Open Disclosure Workshop January 2020 HSE Open Disclosure















































































- Slides: 82

Open Disclosure: Workshop January 2020

HSE | Open Disclosure Part 1 Introduction

HSE | Open Disclosure

HSE | Open Disclosure Introduction • Housekeeping Fire exits Breaks/Refreshments • Ground Rules • Workbooks

HSE | Open Disclosure Background Recommendations: “Building a Culture of Patient Safety 2008” Joint HSE/SCA approach supported by MPS Pilot October 2010 - March 2013 Launch of national documents November 2013 On-going roll out of policy and programme across all health and social care services since 2013 – national training programme – area and site leads Independent evaluation of pilot programme published in 2016

HSE | Open Disclosure Background • QAVD audit of x 4 early adopter sites in 2016 • Matters arising in Cervical Check Screening Programme 2018 and Scally Report and Recommendations September 2018 • Protective legislation: Commencement of Part 4 of the Civil Liability Amendment Act 2017 – September 2018 • Establishment of National OD Office and National Steering Committee 2018 -2019 • Interim Revision of HSE National Open Disclosure Policy launched in June 2019

HSE | Open Disclosure Workshop Objectives 1. To provide an overview of the national open disclosure programme. 2. To build understanding as to how the principles of open disclosure link into existing HSE Quality, Patient Safety and Risk procedures/frameworks. 3. To provide best practice guidance on how to implement the principles of open disclosure. 4. To provide information and training via case scenarios and role play on delivering on the principles of open disclosure

HSE | Open Disclosure 5. To demonstrate the benefits for patients/service users, their families and staff. 6. To practice the key skills required when engaging in open disclosure discussions. 7. To explore the key components involved in the open disclosure process. 8. To update attendees on current and pending legislation. 9. To provide awareness on the resources available.

HSE | Open Disclosure and Empathy www. youtube. com/watch? v=c. DDWvj_q-o 8

HSE | Open Disclosure Part 2 An Overview of Open Disclosure

HSE | Open Disclosure The reality of poor communication “Our family did not get open disclosure. We felt excluded and badly treated and none of the undertakings to give us answers were honoured. We pursued the legal route for three years but that was fraught with lack of conclusions and we feared for our financial security”.

HSE | Open Disclosure Meaning of Patient Safety Incident (Civil Liability Amendment Act 2017) “An incident which occurs during the course of the provision of a health service” which: (a)has caused an unintended or unanticipated injury, or harm, to the patient (b) did not result in actual injury or harm to the patient but was one which the health services provider has reasonable grounds to believe placed the patient at risk of unintended or unanticipated injury or harm or (c) unanticipated or unintended injury or harm to the patient was prevented, either by “timely intervention or by chance”, but the incident was one which the health services provider has reasonable grounds for believing could have resulted in injury or harm, if not prevented. Therefore a patient safety incident includes harm events, no harm events and near miss events.

HSE | Open Disclosure Meaning of Open Disclosure of a Patient Safety Incident (CLA Act 2017) Open disclosure is where a health services provider discloses, at an open disclosure meeting, to— • a patient that a patient safety incident has occurred in the course of the provision of a health service to him or her • a relevant person that a patient safety incident has occurred in the course of the provision of a health service to the patient concerned, or • a patient and a relevant person that a patient safety incident has occurred in the course of the provision of a health service to the patient.

HSE | Open Disclosure Definition of Open Disclosure The HSE defines Open Disclosure as: “an open, consistent, compassionate and timely approach to communicating with patients and, where appropriate, their relevant person following patient safety incidents. It includes expressing regret for what has happened, keeping the patient informed and providing reassurance in relation to on-going care and treatment, learning and the steps being taken by the health services provider to try to prevent a recurrence of the incident”. (HSE 2019)

HSE | Open Disclosure What is Open Disclosure? Open disclosure describes the way staff communicate with patients who have experienced harm during health care – this harm may or may not be as a result of error/failure Open disclosure is a discussion and an exchange of information that may take place in one conversation or over one or more meetings

HSE | Open Disclosure The Events that Trigger Open Disclosure • Harm events: Always disclose • Suspected Harm Events: Always disclose • No Harm Events: Generally disclose. Rationale – how can you ensure that harm has not occurred if you don’t talk to the patient? • Near Miss Events: Assess on a case by case basis – if potential for future harm always disclose.

