Ophthalmologic and ENT Emergencies OUWB School Of Medicine

Ophthalmologic and ENT Emergencies OUWB School Of Medicine Beaumont Health System Department of Emergency Medicine

Ophthalmologic emergencies • Sudden loss of vision – Central retinal artery occlusion – Central retinal vein occlusion – Retrobulbar neuritis – Amaurosis fugax – Retinal detachment – Acute iritis

Central retinal artery occlusion • Sudden monocular painless, complete loss of vision • Embolic event to the Central Retinal Artery • Fundoscopic exam: pale retina with macular red spot – Macula has blood supply from choroid, supplied by post ciliary arteries • Treatment – stat opthy consult – Intermittent digital massage of the globe – Increase CO 2 (arteriolar dilatation) – carbonic anhydrase inhibitor (ie acetazolamide) – Definitive tx – paracentesis of the anterior chamber
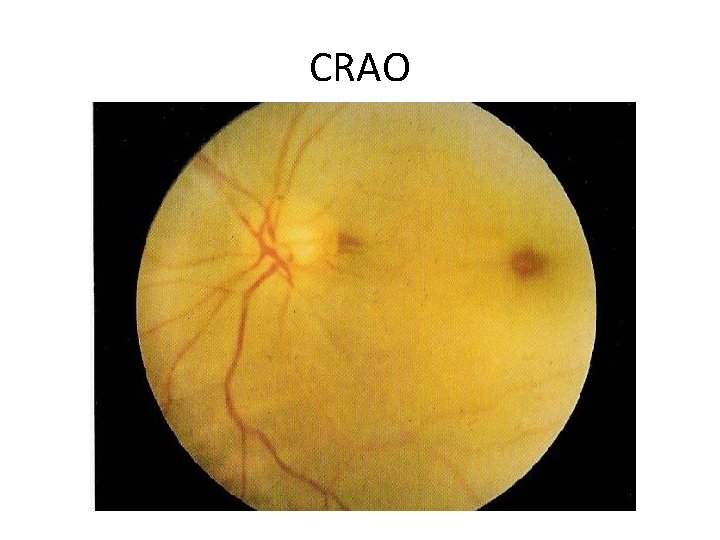
CRAO
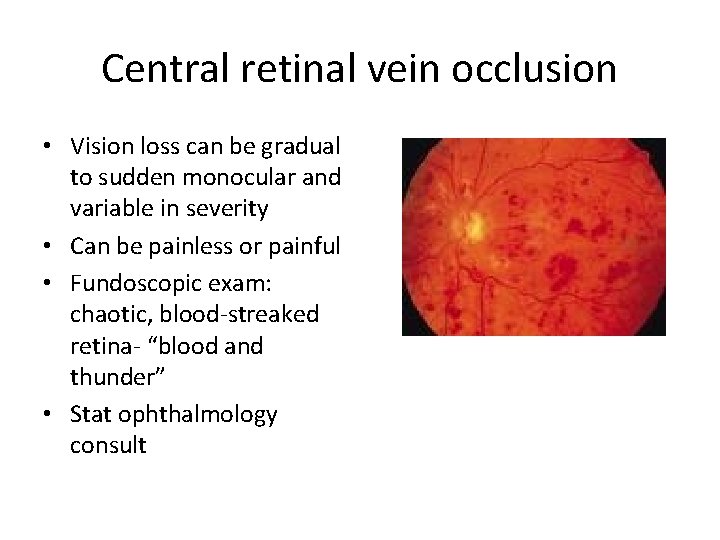
Central retinal vein occlusion • Vision loss can be gradual to sudden monocular and variable in severity • Can be painless or painful • Fundoscopic exam: chaotic, blood-streaked retina- “blood and thunder” • Stat ophthalmology consult
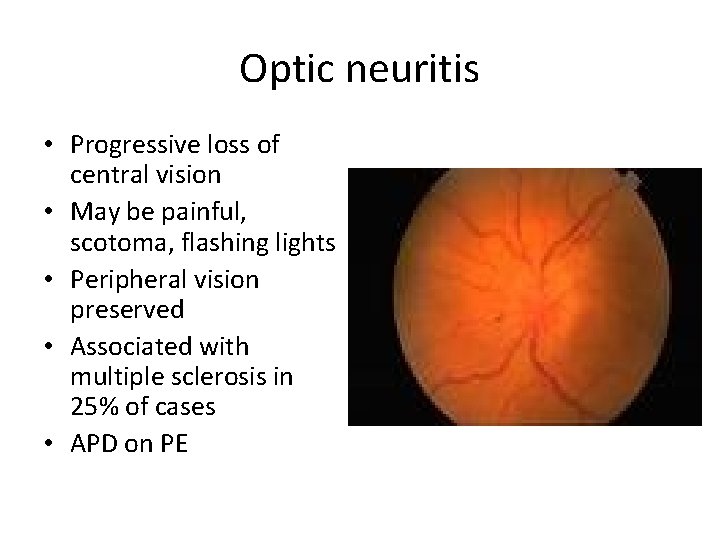
Optic neuritis • Progressive loss of central vision • May be painful, scotoma, flashing lights • Peripheral vision preserved • Associated with multiple sclerosis in 25% of cases • APD on PE

Amaurosis fugax • Fleeting painless loss of monocular vision • “a shade came down over my eye” • Due to minute emboli of the central retinal artery • Consult neurology for TIA
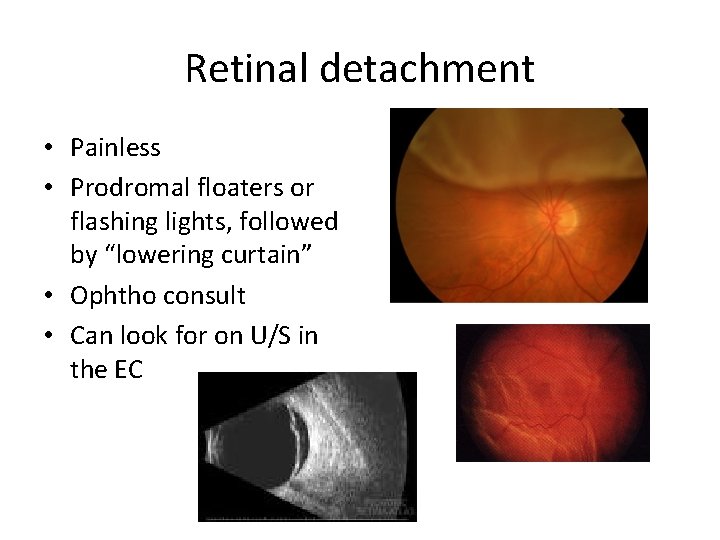
Retinal detachment • Painless • Prodromal floaters or flashing lights, followed by “lowering curtain” • Ophtho consult • Can look for on U/S in the EC

Red eye • • Acute angle closure glaucoma Acute iritis Conjunctivitis Herpes simplex keratitis Corneal ulceration Chemical conjunctivitis Corneal abrasions Subconjunctival hemorrhage

