OROFACIAL PAIN Clin AProf Robert Delcanho BDSc MS

OROFACIAL PAIN Clin A/Prof Robert Delcanho BDSc MS Cert OFP FFPMANZCA FICD FAAOP Diplomate, American Board of Orofacial Pain St John of God Hospital, Subiaco Clinic 25 Mc. Court Street Subiaco WA

OROFACIAL PAIN The field of Dentistry that includes the Assessment, Diagnosis and Treatment of ÿ Complex chronic orofacial pain and dysfunction ÿ Oromotor and jaw behaviour disorders ÿ Chronic facial, head and neck pain

OROFACIAL PAIN 1. Dental (Odontogenic) Pain 2. Musculoskeletal Pain – Temporomandibular disorders 3. Neurovascular Pain – Primary headaches 4. Neuropathic Pain • Episodic • Continuous 5. Sinus Pain 6. Psychogenic Pain 7. Intracranial 8. Cervicogenic
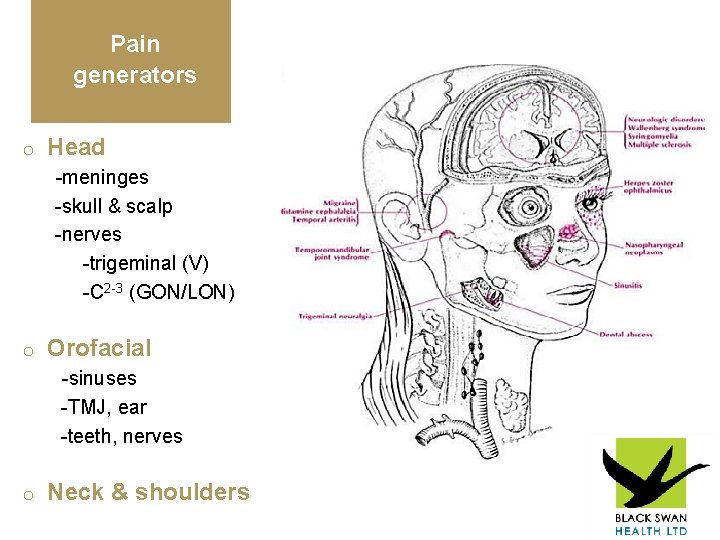
Pain generators o Head -meninges -skull & scalp -nerves -trigeminal (V) -C 2 -3 (GON/LON) o Orofacial -sinuses -TMJ, ear -teeth, nerves o Neck & shoulders
Red flags T. I. N. T Tumour o Temporal arteritis o Intracranial pressure o Infection o Neurovascular o Trigeminal o Trauma o

Red Flag Case Presentation n n n Female 16 years Hx of constant deep aching TMJ/jaw pain worse with chewing, extending to occiput. Initially treated with Occlusal Splint/Physio. Headaches on exertion - paroxysmal with “fainting”. Parents noted subtle personality changes. MRI - Arnold Chiari formation- surgery.

Intracranial Pathology Diagnostic Clues n n Neurological type symptoms/signs. No response to peripheral therapies. Unusual or worsening symptoms despite therapy. Negative response to somatic/sympathetic blocks.
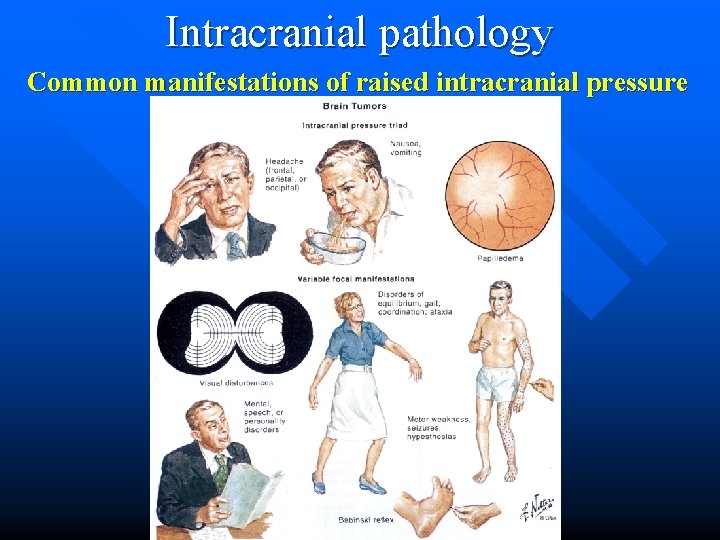
Intracranial pathology Common manifestations of raised intracranial pressure

