Optum Affordable Care Act ACA Overview Taken from

Optum Affordable Care Act (ACA) Overview Taken from Kaiser Summary of ACA Modified 04/23/2013
2 Anonymous Classroom Chat • Navigate to the URL below to enter our classroom chat for any questions or comments that you have – http: //Disposable. Chat. com/chat/Math 4067 • Please use any username that you please to mask your identity, however if you feel the need to have an identifiable username feel free to do so • This site is an external service, assume all messages are stored in an unencrypted and public manner • Please keep questions and comments appropriate • In person questions are still preferred, but we want to allow for more opportunities to engage with students 2
Excel Tips • Google is your friend! – There is no need to reinvent the wheel – Similar questions and problems have likely arisen somewhere in the past – Experts Exchange and other forums provide examples of Excel formulas for specific issues that you may come across • Microsoft provides support and technical information regarding all Excel functions – https: //support. office. com/en-us/article/Excel-functions-by-category-5 f 91 f 4 e 9 -7 b 4246 d 2 -9 bd 1 -63 f 26 a 86 c 0 eb 3
Week 2 Recap - Model Hints • Save your work as you will need to reference it in later weeks • Share your work with team members so that you all have the same starting point • Objective tasks – These are tasks meant to teach Excel formulae and introductory modeling. There is a correct answer! • Subjective tasks – These are the assumptions which you will make. There is no correct or incorrect answer. Quality depends upon your justification. 4

Week 2 Recap - Model Overview • B Tabs – Data inputs – Student assumptions (B-2) – Optum provided assumptions (B-3) • F Tabs – Twists to come in Week 4! • C Tabs – Continuance table/probability distribution • D Tabs – Net claims PMPM calculation (D-1) – Gross premiums PMPM calculation (D-2) • E Tab – Profit and loss projections 5
![Week 2 Recap - Model Overview [Tab B-3] • Optum provided assumptions – #1 Week 2 Recap - Model Overview [Tab B-3] • Optum provided assumptions – #1](http://slidetodoc.com/presentation_image_h2/fdccd65285ccc6a31e49dd8857f80772/image-6.jpg)
Week 2 Recap - Model Overview [Tab B-3] • Optum provided assumptions – #1 Credibility Weight: Extent to which the actuary believes past experience can predict future results. – #2 Age Factors: To go from a single, aggregate PMPM to PMPMs by age. – #3 Manual Claims: Aggregated, fully credible claims PMPM that’s used to scale the probability distribution of the claims and, when averaged with trended experience, reduces variance in the projected claims. – #4 Induced Utilization Factors: How do these impact your projected claims? 6
![Week 2 Recap – Net PMPM Calculation [Tab D-1] • Calculate the net claims Week 2 Recap – Net PMPM Calculation [Tab D-1] • Calculate the net claims](http://slidetodoc.com/presentation_image_h2/fdccd65285ccc6a31e49dd8857f80772/image-7.jpg)
Week 2 Recap – Net PMPM Calculation [Tab D-1] • Calculate the net claims PMPM 1. Determine trend rate 2. Calculate expected 2017 Experience PMPM by trending historical data forward and adjusting for plan design 3. Blend the Allowed Experience PMPM with the Manual Allowed PMPM using the credibility assumption 4. Calculate a Net-to-Allowed ratio based upon the Manual PMPM table 5. Apply Net-to-Allowed ratio to the blended Allowed PMPM to calculate a net PMPM 6. Apply age factors 7

Week 2 Recap – Manual Net to Allowed Demonstration • Visualization to show to tie the manual PMPM values from continuance table (C-1) to calculate the manual net-to-allowed ratio • Use default values below, then press “Submit Query” – Deductible: $1, 000 – Coinsurance: 0. 2 – OOPM: $5, 000 8

Week 2 Recap – What’s been done and Why! • Goal: – Price a Commercial Product • What has been completed? – Aggregate claims data and calculate PMPYs – Select assigned region, apply national and company specific trends – Select PMPM weights by year – Calculate Net PMPM • What are the next steps? – Apply retention – Apply region specific trends 9

Week 3 Lesson ACA and Other Current Topics
Main Components of ACA (aka Obamacare) Individual Mandate • Tax/Non-Tax • Need arose from pre-existing changes • Penalty reduced to $0 Medicaid Expansion • Increased income level for inclusion in Medicaid • States have option to increase • Assistance from federal government provided Affordability and Exchanges • Subsidies, Premium Credits, and Cost Sharing Reductions • Closes Medicaid → Private Insurance Gap • State run Exchanges for purchasing Insurance Overall Changes • Financial/Product Changes—minimum loss ratios • Health Insurance Changes • Proposed Changes by the AHCA 11

