Optimisation of antibiotic use to minimise resistance and

Optimisation of antibiotic use to minimise resistance and maximise clinical efficacy Pierre-Louis Toutain Visiting Professor Royal Veterinary College , London 7 July 2018 Australian & New Zealand College of Veterinary Scientists QT Gold Coast, Surfers Paradise Australia

To maximise efficacy • • • The right diagnosis The right drug The right formulation The right dose The right time to initiate treatment The right duration of treatment 2

1 -The right diagnosis 3

Obtaining an Accurate Diagnosis • Diagnostic specimens submitted to the microbiology laboratory before the institution of AMD therapy • Delay (48 -72 h) • New platforms for rapid diagnosis and testing are expected 4

New platforms for rapid diagnosis and testing • Rapid microbiological identification – Identification of the causative pathogen – Currently culture-based technique (days) – Molecular and genomic (Next generation Sequencing and others) – Mass spectrometry (30 min) • Rapid AST – The current microdilution methods over 4 -6 h rather than 24 h – New technology (microfluidic)
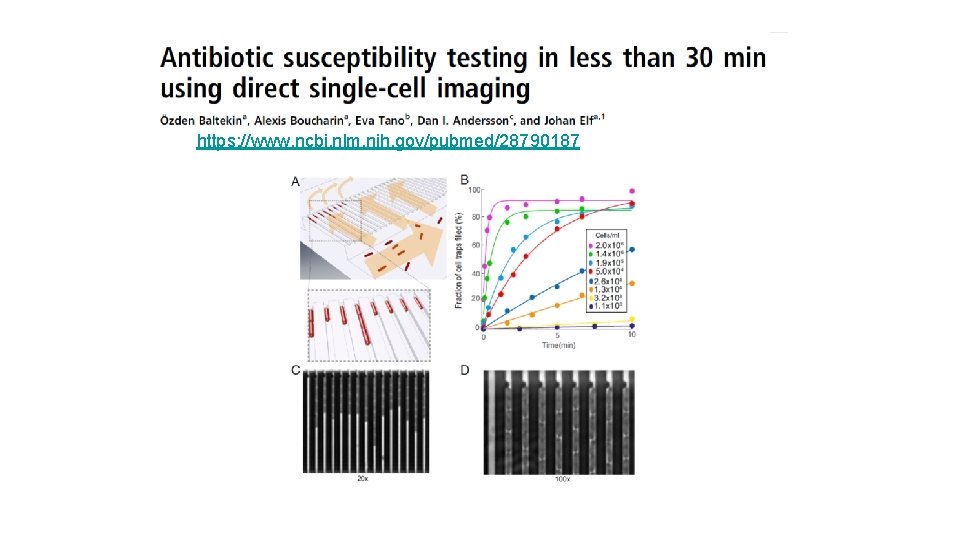
https: //www. ncbi. nlm. nih. gov/pubmed/28790187

https: //www. ncbi. nlm. nih. gov/pubmed/28133869 https: //www. ncbi. nlm. nih. gov/pubmed/27890457

2 -Selection of the right drug for efficacy 8

Empiric vs. Definitive AMD Therapy https: //iscaid. org/guidelines 9

https: //www. ncbi. nlm. nih. gov/pubmed/21776346 10

https: //www. ncbi. nlm. nih. gov/pubmed/24720433 11

Veterinary Record (2013) EMA and the Federation of Veterinarians of Europe (FVE) undertook a survey into the decision-making process of veterinarians in Europe when deciding which antibiotics to prescribe. The survey was completed by 3004 practitioners from 25 European countries AST before starting treatment was frequently undertaken by 37. 8 per cent of practitioners, but 9. 8 per cent never request such tests, and 44. 3 per cent only on a seldom basis prompted by poor response or complicated cases. https: //www. ncbi. nlm. nih. gov/pubmed/24068699

