OpioidDependence and Intravenous Drug Abuse Tom Heaps Consultant

Opioid-Dependence and Intravenous Drug Abuse Tom Heaps Consultant Acute Physician

Clinical Case 1 • 23 -year-old female • Heroin addiction for 2 years • Presents to ED with: – Rigors – Fever 39. 2 C – Headache – Abdominal pain • Started on IV Tazocin® and referred to AMU

Investigations? • • • MSU CXR Blood cultures Wound swabs Sputum culture Stool culture • HIV and Hepatitis Serology
Differentials? Skin & Bone Infections • Cellulitis • Abscesses • Infected ulcers • Thrombophlebitis • Osteomyelitis • Septic arthritis Other Infections • Aspiration pneumonia • TB • Dental abscess • STIs Blood-Borne Infections • HIV • Hepatitis B and C • Bacteraemia • Infective Endocarditis • Tetanus • Anthrax • Septic thrombosis / emboli • False / mycotic aneurysms Common Infections

Clinical Case 1 cont. • Onset of symptoms 5 minutes after last injecting • Draws up heroin through cotton wool ‘filter’ • 8 h after admission – apyrexial – asymptomatic – wants to be discharged Diagnosis?
‘Cotton Fever’ • Use of cotton-wool as a ‘filter’ to draw up heroin • Symptom onset <20 min after injection: – – – Chills High fever Abdominal pain Headache Muscle aches • Endotoxin from Gram –ve rod E. agglomerans which colonizes cotton plants • Raised WCC, no localizing signs of infection • Blood cultures usually negative • Complete resolution of symptoms <12 h • Symptomatic treatment

Clinical Case 2 • 40 -year-old male ‘ex-IVDU’ • Admitted to AMU at 02: 00 with pneumonia • States he normally takes methadone 50 mg OD • Wants this prescribing…. . NOW! • No signs of opioid withdrawal

How should you proceed? • Ask who normally provides their OST (Opiate Substitution Therapy) • Contact Dispensing Chemist / c. SMS / (GP) to confirm: – – Drug / formulation / dose / frequency Supervised (witnessed) or unsupervised? Date / time of last dispensing And suspend community dispensing whilst in hospital • Document conversation, names, contact details in notes • Continue to prescribe usual OST – 50% of dose initially if unsupervised in community – remaining 50% after 8 h if no adverse clinical signs • Involve c. SMS / h. SMP (Sam Adaway) as soon as possible

OST (Opiate Substitution Therapy) Methadone Subutex® (Buprenorphine) • Full agonist at μ receptors • Partial agonist at μ, antagonist at κ receptors • 1 mg/m. L SF liquid • SL tablets 0. 4, 2 and 8 mg • 30 -180 mg daily • 8 -32 mg daily • Half-life 24 -36 h • Half-life 36 -48 h —may be given alt. daily • ‘clouding’ effect preferred by some • ‘clear head’ effect • Risk of overdose / heroin use ‘on-top’ • Less risk of OD and safer if risk of heroin use ‘on-top’ • Drug interactions (CYP 450) • Easier to withdraw from quickly • QTc prolongation • May cause precipitated withdrawal • More suitable for heavy heroin users • Risk of diversion to IV (use Suboxone®) • Cheaper • 5 x more expensive than methadone

How should you proceed if unable to confirm OST or not normally on OST? • Take history of drug use • Confirm recent use with urinary drug screen if available • Opiate withdrawal is distressing/unpleasant but is not a lifethreatening emergency (exception = pregnancy) • Wait up to 24 h and assess for symptoms of withdrawal – within 4 -6 h of last heroin use – >24 h after last methadone use • Use COWS

