Osteoporosis Definition Consensus Development 1993 Normal trabecular bone

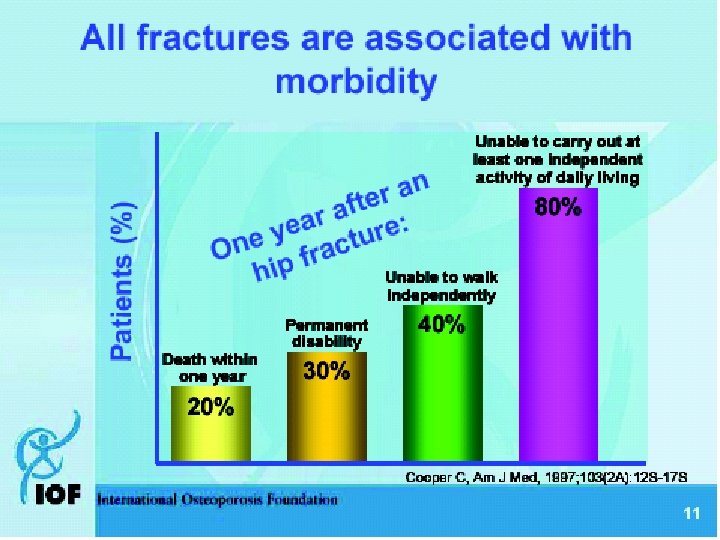
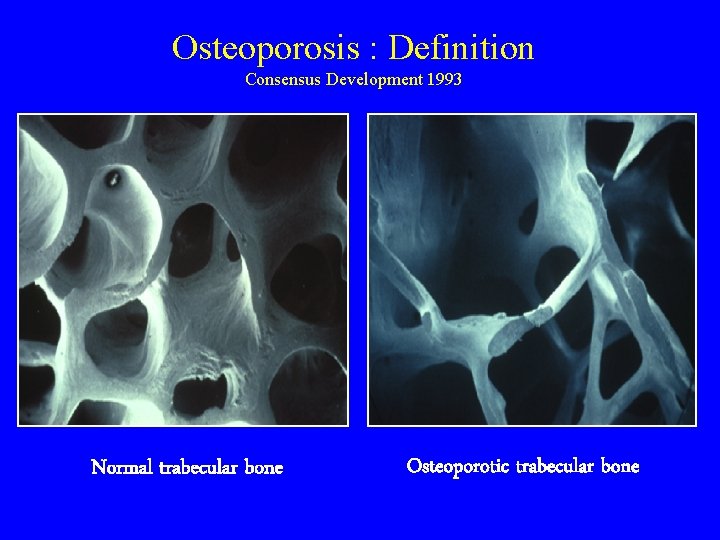
Osteoporosis : Definition Consensus Development 1993 Normal trabecular bone Osteoporotic trabecular bone

Detecting • Risk factors assessment • BMD testing patients at risk.
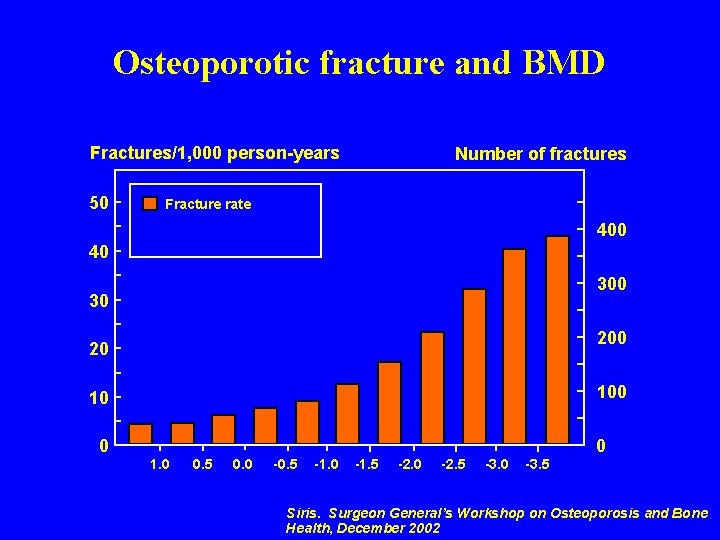
05 ca 0 85 Osteoporotic fracture and BMD Fractures/1, 000 person-years 50 Number of fractures Fracture rate 400 40 30 200 20 10 0 1. 0 0. 5 0. 0 -0. 5 -1. 0 -1. 5 -2. 0 -2. 5 -3. 0 -3. 5 0 Siris. Surgeon General’s Workshop on Osteoporosis and Bone Health, December 2002
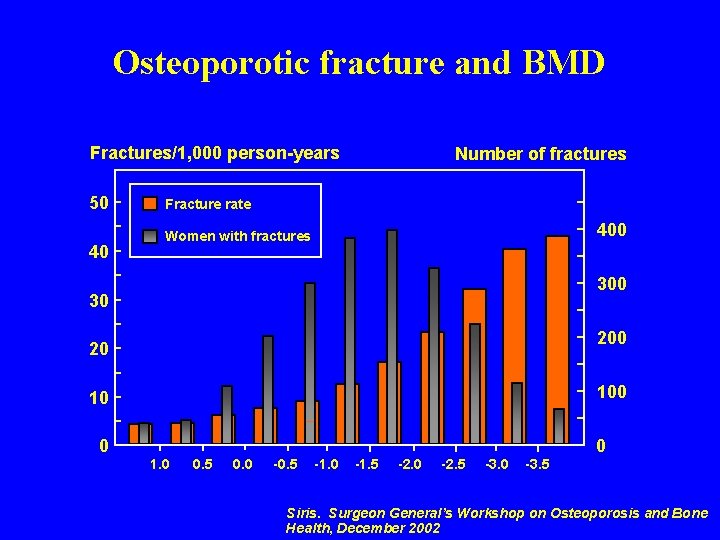
05 ca 0 85 Osteoporotic fracture and BMD Fractures/1, 000 person-years 50 40 Number of fractures Fracture rate 400 Women with fractures 300 30 20 100 10 0 1. 0 0. 5 0. 0 -0. 5 -1. 0 -1. 5 -2. 0 -2. 5 -3. 0 -3. 5 0 Siris. Surgeon General’s Workshop on Osteoporosis and Bone Health, December 2002
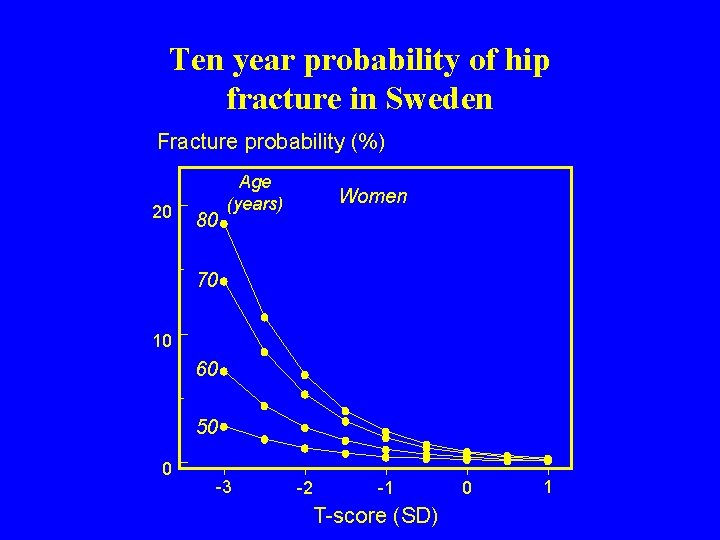
00 ca 104 Ten year probability of hip fracture in Sweden Fracture probability (%) 20 80 Age (years) Women 70 10 60 50 0 -3 -2 -1 T-score (SD) 0 1




