Osteology of the Lower Limb ANA 208 Lecture

Osteology of the Lower Limb ANA 208

Lecture Schedule • Introduction / Osteology of Lower limb • Inguinal region • Gluteal region • Compartments of the thigh • Femoral triangle and adductor canal • Popliteal fossa • Flexor and extensor compartments of the leg • Foot and its arches • Joints of the lower limb • Blood supply and innervation of the lower limb / Dermatomes • Lumbosacral plexus 2
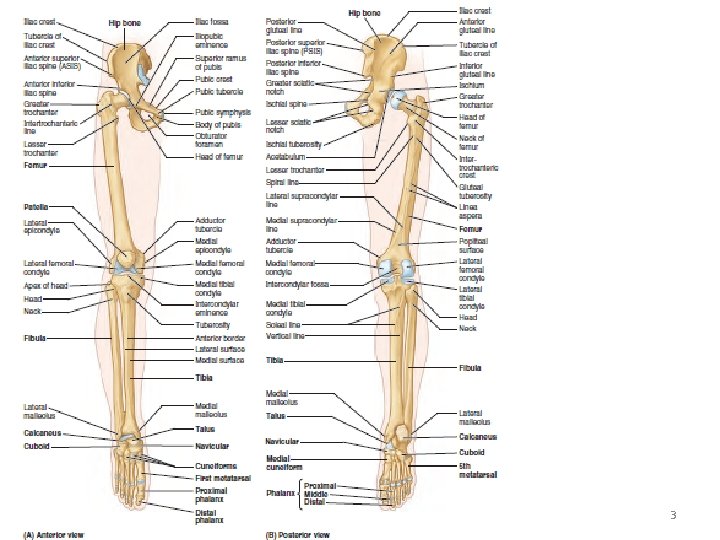
3

