Orthotic Devices Orthotic Devices Definition An orthosis is





















- Slides: 68

Orthotic Devices

Orthotic Devices -Definition An orthosis is a mechanical device that applies forces to the body in an effort to: support limit stabilize moving parts assist and improve motion correct and align deformities prevent and protect susceptible areas.

Orthotic Devices -Definition “orthos” - straight, normal, or true.

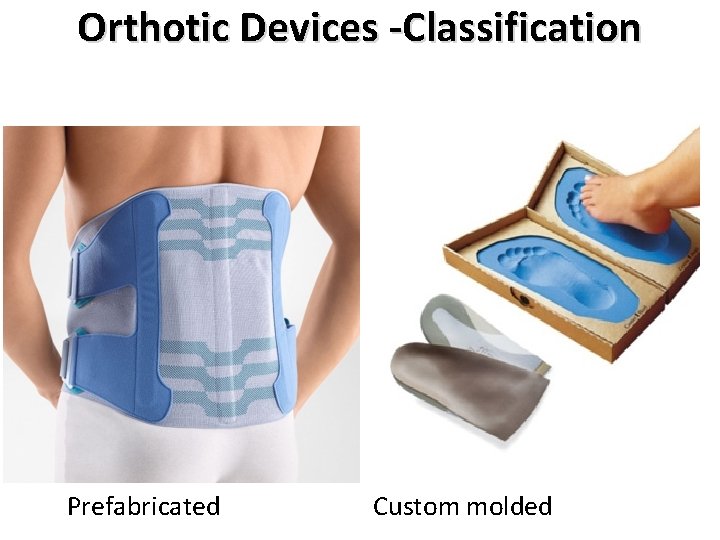
Orthotic Devices -Classification Prefabricated Custom molded

Orthotic Device -Prescription The prescription of an orthosis requires an understanding of the pathology of the disorder to be treated and must take into account: Goals to be achieved Knowledge of anatomy, biomechanics, and kinesiology Understanding of the indications (positive effects) and limitations (negative effects) of the orthosis

Upper Limb Orthosis-Classification ü Static ü Dynamic ü Hybrid

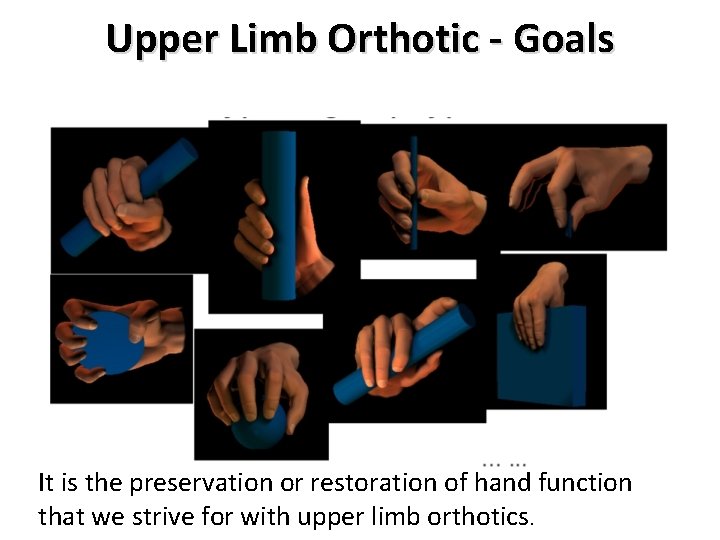
Upper Limb Orthotic - Goals It is the preservation or restoration of hand function that we strive for with upper limb orthotics.

Upper Limb Orthotic Goals Five common goals for upper limb orthotics: 1. Substitute for weak or absent muscles 2. Protect damaged or diseased segments by limiting load or motion 3. Prevention of deformity 4. Correction of contracture 5. Attachment of other assistive devices

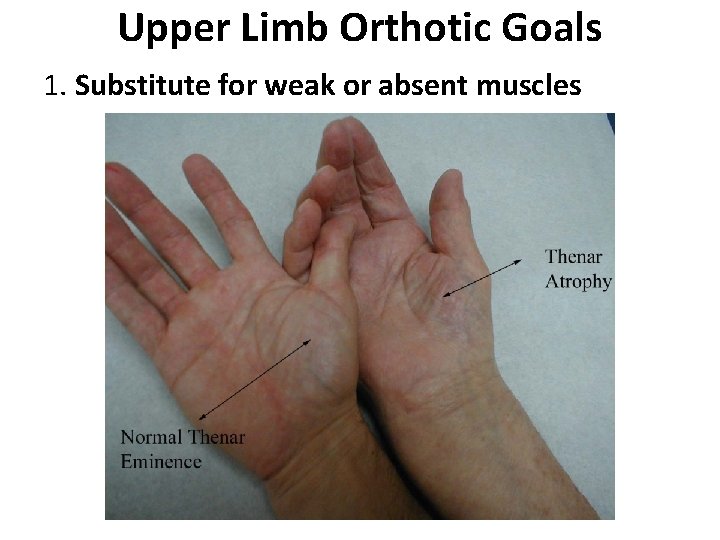
Upper Limb Orthotic Goals 1. Substitute for weak or absent muscles

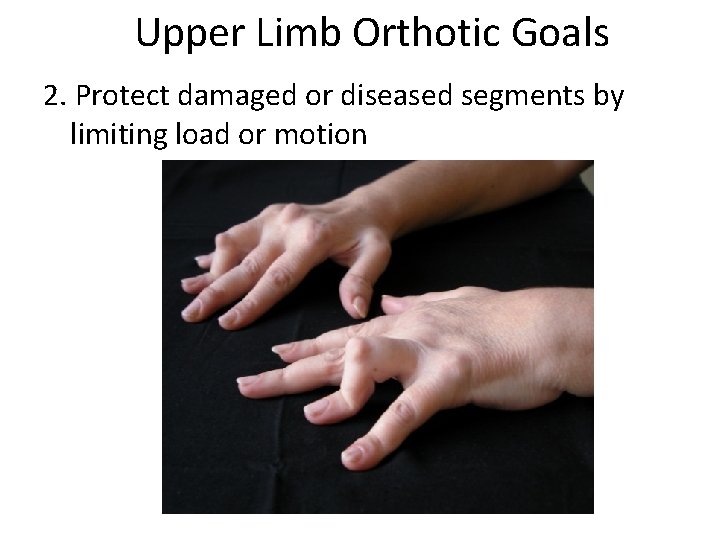
Upper Limb Orthotic Goals 2. Protect damaged or diseased segments by limiting load or motion

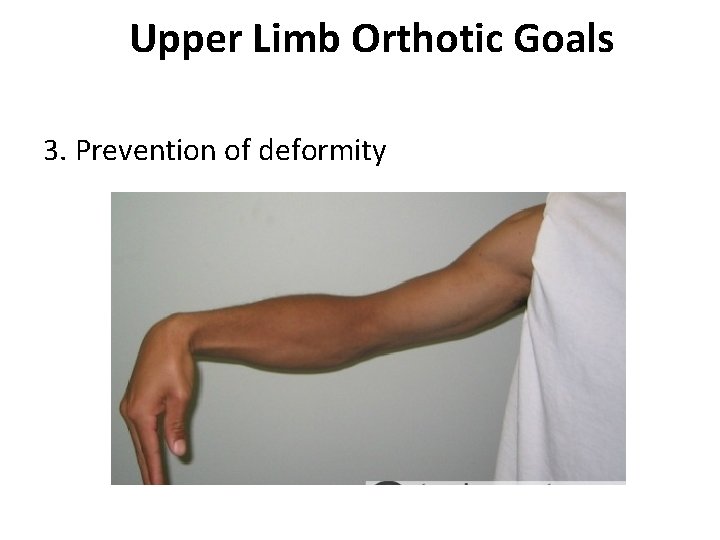
Upper Limb Orthotic Goals 3. Prevention of deformity