Holy Smoke !




FRAX (http: //www. shef. ac. uk/FRAX). • A computer-based algorithm -> 10 yr probability hip & osteoporotic fractures • Clinical risk factors (+ BMD). • From population-based cohorts around the world & validated in independent cohorts with a similar geographic distribution. • should not be considered as a gold standard, but rather as a platform technology • Adapted from Kanis et al 2009

09 ca 001 Cohorts studied 22 population based cohorts from Europe, North America, Asia, Australasia EVOS/EPOS Hiroshima Ca. Mos Rochester Sheffield Rotterdam Kuopio Gothenburg (2) EPIDOS Dubbo OFELY THIN SOF York Geelong (2) OPUS PERF Miyama SEMOF WHI n = 289, 718 person-years = 1, 458, 427 Osteoporotic fractures = 18, 678 hip fractures = 4314
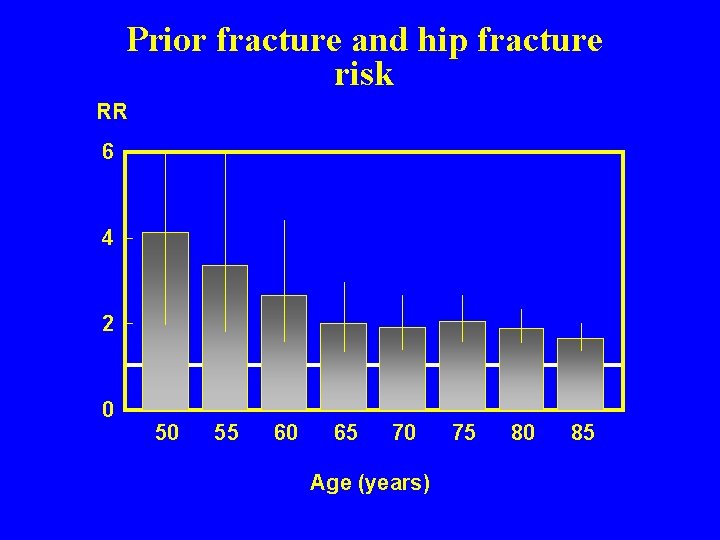
05 ca 186 Prior fracture and hip fracture risk RR 6 4 2 0 50 55 60 65 70 Age (years) 75 80 85
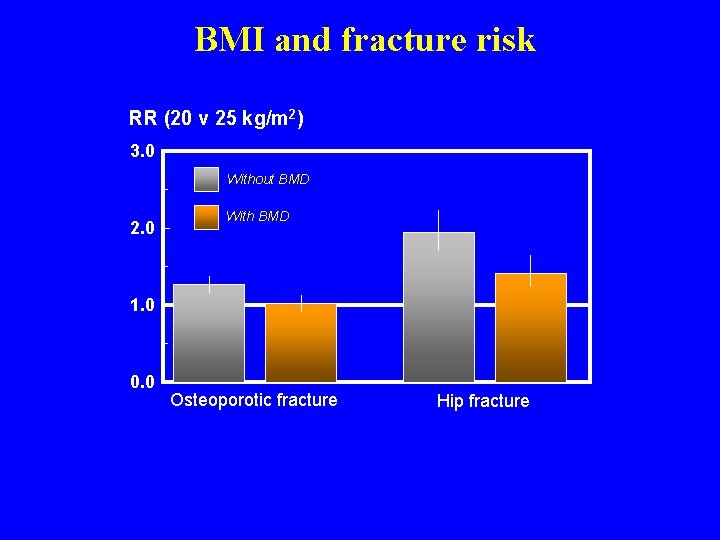
BMI and fracture risk 07 ca 080 RR (20 v 25 kg/m 2) 3. 0 Without BMD 2. 0 With BMD 1. 0 0. 0 Osteoporotic fracture Hip fracture
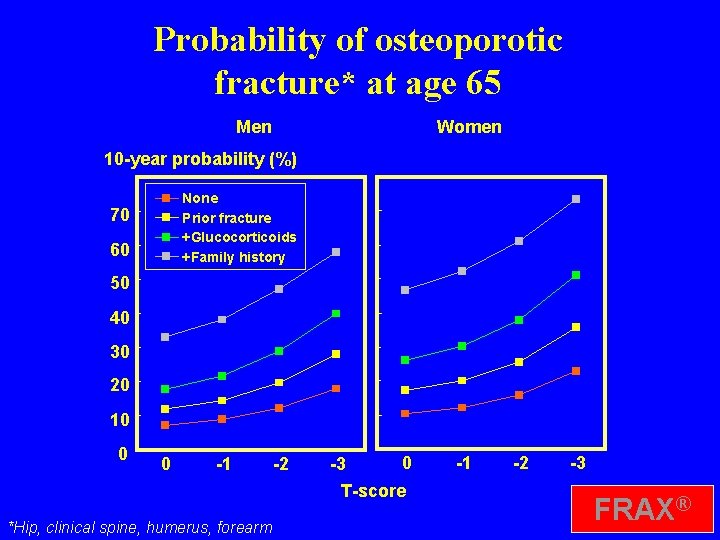
05 ca 106 Probability of osteoporotic fracture* at age 65 Men Women 10 -year probability (%) None Prior fracture +Glucocorticoids +Family history 70 60 50 40 30 20 10 0 0 -1 -2 -3 0 T-score USclinical Caucasian, CRF, BMI=24 *Hip, spine, no humerus, forearm -1 -2 -3 FRAX®
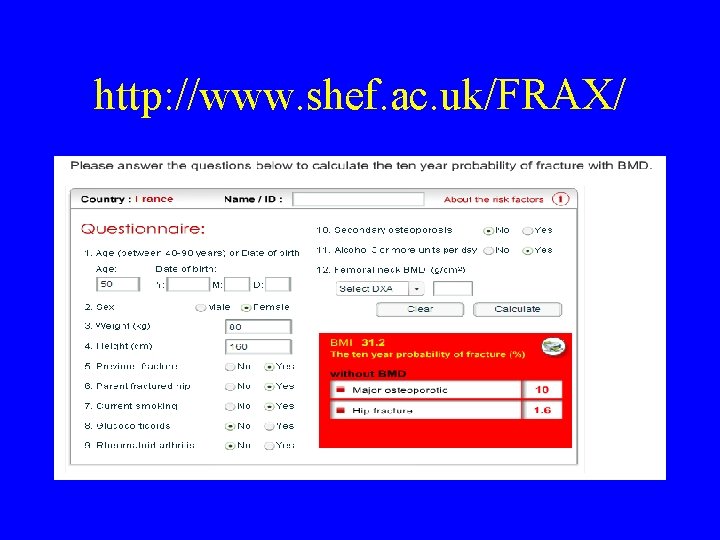
http: //www. shef. ac. uk/FRAX/

