Optometry in Scotland Argyll and Bute CHP Report

Optometry in Scotland Argyll and Bute CHP Report

Donald G Barr l Ophthalmic Optician l Optometrist l ‘Optometerist’ l ‘Opteeshun’ l ‘Optimist’

Recommendations The CHP is asked to: l Consider the National position as outlined in the ‘Review of Eyecare Services in Scotland Interim Report Oct 2005. ’ l Consider the Implications of the new Optometry contract l Consider developing level 2 services in line with other Highland Health Board CHP’s

1 Background and Summary 1. 1 The general public and many health professionals are still unaware of the changes in provision of services since April 2006. 1. 2 With the dissolution of Argyll and Clyde Health Board and subsequent reorganisation and formation of the Argyll and Bute CHP, there is now an asymmetry in service across Highland Health Board’s area. 1. 3 Waiting time targets may require reorganisation of local services.

2. 0 Review of eyecare services in Scotland Interim Report October 2005 2. 1 Background 2. 2 Demographics 2. 3 Workforce 2. 4 Technology 2. 5 Waiting Times 2. 6 Access 2. 7 Communication 2. 8 Multi-disciplinary approach 2. 9 Equity

2. 1 Background “Traditionally within the NHS, the first point of contact for most patients with an eye problem is their General Practitioner. This has limited the level of care being provided for many people as many GP’s do not have the necessary equipment, expertise or experience to adequately diagnose and manage more complex eye conditions. Hospital eye departments have been used to manage the latter, the diagnosis and management of Ophthalmic conditions being undertaken by Ophthalmologists. Demands on the hospital eye service and an acknowledgement that some patients currently attending the hospital eye departments could be dealt with in the community has led to a need to review how eyecare services are designed and provided”
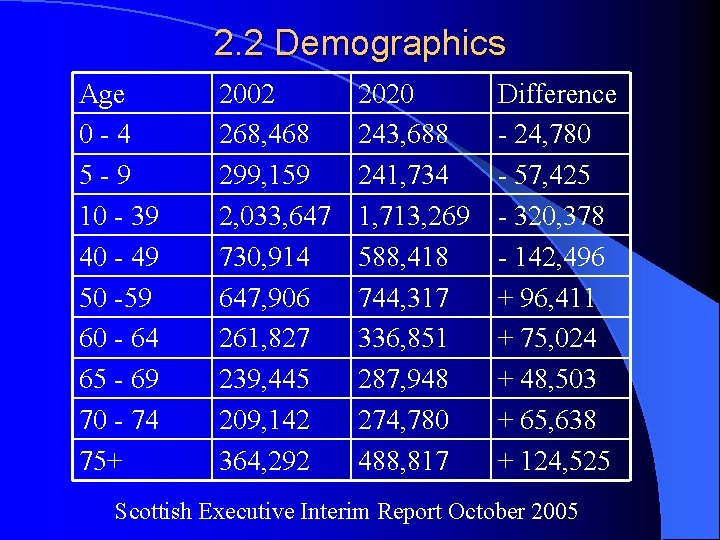
2. 2 Demographics Age 0 -4 5 -9 10 - 39 40 - 49 50 -59 60 - 64 65 - 69 70 - 74 75+ 2002 268, 468 299, 159 2, 033, 647 730, 914 647, 906 261, 827 239, 445 209, 142 364, 292 2020 243, 688 241, 734 1, 713, 269 588, 418 744, 317 336, 851 287, 948 274, 780 488, 817 Difference - 24, 780 - 57, 425 - 320, 378 - 142, 496 + 96, 411 + 75, 024 + 48, 503 + 65, 638 + 124, 525 Scottish Executive Interim Report October 2005

2. 2 Demographics In the year 2000… ‘It is estimated that 80% of the population who have serious eye problems are over 65’ ‘ 1 in 5 of the over 75 population is registerable as blind or partially sighted. ’ Scottish Executive Interim Report October 2005
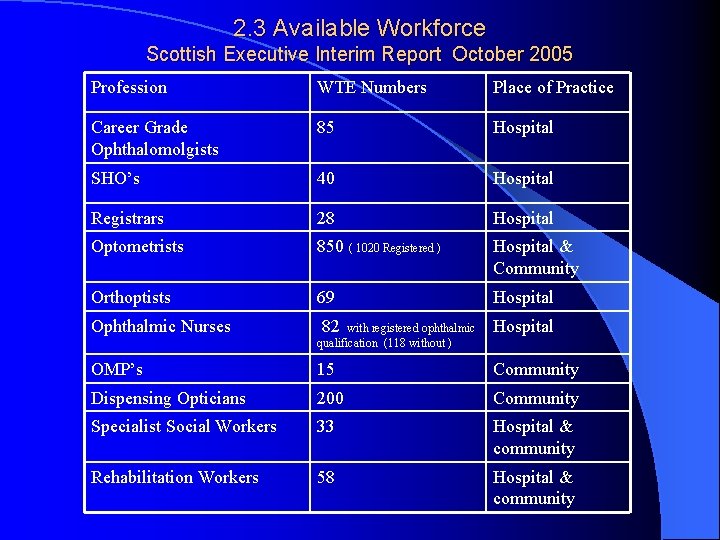
2. 3 Available Workforce Scottish Executive Interim Report October 2005 Profession WTE Numbers Place of Practice Career Grade Ophthalomolgists 85 Hospital SHO’s 40 Hospital Registrars 28 Hospital Optometrists 850 ( 1020 Registered ) Hospital & Community Orthoptists 69 Hospital Ophthalmic Nurses 82 with registered ophthalmic qualification (118 without ) Hospital OMP’s 15 Community Dispensing Opticians 200 Community Specialist Social Workers 33 Hospital & community Rehabilitation Workers 58 Hospital & community