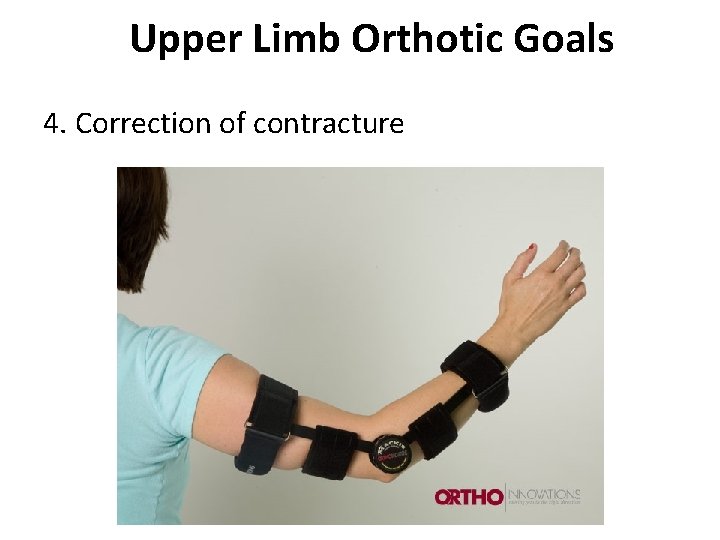
Upper Limb Orthotic Goals 4. Correction of contracture

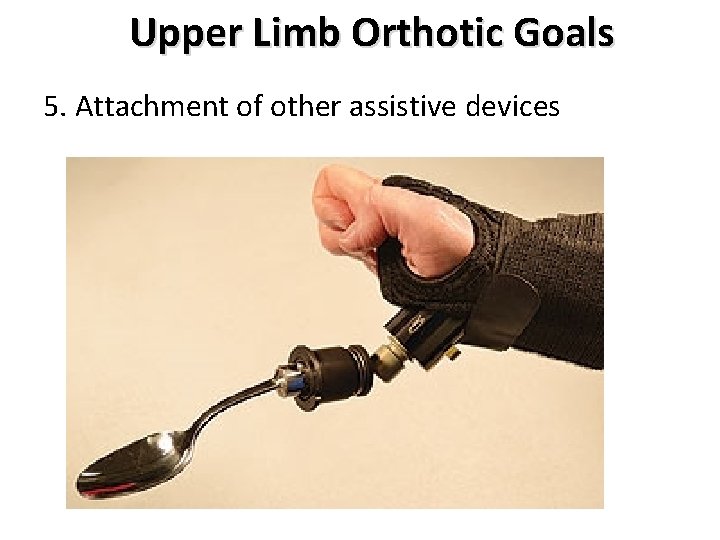
Upper Limb Orthotic Goals 5. Attachment of other assistive devices

Orthotic Devices -Bimechanical Principles The five principles include: 1. Three-point control concept 2. Tissue tolerance to compression and shear forces 3. The biomechanics of levers and forces 4. Selection of materials 5. Static versus dynamic control

Bimechanical Principles 1. Three-point control concept

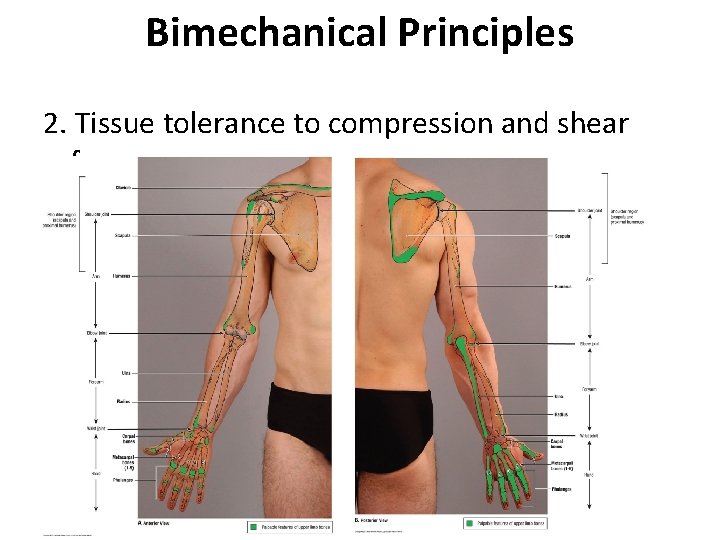
Bimechanical Principles 2. Tissue tolerance to compression and shear forces

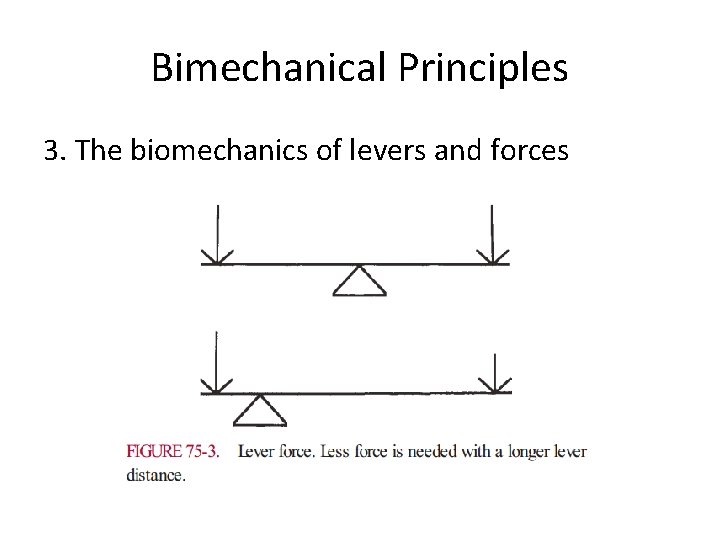
Bimechanical Principles 3. The biomechanics of levers and forces

Bimechanical Principles 4. Selection of materials

Bimechanical Principles 5. Static versus dynamic control

Anatomical principles

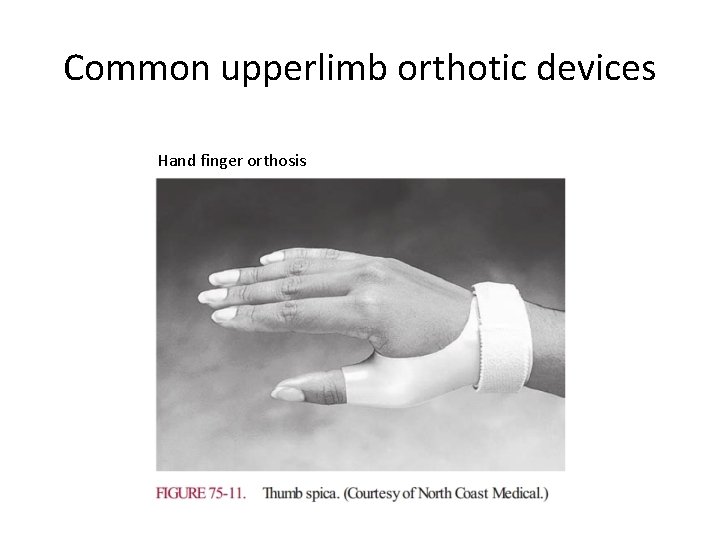
Common upperlimb orthotic devices Hand finger orthosis

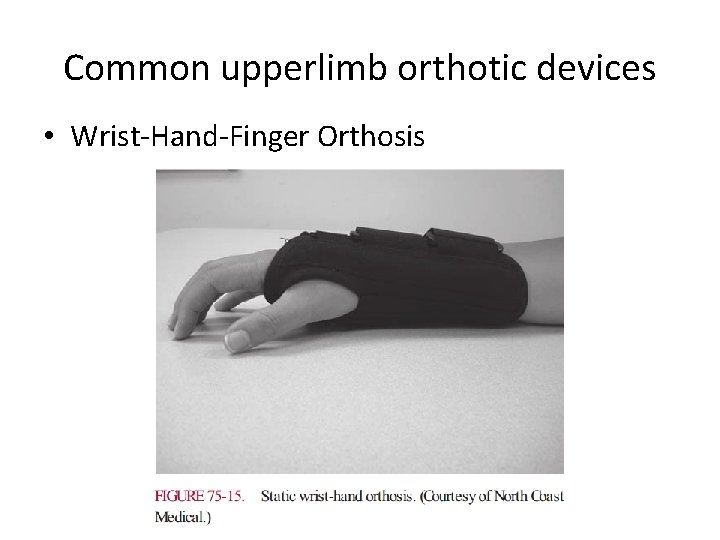
Common upperlimb orthotic devices • Wrist-Hand-Finger Orthosis