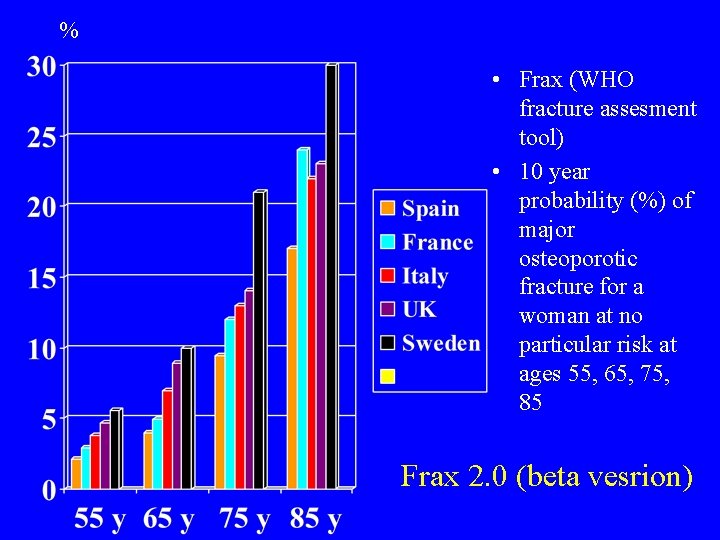
% • Frax (WHO fracture assesment tool) • 10 year probability (%) of major osteoporotic fracture for a woman at no particular risk at ages 55, 65, 75, 85 Frax 2. 0 (beta vesrion)
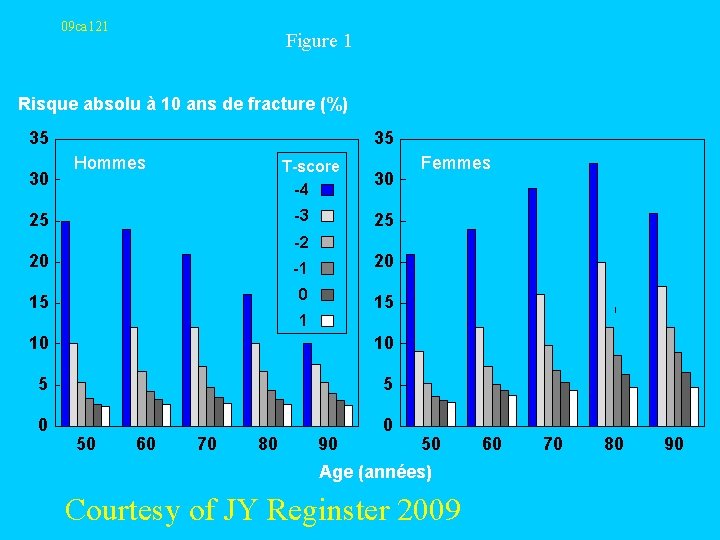
09 ca 121 Figure 1 Risque absolu à 10 ans de fracture (%) 35 30 35 Hommes T-score -4 -3 25 30 Femmes 25 -2 20 -1 20 15 1 10 10 5 5 0 0 50 60 70 80 90 50 Age (années) Courtesy of JY Reginster 2009 60 70 80 90
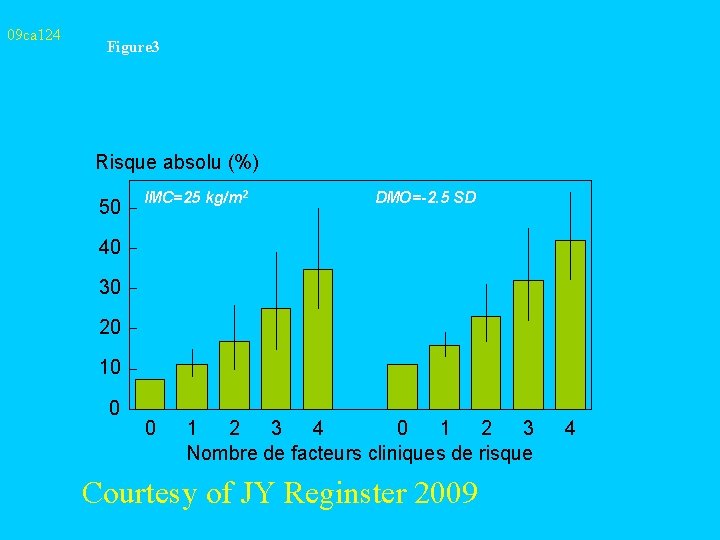
09 ca 124 Figure 3 Risque absolu (%) 50 IMC=25 kg/m 2 DMO=-2. 5 SD 40 30 20 10 0 0 1 2 3 4 0 1 2 3 Nombre de facteurs cliniques de risque Courtesy of JY Reginster 2009 4
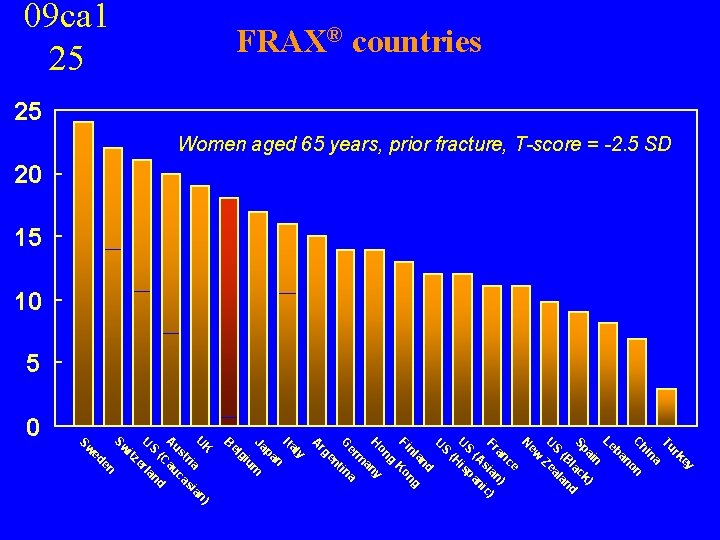
FRAX® countries 09 ca 1 25 25 Women aged 65 years, prior fracture, T-score = -2. 5 SD 20 15 10 5 0 a y an ey rk Tu na hi n C no ba Le n ) ai k Sp lac d (B lan S U Zea ew N ce an n) Fr sia c) i (A an p S U is (H S U d an g nl n Fi Ko g on H m tin um n en er G rg A ly Ita pa Ja gi el B en er n la K n) U ia ia tr as us uc a (C d A S U itz Sw ed Sw