2. 4 Technology l Digital Imaging l Slit Lamp Biomicroscopy l Automated Visual Field Threshold Screening l Tonometry l Gonioscopy l Scanning Laser Ophthalmoscope

2. 5 Waiting Times What are our targets ? l Sco Exec Targ Ident A. 04 T ‘By the end of 2005, no patient will wait longer than 6 months from GP referral to an out-patient appointment, reducing to 18 weeks from December 2007. ’ l Sco Exec Targ Ident A. 06 T ‘ By the end of 2007 the maximum wait for cataract surgery will be 18 weeks from referral to completion of treatment. ’ How do we do it ? l Improve quality of referrals. l Reduce unnecessary referrals by using referral refinement (level 1) and adopting the Highland Integrated Eyecare Scheme (HIES) (level 2). l Remove ‘Chronic and Stable’ patients from the hospital eye service ?

2. 6 Access Optometry is designed to be the new ‘gateway’ to NHS eyecare. l New relationships need to be forged to improve the patient journey / experience. These include relationships between; Patients, Optometrists, Ophthalmologists, PPF, A&B Council (Social work and Low Vision Team) and Voluntary organisations (RNIB, Macular Disease Society etc). l Improve physical Access to NHS services. Many Visual problems are noticeable. Disability Discrimination Act. l

2. 7 Communication Patients should be given useful and appropriate advice and information. l NHS staff should receive sensory awareness training. l NHS contractors should communicate rapidly and efficiently on behalf of the patient e. g using IT for direct Hospital referrals; using digital images for fast diagnosis and streamlined referrals; feedback loops to ensure the probity of diagnosis. l

2. 8 Multi-Disciplinary approach ‘No single agency or professional group can respond to all of the challenges that present when managing visual problems. The development of coordinated multidisciplinary professional groups will ensure that individuals receive the care they need from the most appropriate professional irrespective of where they are in their care journey. ’ e. g The current certification and registration procedure for the blind and partially sighted is archaic.

2. 8 Equity ‘While this review of eye health care looks at the position across Scotland, the impact on the patient will be determined by local arrangements devised to meet local circumstances. It is therefore important that, while the principles of good practice set out in the review apply across Scotland, so that there is equitable access to high quality services, geographical differences will mean that different approaches have to be taken to meet local needs. ’

The New Eye Examination Level 1 l l l l l EVERYONE in Scotland is entitled to a FREE eye examination. Px’s under 16 and over 60 can be seen routinely every year, those in between, every 2 years. Any Px can be seen on a second occasion for referral refinement. ANYONE can be seen at ANYTIME if they have a presenting symptom. Px’s aged 60 and over are encouraged to have dilation and those over 70 are expected to have this as a matter of course. Slit Lamp Bio-microscopy will be carried out on all Px’s. Indirect Ophthalmoscopy will be the choice for retinal examination. Aplanation tonometry will be used for referral refinement. Visual Fields will be performed using Automated Perimetry. Direct referrals are now encouraged. (Highland Looking at NHSnet and digital ‘Bulletin Board’).

Level 2 Examination Community Management /Shared Care l GIES (Glasgow Integrated Eyecare Scheme) (Appendix 1). l HIES (Highland Integrated Eyecare Scheme). l Glaucoma and Diabetes Shared Care. l CCI (Campaign for Change Innovation) clinical pathways (Appendix 2).

3. 0 Contribution to LDP and Corporate objectives l Health Improvement by offering all Px’s a free, and clinically improved service. l Efficiency in cutting unnecessary referrals and reducing waiting times. l Uniform access to eyecare services across the Boards area. l Treatment appropriate to the individual involving a multidisciplinary approach.

4. 0 Governance Implications Staff Governance: All Optometrists require to be registered with the Board, (Disclosure Scotland checked etc), GOC and BCO. PDP’s are encouraged and a mandatory 12 point quality assurance registration scheme applies nationally. For Level 2 initiatives quality assurance is built in with further training, assessment and mandatory audit – Px risk assessment is fundamental to any referral scheme. l Patient Focus and Public Involvement: Improved patient information and consent procedures are now being proposed. Public consultation has resulted in the WTI, CCI pathways and subsequent service development. All improvements have been Px driven. l Clinical Governance: SE key targets are based on Px access (A. 04 T and A. 06 T). These are the success criteria. l Financial Impact: The above proposals will have a cost implication in that although it is hoped to considerably reduce Px waiting times, it may have no impact on Consultant demands. Optometric services are considerably less expensive than Consultant led programmes. l

Impact assessment The impact of these proposals will be measured by the success of achieving targets A. 04 T and A. 06 T. S Sustainable M Measurable A Accessible R Repeatable T Time framed
- Slides: 20