Orthostatic Vitals Signs Valuable or Misleading Lauren Quinn

Orthostatic Vitals Signs Valuable or Misleading? Lauren Quinn, MD PGY‐ 3
Objectives • How was (Orthostatic hypotension) OH defined? • What is the sensitivity and specificity of OVS for volume loss? • How does OH vary with age? • Should all syncope patients have OVS?


Definition of OH (Orthostatic hypotension ) + Orthostatic Vital Signs A reduction in diastolic blood pressure (DBP) of at least 10 mm Hg Need to be standing for 3 minutes Orthostatic reflex tachycardia is a HR increase by ≥ 30 beats per minute A reduction of systolic blood pressure (SBP) of at least 20 mm Hg

Medical Causes of Orthostatic Hypotension VOLUME DEPLETION GASTROINTESTINAL BLEEDING REDUCTION IN SYSTEMIC VASCULAR RESISTANCE MEDICATIONS DISORDERS OF THE AUTONOMIC NERVOUS SYSTEM (PARKINSONS)

Defined by Consensus OH defined by consensus in 1996 (The Consensus Committee of the American Autonomic Society and the American Academy of Neurology) The 2017 (ACC/AHA/HRS) Guidelines OVS in the initial workup of all patients presenting with syncope 1996 2017 2011 One important word was added to the original definition, which was “sustained, ”

Facebook Poll • 89% do not wait longer than one minute • 17 nurses replied no • 1 yes • 1 Neurology resident states 5 minutes • Taking the BP early will increase false positive rates due to normal hemodynamic changes when standing
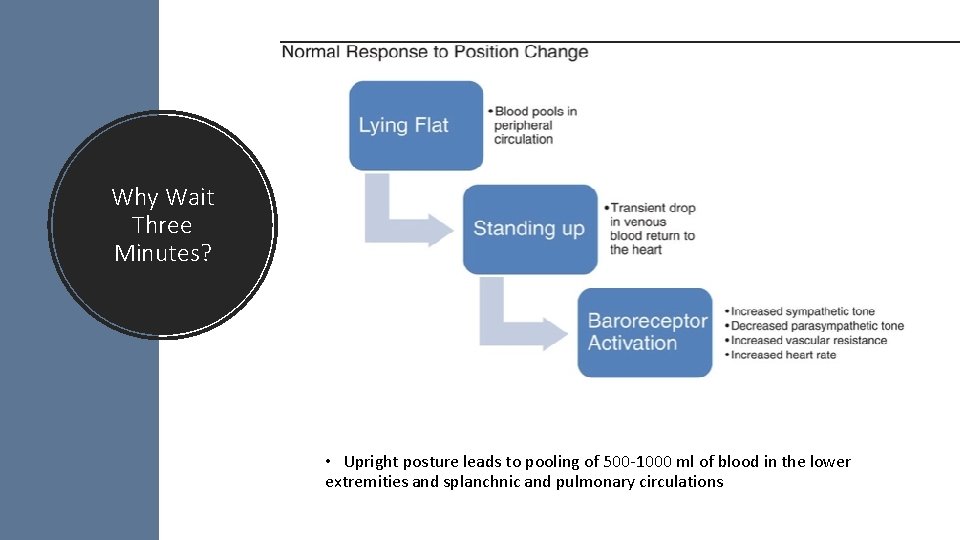
Why Wait Three Minutes? • Upright posture leads to pooling of 500‐ 1000 ml of blood in the lower extremities and splanchnic and pulmonary circulations

PURLs: Best timing for measuring orthostatic vital signs? (2019) Cohort of 11, 429 subjects followed since 1987 Ages of 45 and 64 years (mean 54 years) 5 standing BP measurements OH identified within 1 minute of standing was more clinically meaningful than OH identified after 1 minute for long-term adverse outcome for fall, fx, and MVC Risk of syncope and risk of death were statistically associated with the presence of OH at all 5 BP measurements. (Phipps D)

Atherosclerosis Risk in Communities (ARIC) study Continued 5% of the study population had OH at baseline Limitation : the population in this study was relatively healthy, with a lower prevalence of DM or CVD