What the incentives might be to encourage more widespread use of AST. • More rapid results • Cheaper tests • More reliable laboratory results (e. g quality tests, testing on specific antibiotics used in animals rather than humans); • Need for accurate in-house test kits; for easier sampling methods; ways to send samples
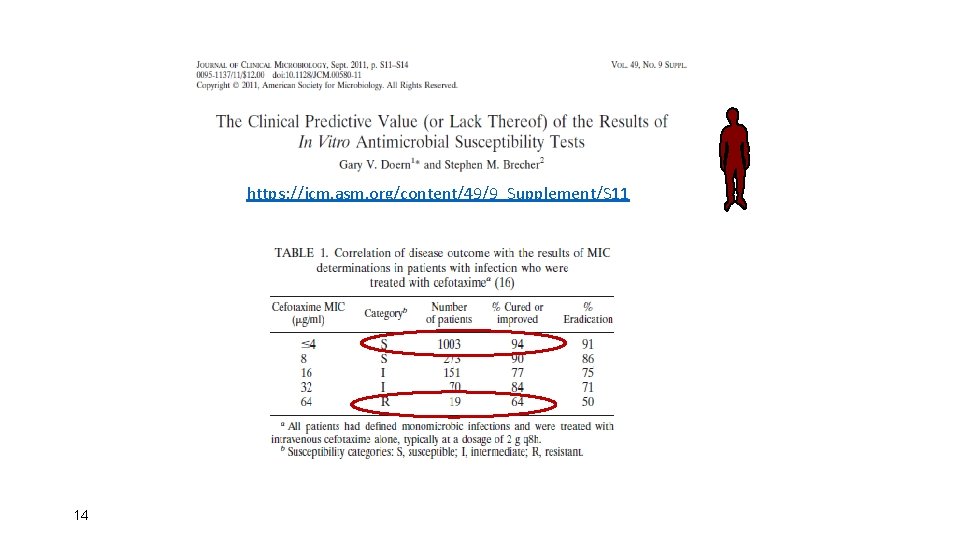

https: //jcm. asm. org/content/49/9_Supplement/S 11 14

2 -the right drug 15

Availability of AMDs WHO and critical AMDs: 2016 • it is recommended by the WHO, to reserve to human medicine the most critical antibiotics keeping for veterinary medicine the most outdated substances.

Is it a good medicinal practice to encourage the use of old antibiotics rather new ones? https: //www. ncbi. nlm. nih. gov/pubmed/17395687 For three antibiotic classes (quinolones, cephalosporins and carbapenems), it was observed that the less active drugs could be worse at hastening the spread of resistance than more active drugs in the same class. This led the authors to qualify the (WHO) stratagem of recommending the use of old antibiotics as part of microbiological folklore 17

3 -The right formulation 18

The right formulation

The right formulation • A long acting antibiotic is desirable for observance reasons: • it is likely best to develop an antibiotic having an intrinsic short half-life but formulated as a long acting formulation: – Difficult to maintain Css for 3 -5 days without a long tail