Hip Bone (L. os coxae) • Fusion of three primary bones—ilium, ischium, and pubis. • Each of the three bones is formed from its own primary center of ossification; five secondary centers of ossification appear later. • At birth, the three primary bones are joined by hyaline cartilage. • At puberty, the three bones are still separated by a Y-shaped triradiate cartilage. • The bones begin to fuse between 15 and 17 years of age; fusion is complete between 20 and 25 years of age. 4
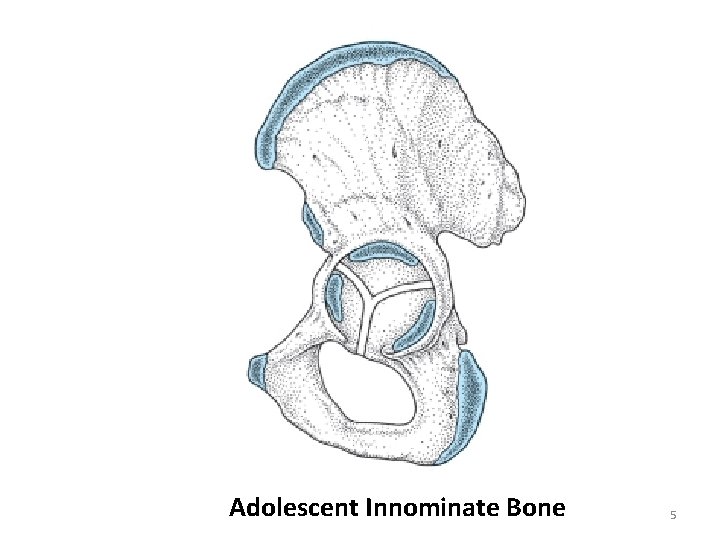
Adolescent Innominate Bone 5
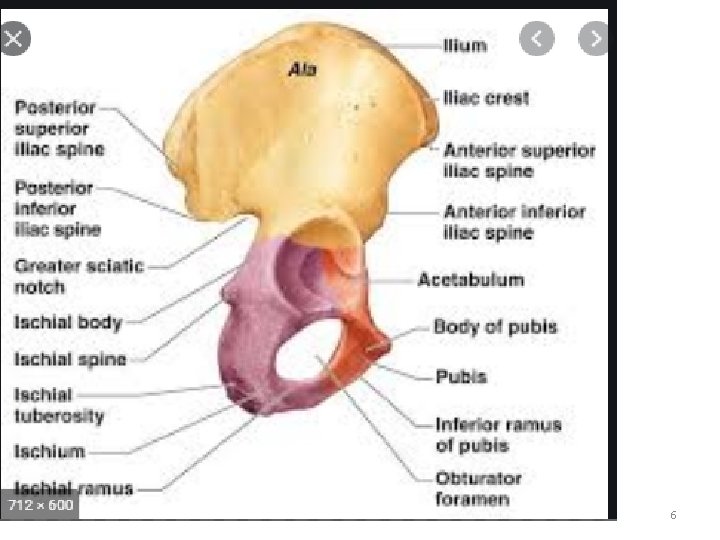
6
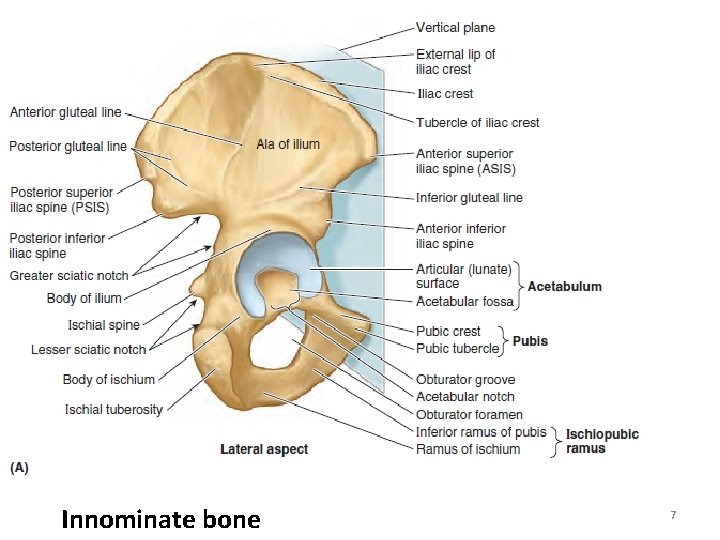
Innominate bone 7
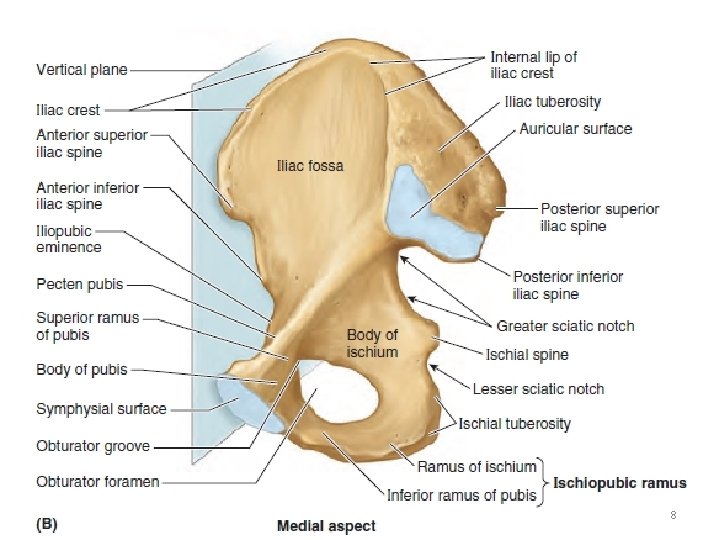
