Operative Vaginal Delivery Robert D Auerbach M D

Operative Vaginal Delivery Robert D. Auerbach, M. D. FACOG Senior Vice President & Chief Medical Officer Cooper. Surgical, Inc. Associate Clinical Professor Yale University School of Medicine
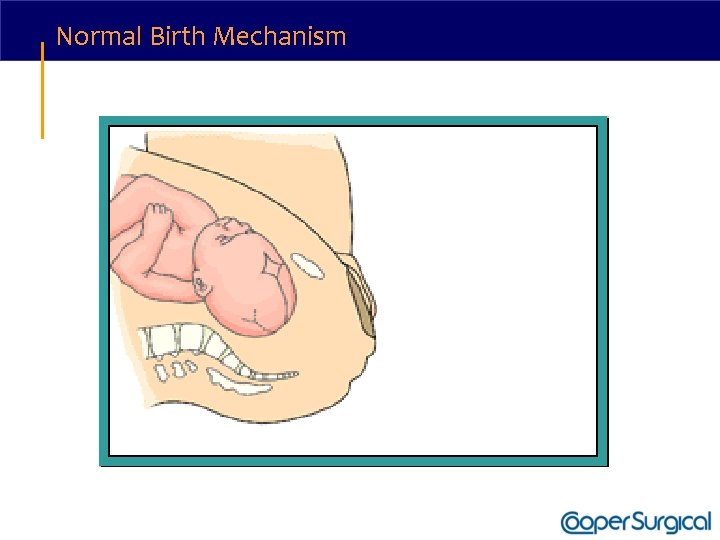
Normal Birth Mechanism

Introduction • US incidence of Operative Vaginal Delivery (OVD) – 10 -15%* • Percentage of forceps declining compared with vacuum extraction • Geographic differences § Lowest in the Northeast § Highest in the South * Bofill JA. Operative Vaginal Delivery: A survey of fellows of ACOG. OG 1996; 88: 1007

Indications for OVD No indication is absolute • Prolonged 2 nd stage • Nulliparous: lack of continuous progress § >3 hrs with regional anesthesia § >2 hrs w/o regional anesthesia • Multiparous: lack of continuous progress § >2 hrs with regional anesthesia § >1 hr w/o regional anesthesia • Fetal compromise • Maternal benefit to shortened 2 nd stage
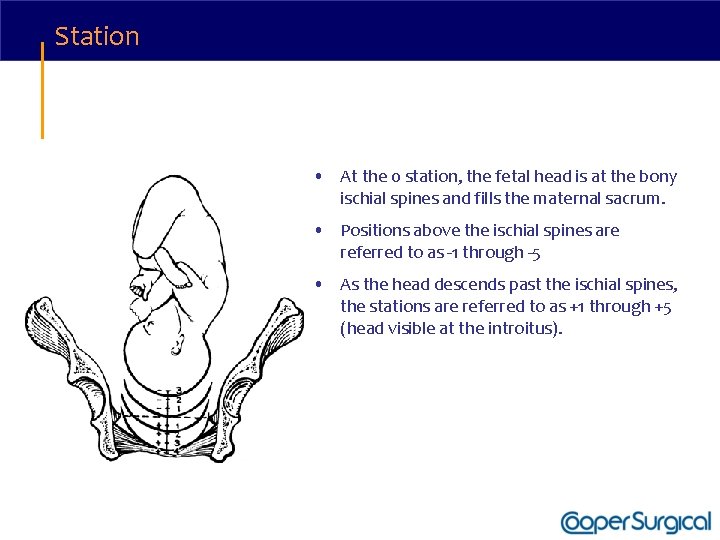
Station • At the 0 station, the fetal head is at the bony ischial spines and fills the maternal sacrum. • Positions above the ischial spines are referred to as -1 through -5 • As the head descends past the ischial spines, the stations are referred to as +1 through +5 (head visible at the introitus).
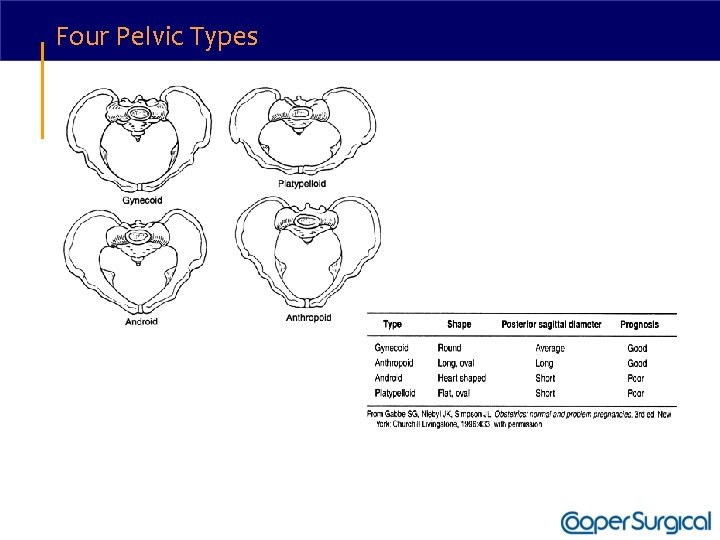
Four Pelvic Types
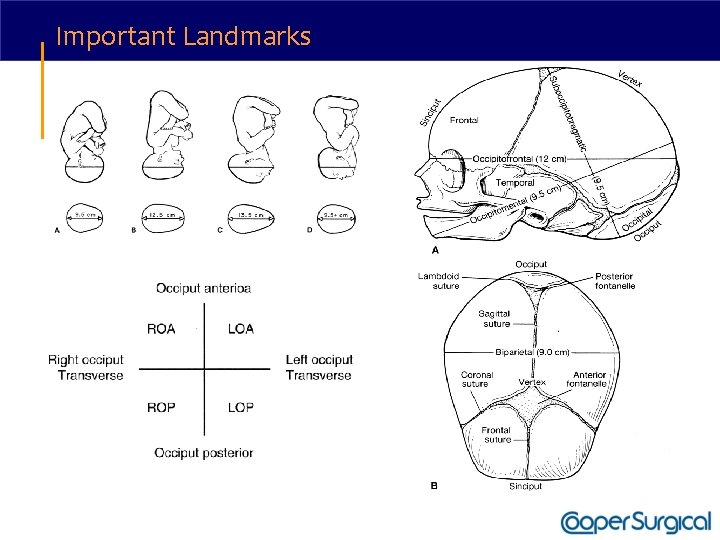
Important Landmarks
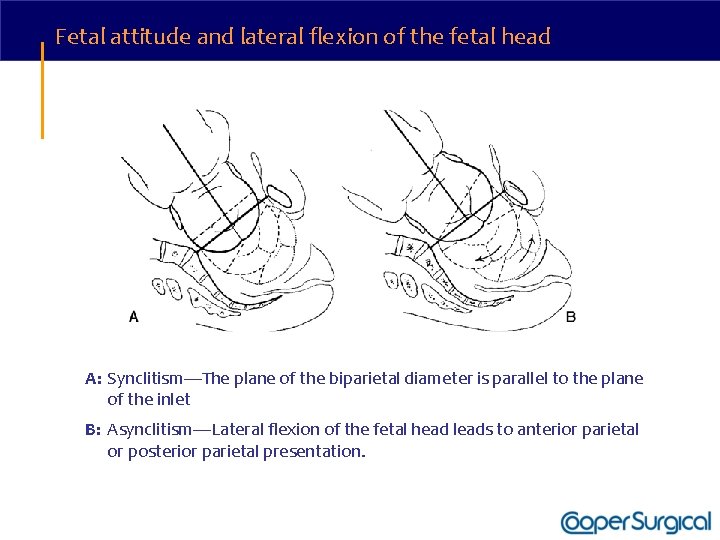
Fetal attitude and lateral flexion of the fetal head A: Synclitism—The plane of the biparietal diameter is parallel to the plane of the inlet B: Asynclitism—Lateral flexion of the fetal head leads to anterior parietal or posterior parietal presentation.

