Oral Hypoglycemics Roland Halil BSc Pharm ACPR Pharm

Oral Hypoglycemics Roland Halil, BSc. Pharm, ACPR, Pharm. D Clinical Pharmacist, Bruyere Academic Family Health Team Assistant Professor, Dept of Family Medicine, U of Ottawa July 2016

Objectives • List the classes of oral antihyperglycemic agents and understand their place in therapy. – Determine the relative efficacy, toxicity, cost and convenience of these agents before choosing therapy – Rationalize prescribing of oral hypoglycemics • Describe the current approach to pharmacologic management of type 2 diabetes.
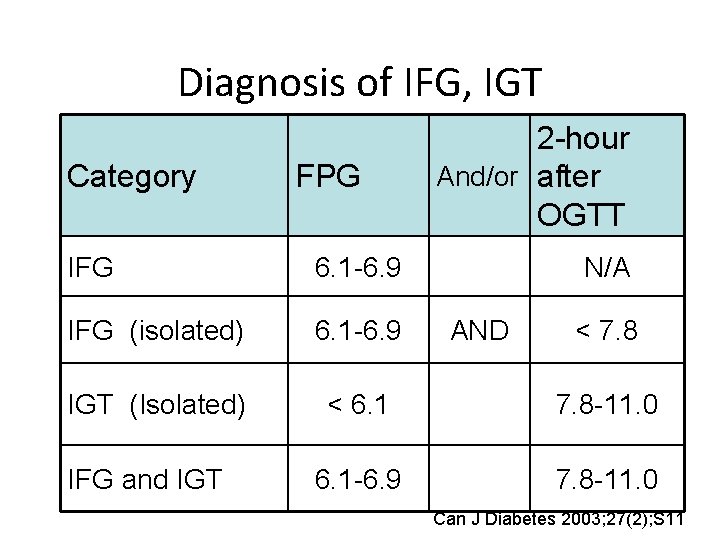
Diagnosis of IFG, IGT Category FPG 2 -hour And/or after OGTT IFG 6. 1 -6. 9 IFG (isolated) 6. 1 -6. 9 IGT (Isolated) < 6. 1 7. 8 -11. 0 6. 1 -6. 9 7. 8 -11. 0 IFG and IGT N/A AND < 7. 8 Can J Diabetes 2003; 27(2); S 11
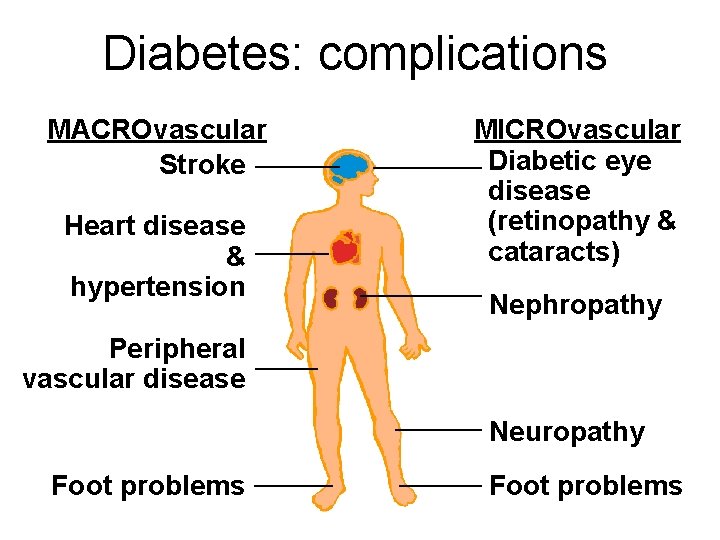
Diabetes: complications MACROvascular Stroke Heart disease & hypertension MICROvascular Diabetic eye disease (retinopathy & cataracts) Nephropathy Peripheral vascular disease Neuropathy Foot problems
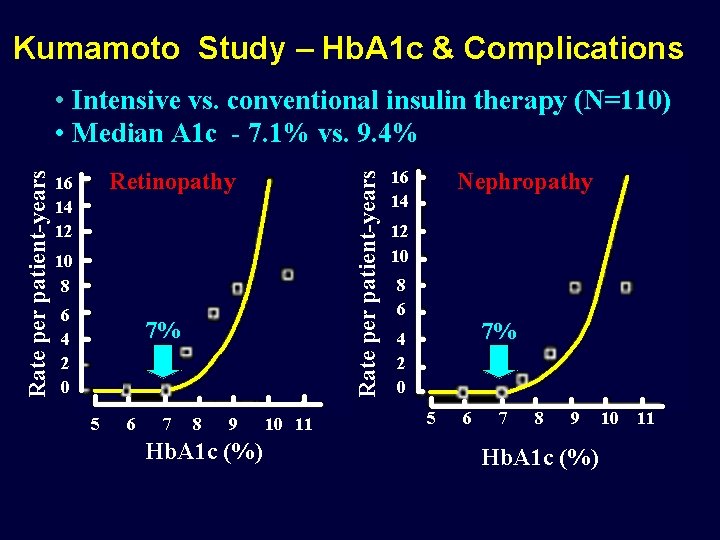
Kumamoto Study – Hb. A 1 c & Complications Retinopathy 16 14 12 Rate per patient-years • Intensive vs. conventional insulin therapy (N=110) • Median A 1 c - 7. 1% vs. 9. 4% 10 8 6 4 2 0 7% 5 6 7 8 9 Hb. A 1 c (%) 10 11 16 14 Nephropathy 12 10 8 6 7% 4 2 0 5 6 7 8 9 Hb. A 1 c (%) 10 11