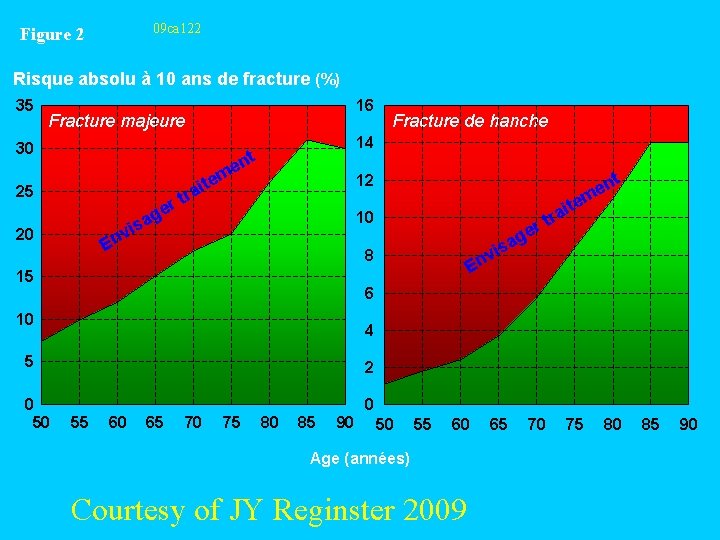
09 ca 122 Figure 2 Risque absolu à 10 ans de fracture (%) 35 16 Fracture majeure 30 25 er g isa te i a r 14 t en m nt e m 12 t 10 v En 20 Fracture de hanche 70 75 e ag is v En 8 15 r ite a r t 6 10 4 5 2 0 50 0 55 60 65 70 75 80 85 90 50 55 60 Age (années) Courtesy of JY Reginster 2009 65 80 85 90

Reducing fracture risk is the goal • Modeling suggests that intervention can be costeffective at around 10 -15% 10 year individualised fracture risk • Can estimate 10 yr. fracture risk by using – FRAX website programme – Tables from FRAX website relating BMD/age/risk factors

08 ca 100 Limitations of FRAX® Does not accommodate all known risk factors Falls, biochemical markers, QUS etc Lacks detail on some risk factors Dose response effects of glucocorticoids, smoking, prior fracture etc Depends on adequacy of epidemiological information Limited country models available Model relevant only for untreated patients Does not replace clinical judgment





Application of the WHO fracture risk assessment tool FRAXR in a Spanish population • 8, 573 women were included, 69% were under 60 years and 14% presented a previous fracture. After follow-up, 12% had a major osteoporotic fracture. Wrist was the most incident fracture site and hip was accounted only for 0. 9% of the total. • 10% of women with none risk factors had a major osteoporotic fracture, in turn 57% of those women with more than three risk factors had a major osteoporotic fracture. However the fracture ratio (O/E) was 3. 1 CI 95% [2. 8; 3. 5]. • Del Rio et al ASBMR 2009 Poster 0319

