholic Fatty Liver Disease and Liver Fibrosis in Bariatric Patients: Tehran Obesity Treatment Study (TOTS). Hepat Mon. 2018 May 7. Prevalence of Micronutrient Deficiencies Prior to Bariatric 53 Surgery: Tehran Obesity Treatment Study (TOTS) Obesity Surgery 2018 March

A total of 425 patients from a prospectively collected database of morbid obese subjects between 18 and 65 years of age undergoing a primary bariatric procedure from March 2013 to September 2015 were included. Statistical analysis was performed using general estimation equation and propensity scores, and odds ratios were calculated. 54
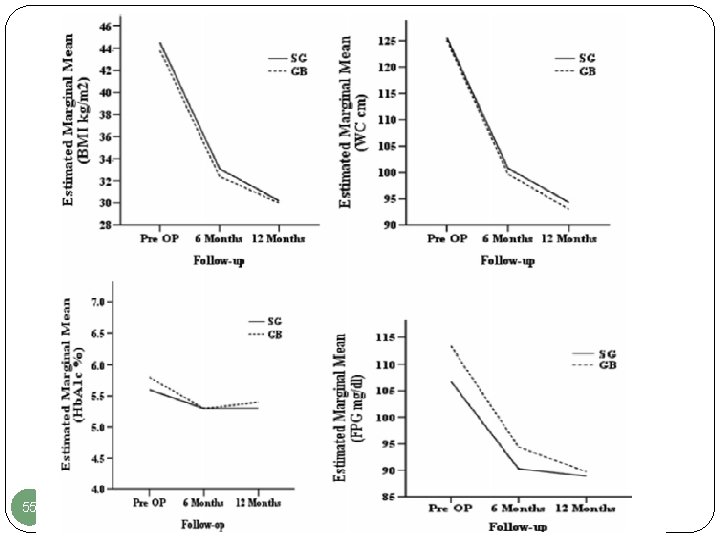
55
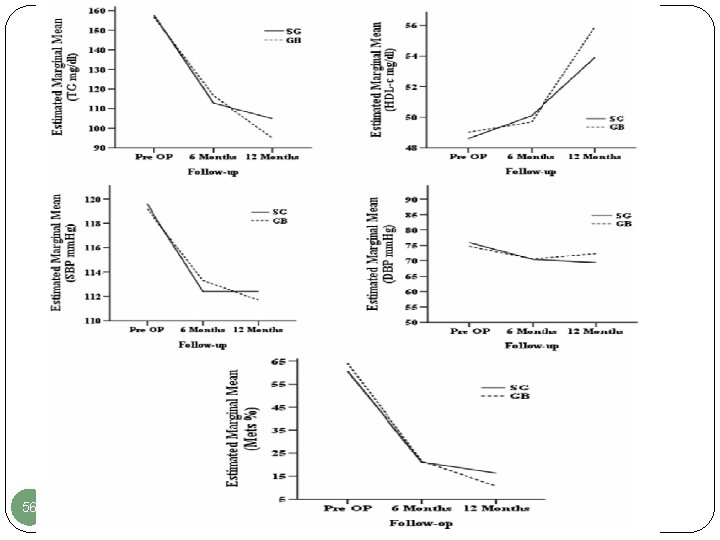
56

57 Thanks for your attention.

Thanks for your attention. 58

Study population This study has recruited 3407 participants as of 3407 December 2017 and is ongoing. From these, 3021 patients undergoing bariatric 3021 procedure. 59
- Slides: 59