OPERATIVE VAGINAL DELIVERY OVD ASEEL ABUALNIL OPERATIVE VAGINAL

OPERATIVE VAGINAL DELIVERY (OVD) ASEEL ABUALNIL

OPERATIVE VAGINAL DELIVERY (OVD) • Operative vaginal delivery (OVD) refers to a vaginal birth with the use of any type of forceps or vacuum extractor (ventouse) • OVD = instrumental delivery = assisted vaginal delivery • .

INDICATIONS • The indications for OVD can be divided into fetal or maternal, although in many cases these factors coexist. Ø The most common fetal factor is suspected fetal compromise, usually based on a pathological cardiotocograph (CTG). other indications are abnormal ph , lactate on fetal sampling , or thick meconium Ø The most common maternal factor is a prolonged active second stage of labour.

CONTRAINDICATIONS • Safety criteria for operative vaginal delivery consist of: A. Full abdominal and vaginal examination (Head is minimal palpable per abdomen, Cervix is fully dilated and the membranes ruptured, Station at level of ischial spines or below, position of the head, Caput and moulding is no more than moderate) B. Preparation of mother (Informed consent, Appropriate anaesthesia, Empty maternal bladder and Remove in-dwelling catheter or balloon deflated) C. Preparation of staff (Operator, Adequate facilities, Back-up plan “caesarean section”, Anticipation of complications, Trained in neonatal resuscitation) D. When safety criteria are not met OVD is contraindicated • Forceps and vacuum extractor deliveries before full dilatation of the

PROCEDURE q. Analgesia • Analgesic requirements are greater forceps than for ventouse delivery q. Positioning OVDs are traditionally performed with the patient in the lithotomy position Contingency It may be possible to complete a failed vacuum delivery with forceps, but failed forceps delivery will almost always result in caesarean section.

) Vaccum/ventous

INSTRUMENT TYPES q. Ventouse/vacuum extractors v. Technique v–positioning v. The cup inserted on flexion point of baby’s head (2 cm anterior to posterior fontanelle. v. Variation of cup sizes depends on baby’s head • Soft vacuum cups are significantly more likely to fail to achieve vaginal delivery than rigid cups; however, they are associated with less scalp injury. • There appear to be no difference in terms of maternal trauma.

• Recent developments have removed the need for external suction generators and have incorporated the vacuum mechanism into ‘hand-held’ pumps (e. g. Omni-Cup) • It is not acceptable to use a ventouse when: • Premature baby’s 1. The position of the fetal head is unknown. 2. There is a significant degree of caput that may either preclude correct placement of the cup or, more sinisterly, indicate a substantial degree of CPD. 3. The operator is inexperienced in the use of the instrument
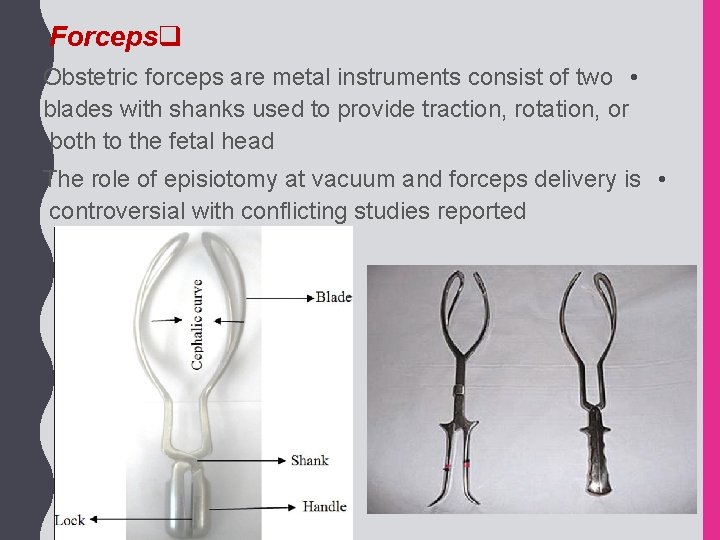
Forcepsq Obstetric forceps are metal instruments consist of two • blades with shanks used to provide traction, rotation, or both to the fetal head The role of episiotomy at vacuum and forceps delivery is • controversial with conflicting studies reported

