OUTBREAK INVESTIGATION Definition Occurrence of more cases of

OUTBREAK INVESTIGATION

Definition • Occurrence of more cases of disease than expected • Nosocomial outbreak-any group of illnesses of common etiology occurring in patients of a medical care facility acquired by exposure of those patients to the disease agent while confined in such a facility.

Reasons to investigate • • • Control/prevention Research opportunities Training Public, political, or legal concerns Program considerations

Control/prevention • Where are we in the outbreak? – Goals will be different depending on answer(s) • Cases continuing to occur – Goal: prevent further cases – Assess population at risk, implement control measures • Outbreak appears to be coming to an end – Goal: prevent future outbreaks – Identify factors contributing to outbreak, implement measures to prevent similar events in the future

Research opportunities • Gain additional knowledge • Opportunity to study natural history of the disease • Newly recognized disease – Define natural history – Characterize the population at risk • Well recognized diseases – Assess impact of control measures – Usefulness of new epidemiology and laboratory techniques

Training • Requirements of an epidemiologist! – Diplomacy – Logical thinking – Problem solving ability and quantitative skills – Epidemiologic know-how – Judgment • Pair a new epidemiologist with an experienced epidemiologist

Public, political, or legal concerns • Sometimes override scientific concerns • Health department needs to be responsible and responsive to public concerns – Even if the concern has little scientific basis

Program considerations • Outbreak of disease targeted by a public health program – Reveal a weakness and opportunity to change or strengthen the program • Identify population that may have been overlooked • Failure of intervention strategy • Changes in the agent • Events beyond scope of the program

Steps of an Outbreak Investigation

1. Preparation • Investigation – Scientific knowledge • Review literature • Consult experts • Sample questionnaires – Supplies • Consult with laboratory – Equipment • Laptop, camera etc.

Preparation cont. • Administration-assure personnel resources, funding – Travel arrangements (orders) – Approval – Personal matters • Consultation-make sure you know your role and its parameters – Lead investigator or just lending a hand? – Know who to contact when you arrive

2. Establish existence of an outbreak • Is an outbreak truly occurring? – True outbreak – Sporadic and unrelated cases of same disease – Unrelated cases of similar unrelated disease • Determine the expected number of cases before deciding whether the observed number exceeds the expected number

Establish existence of an outbreak cont. • Comparing observed with expected – through surveillance records for notifiable diseases – hospital discharge data, registries, mortality statistics – data from other facilities, states, surveys of health care providers – community survey

3. Verify the Diagnosis • Ensure proper diagnosis and rule out lab error as the bias for increased diagnosis – Review clinical findings, lab results • Summarize clinical findings with frequency distributions – Characterize spectrum of disease – Verify diagnosis – Develop case definition

Verify the Diagnosis cont. • See and talk with patients if at all possible – Better understand clinical features – Mental image of disease and the patients affected – Gather critical information • • • Source of exposure What they think caused illness Knowledge of others with similar illness Common denominators Helpful in generating ideas for hypothesis about etiology and spread

4 a. Establish a case definition • Case definition – Standard set of criteria for deciding whether an individual should be classified as having the health condition of interest – Includes clinical criteria and restrictions by time, place and person – Must be applied consistently and without bias to all persons under investigation – Must not contain an exposure or risk factor you want to test

4 a. Establish a case definition cont. • Classification – Definite (confirmed) • Laboratory confirmed – Probable • Typical clinical features without lab confirmation – Possible (suspected) • Fewer of the typical clinical features

4 a. Establish a case definition cont. • Early in investigation may use a “loose” case definition – Better to collect more than necessary so you don’t need to make repeat visits – Identify extent of problem and population affected – Generating hypotheses • Later when hypotheses are sharpened investigator may “tighten” case definition

4 b. Identify and count cases • Target health care facilities where diagnosis likely to be made – Enhanced passive surveillance e. g. letter describing situation and asking for reports – Active surveillance e. g. phone or visit facility to collect information • Alerting the public – Media alert to avoid contaminated food product and seek medical attention if symptoms arise

4 b. Identify and count cases cont. • OB population restricted and large proportion of cases are unlikely to be diagnosed e. g. on a cruise ship – Survey entire population • Always ask case-patients if they know of any others ill with the same symptoms

4 b. Identify and count cases cont. • Information to be collected about every case – Identifying information • Re-contact if additional questions come up • Notification of lab results and outcomes of investigation • Check for duplicate records • Map geographic extent – Demographics • Provide “person” characteristics for defining population at risk