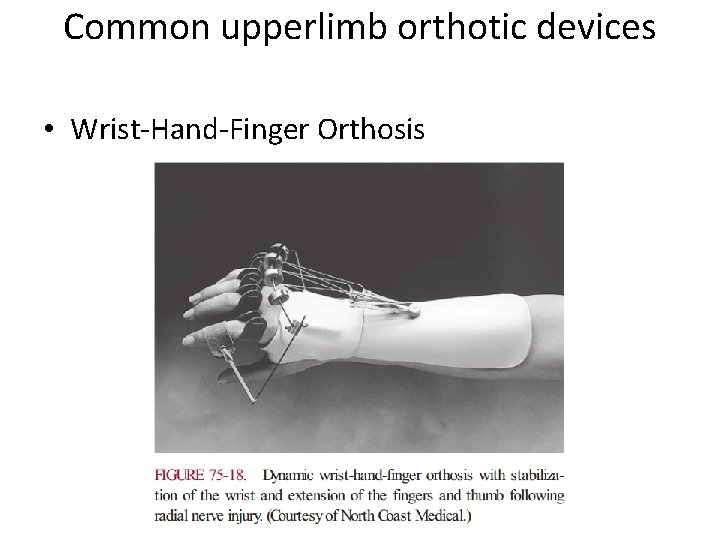
Common upperlimb orthotic devices • Wrist-Hand-Finger Orthosis

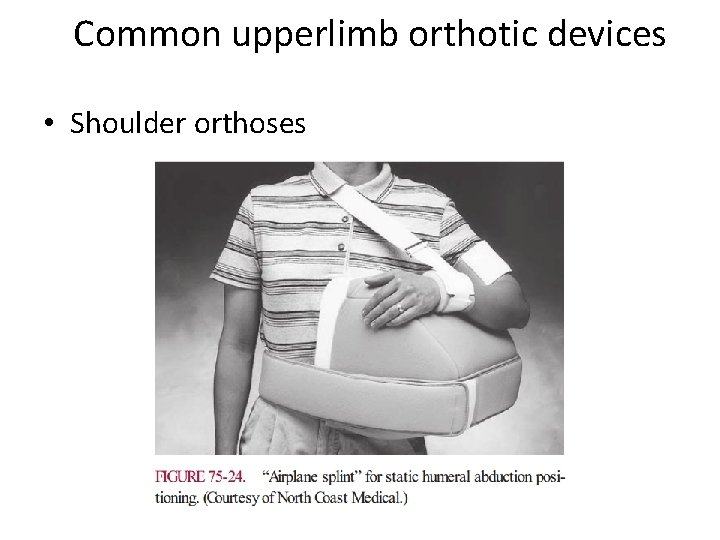
Common upperlimb orthotic devices • Shoulder orthoses

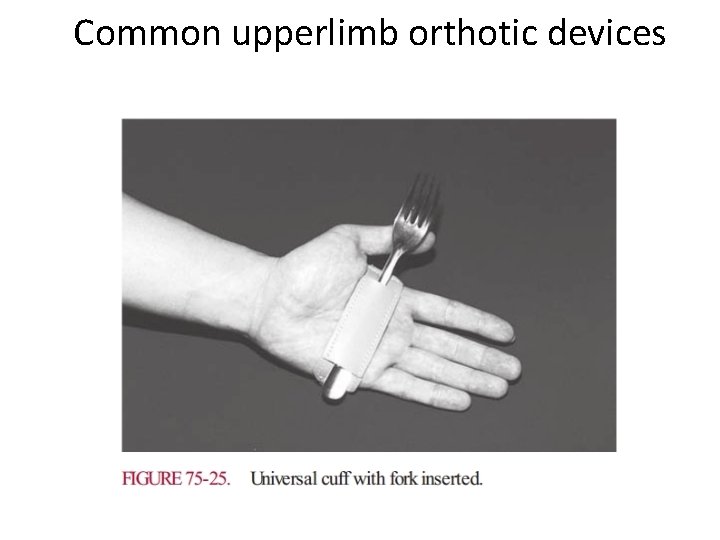
Common upperlimb orthotic devices

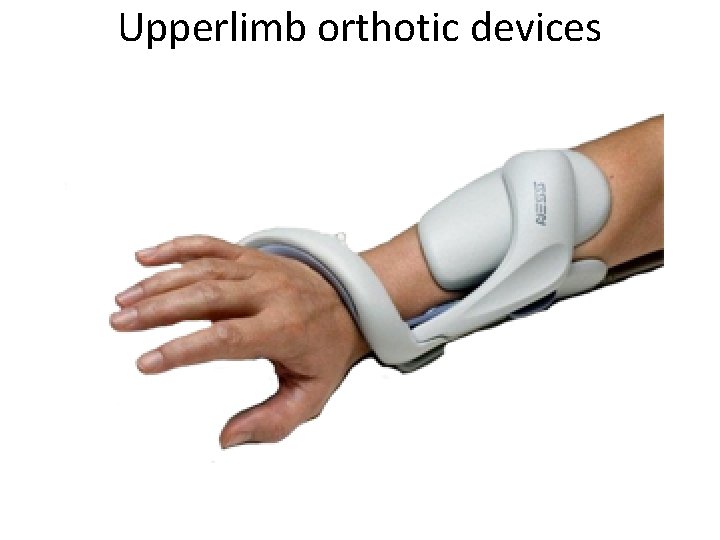
Upperlimb orthotic devices

Radial nerve palsy What could possibly go wrong? Ana Poljičanin, MD. Ph. D. 1, 2 , PMR resident Mentor: Asja Tukić, MD. MSc. 1 Department of Physical Medicine and Rehabilitation University Hospital Split, Croatia 1 School of Medicine University of Split, Croatia 2 AAF Salzburg, June 2015.

Case characteristics Male, 32 years 05. 2014. high speed motor vehicle accident § Polytrauma § Humeral shaft fracture § Left arm paralysis: Brachial plexus contusion Radial nerve transection § II-IV left carpometacarpal joint subluxation § Fracture of left proximal phalanx of index finger

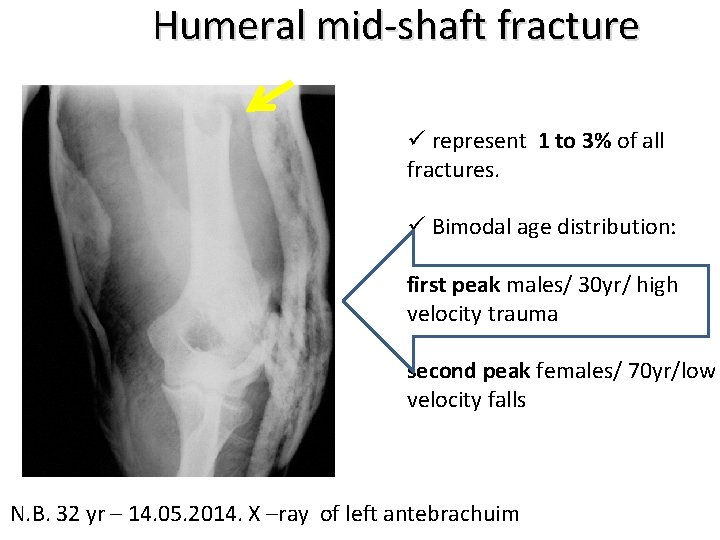
Humeral mid-shaft fracture ü represent 1 to 3% of all fractures. ü Bimodal age distribution: first peak males/ 30 yr/ high velocity trauma second peak females/ 70 yr/low velocity falls N. B. 32 yr – 14. 05. 2014. X –ray of left antebrachuim

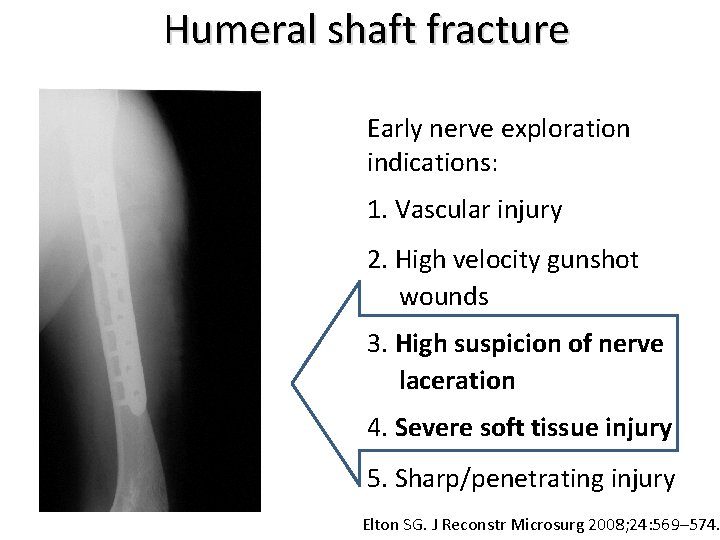
Humeral shaft fracture Early nerve exploration indications: 1. Vascular injury 2. High velocity gunshot wounds 3. High suspicion of nerve laceration 4. Severe soft tissue injury 5. Sharp/penetrating injury Elton SG. J Reconstr Microsurg 2008; 24: 569– 574.