Prerequisites for OVD • Informed consent • Vertex • Engaged • ≥ 34 weeks (vacuum delivery) • Fully dilated • Membranes ruptured • Adequate maternal pelvis • Adequate anesthesia • Maternal empty bladder • Backup plan • Ongoing fetal and maternal assessment

Contraindication - OVD • Non-cephalic, face or brow presentation • Unengaged vertex • Incompletely dilated cervix • Clinical evidence of CPD • < 34 weeks gestation (vacuum) • Need for device rotation (vacuum) • Deflexed attitude of fetal head • Fetal conditions (e. g. thrombocytopenia)

Classification of OVD • Outlet • • • Scalp visible @ introitus w/o separating labia Fetal skull @ pelvic floor Saggital suture in AP plane (or ROA/LOA) Fetal head at or on perineum Rotation < 45 degrees • Low • Leading point of fetal skull > or = +2 station • Rotation < 45 degrees • Rotation > 45 degrees • Mid • Station above +2 station but the head is engaged • High • Not included in classification

Vacuum versus Forceps • “Selection of the appropriate instrument and decisions about the maternal and fetal consequences should be based on clinical findings at the time of delivery. ”* • A meta-analysis comparing vacuum extraction to forcep delivery showed that vacuum extraction was associated with significantly less maternal trauma and less need for general and regional anesthesia** *ACOG Practice Bulletin #17 (June 2000) **Johnson RB. The Cochrane Library Issue 4, 1999
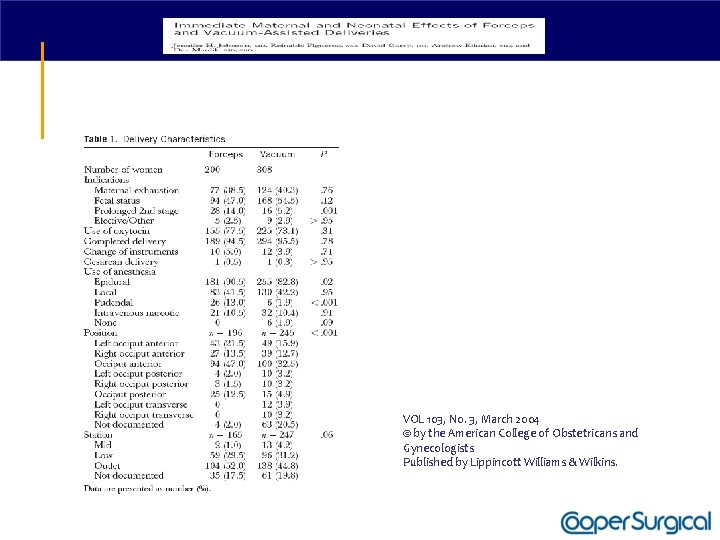
VOL 103, No. 3, March 2004 © by the American College of Obstetricans and Gynecologists Published by Lippincott Williams & Wilkins.

