Osteoporosis Moving Beyond Bone Mineral Density Tuan V

Osteoporosis: Moving Beyond Bone Mineral Density Tuan V. Nguyen Bone and Mineral Research Program Garvan Institute of Medical Research Sydney, Australia

Osteoporosis, Fracture and BMD • Fracture is the ultimate outcome of osteoporosis • Osteoporosis is defined by bone mineral density (BMD) • BMD is a good predictor of fracture risk, but a poor discriminator of fracture • There are BMD-independent predictors of fracture risk • The current definition of osteoporosis is inadequate • A probability-based definition is proposed

A Shift in Thinking Low bone mass, microarchitectural deterioration of bone tissue leading to enhanced bone fragility and a consequent increase in fracture risk (Consensus Development Conference, 1991) Osteoporosis: Risk factor Fracture: Outcome
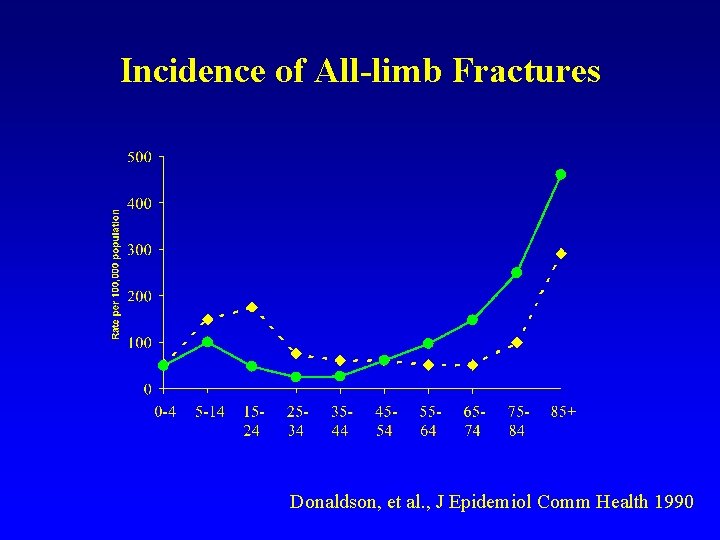
Incidence of All-limb Fractures Donaldson, et al. , J Epidemiol Comm Health 1990
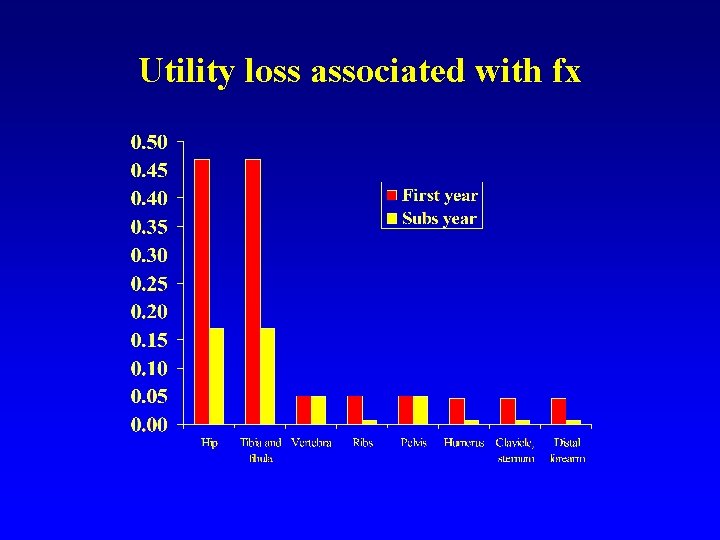
Utility loss associated with fx

Risk of Death From Hip Fracture 50 -year old women: Lifetime risk of mortality from: Hip Fracture: 2. 8% Breast Cancer: 2. 8% Endometrial Cancer: 0. 7% Cummings et al. Arch Intern Med 1989; 149: 2445 -8
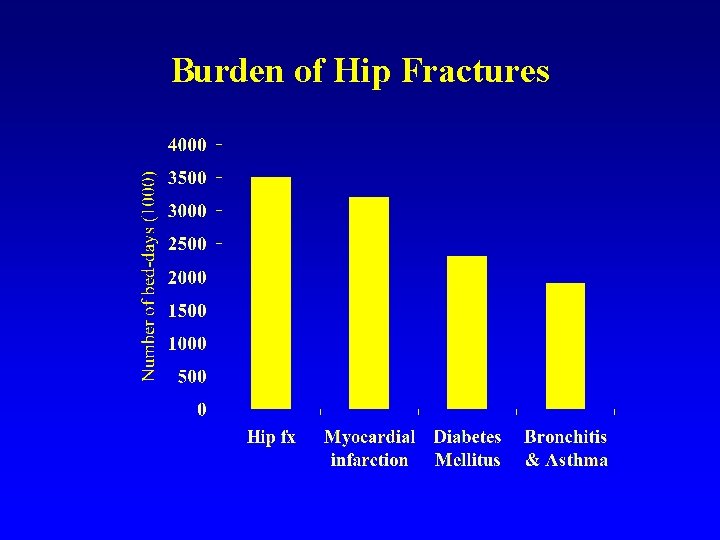
Burden of Hip Fractures

Cost of Fractures Disease Prevalence Annual Direct Cost (US$ Billion) Osteoporosis 10 million 13. 8 Asthma 15 million 7. 5 Chronic Heart Failure 4. 6 million 20. 3 National Heart Lung and Blood Institute National Osteoporosis Foundation American Heart Association

