Osteoarthritis By Sara Anderson Osteoarthritis AKA Degenerative joint

Osteoarthritis By: Sara Anderson

Osteoarthritis AKA: Degenerative joint disease (DJD) Hypertrophic arthritis Osteoarthrosis Senescent arthritis. Primary cause is unknown Secondary cause: Trauma Infections Previous fractures Rheumatoid arthritis Stress on weightbearing joints from obesity Or certain occupations

Osteoathritis Osteoarthritis is a nonsystemic, noninflammatory disorder that progressively causes bones and joints to degenerate. Surface layer of cartilage breaks down and wears away. Allows bones under cartilage to rub together
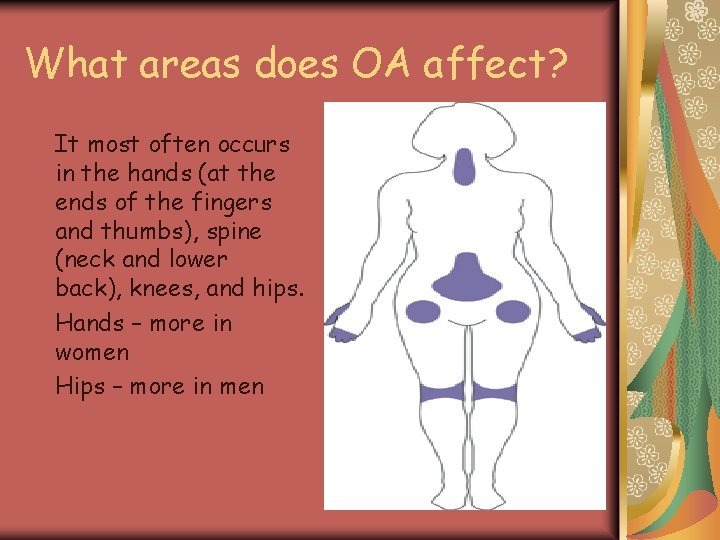
What areas does OA affect? It most often occurs in the hands (at the ends of the fingers and thumbs), spine (neck and lower back), knees, and hips. Hands – more in women Hips – more in men

Assessment Subjective: Pain and stiffness (which is usually relieved with rest in early stages) Past illnesses Surgical procedures Trauma Excessive weight gain C/O muscle spasms Reduced grip strength Lifestyle effects may include: Depression Anxiety Feelings of helplessness Limitations of ADL’s Job limitations Difficulty participating in everyday personal and family joys and responsibilities

Assessment Objective: Joint edema, tenderness, and deformity. Heberden’s nodes Bouchard’s nodes Gait will reveal a limp (especially if hips are involved)
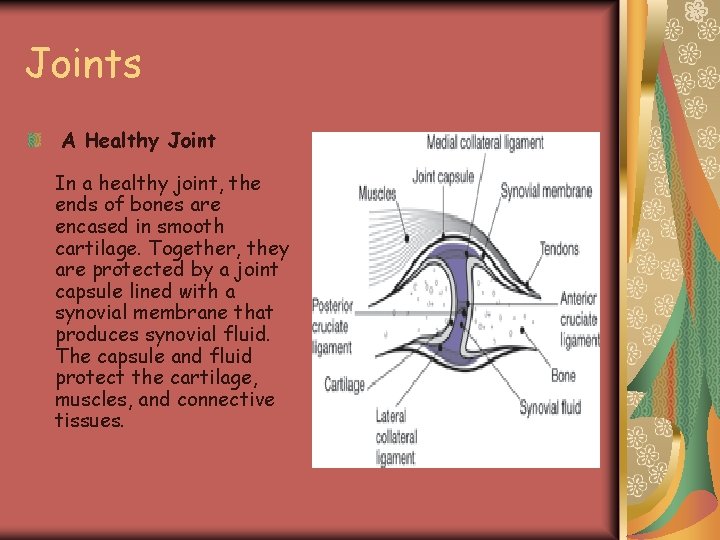
Joints A Healthy Joint In a healthy joint, the ends of bones are encased in smooth cartilage. Together, they are protected by a joint capsule lined with a synovial membrane that produces synovial fluid. The capsule and fluid protect the cartilage, muscles, and connective tissues.
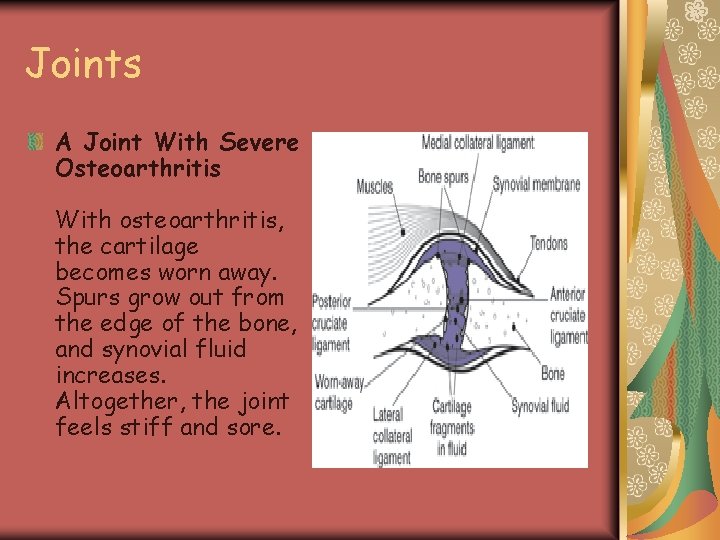
Joints A Joint With Severe Osteoarthritis With osteoarthritis, the cartilage becomes worn away. Spurs grow out from the edge of the bone, and synovial fluid increases. Altogether, the joint feels stiff and sore.

Diagnosis There is no single test to diagnose osteoarthritis. Combination of following methods to rule out other conditions: Physical Exam X- Rays MRI Arthroscopy Synovial fluid exam Bone Scan Clinical History

Four Main Goals of Treatment To control pain To improve joint function To maintain normal body weight To achieve a healthy lifestyle

Treatment Approaches Weight Control Rest and relief from stress on joints Medications to control pain Surgery Complementary and alternative therapies Nondrug pain relief Heat and cold therapy TENS Massage

Treatment Approaches Exercise Strengthening exercises Aerobic activities ROM activities Agility exercises Physical Therapy Gait enhancers

Medical Management Large doses of salicylates (ASA) or NSAID’s (ie Motrin) Steroids (Cortisone) Glucosamine Lubricant and shock absorber necessary for repairing and maintaining healthy joint function.
Surgical Interventions Osteotomy: bone is cut to shorten, lengthen or change it’s alignment Joint replacement Arthroplasty

Nursing Interventions and Patient Teaching Maintain ADL’s Encourage to alternate sitting, standing and walking Encourage rest periods Weight reduction plan (if needed) Splints Guaiac test on stool and emesis for presence of occult blood

Prognosis Osteoarthritis is a chronic disease that ultimately causes permanent destruction of affected cartilage and underlying bone with variable pain and disability.
- Slides: 16