8
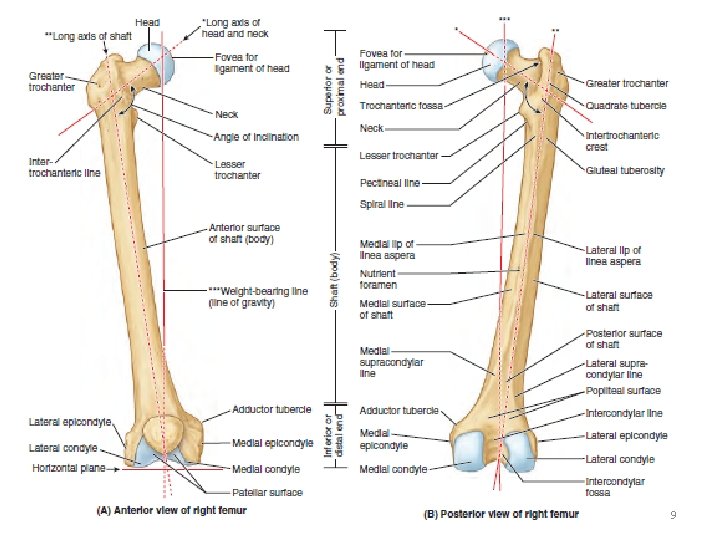
9
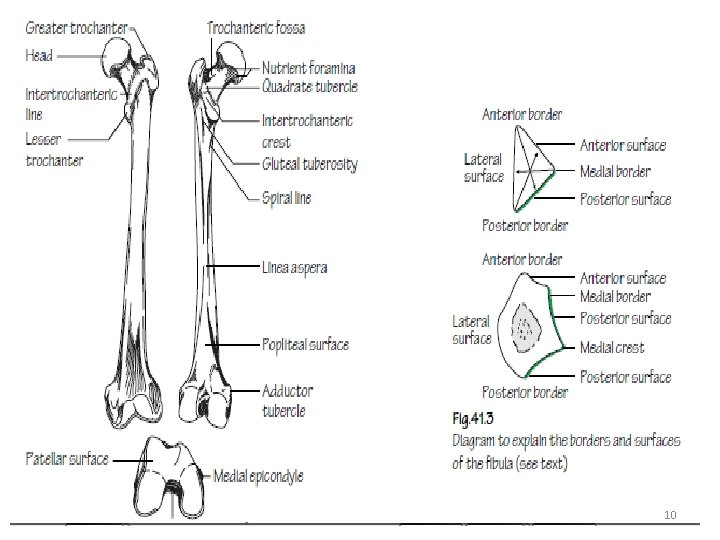
10
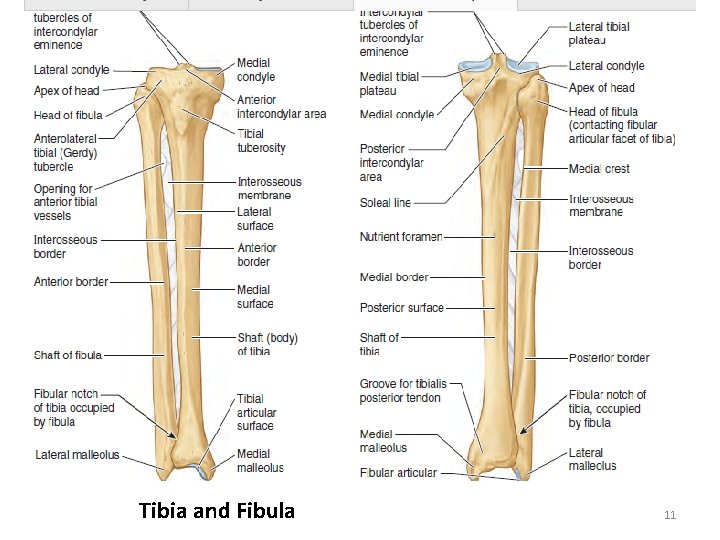
Tibia and Fibula 11
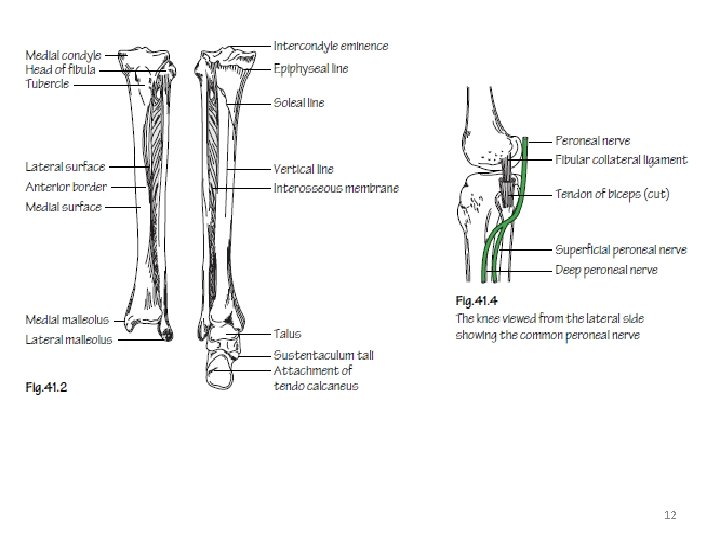
12
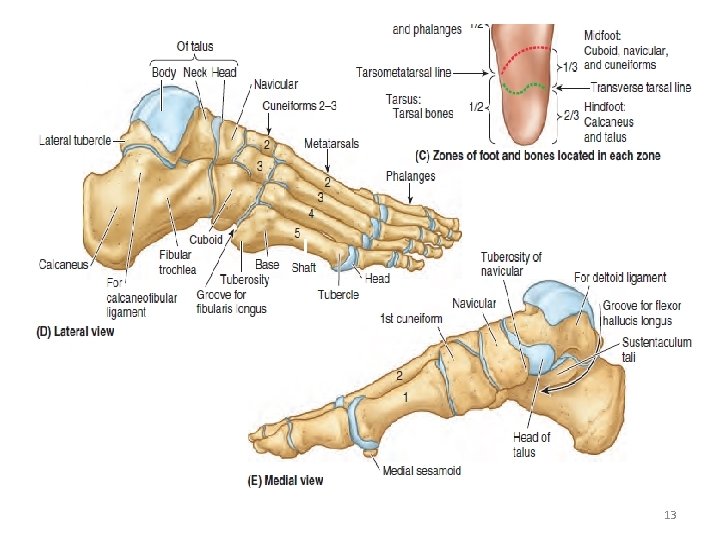
13
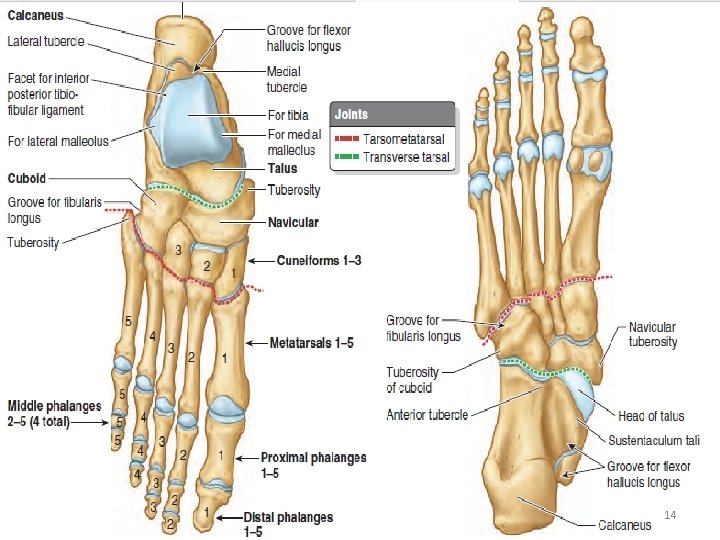
14
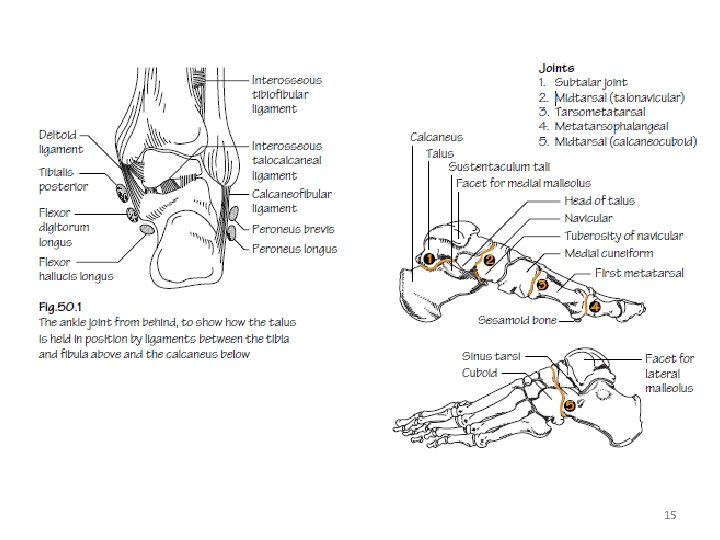
15