Acute angle closure glaucoma • Sudden severe unilateral ocular pain and decreased visual acuity • Patients may present with headache or nausea, blurred vision or rainbow halos • Precipitous increase in IOP leads to blindness within a few days if left untreated • In patients predisposed (ie far sighted, cataracts), pupil dilatation is often precipitant event (sympathomimetics, parasympatholytics, stress, fatigue, darkness) – Closes off aqueous outflow tract • Classic case is eye pain starting at the movie theater
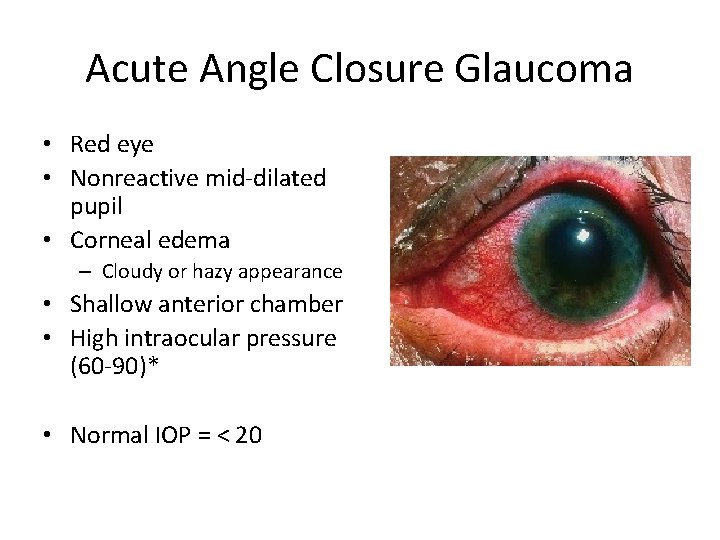
Acute Angle Closure Glaucoma • Red eye • Nonreactive mid-dilated pupil • Corneal edema – Cloudy or hazy appearance • Shallow anterior chamber • High intraocular pressure (60 -90)* • Normal IOP = < 20

Acute Angle Closure Glaucoma • Stat ophtho consult for definitive tx – iridotomy • Timolol gtt– beta blocker • Acetazolamide (diamox) – IV and po – carbonic anhydrase inhibitor • Pilocarpine gtt – parasympathomimetic – Usually starts 1 hr after initiation of initial tx • Mannitol • 50% glycerol – oral hyperosmotic – if patient can tolerate po – give in place of mannitol – Avoid in diabetics

Timolol • Timoptic solution – beta blocker • Decreases aqueous humor formation • 0. 5% solution – 1 -2 drops at 10 -15 min intervals x 3, then 1 drop every 12 hours

Acetazolamide Diamox Carbonic anhydrase inhibitor Inhibits aqueous humor formation Cross reactive allergen with sulfa 500 mg IV every 12 hours or 500 mg po every 6 hours • Side effects: respiratory depression, metabolic acidosis • • •

Pilocarpine • Parasympathomimetic • Produces miosis • 2% solution – 1 drop every 30 minutes until the pupil constricts, then 1 drop every 6 hours • Side effects: bradycardia, hypotension, sweating, tremors

Mannitol • 20% 1 -2 grams/kg IV over 30 -60 minutes • Increases blood osmolality, creating a gradient that draws water from the vitreous cavity • Side effects: headache, confusion, CHF, dehydration

Acute iritis • Blurred vision, photophobia, ocular pain • Pain on direct and consensual pupillary response • Exam: ciliary flush, anterior chamber cells and flare, constricted pupil, decreased visual acuity, lower IOP • Treatment: – Cycloplegics – ie Homatropine – dilates the eyes – Topical steroids – Close ophtho follow up
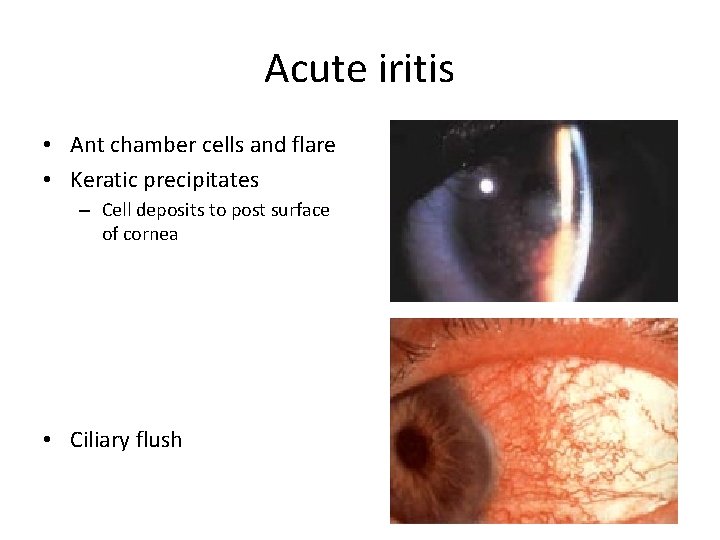
Acute iritis • Ant chamber cells and flare • Keratic precipitates – Cell deposits to post surface of cornea • Ciliary flush
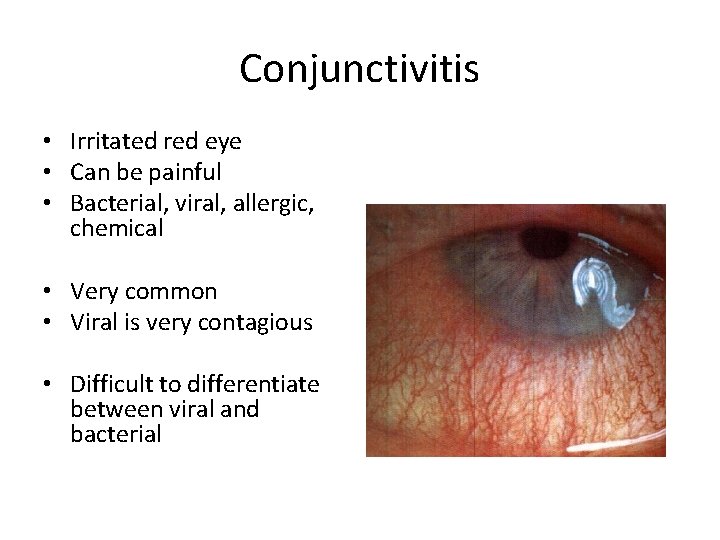
Conjunctivitis • Irritated red eye • Can be painful • Bacterial, viral, allergic, chemical • Very common • Viral is very contagious • Difficult to differentiate between viral and bacterial
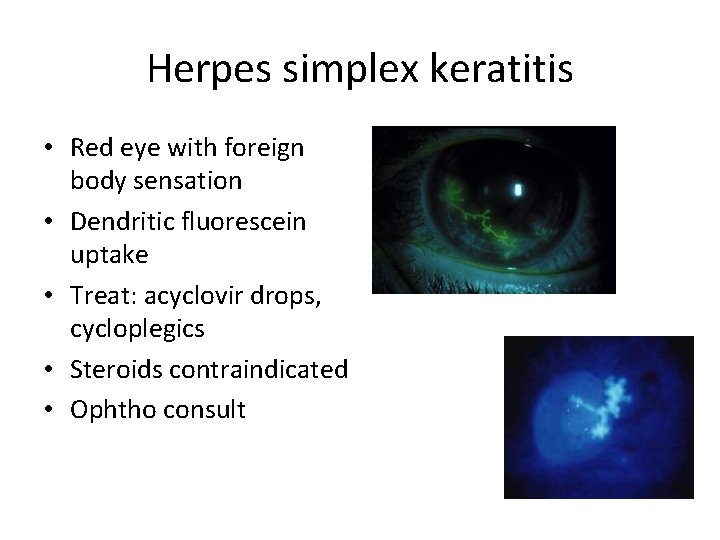
Herpes simplex keratitis • Red eye with foreign body sensation • Dendritic fluorescein uptake • Treat: acyclovir drops, cycloplegics • Steroids contraindicated • Ophtho consult
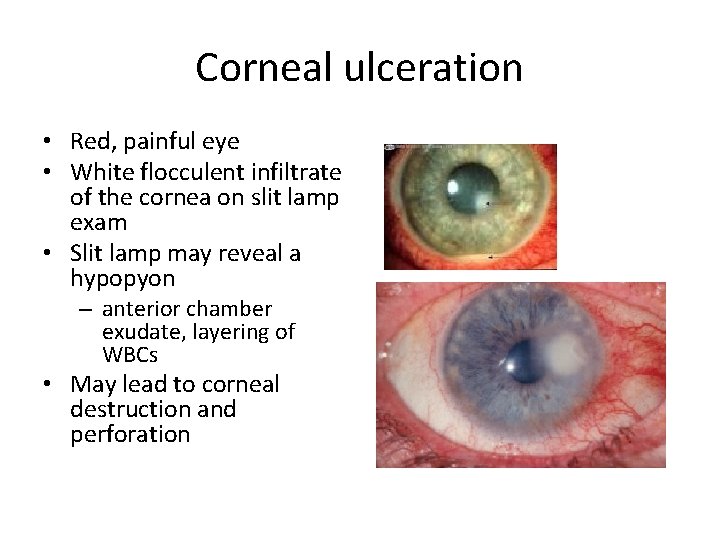
Corneal ulceration • Red, painful eye • White flocculent infiltrate of the cornea on slit lamp exam • Slit lamp may reveal a hypopyon – anterior chamber exudate, layering of WBCs • May lead to corneal destruction and perforation