https: //www. youtube. com/watch? v=y 0 J 3 W_W 73 3 w

COMPLICATIONS Maternal Complicationsq vacuum deliveries as a result Maternal deaths have been reported with Ø of cervical tearing in women delivered before full dilatation. Traumatic and non-traumatic vaginal delivery is considered to be the Ø most important risk factor fecal incontinence (anal sphincter injury is twice as common with forceps delivery compared to ventouse). PPH and Under-estimation of blood loss is more common in women Ø needing OVD compared to women who deliver spontaneously, but less common than in women delivered by caesarean section in the second stage.
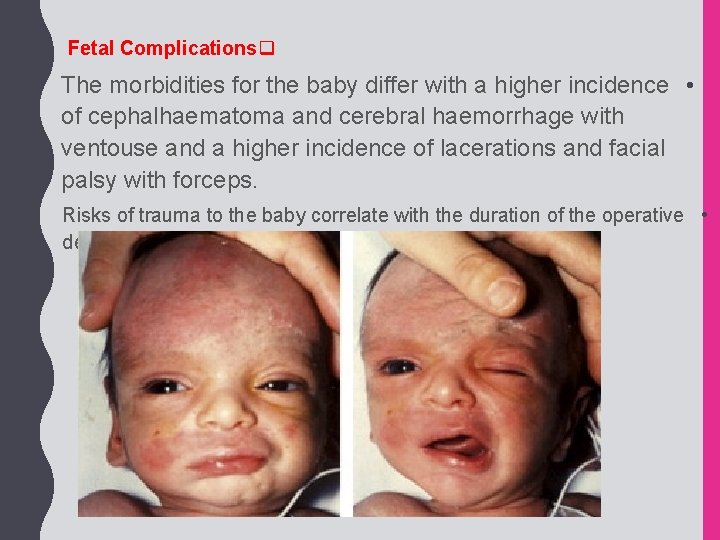
Fetal Complicationsq The morbidities for the baby differ with a higher incidence • of cephalhaematoma and cerebral haemorrhage with ventouse and a higher incidence of lacerations and facial palsy with forceps. Risks of trauma to the baby correlate with the duration of the operative • delivery.

The ventouse comp to forceps is significantly more likely to be associated with: (ventouse side effect) 1. 2. 3. Failure to achieve a vaginal delivery. Cephalo-haematoma (subperiosteal bleed). Retinal haemorrhage. The ventouse compared to forceps is significantly less likely to be associated with: (forceps side effect) 1. 2. 3. Use of maternal regional/general anaesthesia. Significant maternal perineal and vaginal trauma. Severe perineal pain at 24 hours. ared 1. Side effects FORCEPS>VENTOUS 2. Success FORCEPS>VENTOUS

CAESAREAN SECTION Def : A caesarean section is a surgical procedure in which incisions are made through a woman’s abdomen (laparotomy) and uterus (hysterotomy) to deliver one or more babies it is the most common operation performed worldwide Increased incidence worldwide during last 25 years

CLASSIFICATION ACCORDING TO TIMING: • - Elective CS • -Emergency CS • ACCORDING TO GESTATIONAL AGE: • -before age of viability (hysterectomy) • -after the age of viability (caesarean) • ACCORDING TO UTERINE INCISION • -Transverse LSCS • -Vertical (classical) •

>CLASSIFICATION ELECTIVE VS EMERGENCY � Elective caesarean sections are usually booked days or weeks ahead of time emergency caesarean section • �Category 1: Immediate threat to life of woman or fetus • �Category 2: No immediate threat to life of woman or fetus • �Category 3: Requires early delivery • �Category 4: At a time to suit the woman and maternity services •

INDICATIONS: THE FOUR MAJOR INDICATIONS ACCOUNTING FOR GREATER THAN 70% OF OPERATIONS ARE: • PREVIOUS CAESAREAN SECTION. • MALPRESENTATION (MAINLY BREECH). • FAILURE TO PROGRESS IN LABOUR. • SUSPECTED FETAL COMPROMISE IN LABOUR

RELATIVE INDICATIONS : • • Fetal distress in first stage of labour or a prolapsed cord. • • CPD • • Failure of labour to progress despite adequate stimulation. • To avoid • fetal hypoxia of labour: pre-eclampsia; intrauterine growth restriction. • Antepartum bleeding: placenta praevia; abruptio placentae. • • Poor past obstetric history. • Malpresentations: brow. • Malpositions: • transverse lie, breech. • Death of mother in late pregnancy, a live fetus removed peri • mortem. The only ABSOLUTE ones are: • • gross disproportion, • • the higher grades of placenta praevia. •

THANKS!
- Slides: 19