Current Status • BMD is a golden standard for assessment of osteoporosis • BMD is used as (a) selection criteria, and (b) an endpoint in clinical trials • BMD is the major focus of basic, clinical and epidemiological research in osteoporosis
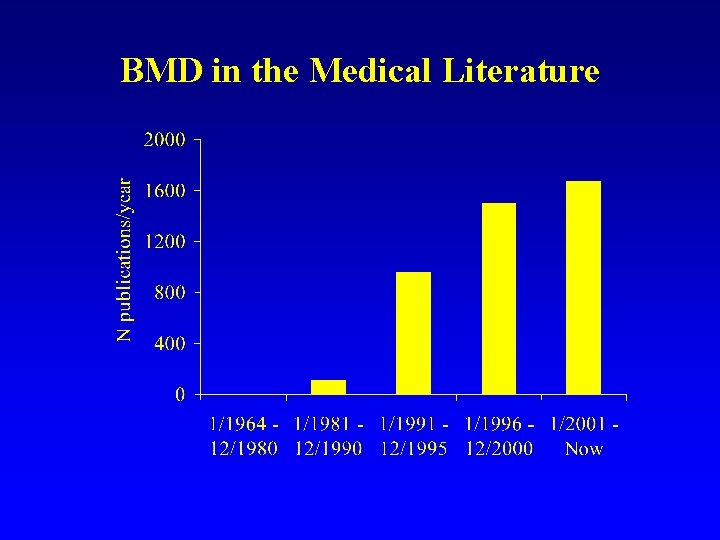
BMD in the Medical Literature
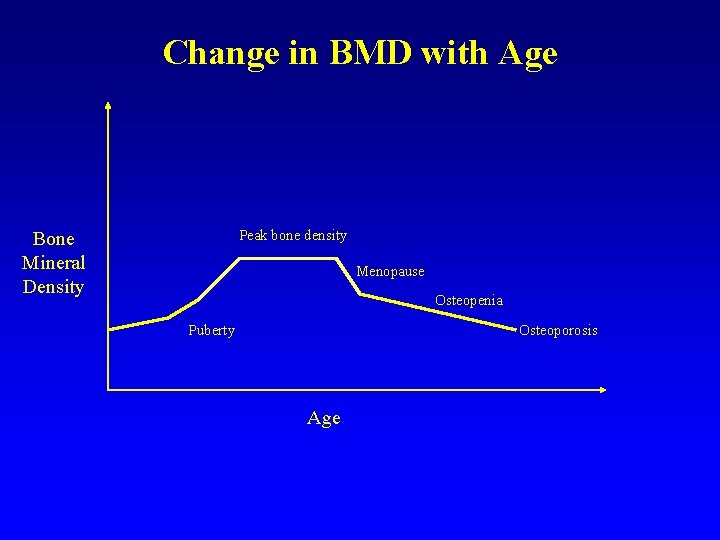
Change in BMD with Age Peak bone density Bone Mineral Density Menopause Osteopenia Puberty Osteoporosis Age

Bone Mineral Density and Definition of “Osteoporosis” Gaussian distribution Constant standard deviation Decrease with advancing age T-scorei = (BMDi – Peak BMD) / SD

The Use of T-scores • Define “osteoporosis” and “osteopenia” T-score < -2. 5 = “osteoporosis” -2. 5 < T-scores < -1 = “osteopenia” • Criteria for clinical trial entry • Intervention threshold
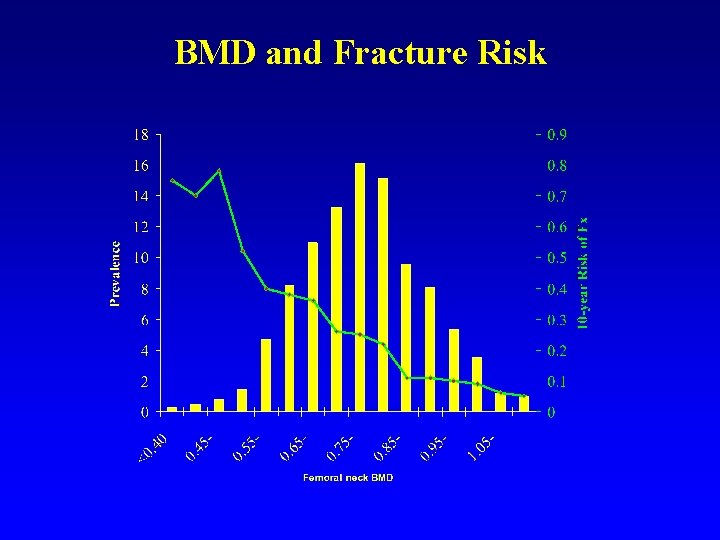
BMD and Fracture Risk
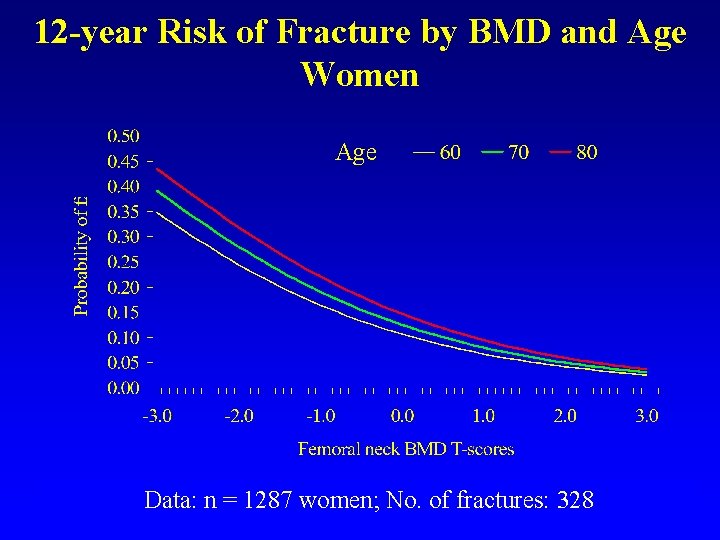
12 -year Risk of Fracture by BMD and Age Women Age Data: n = 1287 women; No. of fractures: 328
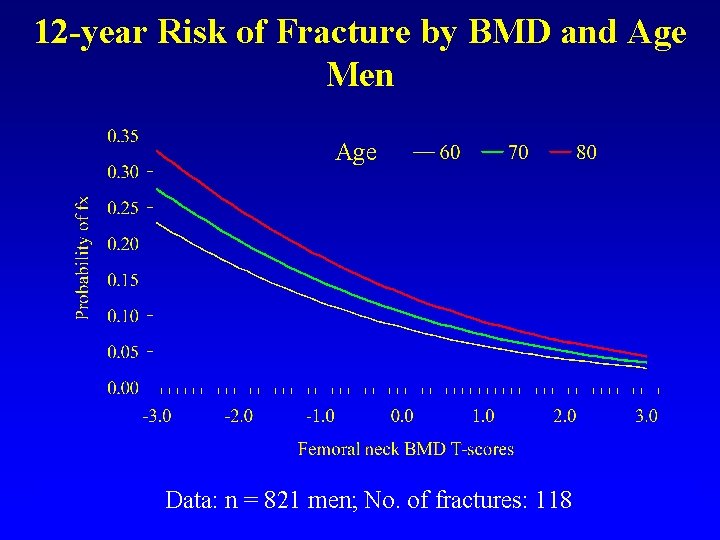
12 -year Risk of Fracture by BMD and Age Men Age Data: n = 821 men; No. of fractures: 118
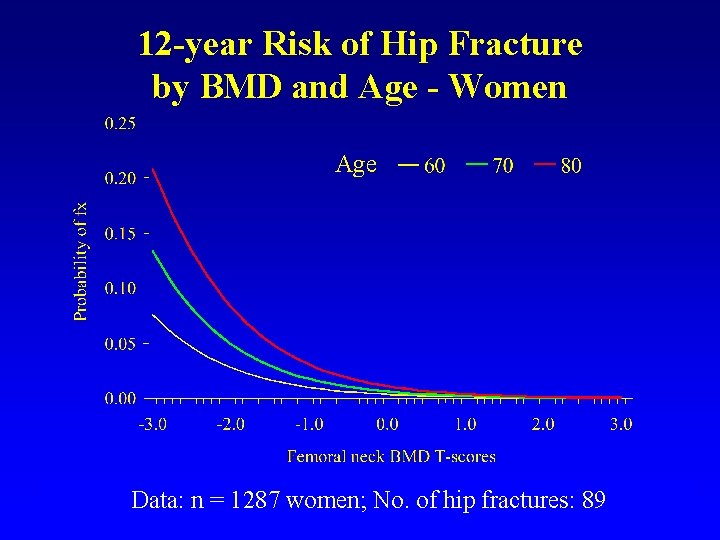
12 -year Risk of Hip Fracture by BMD and Age - Women Age Data: n = 1287 women; No. of hip fractures: 89
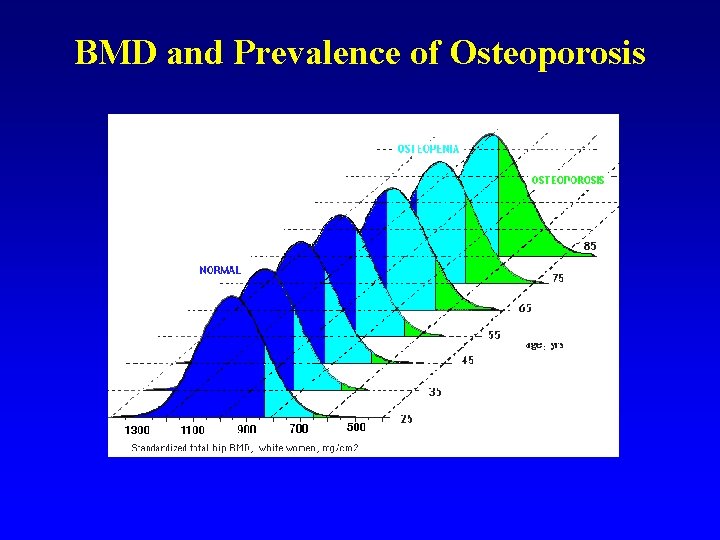
BMD and Prevalence of Osteoporosis
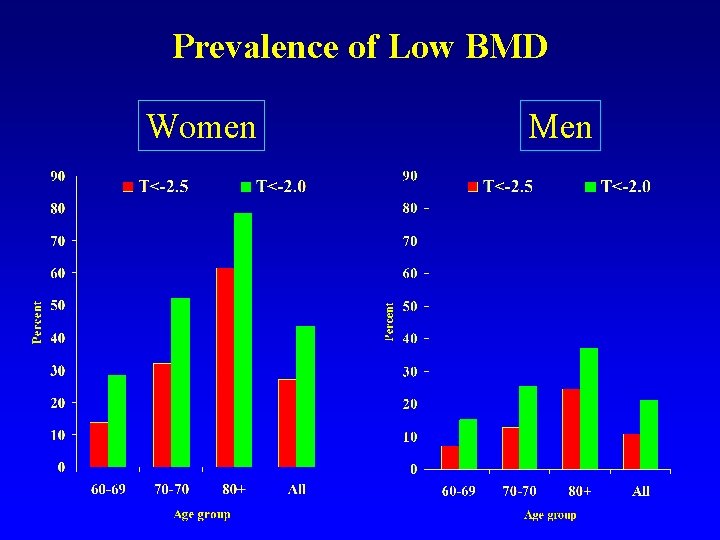
Prevalence of Low BMD Women Men

