Other Blood Groups Lewis Kell Duffy Kidd Ii

Other Blood Groups Lewis, Kell, Duffy, Kidd, Ii, MNSs & P

Introduction p Over 500 blood group antigens p “High incidence”, “public” or “high frequency” antigens are those present on almost every person’s red blood cells p “Low incidence”, “private” or “low frequency” antigens are present on very, very few individuals red blood cells

Introduction p Each known antigen initially identified through the detection of its specific antibody in the serum. p Knowledge of serologic behavior and characteristics of blood group antibodies is CRITICAL for identification

Introduction p Essential when evaluating antibody screen and panel studies. p Considerations given to: n Phase of reactivity n Antibody class involved n Ability to cause HDFN and HTR

Major Blood Group Systems p Lewis p I p P p MNSs p Kell p Kidd p Duffy

Lewis System p Major antigens Lea and Leb , other antigens include Lec, Led and Lex p Antigens ARE NOT intrinsic to RBCs but are absorbed from the plasma and inserted into RBC membrane.
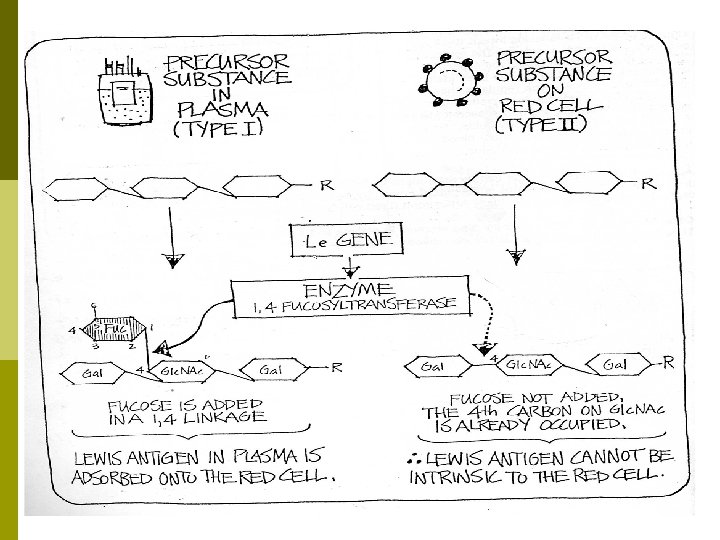

Lewis System p p Antigenic Development n Genetic control reside in single gene “Le” n Amorph le, if homozygous will not have Lewis antigens n Lea formed first, then modified to form Leb which is adsorbed preferentially over Lea Lewis phenotype of RBC can be changed by incubating with plasma containing Lea or Leb glycoplipid.
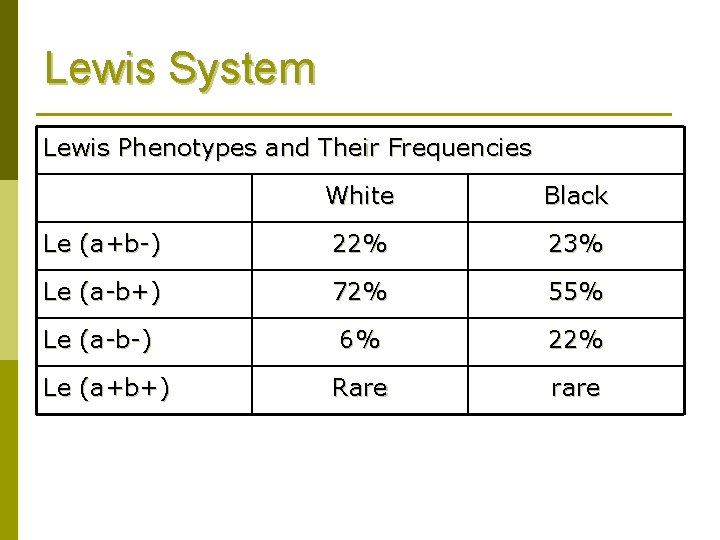
Lewis System Lewis Phenotypes and Their Frequencies White Black Le (a+b-) 22% 23% Le (a-b+) 72% 55% Le (a-b-) 6% 22% Rare rare Le (a+b+)

Lewis System p Lewis antigens in infants n Antigens absent or extremely weak at birth n Expression of Leb gradual p Birth Le (a-b-) p 2 months Le(a+b-) p 12 to 18 months Le(a+b+) p 2 to 3 years Le (a-b+)

Lewis System p Lewis antigens and pregnancy n Antigen strength may decline dramatically n Transiently Le (a-b-) may produce Lewis antibodies during pregnancy n Antigens return after delivery and antibodies disappear

