Open Periarticular Tibial Plateau Case for small group

Open Periarticular Tibial Plateau Case for small group discussion: Acute trauma AOTrauma External Fixation
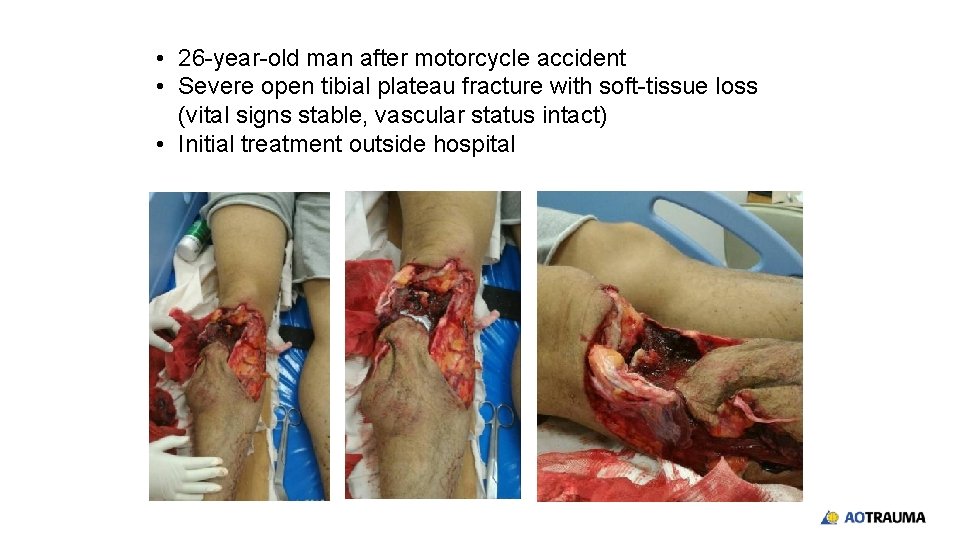
• 26 -year-old man after motorcycle accident • Severe open tibial plateau fracture with soft-tissue loss (vital signs stable, vascular status intact) • Initial treatment outside hospital
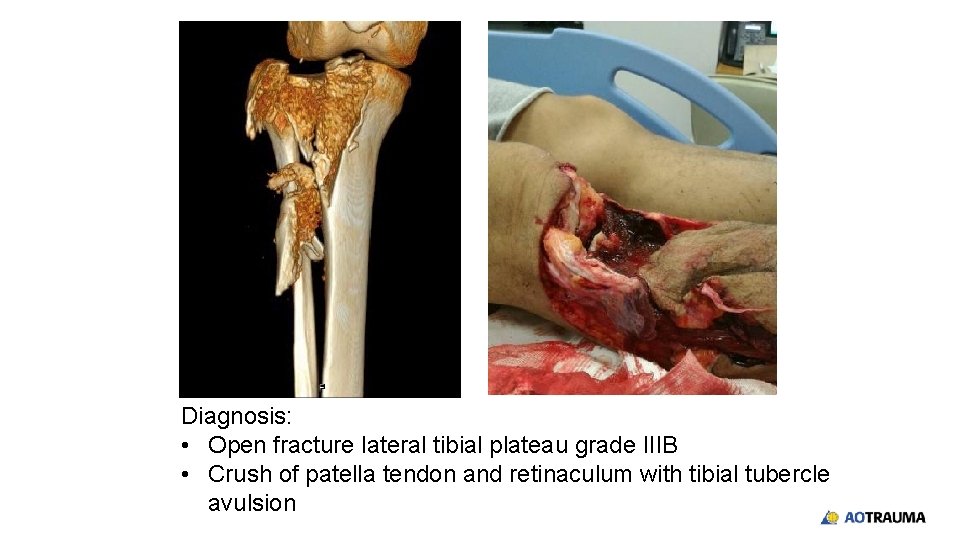