Space Occupying Lesions n n n n Neoplasms Arterial dissection Aneurysms Infection/Abscess Infarction/haemorrhage Oedema Angioma
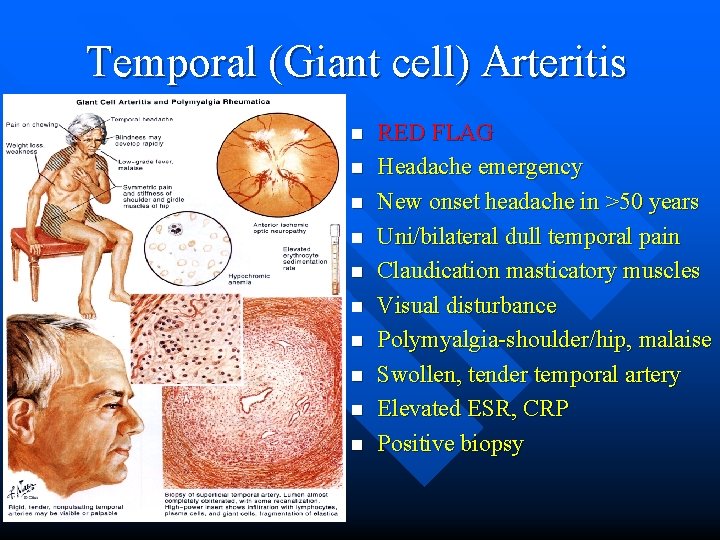
Temporal (Giant cell) Arteritis n n n n n RED FLAG Headache emergency New onset headache in >50 years Uni/bilateral dull temporal pain Claudication masticatory muscles Visual disturbance Polymyalgia-shoulder/hip, malaise Swollen, tender temporal artery Elevated ESR, CRP Positive biopsy

Temporal Arteritis n n RED FLAG Headache of vascular origin Initial symptoms may resemble TMD - Pain/stiffness in jaw - Pain/fatigue of jaw when chewing - Pain may radiate to ear, teeth - Temporal headache If untreated may cause blindness, stroke and death! Generally resolves with high dose steroids
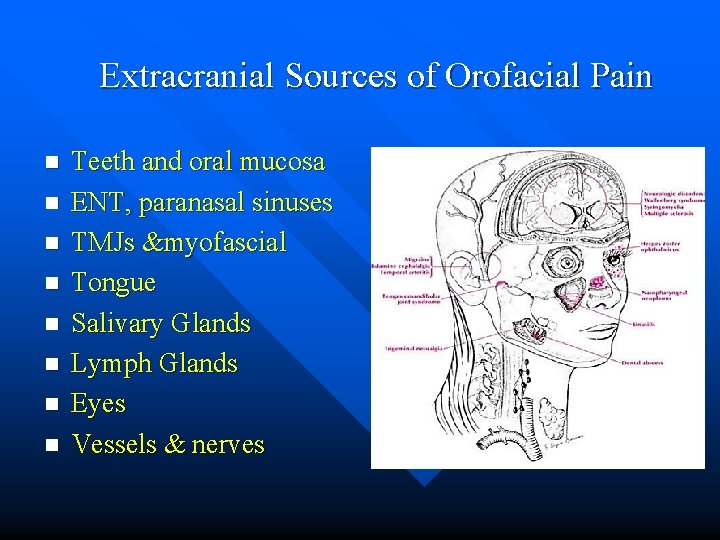
Extracranial Sources of Orofacial Pain n n n n Teeth and oral mucosa ENT, paranasal sinuses TMJs &myofascial Tongue Salivary Glands Lymph Glands Eyes Vessels & nerves

Odontogenic Pain – Toothache § § § § Most common cause of orofacial pain! Often missed by medical people Dental caries into dentine / pulp Pulpitis, pulp necrosis Cracked teeth Periodontal infection ASK ABOUT HOLES IN TEETH Hot/cold/bite SENSITIVITY, PAIN AT NIGHT