Sensitivity and Specificity of OVS
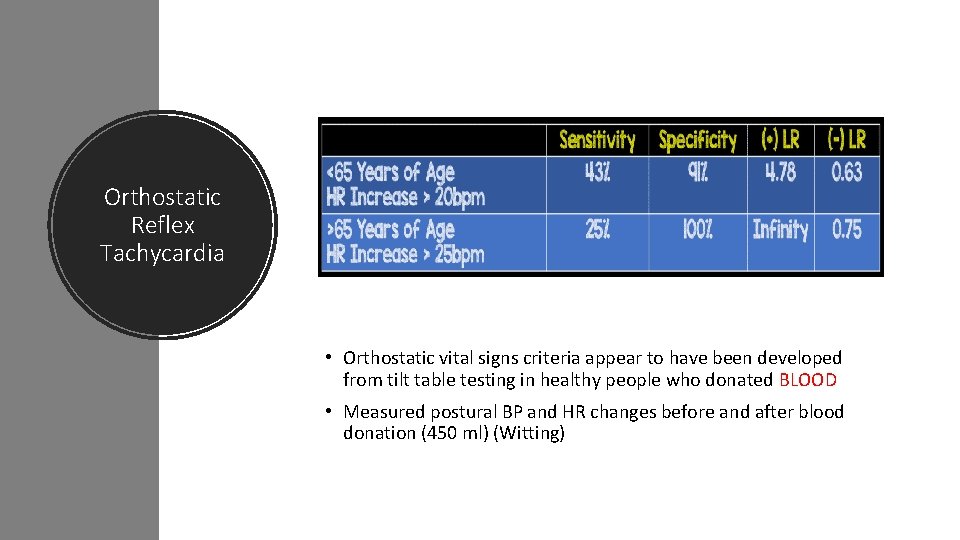
Orthostatic Reflex Tachycardia • Orthostatic vital signs criteria appear to have been developed from tilt table testing in healthy people who donated BLOOD • Measured postural BP and HR changes before and after blood donation (450 ml) (Witting)
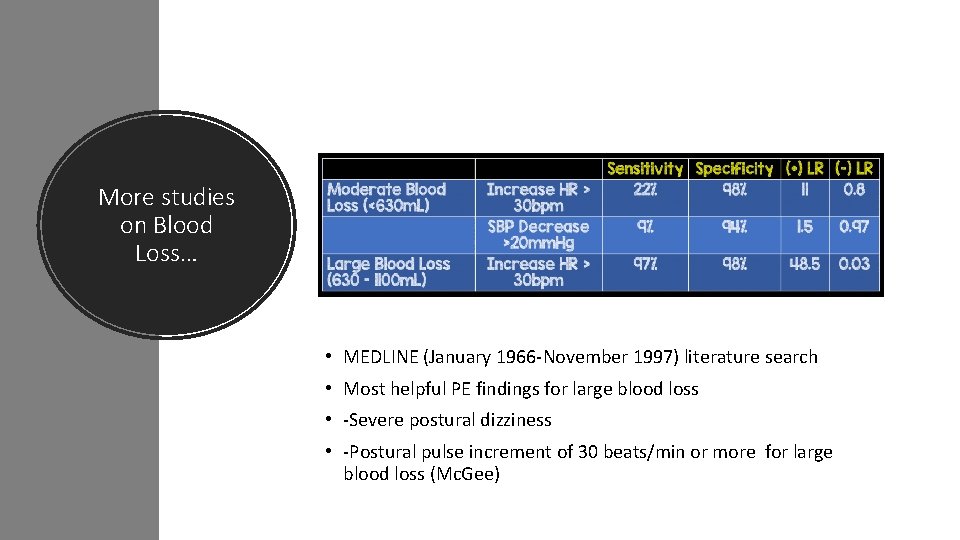
More studies on Blood Loss… • MEDLINE (January 1966‐November 1997) literature search • Most helpful PE findings for large blood loss • ‐Severe postural dizziness • ‐Postural pulse increment of 30 beats/min or more for large blood loss (Mc. Gee)

Non-Blood Volume Loss • OVS in Non-Blood Volume Loss (i. e. vomiting, diarrhea) • ( 23 women in study they were their own control and were in each position for 5 minutes) • Poor sensitivity and specificity for HR and BP • Limitations: small study • (Johnson DR )


• Abstract • STUDY OBJECTIVE: Orthostatic vital signs in emergency department patients • To examine the variability and define the normal ranges of orthostatic vital signs in an emergency department population. • DESIGN: • Descriptive. • TYPE OF PARTICIPANTS: • Adult ED patients with no history of recent blood or fluid losses. • MEASUREMENTS: • Lying and standing heart rate and blood pressure measured by an automated instrument.