HSE | Open Disclosure The Irish National Adverse Event Study 2009 – published 2016 • 1574 patients (53% women) – 8 hospitals • The prevalence of adverse events in admissions was 12. 2% • Over 70% of events were considered preventable. • Two-thirds were rated as having a mild-to-moderate impact on the patient, 9. 9% causing permanent impairment and 6. 7% contributing to death. (An adverse event is an incident that resulted in harm that may or may not be the result of error) (Reference: The Irish National Adverse Events Study (INAES): the frequency and nature of adverse events in Irish hospitals —a retrospective record review study Natasha Rafter, Anne Hickey, Ronan M Conroy, Sarah Condell, Paul O'Connor, David Vaughan, Gillian Walsh, David J Williams)

HSE | Open Disclosure CARE COMPASSION TRUST LEARNING KINDNESS EMPATHY

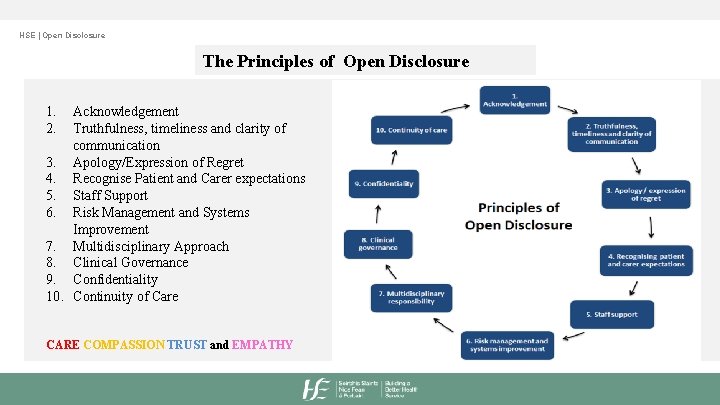
HSE | Open Disclosure The Principles of Open Disclosure 1. 2. Acknowledgement Truthfulness, timeliness and clarity of communication 3. Apology/Expression of Regret 4. Recognise Patient and Carer expectations 5. Staff Support 6. Risk Management and Systems Improvement 7. Multidisciplinary Approach 8. Clinical Governance 9. Confidentiality 10. Continuity of Care CARE COMPASSION TRUST and EMPATHY

HSE | Open Disclosure What does open disclosure involve? Open disclosure involves: • A process of open, honest, transparent and timely communication with patients and/or their relevant person following a patient safety incident • An acknowledgement and factual explanation in relation to what has happened and how/why it happened • Providing a meaningful apology or expression of regret • Demonstrating Empathy and Compassion towards all those involved in the patient safety incident • Listening to the patient and/or their relevant person and hearing their story • Providing reassurance in relation to on going care and treatment, learning and quality improvement

HSE | Open Disclosure Exercise 1: Discussion What are the skills involved in effective open disclosure?

HSE | Open Disclosure Exercise 2: Just Culture What are the cultural changes required to implement effective Open Disclosure? “A just culture is an environment which seeks to balance the need to learn from mistakes and the need to take disciplinary action. (HSE Incident Management Framework 2018)

HSE | Open Disclosure Part 3 Open Disclosure The Drivers

HSE | Open Disclosure Our Natural Instinct “Open disclosure represents the best of Irish healthcare. I think our instinct is to be open with patients and open disclosure guides staff to do what they know is right even in difficult circumstances when an error has occurred” Dr Philip Crowley: National Director of Quality Improvement HSE QID January 2018