TOOTHACHE • Toothache - most common orofacial pain complaint • 12. 2% of population reported toothache in last 6 M • Diagnosis can be challenging and complicated • Pain from one tooth may be referred from another tooth or from other orofacial structures • Other craniofacial pain disorders may mimic the symptoms of toothache • Proper diagnosis is critical
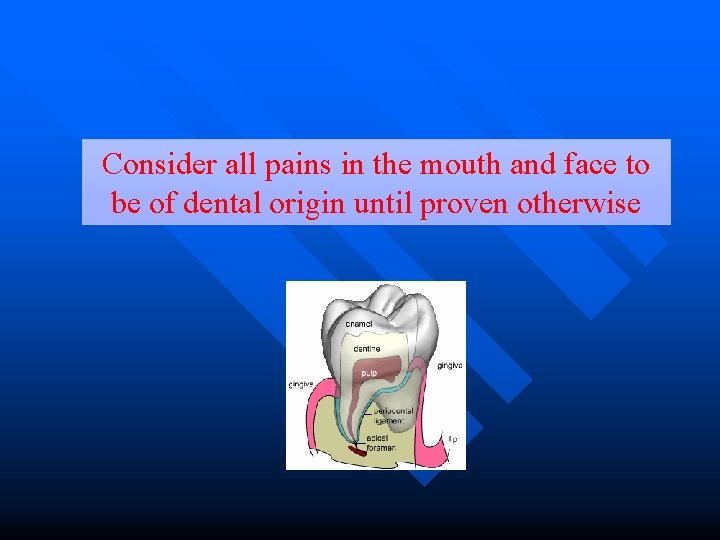
Consider all pains in the mouth and face to be of dental origin until proven otherwise

TEMPOROMANDIBULAR DISORDERS Major cause of Non Dental Pain in Orofacial Region�

TEMPOROMANDIBULAR DISORDERS Collection of medical and dental conditions affecting the temporomandibular joint and/or muscles of mastication and/or contiguous tissues resulting in pain and/or dysfunction

TEMPOROMANDIBULAR DISORDERS Primary Clinical Features n n n Ear ache (pre-auricular pain) Painful jaw use e. g. with chewing, yawning Tender TMJs and muscles of mastication Restriction of jaw movement Interference with jaw movement TMJ sounds e. g. clicking, cracking, popping sounds

TEMPOROMANDIBULAR DISORDER Other Clinical Features Headache n Ear symptoms eg discomfort, fullness n Occlusal discomfort or change n Mandibular dyskinesia n Intermittent facial swelling n

TEMPOROMANDIBULAR DISORDERS The pain/dysfunction should be directly related and aggravated by jaw use (Solberg)

Temporomandibular Disorders TMJ ARTHRALGIAS 1. Traumatic arthralgia 2. Arthromyalgia 3. Internal Derangement - painful TMJ dysfunction 4. Osteoarthritis 5. Systemic (poly)arthritis . OROFACIAL MYALGIAS - Muscle splinting/strain - Muscle spasm - Myofascial Pain +/- TPs - Myositis - Fibromyalgia
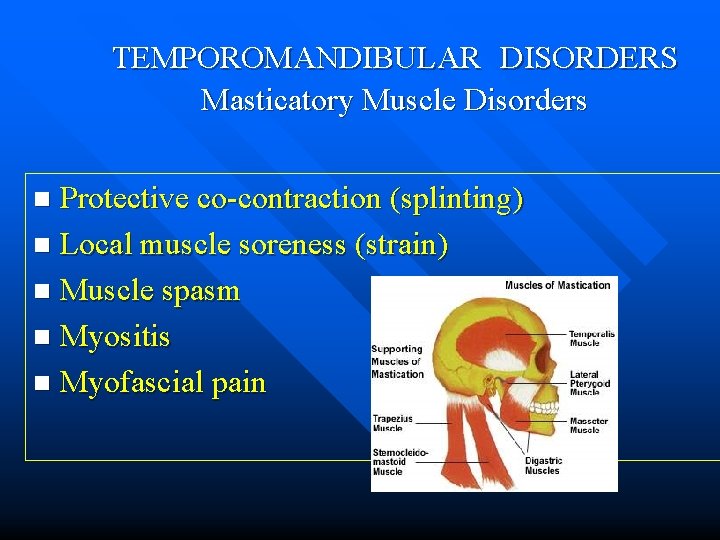
TEMPOROMANDIBULAR DISORDERS Masticatory Muscle Disorders Protective co-contraction (splinting) n Local muscle soreness (strain) n Muscle spasm n Myositis n Myofascial pain n
NEUROVASCULAR PAIN

Case Presentation n n n 48 year old female Intermittent dull throbbing pain in upper tooth/jaw, radiating to temple and eye. Severe attacks, last 1 -3 days with constant dull pain. When severe, feels sick and prefers dark, quiet room to sleep. Attacks used to respond well to NSAIDs. Had a root canal, crown of upper premolar + splint

Migraine

Case Presentation n n n Male in mid forties. Right sided face pain attacks on/off over three years Extending into right eye. Often awakened from sleep with severe throbbing pain. Would get up and pace around holding his R. eye. Face would feel sweaty, tearing of eye. Numerous dental visits – Root canals/ extractions.