U. S Preventive Services Taskforce "… recommendation that women 65 and older be routinely screened for osteoporosis to reduce the risk of fracture and spinal abnormalities often associated with the disease. … recommends that routine screening begin at 60 for those women identified as high risk because of their weight or estrogen use. " Annals of Internal Medicine, Sept 17, 2002

Low BMD (T<-2. 5) and Fractures in Women 1287 women Low BMD 345 (27%) Fx = 137 (40%) No Fx = 208 (60%) 42% Not Low BMD 942 (73%) Fx = 191 (20%) No Fx = 751 (80%)

Low BMD (T<-2. 0) and Fractures in Women 1287 women Low BMD 562 (44%) Fx = 199 (35%) No Fx = 363 (65%) 61% Not Low BMD 725 (56%) Fx = 129 (18%) No Fx = 596 (82%)
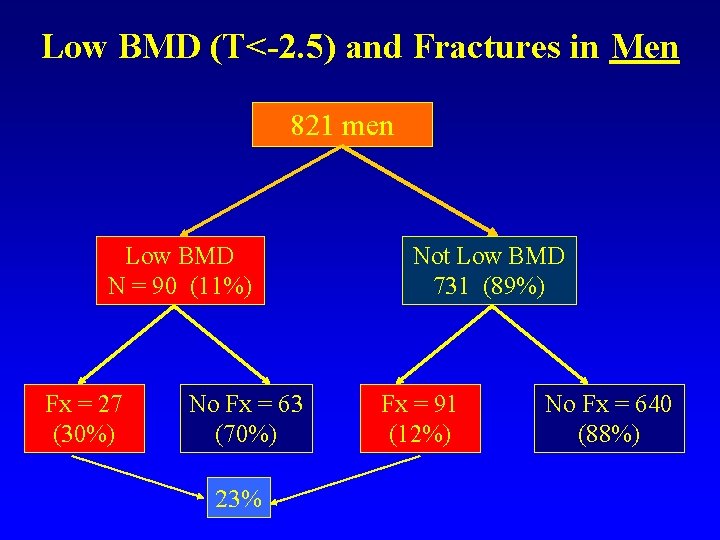
Low BMD (T<-2. 5) and Fractures in Men 821 men Low BMD N = 90 (11%) Fx = 27 (30%) No Fx = 63 (70%) 23% Not Low BMD 731 (89%) Fx = 91 (12%) No Fx = 640 (88%)
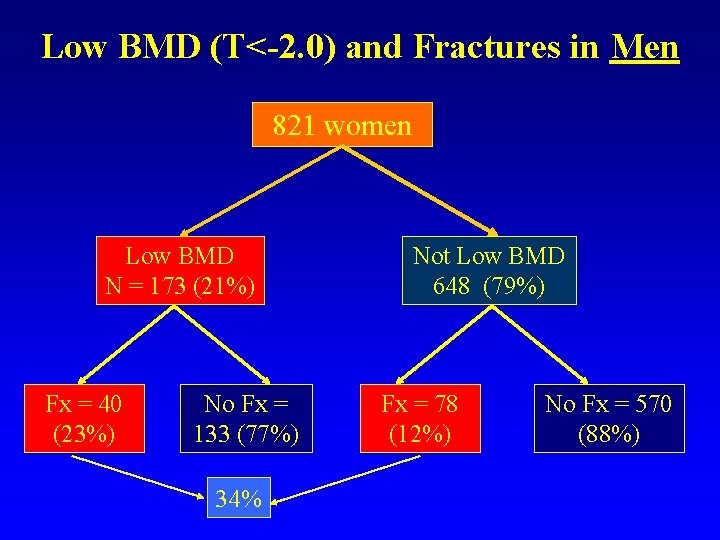
Low BMD (T<-2. 0) and Fractures in Men 821 women Low BMD N = 173 (21%) Fx = 40 (23%) No Fx = 133 (77%) 34% Not Low BMD 648 (79%) Fx = 78 (12%) No Fx = 570 (88%)
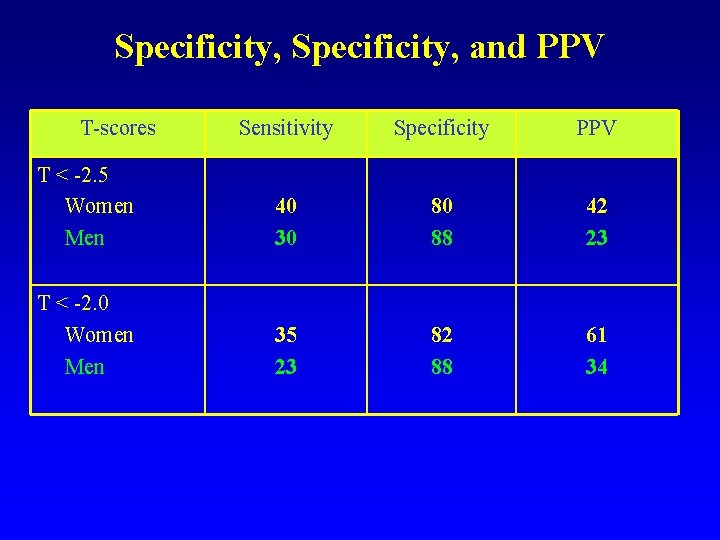