HSE | Open Disclosure: The right thing to do • Open disclosure is the professional, ethical and human response to patients involved in/affected by patient safety incidents • It is what patients want and expect • It is what we would expect for ourselves or a loved one • Learning from past experiences

HSE | Open Disclosure: The Drivers 1. HSE Policy/Incident Management/YSYS 2. Professional and Regulatory • NMBI - code • Medical Council - code • HIQA - standards • CORU - code • Mental Health Commission • Pre Hospital Emergency Care Council • Pharmaceutical Society of Ireland (PSI) - code

HSE | Open Disclosure: 3. The Department of Health: Government Policy/Code of conduct for staff (2018) 4. Indemnifying Bodies: SCA/MPS/MDU/MEDISEC 5. Royal Colleges: RCSI, RCPI, ICO, ICGP, Faculty of Radiologists 6. WHO 7. Media

HSE | Open Disclosure Part 4 Open Disclosure Legal considerations and Legislation

HSE | Open Disclosure • Culture: Historic Medical Culture of Non disclosure • Institutional Barriers: “Blame and Shame” approach – no institutional support or mechanisms to facilitate disclosure • Feelings of Shame & Embarrassment • Fear of litigation • Fear concerning professional advancement • Fear with regard to reputation

HSE | Open Disclosure Why disclosure can be difficult • Fear of being reported to professional body • Fear of the Media • Fear of the patient’s/family’s response • Financial concerns • Uncertainty with regard to extent of information to be disclosed • Lack of training and guidance for healthcare professionals

HSE | Open Disclosure Why do patients sue • To get answers • The need for acknowledgement and apology • Patients felt rushed • Felt less time spent/ignored • The attitude of staff • Patients wanted their perceptions of the event/their story validated

HSE | Open Disclosure Why do patients sue? • The experience of “second harm” – poor or no communication after the patient safety incident occurred • To seek financial compensation • To enforce accountability • To correct deficient standards of care • To try to prevent a recurrence of the incident

HSE | Open Disclosure Impact of Open Disclosure on Litigation University of Michigan Health System 2002, Adopted full disclosure policy. Moved from, “Deny and defend” to “Apologise and learn when we’re wrong, explain and vigorously defend when we’re right and view court as a last resort” August 2001 -August 2007 Ratio of litigated cases : total reduced from 65 -27%. Average claims processing time reduced from 20. 3 months to 8 months. Insurance reserves reduced by > two thirds. Average litigation costs more than halved. Savings invested into patient safety initiatives

HSE | Open Disclosure Protective legislative provisions in Part 4 of the Civil Liability Amendment Act 2017 (CLA Act) – Commenced in September 2018 1. Open disclosure: (a) shall not constitute an express or implied admission of fault or liability (b) shall not, notwithstanding any other enactment or rule of law, be admissible as evidence of fault or liability and (c) shall not invalidate insurance or otherwise affect the cover provided by such policy

HSE | Open Disclosure 2. Information provided, and an apology where it is made, shall not (a) constitute an express or implied admission, by a health practitioner, of fault, professional misconduct, poor professional performance, unfitness to practice (b) be admissible as evidence of fault, professional misconduct, poor professional performance, unfitness to practise, in proceedings to determine a complaint, application or allegation

HSE | Open Disclosure • Part 4 of the CLA Act 2017 relates to voluntary open disclosure • There are 8 regulations that accompany Part 4 of the CLA Act 2017 • Staff can opt to seek the protective provisions of the Act or not. • To avail of the protective provisions within Part 4 of the Act open disclosure must be managed strictly in accordance with the procedure as set out within the Act and the regulations that accompany Part 4 of the Act • The protections of the Act will be automatic when OD is managed as per the procedure set out in Part 4 of the Act