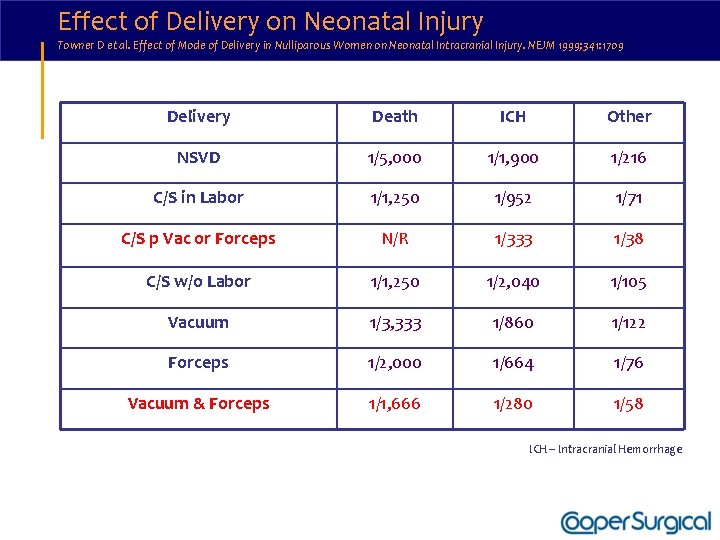
Effect of Delivery on Neonatal Injury Towner D et al. Effect of Mode of Delivery in Nulliparous Women on Neonatal Intracranial Injury. NEJM 1999; 341: 1709 Delivery Death ICH Other NSVD 1/5, 000 1/1, 900 1/216 C/S in Labor 1/1, 250 1/952 1/71 C/S p Vac or Forceps N/R 1/333 1/38 C/S w/o Labor 1/1, 250 1/2, 040 1/105 Vacuum 1/3, 333 1/860 1/122 Forceps 1/2, 000 1/664 1/76 Vacuum & Forceps 1/1, 666 1/280 1/58 ICH – Intracranial Hemorrhage