Case Presentation n EXAMINATION Cranial nerve screen - Normal TMJ/Myofascial – Normal Oro-dental- Normal n Medication Trial - response to oxygen/sumatriptan

TRIGEMINAL AUTONOMIC CEPHALGIAS (TACs) CLUSTER HEADACHE n CHRONIC PAROXYSMAL HEMICRANIA n HEMICRANIA CONTINUA n Unilateral, severe attacks with typical autonomic headache accompanying symptoms. Peri-orbital or maxillary pain. Frequently leads to dental work including extractions.

Cluster Headache Clinical Features • Attacks are severe - boring • Strictly unilateraln in and around eye and/or temporal region - “hot poker” • Attack duration 15 -180 min • Attacks occur from once every 2 nd day up to 8 x day. • Attacks occur in series lasting weeks to months Remissions mths-yrs • Autonomic features +++ • Males 5 -7: 1 65% had dental Tx

Chronic Paroxysmal Hemicrania Similar to Cluster but n n n Female preponderance (3: 1) Attacks are more frequent and of shorter duration 5 -40 attacks per day (median 5 -10) Attacks last 2 -45 minutes At least one autonomic symptom on the side of pain conjunctival injection lacrimation nasal congestion rhinorrhoea, ptosis eyelid oedema

Chronic Paroxysmal Hemicrania n n Always unilateral orbital, and/or temporal. Severe stabbing/boring type pain that throbs as it builds up. Episodic form occursin bouts lasting months to years with clear intervals (rare). In most cases responds rapidly and absolutely to Indomethacin (diagnostic test).

Tension Type Headache (TTH) n n n n Previously called tension headache, muscle contraction headache, stress headache Most common primary headache (30 -70% prevalence) Episodic (frequent/infrequent) and chronic forms Usually frontal /temporal location Tightness, pressure in hat-band like distribution +/- pericranial muscle tenderness Often co morbid with migraine w/o aura.
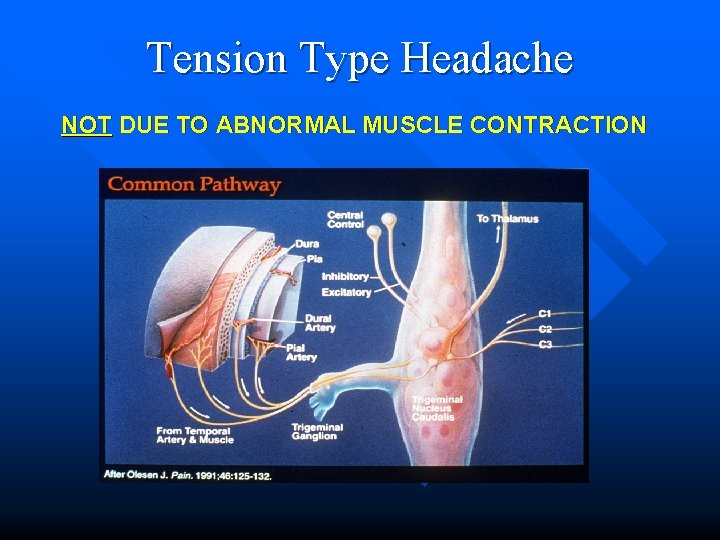
Tension Type Headache NOT DUE TO ABNORMAL MUSCLE CONTRACTION

Neuropathic Orofacial Pains EPISODIC n Trigeminal Neuralgia n Glossopharyngeal Neuralgia n n n CONTINUOUS Painful Traumatic Trigeminal Neuropathy Post Herpetic Neuralgia Persistent Idiopathic Facial Pain (PIFP) Persistent Dento-alveolar Pain (PADP) Burning Mouth Syndrome

