Osteoporosis Karen Melton BSN What is Osteoporosis is

Osteoporosis Karen Melton, BSN
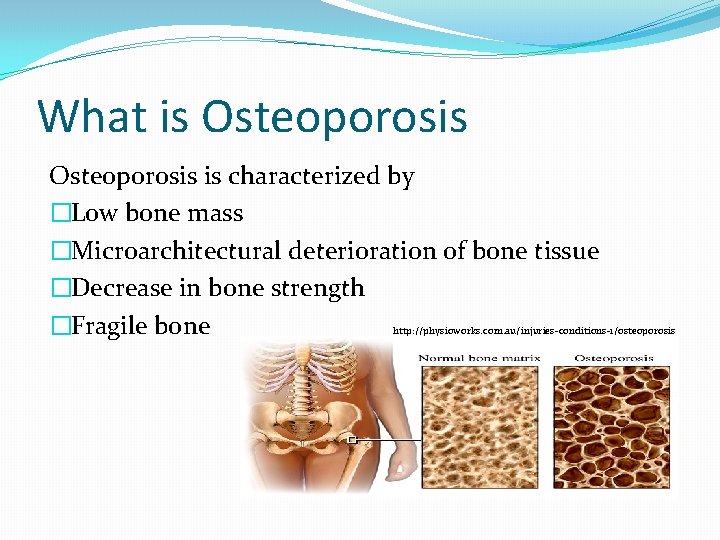
What is Osteoporosis is characterized by �Low bone mass �Microarchitectural deterioration of bone tissue �Decrease in bone strength �Fragile bone http: //physioworks. com. au/injuries-conditions-1/osteoporosis

Pathophysiology �Bone stays in a constant state of remodeling. Osteoblasts form/remodel bone while osteoclasts are responsible for bone resorption. These two must be in balance to maintain healthy bones. If bone resorption occurs at a faster rate than bone remodeling the bone becomes brittle resulting in osteoporosis.

Causes Primary osteoporosis in men and women �Bone loss due to normal aging �May result from sub-optimal bone growth in childhood and adolescence �Reduced estrogen production in women �Reduced sex hormone levels likely cause in men

Secondary osteoporosis �Endocrine disorders �Genetic factors �Gastrointestinal disorders �Hematologic disorders �Rheumatologic/autoimmune disorders �Central nervous system disorders �Hypogonad disorders �Drug induced

Risk Factors Non-modifiable �Age for men and women �Genetic/ethical background �History of previous fractures

Risk Factors Continued Modifiable �Low body mass and weight �Smoking �Alcohol consumption �Caffeine consumption �Hormonal deficiencies �Inactivity �Long term use of medications that contribute to osteoporosis �Diet low in calcium and vitamin D

Case Study • D. M. is a 71 year old white female. She is complaining of low back pain that started after she lost her balance while going to the bathroom and fell back onto the toilet 1 weeks ago.

History �Past Medical History- hypothyroidism, depression, menopause at 56 however she has declined offers of hormonal replacement. �Family History- mother had osteoporosis, hip fx, and died of breast cancer. Father died of heart attack. �Social History- Retired teacher, lives with her husband, and has 3 grown children. She denies smoking and drinks a glass of wine 3 -4 times a year. She walks 4 -5 days a week for 30 -45 min. �Surgical History- Gallbladder removed 1990.

Medications �Multivitamin po qd �Synthroid 75 mcg po qd �Paxil 20 mg po qd �Ibuprofen 400 mg po every 8 -12 hrs

Subjective Data �Patient states pain in lower back since her fall 1 week ago. States is throbs and is constant. She stated pain was mild in the beginning but has gotten progressively worse. She states that sitting and bending makes pain worse. She denies shooting pain down either leg. She has been icing the area a few times a day and has been taking over the counter ibuprofen 400 mg po every 8 -12 hrs and it has helped a little.

Objective Data �B/P- 130/70 P- 72 R- 18 T- 98. 0 �Ht- 5’ 4” Wt- 130 BMI-22. 3 �Pain 4/10; tolerable level is a 4; best it gets 4/10; worse it gets 8/10 ibuprofen and ice relieve pain from a 7/10 to a 5/10 �Neuro: patellar and achilles reflexes +2, superficial pain and superficial touch assessments did not indicate a loss of

Objective Data Continued �Musculoskeletal: Gait is smooth and steady. Patient grimaced when sitting back down. Spinal tenderness noted in lumbar area upon palpation. Spine flexion 50 degrees with pain noted. Straight leg raise test: patient unable to raise right leg more than 30 degrees without increased pain. Muscle strength in bilateral lower extremities 5/5.