4 -The right dose for efficacy 21

The PK/PD targets to achieve are known 22
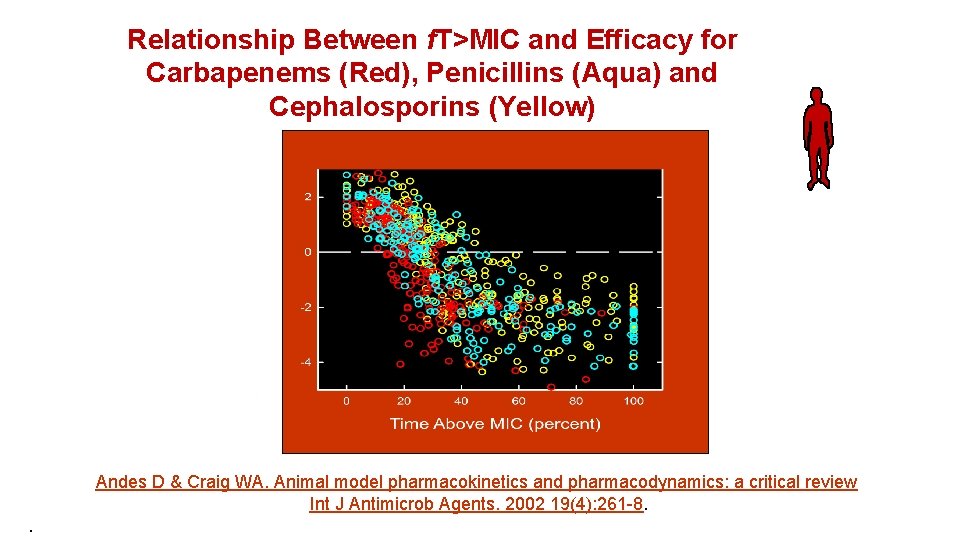
Relationship Between f. T>MIC and Efficacy for Carbapenems (Red), Penicillins (Aqua) and Cephalosporins (Yellow) Andes D & Craig WA. Animal model pharmacokinetics and pharmacodynamics: a critical review Int J Antimicrob Agents. 2002 19(4): 261 -8. .
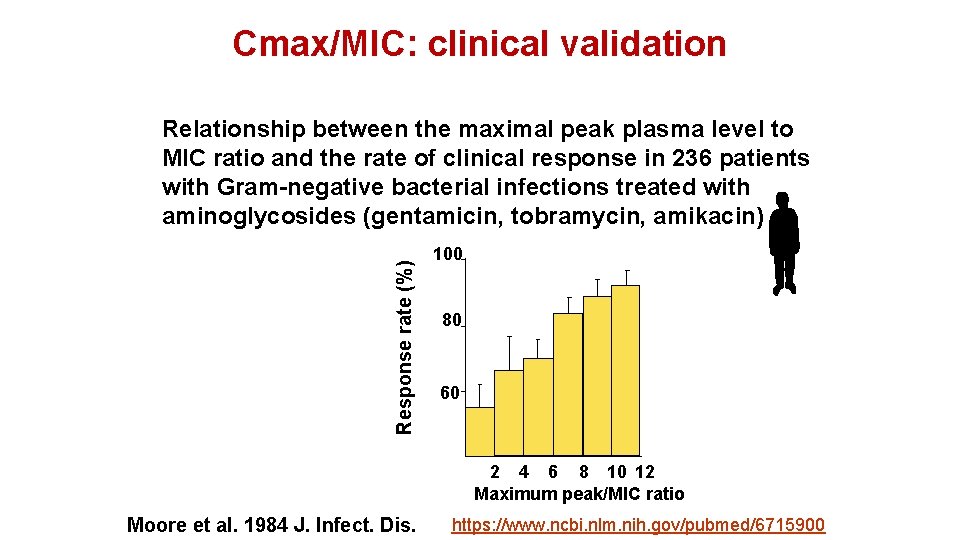
Cmax/MIC: clinical validation Response rate (%) Relationship between the maximal peak plasma level to MIC ratio and the rate of clinical response in 236 patients with Gram-negative bacterial infections treated with aminoglycosides (gentamicin, tobramycin, amikacin) 100 80 60 2 4 6 8 10 12 Maximum peak/MIC ratio Moore et al. 1984 J. Infect. Dis. https: //www. ncbi. nlm. nih. gov/pubmed/6715900
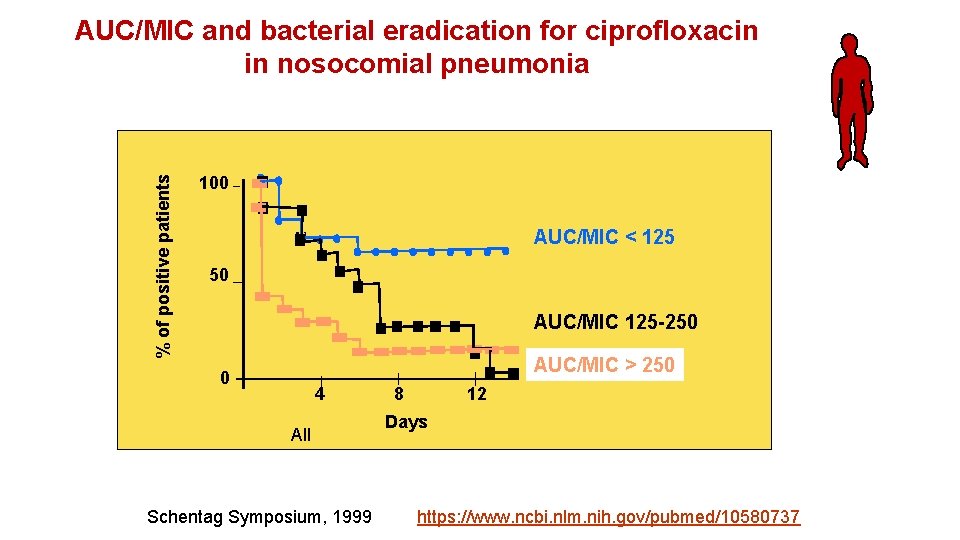
% of positive patients AUC/MIC and bacterial eradication for ciprofloxacin in nosocomial pneumonia 100 AUC/MIC < 125 50 AUC/MIC 125 -250 AUC/MIC > 250 0 4 All Schentag Symposium, 1999 8 12 Days https: //www. ncbi. nlm. nih. gov/pubmed/10580737

