ORISSA NRHM Second Common Review Mission ORISSA NovemberDecember

ORISSA

NRHM Second Common Review Mission ORISSA November-December 2008

OVERVIEW of 2 nd CRM FINDINGS NRHM has brought a significant improvement in the state and district health system • JSY and ASHA are the most visible faces of change • The State & District Project management teams are active and dynamic • Untied/ RKS funds are being used effectively for facility improvement and public credibility • Effective Decentralization, Community participation & other management & governance paradigm shifts

Overview contd… Appreciable steps have been taken to improve: • The Human Resources situation • Drug availability • Strengthen Community Processes • Financing system and Fund flows • HMIS & GIS; IDSP Gaps remain & need to be addressed if efforts are to be sustained and outcomes maximised

Facility Strengthening & Service Delivery Achievements • Service Utilisation increased at Secondary level-SDH/DH /CHCs • Improved drug availability • Improvements in infrastructure, cleanliness, waste disposal, electrification, water supply, but inadequate • AYUSH Doctors contributing effectively to OPD services in PHC (N) & MMUs • Janani Express facilitating access; NGO partnership Areas for Improvement • Overcrowding in CHC/DH • PHC and SC services by-passed; to be strengthened. • Quality of ANC, PNC and deliveries by ANMs needs priority attention • 25% of malaria deaths. Antimalaria activities strengthening • Toilets, Casualty services, New born care, OT, Waste Management. • Inadequate budget for Drugs still puts “out of pocket” burden on patients • Non-resident Drs. /SNs

Human Resources Areas for Improvement Achievements • Vacancy gap decreased: M. O. s/ AYUSH doctors recruited; Increase in No. of ANMs, 2 nd ANMs in some SCs • Pro-active Efforts to attract doctors & specialists • Special allowance for underserved areas • Multi-skilling of MOs for Anaesthesia, Em. OC • Shortage of Specialists (Anesthesia, Ob&Gyn), Staff Nurses, MBBS doctors, LT and MPW (M) • Long term Strategy should include: Ø Ø Ø • • • Increased reservation for in-service candidates for PG Reservation of seats for Nursing and ANMs for KBK plus districts Nursing colleges and ANM training centers in KBK plus districts Enhance Training for SBA & IMNCI Sensitisation of all Healthcare providers for cross-referral with AYUSH Creating and nurturing a public health cadre

Community Participation Achievements • Community Processes Resource Centre set up at state level recently, incorporating the ASHA resource centre • ASHA programme running well; Good team work with ANM, AWW & SHG • VHND good forums for increasing community ownership • Gram Kalyan Samitis (VHSC) have been formed recently & active • District and block level health committees, RKS are meeting regularly • Community monitoring taken up in 4 Districts as a pilot Areas for Improvement • Active involvement of SC/ST/BPL members to be encouraged; Vulnerable social groups have been included in the GKS but participation limited • State specific strategies for vulnerable groups should be enhanced in State PIP

Management & Governance Achievements Areas for Improvement • State PMU has strong leadership and good working ethos • District PMU are active, professional and vibrant • Good team work and integration with district and block medical team exists • State and district Health societies functional • Good cooperation between General and Health administrators, PRI, NGOs and SHGs at all levels • E-Governance: Computerize recruitment, transfers, promotions, eprocurement, for transparency and accountability • Effective Monitoring of residence of health personnel at the HQ (Private practice, absenteeism, …) • Strengthening Drug Control department - Immediate withdrawal of sub-std. drugs, black listing and debarring of companies/suppliers • Strengthening Hospital & Health Committees – Citizen’s Charter, Report card system, Public grievance redressal mechanisms Adopting Good Governance Practices

Summary: The thrust on Public System Strengthening is well on its way & must be sustained Primary Level Services to receive greater attention; Improvements in secondary level to be taken further Malaria: Initiate Integrated Vector Control; Fill posts of District Programme Officers, LTs & MPW(M); Strengthen laboratory services. Good HMIS/GIS to be now used for planning and monitoring at district & state levels. Strong management capacities have been built up. Good Governance practices to be adopted.