Symptoms of Opiate Withdrawal • Nausea & vomiting • Lacrimation • Stomach cramps / diarrhoea • Rhinorrhoea (runny nose) • Anxiety / irritability • Sneezing / yawning • Restlessness / insomnia • Sweating / flushing • Muscular and joint pain • Piloerection (‘goose bumps’) • Tremor • Dilated pupils
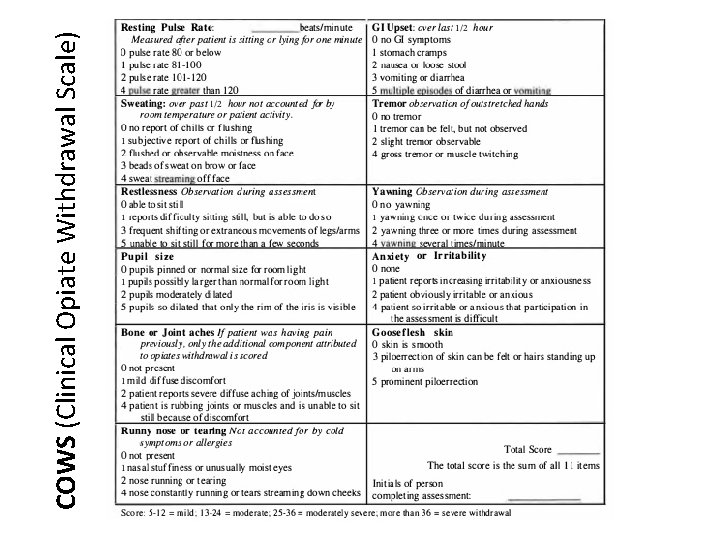
COWS (Clinical Opiate Withdrawal Scale)

COWS <5 → Symptomatic Relief Stomach cramps: mebeverine / buscopan Diarrhoea: loperamide Headache / muscle pains: paracetamol / NSAIDs Nausea / vomiting: metoclopramide / prochlorperazine Agitation / insomnia: diazepam / zopiclone

COWS ≥ 5 → start OST Day 1: • Methadone 10 -20 mg depending on COWS • Reassess after 4 -6 h and give ONE further dose of methadone according to repeat COWS Day 2 onwards: • • • give total dose of methadone administered on day 1 as a single dose Involve h. SMP / c. SMS as soon as possible Titrate dose by 5 -10 mg daily depending on response DO NOT exceed 50 mg / day without expert advice Observe for signs of cumulative toxicity (steady state ~5 d)

Discharge • Liaise with h. SMP / c. SMS 24 h prior to discharge • Contact Dispensing Chemist to reinstate script / dispensing (if taking OST prior to admission) • DO NOT prescribe methadone / buprenorphine or symptomatic relief on TTO – unless specifically advised to do so by h. SMP / c. SMS

Clinical Case 3 • 36 -year-old female ‘ex-IVDU’ • Confirmed OST (methadone 30 mg) • Admitted to AMU with seizure and fractured olecranon • Reports significant elbow pain despite regular paracetamol

How should you proceed? A. Limit analgesia to non-opioids (paracetamol, NSAIDs) due to risk of ‘relapse’ with opioids? B. Do nothing because she is already taking methadone and is probably ‘drug seeking’? C. Prescribe opioid analgesia (titrated to pain) if nonopioid analgesia fails to control pain? D. Increase her dose of methadone to provide additional analgesia?

Pain & Opioid-Dependence → Common Misconceptions 1. OST provides analgesia – – – duration of analgesic action usually 4 -8 h tolerance opioid-induced hyperalgesia (NMDAR agonism) 2. Use of opiate analgesia risks addiction relapse – inadequate pain control more likely to trigger relapse 3. Opiate analgesia with OST causes respiratory / CNS depression – tolerance to CNS and respiratory depression 4. Reports of pain are usually manipulative ‘drug-seeking’ behaviour

Analgesia in patients on methadone • Use non-opioid analgesia (e. g. paracetamol, NSAIDs) first • If pain not controlled prescribe opiate analgesia and titrate to pain • More frequent and higher doses of opiate analgesia are often required (cross -tolerance) • Consider dividing total daily dose of methadone into 6 -8 h (TDS-QDS) dosing • DO NOT increase methadone dose to provide analagesia

Analgesia in patients on buprenorphine • Use non-opioid analgesia (e. g. paracetamol, NSAIDs) first • Opiate analgesia likely to be ineffective – partial agonist with high affinity for μ receptors – Tramadol may have some analgesic effect – consider increasing total daily buprenorphine dose and/or dividing dose into 6 -8 h dosing – convert to short-acting opiates or to methadone plus opiate analgesia for duration of hospital admission – expert advice • Seek advice from Acute Pain Team

Key Learning Points 1. Wide differential for fever in IVDUs – Screen for blood-borne viruses; blood cultures are mandatory 2. Opioid withdrawal is rarely life-threatening – Take time to confirm OST prescription or assess for signs of withdrawal 3. Risks of initiating OST must be balanced against risks of self-discharge 4. Liaise with Dispensing Chemist, h. SMP, c. SMS, ward pharmacist 5. Opioid analgesia should not be withheld from patients with opiate-dependence – Higher / more frequent doses often required
- Slides: 21