ORAL HEALTH Dr Subhash Ghimire BDS MDS Oral

ORAL HEALTH � Dr Subhash Ghimire � BDS, MDS � Oral Maxillofacial Surgeon

SANN INTERNATIONAL COLLEGE
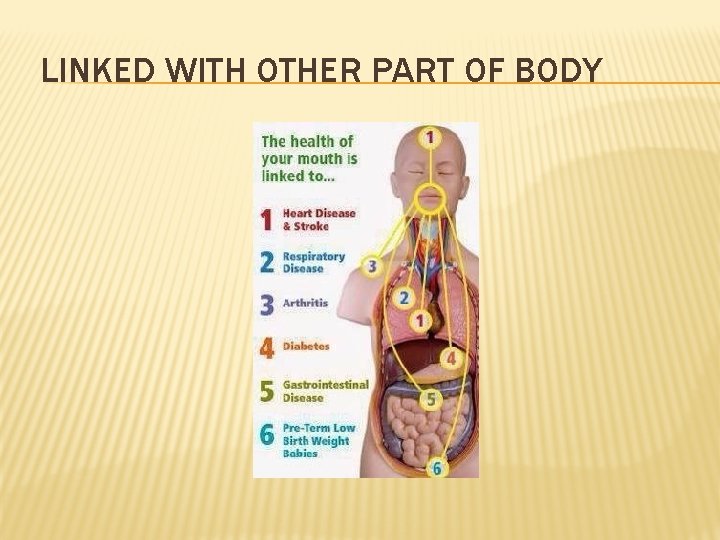
LINKED WITH OTHER PART OF BODY


TOBACCO

CANCER PATIENT BEFORE OPERATION
DURING OPERATION
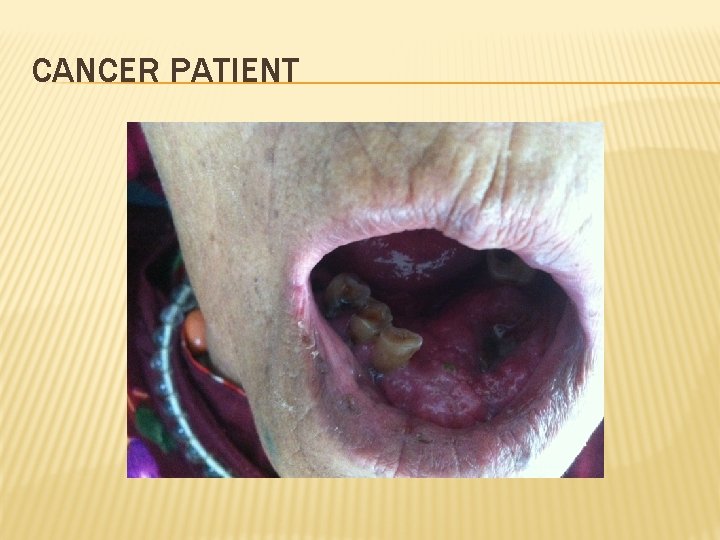
CANCER PATIENT

TO BE HEALTHY USE BRAIN





SMOKING CAUSES BREATH

DATA FOR DENTAL PROBLEM �. The prevalence of dental decay worldwide is 60 -90% in school children. The incidence of oral cancer ranges from 1 to 10 cases per 1, 000 populations in most countries.

STRESS RELIEF � � � A stressful lifestyle may not only lead to depression, high blood pressure , diabetes, heartdisease and anxiety, but it can also cause dental problems. Studies have shown that people who are stressed are more likely to neglect their dental care. Stressed-out people also have a tendency to grind their teeth. This can wear down the teeth. Stress can also cause a condition called dry mouth. Dry mouth occurs when there is not enough saliva produced in the mouth. Adequate saliva flow helps keep the mouth clean. Therefore, dry mouth can potentially lead to tooth decay. Fortunately, yoga is effective for alleviating stress. It helps alleviate stress by calming the mind and promoting relaxation.

DIABETES MELLITUS � � Diabetes mellitus is a clinical syndrome characterized by hyperglycemia due to an absolute or relative deficiency of insulin. Recent studies by the American Diabetes Association stated that about 18 million people in the United States have diabetes. An estimated 13 million are aware of the condition, however 5. 2 million have yet to be diagnosed and have no idea that they have the disease. In the United States alone 200, 000 die every year due to complications from diabetes. Dr. Smith and her talented team at Dental Health and Wellness Boston help diabetic patients understand how diabetes affects their dental health. As with any condition, good oral hygiene, including regular brushing, flossing and rinsing, as well as the proper diabetic diet, will go a long way in preventing needless problems. Yet, there are other aspects of dental health and wellness that should be considered for your optimum oral health. If you are diabetic, we are your dental partners, a diabetes dentist conveniently located in the Financial District of Boston