Computation of a dose for a fluoroquinolone e. g. if the objective is an AUC/MIC=125 h, therapeutic concentration should be 125 h/24 h≈5 XMIC
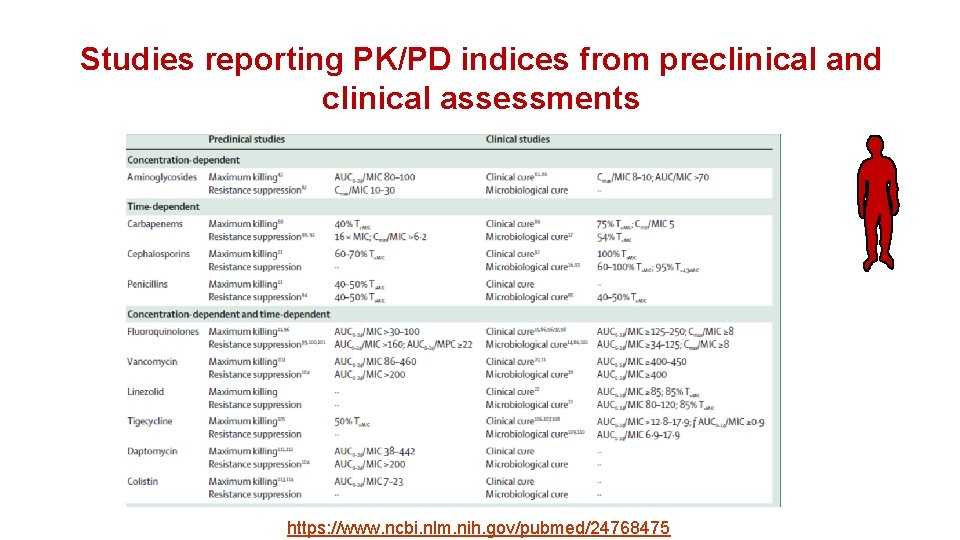
Studies reporting PK/PD indices from preclinical and clinical assessments https: //www. ncbi. nlm. nih. gov/pubmed/24768475

Now what dosage adjustments are needed to achieve the PK/PD index regarding all possible factors of variability?

Population PK • Precision medicine – Dosage adjustment using covariates (if required) – TDM for some AMD – Computation of the best individual dose (bayesian approach)

The right dose: 3 D printing pharmaceuticals The concept of personalised medicines becoming a reality Fabricating customised small or ‘one-off’ batches. Dose individualization and Flexibility including combination

in 2016, the first 3 D-printed tablet approved by the US Food and Drug Administration (FDA) was commercialised for the treatment of epilepsy (Spritam by Aprecia Pharmaceuticals ). 1 https: //www. ncbi. nlm. nih. gov/pubmed/29534837 i

5 -The right time to start a treatment 32

Timing of Initiation of Antimicrobial Therapy • As early as possible: – sepsis • Delayed: – for some chronic conditions until specimens have been obtained
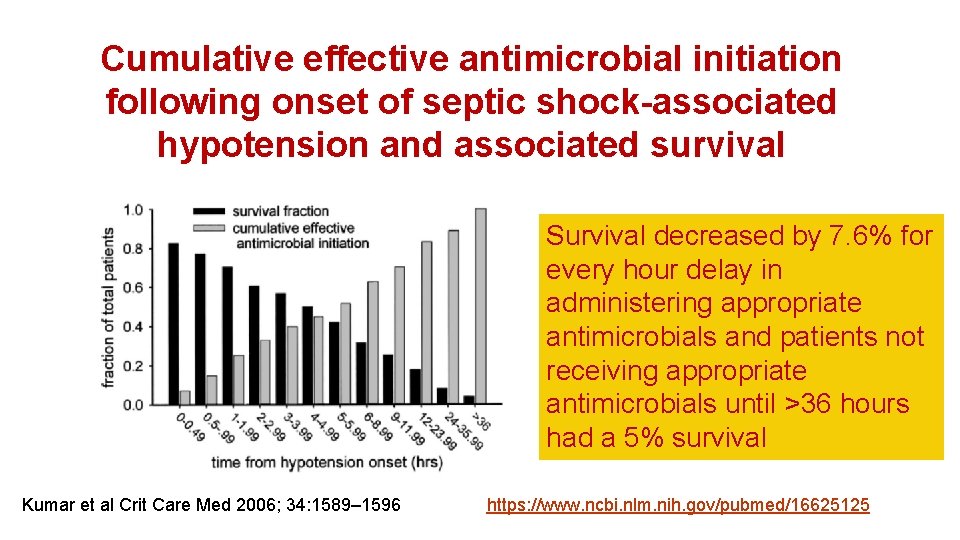
Cumulative effective antimicrobial initiation following onset of septic shock-associated hypotension and associated survival Survival decreased by 7. 6% for every hour delay in administering appropriate antimicrobials and patients not receiving appropriate antimicrobials until >36 hours had a 5% survival Kumar et al Crit Care Med 2006; 34: 1589– 1596 https: //www. ncbi. nlm. nih. gov/pubmed/16625125