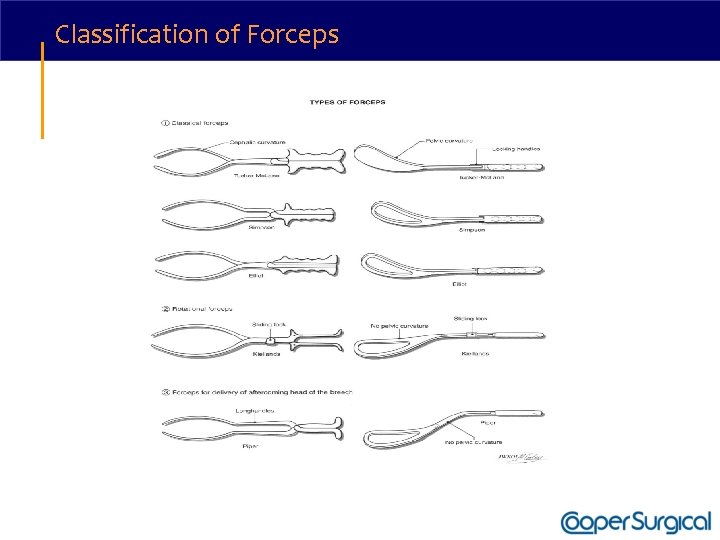
Classification of Forceps
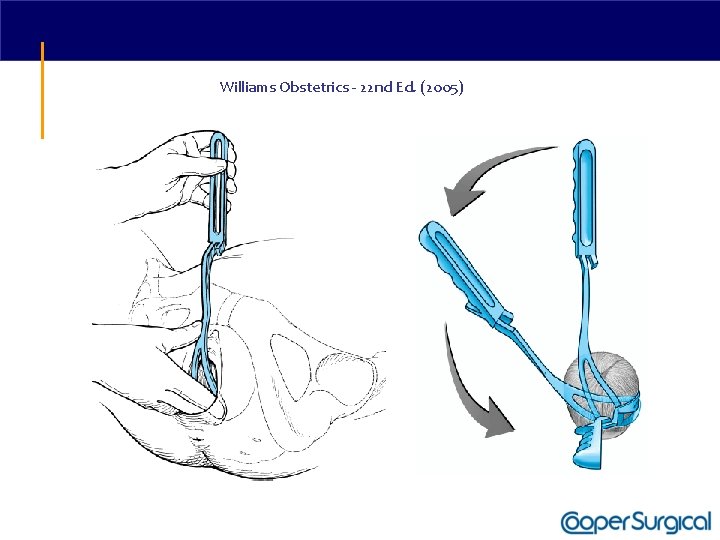
Williams Obstetrics - 22 nd Ed. (2005)
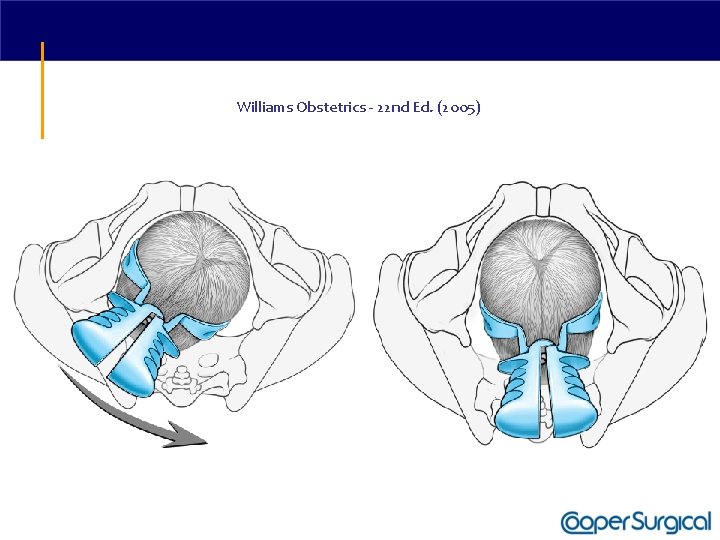
Williams Obstetrics - 22 nd Ed. (2005)
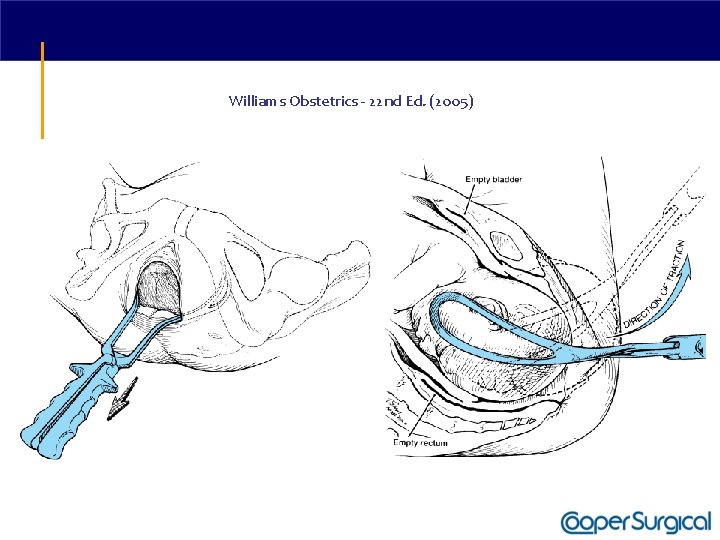
Williams Obstetrics - 22 nd Ed. (2005)
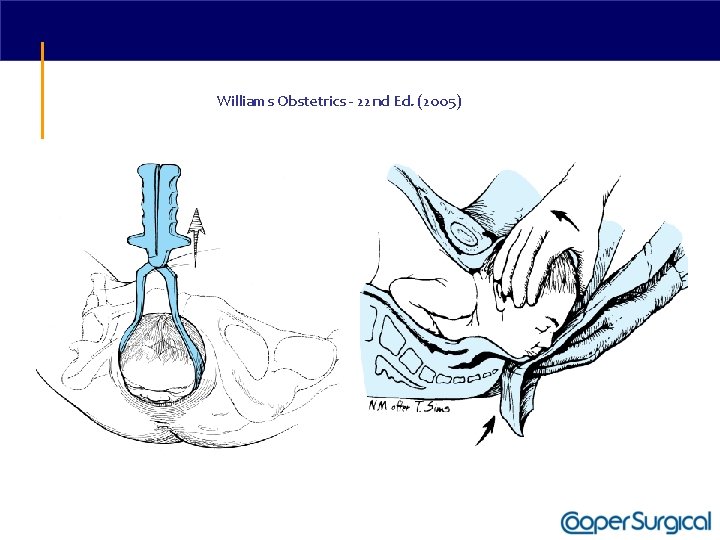
Williams Obstetrics - 22 nd Ed. (2005)
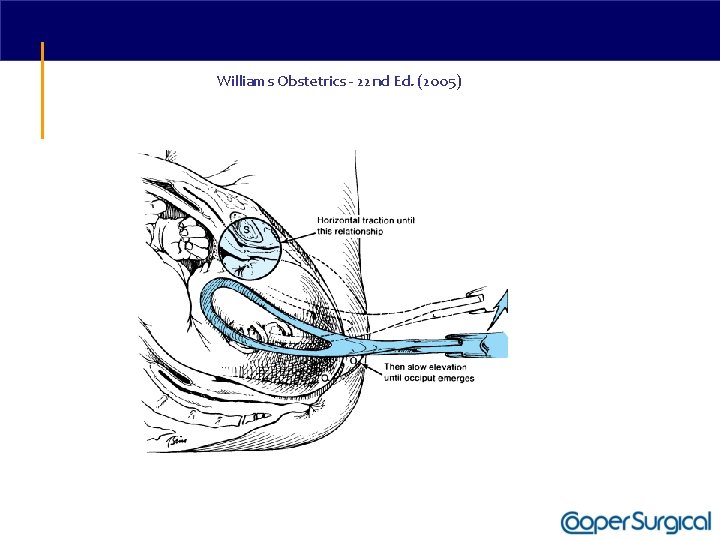
Williams Obstetrics - 22 nd Ed. (2005)