CARDIAC HEALTH DID YOU KNOW THAT GUM DISEASE IS CONNECTED TO HEART HEALTH? � Most people do not know that the health of their mouth is connected to the health of their heart. Several medical studies have shown that severe oral conditions including periodontal disease, tooth decay and tooth loss result in an increased risk for a heart attack or stroke. Therefore, when you get dental treatment, like non-surgical periodontal therapy, you are caring for your cardiac health and your oral health at once

DENTAL CARE FOR CARDIAC HEALTH – UNDERSTANDING THE CARDIAC-ORAL HEALTH CONNECTION Studies suggest that periodontal disease (gum disease) is associated with subclinical evidence of risk factors for heart attacks and strokes, including: inflammation and pathogens leading to thrombosis (formation of blood clots) and atherosclerosis (thickening of arterial blood vessel walls).

Avoiding Increased Systemic Inflammation � New information links gum disease with systemic inflammation. Gum disease causes the liver to increase production of C-reactive protein, which is an indicator of increased systemic inflammation. Systemic inflammation is a risk factor for heart problems (including myocardial infarction or diagnosis of peripheral artery disease) in otherwise healthy individuals. Studies have shown that treatment of periodontitis caused a 65% decrease in C-reactive proteins over a period of 3 months. �

� � The Same Damaging Pathogens Live in Your Gums and Your Heart Certain bacteria present in periodontal disease leads to increased blood platelet formation, and thus increased thrombosis, or, formation of blood clots. Recent evidence also shows the relationship between gum disease and heart disease by demonstrating the presence of a pathogen called LPS in the gums and plaque buildup in blood vessels around the heart. The pathogen Lipopolysaccharide (LPS) is present in the gums of patients with periodontal disease. The LPS travels to the heart through blood vessel endothelium (the thin, interior surface of the vessel). New evidence is suggesting that when the LPS pathogen arrives at the heart and encounters an atheroma (a buildup and swelling of cell and cell debris in artery walls), these harmful organisms can lodge in the vessel walls and stay there. Thus the bacteria is associated with the plaques within the vessels themselves. The presence of atheroma leads to atherosclerosis, a heart disease risk factor and the cause of about 50% of US deaths due to its complications. You can combat the harmful bacteria and microorganisms that live in both your mouth and your heart with proper dental treatment and care.

� How Does Acid Reflux Affect Your Dental Health The enamel of the teeth begins dissolving at a p. H of 5. 5, and the p. H of stomach acid is 2 or less.

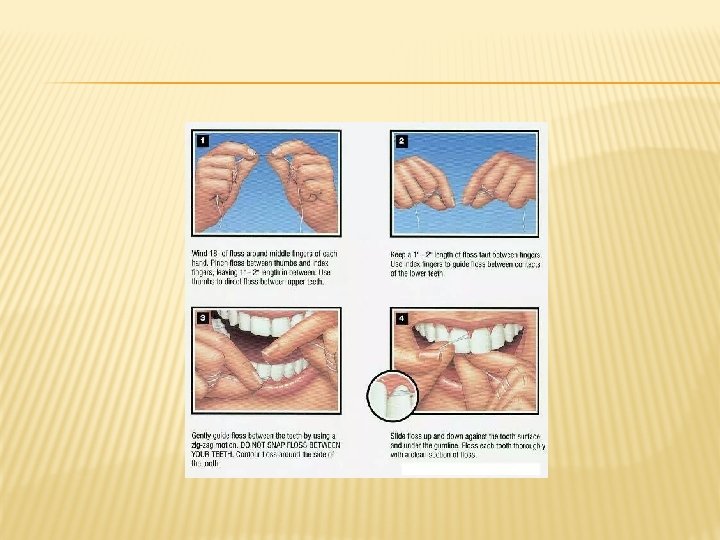
� � � � What Can I Do to Prevent Bad Breath? Bad breath can be reduced or prevented if you: Practice good oral hygiene. Brush twice a day with fluoride toothpaste to remove food debris and plaque. Brush teeth after you eat (keep a toothbrush at work or school to brush after lunch). Don't forget to brush the tongue, too. Replace your toothbrush every 2 to 3 months or after an illness. Use floss or an interdental cleaner to remove food particles and plaque between teeth once a day. Rinse with an antibacterial mouthwash twice a day. Dentures should be removed at night and cleaned thoroughly before being placed in your mouth the next morning. See your dentist regularly -- at least twice a year. He or she will conduct an oral exam and professional teeth cleaning and will be able to detect and treat periodontal disease, dry mouth, or other problems that may be the cause of bad mouth odor. Stop smoking and chewing tobacco-based products. Ask your dentist for tips on kicking the habit. Drink lots of water. This will keep your mouth moist. Chewing gum (preferably sugarless) or sucking on candy (preferably sugarless) also stimulates the production of saliva, which helps wash away food particles and bacteria. Gums and mints containing xylitol are best. Keep a log of the foods you eat. If you think they may be causing bad breath, bring the log to your dentist to review. Similarly, make a list of the medications you take. Some drugs may play a role in creating mouth odors.