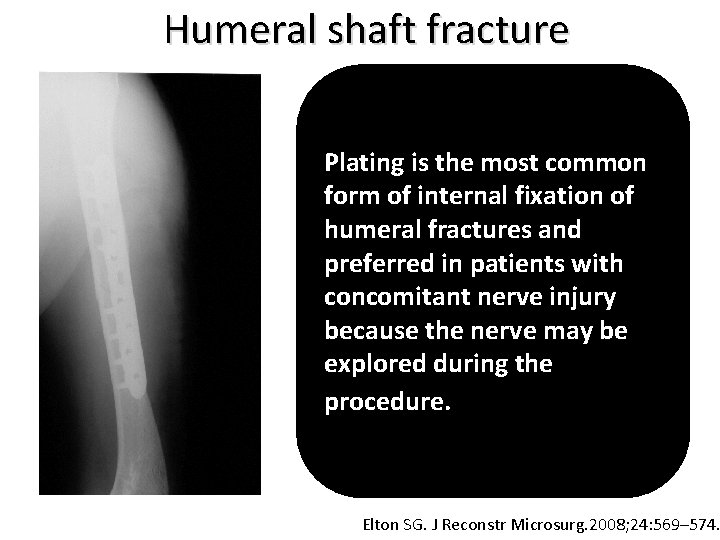
Humeral shaft fracture Plating is the most common form of internal fixation of humeral fractures and preferred in patients with concomitant nerve injury because the nerve may be explored during the procedure. . Elton SG. J Reconstr Microsurg. 2008; 24: 569– 574.

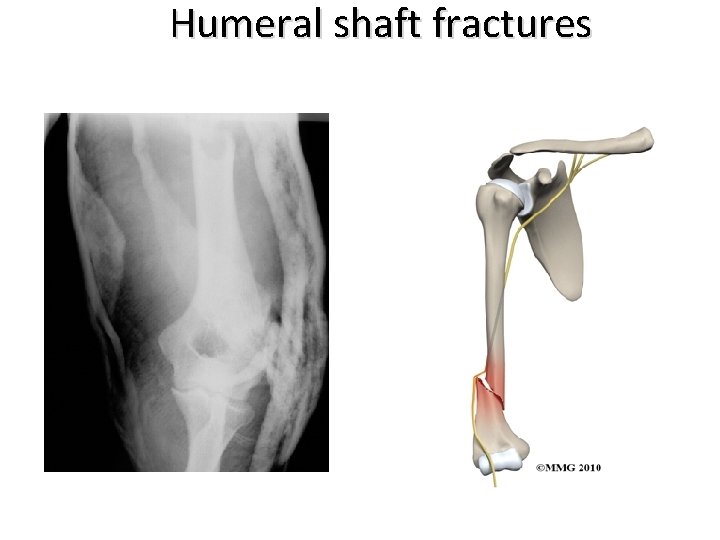
Humeral shaft fractures

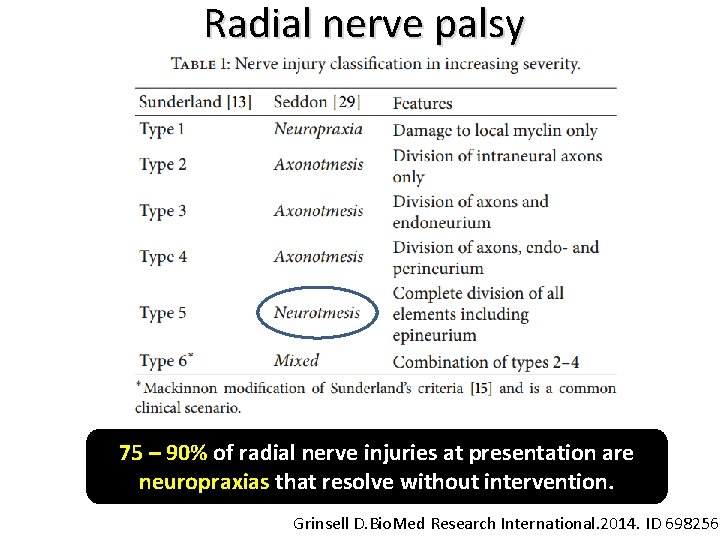
Radial nerve palsy 75 – 90% of radial nerve injuries at presentation are neuropraxias that resolve without intervention. Grinsell D. Bio. Med Research International. 2014. ID 698256

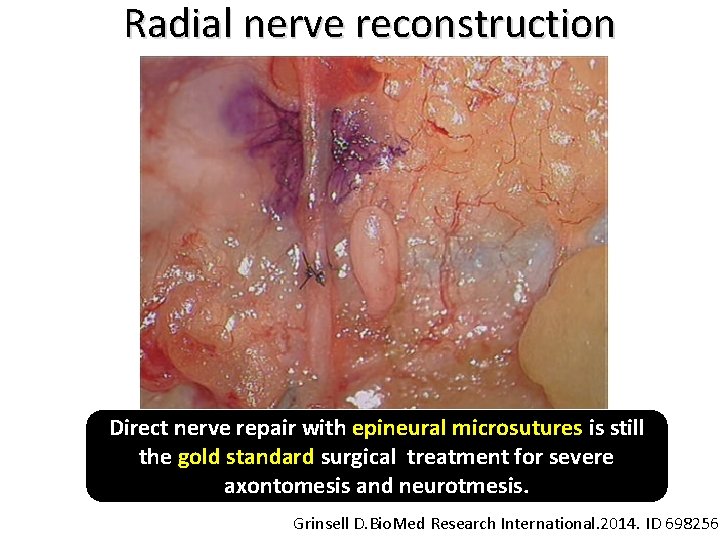
Radial nerve reconstruction Direct nerve repair with epineural microsutures is still the gold standard surgical treatment for severe axontomesis and neurotmesis. Grinsell D. Bio. Med Research International. 2014. ID 698256

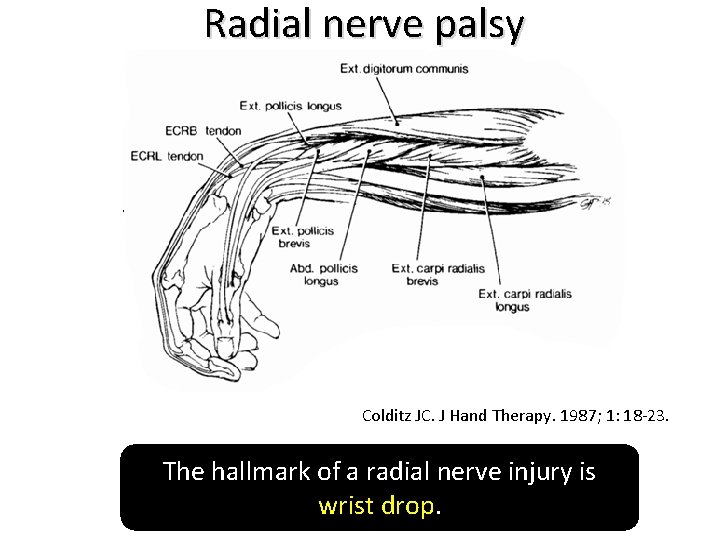
Radial nerve palsy Colditz JC. J Hand Therapy. 1987; 1: 18 -23. The hallmark of a radial nerve injury is wrist drop.

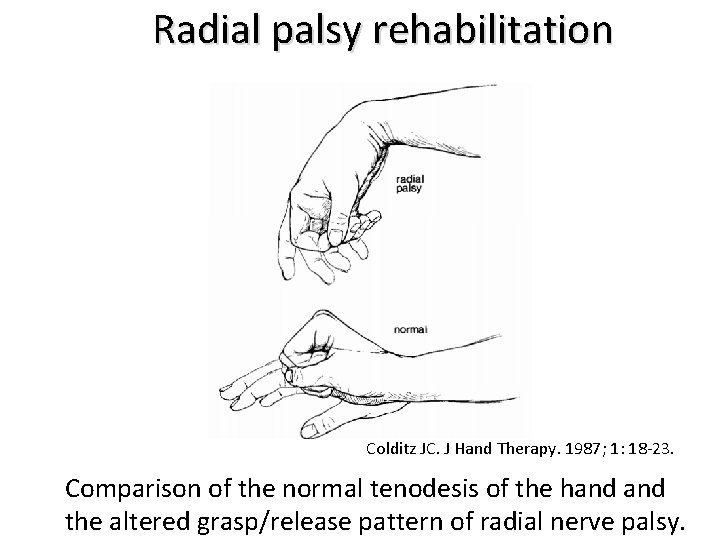
Radial palsy rehabilitation Colditz JC. J Hand Therapy. 1987; 1: 18 -23. Comparison of the normal tenodesis of the hand the altered grasp/release pattern of radial nerve palsy.