Corneal ulceration • Tx: – Ophtho consult – Abx gtts usually q 1 -2 hrs initially, possible systemic Abx depending on potential pathogen • Ex: pseudomonas in contact lens wearers – Small ulcers may d/c home with close f/u – large ulcers, potential noncompliance, admit

Chemical conjunctivitis • Alkali burn – absolute ocular emergency – Liquefactive necrosis – worse – Immediate irrigation to continue until p. H returns to 7. 0 – 7. 5 and ophtho consult – Only ophtho emergency in which visual acuity is not indicated until after therapy has begun • i. e. Irrigate first! • Acid burns – Coagulative necrosis – Immediate irrigation as above and ophtho consult
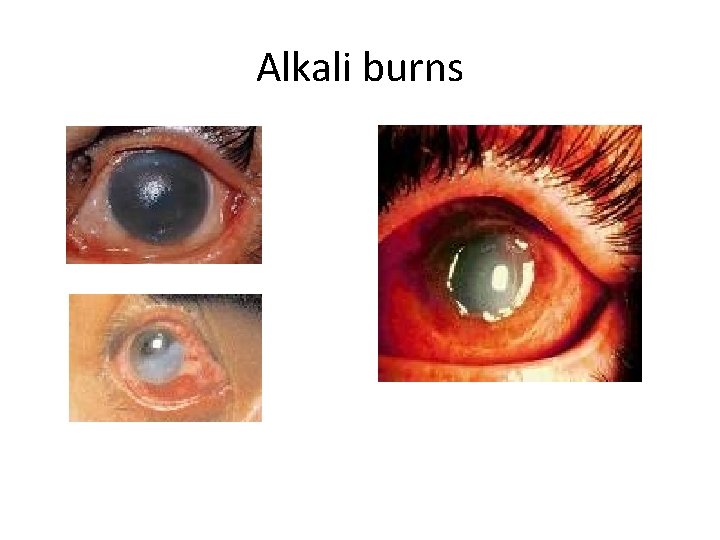
Alkali burns

Corneal abrasions • Foreign body sensation and photophobia • Diagnose: fluorescein uptake with slit lamp exam, rule out foreign body with upper lid eversion • Suspect foreign body if “ice rink sign” – fine linear abrasions in upper 1/3 cornea • Rule out corneal ulceration • Do not use steroid drops – it may be difficult to rule out early herpetic keratitis • Treat: antibiotic ointment/drops, analgesics • Prognosis is very good
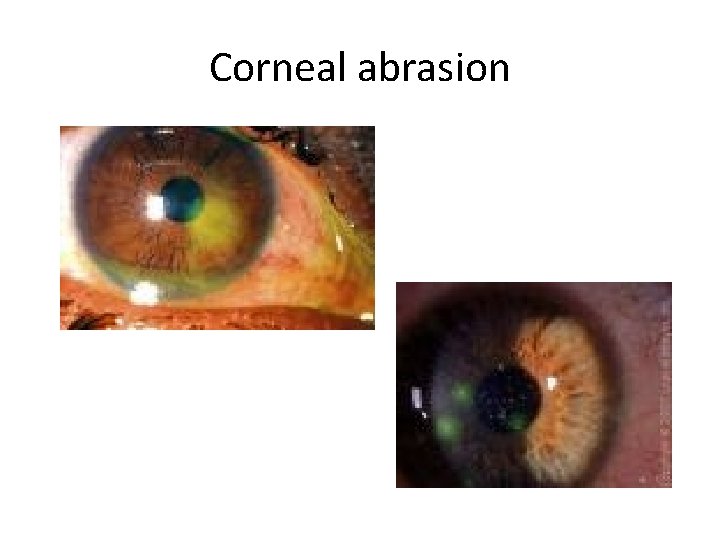
Corneal abrasion
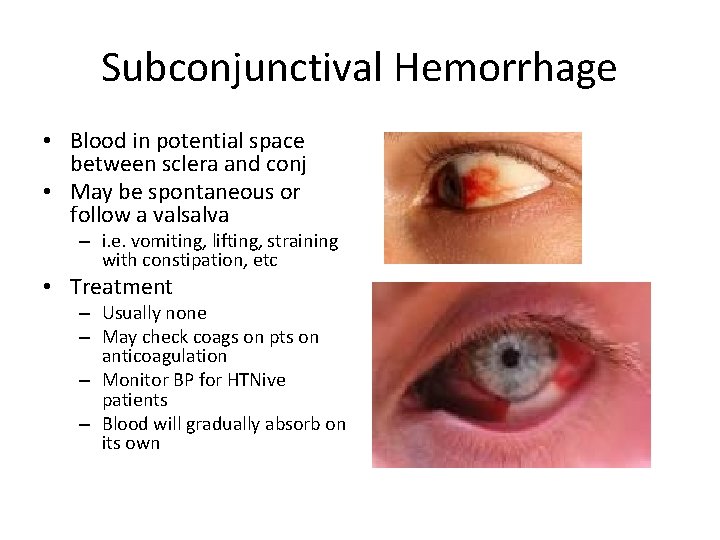
Subconjunctival Hemorrhage • Blood in potential space between sclera and conj • May be spontaneous or follow a valsalva – i. e. vomiting, lifting, straining with constipation, etc • Treatment – Usually none – May check coags on pts on anticoagulation – Monitor BP for HTNive patients – Blood will gradually absorb on its own