Vacuum Delivery • The advantage of the vacuum extractor over forceps include the avoidance of insertion of space-occupying steel blades within the vagina. • Previously described instruments were mostly unsuccessful until Malmstrom (1954) applied traction on a metal cap designed so that the suction creates an artificial caput, or chignon, within the cup that holds firmly and allows adequate traction. • In the United States, the metal cup generally has been replaced by newer soft cup vacuum extractors

Vacuum Cups • Bell vs. Mushroom • Most soft cups are bell shaped while most rigid cups are mushroom (M-cup). • Bell cups generate less traction force than M-cups. * • M-cup is low profile and may facilitate application with asynclitism or non-OA presentations. • Soft vs. Rigid • Soft cups were more likely to fail to achieve vaginal delivery (OR 1. 65; 95% CI 1. 192. 29)** • Soft cups were associated with less scalp injury (OR 0. 45; 95% CI 0. 15 -0. 60)** * Muise, KL, Duchon, MA, Brown, RH. The effect of artificial caput on performance of vacuum extractors. Obstet Gynecol 1993; 81: 170. ** Johanson, R, Menon, V. Soft versus rigid vacuum extractor cups for assisted vaginal delivery. Cochrane Database Syst Rev 2000
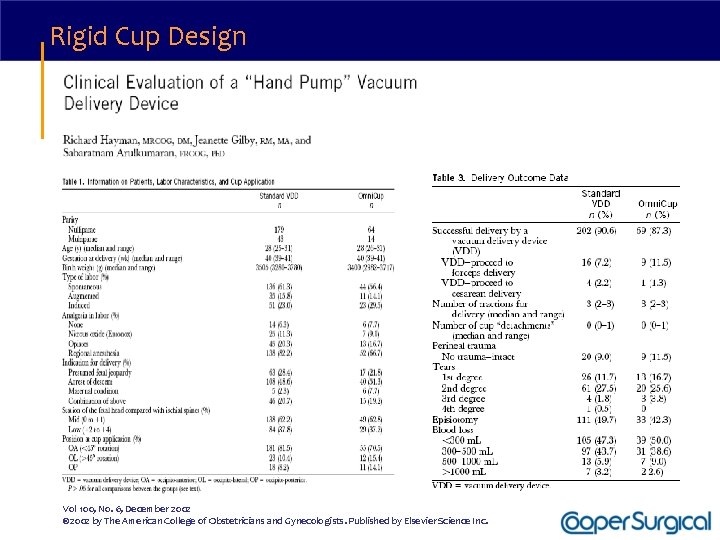
Rigid Cup Design Vol 100, No. 6, December 2002 © 2002 by The American College of Obstetricians and Gynecologists. Published by Elsevier Science Inc.
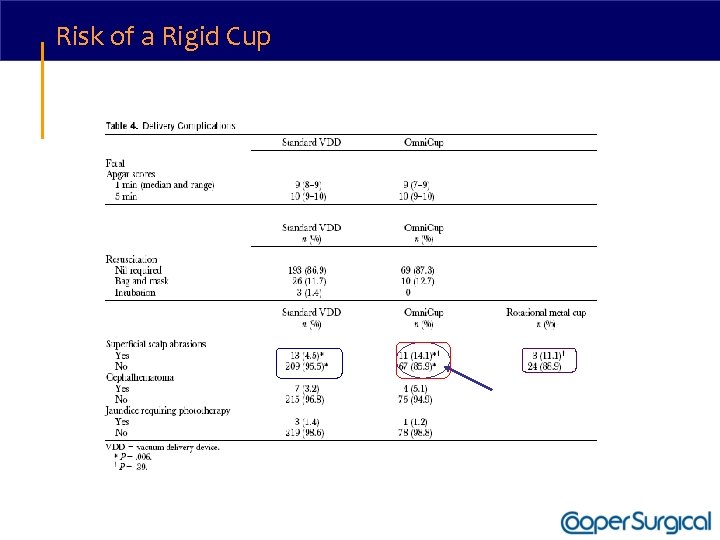
Risk of a Rigid Cup

Vacuum Cups • The use of soft, bell-shaped vacuum extractor is recommended for uncomplicated, occiput anterior deliveries. • The rigid M-style cup is recommended for deliveries likely to require greater traction forces. • Non OA • Asynclitism • Use at cesarean section
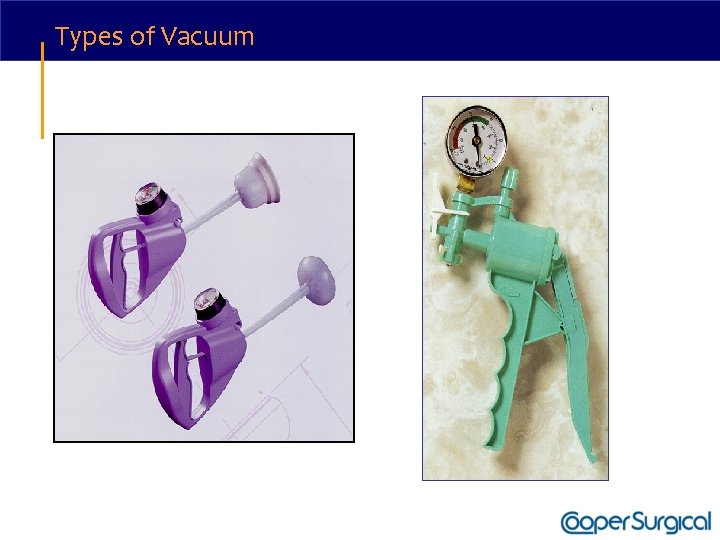
Types of Vacuum
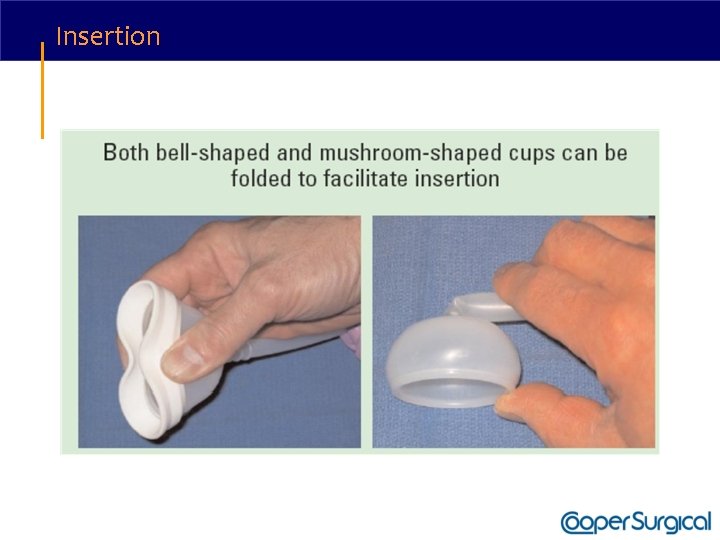
Insertion

Vacuum Placement • Proper cup placement is the most important determinant of success in vacuum extraction. • The center of the cup should be over the sagittal suture and about 3 cm in front of the posterior fontanelle toward the face – median flexion point.

Vacuum Procedure • The entire 360º circumference of the cup must then be digitally inspected to insure that no vaginal or vulvar tissues are trapped between the cup and the fetal surface. • After correct placement of the cup is confirmed, vacuum pressure should be raised to 100 to 150 mm. Hg to maintain the cup's position. • Vacuum suction pressures of 500 to 600 mm. Hg have been recommended during traction.

Vacuum Procedure • A slow, stepwise increase in vacuum pressure was initially practiced, but is no longer recommended. • gradual versus rapid application of vacuum pressure demonstrated the rapid technique reduced the duration of the vacuum extraction procedure without compromising efficiency and safety Lim, FT, Holm, JP, Schuitemaker, NW, et al. Stepwise compared with rapid application of vacuum in ventouse extraction procedures. Br J Obstet Gynaecol 1997; 104: 33. Svenningsen, L. Birth progression and traction forces developed under vacuum extraction after slow or rapid application of suction. Eur J Obstet Gynecol Reprod Biol 1987; 26: 105.