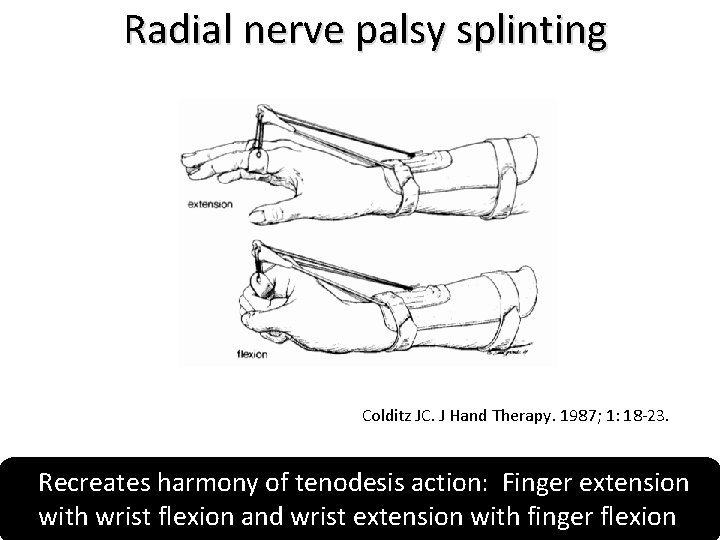
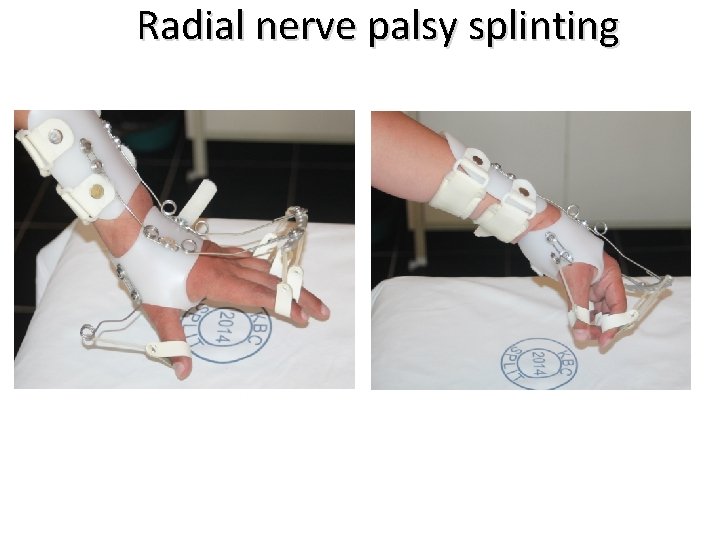
Radial nerve palsy splinting Colditz JC. J Hand Therapy. 1987; 1: 18 -23. Recreates harmony of tenodesis action: Finger extension with wrist flexion and wrist extension with finger flexion.

Radial nerve palsy splinting

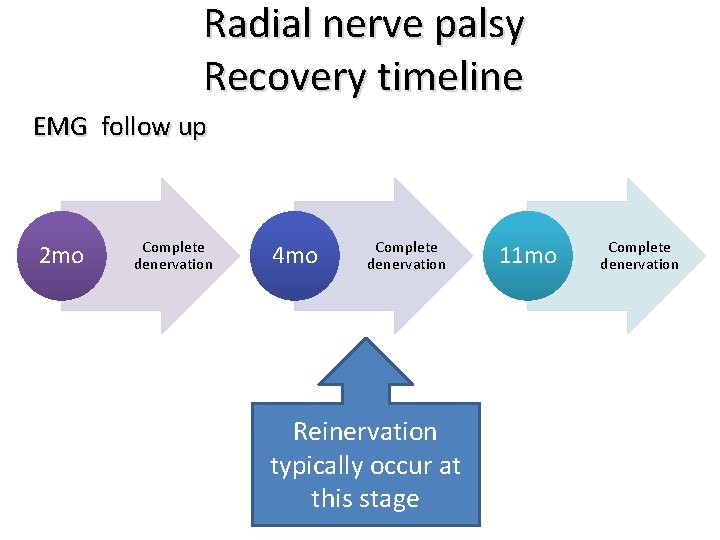
Radial nerve palsy Recovery timeline EMG follow up 2 mo Complete denervation 4 mo Complete denervation Reinervation typically occur at this stage 11 mo Complete denervation

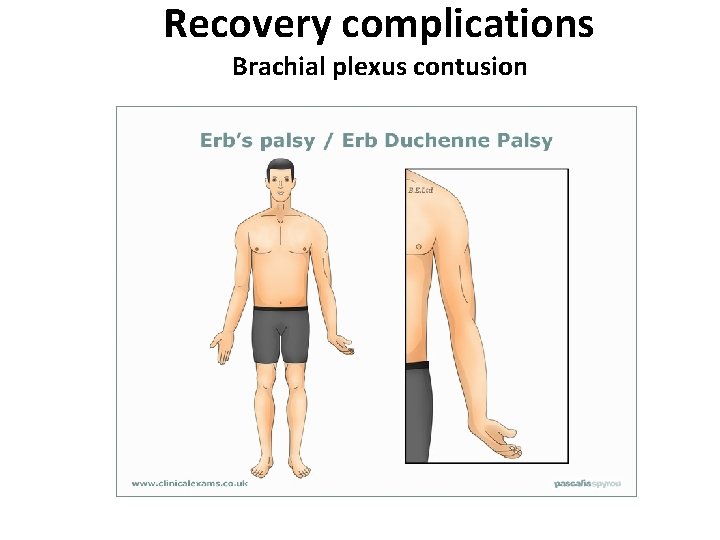
Recovery complications Brachial plexus contusion

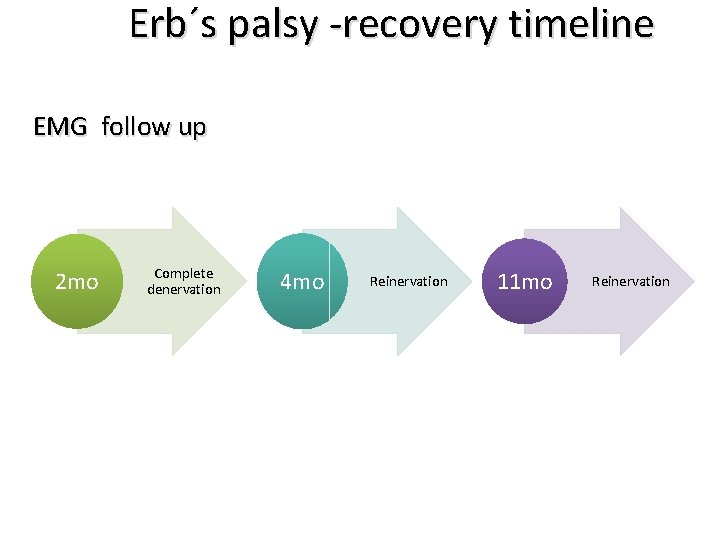
Erb´s palsy -recovery timeline EMG follow up 2 mo Complete denervation 4 mo Reinervation 11 mo Reinervation

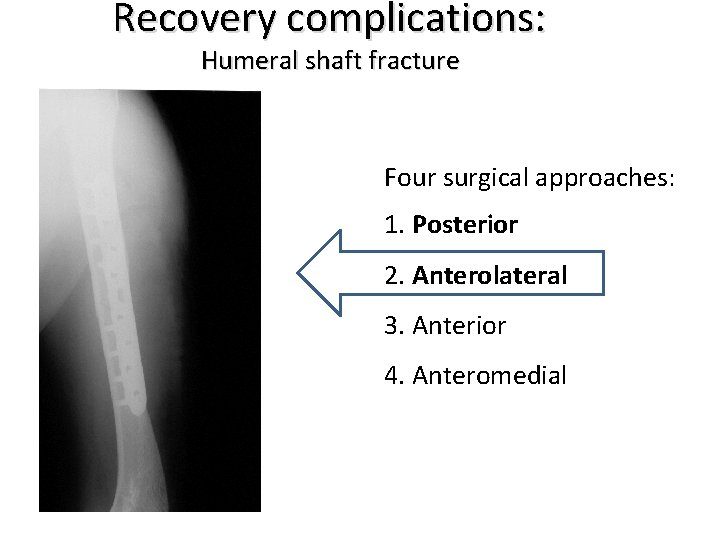
Recovery complications: Humeral shaft fracture Four surgical approaches: 1. Posterior 2. Anterolateral 3. Anterior 4. Anteromedial