Diagnosis: • Open fracture lateral tibial plateau grade IIIB • Crush of patella tendon and retinaculum with tibial tubercle avulsion
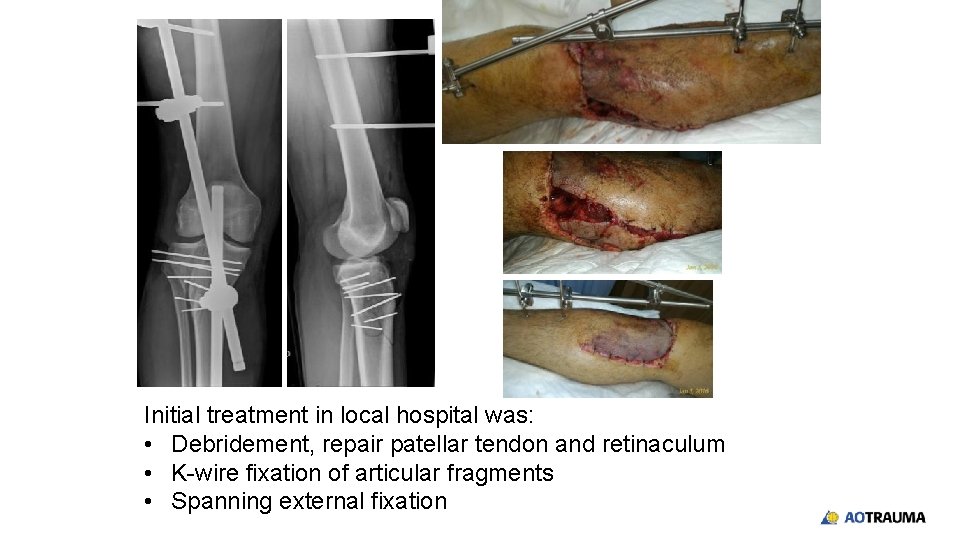
Initial treatment in local hospital was: • Debridement, repair patellar tendon and retinaculum • K-wire fixation of articular fragments • Spanning external fixation
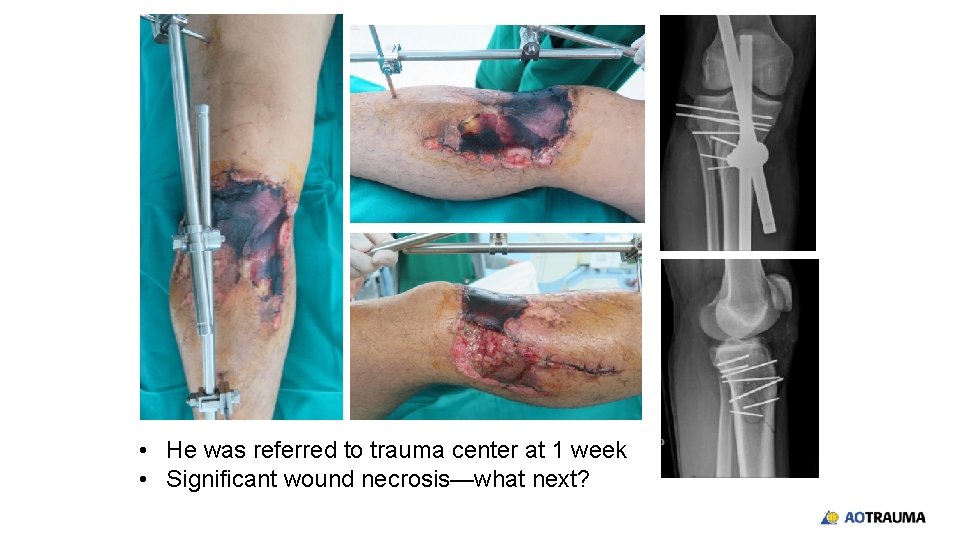
• He was referred to trauma center at 1 week • Significant wound necrosis—what next?