HSE | Open Disclosure In addition to the HSE Policy requirements: • The relevant prescribed statements (forms) must be prepared and signed by the health services provider and provided to the patient/relevant person, as appropriate. • A copy of all forms must be kept on record by the health services provider – in a file separate to the clinical/care record • The name of the designated person (key contact person) must be documented in a file separate to the healthcare record e. g. OD file/Incident Management File

HSE | Open Disclosure There are 8 regulations The regulations take the form of prescribed statements which staff are obliged to • Complete • Sign (signed by principal health care practitioner or another person deemed appropriate by the health services provider) • Provide (relevant forms) to patients as set out in the procedure • Maintain on record in a file separate to the healthcare record e. g. OD file or incident management file

HSE | Open Disclosure Form A - Statement of Information Provided at an Open Disclosure Meeting Form B - Statement of Non-Attendance patient or Relevant Person at open disclosure meeting Form C - Statement of Non-Attendance patient and relevant person at open disclosure meeting Form D - Refusal to accept Statement Form E - Statement of Additional Information Form F - Request for Clarification Meeting Form G - Statement of Clarification of Information Form H - Statement of Steps Taken to Establish Contact Available: https: //www. hse. ie/eng/about/who/qid/other-qualityimprovement-programmes/opendisclosure-legislation/civil-liability-forms. html

HSE | Open Disclosure “A Bill to provide for mandatory open disclosure of serious reportable patient safety incidents, notification of reportable incidents, clinical audit to improve patient care and outcomes and extend the Health Information Quality Authority remit to private health services” (Department of Health 5 July 2018) Note: The progress of the 2019 Bill can be followed on the Oireachtas website: https: //www. oireachtas. ie/en/bills/bill/2019/100/

HSE | Open Disclosure The Patient Safety Bill List of Current Notifiable Incidents (14 in total) (Summary) Note: The Minister reserves the rights to make further regulations (additions to current list of notifiable incidents) 1. Unintended and unanticipated patient death which did not arise from/was a consequence of an illness/underlying condition q Following wrong patient surgery q Following wrong site surgery q Following wrong surgical procedure q Following unintended retention of foreign object q Following elective surgery q Directly related to treatment q Due to transfusion of incompatible blood or blood components q Associated with medication error q Death of a woman while pregnant or within 42 days of delivery q Still born child born without foetal abnormality at prescribed gestational age/birth weight not related to underlying condition of the child q Perinatal death of a child who was alive at the onset of care in labour who had reached a prescribed gestational age and a prescribed birth weight q Suicide of patient while being cared for at a place or premises where care is being provided 2. Baby referred for therapeutic hypothermia or considered for and did not undergo therapeutic hypothermia.

HSE | Open Disclosure The Patient Safety Bill Communication Record Written information to be provided to the patient and/or the relevant person. • Give the patient and/or the relevant person a copy of the statement, as appropriate, in writing at the meeting or not later than five days from the date on which the meeting was held. • Health service provider to maintain a copy of this statement on record.

HSE | Open Disclosure Patient Safety Bill – Part 7 Offences • A person who fails to comply without a reasonable excuse shall be guilty of an offence and shall be liable on summary conviction to a Class A fine (Fine may vary up to € 5000) • The above relates to failure to hold an open disclosure meeting and/or to report the patient safety incident to the Relevant Authority e. g. HIQA, Chief Inspector, Mental Health Commission

HSE | Open Disclosure Legal Services Regulations Act 2015 This act (not yet commenced) contains the following protections for an apology in clinical negligence claims: (1) An apology made in connection with an allegation of clinical negligence— (a) shall not constitute an express or implied admission of fault or liability, and (b) shall not, despite any provision to the contrary in any contract of insurance and despite any other enactment, invalidate or otherwise affect any insurance coverage that is, or but for the apology would be, available in respect of the matter alleged. (2) Despite any other enactment, evidence of an apology referred to in subsection (1) is not admissible as evidence of fault or liability of any person in any proceedings in a clinical negligence action.