Application of the WHO fracture risk assessment tool FRAXR in a Spanish population • The O/E ratio was lower as higher was the age of women (for those older than 70 O/E=1. 8 CI 95% [1. 2; 2. 2]), longer the follow-up time (for those with more than 10 years O/E=2. 7 CI 95% [2. 2; 3. 4]) or lower the number of risk factors (for those without risk factors O/E=4. 2 CI 95% [3. 5; 5. 3]). • In conclusion, the Spanish version of the FRAX algorithm for this population underestimates the observed fracture incidence independently of the T-score, number of risk factors and follow-up time. More in-depth analyses are warranted to find a reasonable explanation to this issue. • Del Rio et al ASBMR 2009 Poster 0319
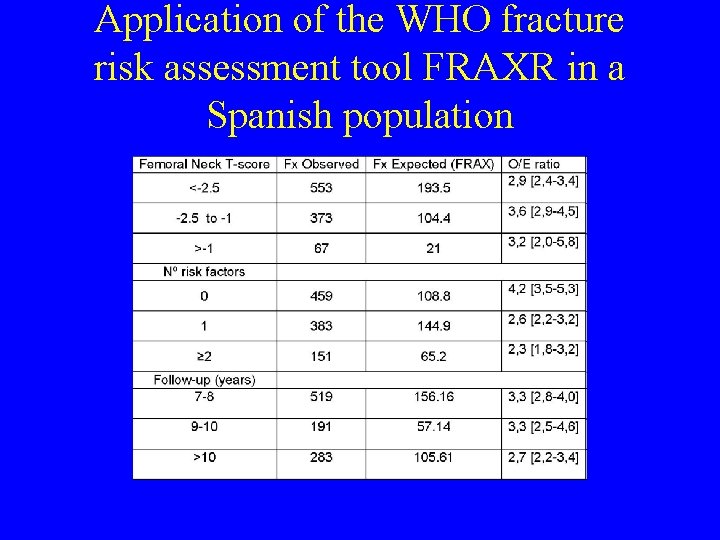
Application of the WHO fracture risk assessment tool FRAXR in a Spanish population

Comparison of 10 -Year Probability of Hip Fracture Predicted by FRAX and Observed Hip Fracture Incidence in the Framingham Osteoporosis Study • Expected number of hip fracture was determined by multiplying FRAX probabilities by the population at risk. Observed 10 -yr cumulative incidence of hip fracture was calculated as number of cases divided by the population at risk. Number of hip fractures observed was divided by number expected (O/E) to assess performance of FRAX. Analysis was stratified by sex-specific quintiles of FRAX and by age group (40 -75, 76 -90 yr). • Samelson et al ASBMR 2009 (Poster 0295)

Comparison of 10 -Year Probability of Hip Fracture Predicted by FRAX and Observed Hip Fracture Incidence in the Framingham Osteoporosis Study • • Mean age of participants was 65 yrs. 10 -yr incidence of hip fracture was 0. 031 (163 observed), nearly identical to FRAX predicted probability (0. 032; 166 expected), yielding O/E=0. 980 (CI: 0. 835 -1. 136). O/E ratios were similar across quintiles of predicted probabilities (TABLE). Findings were similar for women and men, however, the relatively small number of fractures in men resulted in unstable estimates. For example, 10 -yr incidence in women was 0. 045 (133 observed) compared to predicted probability of 0. 042 (125 expected) yielding O/E=1. 060 (CI: 0. 887 -1. 248); incidence in men was 0. 013 (30 observed) compared to predicted probability of 0. 018 (40 expected), yielding O/E=0. 733 (CI: 0. 494 -1. 019). In persons 76 -90 yrs, O/E=1. 315 (CI: 1. 061 -1. 596). In contrast, O/E=0. 732 (CI: 0. 570 -0. 913) for participants 4075 yrs. Overall, FRAX performed well in predicting 10 -yr probability of hip fracture in a large, population-based study of U. S. Caucasian women and men. However, FRAX underestimated hip fracture risk 32% in persons 76 -90 yrs and overestimated risk 27% in those 40 -75 yrs. Samelson et al ASBMR 2009 (Poster 0295)

Comparison of 10 -Year Probability of Hip Fracture Predicted by FRAX and Observed Hip Fracture Incidence in the Framingham Osteoporosis Study • Overall, FRAX performed well in predicting 10 -yr probability of hip fracture in a large, populationbased study of U. S. Caucasian women and men. • However, FRAX underestimated hip fracture risk by 32% in persons 76 -90 yrs and overestimated risk by 27% in those 40 -75 yrs. • Samelson et al ASBMR 2009 (Poster 0295)

Prediction of absolute risk of fracture by validation of risk factors in a Belgian cohort followed during 10 years FRISBEE (Fractures RIsk Study Brussels Epidemiological Enquiry) Courtesy of JJ Body

Results Descriptive analysis of the first 922 women Mean age : 69. 4 + 6. 0 years Mean age at menopause : 48. 6 + 5. 3 years (n = 711) Courtesy of JJ Body
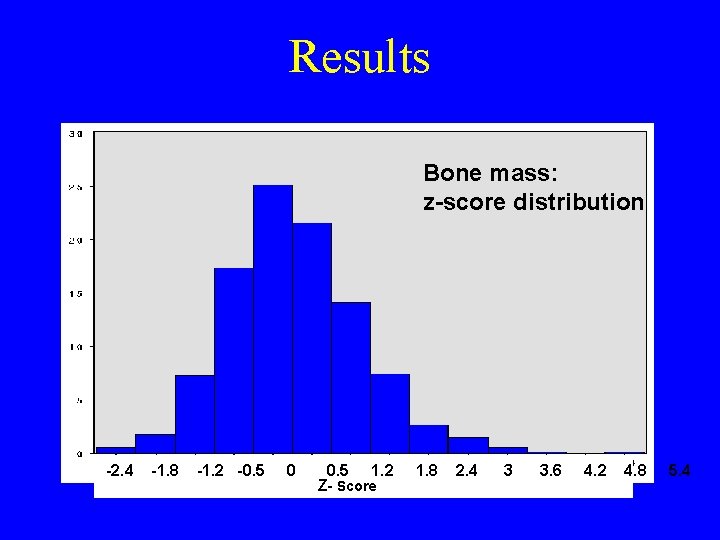
Results Bone mass: z-score distribution -2. 4 -1. 8 -1. 2 -0. 5 0 0. 5 1. 2 Z- Score 1. 8 2. 4 3 3. 6 4. 2 4. 8 5. 4
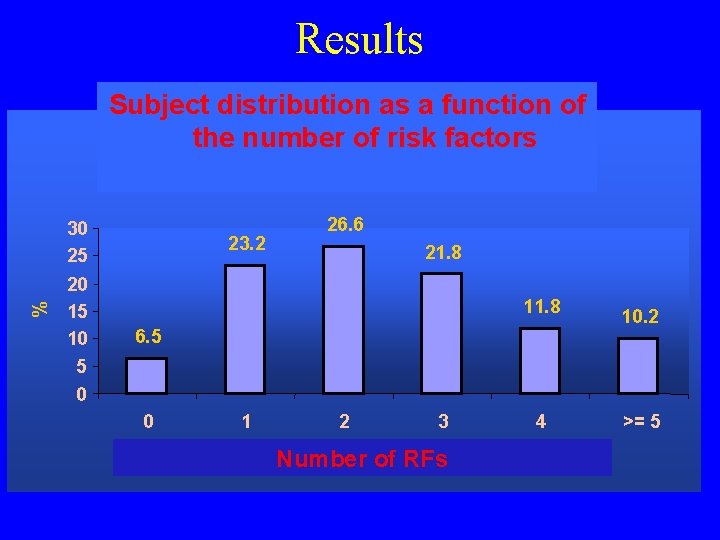
Results Subject distribution as a function of the factors Nombre denumber facteurs of de risk risque de fracture présents % 30 25 20 15 10 23. 2 26. 6 21. 8 11. 8 6. 5 10. 2 5 0 0 1 2 3 Nombre de facteurs Number of RFsde risque 4 >= 5