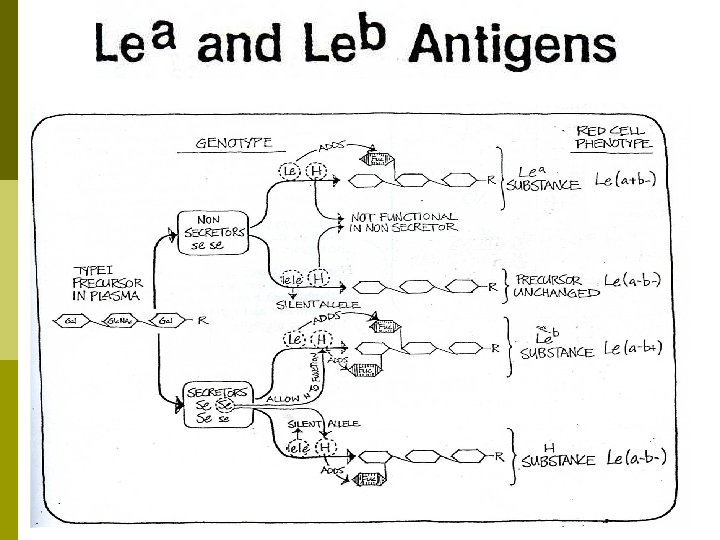
Lewis System p Interaction of Le, Se and H Genes n lele will not have Lewis antigens, but if Se present will have A, B and H in secrections n Genotype se/se and have one Lewis antigen will have Lea in their secretions but no A, B or H.
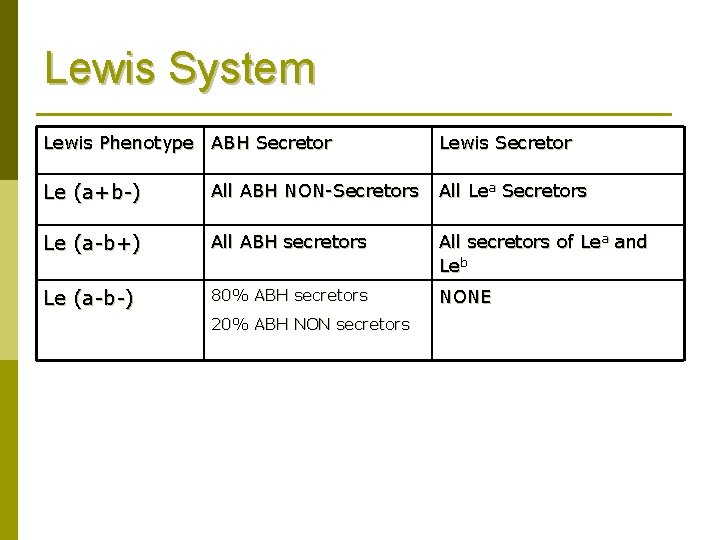
Lewis System Lewis Phenotype ABH Secretor Lewis Secretor Le (a+b-) All ABH NON-Secretors All Lea Secretors Le (a-b+) All ABH secretors All secretors of Lea and Leb Le (a-b-) 80% ABH secretors NONE 20% ABH NON secretors

Lewis System p Lewis Antibodies n Almost always Ig. M, react strongly at RT, may cause ABO discrepancy if reverse cells have Lewis antigen. n Occur almost exclusively in Le (a-b-) and production of anti-Lea AND –Leb not unusual n Anti-Lea frequently encountered, anti-Leb rarely encountered.


Lewis System p Lewis Antibodies n Although most react at RT reactivity may be seen at 37 C, but is weaker and may be weakly reactive at AHG n Can bind complement and cause IN-VITRO hemolysis, most often with enzyme treated cells n Because antibodies are Ig. M and antigens are poorly developed at birth antibodies NOT implicated in HDFN.


Lewis System p Lewis antibodies n Can be neutralized in-vitro by additions of Lewis Substance p p p Le antigens are present in secretions Add to serum with Lewis antibodies and the antibodies will be bound to the soluble Lewis antigens Useful when multiple antibodies are present and 1 is a Lewis, eliminates the activity of the antibody

Lewis Antibodies p Anti-Le a, Anti-Le b, Anti-Lex p Most react at room temperature or below - p Often fix complement p Some in vitro hemolysis p Le a may cause HTR

Lewis Antibodies p Anti-Le a p Found in Lea-b- secretors p best room temperature or below p Often fix complement p Some in vitro hemolysis p Le a may cause HTR

Lewis Antibodies p Anti-Le b p Often found with Anti-Lea p Most react at room temperature or below p Two types - Anti-Leb. H and Anti-Leb. L p Rare cause of HTR

Lewis Antibodies p Anti-Lex p Most react at room temperature or below - p Reacts with both Lea and Leb as a single antibody

Lewis Antibodies p Special Problems in the Blood Bank n Lewis antigens may be weaker during pregnancy and women produce antibodies n Can neutralize Lewis antibodies with Lewis plasma n Pregnant woman with room temperature antibodies, neutralize with Lewis antigen when testing for HDN antibodies

Lewis System p Transfusion Practice n Transfused RBCs will acquire the Lewis phenotype of the recipient within a few days n Lewis antibodies in patient will be neutralized by Lewis substance in donor plasma n Lewis antibodies rarely cause in-vivo hemolysis n It is not necessary to phenotype donors for Lewis antigens prior to transfusion, give crossmatch compatible

The Kell Blood Group System

Background information p The Kell blood group system was discovered in 1946. p Number of Kell antigens: > 20 p These antigens are third most potent, after those of the ABO and Rh blood groups, at triggering an immune reaction.

Molecular information p The KEL gene is found on chromosome 7 p The KEL gene is highly polymorphic, with different alleles at this locus encoding the 25 antigens that define the Kell blood group. p The Kell protein is a polypeptide chain of 732 amino acids in length that becomes glycosylated at five different sites. It makes a single pass through the RBC membrane.
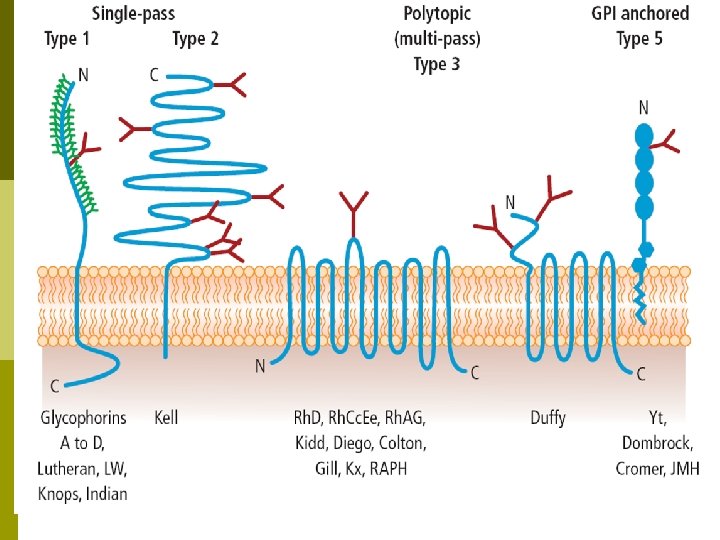

