OSTEOARTHRITIS DEGENERATIVE JOINT DISEASE DEFINITION Osteoarthritis OA is




































- Slides: 48

OSTEOARTHRITIS DEGENERATIVE JOINT DISEASE

DEFINITION Osteoarthritis OA is a degenerative joints disease, characterized by Breakdown of articular cartilage and proliferative changes of surrounding bones. Synovial inflammation OA is a chronic disease of the musculoskeletal system, without systemic involvement

EPIDEMIOLOGY Osteoarthritis(OA) is the most common joint disease OA of the knee joint is found in 70% of the population over 60 years of age Radiological evidence of OA can be found in over 90 % of the population

LIMITED FUNCTION OA may cause functional loss Activites of daily living (ADL) Most important cause of disability in old age Major indication for joint replacement surgery

CLASSIFICATION OF OA Primary OA Etiology is unknown Secondary OA Etiology is known

AGE Primary OA > 40 years Direct correlation Aging process

RISK FACTORS FOR PRIMARY OA Age Sex Obesity Genetics Trauma (daily)

SECONDARY OSTOARTHRITIS Trauma Previous joint disorders; Congenital hip dislocation Infection: Septic arthritis, Brucella, Tb Inflammatory: RA Metabolic: Gout Hematologic: Hemophilia Endocrine: DM

ETIOLOGY OF OA Cartilage properties Biomechanical problem

OA: Symptoms and Signs Pain is related to use Pain gets worse during the day Minimal morning stiffness (<20 min) and after inactivity (gelling) Range of motion decreases Joint instability Bony enlargement Deformity – restricition of ADL Restricted movement Crepitus Variable swelling and/or instability