https: //www. ncbi. nlm. nih. gov/pubmed/20888712
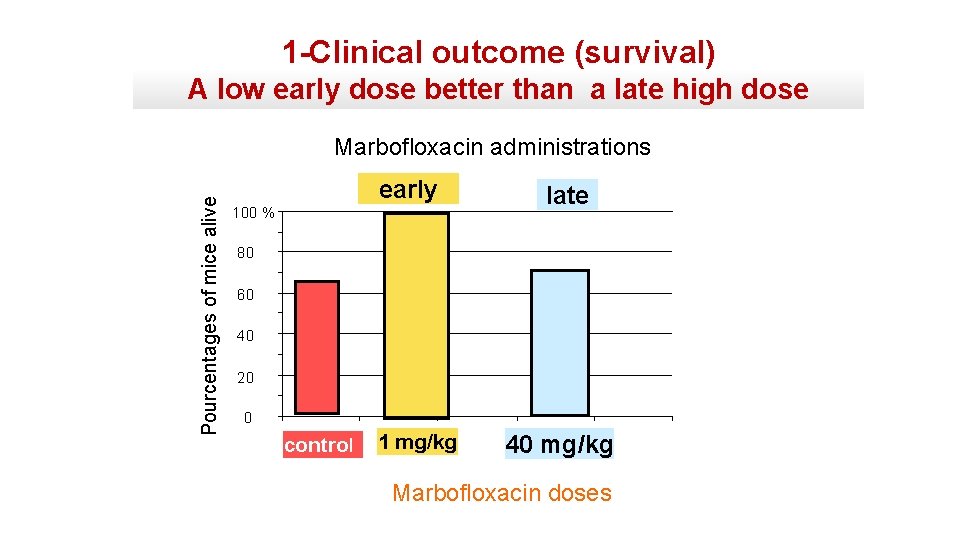
1 -Clinical outcome (survival) A low early dose better than a late high dose Pourcentages of mice alive Marbofloxacin administrations early 100 % late 80 60 40 20 0 control 1 mg/kg 40 mg/kg Marbofloxacin doses

3 -Selection of resistant target bacteria A late 1 mg/kg marbofloxacin dose select resistance (observation at 16 or 38 h after the marbofloxacin administration) % of mice with resistant bacteria Marbofloxacin administrations 50 % late Early 40 observation 16 hours after marbofloxacin administration = 48 hours after the infection = like early administration 30 20 +38 h 10 0 control 1 mg/kg 40 mg/kg 1 mg/kg Marbofloxacin doses 40 mg/kg +38 h

6 -The right Duration of AMD therapy

https: //www. ncbi. nlm. nih. gov/pubmed/24673608 No difference in cure rates between shortduration sulfonamide (3 days) and longduration cephalexin (10 days) treatments in female dogs with uncomplicated cystitis

The right Duration of AMD therapy • With rare exceptions (e. g. bacteremia due to S. aureus, endocarditis, osteomyelitis), there is no evidence to support most of the traditional 10– 14 -day courses of antibiotics, which are based more on conventional wisdom than strong evidence. • Short-course therapy for urinary tract infection, acute otitis media, tonsillopharyngitis, sinusitis and pneumonia is slowly gaining support (MASTIN study group, 2002; Lutters and Vogt, 2002). https: //www. ncbi. nlm. nih. gov/pubmed/12137628 40

To minimise resistance 41

https: //www. ncbi. nlm. nih. gov/pubmed/29916349

An overview of the general principles of optimal antimicrobial treatment, including species-specific recommendations for improving antimicrobial use in pig, cattle, small animal, and equine veterinary practices https: //www. ncbi. nlm. nih. gov/pubmed/29932044

1 - No misuse 44

Selected examples of misuses of AMD in vet medicine • Elective arthroscopies in horses – A clean procedure where AMD are not recommended in humans – perioperative AMD administration to 98% of horses (Weese et al 2009) • Superficial pyoderma in dogs – National and international guidelines recommend topical therapy alone (without coadministration of systemic antimicrobial drugs) – A UK study revealed that 92% of dogs with a diagnosis of pyoderma were prescribed systemic therapy, whereas only 5% of dogs were prescribed topical therapy alone (Summers et al 2014) • AMD treatment of subclinical bacteriuria or pyuria and Feline Lower Urinary Tract Disease (FLUTD) – In Canada , 74% of cases associated with FLUTD were treated with antimicrobials (Murphy et al 2012) https: //www. ncbi. nlm. nih. gov/pubmed/19412399 https: //www. ncbi. nlm. nih. gov/pubmed/25293803 https: //www. ncbi. nlm. nih. gov/pubmed/22942447

2 - No overuse 46

Generics and antibiotic consumption https: //www. ncbi. nlm. nih. gov/pubmed/20363806

Generics, me-too and antibiotic consumption https: //www. ncbi. nlm. nih. gov/pubmed/23713785