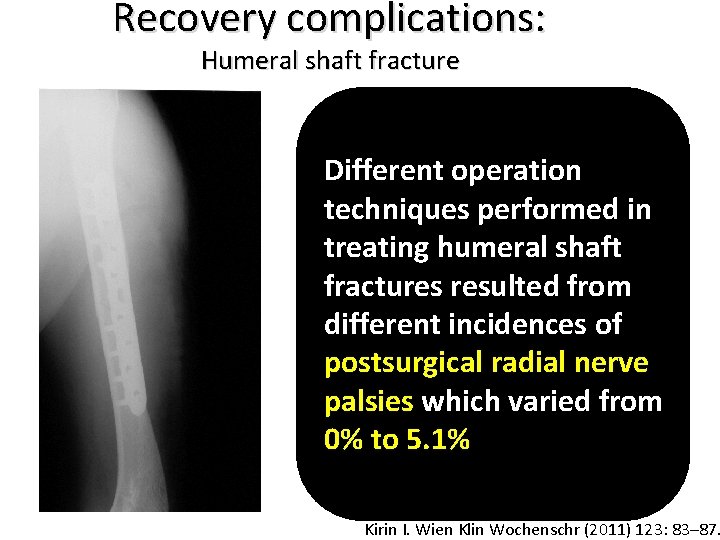
Recovery complications: Humeral shaft fracture Different operation techniques performed in treating humeral shaft fractures resulted from different incidences of postsurgical radial nerve palsies which varied from 0% to 5. 1% Kirin I. Wien Klin Wochenschr (2011) 123: 83– 87.

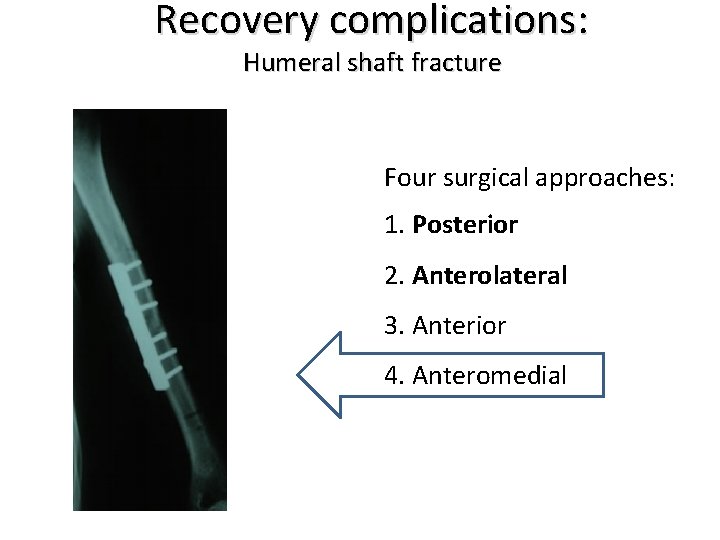
Recovery complications: Humeral shaft fracture Four surgical approaches: 1. Posterior 2. Anterolateral 3. Anterior 4. Anteromedial

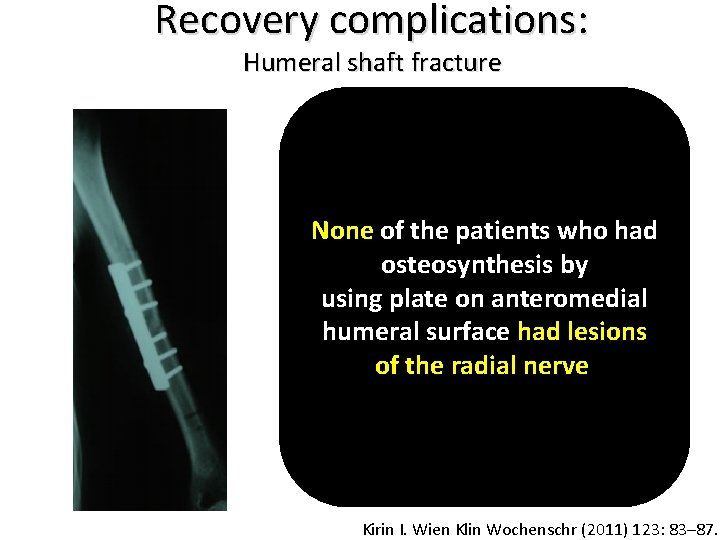
Recovery complications: Humeral shaft fracture None of the patients who had osteosynthesis by using plate on anteromedial humeral surface had lesions of the radial nerve. Kirin I. Wien Klin Wochenschr (2011) 123: 83– 87.

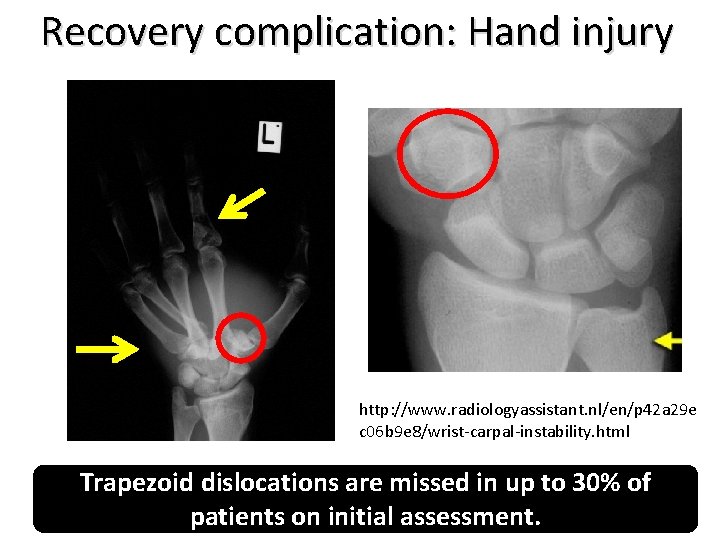
Recovery complication: Hand injury http: //www. radiologyassistant. nl/en/p 42 a 29 e c 06 b 9 e 8/wrist-carpal-instability. html Trapezoid dislocations are missed in up to 30% of patients on initial assessment.

What the future brings? ü Removal of osteosynthetic material ü Intensive rehabilitation ü How long should we wait for nerve recovery to occur? ü When should we consult plastic surgeon?

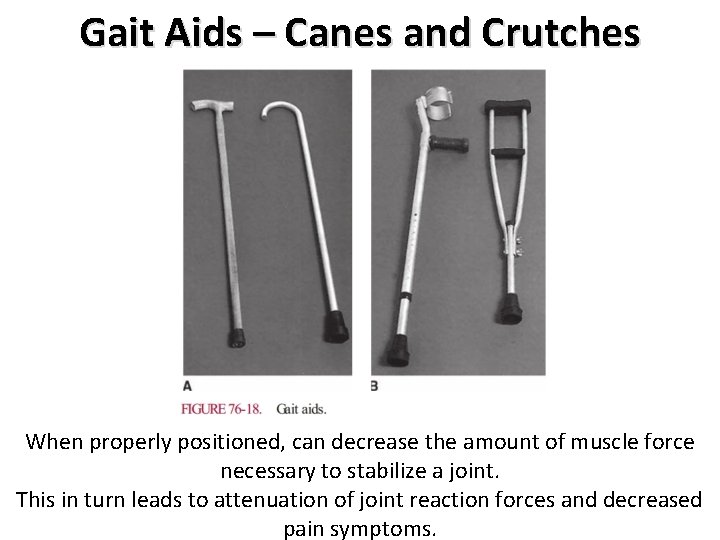
Gait Aids – Canes and Crutches When properly positioned, can decrease the amount of muscle force necessary to stabilize a joint. This in turn leads to attenuation of joint reaction forces and decreased pain symptoms.