Specificity, and PPV T-scores Sensitivity Specificity PPV T < -2. 5 Women Men 40 30 80 88 42 23 T < -2. 0 Women Men 35 23 82 88 61 34
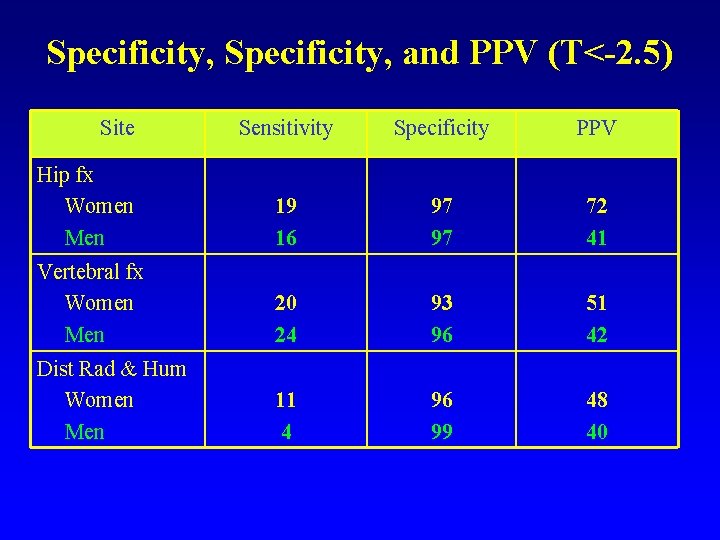
Specificity, and PPV (T<-2. 5) Site Sensitivity Specificity PPV Hip fx Women Men 19 16 97 97 72 41 Vertebral fx Women Men 20 24 93 96 51 42 Dist Rad & Hum Women Men 11 4 96 99 48 40
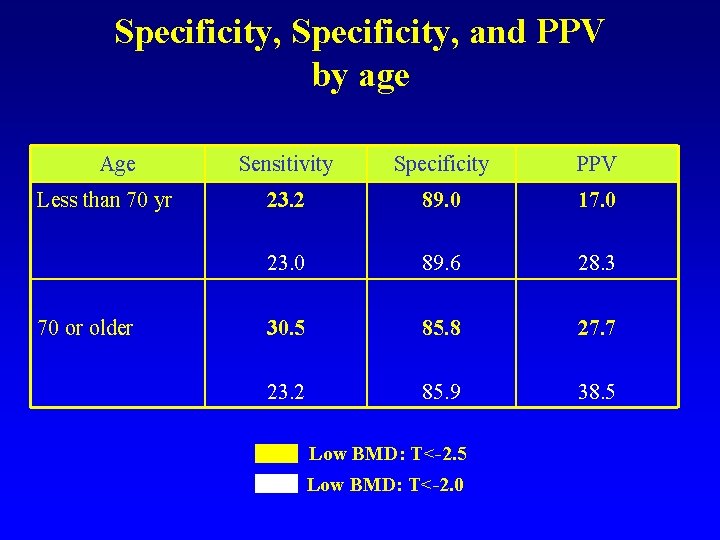
Specificity, and PPV by age Age Less than 70 yr 70 or older Sensitivity Specificity PPV 23. 2 89. 0 17. 0 23. 0 89. 6 28. 3 30. 5 85. 8 27. 7 23. 2 85. 9 38. 5 Low BMD: T<-2. 0
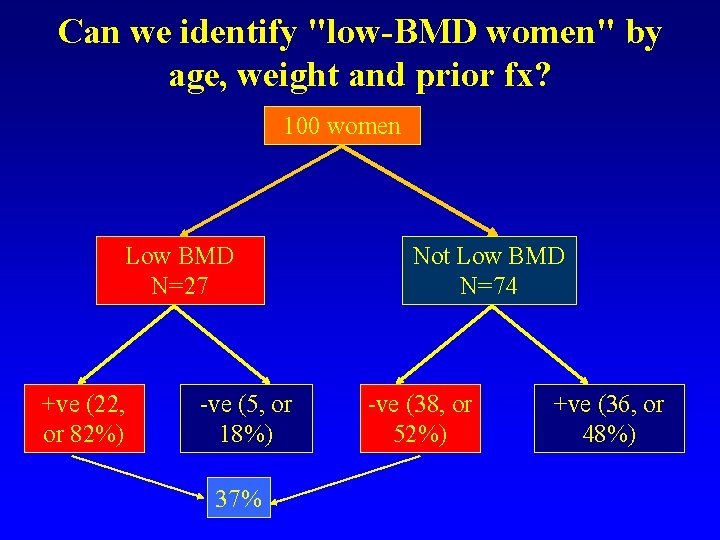
Can we identify "low-BMD women" by age, weight and prior fx? 100 women Low BMD N=27 +ve (22, or 82%) -ve (5, or 18%) 37% Not Low BMD N=74 -ve (38, or 52%) +ve (36, or 48%)
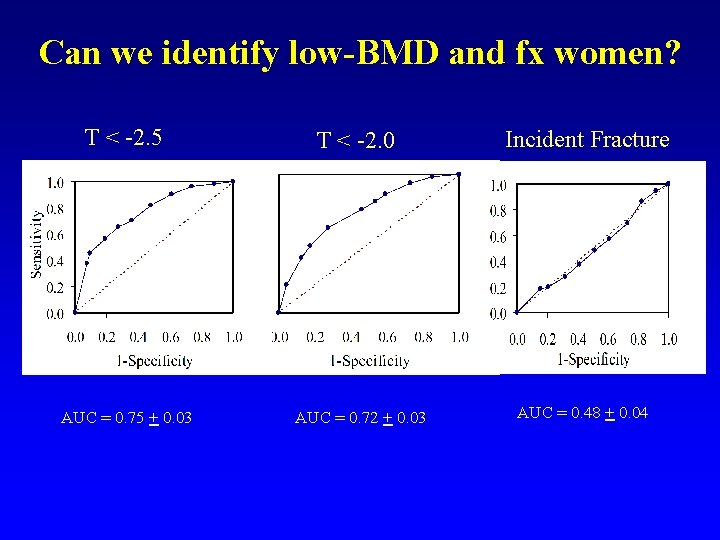
Can we identify low-BMD and fx women? T < -2. 5 AUC = 0. 75 + 0. 03 T < -2. 0 AUC = 0. 72 + 0. 03 Incident Fracture AUC = 0. 48 + 0. 04
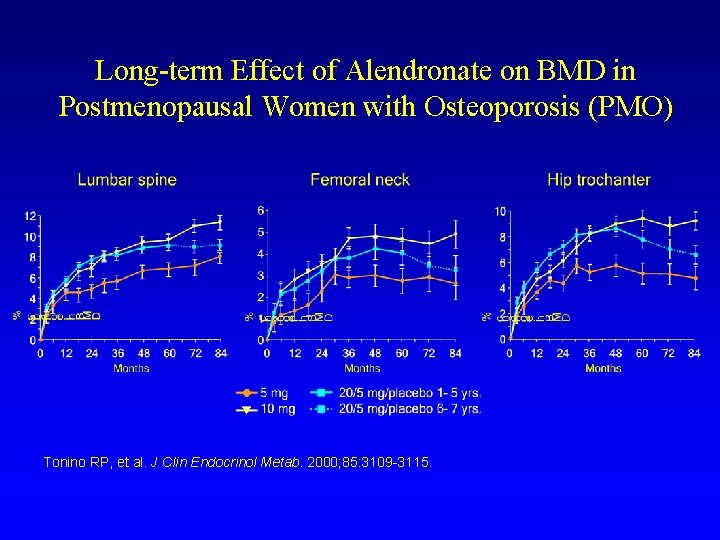
Long-term Effect of Alendronate on BMD in Postmenopausal Women with Osteoporosis (PMO) Tonino RP, et al. J Clin Endocrinol Metab. 2000; 85: 3109 -3115.