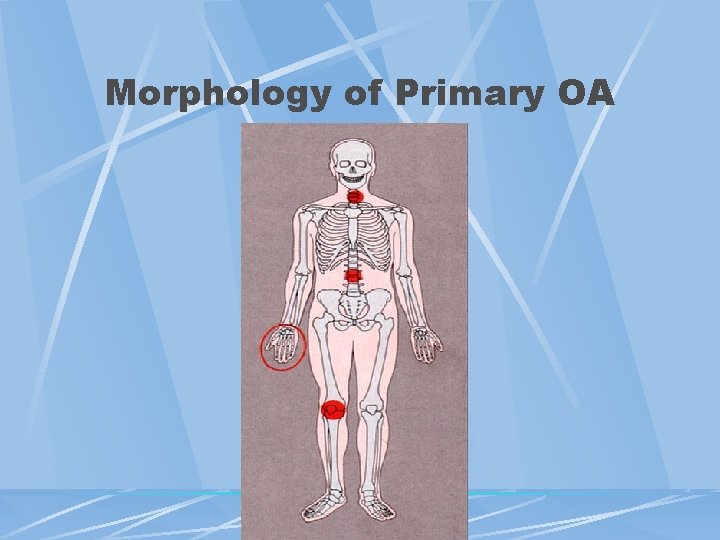
Morphology of Primary OA

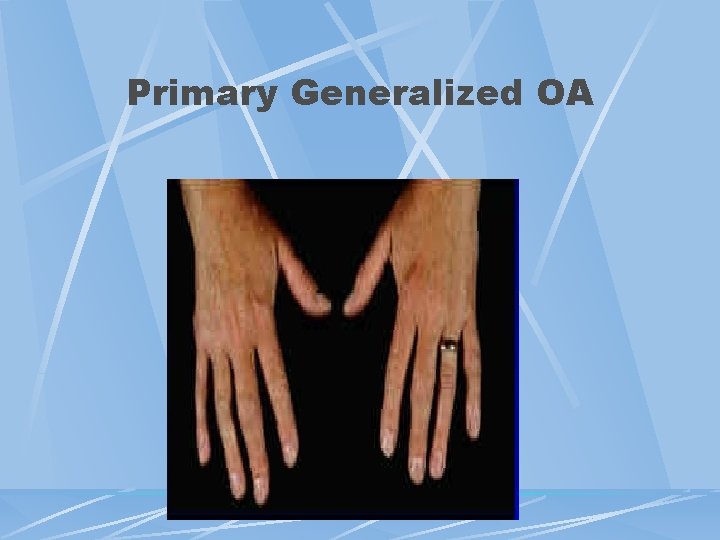
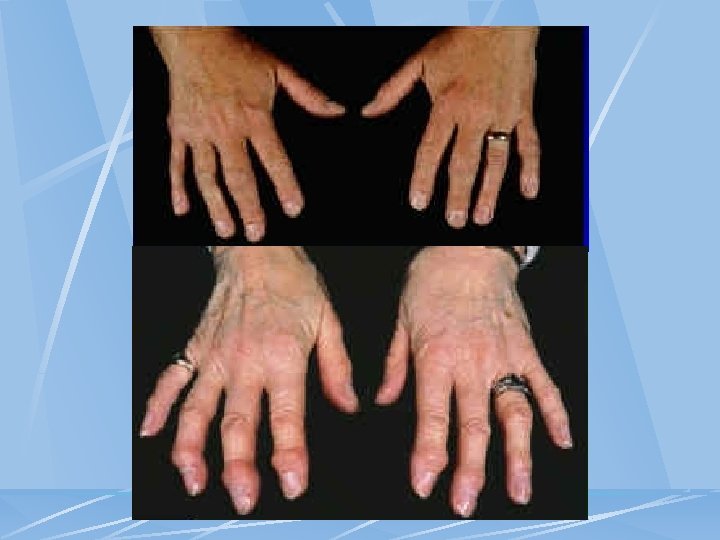
Primary Generalized OA


LABORATORY FINDINGS OF OA There are no pathognomonic laboratory findings for OA Laboratory analysis is performed for differential diagnosis

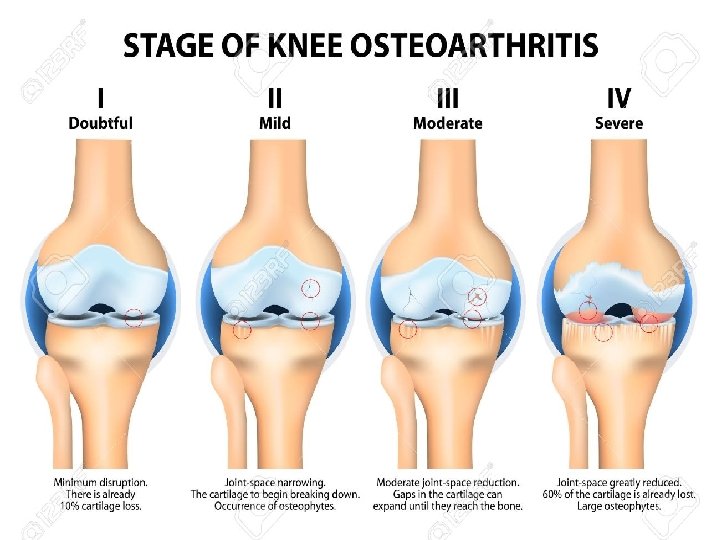
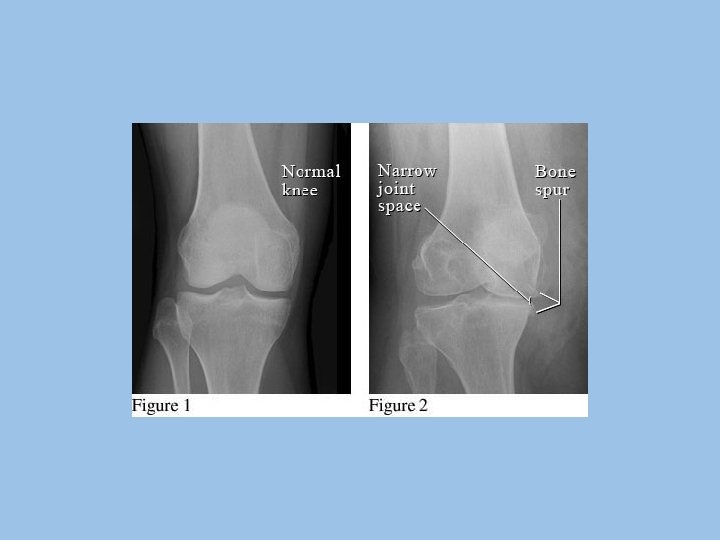
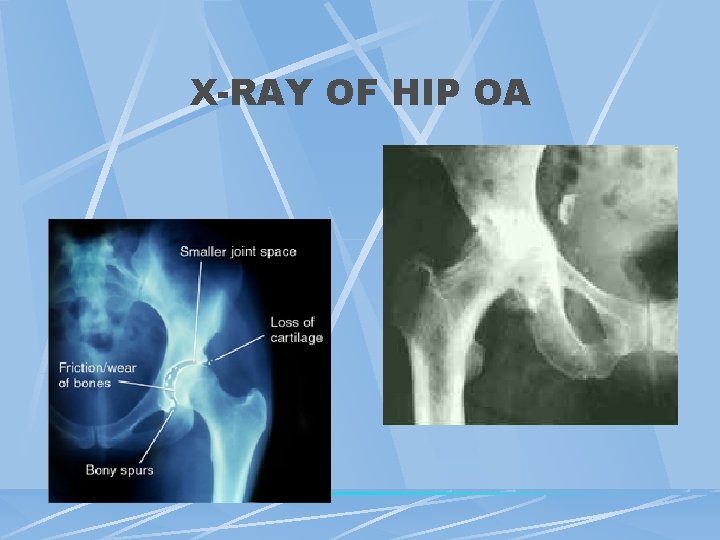
RADIOLOGIC FINDINGS OF OA Narrowing of joint space (due to loss of cartilage) Osteophytes Subchondral (paraarticular) sclerosis Bone cysts