FRAX • Le mérite d’exister! • Devrait permettre de mieux traiter et de dispenser les traitements aux patientes qui en ont besoin • D’incorporer des données cliniques (même si imparfaites) • Mérite d’avoir des données Belges


Need for BMD at menopause • Most guidelines do not recommend systematic screening of BMD, unless risk factors • Help to decide to treat ? • In UK : if decision is yes : no need • If decision : no need • If undicised: place

Application of the WHO fracture risk assessment tool FRAXR in a Spanish population • Clinical and BMD data large population cohort of Barcelona. • Inclusion criteria were: age range 40 -90 yrs, clinical risk factors, femoral neck BMD T-score available and follow-up longer than 7 years. • Main outcome was: major osteoporotic fracture at least 7 years after the first BMD measurement. The total number of predicted fractures by the FRAX algorithm was compared with the total number of new registered fractures during the follow-up time in the study population and expressed as observed - expected fracture (O/E) ratio. Results were stratified by age group, follow-up time and number of clinical risk factors used in the FRAX algorithm • Del Rio et al ASBMR 2009 Poster 0319

Validity of the WHO FRAX Model to Predict the Risk of Fracture in Early Postmenopausal Women • compared the predictive validity of the FRAX model and femoral neck (FN) BMD in a large cohort of early PM women. • The analysis was conducted in the MENOS cohort that included an initial population of 4, 024 women ≥ 45 years of age, from whom 2, 650 (mean age 54± 4 yrs) were followed over a period of time of 13. 4 yrs. • Baseline characteristics were obtained through a structured questionnaire as well as BMD measurement (Lunar DPX). • Excluded women with current or past OP treatment >3 months at baseline (n=544). Due to changes in the procedure of BMD measurements that occurred during the baseline examination period of time, only 1, 399 out of 2, 196 women had a valid FN BMD. Therefore, the WHO FRAX score was calculated only in those 1, 399 women according to the CRFs and the FN T-score as given by the Lunar device.

Validity of the WHO FRAX Model to Predict the Risk of Fracture in Early Postmenopausal Women • The prevalence of the CRFs were as follows: low BMI=5. 2%; history of prior fracture=2. 4%; parental history of hip fracture=10. 4%; current smoking=8. 7%; ever use of glucocorticoids=1. 4%; rheumatoid arthritis=0. 1%; secondary OP=5%; alcohol consumption (1+U/d)=0. 1%. • A 1 st incident major low-trauma fracture was recorded in 98 women over the follow up period and all events were confirmed by radiographs or by medical/surgical reports. The performances of the scores were compared using areas under receiver operating characteristics (ROC) curves (AUC).

Validity of the WHO FRAX Model to Predict the Risk of Fracture in Early Postmenopausal Women • The AUC (0. 66) for the FRAX model was not significantly different • • • from that of FN BMD alone (0. 69). The WHO FRAX model lack sensitivity i. e. the detection rate was low. For example, for a specificity of 80%, the FRAX model had a sensitivity of about 38%. Since, 381 out of 1, 399 women started HRT during follow-up, the analyses were re-runned in the remaining women. The AUCs increased to 0. 69 and 0. 71, respectively for the FRAX model and FN BMD. In this population, the FRAX model has a poor value to predict the risk of fracture and does not significantly improve the predictive value of hip BMD alone. These results raise the question of the selection of the CRFs that need to be considered in the clinical assessment of the risk of fracture in early PM women. Dargent-Molina; et al ASBMR 2009 Oral 1094
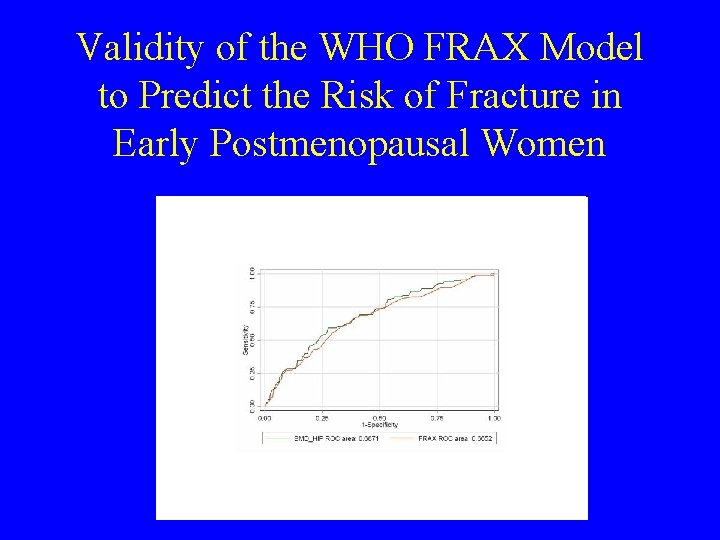
Validity of the WHO FRAX Model to Predict the Risk of Fracture in Early Postmenopausal Women