Traumatic eye injuries • • Corneal laceration Perforated globe Intraocular foreign body Hyphema Blow-out orbital fracture Traumatic lens dislocation Traumatic mydriasis Traumatic iritis or retinal detachment

Corneal laceration • Tear shaped pupil – from prolapse of the iris • Small black fragments representing iris pigment may be seen and initially mistaken for a foreign body • May not see the laceration itself • Treat: metal shield, stat ophtho consult for surgical repair
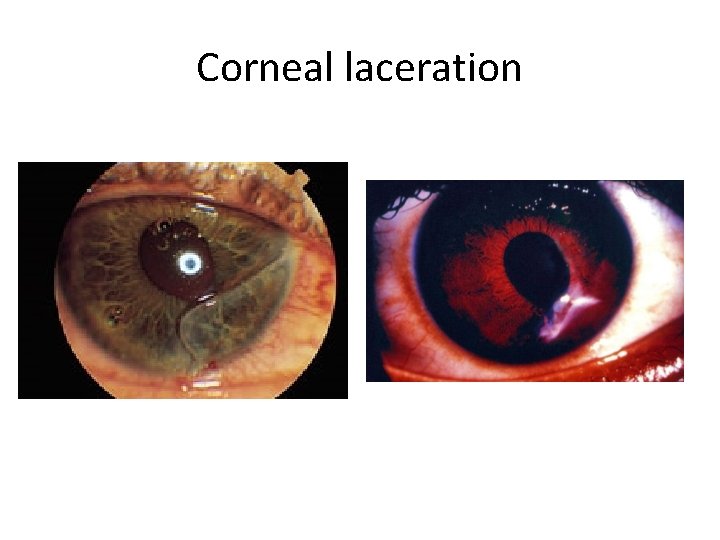
Corneal laceration

Perforated globe • Suspect if penetrating wound to the eyelid • Decreased visual acuity, soft globe (do not palpate however) • Fundoscopic exam may reveal vitreous hemorrhage • Treatment: – Metal shield – stat ophtho consult for surgical repair

Intraocular foreign body • Patient often gives a history of striking metal on metal • May be initially painless, but then patient develops monocular pain and decreased visual acuity • May not see the wound • Diagnosis: CT scan, ultrasound or plain x-ray of the globe • Stat Ophtho consult
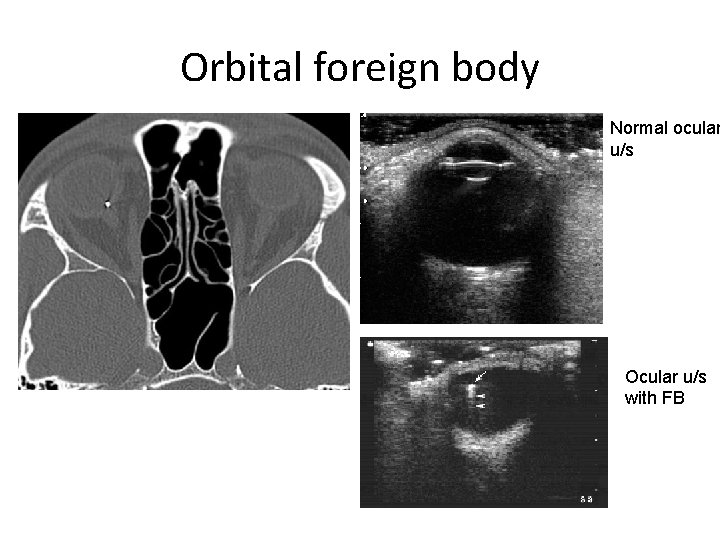
Orbital foreign body Normal ocular u/s Ocular u/s with FB
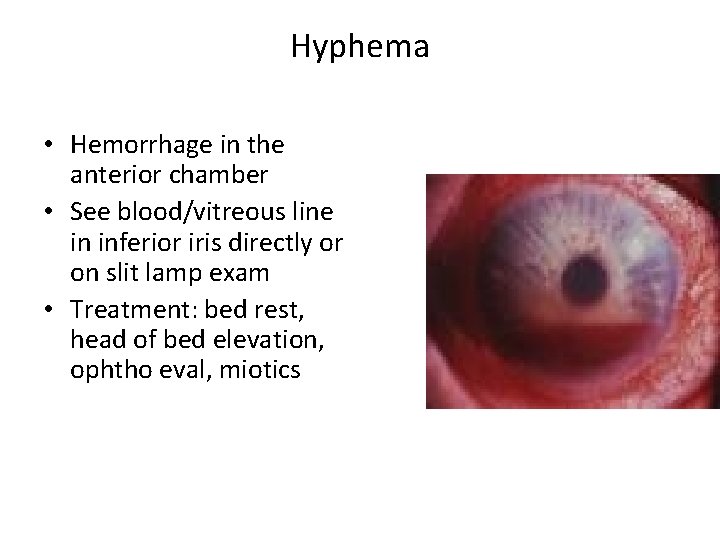
Hyphema • Hemorrhage in the anterior chamber • See blood/vitreous line in inferior iris directly or on slit lamp exam • Treatment: bed rest, head of bed elevation, ophtho eval, miotics