Individual Mandate Designed to get to full population coverage

Individual Mandate • Added in at request of insurance companies to combat anti-selection – Also it guarantees that uninsured percentage decreases – ACA requires coverage of pre-existing medical conditions – Without some sort of non-insurance penalty, many health individuals would skip coverage (i. e. , moral hazard) – Designed to produce an average cross-section of risks • Penalty reduced to $0 by current administration – Uninsured percentage has risen 13
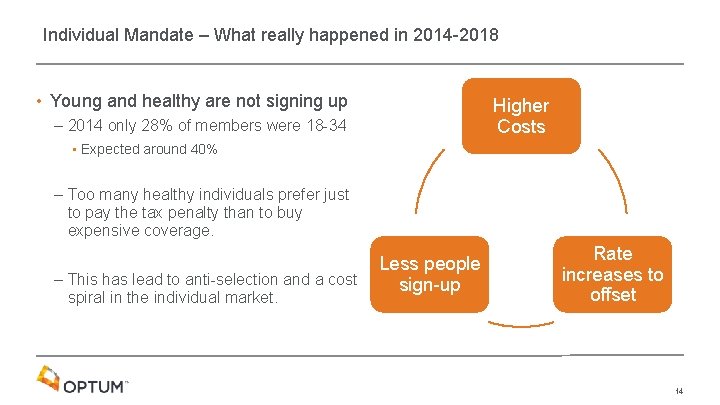
Individual Mandate – What really happened in 2014 -2018 • Young and healthy are not signing up Higher Costs – 2014 only 28% of members were 18 -34 • Expected around 40% – Too many healthy individuals prefer just to pay the tax penalty than to buy expensive coverage. – This has lead to anti-selection and a cost spiral in the individual market. Less people sign-up Rate increases to offset 14
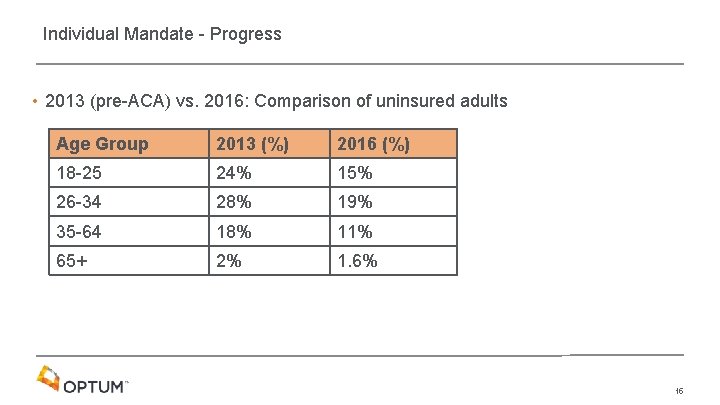
Individual Mandate - Progress • 2013 (pre-ACA) vs. 2016: Comparison of uninsured adults Age Group 2013 (%) 2016 (%) 18 -25 24% 15% 26 -34 28% 19% 35 -64 18% 11% 65+ 2% 1. 6% 15

On the other hand…. • Cost increases for large group (100 or more employees) plans have been at historically low levels. • Rates for small group (2 to 99 employees) plans initially jumped significantly with the removal of underwriting but later stabilized with relatively low rates of increase. • Reasons: ØGroup market is less affected by anti-selection and underwriting changes. ØACA significantly reduced uncompensated care—i. e. , care for people who can’t or don’t pay. Cost for this care is shifted to other payers. 16

Medicaid Expansion Designed for working, low income families

Medicaid Expansion • Began in 2014 • Expanded coverage to more non-Medicare eligible people under 65 • Expanded coverage to families with household incomes at 133% of Federal Poverty Level (FPL), or about $33, 000 per year in 2017. 18

Medicaid Expansion - Funding • For states that already met the expanded criteria no additional Federal Funding • For states that expanded their State Medicaid to meet Federal plan – 100% of coverage increase funded by Federal in 2014 -2016 – This % decreases over time until minimum amount in 2020 of 90% 19