Prevention of Diabetes in IGT • Lifestyle modification – (see Finnish Diabetes Trial) – Moderate weight loss (5%) (esp. abd fat) – Regular physical activity • > 150 minutes per week – 58% RRR for type 2 Diabetes at four years • Pharmacotherapy – Multiple effective trials • Eg. LIFE trial - Losartan onset of new DM 2 Can J Diabetes 2003; 27(2); S 12
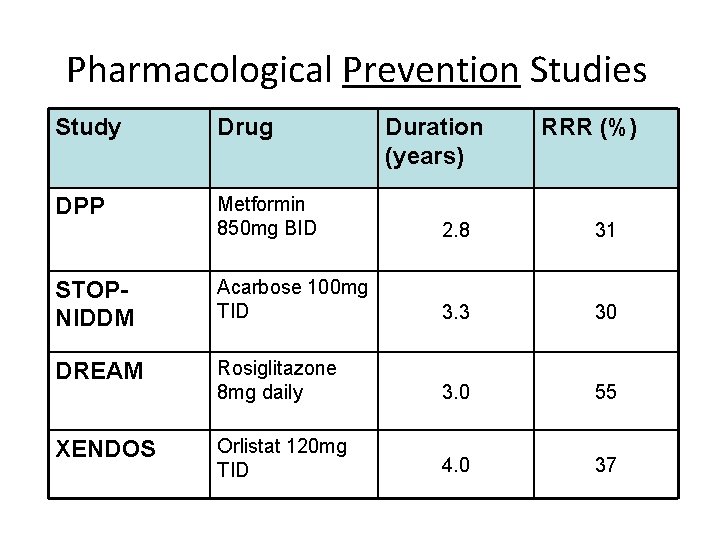
Pharmacological Prevention Studies Study Drug Duration (years) RRR (%) DPP Metformin 850 mg BID 2. 8 31 STOPNIDDM Acarbose 100 mg TID 3. 3 30 DREAM Rosiglitazone 8 mg daily 3. 0 55 XENDOS Orlistat 120 mg TID 4. 0 37

Non-Pharmacologic Tx Mainstay of therapy! • Nutrition therapy – ↓ A 1 c 1 -2% – CDA recommends counseling by a dietician for all type 2 diabetics – www. cvtoolbox. com diet for Type 2 diabetes Can J Diabetes 2003; 27(2); S 27

Pharmacotherapy Comparison of antihyperglycemics

Drug Classes Sensitizers Secretagogues Other
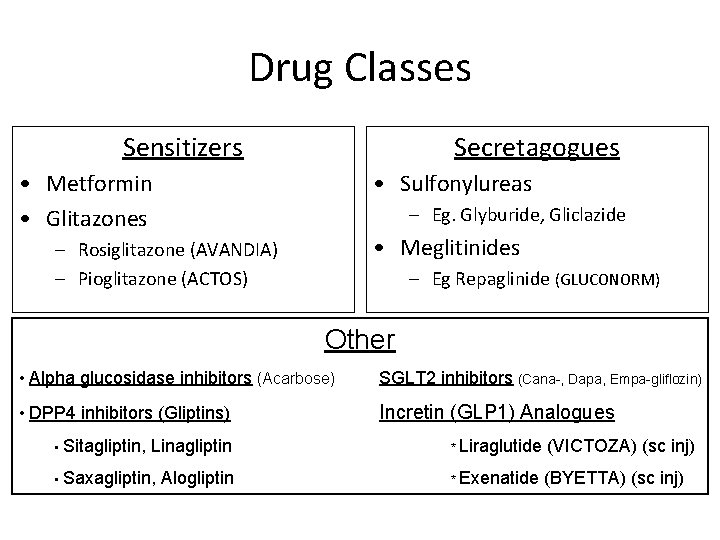