RADIOLOGIC GRADE OF OA G 1 G 2 G 3 G 4 Normal Mild Moderate Severe Kellgren Lawrence Classification


DIAGNOSIS OF OA CLINICAL FINDINGS Joint pain + RADIOLOGIC FINDINGS Osteophytes

OA OF KNEE JOINT More common in obese females over 50 years of age Joint stiffness (<30 minutes) Mechanical pain Physical examination findings: Crepitus Pain on pressure Painful ROM and functional limitation Limitation of ROM in later stages of OA (first extension) Laboratory analysis within normal limits



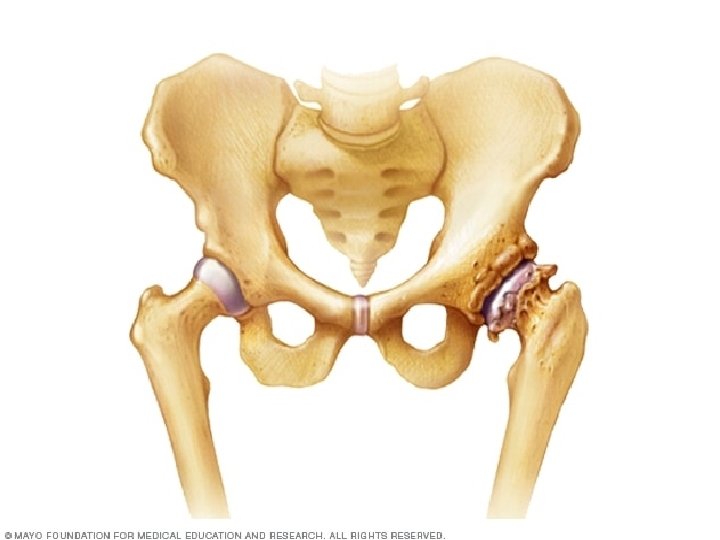
OA OF HIP JOINT More common in males over 40 years of age Joint stiffness Pain of hip, gluteal and groin areas radiating to the knee Mechanical pain Limited walking function

Hip Osteoarthritis Physical examination: Antalgic limping Limitation of ROM Painful ROM Leg length discrepancy Laboratory analysis within normal limits