Inguinal Canal / Region • Oblique intermuscular slit about 4 cm long lying parallel and above the medial half of the inguinal ligament. • Hiatus in the tissues of the anterior abdominal wall • Size and form vary with age, it is most well developed in the male. • In the newborn, the canal is short. • Commences at the deep inguinal ring, ends at the superficial inguinal ring 16
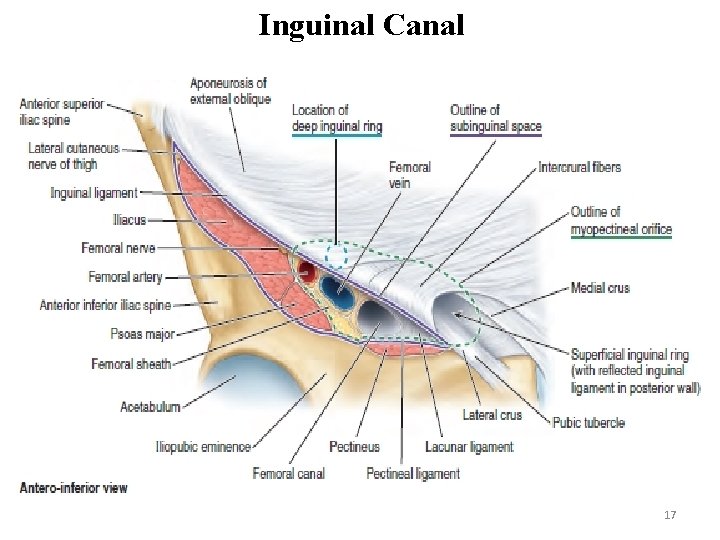
Inguinal Canal 17
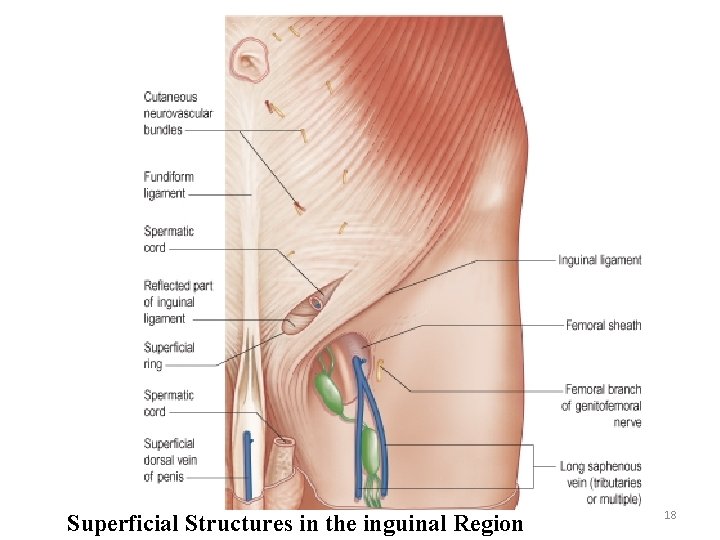
Superficial Structures in the inguinal Region 18