� � � � � Why is basic dental care important? Practicing basic dental care: Prevents tooth decay. Prevents gum (periodontal) disease , which can damage gum tissue and the bones that support teeth , and in the long term can lead to the loss of teeth. Shortens time with the dentist and dental hygienist, and makes the trip more pleasant. Saves money. By preventing tooth decay and gum disease, you can reduce the need for fillings and other costly procedures. Helps prevent bad breath. Brushing and flossing rid your mouth of the bacteria that cause bad breath. Helps keep teeth white by preventing staining from food, drinks, and tobacco. Improves overall health. Makes it possible for your teeth to last a lifetime.

� � � � Are there ways to avoid dental problems? Keeping your teeth and gums healthy requires good nutrition and regular brushing and flossing. Brush your teeth twice a day-in the morning and before bed-and floss once a day. This removes plaque, which can lead to damaged teeth, gums, and surrounding bone. Use a toothpaste that contains fluoride, which helps prevent tooth decay and cavities. Ask your dentist if you need a mouthwash that contains fluoride or one with ingredients that fight plaque. Look for toothpastes that have been approved by the American Dental Association. Avoid foods that contain a lot of sugar. Sugar helps plaque grow. Avoid using tobacco products, which can cause gum disease and oral cancer. Exposure to tobacco smoke (secondhand smoke) also may cause gum disease as well as other health problems. 1 Practice tongue cleaning. You can use a tongue cleaner or a soft-bristle toothbrush, stroking in a back-to-front direction. Tongue cleaning is particularly important for people who smoke or whose tongues are coated or deeply grooved. Schedule regular trips to the dentist based on how often you need exams and cleaning.

� � � What Are the Symptoms? TMD often causes severe pain and discomfort. It can be temporary or last many years. It might affect one or both sides of your face. More women than men have it, and it’s most common among people between the ages of 20 and 40. Common symptoms include: Pain or tenderness in your face, jaw joint area, neck and shoulders, and in or around the ear when you chew, speak, or open your mouth wide Problems when you try to open your mouth wide Jaws that get "stuck" or "lock" in the open- or closed-mouth position Clicking, popping, or grating sounds in the jaw joint when you open or close your mouth or chew. This may or may not be painful. A tired feeling in your face Trouble chewing or a sudden uncomfortable bite -- as if the upper and lower teeth are not fitting together properly Swelling on the side of your face You may also have toothaches, headaches, neck aches, dizziness, earaches, hearing problems, upper shoulder pain, and ringing in the ears (tinnitus).

FOOD AND TEETH DIRECTORY � What foods you eat can directly affect your teeth in either a positive or negative way. Foods and drinks that you should avoid are those that are high in sugar like candies, pies, cakes, cookies, sodas, juices, and gum. These have loads of sugar that is a fuel source for bacteria, and frequent snacking or sipping leads to increased exposure. However, there are lots of things that you can eat and drink that will help keep your teeth healthy. Water, unsweetened tea, and milk are better choices for drinks during the day, and foods like meats, cheese, and nuts help keep teeth healthy. Find out more about what you should eat and not eat to keep your teeth healthy.

DIET � � � � � Diet is a risk factor for dental caries, coronary heart disease, stroke, diabetes, cancers and obesity. Diet – the foods and drinks we consume to nourish our body – and our eating habits have an important influence on our health and well being. A good diet provides the body with the appropriate quantity and quality of nutrients it requires to sustain health. Deficiency diseases such as anaemia and osteoporosis result from the inadequate intake of essential specific nutrients (undernutrition). Overeating or excessive intake of nutrients (overnutrition) leads to obesity, a recognised major health risk factor. Obesity is a serious problem in Ireland: in 2007, 25% of adults (24% of men; 26% of women) were obese; in 2002, 23% of boys and 28% of girls were either overweight or obese. Being overweight and obese increases the risk of coronary heart disease, stroke and Type 2 diabetes. Dietary guidelines in Ireland are based on the Food Pyramid published by the Health Promotion Unit ( www. healthpromotion. ie ) of the Department of Health. The Food Pyramid is designed to help people to eat a balanced diet combining several different types of food in the right amounts. The “top shelf” of the pyramid represents foods high in fat, sugar and salt which are not essential for health and which should be used sparingly (maximum 1 daily serving); the “bottom shelf” represents foods high in carbohydrates (e. g. , breads, cereals and potatoes) which should comprise the bulk of our diet (i. e. , 6+ daily servings). A survey of dietary habits of the Irish population (SLÁN 2007) found that only 14% of all adults surveyed (13% of men; 16 % of women) complied with the “top shelf” recommendation to use foods high in fat, sugar and salt sparingly. The top shelf of the Food Pyramid is of particular relevance to oral health as high consumption of foods/drinks containing added sugars is a direct cause of dental caries. The oral health message to restrict consumption of foods/drinks containing added sugars to mealtimes complements the healthy heart message to reduce consumption of foods high in oils and fats. Studies aslo show that eating more fruits and vegetables can have a protective influence against cancers and systemic inflammatory (including periodontal) diseases. Oral Health - the facts How to look after your teeth Nutrition & oral health Causes of oral ill health � � � � � � Oral Health & Disease Prevention » Health Factors » Dental Caries » Periodontal Disease » Oral Cancer Dental Trauma » Halitosis » Tooth Wear » Teeth Sensitivity » Cold Sores » Mouth Ulcers » Fractured Incisors Links between oral & general health Smoking & your dental health Alcohol Consumption Hygiene Injuries Stress and Control Socio-Economic Status Fear of the Dentist Fluorides & your oral health Dental services