Imputation of Ten Year Osteoporotic Fracture Rates from Hip Fractures: A Clinical Validation Study. • to evaluate the method for imputation of osteoporotic fracture rates from hip fractures alone. • 38, 784 women age 47. 5 years or older at the time of baseline femoral neck BMD identified in a database containing all clinical DXA results for the Province of Manitoba, Canada. • Health service records were assessed for the presence of non-trauma osteoporotic fracture codes after BMD testing (431 hip, 787 forearm, 336 clinical vertebral, and 431 humerus fractures). • Ten year hip and osteoporotic fracture rates were estimated by the Kaplan-Meier method. • The population was stratified by age (50 to 90, 5 year width strata) and again by femoral neck T-scores (-4. 0 to 0. 0, 0. 5 SD width strata). • Within each stratum, the ratio of hip to osteoporotic fractures was calculated and compared to the predicted ratio from FRAX. • Leslie WD, Lix LM; for the Manitoba Bone Density Program. J Bone Miner Res. 2009 Aug 4. [Epub ahead of print]

Imputation of Ten Year Osteoporotic Fracture Rates from Hip Fractures: A Clinical Validation Study. • Increasing age was associated with greater predicted hip-to -osteoporotic ratios (youngest 0. 07 vs oldest 0. 41) and observed ratios (youngest 0. 10 vs oldest 0. 48). • Lower T-scores were associated with greater predicted (highest 0. 04 vs lowest 0. 71) and observed ratios (highest 0. 06 vs lowest 0. 44). • There was a strong positive correlation between predicted and observed ratios (Spearman r = 0. 90 -0. 97, p <. 001). • For 14 of the 18 strata, the predicted ratio was within the observed 95% confidence interval. • Since collection of population-based hip fracture data is considerably easier than collection of non-hip fracture data, this study supports the current emphasis on using hip fractures as the preferred site for FRAX model calibration. • Leslie WD, Lix LM; for the Manitoba Bone Density

Understanding the definitions in the Management of Osteoporosis • Osteoporosis – primary prevention – stop the deterioration of BMD • Osteopenia • Risk factors • Osteoporosis – secondary prevention – BMD t score <-2. 5 SD • Fracture – primary prevention – No fracture – prevent fracture • Fracture – secondary prevention – Previous fracture – prevent another fracture




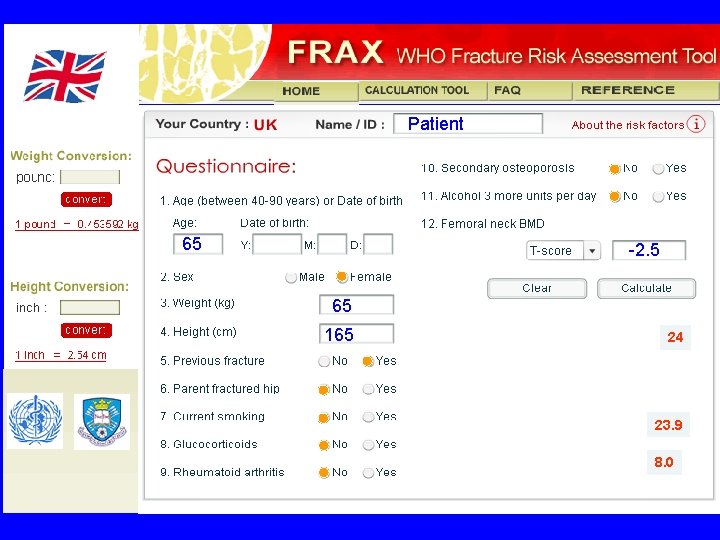
FRAX 08 ca 032 Patient 65 -2. 5 65 165 24 23. 9 8. 0
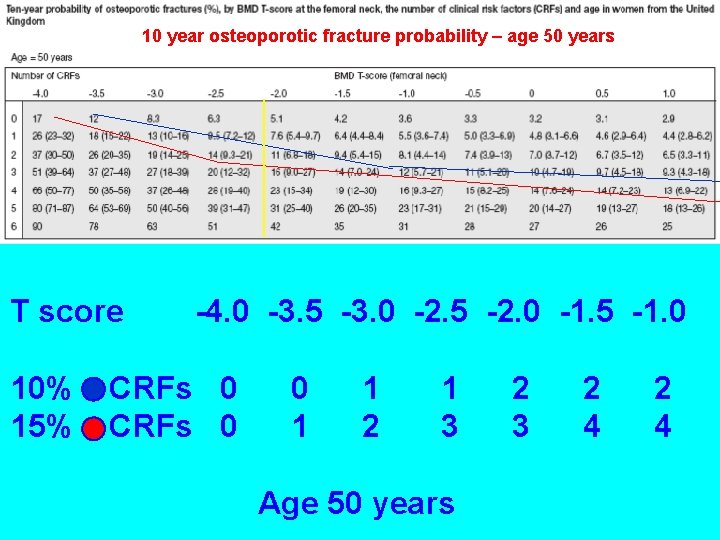
10 year osteoporotic fracture probability – age 50 years T score 10% 15% -4. 0 -3. 5 -3. 0 -2. 5 -2. 0 -1. 5 -1. 0 CRFs 0 0 1 1 2 1 3 Age 50 years 2 3 2 4


Systematic review • 145 articles

Updated fracture incidence rates for the US version of FRAX(R). • recommend revising the US-FRAX by updating current base population values for hip fracture and major osteoporotic fracture. The impact of these revisions on FRAX(R) is likely to be lowering of 10 -year fracture probabilities, but more precise estimates of the impact of these changes will be available after these new rates are incorporated into the FRAX(R) tool. • Ettinger et al Osteoporos Int. 2009 Aug 25.

Updated fracture incidence rates for the US version of FRAX(R). • US hospital discharge data from 2006 to calculate annual age- and sexspecific hip fracture rates and age-specific ratios to estimate clinical vertebral fracture rates. • To estimate the incidence of any one of four major osteoporotic fractures, They first summed these newly derived hip and vertebral fracture estimates with Olmsted County, MN, wrist and upper humerus fracture rates, and then applied 10 -20% discounts for overlap. RESULTS: Compared with rates used in the current FRAX(R) tool, 2006 hip fracture rates are about 16% lower, with greatest reductions observed among those below age 65 years; major osteoporotic fracture rates are about one quarter lower, with similar reductions across all ages. • Ettinger et al Osteoporos Int. 2009 Aug 25.