X-RAY OF HIP OA

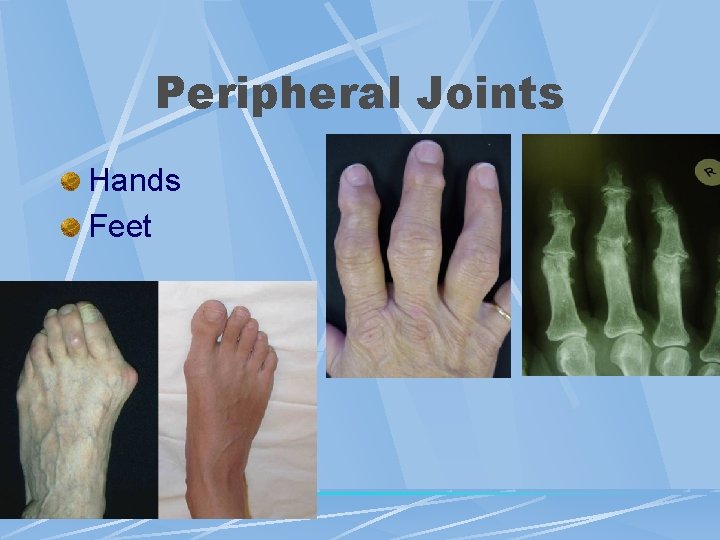
Peripheral Joints Hands Feet

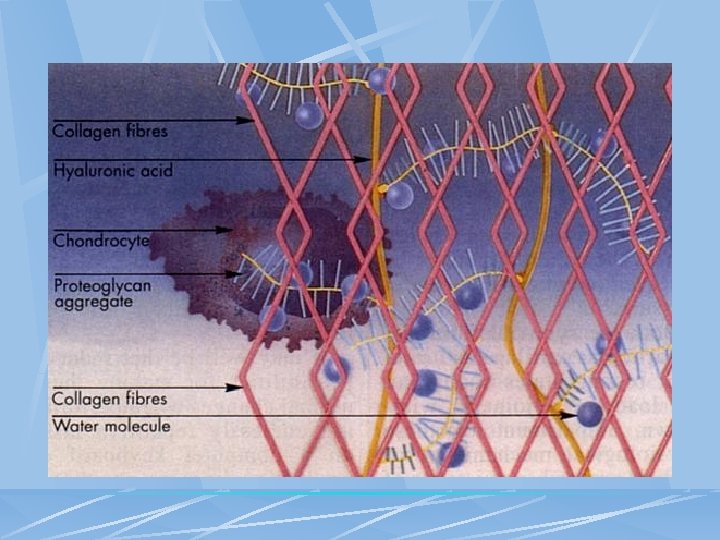
STRUCTURE OF JOINT CARTILAGE Collagen (Type 2) Proteoglycan - Hyaluronic acid - Glycoseaminoglycan Water Condrocyte Regeneration and Degeneration


ETIOPATHOGENESIS OF OA Age, gender Local Genetic biochemical Other factors OA effects

ETIOPATHOGENESIS OF OA Dysfunction of joint cartilage Condrocyte function: 1 - Degredative enzymes (metalloproteases) 2 - Inhibitors Degeneration and regeneration functions are balanced IL-1 , degredative enzymes + synovial inflammation results: Breakdown of cartilage

PATHOGENESIS OF OA Cytokines IL-1, IL-6, TNF- Cell destruction Membrane phospholipids Arachidonic acid Cox-1, Cox-2

IL-1 and metalloproteases have been found to play an important role in cartilage destruction. Local growth factors, especially transforming growth factor (TGF) are involved in the formation of osteophytes

TREATMENT OF OA Symptomatic treatment Structure modifying treatment Surgical treatment

PRIMARY PREVENTION OF OA ? ? Regular exercises Weight control Prevention of trauma

AIMS OF OA TREATMENT Pain relief Preservation and restoration of joint function Education

Non-Pharmacologic Treatment of OA Patient education Weight loss (if overweight) Aerobic exercise programs Physical therapy Range-of-motion exercises Muscle-strengthening exercises Assistive devices for ambulation Appropriate footwear Lateral-wedged insoles Bracing Occupational therapy Joint protection and energy conservation

Pharmacologic Management of OA Non-opioid analgesics Topical agents Intra-articular agents Opioid analgesics NSAIDs Unconventional therapies

Non-opioid Analgesic Therapy First-line—Acetaminophen • • • Pain relief comparable to NSAIDs, less toxicity Beware of toxicity from use of multiple acetaminophen-containing products Maximum safe dose = 4 grams/day