Continued • RESULTS: • In 132 presumed euvolemic patients, the statistical normal ranges (mean +/‐ 2 SD) of orthostatic vital signs were wide: In this sample, 43% had "positive" orthostatic vital signs according to currently accepted values. • CONCLUSION: • The data from this study indicate that there is a wider than expected variation in orthostatic vital signs among presumed euvolemic ED patients. (Koziol‐Mc. Lain J 1) (1991)
30% in those >70 years of age Up to two‐thirds of people in long‐term care (Ricci 2015) (Frith) Prevalence of OH in Elderly

Abstract Orthostatic Hypotension in Acute Geriatric Ward Is It a Consistent Finding? (2002) Background Orthostatic hypotension (OH) is a common finding among older patients. We designed a study to examine the prevalence and consistency of OH during the day. Methods A total of 502 inpatients (241 men and 261 women) with a mean age of 81. 6 years were included in the study. Orthostatic tests were performed 3 times during the day, 30 minutes after meals.

Continued • Results Three hundred thirty-two (67. 9%) of 489 patients experienced OH at least once during the day. Of these, 170 patients (34. 8% of the 489) had OH at least twice (persistent OH) and 162 patients (33. 1%) experienced OH only once (variable OH). • Conclusions Orthostatic hypotension is very common in the elderly, and diastolic OH is more common than systolic OH. (Weiss)
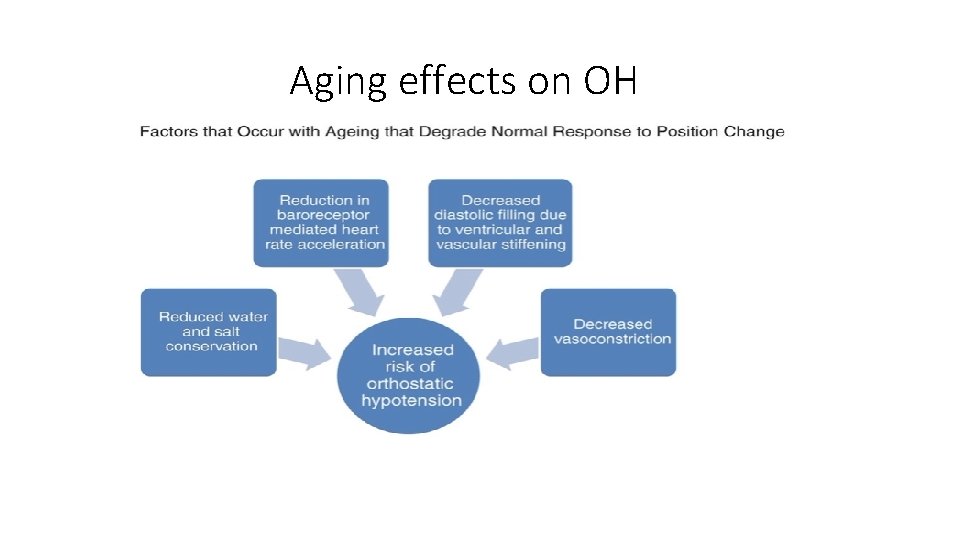
Aging effects on OH
307 healthy high school students aged 15‐ 17 yo were checked for orthostatic vitals. A third of participants experienced orthostatic symptoms OH in Adolescents Pulse changes within the population to be 61% sensitive and 56% specific for predicting postural orthostatic symptoms 23% heart changes >30 bpm Conclusion: Using adult heart change criteria in adolescents should be reevaluated (Skinner 2010)

• Abstract • Background Do Orthostatic Vital Signs Have Utility in the Evaluation of Syncope? (Schaffer 2018) • Syncope is a common presentation in the emergency department (ED). The differential diagnosis is long and includes benign conditions as well as acute life threats, such as dysrhythmias or pulmonary embolism. • Objective • 1) to define the diagnostic utility of orthostatic vital signs (OVS) as a test for orthostatic syncope, and 2) to determine whether OVS help diagnose or exclude life‐threatening causes of syncope in ED patients. • Methods • Three prospective cohort studies plus 2017 national guidelines for syncope management were identified, reviewed, and critically appraised.