Gait Aids -Walker

Spinal Orthosis

Control of Motion

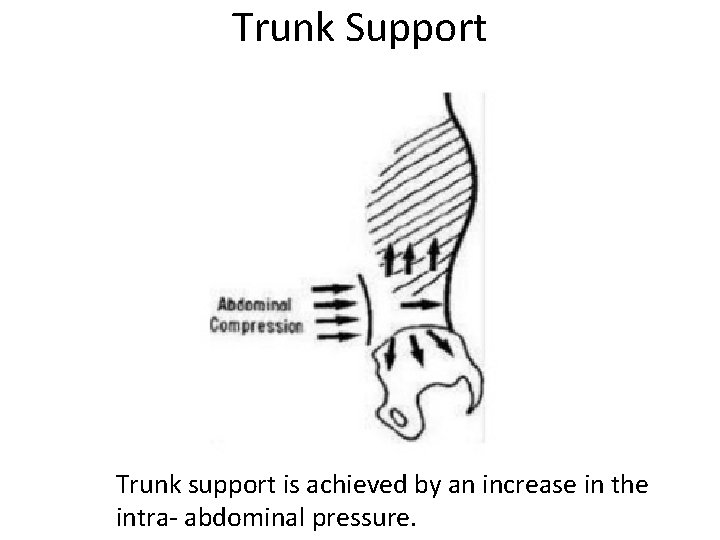
Trunk Support Trunk support is achieved by an increase in the intra- abdominal pressure.

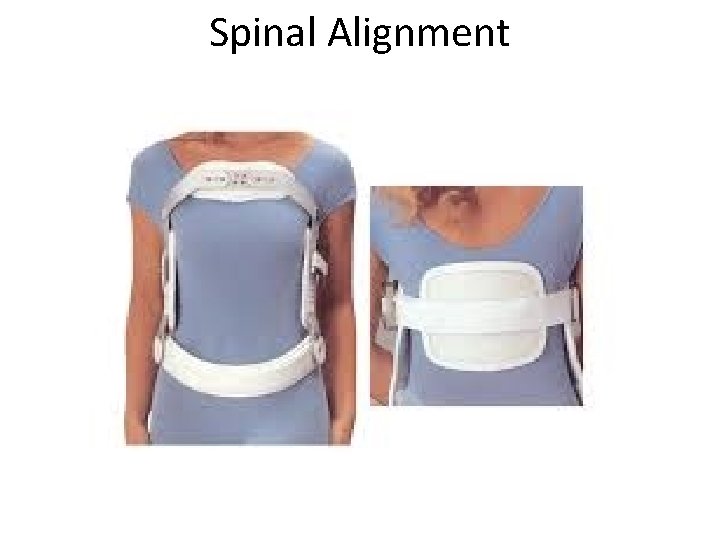
Spinal Alignment

Spinal Orthosis

Negative Effect of Orthotic Devices • • • Weaknes, atrophy and contracture Skin irritation Impaired ambulation and balance Decrease in pulmonary capacity Psyhological dependence