Orbital floor fracture • Blunt globe trauma (ie fist to eye) transmits forces that may lead to orbital floor fracture • Inferior rectus muscle may prolapse through the fracture • Signs/Sx’s: – Pain – diplopia or loss of upward gaze – enophthalmos (sunken eye) – infraorbital anesthesia (injury of infraorbital nerve) • CT orbits • Ophtho consult
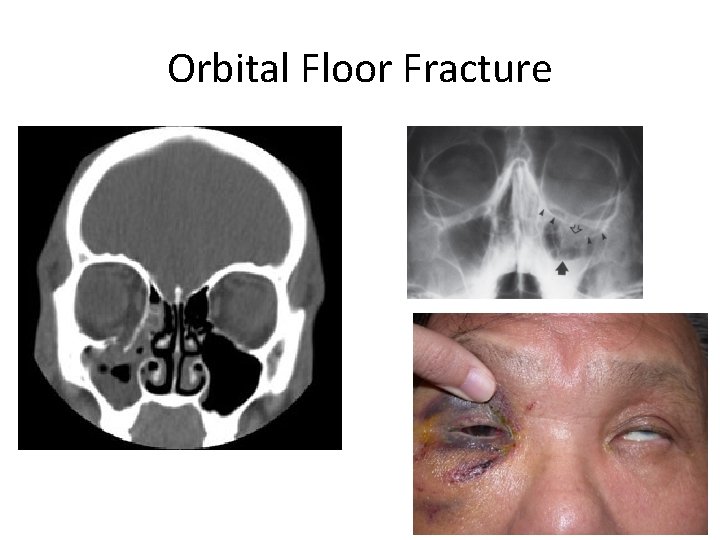
Orbital Floor Fracture
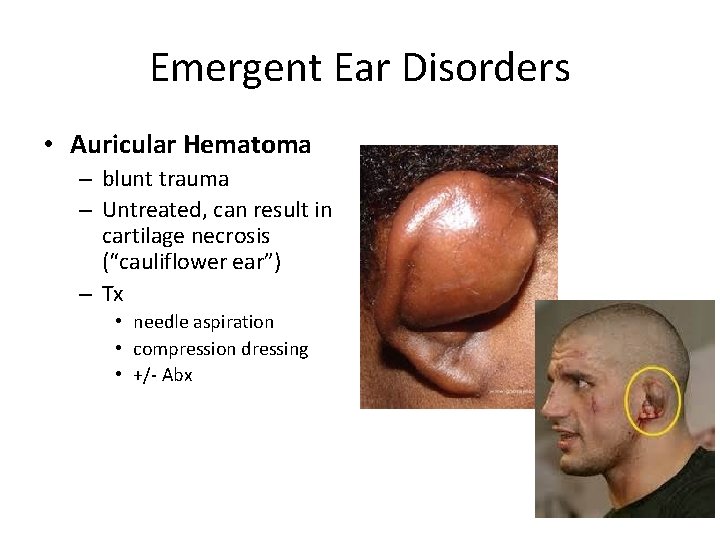
Emergent Ear Disorders • Auricular Hematoma – blunt trauma – Untreated, can result in cartilage necrosis (“cauliflower ear”) – Tx • needle aspiration • compression dressing • +/- Abx
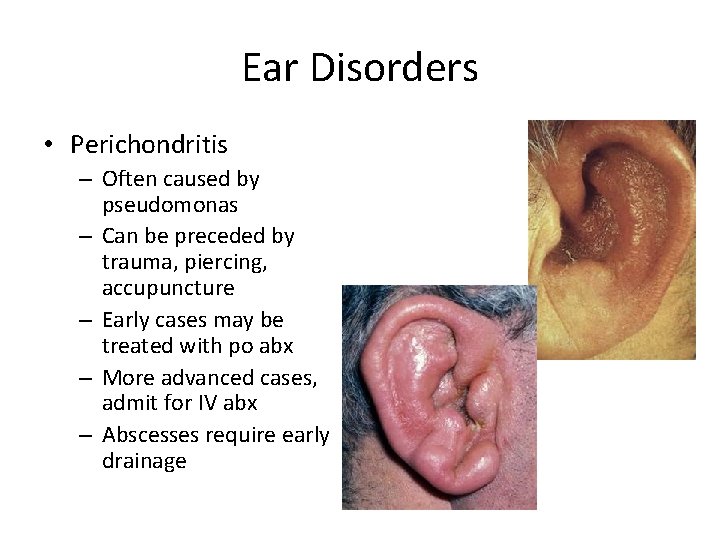
Ear Disorders • Perichondritis – Often caused by pseudomonas – Can be preceded by trauma, piercing, accupuncture – Early cases may be treated with po abx – More advanced cases, admit for IV abx – Abscesses require early drainage
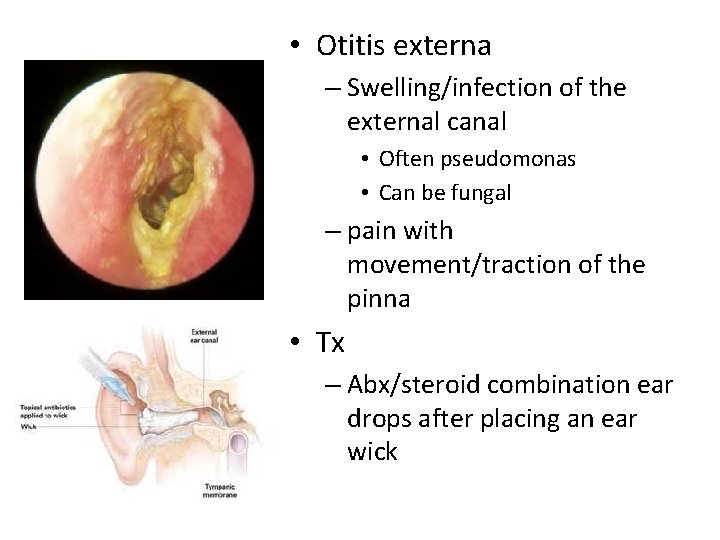
• Otitis externa – Swelling/infection of the external canal • Often pseudomonas • Can be fungal – pain with movement/traction of the pinna • Tx – Abx/steroid combination ear drops after placing an ear wick

Ear Disorders Malignant (Necrotizing) Otitis Externa • Invasive infection of the external auditory canal • immunocompromised pts, diabetics • Pseudomonas aeruginosa is typical organism (~95%) • Infection progresses from the EAC to the skull base, TMJ • Facial nerve paralysis multiple CN involvement meningitis