Case Presentation § § § 65 year old female Sharp shooting pains upper anterior teeth 22/23 Saw dentist - fillings, root canals, extraction, bridge, removal of bridge Inserting denture triggers sharp pain Repeated denture adjustments
Case Presentation EXAMINATION n Cervical spine - normal n Cranial nerve screen - normal n TMJ/MM - normal n Myofascial - tender masseter. n Intraoral - mucosa normal appearance trigger area palatal to 23 site.
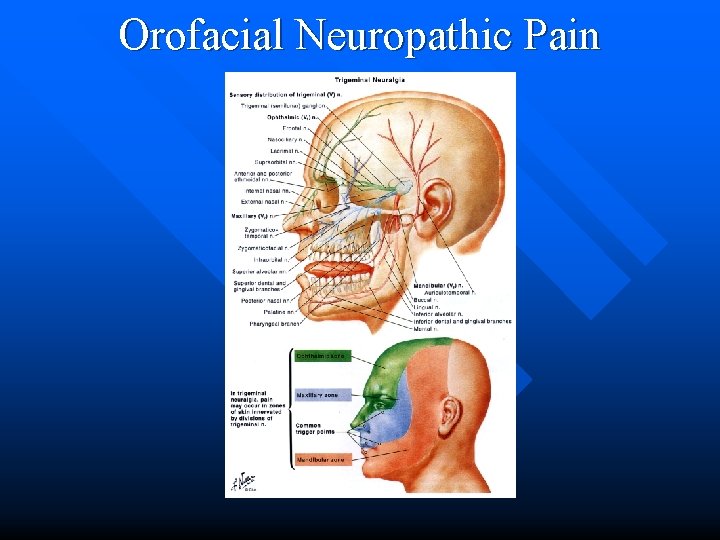
Orofacial Neuropathic Pain
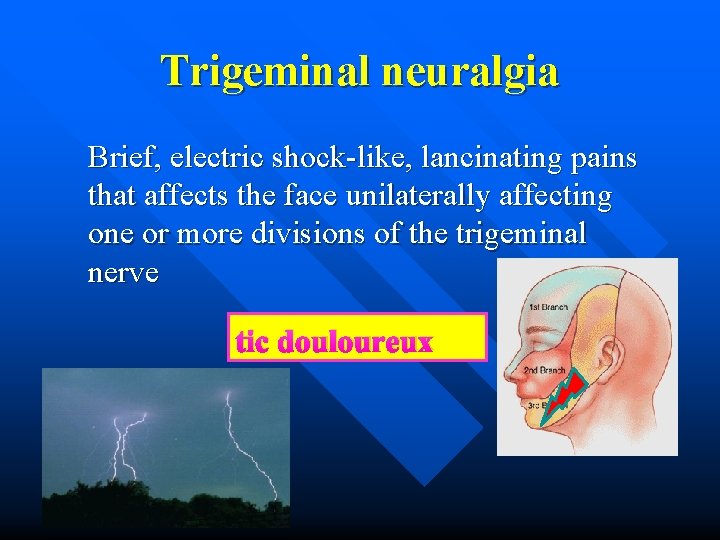
Trigeminal neuralgia Brief, electric shock-like, lancinating pains that affects the face unilaterally affecting one or more divisions of the trigeminal nerve tic douloureux

Trigeminal Neuralgia n n n n Intermittent brief paroxysmal pain (secs-mins) Limited distribution: V 2 and/or V 3 > V 1 Trigger zone –minor stimuli- touch, wind, shave Abrupt in onset and termination and may remit Remission period can spontaneously occur that lasts for weeks to years, and may return Triggerable or spontaneous No obvious local cause

Painful Post Traumatic Trigeminal Neuropathy (AFP, PIFP) n n n n Unilateral facial and/or oral pain Usually continuous +/- sharp jolts of pain History of trauma to same V nerve branch Positive and/or negative neurosensory signs (allodynia, hyperalgesia, hypoesthesia etc) Equivocal response to LA nerve block Varying degree of central & sympathetic involvement

Case presentation n n 40 yo female Complains of 3 years continuous dull aching pain in lower left quadrant. Occasional sharp pains. Problem commenced after periodontal surgery and surgical extraction of third molar. Since had RCT of 1 st and 2 nd molars w/o effect Aggravated by eating on that side and brushing teeth.