Relationships between Change in BMD and Fracture Risk • Each standard deviation lowering in BMD is associated with a 2. 5 (or higher)-fold increase in the risk of hip fracture. • An increase by 3% would be predicted to reduce fracture risk by 12%.
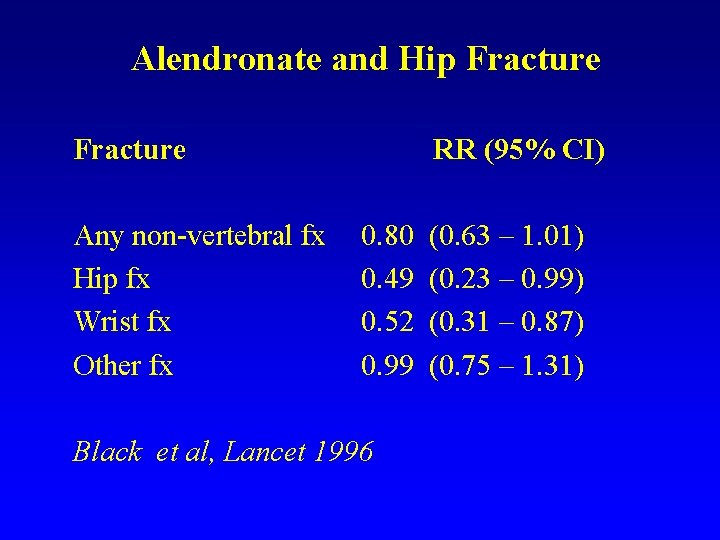
Alendronate and Hip Fracture Any non-vertebral fx Hip fx Wrist fx Other fx RR (95% CI) 0. 80 0. 49 0. 52 0. 99 Black et al, Lancet 1996 (0. 63 – 1. 01) (0. 23 – 0. 99) (0. 31 – 0. 87) (0. 75 – 1. 31)
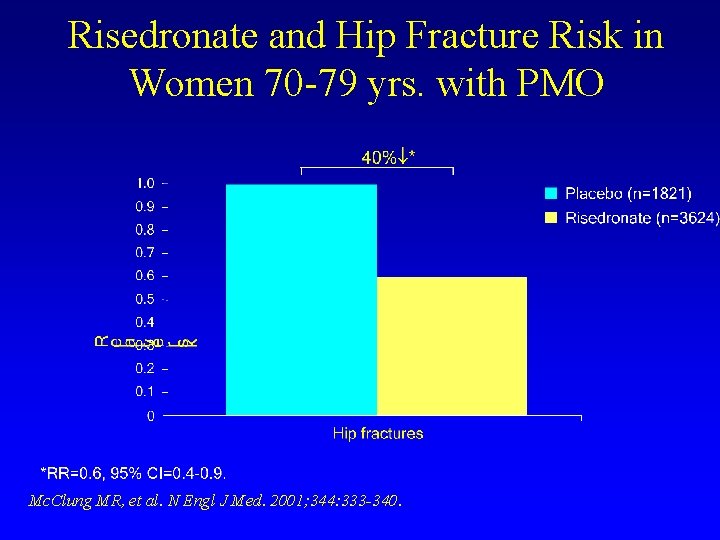
Risedronate and Hip Fracture Risk in Women 70 -79 yrs. with PMO Mc. Clung MR, et al. N Engl J Med. 2001; 344: 333 -340.