Medicaid Expansion – Supreme Court Challenge • Supreme Court upheld that Medicaid expansion was constitutional • However, they struck down a component that would have allowed the Federal Government to withhold Medicaid funds from States that did not expand. – This makes it difficult for federal government to enforce expansion. – Thus making the expansion optional by states. 20
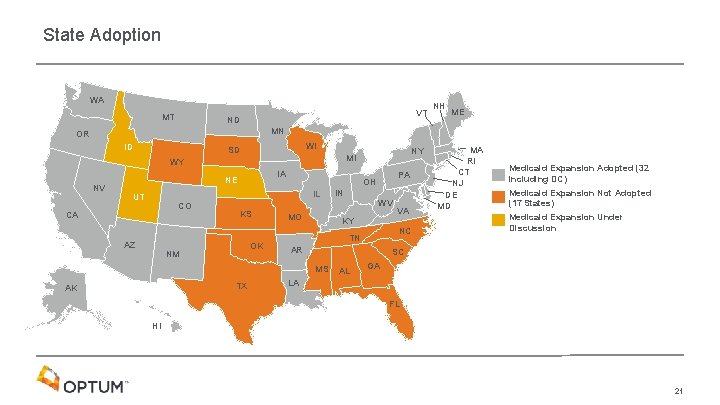
State Adoption WA MT VT ND NH ME MN OR ID WI SD NV IA NE CO CA AZ KS OK NM MO TX IN WV KY VA NC TN AR MA RI CT NJ DE MD Medicaid Expansion Adopted (32 including DC) Medicaid Expansion Not Adopted (17 States) Medicaid Expansion Under Discussion SC MS AK PA OH IL UT NY MI WY AL GA LA FL HI 21

Affordability Premium help for low income families and individuals

Affordability • Who is eligible for premium and cost sharing subsidies? – Premium subsidies: <400% FPL – Cost Sharing reductions: <250% FPL – Legal Immigrants – Employees not covered by their employer’s plan • Or employees whose plan or cost share does not meet certain categories 23

Affordability – cont. • Premium Credits – Used to purchase insurance on Exchanges – Tiered to offset premium costs – Tied to FPL and second lowest silver plan – Goal: Family should pay no more than 9. 5% of household income for insurance. • Cost Sharing Reductions – Increase a plan’s actuarial value, by lowering deductible, coinsurance, and/or OOP max to certain thresholds that vary by income level. – Insurers are supposed to be reimbursed for increased actuarial value, but Trump Administration has rescinded these payments, pending Congressional action. 24

Exchanges For individual and some small group coverage

Exchanges • Exchanges (HIX) are “places” where individuals and small businesses can go to shop for healthcare coverage • Exchanges can take many forms – State Based – State/Federal Partnership – Federally Managed 26
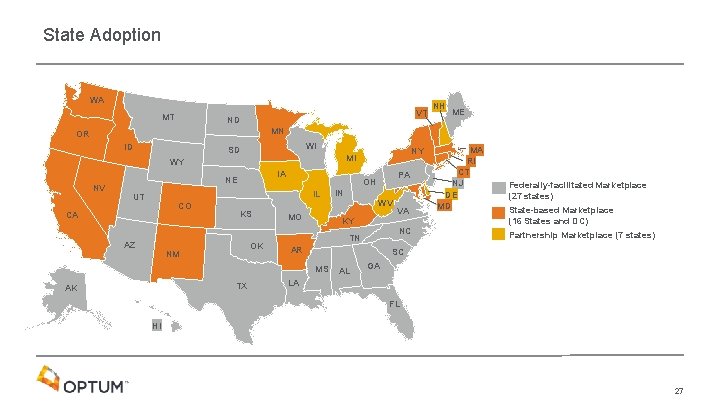
State Adoption WA MT VT ND NH ME MN OR ID WI SD NV IA NE CO CA AZ KS OK NM MO TX IN WV KY VA NC TN AR MA RI CT NJ DE MD Federally-facilitated Marketplace (27 states) State-based Marketplace (16 States and DC) Partnership Marketplace (7 states) SC MS AK PA OH IL UT NY MI WY AL GA LA FL HI 27