Kell Blood Group System p XK gene produces Kx substance, which is a precursor of of Kell Ags p Kel genes convert Kx substance into the Kell Ags on RBCs p K (Kell) & k (cellano) are produced by allelic genes, this results into 3 phenotypes: p p K+k- (genotype KK) K+k+ (genotype Kk) K-k+ (genotype kk) Other allelic genes include: Kpa/Kpb, Jsa/Jsb
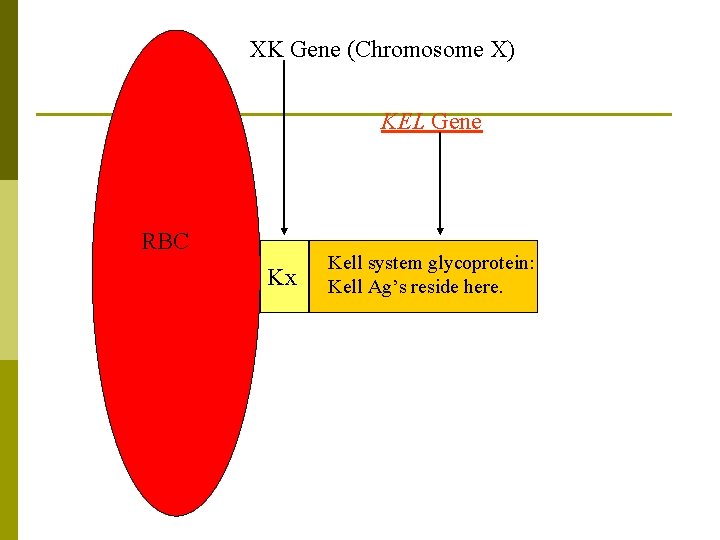
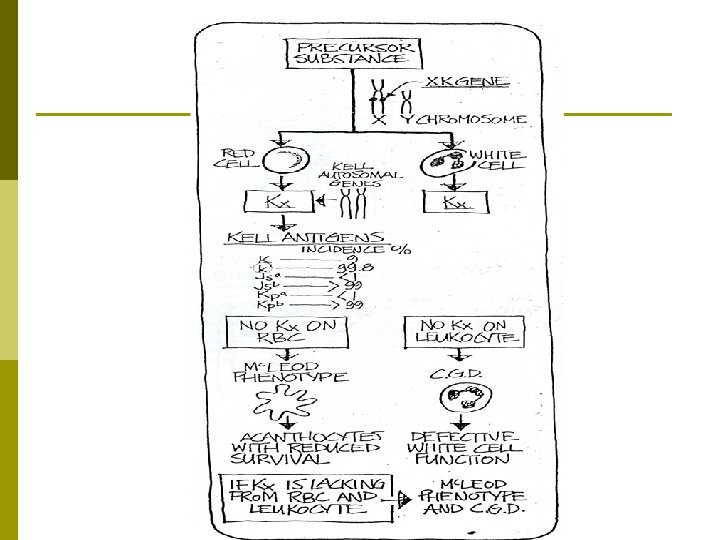
XK Gene (Chromosome X) KEL Gene RBC Kx Kell system glycoprotein: Kell Ag’s reside here.
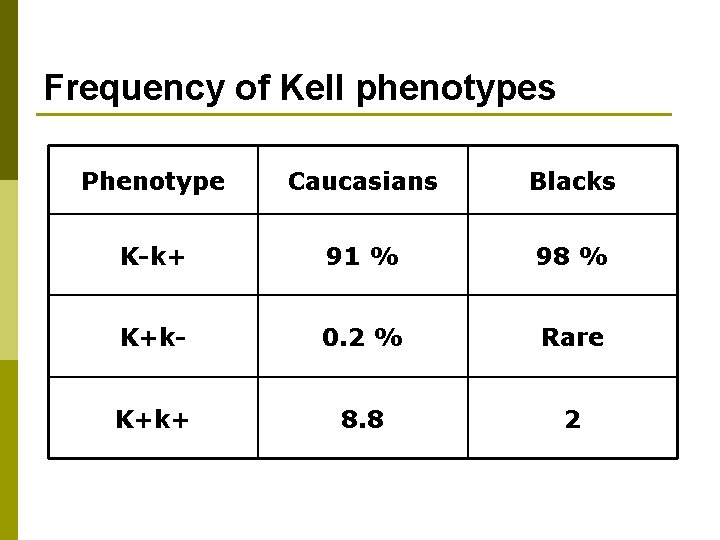
Frequency of Kell phenotypes Phenotype Caucasians Blacks K-k+ 91 % 98 % K+k- 0. 2 % Rare K+k+ 8. 8 2

Kx Substance p Kx substance is present on RBCs & WBCs p Kell genes convert Kx substance into the Kell Ags on RBCs p Kell genes do not convert Kx on WBCs
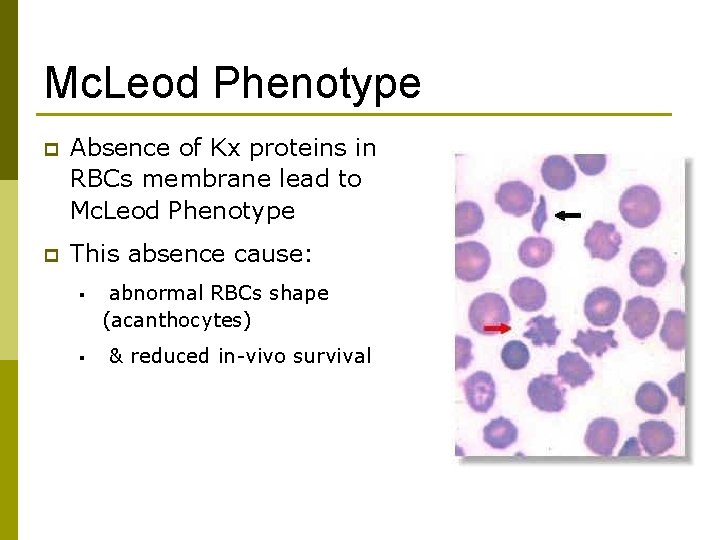
Mc. Leod Phenotype p Absence of Kx proteins in RBCs membrane lead to Mc. Leod Phenotype p This absence cause: § § abnormal RBCs shape (acanthocytes) & reduced in-vivo survival