HSE | Open Disclosure Part 5 The Patient Perspective

HSE | Open Disclosure Exercise 3 • Watch the DVD – (approximately 4 -5 minutes) • Focus on the patient – Mrs Ling • As you are watching it think about what the patient’s needs are. • What does the patient require/expect from her GP during the consultation? • What does the patient expect following the consultation in relation to her on-going care?

HSE | Open Disclosure A – Acknowledge – problem and impact S – Sorry – express regret S – Story – hear patient’s story and summarise back to them I – Inquire – seek questions to be answered, provide answers, give information S – Solution – seek patient’s ideas on the way forward – agree a plan T – Travel – avoid abandonment – continued care – increased contact.

HSE | Open Disclosure Honesty Respect Empathy To be informed about their situation Dedicated attention by someone who is knowledgeable about it To have their questions answered in language Professionalism they understand Competent, efficient service To be listened to (and heard) To be updated in a timely manner Basic courtesy / friendliness To be taken seriously Follow-through 1. A timely and comprehensive explanation of what happened and why 2. Someone to acknowledge and apologise if things went wrong 3. A reassurance that steps have been taken to ensure the event will not happen again

HSE | Open Disclosure

HSE | Open Disclosure “Open disclosure is not about blame. It is not about accepting the blame. It is not about apportioning blame. It is about integrity and being truly professional And the reason: You hold our lives in your hands and we, as patients, want to hold you in high regard. ” (Mrs Margaret Murphy)

HSE | Open Disclosure Exercise 4: Open Disclosure using the ASSIST Model of Communication Watch the DVD – same scenario as before (Exercise 1) GP consultation now using the A. S. S. I. S. T model Record the terminology used by the Dr which applied to the various components of the A. S. S. I. S. T model.

HSE | Open Disclosure • Read the case scenario provided. • In your allocated groups of three you will take turns in playing the role of (a) Doctor, (b) Patient and (c) Observer • You will be allocated 5 minutes for each role play. • Do not be concerned if you have not completed the consultation. • At the end of 5 minutes provide feedback on the consultation using the A. S. S. I. S. T Model. • You will then swap roles. • There will be a general feedback session at the end of the session when all three persons have experienced the role of the Doctor, Patient and Observer.

HSE | Open Disclosure Part 6 The Clinicians Perspectives and Considerations

HSE | Open Disclosure • Watch the DVD • Consider the feelings and emotions of the doctor whose patient is being referred to by their medical colleague. • Consider that you are this doctor. • Write down all the feelings you may be experiencing and your possible reactions to this conversation.

HSE | Open Disclosure The six recognised stages of staff reaction following an adverse event 1. Chaos: Error realised and recognised. How and why did it happen. Care for the patient. 2. Intrusive reflections: Re-evaluate the event. Haunted re-enactments of the event. Self isolation. 3. Restoring personal integrity: Managing gossip Questioning trust. Fear. 4. Enduring the inquisition: Realisation of seriousness. Wonder about repercussions. Who can I talk to? 5. Obtaining emotional first aid: Seeking personal and professional support. Where can I turn to for help?

HSE | Open Disclosure The six recognised stages of staff reaction following an adverse event: 6. Moving On—Dropping Out, Surviving or Thriving: Despite a desire to move on, many professionals find it difficult to do so. This stage has three potential paths: • Dropping Out—changing professional role, leaving the profession or moving to a different practice location. • Surviving—performing at the expected performance levels (“doing OK”) but continue to be affected by the event. • Thriving—making something good out of the adverse event.