3 -The right drug to prevent emergence of resistance (target pathogen and commensal microbiota)

Broad vs narrow spectrum antibiotherapy for empirical antibiotherapy in newborn • Comparison in two units of narrow (Penicillin G and tobramycin) vs. broad (amoxicillin with cefotaxime) for an empiric therapy of septicaemia, • After 6 months of the study the units exchanged regimens. • Rectal and respiratory cultures were taken on a weekly basis.
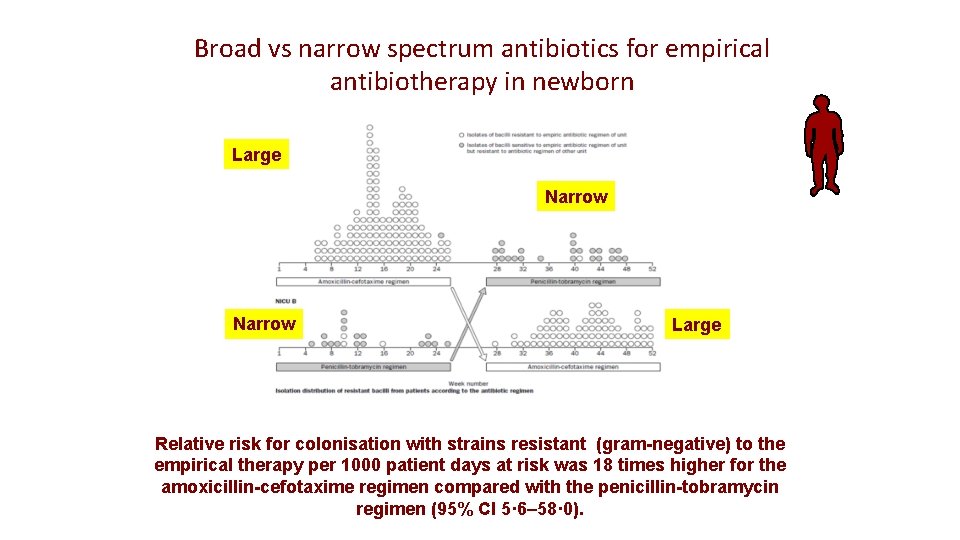
Broad vs narrow spectrum antibiotics for empirical antibiotherapy in newborn Large Narrow Large Relative risk for colonisation with strains resistant (gram-negative) to the empirical therapy per 1000 patient days at risk was 18 times higher for the amoxicillin-cefotaxime regimen compared with the penicillin-tobramycin regimen (95% CI 5· 6– 58· 0).