Drug Classes Sensitizers Secretagogues • Metformin • Glitazones • Sulfonylureas – Eg. Glyburide, Gliclazide • Meglitinides – Rosiglitazone (AVANDIA) – Pioglitazone (ACTOS) – Eg Repaglinide (GLUCONORM) Other • Alpha glucosidase inhibitors (Acarbose) SGLT 2 inhibitors (Cana-, Dapa, Empa-gliflozin) • DPP 4 inhibitors (Gliptins) Incretin (GLP 1) Analogues • Sitagliptin, Linagliptin • Saxagliptin, Alogliptin * Liraglutide (VICTOZA) (sc inj) * Exenatide (BYETTA) (sc inj)
Drug Classes Sensitizers • Metformin • Glitazones – Rosiglitazone (AVANDIA) – Pioglitazone (ACTOS) • Sensitizers – reduce insulin resistance • Increase glucose uptake & utilization in muscle and adipose tissue • Reduce hepatic glucose output

Drug Classes • ↑Basal & prandial insulin Secretagogues secretion, ↓hepatic gluconeogenesis • Doesn’t correct impaired • Sulfonylureas – Eg. Glyburide, Gliclazide 1 st phase insulin secretion; primarily affects 2 nd phase • Meglitinides • Beta-cell sensitizer – – Eg Repaglinide primes glucose mediated (GLUCONORM) insulin secretion (1 st phase)

Drug Classes: Other • Alpha glucosidase inhibitors (Acarbose) • Competitive inhibitor of pancreatic α-amylase and intestinal brush border α-glucosidases, resulting in delayed hydrolysis of ingested complex carbohydrates and disaccharides and absorption of glucose; Dose-dependent reduction in postprandial serum insulin and glucose peaks; inhibits the metabolism of sucrose to glucose and fructose • SGLT 2 inhibitors (Canagliflozin, Dapagliflozin, Empagliflozin) – Inhibits sodium-glucose cotransporter 2 (SGLT 2) in the proximal renal tubules, reducing reabsorption of filtered glucose from the tubular lumen and lowering the renal threshold for glucose (RTG). SGLT 2 is the main site of filtered glucose reabsorption; reduction of filtered glucose reabsorption and lowering of RTG result in increased urinary excretion of glucose, thereby reducing plasma glucose concentrations. • DPP 4 inhibitors (Gliptins) – (Sitagliptin, Lingliptin, Saxagliptin, Alogliptin) • Prolongs the action of endogenous incretin hormones by blocking their breakdown by the enzyme, dipeptidyl peptidase-4 (DPP-4). This leads to more insulin release after eating. • Incretin (GLP 1) Analogues – (Liraglutide (Victoza®), Exenatide (Byetta®)) – sc injection – mimic endogenous incretin hormones

Rational Prescribing • FOUR steps to Rational Prescribing: 1. Benefit 2. Harm 3. Cost 4. Convenience
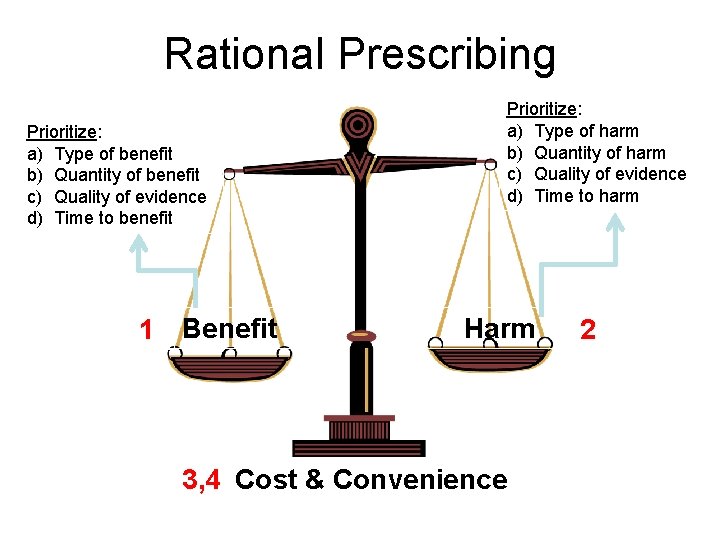
Rational Prescribing Prioritize: a) Type of benefit b) Quantity of benefit c) Quality of evidence d) Time to benefit 1 Benefit Prioritize: a) Type of harm b) Quantity of harm c) Quality of evidence d) Time to harm Harm 3, 4 Cost & Convenience 2

Benefit– Ask… 1. HARD Outcomes a) Any mortality benefit? b) Any morbidity benefit? Then, 2. SURROGATE Outcomes a) Clinically relevant?