4 b. Identify and count cases cont. • Information to be collected about every case cont. – Clinical findings • Verify case definition met • Chart time course • Supplemental date e. g. deaths – Risk factor information • Tailored to specific disease in question – Reporter information • Id of person making report

4 b. Identify and count cases cont. • Collection forms – Standard case report form – Questionnaire – Data abstraction form • Line listing – Abstraction of selected critical items from above forms – Contains key information

5. Perform Descriptive Epidemiology • After collection of data characterize the outbreak by: – Time – Place – Person

Time • Epidemic curve – Histogram of the number of cases by their date of onset – Visual display of the outbreak’s magnitude and time trend – Where you are in the time course of the outbreak – Future course? – Probable time period of exposure – Helps in development of questionnaire focusing on that time period – Common source vs. Propagated
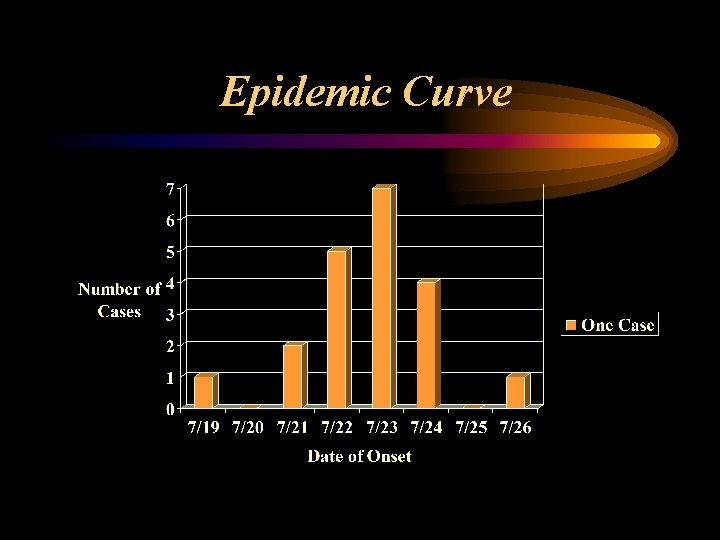
Epidemic Curve

Place • Geographic extent of problem • Clusters or patterns providing important etiologic clues • Spot maps – Where cases live, work or may have been exposed

Person • Determine what population at risk • Usually define population by host characteristics or exposure • Use rates to identify high-risk groups – Numerator = number of case – Denominator = number of people at risk

6. Develop Hypotheses • Hypotheses should address – Source of the agent – Mode of transmission • Vector or vehicle – Exposure that caused disease

Develop Hypotheses • Generating the hypothesis – What do you know about the disease? • Reservoir, transmission, common vehicles and known risk factors – Talk to several case-patients • Use open ended questions • Ask lots of questions – Talk to local health department staff – Use descriptive epidemiology e. g. epi curve

7. Test Hypotheses • Evaluate the credibility of your hypotheses – Compare with established facts • When clinical, lab, environmental and/or epi data undoubtedly support hypothesis – Use analytic epidemiology to quantify relationships and explore the role of chance • Cohort studies • Case control studies

Cohort studies start with an exposure and go forward to diseases. Drawing by: Nick Thorkelson

7. Test Hypotheses cont. • Cohort – – Small, well defined population Contact each attendee and ask a series of questions Ill Vs not ill Look for source exposure • Attack rate is high among those exposed • Attack rate is low among those not exposed • Most of the cases were exposed, so that the exposure could explain most, if not all, of the cases • Relative risk = measure of association between exposure and disease

Case-control studies start with a disease and go back to exposures. Drawing by: Nick Thorkelson

7. Test Hypotheses cont. • Case-control – Population not well defined – Case patients and comparison group (controls) questioned about exposure(s) – Compute measure of association = Odds Ratio • Quantify relationship between exposure and disease

8. Refine hypotheses and do additional studies • Epidemiologic – When analytical epi unrevealing need to reconsider your hypotheses – Go back and gather more information – Conduct different studies • Laboratory – Additional tests • Environmental studies

9. Implement Control /Prevention Measures • Implement control measures as soon as possible • May be aimed at agent, source, or reservoir • Short or long term

10. Communicate the Findings • Orally within facility/community – Local health authorities and persons responsible for implementation of control and prevention measures • Written reports (consider publication) for planning, record of performance, legal issues, reference, adding to knowledge base
- Slides: 38