BMD and Fracture: Summary • BMD and fracture risk: Good predictor • BMD and fracture event: Poor discrimination • Moderate increase in BMD => larger-thanexpected decrease in fracture risk • BMD has been a major focus in osteoporosis research during the past 20 years
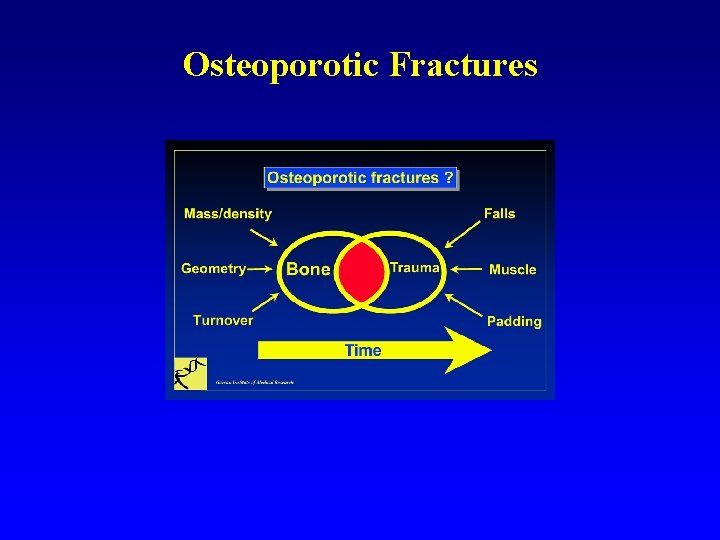
Osteoporotic Fractures
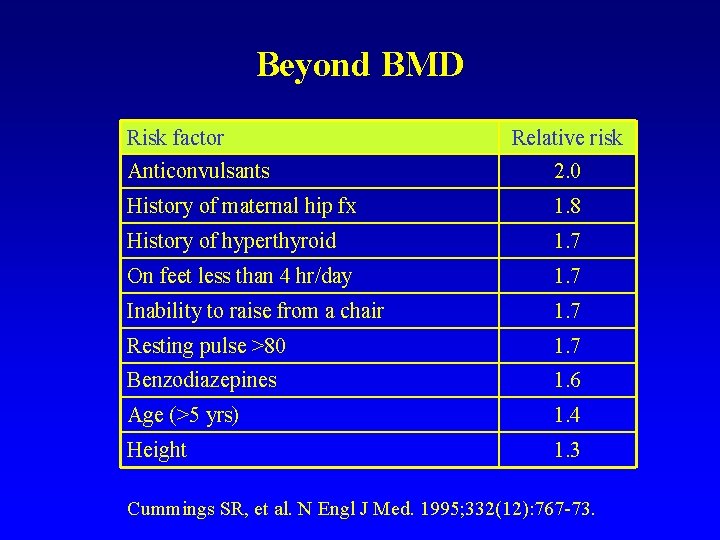
Beyond BMD Risk factor Relative risk Anticonvulsants 2. 0 History of maternal hip fx 1. 8 History of hyperthyroid 1. 7 On feet less than 4 hr/day 1. 7 Inability to raise from a chair 1. 7 Resting pulse >80 1. 7 Benzodiazepines 1. 6 Age (>5 yrs) 1. 4 Height 1. 3 Cummings SR, et al. N Engl J Med. 1995; 332(12): 767 -73.