RAJASTHAN

2 nd Common Review Mission (CRM) under NRHM in Rajasthan (December 16 -22, 2008) Districts: Jaipur and Dungarpur Team: 1. Dr. Gian Chand (Retd. DHS, Govt. of HP) 2. Gautam Chakraborty (NHSRC) 3. Dr. Rajib Dasgupta (JNU) 4. Sanjay Saxena (NIPI-UNOPS) 5. Dr. Ute Schumann (EC)
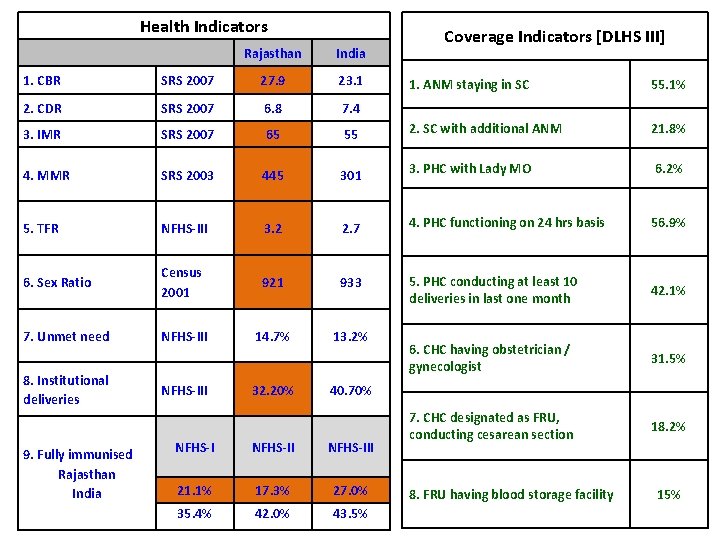
Health Indicators Rajasthan India 1. CBR SRS 2007 27. 9 23. 1 2. CDR SRS 2007 6. 8 7. 4 3. IMR SRS 2007 65 4. MMR SRS 2003 5. TFR Coverage Indicators [DLHS III] 1. ANM staying in SC 55. 1% 55 2. SC with additional ANM 21. 8% 445 301 3. PHC with Lady MO 6. 2% NFHS-III 3. 2 2. 7 4. PHC functioning on 24 hrs basis 56. 9% 6. Sex Ratio Census 2001 921 933 5. PHC conducting at least 10 deliveries in last one month 42. 1% 7. Unmet need NFHS-III 14. 7% 13. 2% 6. CHC having obstetrician / gynecologist 31. 5% 7. CHC designated as FRU, conducting cesarean section 18. 2% 8. Institutional deliveries 9. Fully immunised Rajasthan India NFHS-III 32. 20% 40. 70% NFHS-III 21. 1% 17. 3% 27. 0% 35. 4% 42. 0% 43. 5% 8. FRU having blood storage facility 15%

Major Findings • Increase in institutional deliveries (70% of ANC registered) • 10% of SCs conducting institutional deliveries in Dungarpur • Mothers reportedly staying in CHCs and PHCs for 24 -48 hours after delivery • Critical functions missing in FRUs / CHCs C-sections, blood transfusion, management of complicated APH/PPH cases, routine surgeries • Significant numbers of non-communicable disease including heart disease, diabetes mellitus, cancers and degenerative disorders being diagnosed • Rapid diagnostic kits (malaria), IDD kits, haemoglobin testing kits and pregnancy testing kits available with ANMs utilisation very low • Adequate supply of medicines, expensive antibiotics, out-of-stock for 2 weeks to 4 -5 months; ‘stock-outs’ more in higher level facilities (DH/SDH)

Major Findings • 25% BPM posts still vacant, most have joined in last one month • Untied grants transferred and available all levels utilisation 20 -30% • Block level health “Society” not formed; Block Health Plans prepared • VHSCs being formed: – Not active to their full potential; however, village health plans were prepared – Money lying with SC, mostly unused – VHSC members need greater orientation/training to utilize untied funds • Adequate accounting personnel in place; more IT enabled solutions, focus on internal controls, further rationalization of delegation of powers, communitization of audit process of VHSC / RKS necessary An operational study to review financial management – staffing, training, bank account and flow of funds, auditing and Internal control, in details is recommended • Design specific interventions to address neonatal mortality – like National Newborn Infection control programme; incentivize home based ASHA visits during neonatal period • Focus on immunization programme by identifying more vaccination sites, vaccinators, regular supply of vaccines and tracking of child.

Major Findings • Shortage of specialists at FRU/CHC/DH; 3/4 posts vacant in Dungarpur • Rural Medical Officer (RMO) cadre has increased availability at PHC levels: – No pre-induction training; post-induction training in small batches – RMOs lack adequate programme management experience • Multi-skilling training in progress; utilisation inadequate – In Dungarpur, training (anaesthesia) given to 4 MOs; services not utilized owing to shortage of surgeons/obstetricians, equipments and transfusion • ANM Training School, Dungarpur: – Very few refresher courses for ANMs – Curriculum content of ANM training courses not updated since long • Human resource training is fragmented and requires strengthening: – SIHFW currently under ad hoc funding – Regional Institutes at Jaipur and Ajmer are under the Directorate; not under SIHFW; no ‘regional’ distribution – Schools for LHV and ANM training are operating under the RCH

Major Findings • ASHA Sahayogini model is unique in Rajasthan – Attempted convergence between ICDS and Health – WCD controls recruitment and termination; fixed payments – Health department lacking administrative control and ownership – Cabinet approval for separate monitoring structure for ASHA • Referral transport: – Mostly hired by patients/families from the market – Utilisation of 102 ambulance service is limited – In some cases, payment being made from untied/VHSC funds – Inter-institutional referral transport arrangements working well • Pregnancy Tracking System (Dungarpur) requires adaptation and upscaling • Integrated reporting system modules available for RCH, NDCP, IDSP; to be expanded in 2009 -10; need to integrate ‘C to E’ forms • Several collaborations, including PPPs and social marketing: need for better management of contracts at district level • Health insurance is in crisis Rajasthan Swasthya Bima Yojana stopped after launch of RSBY (Ministry of Labor); Bhamashah scheme stopped due to non-compatibility of cards with RSBY software
- Slides: 16