Chronic Granulomatous Disease p Absence of Kx proteins in WBCs cause CGD p Leukocytes are able to phagocytose but not to kill bacteria p Patients with CGD have recurrent bacterial infections p Patients who lack Kx on RBCs & WBCs have both Mcleod and CGD

Kell Antibodies p K- individuals produce anti-K when exposed to K+ cells n p Frequency of K+ is low (9%), easy to find blood On the other hand frequency of k is 99. 9% n k- individuals produce anti-k when exposed to k+ cells n Difficult to find blood

Antibodies produced against Kell antigens Kell Abs Clinically Significant Abs class Yes Ig. G (rarely) Ig. M Thermal range HDNB 4 - 37 Yes Transfusion Reactions Extravascular Intravascular Yes Rare

Duffy Blood Group System

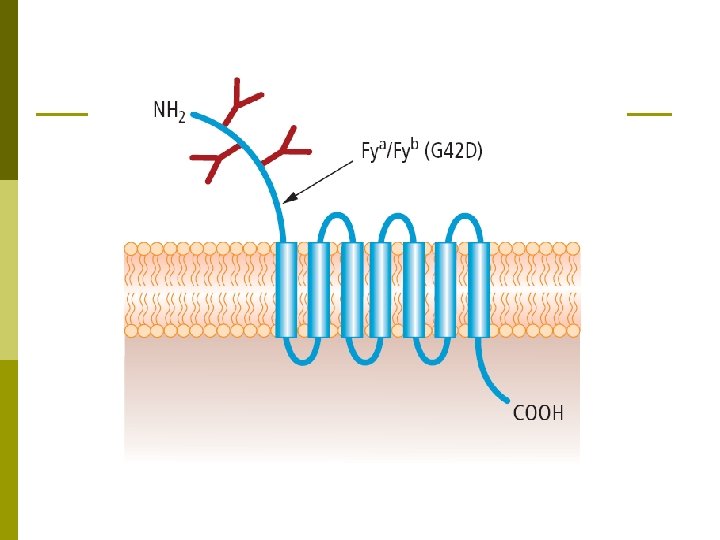
Duffy Blood Group System p The Duffy blood group was discovered in 1950. p The Duffy glycoprotein is encoded by the FY gene, found on chromosome 1 , of which there are two main alleles, FYA and FYB. They are codominant. p The Duffy gene codes for a glycoprotein also found in other tissues: brain, kidney, spleen, heart and lung. p The Duffy glycoprotein is a transmembrane protein p Five alleles at Duffy locus, the most important: Fya, Fyb & Fy (Silent Allele) p Fya is more immunogenic than Fyb
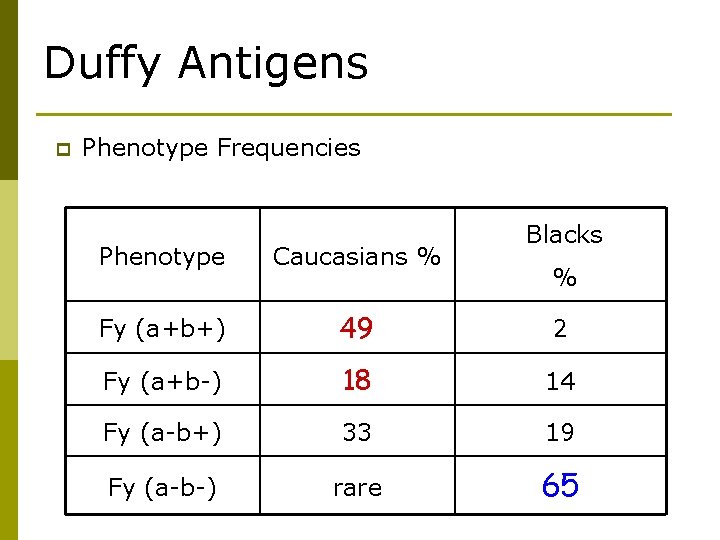
Duffy Antigens p Phenotype Frequencies Blacks Phenotype Caucasians % Fy (a+b+) 49 2 Fy (a+b-) 18 14 Fy (a-b+) 33 19 Fy (a-b-) rare 65 %

Different genes p Fy(a-b-) blacks do not produce anti-Fya or anti-Fyb following transfusion with Fy(a+) or Fy(b+) blood p Fy(a-b-) Caucasians become sensitized following transfusion with Fy(a+) or Fy(b+) blood p This suggest that Fy(a-b-) phenotype arises from different genes in the two populations

Duffy Antigens p Fya, Fyb antigens are Destroyed by enzymes p Abs DO NOT agglutinate enzyme treated cells p Moderately immunogenic p Fya is more immunogenic than Fyb
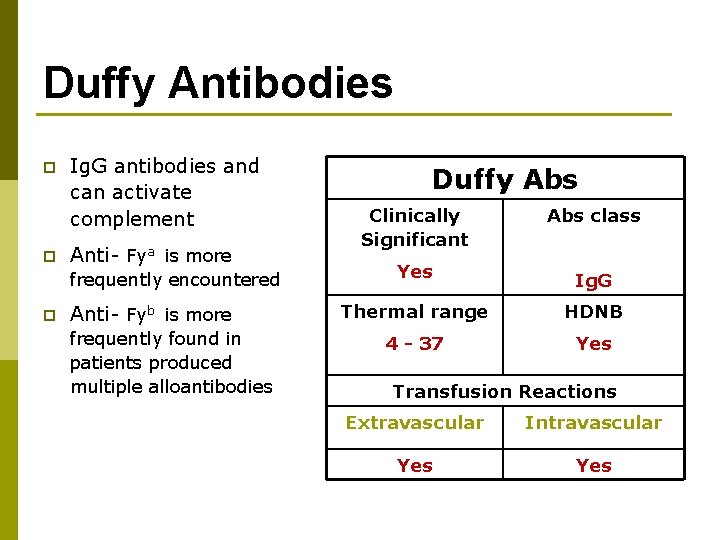