Non-opioid Analgesic Therapy (cont’d) NSAIDs • • Use generic NSAIDs first If no response to one may respond to another Lower doses may be effective Do not retard disease progression Gastroprotection increases expense Side effects: GI, renal, worsening CHF, edema Antiplatelet effects may be hazardous

Non-opioid Analgesics in OA Cyclooxygenase-2 (COX-2) inhibitors • • • Pain relief equivalent to older NSAIDs Probably less GI toxicity Side effects: Renal, edema Older populations with multiple CV medical problems should be tested Cost similar to generic NSAIDs plus proton pump inhibitor or misoprostol

Opioid Analgesics in OA Tramadol • • Affects opioid and serotonin pathways Nonulcerogenic May be added to NSAIDs, acetaminophen Side effects: Nausea, vomiting, lowered seizure threshold, rash, constipation, drowsiness, dizziness

Opioid Analgesics for OA Codeine, oxycodone • Long-acting oxycodone may have fewer CNS side effects Propoxyphene Morphine and fentanyl patches for severe pain interfering with daily activity and sleep

Topical Agents for Analgesia in OA Local cold or heat: Hot packs, hydrotherapy Capsaicin-containing topicals • • Use well supported by evidence Use daily for up to 2 weeks before benefit Compliance poor without full instruction Avoid contact with eyes Liniments = methyl salicylates • Temporary benefit

OA: Intra-articular Therapy Intra-articular steroids • Good pain relief • Most often used in knees, up to q 3 months • With frequent injections; risk infection, worsening diabetes, or CHF Joint lavage • Significant symptomatic benefit demonstrated Hyaluronate injections • Symptomatic relief • Improved function • Require series of injections • No evidence of longterm benefit • Limited to knees • Expensive

OA: Unconventional Therapies Polysulfated glycosaminoglycans— nutriceuticals • Glucosamine +/- chondroitin sulfate: Symptomatic benefit, no known side effects, long-term controlled trials pending Tetracyclines as protease/cytokine inhibitors • • Under study Have disease-modifying potential

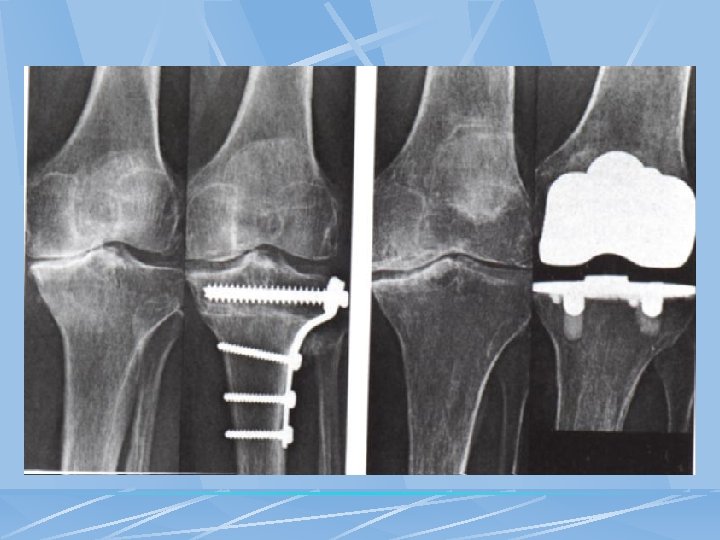
Surgical Therapy for OA Arthroscopy • • • May reveal unsuspected focal abnormalities Results in tidal lavage Expensive, complications possible Osteotomy: May delay need for TKR for 2 to 3 years Total joint replacement: When pain severe and function significantly limited

OA: Management Summary First: Be sure the pain is joint related (not a tendonitis or bursitis adjacent to joint) Initial treatment • • Muscle strengthening exercises and reconditioning walking program Weight loss Acetaminophen first Local heat/cold and topical agents

OA: Management Summary (cont’d) Second-line approach • • • NSAIDs if acetaminophen fails Intra-articular agents or lavage Opioids Third-line • • • Arthroscopy Osteotomy Total joint replacement