Clinical Uses for Spinal Orthotics

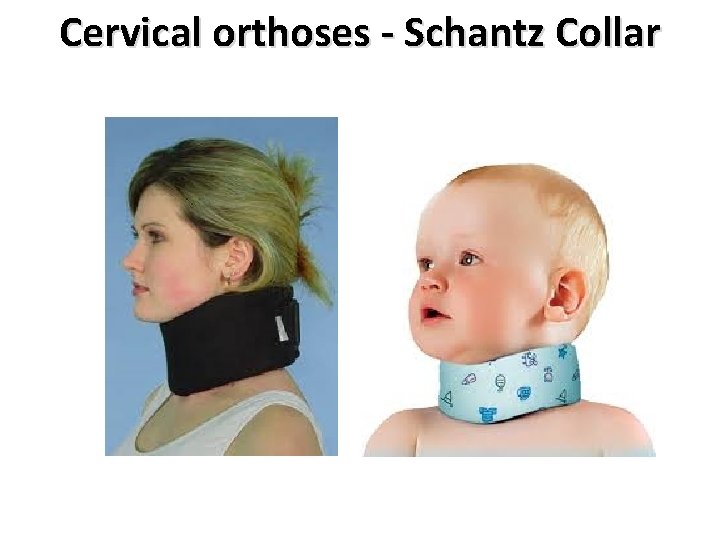
Cervical orthoses - Schantz Collar

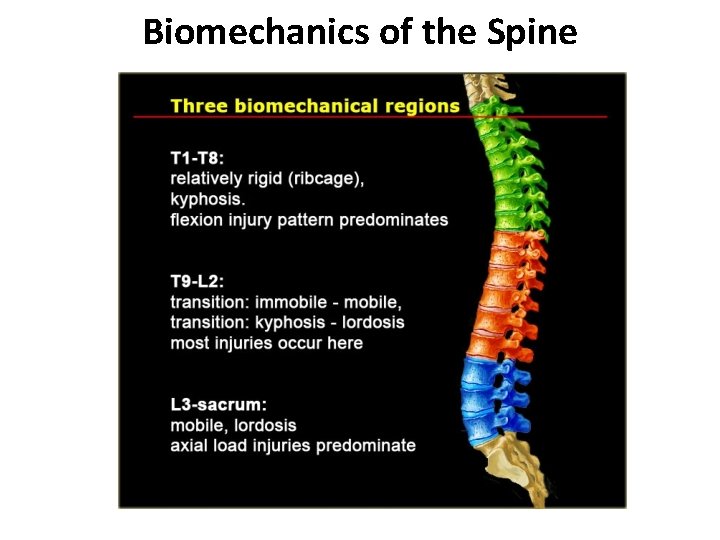
Biomechanics of the Spine

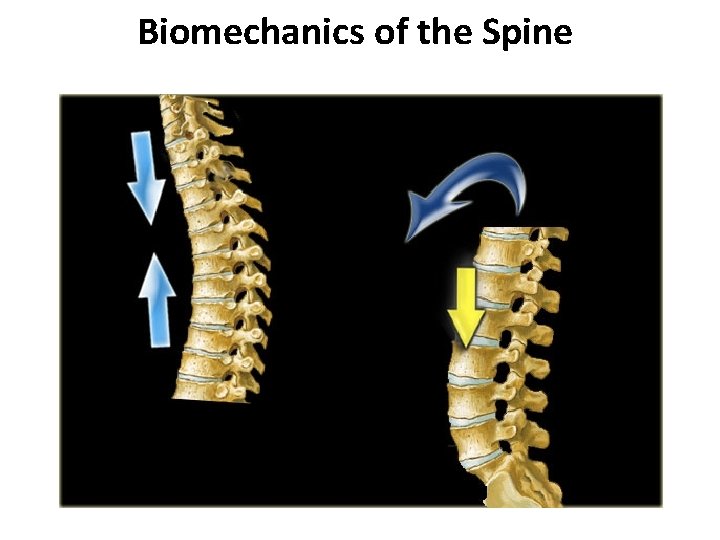
Biomechanics of the Spine

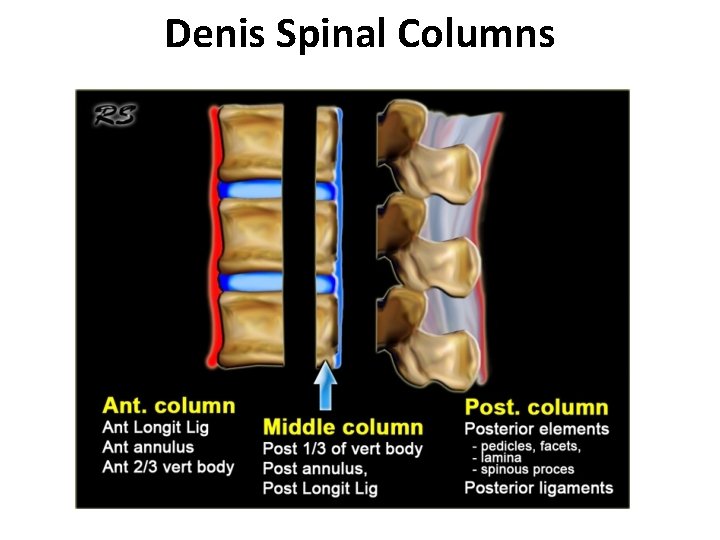
Denis Spinal Columns

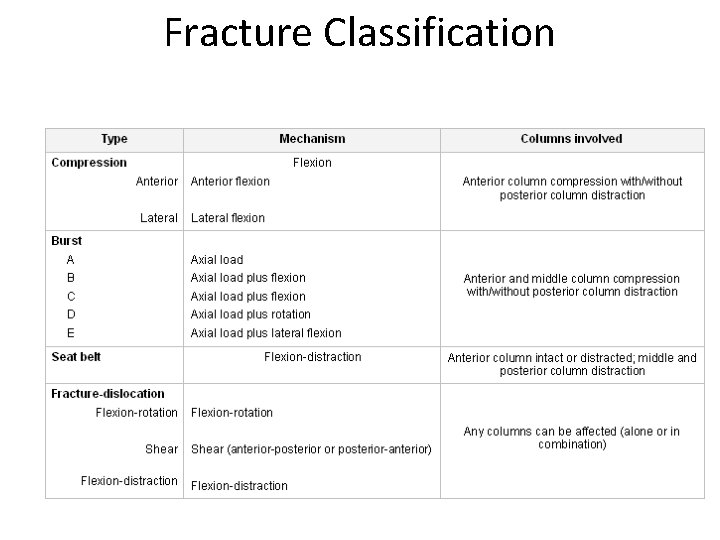
Fracture Classification

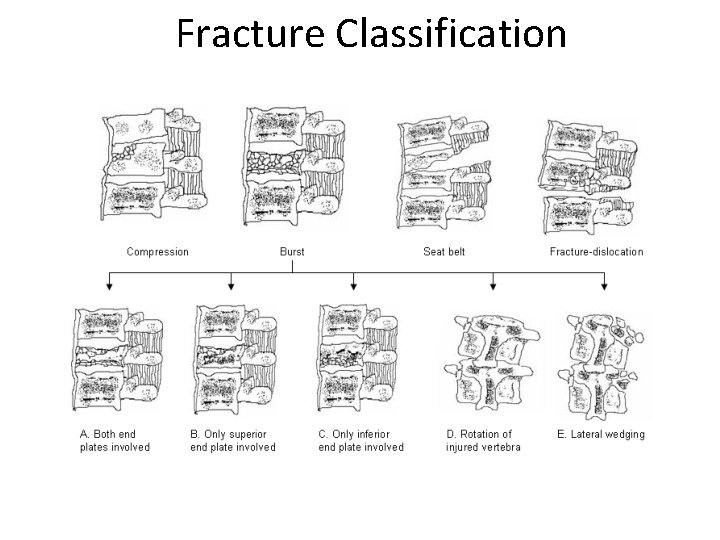
Fracture Classification

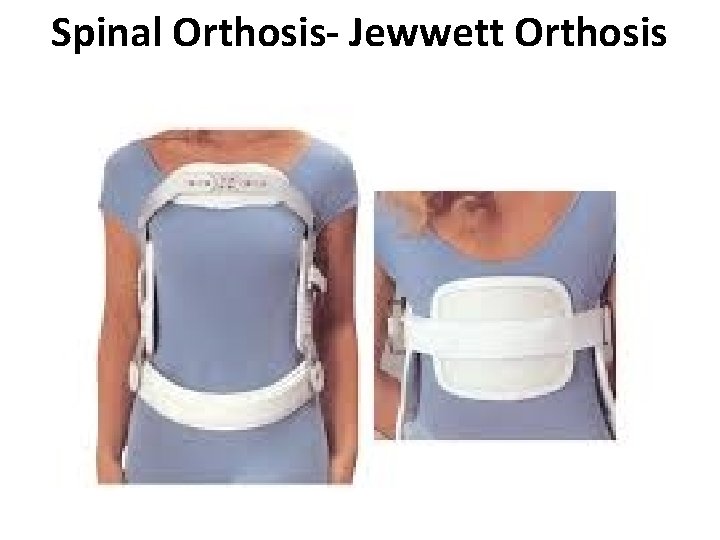
Spinal Orthosis- Jewwett Orthosis

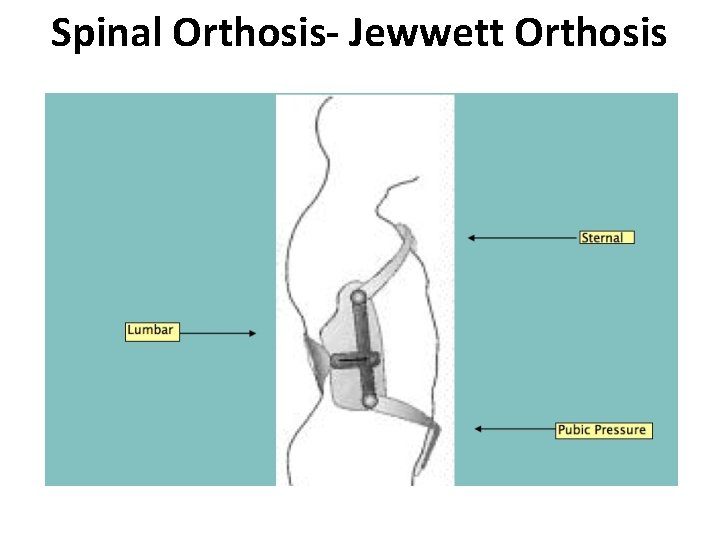
Spinal Orthosis- Jewwett Orthosis

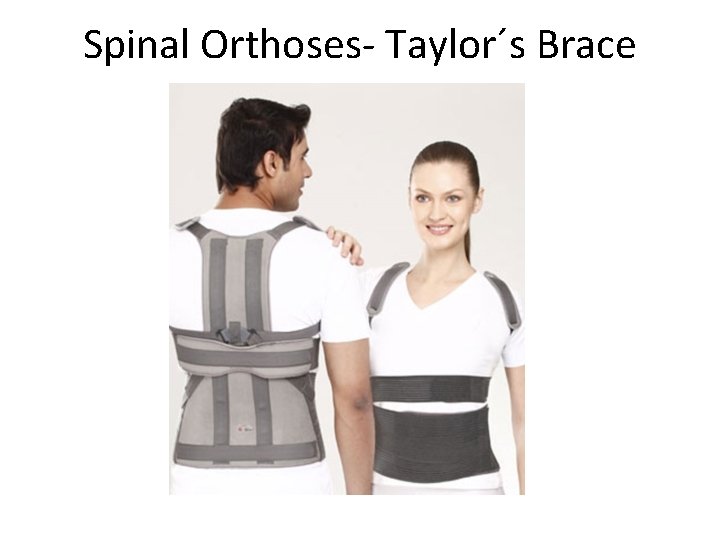
Spinal Orthoses- Taylor´s Brace

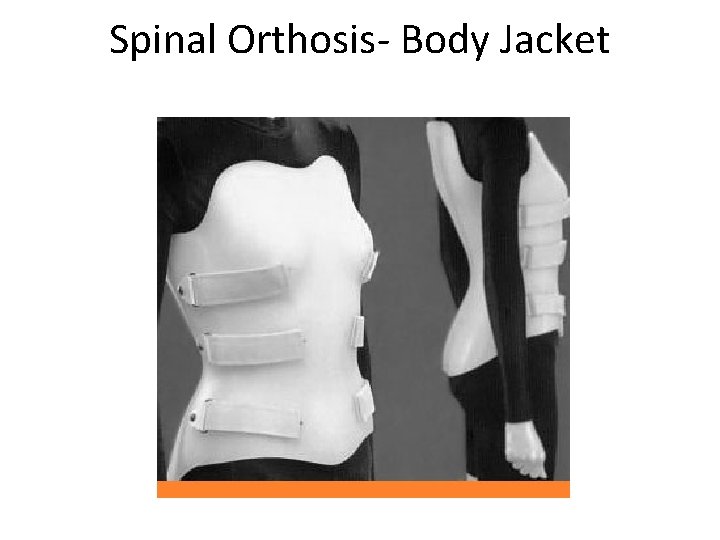
Spinal Orthosis- Body Jacket

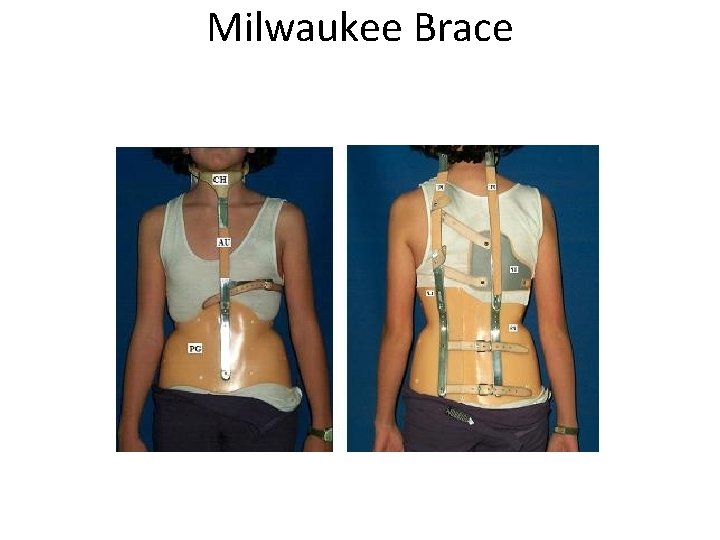
Milwaukee Brace

ana. poljicanin@mefst. hr