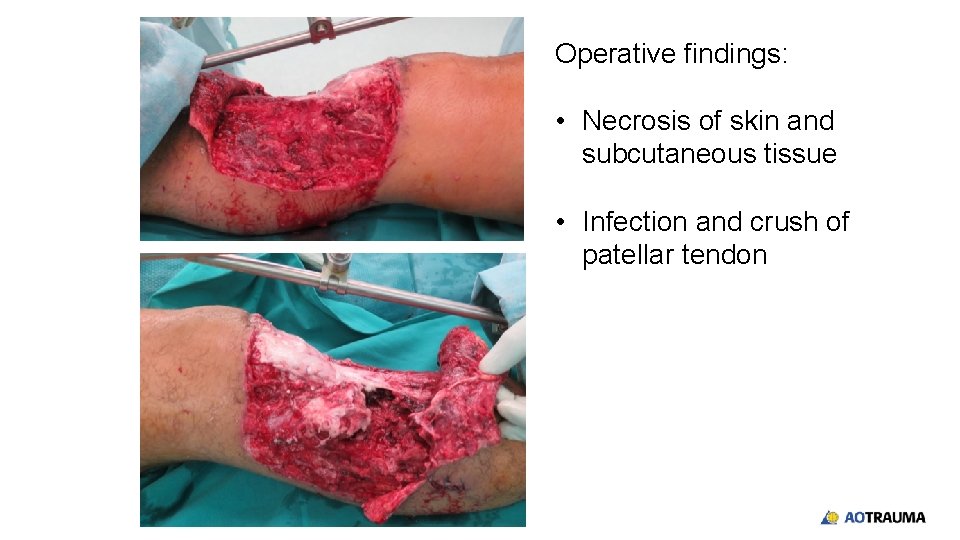
Operative findings: • Necrosis of skin and subcutaneous tissue • Infection and crush of patellar tendon
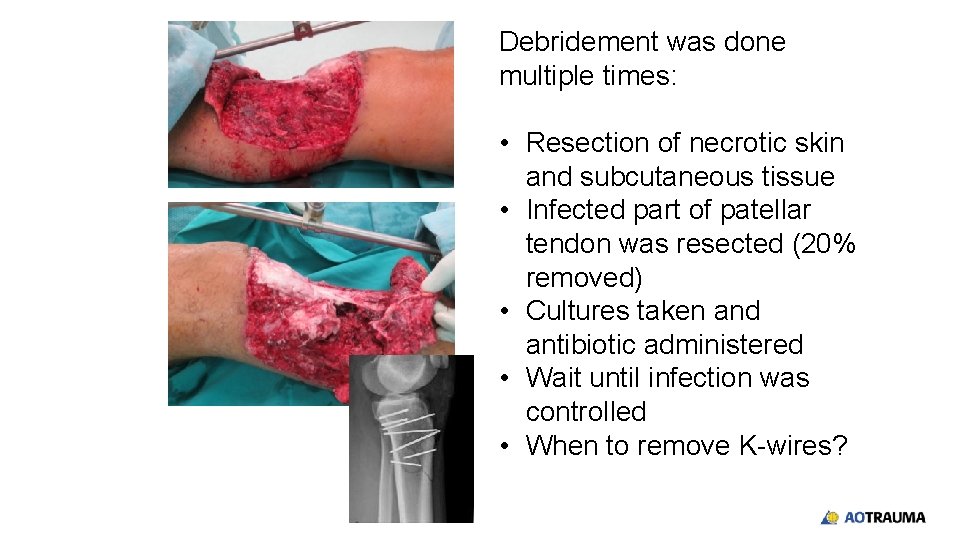
Debridement was done multiple times: • Resection of necrotic skin and subcutaneous tissue • Infected part of patellar tendon was resected (20% removed) • Cultures taken and antibiotic administered • Wait until infection was controlled • When to remove K-wires?