Contents • Spermatic cord in the male • Round ligament of the uterus • Ilioinguinal nerve • Genitofemoral nerve 19

Superficial inguinal ring • End of the inguinal canal and lies superior to the pubic tubercle • Exit by which inguinal contents emerges from the inguinal canal. • Formed by evagination of the external oblique aponeurosis • Triangular • Form the margins called crura. - Lateral crus attaches to the pubic tubercle, stronger and reinforced by fibres of the inguinal ligament - Medial crus attaches to the pubic crest, thin. 20

• Does not extend beyond the medial one-third of the inguinal ligament. • Some fibres arch above the apex as intercrural fibres which prevent the crura from spreading apart. • In the male, the lateral crus forms a groove, in which the spermatic cord rests. • Smaller in the female. 21

Deep (internal) inguinal ring • Lateral to inferior epigastric vessels • Situated in the transversalis fascia and projected as the internal spermatic fascia around the spermatic cord • Midway between the anterior superior iliac spine and the symphysis pubis • 1. 25 cm above the inguinal ligament. • Oval • Size varies between individuals, larger in the male. 22

• In the female they are replaced by the obliterated processus vaginalis, the round ligament and lymphatics from the uterus. • Ilioinguinal nerve does not enter the canal through the deep ring, but pierces the internal oblique muscle, and leaves the canal through the superficial ring 23

Boundaries • Anteriorly - skin, superficial fascia and aponeurosis of external oblique, its lateral one-third is reinforced by internal oblique muscle. • Posteriorly - inguinal ligament, the conjoint tendon (inguinal falx) and the transversalis fascia. • Superiorly - internal oblique and transversus abdominis forming the conjoint tendon. • Inferiorly - union of the transversalis fascia with the inguinal ligament and, at the medial end, the lacunar ligament. 24

INGUINAL LIGAMENT AND ILIOPUBIC TRACT • Extend from the ASIS to the pubic tubercle • The inguinal ligament (of Poupart) is a dense band constituting the inferiormost part of the external oblique aponeurosis. • Most fibers of the ligament’s medial end insert into the pubic tubercle, some attach to the superior pubic ramus, forming lacunar ligament (of Gimbernat) • The most lateral of these fibers continue to run along the pecten pubis as the pectineal ligament (of Cooper). • Iliopubic tract is the thickened inferior margin of the transversalis fascia, running parallel and posterior to the inguinal ligament 25

Relations • Posteriorly, inferior epigastric vessels lie on the transversalis fascia • Lateral to the artery are the vas deferens in the male and the round ligament of the uterus in the female. • Inguinal triangle lies in the posterior wall of the canal. • Overlies the medial inguinal fossa and, in part, the supravesical fossa. • Lacunar ligament 26

Inguinal triangle (of Hesselbach) Area of potential weakness through which herniation can occur - Laterally by the inferior epigastric artery - Medially by the lateral border of the rectus muscle - Inferiorly by the inguinal ligament Contents • Layers of the abdominal wall 27

Lacunar ligament • A triangular band of tissue lying posterior to the medial end of the inguinal ligament. • Measures 2 cm from base to apex and is a little larger in the male. • Formed from fibres of the medial end of the inguinal ligament and fibres from the fascia lata of the thigh. • Apex of the triangle is attached to the pubic tubercle. 28