Duffy Antibodies p p Ig. G antibodies and can activate complement Anti- Fya is more frequently encountered p Anti- Fyb is more frequently found in patients produced multiple alloantibodies Duffy Abs Clinically Significant Abs class Yes Ig. G Thermal range HDNB 4 - 37 Yes Transfusion Reactions Extravascular Intravascular Yes

Duffy and Malaria p p Black people with the Duffy phenotype of Fy(a–b–) appear to have resistance to Plasmodium vivax & Plasmodium knowlesi causative agents of Malaria. n Duffy antigens appear to be a receptor for the P. vivax organism and when the antigen is not present on the red blood cell membrane P. vivax is unable to access the red blood cell n Some area’s of West Africa are 100% Fy(a–b–). Plasmodium falciparum binds to RBCs at integral glycophorin A & B
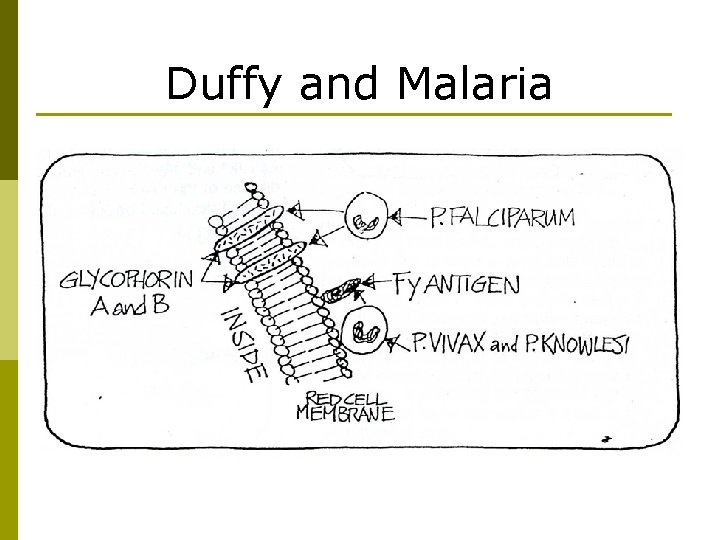
Duffy and Malaria

Kidd Blood Group System

Kidd Blood Group System p The Kidd blood group was discovered in 1950. p The Kidd gene is located on chromosome 18 p Three alleles: Jka, Jkb, Jk p n Codominant Inheritance n Jk is a silent allele (amorph) The Kidd protein is an integral protein of the RBC membrane.
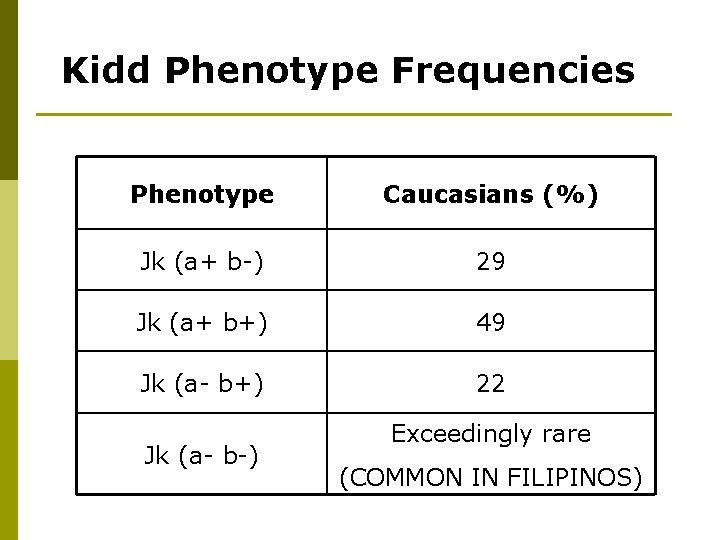

Kidd Phenotype Frequencies Phenotype Caucasians (%) Jk (a+ b-) 29 Jk (a+ b+) 49 Jk (a- b+) 22 Jk (a- b-) Exceedingly rare (COMMON IN FILIPINOS)

Phenotype Frequencies What is the purpose of learning the phenotype frequencies of each blood group antigen? – When crossmatches are required it helps the Tech know how many units to crossmatch or antigen type to find compatible blood. If a patient has anti-Jka antibody how many RBC units need to be antigen typed to find 2 compatible units? 78% of the population is positive for the antigen therefore 22% are NEGATIVE for the antigen. Approximately 2 out of 10 units are compatible. Need to antigen type 10 units.

Kidd Antigens & Antibodies p Ags are well developed at birth p Have tendency to drop to low or undetectable levels following formation. p Abs are of Ig. G type & can activate complement (Anti-Jka, Anti-Jkb ) p Produced following transfusion or pregnancy p Can cause HDNB p They are also a very common cause of delayed HTRs
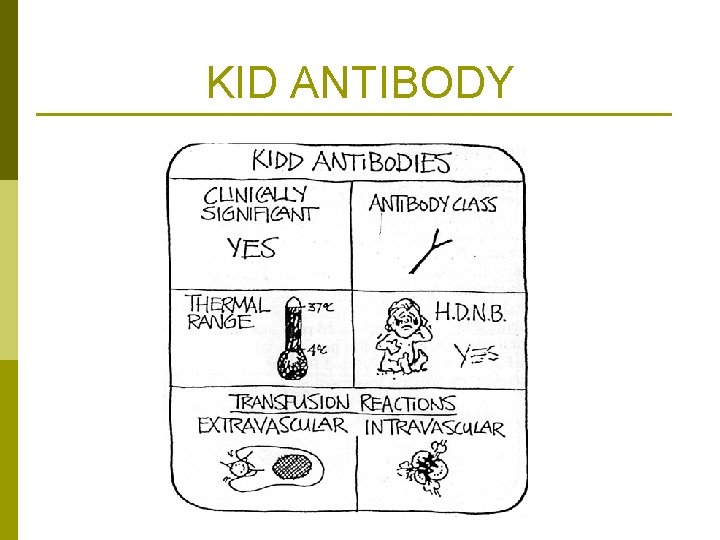
KID ANTIBODY

Ii Blood Group p Found nearly on all RBCS p Their products are transferase enzymes that attach repeating units of Gal and Glc. NAc to the ABO Precursor Substance. p Big I gene codes for branching of the Precursor Substance.