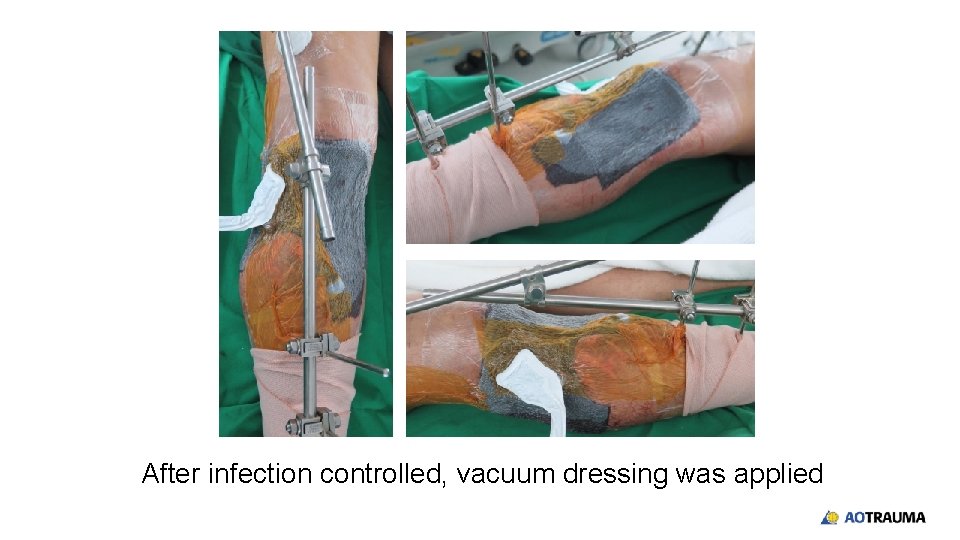
After infection controlled, vacuum dressing was applied
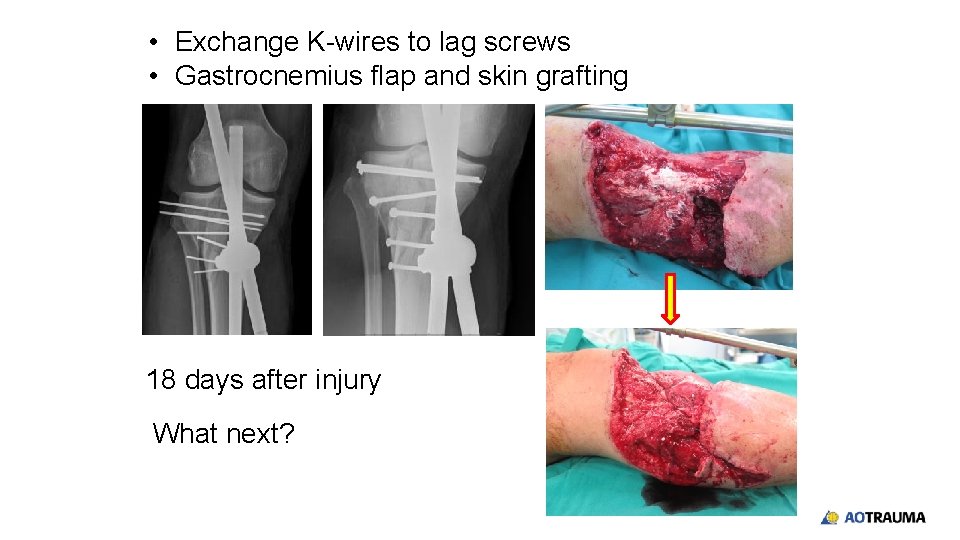
• Exchange K-wires to lag screws • Gastrocnemius flap and skin grafting 18 days after injury What next?