Malignant Otitis Externa • Signs/Sx’s – Toxic appearing – Deep pain with movement of TMJ, pinna – Swollen, erythematous EAC, may have drainage – granulation tissue on the floor of the auditory canal at bony-cartilage junction • Tx: – stat ENT consult for surgical debridement and IV antibiotics (anti-pseudomonal) – CT scan
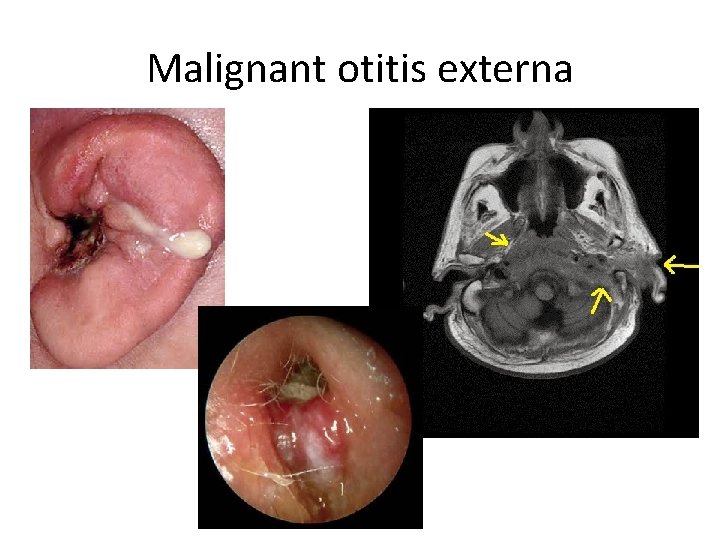
Malignant otitis externa
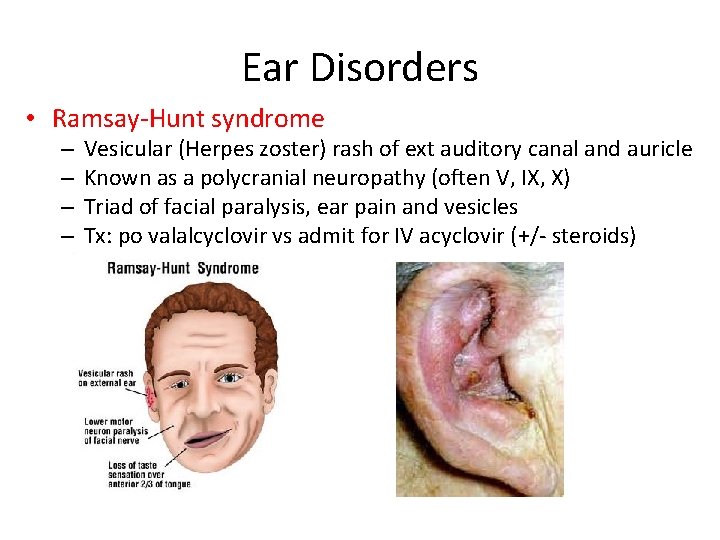
Ear Disorders • Ramsay-Hunt syndrome – – Vesicular (Herpes zoster) rash of ext auditory canal and auricle Known as a polycranial neuropathy (often V, IX, X) Triad of facial paralysis, ear pain and vesicles Tx: po valalcyclovir vs admit for IV acyclovir (+/- steroids)

Ear Disorders • Foreign body – Tools for removal • irrigation (not vegetable matter) • alligator forceps, suction, hook, cerumen loop – Live insects should be stupefied with lidocaine or mineral oil prior to removal • Tympanic membrane rupture – Most often due to otitis media, can be due to trauma – ENT referral – Avoidance of ototoxic gtts • Otitis media – hopefully you all know what this is

Nose • Epistaxis – – Anterior most common – Kiesselbach’s plexus Posterior often due to uncontrolled HTN Rule out coagulopathy Tx: • Silver nitrate or cautery • Packing • If posterior: ENT consult/admission – Oral antibiotics if nasal pack • Foreign bodies – suction, ear curette, forceps • Acute sinusitis – 1 st line tx is simply decongestants! (po and nasal spray) – Difficult to distinguish viral from bacterial on sx’s alone – Antibiotics (augmentin, macrolide, 2 nd or 3 rd cephalosporin) only for prolonged sx’s (greater than 10 days), assoc facial cellulitis, high fever
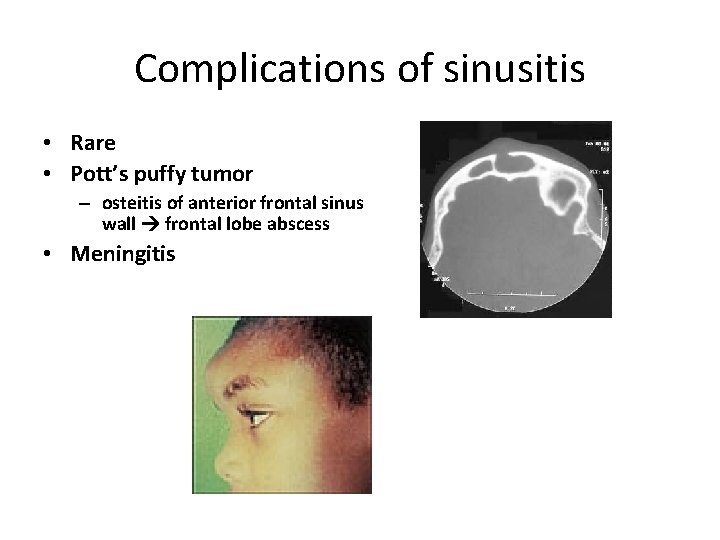
Complications of sinusitis • Rare • Pott’s puffy tumor – osteitis of anterior frontal sinus wall frontal lobe abscess • Meningitis
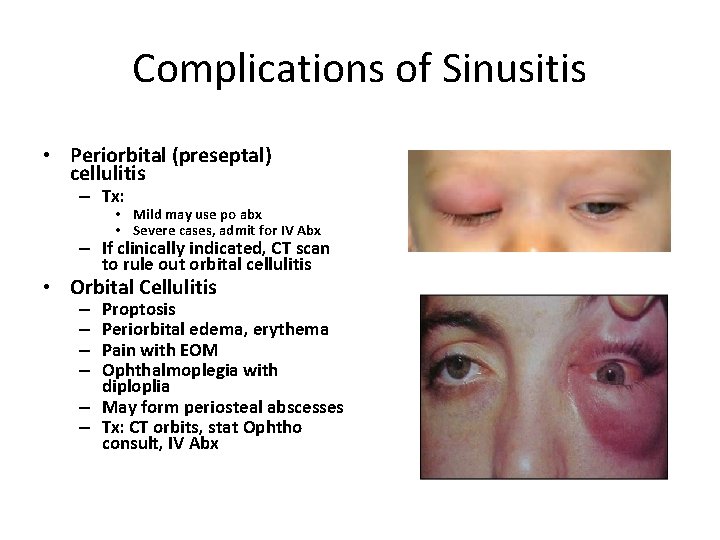
Complications of Sinusitis • Periorbital (preseptal) cellulitis – Tx: • Mild may use po abx • Severe cases, admit for IV Abx – If clinically indicated, CT scan to rule out orbital cellulitis • Orbital Cellulitis Proptosis Periorbital edema, erythema Pain with EOM Ophthalmoplegia with diploplia – May form periosteal abscesses – Tx: CT orbits, stat Ophtho consult, IV Abx – –
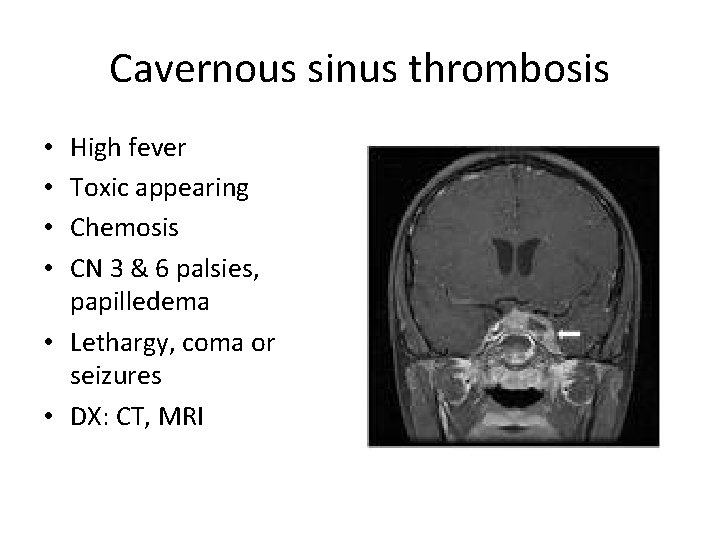
Cavernous sinus thrombosis High fever Toxic appearing Chemosis CN 3 & 6 palsies, papilledema • Lethargy, coma or seizures • DX: CT, MRI • •
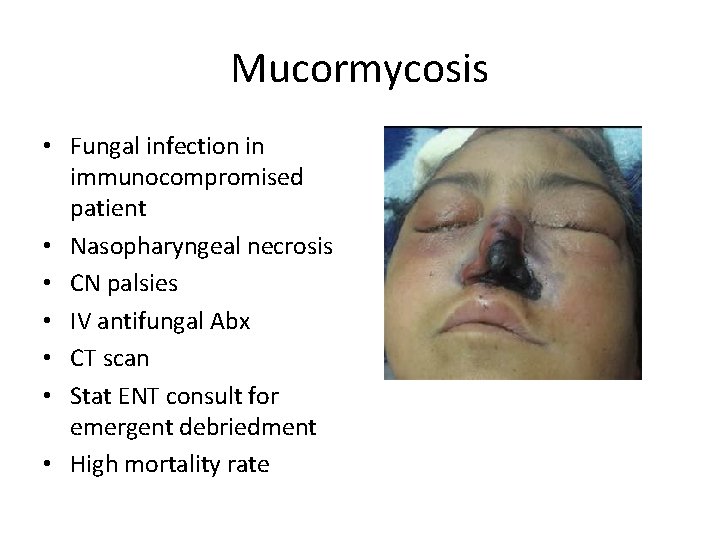
Mucormycosis • Fungal infection in immunocompromised patient • Nasopharyngeal necrosis • CN palsies • IV antifungal Abx • CT scan • Stat ENT consult for emergent debriedment • High mortality rate