Persistent Dento-Alveolar Pain Disorder (PDAP) (Atypical Odontalgia, Phantom tooth pain) n n n n Continuous variable pain Localized to dento-alveolar region – tooth/extrn sites Usually multiple (unsuccessful) dental procedures No obvious local pathology-clinical/radiography Not caused by another disease or disorder +/- Sensory abnormalities Somatic block equivocal

Case Presentation n n n 48 year old female 2 years continuous dull, aching, burning pain in upper right jaw Presumed pulpitis so over time 3 x root canals Extractions all upper molars, now wants premolar out Extractions only aggravated pain, which has spread Some sinus and menopausal symptoms Hx of depression - not current

Case Presentation n n n n Cervical Spine - normal Cranial Nerve Screen - normal Stomatognathic- normal Myofascial – trigger points but not replicating pain Intraoral- Extraction sites hyperaesthetic Somatic block – negative Sympathetic block- partially positive Cone Beam CT, MRI- normal

Persistent Dento-Alveolar Pain Disorder (PDAP) (Atypical Odontalgia, Phantom Tooth pain) n n n n Females > males – usually mid 40 s on Posterior maxillary quadrant most often Hx of trauma - multiple dental procedures Somatosensory abnormalities around tooth site No evidence of psychopathology <50% responded to LA block Variable response to TCA, gabapentinoids, topicals etc Repeated dental procedures are contraindicated

EETS Excessive Endodontic Treatment Syndrome

THANK YOU !!!! dr@orofacialpain. com. au
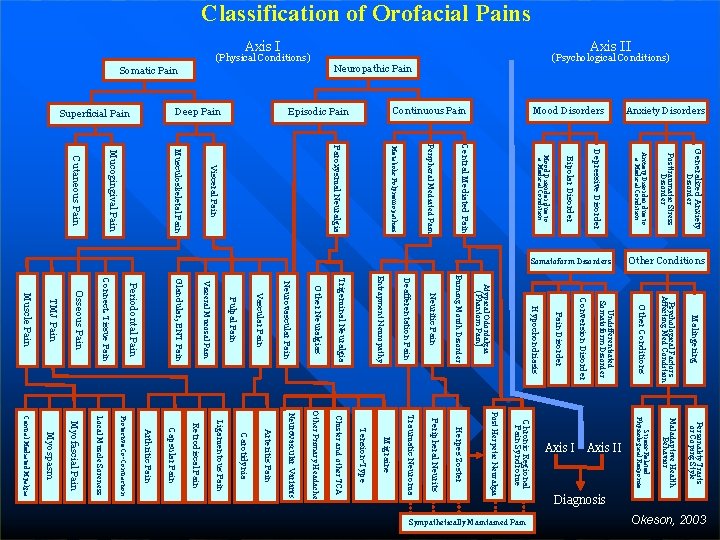
Classification of Orofacial Pains Neuropathic Pain Somatic Pain Disorder Generalized Anxiety Posttraumatic Stress Disorder Anxiety Disorder due to a Medical Condition Depressive Disorder Bipolar Disorder Mood Disorder due to a Medical Condition Central Mediated Pain Peripheral Mediated Pain Metabolic Polyneuropathies Paroxysmal Neuralgia Visceral Pain Musculoskeletal Pain Mucogingival Pain Cutaneous Pain Other Conditions Psychological Factors Affecting Med Condition Malingering Stress-Related Physiological Response Maladaptive Health Behavior Personality Traits or Coping Style Undifferentiated Somatoform Disorder Conversion Disorder Pain Disorder Hypochondriasis Chronic Regional Pain Syndrome Herpes Zoster Post Herpetic Neuralgia Burning Mouth Disorder Peripheral Neurits Atypical Odontalgia (Phantom Pain) Diagnosis Central Mediated Myalgia Myospasm Myofascial Pain Local Muscle Soreness Protective Co-Contraction Arthritic Pain Capsular Pain Retrodiscal Pain Ligamentous Pain Carotidynia Arteritis Pain Neurovascular Variants Other Primary Headache Cluster and other TCA Tension-Type Migraine Traumatic Neuroma Neuritic Pain Deafferentation Pain Entrapment Neuropathy Trigeminal Neuralgia Other Neuralgias Neurovascular Pain Vascular Pain Pulpal Pain Visceral Mucosal Pain Glandular, ENT Pain Periodontal Pain Connect. Tissue Pain Osseous Pain TMJ Pain Muscle Pain Okeson, 2003 Sympathetically Maintained Pain Axis II Other Conditions Somatoform Disorders Anxiety Disorders Mood Disorders Continuous Pain Episodic Pain Deep Pain Superficial Pain (Psychological Conditions) Axis II Axis I (Physical Conditions)
- Slides: 48