Revisit Risk Factors • Aetiologic risk factors – Genotypes – Lifestyle factors (eg smoking, alcohol, dietary habit, physical activity, etc) – Mechanical factors – Falls and fall-related factors • Clinical risk factors – BMD – Quantitative ultrasound measurements (QUS) – History of fx
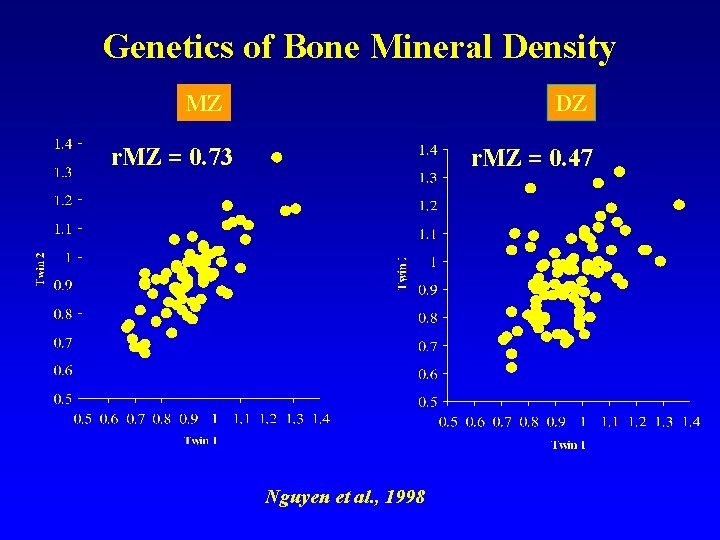
Genetics of Bone Mineral Density DZ MZ r. MZ = 0. 73 r. MZ = 0. 47 Nguyen et al. , 1998
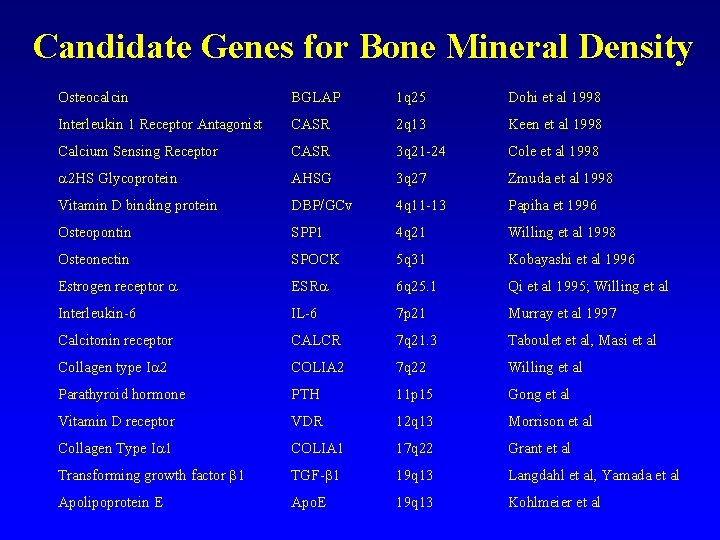
Candidate Genes for Bone Mineral Density Osteocalcin BGLAP 1 q 25 Dohi et al 1998 Interleukin 1 Receptor Antagonist CASR 2 q 13 Keen et al 1998 Calcium Sensing Receptor CASR 3 q 21 -24 Cole et al 1998 a 2 HS Glycoprotein AHSG 3 q 27 Zmuda et al 1998 Vitamin D binding protein DBP/GCv 4 q 11 -13 Papiha et 1996 Osteopontin SPP 1 4 q 21 Willing et al 1998 Osteonectin SPOCK 5 q 31 Kobayashi et al 1996 Estrogen receptor a ESRa 6 q 25. 1 Qi et al 1995; Willing et al Interleukin-6 IL-6 7 p 21 Murray et al 1997 Calcitonin receptor CALCR 7 q 21. 3 Taboulet et al, Masi et al Collagen type Ia 2 COLIA 2 7 q 22 Willing et al Parathyroid hormone PTH 11 p 15 Gong et al Vitamin D receptor VDR 12 q 13 Morrison et al Collagen Type Ia 1 COLIA 1 17 q 22 Grant et al Transforming growth factor b 1 TGF-b 1 19 q 13 Langdahl et al, Yamada et al Apolipoprotein E Apo. E 19 q 13 Kohlmeier et al
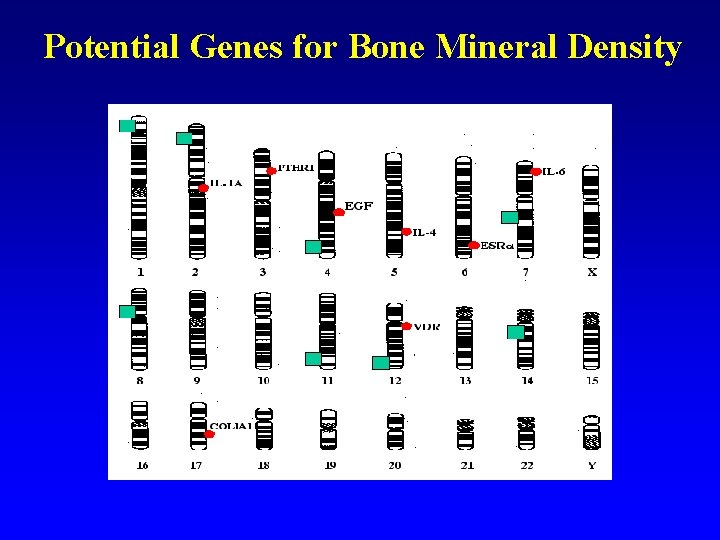
Potential Genes for Bone Mineral Density
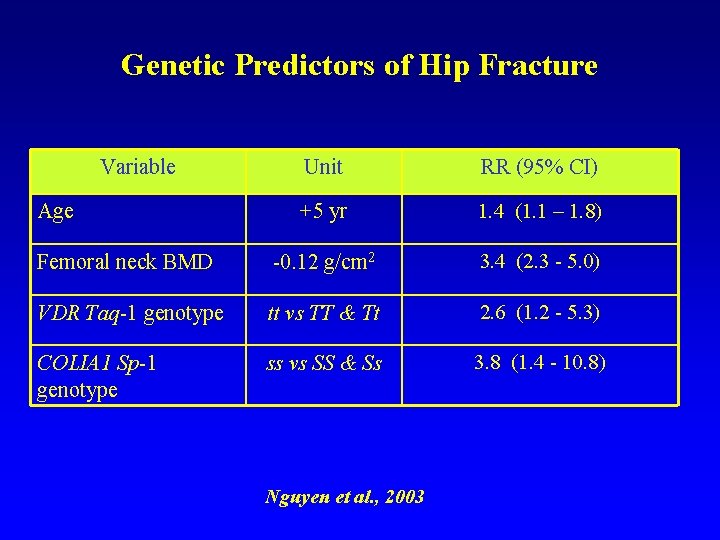
Genetic Predictors of Hip Fracture Variable Unit RR (95% CI) +5 yr 1. 4 (1. 1 – 1. 8) Femoral neck BMD -0. 12 g/cm 2 3. 4 (2. 3 - 5. 0) VDR Taq-1 genotype tt vs TT & Tt 2. 6 (1. 2 - 5. 3) COLIA 1 Sp-1 genotype ss vs SS & Ss 3. 8 (1. 4 - 10. 8) Age Nguyen et al. , 2003
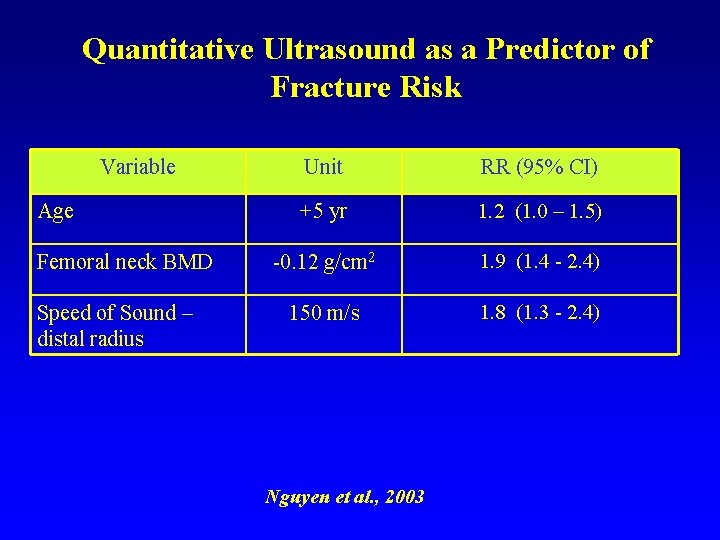
Quantitative Ultrasound as a Predictor of Fracture Risk Variable Age Femoral neck BMD Speed of Sound – distal radius Unit RR (95% CI) +5 yr 1. 2 (1. 0 – 1. 5) -0. 12 g/cm 2 1. 9 (1. 4 - 2. 4) 150 m/s 1. 8 (1. 3 - 2. 4) Nguyen et al. , 2003
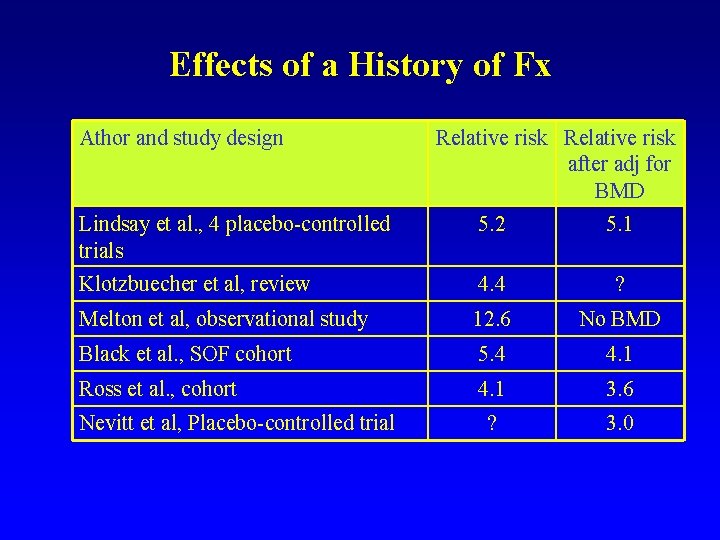
Effects of a History of Fx Athor and study design Relative risk after adj for BMD Lindsay et al. , 4 placebo-controlled trials 5. 2 5. 1 Klotzbuecher et al, review 4. 4 ? Melton et al, observational study 12. 6 No BMD Black et al. , SOF cohort 5. 4 4. 1 Ross et al. , cohort 4. 1 3. 6 ? 3. 0 Nevitt et al, Placebo-controlled trial