Treatment Plan Diagnostics � X-ray of lumbar spine- confirmed L 4 compression fracture � Dexa Scan- T-score -3. 0 confirmed osteoporosis. � CBC- All values within therapeutic range � Serum Calcium 9. 1 (8. 9 -10. 1 mg/Dl) � Creatine - 1. 1 ml/deciliter (0. 6 -1. 1 mg/d. L) � 25 -hydroxyvitamin D level-19 ng/ml (range 25 -80 ng/ml)- mild deficiency � FRAX tool- 41% probability of major fracture within 10 years. 21% probability of hip fracture in the next 10 years


Treatment Plan Continued Medications management �Oxycodone 5 mg po q 6 hrs prn pain �Discontinue ibuprofen �Fosamax 10 mg po qd �Caltrate 600 mg/800 u OTC po qd Referral made to Watauga Orthopedics for vertebral fracture

Prescription Name: D. M. RX: Oxycodone 5 mg Date: 04/17/15 Take one pill by mouth every 6 hours as needed for pain. # 16 Refills: 0 Signature: Karen Melton FNP

Prescription Name: D. M. Date: 04/17/15 RX: Fosamax 10 mg Take one pill by mouth every morning with plenty of water minutes before any food, drink, or medications. # 30 Refills: 3 Signature: Karen Melton FNP 30

Patient Education Fosamax �Take with plenty of water at least 8 ozs �Take in the am 30 min before your first meal, drink, or other medication. �Do not lay down, recline or bend over for 30 minutes after taking this medication �Call if difficulty swallowing, rash, shortness of breath, acid reflux , abdominal pain, or musculoskeletal pain occur. �This medication may cause constipation and nausea.

Patient Education Continued Oxycodone �May cause drowsiness or dizziness �May cause constipation �Use caution driving until you see how you react to this medication �Call if you develop a rash or shortness of breath

Patient Education Continued Caltrate (calcium 600 mg plus D 3 800 u) �This has potential to decrease effects of synthroid. �Take Caltrate 4 hours apart from synthroid. �Call if rash or shortness of breath occur. Keep appointment with the orthopedic on 4/20/14. �Follow with this office in one month. �Minimize activity until your orthopedic appointment. �Continue rest and ice. Decrease stress on spine with pillows under head and legs when resting on back and if on side pillow between legs with both hips slightly flexed.

Mechanism of Action of Fosamax �Fosamax is a bisphonate. Bisphonates are classified as antiresorptive agents. They increase bone density by inhibiting osteoeclast activity(inhibit bone resorption), decreasing bone turnover, and promotes bone formation. These medications are deposited in the bone at the site of mineralization and in resorption lacunae (pits in the bone surface). �Fosamax has been shown to increase bone mass in the spine and hip. Studies have also shown a 48% decrease in the rate of vertebral compression fractures with the use of Fosamax.

Side Effects �Esophagitis �Gastrointestinal disturbances �Diarrhea �Abdominal pain �Dysphagia

References � Arcangelo, V. P. (Eds. ). (2013). Osteoporosis. In V. P. Arcangelo & A. M. Peterson Pharmacotherapeutics for advanced practice. A practical approach (3 th ed. , pp. 896 -903). Ambler, PA: Lippincott Williams &Wilkins. � FRAX ®WHO Fracture Risk Assessment Tool. Retrieved from http: //www. shef. ac. uk/FRAX/ � National Osteoporosis Foundation. (n. d. ). Making a Diagnosis. Retrieved from http: //nof. org/articles/8 � Physioworks. (n. d. ). Osteoporosis. Retrieved from http: //physioworks. com. au/injuries-conditions-1/osteoporosis � Rizzoli, R. , Cooper, C. , Reginster, J. Y. , Abrahamsen, B. , Adachi, J. D. , Brandi, M. L. , Bruyère, O. , Compston, J. , Ducy, P. , Ferrari, S. , Harvey, N. C. , Kanis, J. A. , Karsenty, G. , Laslop, A. , Rabenda, V. , & Vestergaard, P. (2012). Antidepressant medications and osteoporosis. Pubmed, 2012 Sep; 51(3): 606 -613. doi: 10. 1016/j. bone. 2012. 05. 018. � Uphold, C. R. & Graham, M. V. (Eds. ). (2013). Clinical guidelines in family practice (5 th ed. , pp. 849 -860). Gainesville, FL: Barmarrae Books.
- Slides: 24