Ii Antigens p Little i antigen is LINEAR n p Big I antigen is BRANCHED n p Found on cord cells, predominantly Gradually convert from i to I during the first 18 months of life. Not all i converted to I, some i still present on adult cells, normally. Rare adult individuals termed iadult do not express i Ag on their red cells


q The I and i antigen sites are considered uncompleted ABH active chains. q When ABH are removed from RBCs more I Ags are expressed q I structure located beneath the ABH Ags
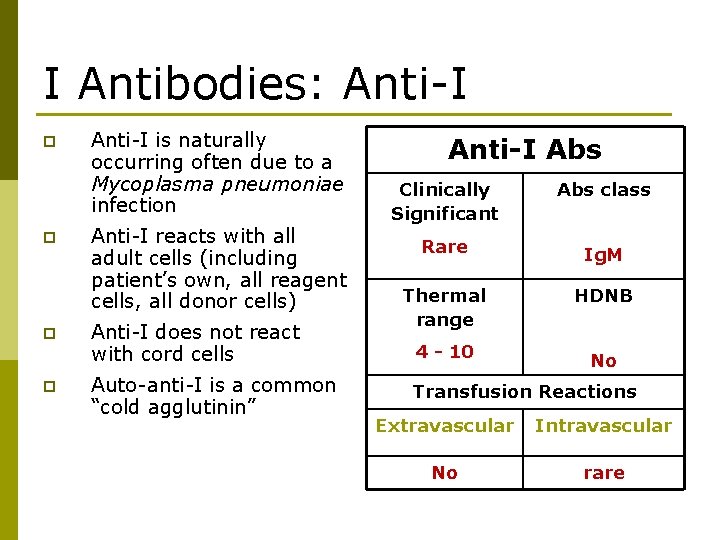
I Antibodies: Anti-I p p Anti-I is naturally occurring often due to a Mycoplasma pneumoniae infection Anti-I reacts with all adult cells (including patient’s own, all reagent cells, all donor cells) Anti-I does not react with cord cells Auto-anti-I is a common “cold agglutinin” Anti-I Abs Clinically Significant Abs class Rare Ig. M Thermal range HDNB 4 - 10 No Transfusion Reactions Extravascular Intravascular No rare

Anti i Antibodies p Anti i is rarely found in healthy individuals p Reacts preferably with cord cells p anti-i can be found secondary to Infectious Mononucleosis. n Transient: Only present with active disease

MNSs Blood Group System p The antigens M and N are produced by co-dominant alleles p closely linked to the S and s genes, which are also co-dominant. p Chromosome 4 contains these linked genes p Genes produce two distinct glycophorins or sialyglycoproteins (SGP) on the RBC membrane.

MN Genetics p p MN Locus genes produce Glycophorin A (GPA) n M-GPA’s 1 st five aa’s = Serine-Ser-Thr. Glycine n N-GPA’s 1 st five aa’s = Leucine-Ser-Thr. Glutamic acid n Amino acids (aa) 2, 3 & 4 are the same for both Glycophorin A (GPA) is a glycoprotein also known as MN-sialoglycoprotein
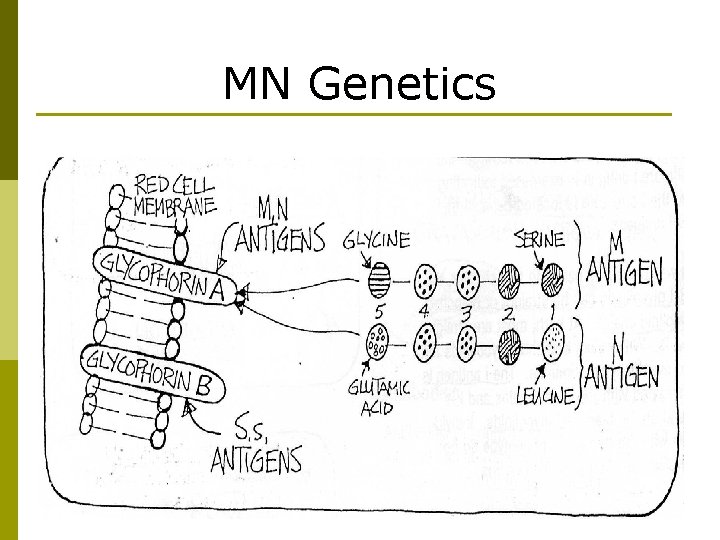
MN Genetics
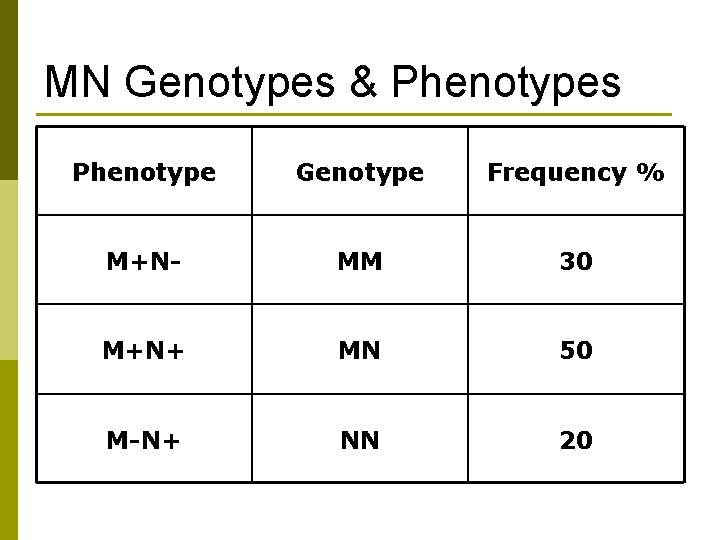
MN Genotypes & Phenotypes Phenotype Genotype Frequency % M+N- MM 30 M+N+ MN 50 M-N+ NN 20
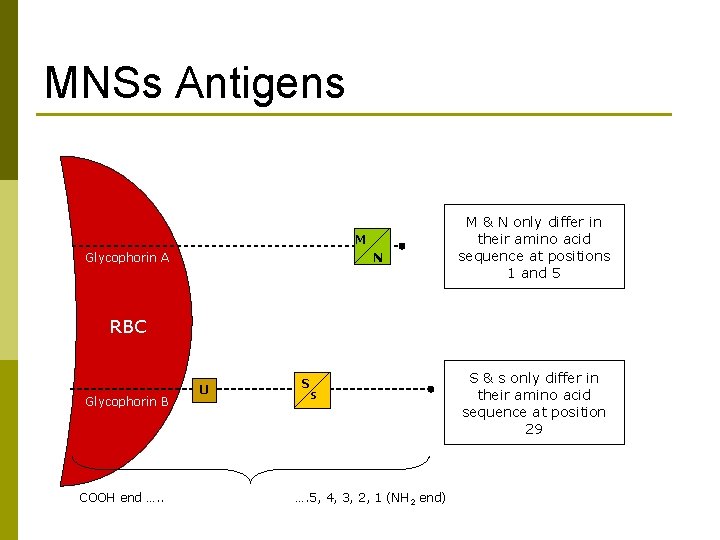
MNSs Antigens M Glycophorin A N M & N only differ in their amino acid sequence at positions 1 and 5 RBC Glycophorin B COOH end …. . U S s …. 5, 4, 3, 2, 1 (NH 2 end) S & s only differ in their amino acid sequence at position 29