Benefit 1. HARD Outcomes – Mortality benefit – Metformin – UKPDS-34 trial – Liraglutide – LEADER trial – ? Empagliflozin – EMPA-REG OUTCOME trial – Morbidity – Reduction in microvascular complications (nephropathy, retinopathy, neuropathy) 2. SURROGATE Outcomes a) Hgb-A 1 c reduction • Blood glucose level reduction – Fasting or Prandial b) Insulin Sparing Effects

Benefit A) Surrogate Outcome - Hgb-A 1 c – – ~ 1% to 2% • • • Metformin Sulfonylureas Repaglinide Glitazones (TZDs) Canagliflozin (1% - 2%) • Liraglutide / Exanatide (1% - 2%) (1% - 1. 5%) (0. 4% - 1. 5%) (0. 8 – 1%) ~ 0. 5% to 0. 9% • • Acarbose DPP 4 inhibitors (‘Gliptins) Dapagliflozin, Empagliflozin Nateglinide Nathan DM, et al. Diabetes Care 2008 (Dec); 31: 1 -11.

Benefit B) Surrogate Outcome - Insulin Sparing Effect – METFORMIN – ACARBOSE – TZD’s (GLITAZONE’s) – DPP 4 inh (‘gliptins) – Incretin Analogues (Liraglutide, Exenatide) – SGLT 2 inh (Canagliflozin, Dapagliflozin, Empagliflozin) = Weight neutral or weight negative = Reduction of hyperinsulinemia

Harm – Ask… 1. Serious / Rare Side Effects 2. Bothersome / Common s. e. 3. Age? • • Newer agents = Less Safety Data Older agents = More Safety Data
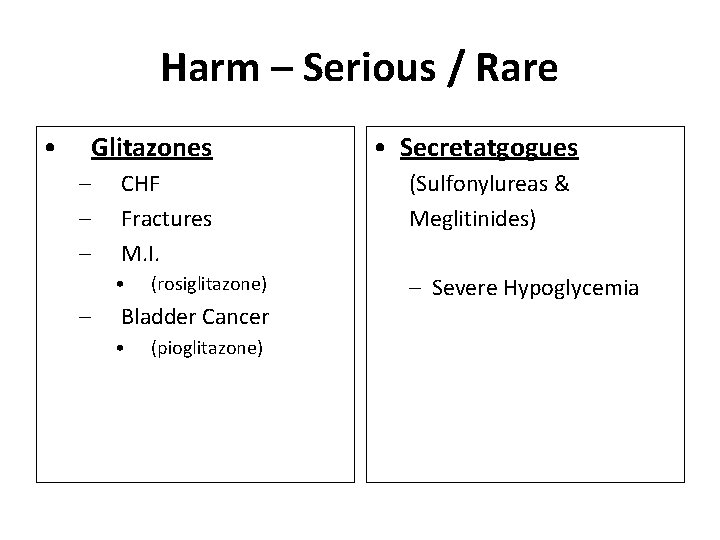

Harm – Serious / Rare • Glitazones – – • Secretatgogues CHF Fractures M. I. (Sulfonylureas & Meglitinides) • – Severe Hypoglycemia (rosiglitazone) Bladder Cancer • (pioglitazone)
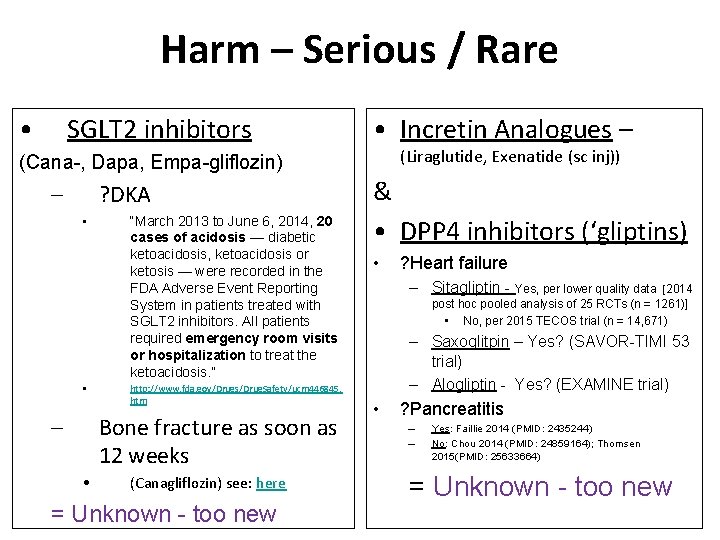