4 -The right dose to prevent resistance 52

Mutant Prevention Concentration (MPC) and the Selection Window (SW) hypothesis 53
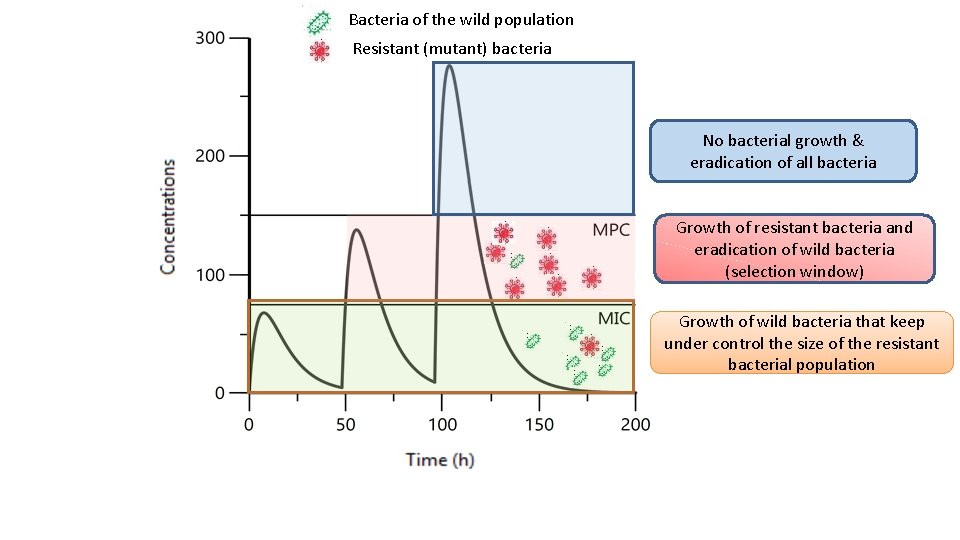
Bacteria of the wild population Resistant (mutant) bacteria No bacterial growth & eradication of all bacteria Growth of resistant bacteria and eradication of wild bacteria (selection window) Growth of wild bacteria that keep under control the size of the resistant bacterial population
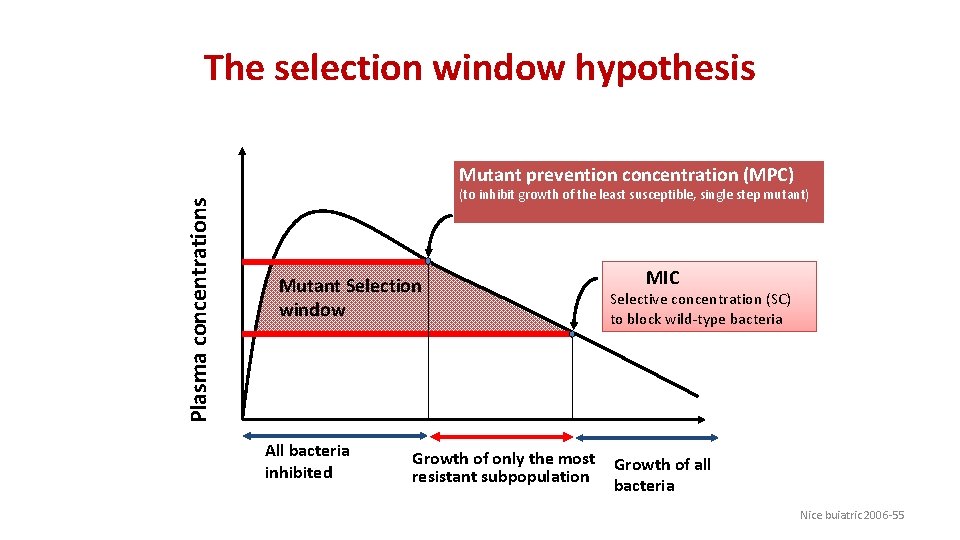
The selection window hypothesis Plasma concentrations Mutant prevention concentration (MPC) (to inhibit growth of the least susceptible, single step mutant) Mutant Selection window All bacteria inhibited Growth of only the most resistant subpopulation MIC Selective concentration (SC) to block wild-type bacteria Growth of all bacteria Nice buiatric 2006 -55
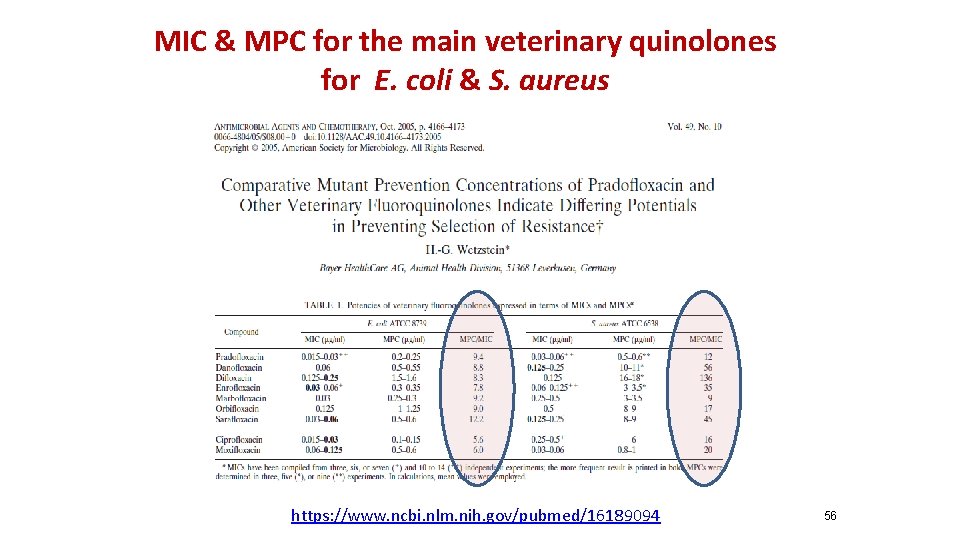