Ss Genetics Ss genes code for the production of Glycophorin B(GPB) p S glycophorin B has Methionine at aa position 29 p s glycophorin B has Threonine at aa position 29 p Glycophorin B (GPB) is a glycoprotein also known as Ss-sialoglyprotein p
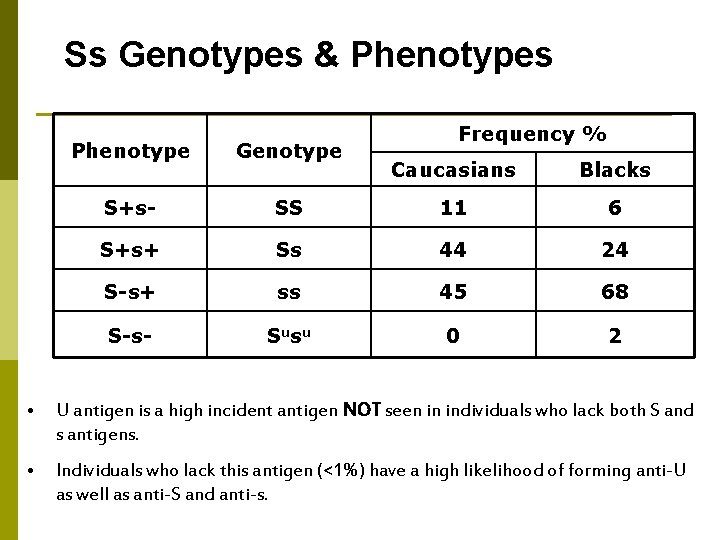
Ss Genotypes & Phenotypes Phenotype Genotype S+s- Frequency % Caucasians Blacks SS 11 6 S+s+ Ss 44 24 S-s+ ss 45 68 S-s- Susu 0 2 • U antigen is a high incident antigen NOT seen in individuals who lack both S and s antigens. • Individuals who lack this antigen (<1%) have a high likelihood of forming anti-U as well as anti-S and anti-s.

Rare Alleles p Rare low incidence alleles found on MN locus p Some may result from crossing over of genes of glycophorin A & B p Such crossing over results in hybrid sialoglycoproteins

Anti-M Antibodies p Variability of reactivity (Dosage) § § Strong reactions with RBCs homozygous for MM Weak reactions with RBCs heterozygous MN Anti-M Abs Clinically Significant Abs class Seldom Ig. G & Ig. M Thermal range HDNB 4 – 22 rare Rare 22 -37 Transfusion Reactions Extravascular Intravascular Rare No
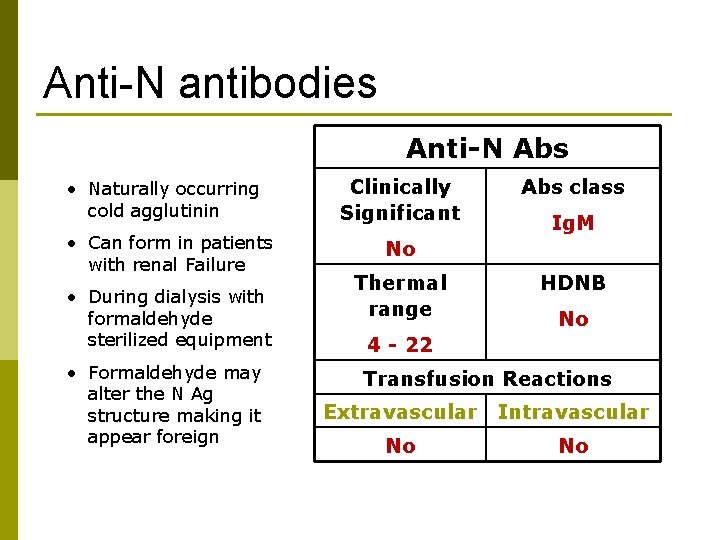