� � � � � The Common Risk Factor Approach Traditionally, oral health promotion has focused on the care of the teeth and gums, in isolation from other health programmes. The Common Risk Factor Approach (CRFA) to health promotion takes a broader perspective and targets risk factors common to many chronic conditions and their underlying social determinants The key concept of this approach is that concerted action against common health risks and their underlying social determinants will achieve improvements in a range of chronic health conditions more effectively and efficiently than isolated, disease-specific approaches. Adoption of a common risk factor approach is more resource-efficient than a targeted disease-specific approach because: most chronic diseases have multiple risk factors one risk factor can impact on several diseases some risk factors cluster in groups of people risk factors can interact – in some instances synergistically – with each other. The common risk factor approach provides a rationale for developing multi-sectoral healthy alliances between health professionals, statutory, voluntary and commercial bodies and the general public. It recognises that engendering lasting changes in individual “lifestyle” behaviours requires supportive social, economic and political environments

� � � � Common Risk Factors for Oral Health Oral disease is the most widespread chronic disease, despite being highly preventable. The common risk factors that oral disease shares with other chronic diseases/conditions are: Diet – Risk factor for dental caries, coronary heart disease, stroke, diabetes, cancers, obesity Tobacco smoking/chewing – Risk factor for oral and other cancers, periodontal disease, coronary heart disease, stroke, respiratory diseases, diabetes Alcohol consumption – Risk factor for oral and other cancers, cardiovascular disease, liver cirrhosis, trauma Hygiene – Risk factor for periodontal disease and other bacterial and inflammatory conditions Injuries – Risk factor for trauma, including dental trauma. Control & Stress – Risk factors for periodontal disease and cardiovascular disease Socio-economic status – Independent risk factor as well as underlying determinant of other risk factors.

� It was last year that a team of NIDCR grantees published several intriguing new details about how the oral pathogen Porphyromonas gingivalis attaches to scavenging immune cells with its long, finger-like projections called fimbriae. Among these details was the discovery of a novel “inside-out” pathway that is wired within the immune cells. As described by the authors, once the fimbriae bind to a specific receptor on the surface of the immune cells, called monocytes, the receptor sends a signal inside the cell that curves back out to the surface and activates the so-called CD 11 b. CD 18 form of integrin, a protein that allows the immune cells to attach to objects. P. gingivalis may contribute to heart disease.

� � � Adult health Will taking care of my teeth help prevent heart disease? Answers from Thomas J. Salinas, D. D. S. Taking care of your teeth isn't a proven way to prevent heart disease. While there appears to be some connection between oral health and heart disease, more research is needed to fully understand it. Poor oral health has been debated as a possible cause of heart disease for many years. In 2012, experts from the American Heart Association reviewed the available scientific evidence and concluded that poor oral health hasn't been proved to cause heart disease — and that treating existing gum disease hasn't been proved to reduce the risk of heart disease. Still, many studies have shown a connection between gum disease (periodontitis) and other serious conditions, including heart disease. Research suggests that periodontitis is associated with an increased risk of developing heart disease and that people with chronic gum disease have increased thickness of their neck blood vessels. There is also a strong correlation between diabetes and cardiovascular disease, and evidence that people with diabetes benefit from professional teeth cleanings. Even though oral health isn't a key to heart disease prevention, it's important to take care of your teeth and gums: Brush your teeth at least twice a day. Floss daily. Replace your toothbrush every three months — or sooner if the bristles become bent. Schedule regular dental checkups and cleanings. If you're concerned about heart disease prevention, ask your doctor about proven ways to reduce your risk — such as stopping smoking and maintaining a healthy weight.

- Slides: 36