Research Directions • Improvement of models for long-term prediction of fractures – Etiologic risk factors • Identification of high-risk individuals – Clinical risk factors

Long-term Prediction of Fractures • “Remaining Lifetime Fracture Probability (RLFP): the sum of rates of fracture over an estimated remaining lifetime. • Make use of etiological risk factors to construct models of prediction –> Risk Index.
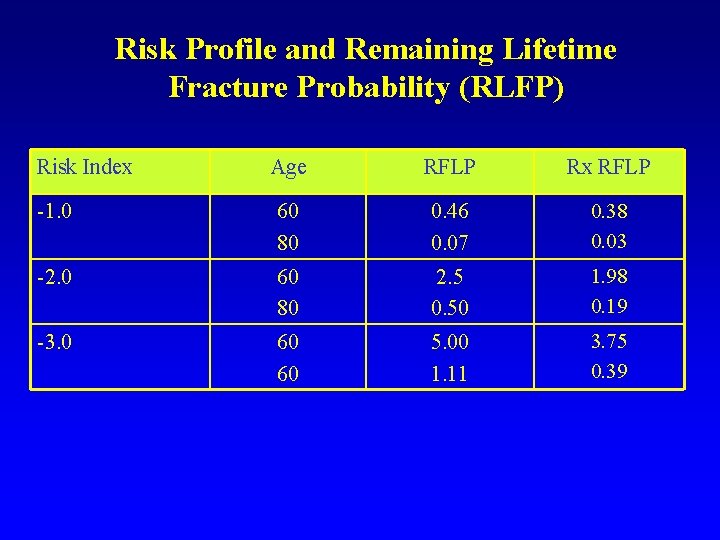
Risk Profile and Remaining Lifetime Fracture Probability (RLFP) Risk Index Age RFLP Rx RFLP -1. 0 60 80 0. 46 0. 07 0. 38 0. 03 -2. 0 60 80 2. 5 0. 50 1. 98 0. 19 -3. 0 60 60 5. 00 1. 11 3. 75 0. 39
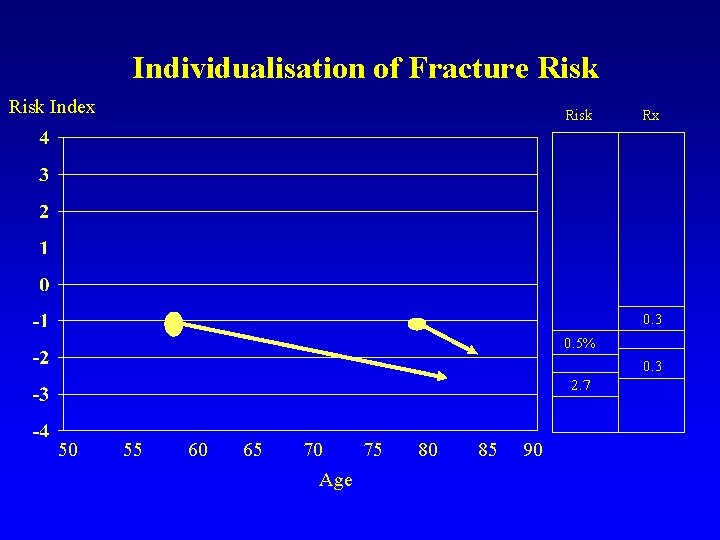
Individualisation of Fracture Risk Index Risk Rx 0. 3 0. 5% 0. 3 2. 7 50 55 60 65 70 75 Age 80 85 90

High-risk Individuals and The Definition of “Osteoporosis” • Make use of clinical risk factors and long-term predictive models for diagnostic purpose. • Toward a probability-based definition of osteoporosis. • Toward a probabilisty-based entry criteria for clinical trials.

The Future: A risk score calculator www. RISKFx. com Welcome to the Garvan Institute's Risk Score Calculator for Osteoporotic Fracture. Please enter your information in the following boxes and press CALCULATE to obtain your risk score. To recalculate, please press RESET and repeat the above procedure. Thank you. Age: Sex: Your femoral neck BMD T-score: Your QUS T-score: Your genotype: Do you have a history of fracture (Y/N)? CALCULATE RESET Are you a current smoker (Y/N): Have you had a fall during the past 12 months (Y/N)? Can you raise from a chair easily (Y/N)?

Thank you • Garvan team: – – John Eisman Jacqueline Center Natasha Ivanovic Jim Mc. Bride and "IT people" • Dubbo team: – Janet Watters – Donna Reeves – Volunteers, participants
- Slides: 50