Harm – Serious / Rare • SGLT 2 inhibitors • Incretin Analogues – (Liraglutide, Exenatide (sc inj)) (Cana-, Dapa, Empa-gliflozin) – ? DKA • • – “March 2013 to June 6, 2014, 20 cases of acidosis — diabetic ketoacidosis, ketoacidosis or ketosis — were recorded in the FDA Adverse Event Reporting System in patients treated with SGLT 2 inhibitors. All patients required emergency room visits or hospitalization to treat the ketoacidosis. ” http: //www. fda. gov/Drugs/Drug. Safety/ucm 446845. htm Bone fracture as soon as 12 weeks • (Canagliflozin) see: here = Unknown - too new & • DPP 4 inhibitors (‘gliptins) • ? Heart failure – Sitagliptin - Yes, per lower quality data [2014 post hoc pooled analysis of 25 RCTs (n = 1261)] • No, per 2015 TECOS trial (n = 14, 671) – Saxoglitpin – Yes? (SAVOR-TIMI 53 trial) – Alogliptin - Yes? (EXAMINE trial) • ? Pancreatitis – – Yes: Faillie 2014 (PMID: 2435244) No: Chou 2014 (PMID: 24859164); Thomsen 2015(PMID: 25633664) = Unknown - too new

Harm – Serious / Rare • Metformin • ? Risk of Lactic Acidosis – 0. 03 to 0. 06 cases / 1000 pt-yrs – ~ 50% fatal – When implicated: • Metformin plasma levels are usually >5 μg/m. L • Cases - primarily diabetics w/ significant renal insufficiency, both intrinsic renal disease and renal hypoperfusion, w/ multiple medical/surgical problems and multiple medications.

Metformin Dosing • Dosing recommendations with renal insufficiency: – (CONTROVERSIAL) • Cr. Cl 60 ml/min→ – 1700 mg/day (Rxfiles) – 2. 5 g/day (Roland) • Cr. Cl 30 ml/min→ – 850 mg/day (Rxfiles) – 2. 5 g/day (Roland) • Cr. Cl < 30 ml/min→ – Contraindicated (Rxfiles) – 1 g/day (>20 m. L/min) (Roland) If NO other risk factors, else D/C. – Take home: assess OTHER RISK FACTORS for L. A. 1) Salpeter SR, et al. Risk of fatal and nonfatal lactic acidosis with metformin use in type 2 diabetes mellitus. Cochrane Database of Systematic Reviews 2010, Issue 4. Art. No. : CD 002967. http: //www. cochrane. org/CD 002967/ENDOC_risk-of-fatal-and-nonfatal-lactic-acidosis-with-metformin-use-in-type-2 diabetes-mellitus Accessed Sept 24, 2015 2) Nasri, H. et al. Metformin: Current knowledge. J Res Med Sci. 2014 Jul; 19(7): 658– 664. PMCID: PMC 4214027 http: //www. ncbi. nlm. nih. gov/pmc/articles/PMC 4214027/ Accessed Sept 24, 2015 3) A A Tahrani, et al. Metformin, heart failure, and lactic acidosis: is metformin absolutely contraindicated? BMJ. 2007 Sep 8; 335(7618): 508– 512. PMCID: PMC 1971167. http: //www. ncbi. nlm. nih. gov/pmc/articles/PMC 1971167/ Accessed Sept 24, 2015 4) Lalau JD. Lactic acidosis induced by metformin: incidence, management and prevention. Drug Saf. 2010 Sep 1; 33(9): 727 -40. PMID: 20701406

Risk Factors - Lactic Acidosis • Severe renal impairment – (caution if Cr. Cl < 30 ml/min) and • • Hepatic disease alcoholism CHF COPD CRF Pneumonia Ongoing acidosis – Lactic, keto etc.