MIC & MPC for the main veterinary quinolones for E. coli & S. aureus https: //www. ncbi. nlm. nih. gov/pubmed/16189094 56
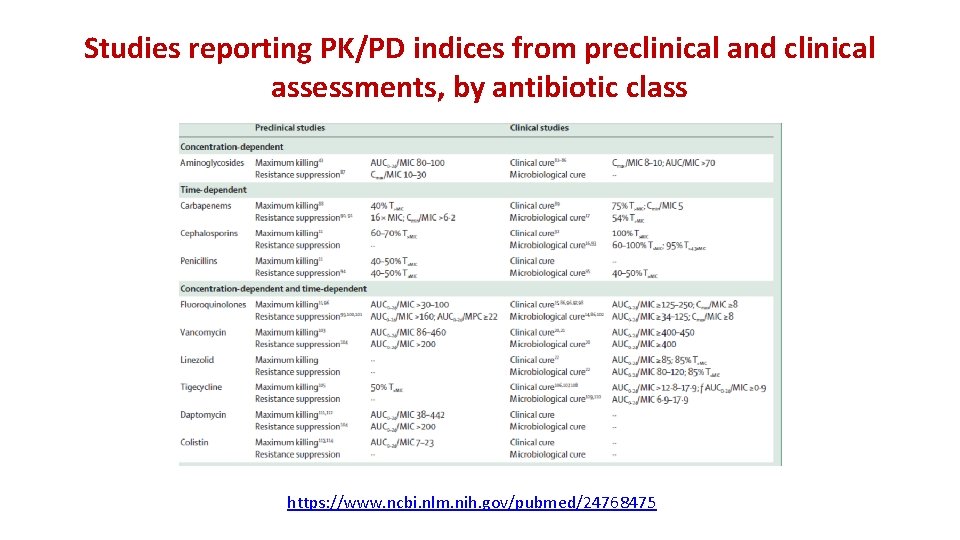
Studies reporting PK/PD indices from preclinical and clinical assessments, by antibiotic class https: //www. ncbi. nlm. nih. gov/pubmed/24768475

5 -The right duration of treatment 58
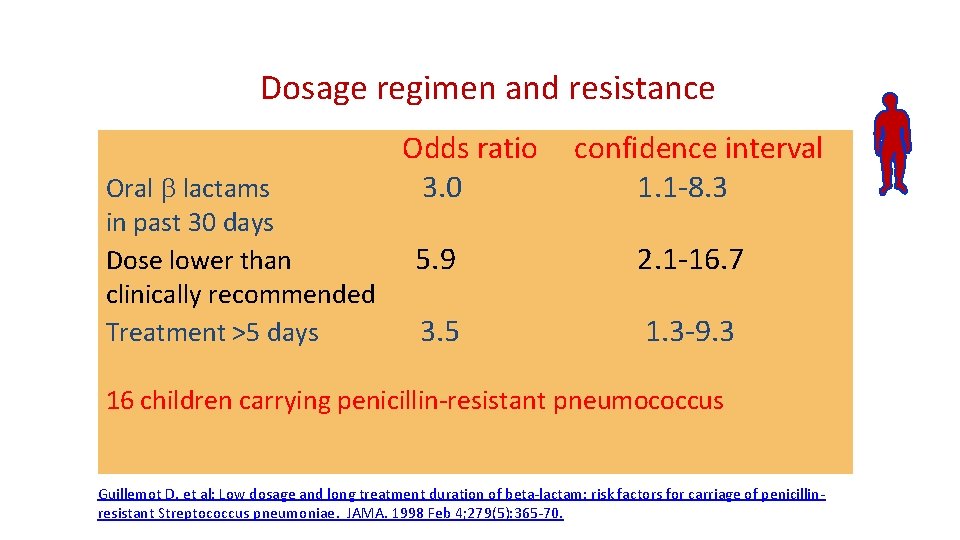

Dosage regimen and resistance Oral b lactams in past 30 days Dose lower than clinically recommended Treatment >5 days Odds ratio 3. 0 confidence interval 1. 1 -8. 3 5. 9 2. 1 -16. 7 3. 5 1. 3 -9. 3 16 children carrying penicillin-resistant pneumococcus Guillemot D, et al: Low dosage and long treatment duration of beta-lactam: risk factors for carriage of penicillinresistant Streptococcus pneumoniae. JAMA. 1998 Feb 4; 279(5): 365 -70.

6 -Increasing exposure to trough combination therapy 60

https: //www. ncbi. nlm. nih. gov/pubmed/21900036 https: //www. ncbi. nlm. nih. gov/pubmed/25746894 We have now more advanced knowledge on combinations thanks to TB and AIDS combination treatment A strain with resistance to one drug often exhibited altered resistance or susceptibility to other drugs, phenomena known as cross-resistance or hyper-susceptibility 61

Conclusion (1) 1. The optimization of dosing regimens should be accomplished by choosing the dose and schedule whose results will achieve the microbiological and clinical outcome desired while simultaneously suppressing emergence of resistance on both the target and commensal flora. 2. Early treatment and short duration are currently the two best options 62

Conclusions (2) 3. To combat resistance and the public health impact, the best strategy is likely to be to develop new antibiotics that are selective for the target pathogens with no impact on the gut microbiota (green antibiotics). 4. While waiting for this new generation of veterinary antibiotics, we have to revisit the current dosage regimens of antibiotics (dose, dosing interval and treatment duration) 63
- Slides: 63