Pectineal ligament of Astley Cooper • Extends laterally along the pectineal line from the pectineal attachment. • Forms the lower extension of the medial border of the femoral canal and femoral sheath. 29
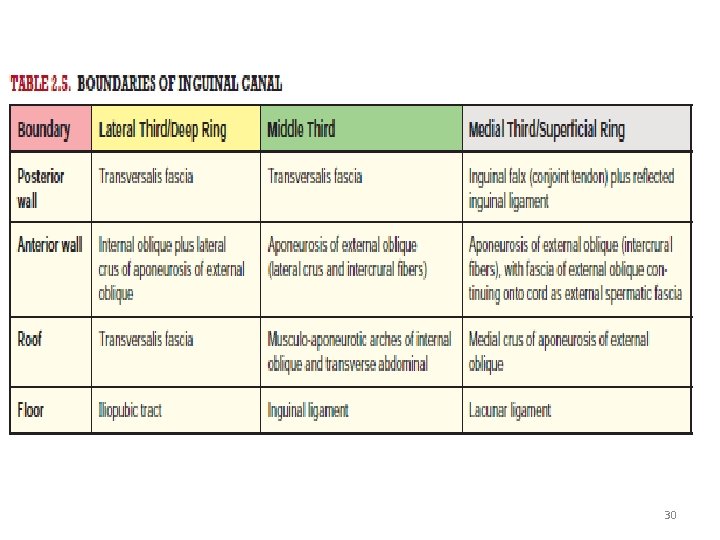
30
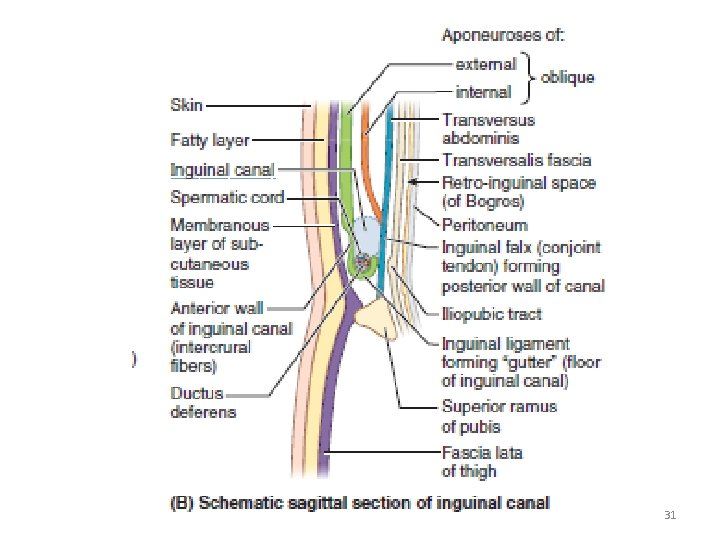
31

INGUINAL HERNIA • Protrusion of an organ or fascia through the walls of the that normally contains it eg inguinal region of the abdominal wall. 32

Indirect inguinal hernia • Commoner • Caused by failure of processus vaginalis to regress • Peritoneal sacs and loops of bowel enter or expand the inguinal canal through the deep inguinal ring (transversalis fascia) • Arises lateral to the inferior epigastric vessels. • Related to the congenital persistence of the vaginal process. • Acquired as a result of weakening of the lateral and posterior walls of the canal. • Small hernias are covered by the spermatic cord, internal spermatic fascia, external spermatic fascia and cremasteric muscle 33

Direct inguinal hernia • Peritoneal sac bulges into the inguinal canal via the posterior wall • Caused by weakness of the inguinal triangle in the medial posterior wall of the canal • Arises medial to the inferior epigastric vessels. • Acquired, usually in adulthood • Extend through the anterior wall of the canal or superficial ring. • Protrude through the transversalis fascia, between the conjoint tendon and the inferior epigastric vessels, and enter the inguinal canal. • Arise either between the fibres of the conjoint tendon • Covered by external spermatic fascia. 34

Femoral hernia • Protrudes through the femoral ring closed by a femoral septum, a weak spot. • In females, the ring is large and subject to changes during pregnancy, more common in women. • Section of intestine bulges through the ring and descends along the femoral canal to the saphenous opening. • Coverings of a femoral hernia are: peritoneum, femoral septum and sheath, cribriform fascia, superficial fascia and skin. • The intestine reaches only to the saphenous opening in incomplete femoral hernia. • Site of strangulation may be at the neck of the hernial sac; or it may be at the saphenous opening. 35

• A hernial sac passing lateral to the artery (i. e. through the deep ring) is an indirect hernia, one passing medial to the artery (through the inguinal triangle) is a direct hernia • Inguinal hernia emerges through the superficial inguinal ring it lies above and medial to the pubic tubercle • While the neck of a femoral hernia is below and lateral to the pubic tubercle. • Pubic tubercle distinguishes inguinal from femoral hernias 36