Harm – Common / Bothersome 1) METFORMIN – GI upset / diarrhea – Start low, go slow! • Initial dose 250 mg QDaily to BID – B 12 / folate deficiency / anemia (6 - 8/100) • Reduced absorption – so, supplement – Anorexia – usually transient – Metallic taste

Harm – Common / Bothersome 2) Sulfonylureas: – Sulfa skin reactions • Rash / photosensitivity ~1% – Weight gain (2 -3 kg) – Mild Hypoglycemia: • Most with glyburide. Least w/ glimepiride & gliclazide • Requires consistent food intake • Major episodes 1 -2% (esp. in elderly)

Harm – Common / Bothersome 3) Glitazones: – Edema 4) Meglitinides: – Hypoglycemia 5) Acarbose: – GI upset / diarrhea / bloating 7) Incretin analogues – 8) SGLT 2 inhibitors – – – 6) Gliptins: – GI upset, edema, ? infection N/V/D, ? infection Hyper. K+, ARF (AKI) UTI (includes bacteriuria [asymptomatic], cystitis: 9%; females: 4%-18%; males: 4%), Genitourinary fungal infection (4%; females: 5% to 11% [includes bacterial vaginosis, cervicitis, vulvovaginal candidiasis, vulvovaginal infection, vulvovaginitis]; – males: 2% to 3% [includes balanitis, balanoposthitis, genitourinary fungal infection, penile infection, scrotal abscess])

Cost – Ask… • Patient cost vs Societal cost • Rx cost? • ODB coverage? • Covered under other plans?
Cost • From Rxfiles May 2013 – (N. B. June 2015 costs ~ same) • Cost per 100 days therapy (in Sask. ) • Alternatively, check ODB eformulary – N. B. Not true pt costs – Only comparative costs http: //www. rxfiles. ca/rxfiles/uploads/documents/members/cht-diabetes. pdf

Convenience • PO vs IV? • QD vs QID?

Convenience • • • Gliptin’s Glitazones SGLT 2 inh DPP-4 inhibitors GLP-1 analogs Sulfonylureas Metformin Meglitinides Acarbose - QD - QD sc inj – QD to BID - QD to TID – QD to TID with meals


• 1 st line – METFORMIN • 2 nd line - SULFONYLUREA or INSULIN – Meglitinide – if poor Cr. CL or irregular eating • 3 rd line – any other hypoglycemic if patients absolutely REFUSE insulin NEVER USE GLITAZONEs! Did I say, never? I meant NEVER!
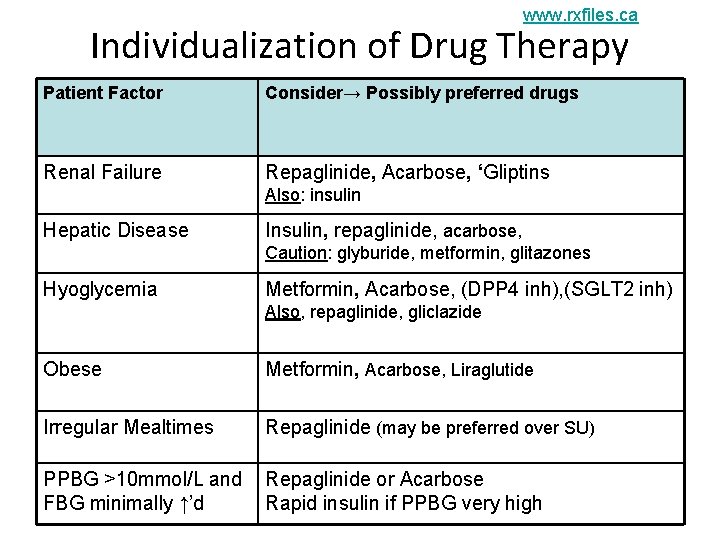
www. rxfiles. ca Individualization of Drug Therapy Patient Factor Consider→ Possibly preferred drugs Renal Failure Repaglinide, Acarbose, ‘Gliptins Also: insulin Hepatic Disease Insulin, repaglinide, acarbose, Caution: glyburide, metformin, glitazones Hyoglycemia Metformin, Acarbose, (DPP 4 inh), (SGLT 2 inh) Also, repaglinide, gliclazide Obese Metformin, Acarbose, Liraglutide Irregular Mealtimes Repaglinide (may be preferred over SU) PPBG >10 mmol/L and FBG minimally ↑’d Repaglinide or Acarbose Rapid insulin if PPBG very high

Questions?
- Slides: 37