Throat • Pharyngitis – Grp A strep – treat to prevent complications: acute rheumatic fever and ARHD – glomerulonephritis not prevented by Abx • Mononucleosis – EBV – Pharyngitis, fever, cervical lymphadenopathy – Splenomegaly in 50% – Dx: monospot, atypical lymphocytes – Tx: fluid, rest, steroids, avoid ampicillin (rash), contact sports/trauma (splenic rupture)

Ludwig’s angina • Cellulitis of the floor of the mouth – Sublingual/submandibular area • True emergency (airway obstruction) • Elderly, debilitated men (alcohol abuse)

Ludwig’s Angina • Dx: – CLINICAL: • • • Tx brawny edema of submandibular area, Febrile protruding elevated tongue respiratory distress – IV antibiotics (clindamycin or Unasyn or Pcn + metronidazole) – airway protection (sx and anesthesia backup) – Best to approach airway in OR if you have time – Will likely need tracheostomy
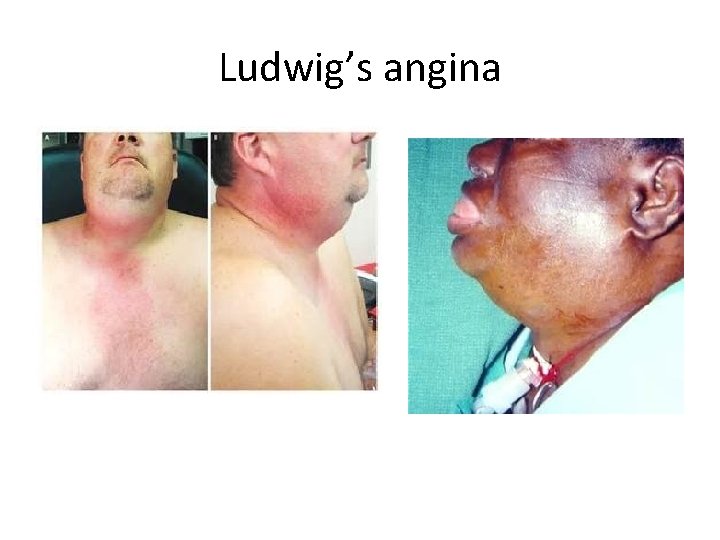
Ludwig’s angina
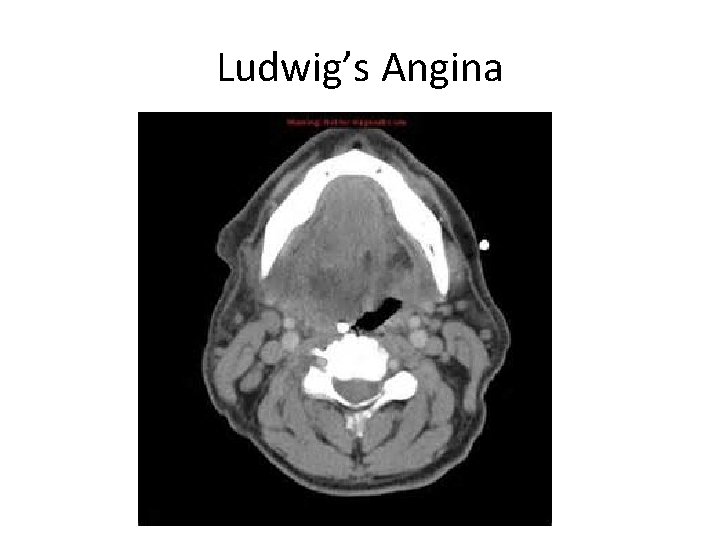
Ludwig’s Angina

Peritonsillar abscess • • • Fever, trismus, dysphagia Adolescents, young adults Enlarged inflamed tonsil extending medially Displaces uvula to opposite side Tx: – I & D: can be done in EC by trained EM physician vs by ENT – IV Abx (Pcn or Clindamycin or Unasyn with Metronidazole) – +/- steroids for edema
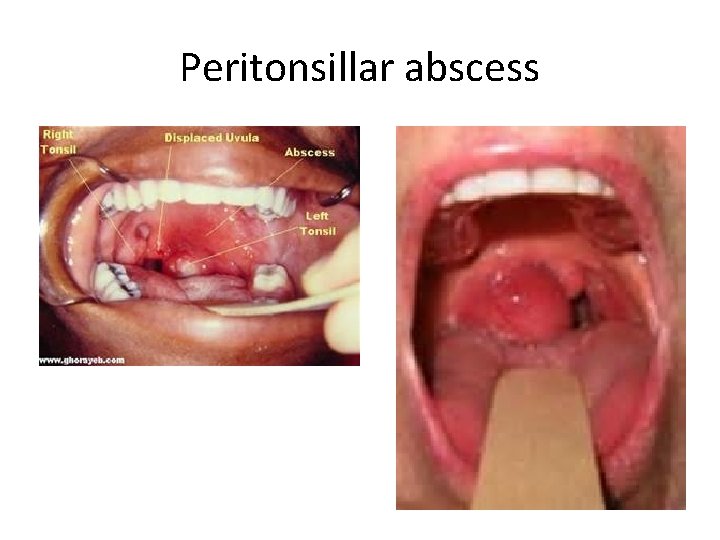
Peritonsillar abscess