Anti-N antibodies Anti-N Abs • Naturally occurring cold agglutinin • Can form in patients with renal Failure • During dialysis with formaldehyde sterilized equipment • Formaldehyde may alter the N Ag structure making it appear foreign Clinically Significant Abs class Ig. M No Thermal range HDNB No 4 - 22 Transfusion Reactions Extravascular Intravascular No No
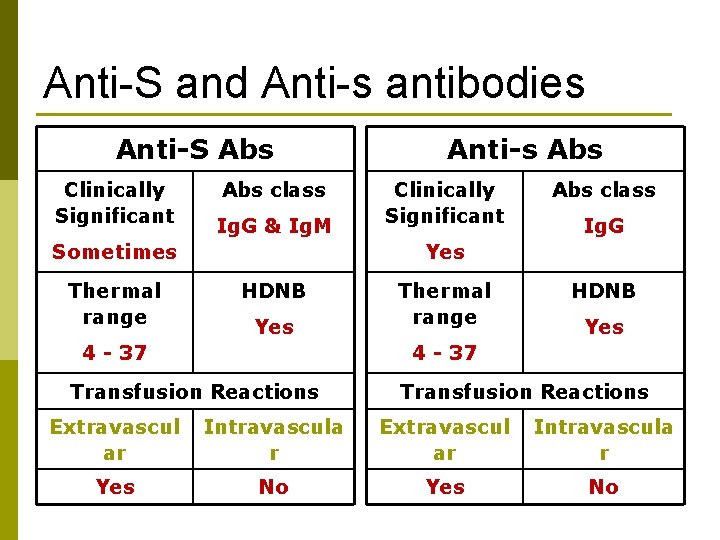
Anti-S and Anti-s antibodies Anti-S Abs Clinically Significant Abs class Ig. G & Ig. M Sometimes Thermal range Anti-s Abs Clinically Significant Abs class Ig. G Yes HDNB Yes 4 - 37 Thermal range HDNB Yes 4 - 37 Transfusion Reactions Extravascul ar Intravascula r Yes No

P Blood Group System p Genetics: These genes code for enzymes that sequentially add sugars to precursor substance. p This system is related to the ABO, Le and Ii systems. p Genes: P 1, Pk, P and lower case p (silent allele) p All antigens are expressed on glycolipids on red cells

Phenotypes, Detectable Antigens & Frequencies Phenotype Detectable Antigens Frequencies P 1, P 79% P 21% Pk 1 P, Pk Rare Pk 2 Pk Rare p N/A Rare Whites % • Pk is the precursor of P. • Rare individuals do not convert Pk into P. • Those will have Pk on RBCs.

Anti-P 1 Antibodies Naturally occcurring Abs found in the serum of P 2 Individuals Anti-P 1 Abs Clinically Significant Abs class Ig. M occasionally Thermal range HDNB 4 – 22 NO Rare 22 -37 Transfusion Reactions Extravascular Intravascular No Rare

Anti-P 1 Antibodies

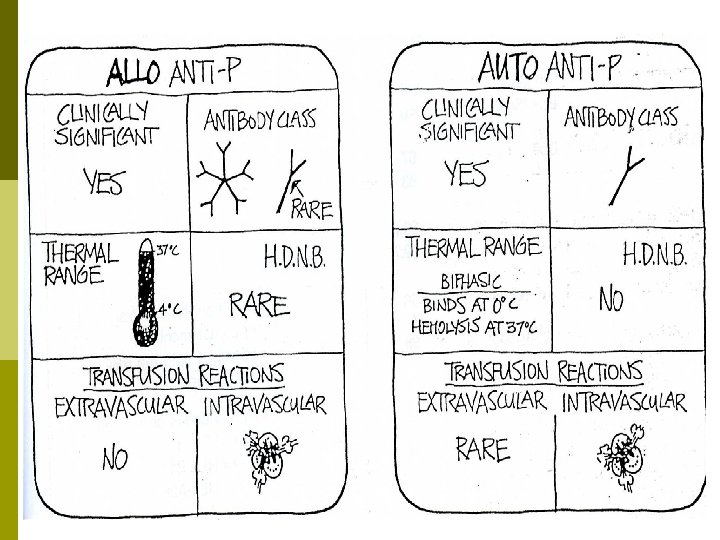
Allo Anti-P Antibodies Naturally occcurring Abs found in the serum of Pk and p Individuals Allo Anti-P Abs Clinically Significant Abs class Yes Rare Ig. G Thermal range HDNB 4 – 37 S Rare Ig. M Transfusion Reactions Extravascular Intravascular No Yes

Auto anti-P Antibodies p p It is an Ig. G biphasic Ab associated with Paroxysmal Cold Hemoglobinuria (PCH) Binds complement at cold temperatures and activates that complement in warm temperatures lysing the red blood cells. Auto Anti-P Abs Clinically Significant Abs class Ig. G Yes Biphasic HDNB Binds at 0 Rare Hemolysis 37 Transfusion Reactions Extravascular Intravascular Rare Yes

Anti Tja Antibodies p Combination of anti-P, anti-P 1 & anti-Pk p Found in serum of individuals who have no P, P 1 & Pk Ags on red cells

RARE BLOOD GROUPS

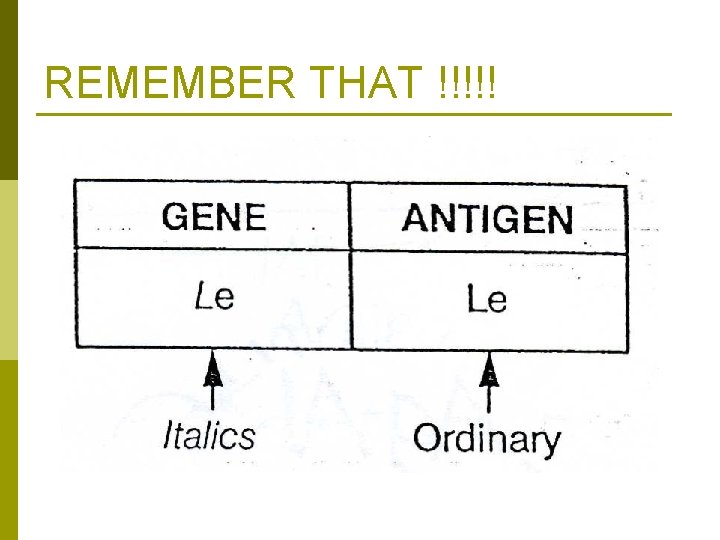
REMEMBER THAT !!!!!
- Slides: 81