Vacuum Procedure • Suction pressure is measured in various units: 0. 8 kg/cm 2 of atmospheric pressure = 600 mm. Hg = 23. 6 inches of Hg = 11. 6 lb/in(2). • Vacuum suction pressures of 500 to 600 mm. Hg have been recommended during traction, although pressures in excess of 450 mm. Hg are rarely necessary Ross, MG, Fresquez, M, El-Haddad, MA. Impact of FDA advisory on reported vacuum-assisted delivery and morbidity. J Matern Fetal Med 2000; 9: 321. 10. Billings, RG. The physics of vacuum extraction. OBG Manag 2004; Suppl S 7 -8.

© 2005 Up. To. Date® www. uptodate. com • The absolute "safe" traction force for vacuum extraction is unknown. • However, since traction force needs to be individually calculated and will vary with cup size, suction pressure, and altitude, it is reasonable and practical to rely solely on the suction pressure, which is displayed on all the commercially available devices. Up. To. Date performs a continuous review of over 330 journals and other resources. Updates are added as important new information is published. The literature review for version 13. 2 is current through April 2005; this topic was last changed on March 28, 2005. The next version of Up. To. Date (13. 3) will be released in October 2005.

Vacuum Delivery • Practitioners assist by adding to the momentum of the maternal expulsive efforts rather than pulling the baby out independently. • The fingertips of the dominant hand pull the device's crossbar, while the nondominant hand monitors the progress of descent and prevents cup detachment by placing counter pressure with the thumb

Vacuum Delivery • Apply traction along the axis of the pelvic curve. • Initially, the angle of traction is downward (toward the floor); the higher the beginning station, the steeper the angle of downward traction required. • The axis of traction is then extended upwards to a 45 degree angle to the floor as the head emerges from the pelvis and crowns. • The handle of the device is allowed to passively turn as the head auto-rotates through its descent.
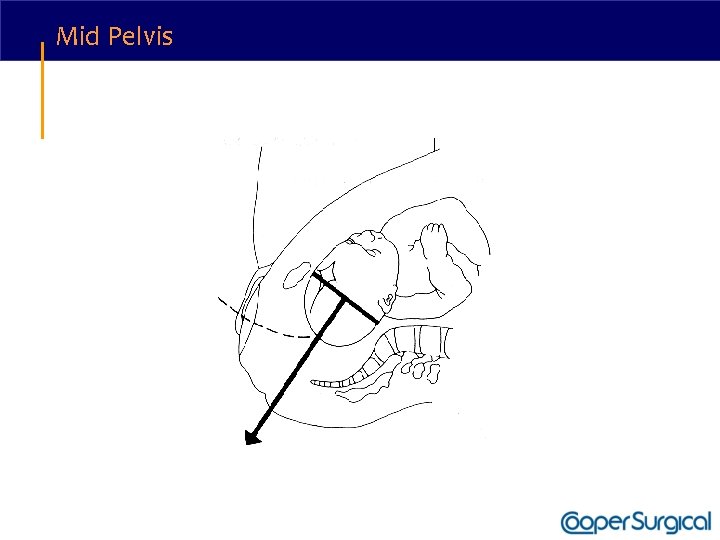
Mid Pelvis
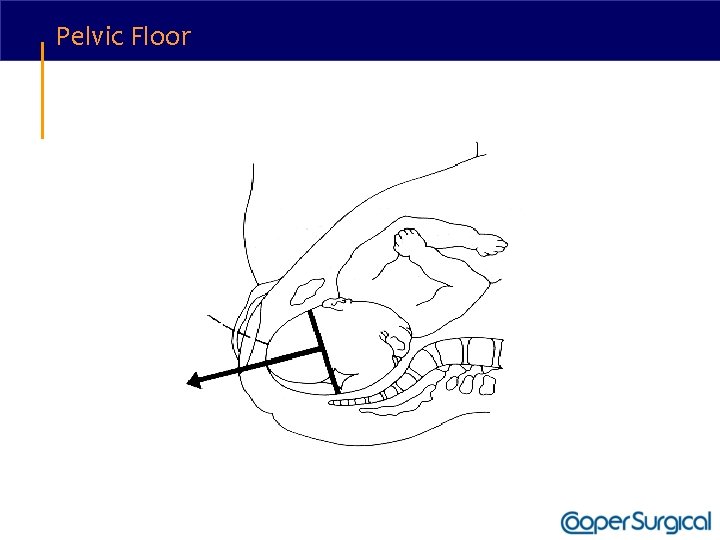
Pelvic Floor
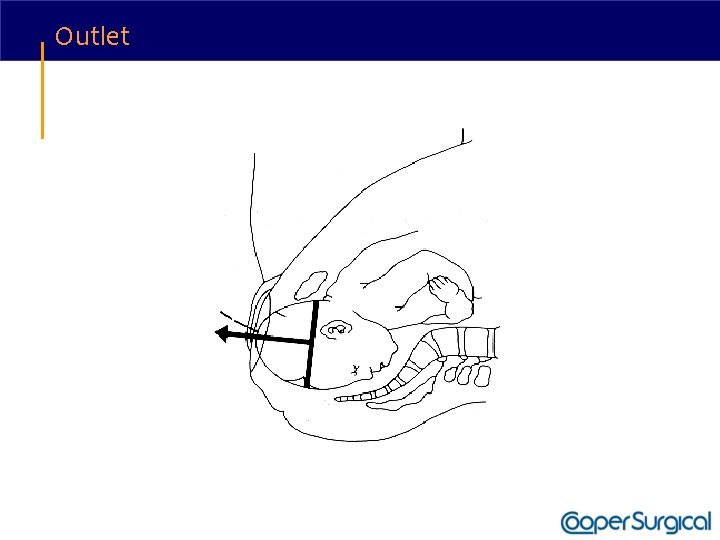
Outlet