Overall Changes to Health Insurance and Health Care

Financial Changes • Tax Changes – Individual Mandate – “Cadillac Tax” assessed on plans with very rich benefits – Medicare Tax increase – 10% Tax on tanning services • Fees/Removal of Deductions – Fees placed on Pharmaceutical Sector – Fees placed on Health Insurance Sector 29
Product Changes • “Metal Plans”: Based on Actuarial Value (AV) = Benefits / Allowed Cost – Bronze (AV = 60% of allowed cost projected benefit level) – Silver (AV = 70% of allowed cost projected benefit level) – Gold (AV = 80% of allowed cost projected benefit level) – Platinum (AV = 90% of allowed cost projected benefit level) (leaving market) – All “metal” plans sold in the individual and small group markets must have an assessed Actuarial Value within + or – 2% of the above percentages. • Catastrophic plan – Available up to age 30 and individuals with low income 30
Health Insurance Changes • Preventive services – No member cost sharing allowed • Preexisting Conditions must be covered • Limit the rating variation by age to 3: 1, with up to 50% surcharge for tobacco use • Dependent Coverage available to age 26 31

Health Insurance Changes – cont. • Minimum Medical Loss Ratio (MLR) rules – 85% Large Group – 80% Small Group and Individual – MLR = [Claims + Health Quality Improvement Expense] / [Premiums – Taxes/Fees] – If actuarial MLR for a year is < minimum MLR, then excess must be refunded to policyholders. 32

Potential Changes Discussed in Prior Years – Repeal individual and employer mandate – Continuous coverage requirement for no underwriting or pre-existing condition waiver – Eliminate cost-sharing reduction (big increase for low income individuals) – Age rating change, from 3: 1 to 5: 1: reduces rates for young adults & hopefully increases their participation – Allow states to drop Medicaid benefits required by the ACA and basically no longer fund the ACA Medicaid expansion. – Allow limited benefit plans (i. e. Short Term Health Plans) that don’t provide “essential benefits” —This could segment the market between healthy and non-health individuals. – Allow small groups to band together for self-insured pools 33
Current State of Healthcare Debate • Versions of Medicare-for-All (M 4 A) • Only government run single payer • Public/Private Partnership • Public Option • Prescription Drugs • Medicare negotiations • Purchase drugs from other countries 34

Week 3 Lesson Retention

Premium Calculation – Retention (Tab B-2, Task 5) • Retention encompasses all non-benefit components of the premium rate and needs to be included in your premium calculation • Retention includes administrative expense, sales cost (commissions, etc. ), profit, risk margin, and government taxes and fees • Retention can be expressed in pricing as % of premium, % of claims, $ PMPM, $ per policy, or any combination of these – Examples: • Commissions are variable costs paid to agents/sales staff as a percentage of gross premium • IT Network development expenses are fixed costs allocated to all members on a PMPM basis • Membership administration and claims processing are typically allocated on a PMPM basis • Gross PMPM amount is calculated by applying Retention Amounts to Net PMPM 36

Retention Items • ACA assessment: Essentially a federal tax, approximately 3% of premium. • State premium tax: Assume 1% of premium. • Administration expenses Ø Member services, claims processing, general overhead: IT, actuarial, C-suite, etc. Ø Assume equal to $15 PMPM plus 4% of premium. • Commission and sales expense: See spreadsheet “GHP Sales Department Actual and Projected Budget. ” • Profit and Risk margin: What’s the difference? Ø For initial set of premiums, management wants 3% of premium for profit, 2% for risk margin. Ø Beware…at twist time, you may want to reconsider these! 37

Week 3 Model Overview – Tab E-1 • Profit and Loss (P&L) Statement – Financial analysis that summarizes projected cash flows – Breaks out revenues and expenses by categories – Used to analyze profitability of product • P&L differences by age: – Do results look reasonable? – How are PMPM margin and profit derived? • Scenario Analysis – Assumptions are educated best guesses. – Scenario analyses are basically “stress tests” that change various assumptions to project P&L performance under more or less favorable assumptions. 38

Week 3 Module Assignment – in class • Tab B-2 Task 5 – Input Retention Amounts • Excel file for assumption information • Hint: Not all line item expenses may be included in your pricing assumption • Tab D-2 Step 2 – Enter Gross Premium formula • This is an Objective Task with a correct answer • Determine formula to convert Net PMPM to Gross PMPM • Cells to fill in are highlighted yellow 39

Your Assignment! – Week 3 Complete the following in the model: • Objective: 1. Complete the Budget Excel Workbook 2. Fill in [B-5] Task 5 3. Fill in [D-2] Task 2 4. Ensure that all team members have the model filled out identically • Subjective 1. If not already done, research issues that are specific to your team’s region. Write 2 -4 paragraphs that answer the following questions: (See Week 2 Slide 26 for hints and details) 40
- Slides: 40