37

38
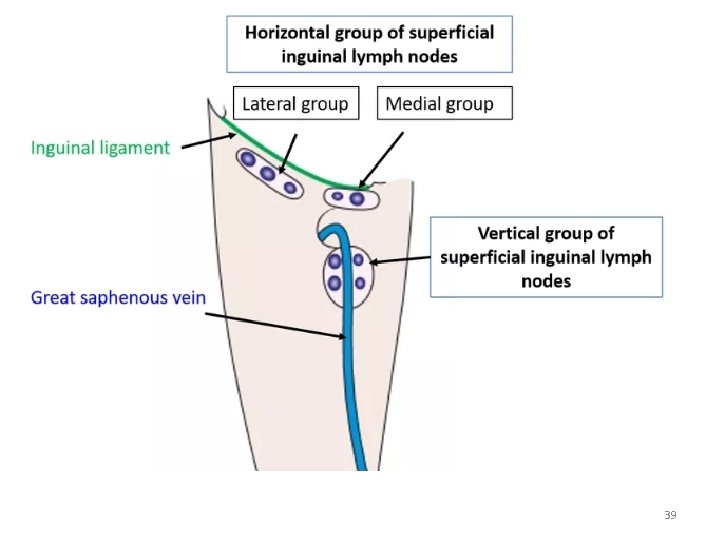
39
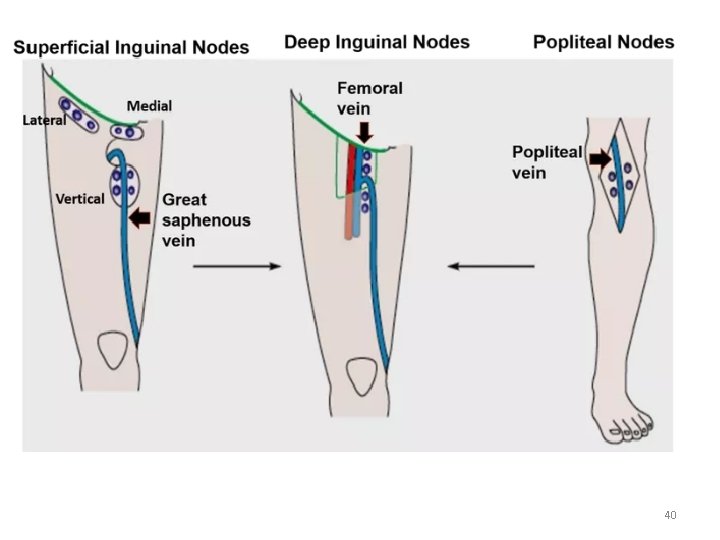
40

41

42

43
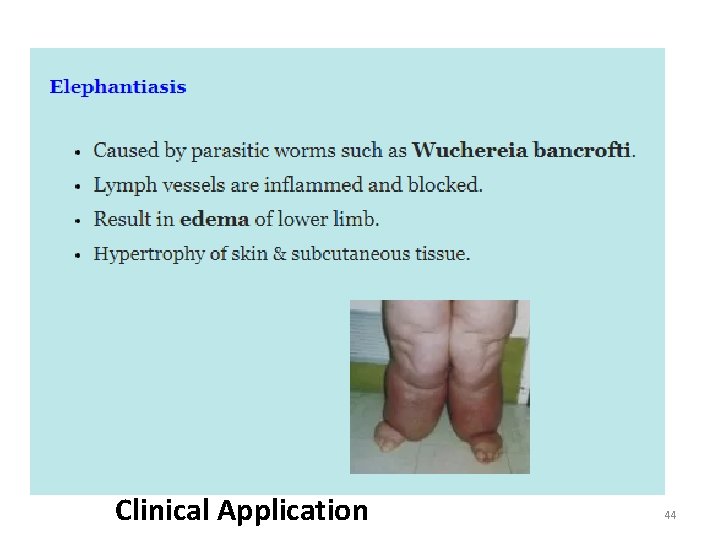
Clinical Application 44
- Slides: 44