Results HRT: 18. 0 % (n= 166) osteoporosis treatment: 11. 4 % (n = 105) Calcium supplements : 31. 2 % (n = 288) Courtesy of JJ Body
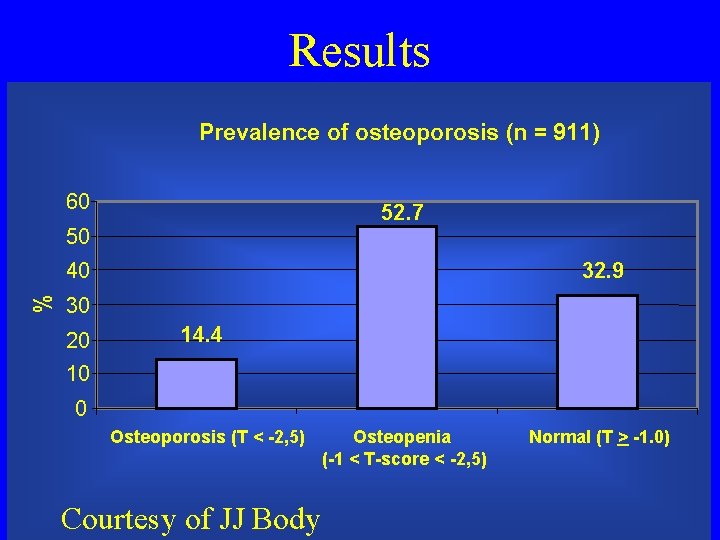
Results Prevalence of osteoporosis (n = 911) 60 52. 7 50 % 40 32. 9 30 20 14. 4 10 0 Osteoporosis (T < -2, 5) Courtesy of JJ Body Osteopenia (-1 < T-score < -2, 5) Normal (T > -1. 0)
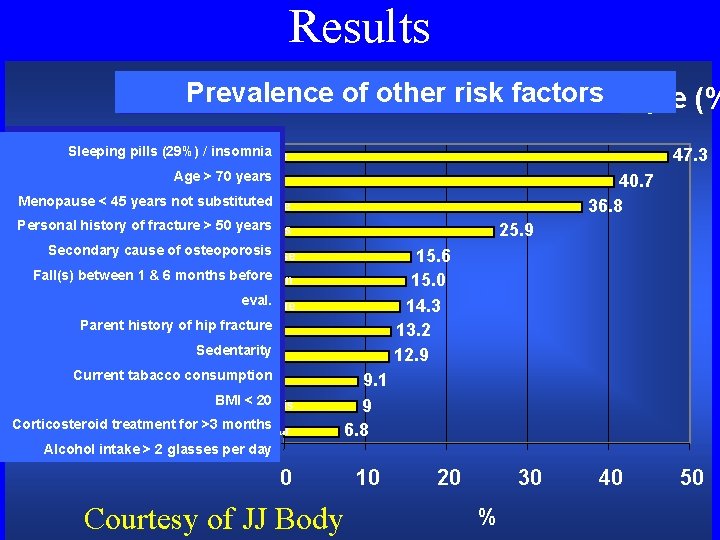
Results Prevalence other risk factors Prevalence ofof other risk factors Prévalence des autres facteurs de risque (% Sleeping pills/ /insomnia Sleeping pills Prise de(29%) somnifères/insomnie Age>>70 70 years Age 47. 3 40. 7 36. 8 Age > 70 ans Menopause<<45 45 yearsnot substituted Menopause Ménopause précocesubstituted non substituée Personalhistoryof offracture>>50 50 years Personal 25. 9 Atcdts personnels de fracture > 50 ans Secondary cause of osteoporosis Maladie chronique causant une perte osseuse 15. 6 15. 0 14. 3 13. 2 12. 9 Fall(s) betw 1 & 6 months before eval Fall(s) between months Chute(s) entre 11 et&66 mois avantbefore évaluation Parent history of hip fracture eval. Atcdts de fracture col fémoral chez père ou mère Sedentarity Parent history of hip fracture Sédentarité Current tabacco consumption Sedentarity Tabagisme habituel BMI < 20 Current tabacco consumption BMI < 20 Corticosteroid treatment for >3 months BMI < 20 Traitements par corticoïdes pendant > 3 mois Alcohol treatment intake > 2 glasse per day Corticosteroid months Consommation alcoolfor > 2>3 verres par jour 9. 1 9 6. 8 Alcohol intake > 2 glasses per day 0 Courtesy of JJ Body 10 20 30 % 40 50

Results Association* between osteoporosis (DXA) and other risk factors in this still limited sample: – Age > 70 years (p = 0. 0001) – Personal history of fracture > 50 years (p < 0. 0001) – Number of risk factors (0 -2 vs > 2) (p < 0. 0001) – BMI < 20 (p = 0. 0001) – Sedentarity (p = 0. 001) – Parental history of hip fracture (p = 0. 03) are significantly associated with « osteoporosis » at DXA * Use of c 2 test

Preliminary conclusions • Elevated level of participation • Selection bias ? : - education level is rather high - relatively high % of women taking HRT (18 %) or calcium supplements (31. 2 %) However, the Z-score distribution is centered around 0, suggesting the ABSENCE of systematic bias !

Preliminary conclusions • The distribution of risk factors for fracture appears to be « classical » : – untreated menopause < 45 yrs, personal history of fractures > 50 yrs, use of sleeping pills, history of falls were the most frequent ones • Significant association between « osteoporosis » (DXA) and the following risk factors: – age > 70 years – personal history of fracture > 50 years – number of risk factors


Osteoporosis strategy in early postmenopause (<60 yr. ) HRT for fracture prevention in unselected group – benefit and risks are in balance Fractures saved and risks events are low HRT for fracture prevention in women at increased fracture risk – improves benefit: risk balance Fractures saved >> risks events 10%-15% 10 year fracture risk threshold delivers cost-effectiveness women need to have osteoporosis and RFs
- Slides: 73