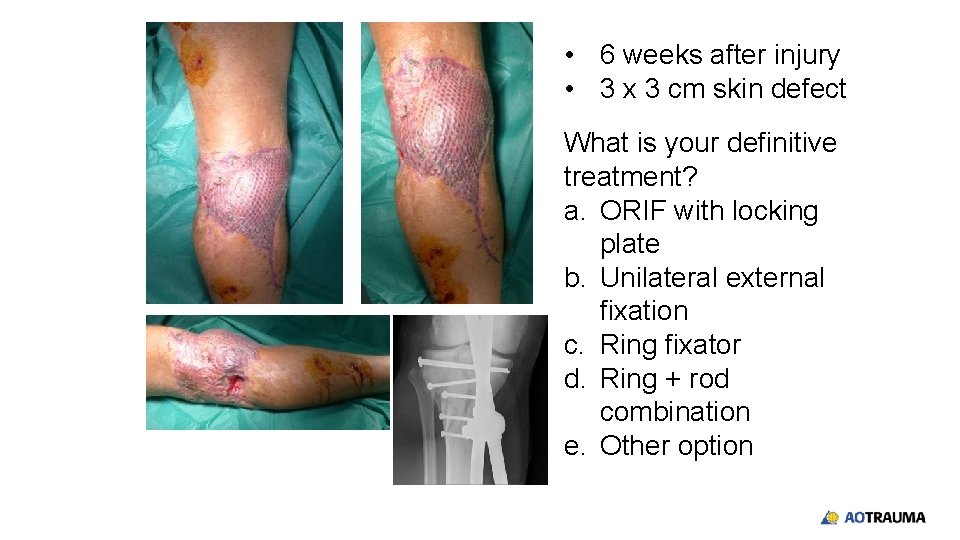
• 6 weeks after injury • 3 x 3 cm skin defect What is your definitive treatment? a. ORIF with locking plate b. Unilateral external fixation c. Ring fixator d. Ring + rod combination e. Other option
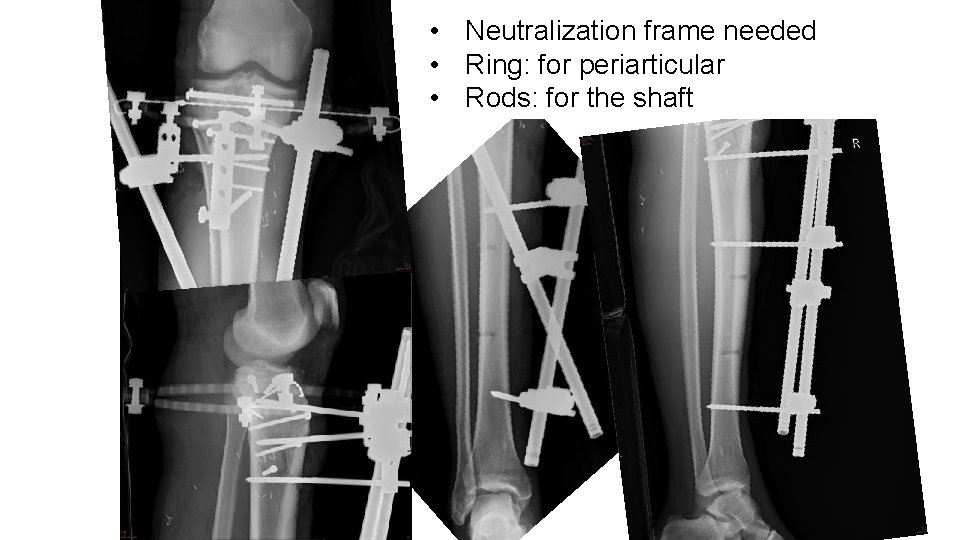
• Neutralization frame needed • Ring: for periarticular • Rods: for the shaft
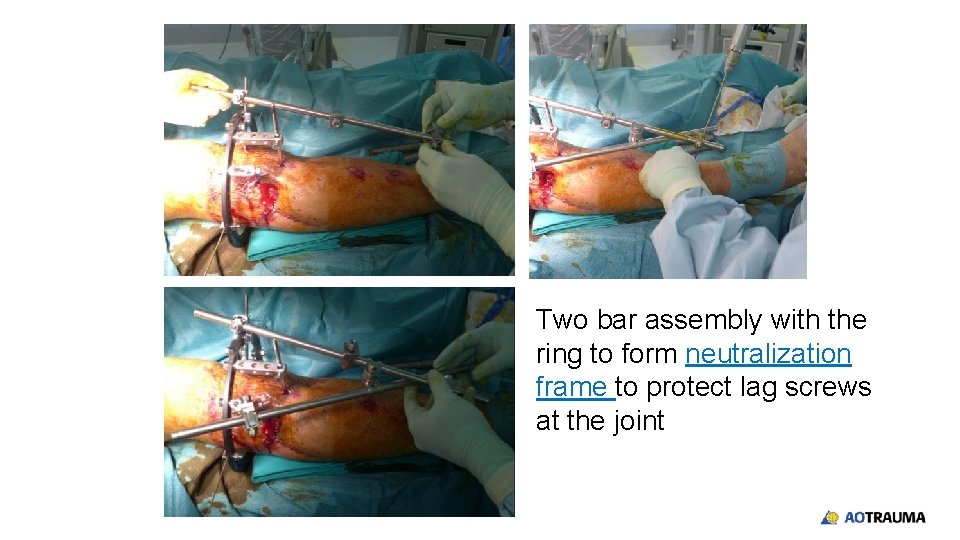
Two bar assembly with the ring to form neutralization frame to protect lag screws at the joint