Retropharyngeal abscess • Children aged 6 mos – 3 yrs though increasing in the adult population • Staph aureus, grp A strep, anaerobes • Fever, neck pain/stiffness, muffled voice, dysphagia • Child prefers to lie supine (do not force to sit up) • Diagnosis: prevertebral edema on lateral soft tissue neck X-ray • Tx: ICU admit for IV Abs and ENT surgical drainage • PCN, Clindamycin, zosyn or Unasyn with Metronidazole
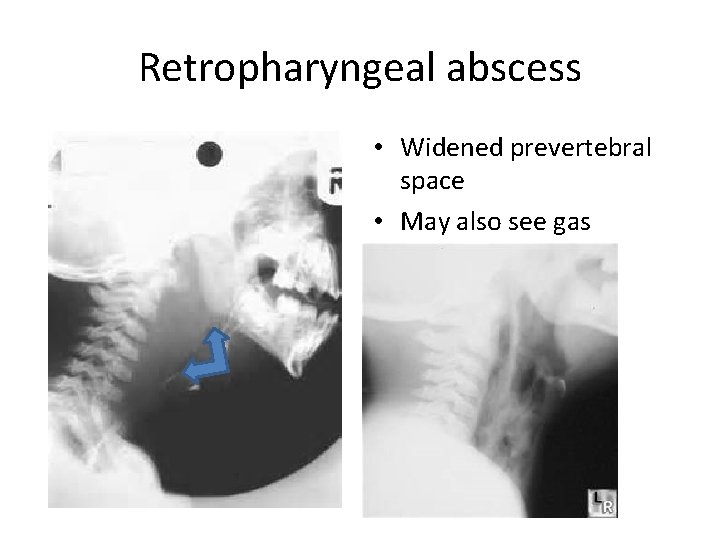
Retropharyngeal abscess • Widened prevertebral space • May also see gas

Epiglottis • Abrupt high fever, sore throat, stridor, dysphagia • Picture: child is drooling, stridorous, sitting up with chin forward and neck extended • Any age – children more worrisome • H influenza, grp A strep, B. catarrhalis – Incidence less due to immunization
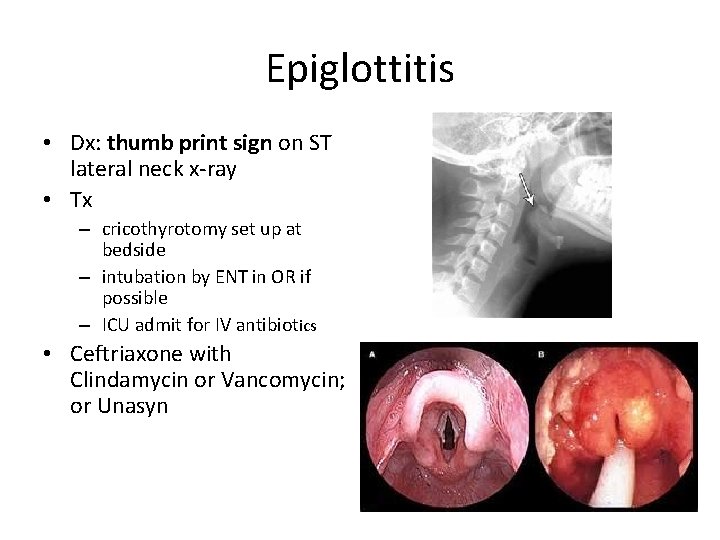
Epiglottitis • Dx: thumb print sign on ST lateral neck x-ray • Tx – cricothyrotomy set up at bedside – intubation by ENT in OR if possible – ICU admit for IV antibiotics • Ceftriaxone with Clindamycin or Vancomycin; or Unasyn

Croup • Inflammation of the larynx and subglottic airway • Parainfluenza most common (RSV, adenovirus) • 2 -3 days of URI sxs, worsening to a barking cough, hoarse voice, and stridorous • Rare after age 6
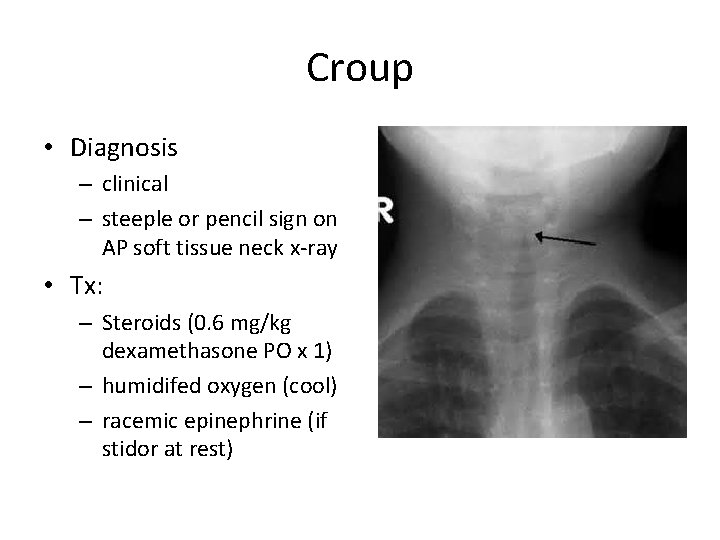
Croup • Diagnosis – clinical – steeple or pencil sign on AP soft tissue neck x-ray • Tx: – Steroids (0. 6 mg/kg dexamethasone PO x 1) – humidifed oxygen (cool) – racemic epinephrine (if stidor at rest)
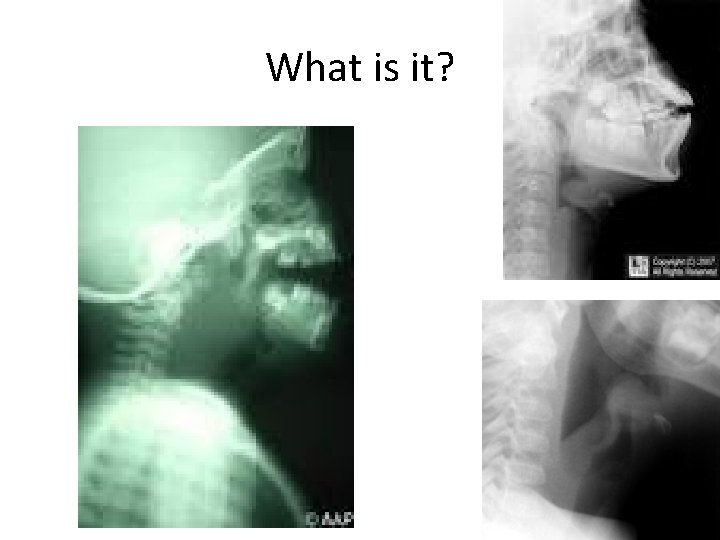
What is it?

THE END ANY QUESTIONS?
- Slides: 65