Vacuum Delivery • Traction is gradually discontinued as the contraction ends or the mother stops pushing. • Between contractions, suction pressure can be fully maintained or reduced to <200 mm. Hg • fetal morbidity is similar for both regimens* • Descent should occur with each application of traction • When the head is delivered, the suction is released, the cup is removed, and the remainder of the delivery proceeds as usual. * Bofill, JA, Rust, OA, Schorr, SJ, Brown, RC, Roberts, WE, Morrison, JC. A randomized trial of two vacuum extraction techniques. Obstet Gynecol 1997; 89: 758.
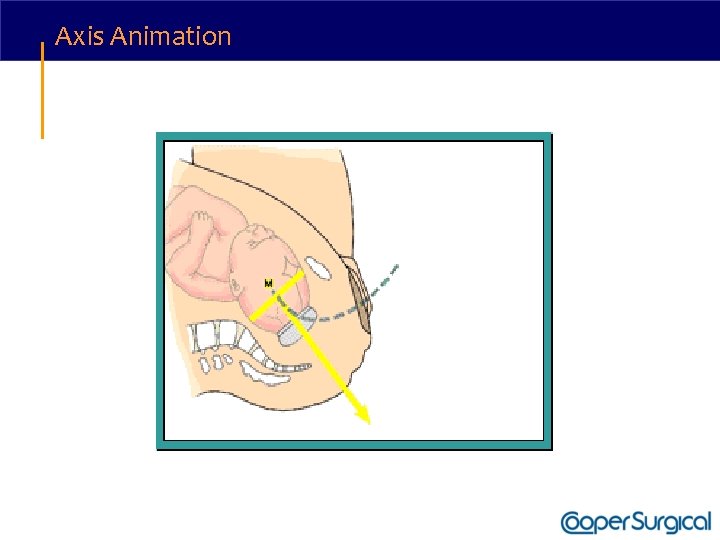
Axis Animation
Outlet Vacuum

DURATION of Vacuum © 2005 Up. To. Date® www. uptodate. com • The maximum time to safely complete a vacuum assisted delivery and the number of acceptable "pop-offs" is unknown. • “These recommendations are based more upon common sense and experience than scientific data as observational series have shown no longterm differences in neonatal outcome related to these variables. ” • A maximum of two to three cup detachments • 3 sets of pulls • Total vacuum application time of 15 to 30 minutes

Failed Procedures • Reasons for failure: • CPD • Incorrect technique § Traction w/o maternal pushing efforts § Upward traction prior to crowning • Paramedian or deflexing application • Large caput seccedaneum § Large volume of scalp into cup reduces the total vacuum area § More pronounced with bell compared to mushroom cups § More pronounced with soft compared to rigid cups

Avoiding Problems • Confirm cup placement • Avoid entrapping vaginal soft tissue • Know when to abandon the procedure • Practitioners must be willing and able to abandon the procedure and proceed to cesarean delivery promptly when the vaginal delivery is not progressing normally. • An indicated vaginal delivery that could not be completed with vacuum assistance is unlikely to progress to a spontaneous vaginal delivery with a little more time and delay may increase the risk of neonatal or maternal morbidity.