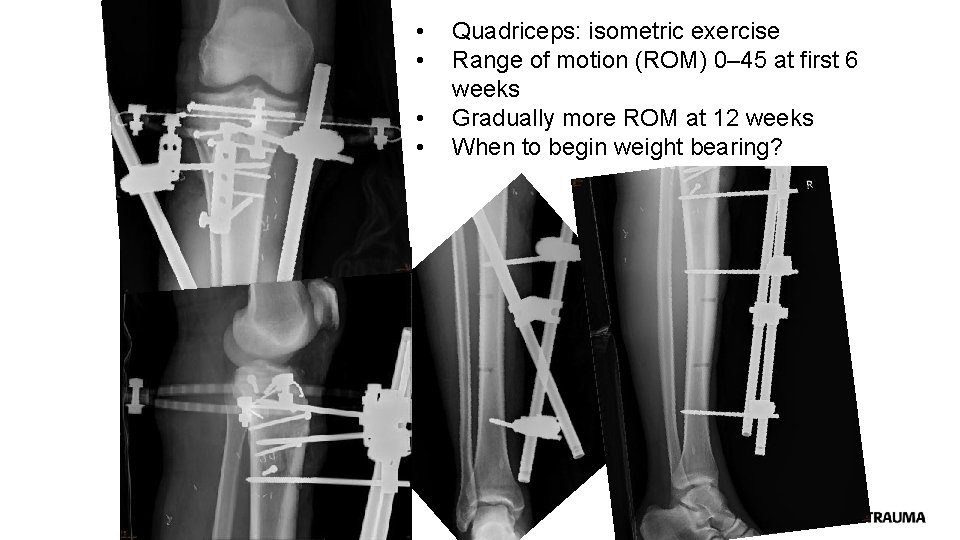
• • Quadriceps: isometric exercise Range of motion (ROM) 0‒ 45 at first 6 weeks Gradually more ROM at 12 weeks When to begin weight bearing?
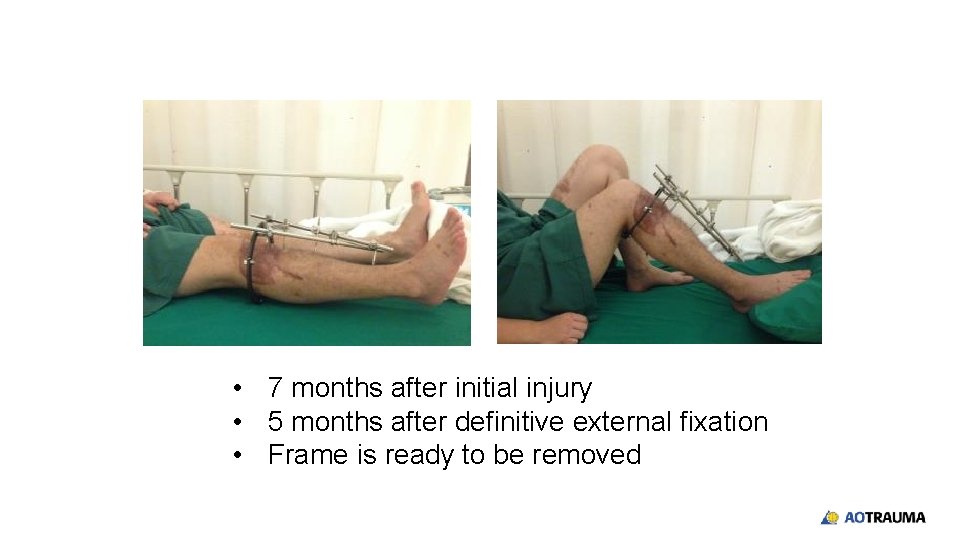
• 7 months after initial injury • 5 months after definitive external fixation • Frame is ready to be removed
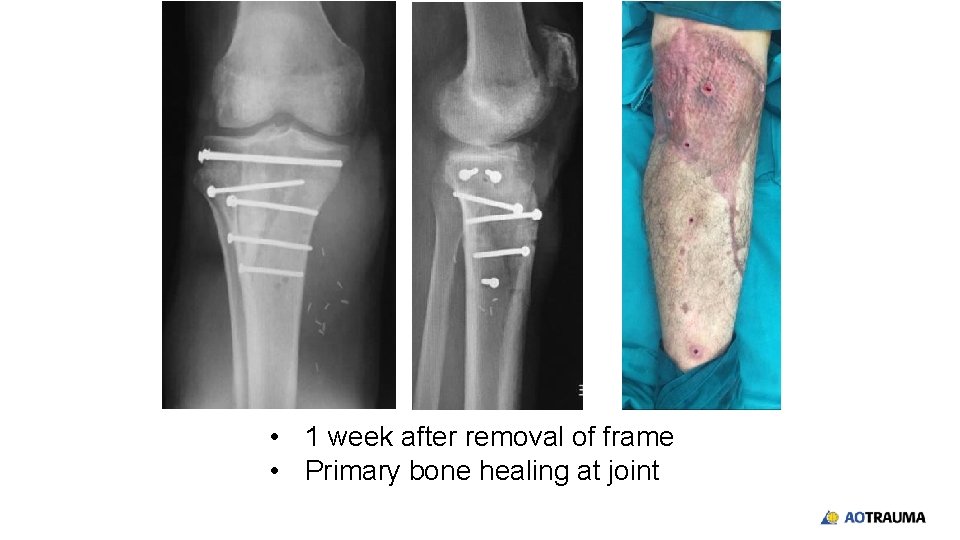
• 1 week after removal of frame • Primary bone healing at joint
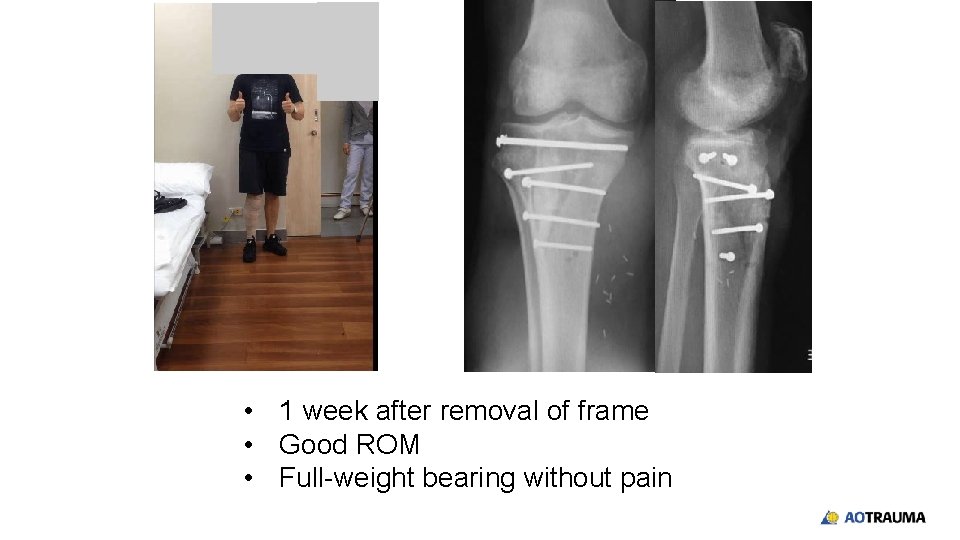
• 1 week after removal of frame • Good ROM • Full-weight bearing without pain

Take-home messages • • 17 Initial spanning external fixation of the limb to maintain alignment and stability In this case, infection risk is high; therefore, consider external fixation (instead of plates) Lag screws in the articular portion of the fracture can be protected by external fixation Definitive external fixation is easiest if done after flap coverage is accomplished
- Slides: 17