• Results • This literature review found that orthostatic hypotension is common among ED patients with syncope and is often diagnosed as the cause of syncope. Continued • Conclusions • OVS measurements do not, in isolation, reliably diagnose or exclude orthostatic syncope, nor do they appear to have value in ruling out life‐threatening causes of syncope. • “Importantly, a substantial subset of patients with other causes of syncope, including cardiac causes, will have abnormal OVS. ”

“Syncope and Orthostatic Hypotension” by Atkins et al. 1991 • Patients aged 16 years + who presented with syncope were prospectively recruited from the ED, ward and outpatient clinics of an urban American hospital during a 2 -year period. • 307 were evaluated for syncope during the study period and after various exclusions, 223 were included.

Continued • Results: OVS did not accurately predict OH as the cause of syncope. OH was found in 71% of those ultimately diagnosed with orthostatic syncope and 25% of those with syncope from other etiologies, including 29% of those with cardiac syncope. (Atkins)

OVS can lead you away from the correct diagnosis Conclusion OH increases significantly with age OVS have low sensitivity and specificity

Two Dangers • Negative for OH, the patient may still have volume loss, blood loss, or orthostatic syncope. Worse, the clinician may feel false assurance that these conditions have been ruled out • Positive OH, conclusion bias not pursue other potentially lethal causes, and miss a critical diagnosis (Smith 2019)

Thank you

References • The Consensus Committee of the American Autonomic Society and the American Academy of Neurology • Neurology May 1996, 46 (5) 1470; DOI: 10. 1212/WNL. 46. 5. 1470 • Witting MD et al. Defining the positive tilt test: a study of healthy adults with moderate acute blood loss. Ann Emerg Med 1994; 23(6): 1320‐ 3. PMID: 8198307 • Mc. Gee S et al. The rational clinical examination. Is this patient hypovolemic. JAMA 1999; 281(11): 1022‐ 9. PMID: 10086438 • Johnson DR et al. Dehydration and orthostatic vital signs in women with hyperemesis gravidarum. Acad Emerg Med 1995; 2(8): 692‐ 7. PMID: 7584747 • Koziol‐Mc. Lain J 1 Emergency Medicine Research Center, University of Colorado Health Sciences Center, Denver 80262. PMID: 2039097 DOI: 10. 1016/s 0196‐ 0644(05)82376‐ 5 • Skinner JE, Driscoll SW, Porter CB, et al. Orthostatic heart rate and blood pressure in adolescents: reference ranges. Journal of child neurology. Oct 2010; 25(10): 1210‐ 1215. • Weiss A, Grossman E, Beloosesky Y, Grinblat J. Orthostatic Hypotension in Acute Geriatric Ward: Is It a Consistent Finding? Arch Intern Med. 2002; 162(20): 2369– 2374. doi: 10. 1001/archinte. 162. 20. 2369 • Atkins D. , Hanusa B. , Sefcik T. , and Kapoor W. : Syncope and orthostatic hypotension. Am J Med 1991; 91: pp. 179‐ 185 • Phipps D, Butler E, Mounsey A, et al. PURL: Best timing for measuring orthostatic vital signs? . J Fam Pract. 2019; 68(9): 512‐ 514. • James Frith, Diagnosing orthostatic hypotension: a narrative review of the evidence, British Medical Bulletin, Volume 115, Issue 1, September 2015 • https: //journalfeed. org/article‐a‐day/2019/orthostatics‐helpful‐or‐useless • Do Orthostatic Vital Signs Have Utility in the Evaluation of Syncope? DOI: https: //doi. org/10. 1016/j. jemermed. 2018. 09. 011
- Slides: 30