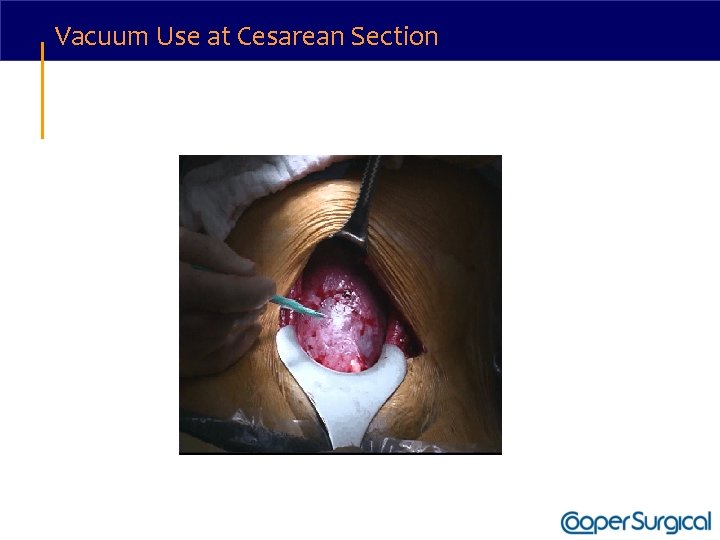
Vacuum Use at Cesarean Section
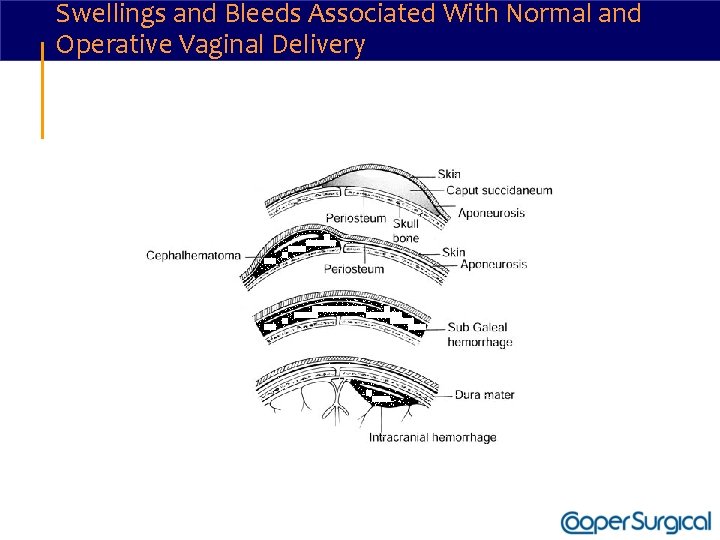
Swellings and Bleeds Associated With Normal and Operative Vaginal Delivery
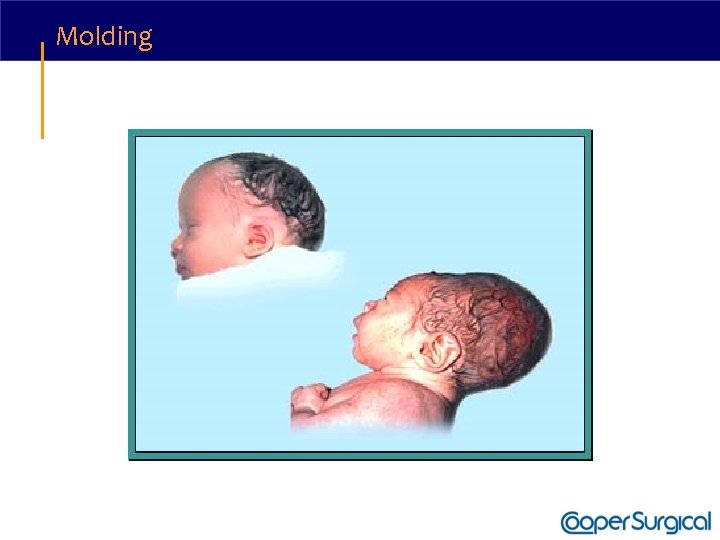
Molding
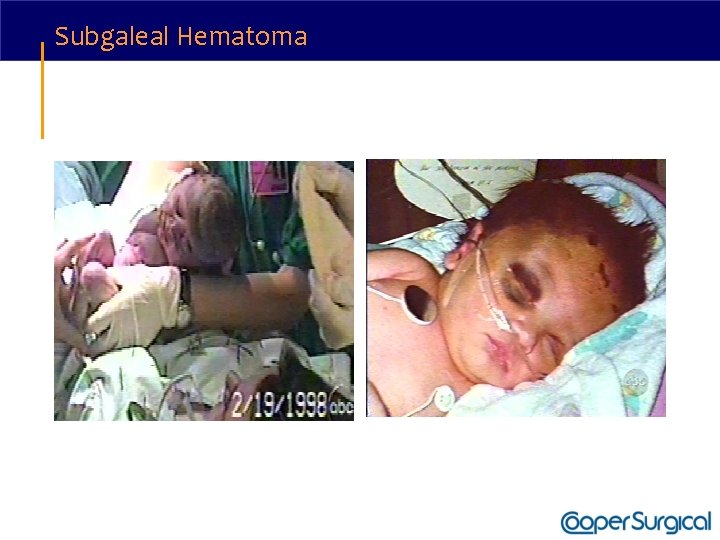
Subgaleal Hematoma
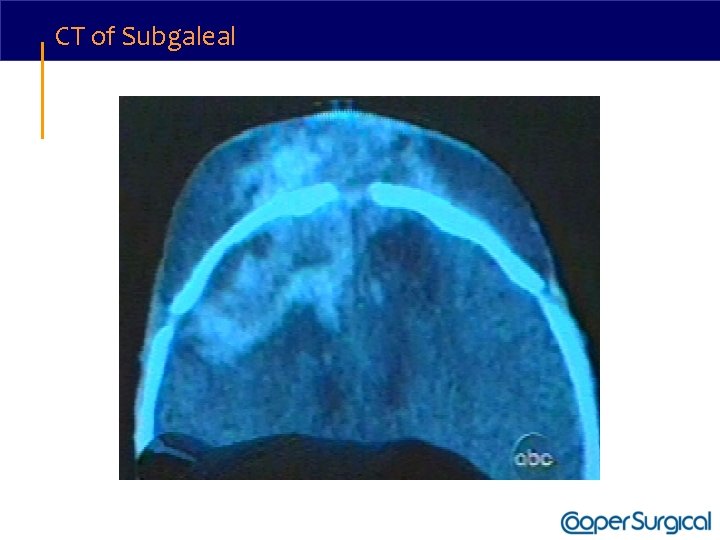
CT of Subgaleal

SUMMARY AND RECOMMENDATIONS - Up. To. Date® March 28, 2005 • There is inadequate evidence upon which to base a recommendation for use of a particular type of vacuum for all circumstances when a vacuum assisted delivery is attempted. • A successful vacuum extraction is most likely: • accurate cup application • appropriate traction technique • a favorable flexed fetal cranial position • low station at the time of application

SUMMARY AND RECOMMENDATIONS - Up. To. Date® March 28, 2005 • Only attempt a vacuum assisted delivery when a specific obstetric indication is present. • No indication is absolute • The use of soft, bell-shaped vacuum extractor is recommended for uncomplicated, OA deliveries. • Apply the cup at the flexion point.

SUMMARY AND RECOMMENDATIONS - Up. To. Date® March 28, 2005 • Rapid application of vacuum suction pressures of 500 to 600 mm. Hg have been recommended during traction. • Apply gentle traction along the axis of the pelvic curve in concert with maternal pushing. • Limit vacuum assisted procedures to 2 to 3 "pop-offs, " and a total time of 15 to 30 minutes.

SUMMARY AND RECOMMENDATIONS - Up. To. Date® March 28, 2005 • Failure of an attempted vacuum assisted delivery increases the likelihood of neonatal morbidity; the subsequent use of sequential forceps in this setting should be undertaken with extreme caution. • Prompt cesarean delivery is advised after an unsuccessful vacuum assisted procedure.

FDA: Vacuum Delivery Devices
- Slides: 56