HSE | Open Disclosure Benefits for Staff • Improved staff recovery • It encourages a culture of honesty and openness. • Staff are more willing to learn from patient safety incidents • It enhances management and clinician relationships • It leads to better relationships with patients and their relevant persons • Maintains personal and professional integrity • Lightens the burden of guilt • Allows for reflective learning

HSE | Open Disclosure Provides information for staff on: • The potential normal reactions to what is an abnormal event • How to help yourself • How to support a colleague /peer using the ASSIST ME model • Advice on when to seek professional assistance i. e. GP/EAP/OH

HSE | Open Disclosure A – Acknowledge – what has happened and the impact on staff member S – Sorry – express regret for their experience S – Story –allow the staff member time to talk about what has happened - listen and summarise back to them I – Inquire – seek questions to be answered, do not go into investigative mode - provide answers, give information S – Solution – Talk about next steps – the management of the patient and event – seek their ideas/suggestions – agree a plan – check if they are ok to remain at work T – Travel – maintain communication and support – check in regularly avoid abandonment – continued care M – Monitor - monitor their progress E - Evaluate – talk to the staff about their experience of the process End - close the process when staff member feels ready – open door

HSE | Open Disclosure • Employing organisation: Work Colleagues/Peers/Managers/OD Lead • GP • EAP/Occupational Health/CISM • Indemnifying bodies/Royal Colleges • The HSE Policy for Preventing and Managing Critical Incident Stress 2012 developed by the National Health and Safety Advisers Group. • The HSE and State Claims Agency staff support booklet 2013: Supporting staff following an adverse event: The “ASSIST ME” model See Appendix B of Workbook for a list of Resources

HSE | Open Disclosure Part 7 The Disclosure Process

HSE | Open Disclosure Levels of Disclosure Criteria for determining the appropriate level of response Low level Response: A low level response is usually initiated for patient safety Incidents where there has been no harm to the patient or the harm to the patient is minimal – this level of response may involve just one meeting with the patient (i. e. Category 3 incidents as per the HSE Risk Impact Table ). High Level Response: A high level response involves the full open disclosure process and will usually be initiated for patient safety incidents where the patient has suffered a moderate or higher level of harm (i. e. Category 1 and Category 2 Incidents as per HSE Risk Impact Table)

HSE | Open Disclosure Preparation for Open Disclosure: • A preliminary MDT discussion with all necessary stakeholders to establish the known facts • Consider if the protections of the CLA Act are being sought and refer to CLA open disclosure procedure • To establish the facts takes time, not all facts need to be established prior to meeting the patient/relevant person • Think ahead and plan responses to questions that may arise • Consider if an apology is required and the wording of such apology • Consider who will make the open disclosure and who the open disclosure will be made to • Agree OD Team • Appointment of the designated person /key contact person– name documented • Consider if additional supports are required? e. g. interpreter, assisted decision making, patient advocate • Prepare documentation e. g. checklist, (CLA forms if legal protections sought)

HSE | Open Disclosure Does the CEO/GM know that a disclosure meeting is happening. . ? Should they be there? Are there any other members of the healthcare team that need to know e. g. • • • Clinical Director of Nursing Allied Healthcare Public Health Microbiologist/Radiologist

HSE | Open Disclosure • Lead Discloser – Ideally the principal healthcare practitioner involved e. g. Consultant or another staff member deemed appropriate by the health services provider • Deputy Discloser – To assist, ensure patient/ relevant person understands – e. g. Registrar, Director of Nursing, CNM • Designated Person/Key Contact q Links with patient/ relevant person q Keeps them informed q Helps patient/relevant person prepare for meeting q Meet and Greet q Follow up after meeting • Scribe – Confidential minutes of meeting

HSE | Open Disclosure • Preparation again essential • Designated person to liaise with patient/family • Meet and greet patient/relevant person at pre-determined location • Consideration given to off site meeting • Informal surroundings – consider room layout • Well ventilated room • Refreshments • Bleeps, mobiles off.

HSE | Open Disclosure Information to be Provided at Open Disclosure Meeting q A description of the patient safety incident – an acknowledgement of what happened, when it happened and when/how the patient safety incident came to the attention of the health services provider. q The facts available at the time of the open disclosure meeting – how/why /any known contributing factors. q A description of the actions being taken and the timeframe expected by the health services provider to establish further information q The impact of the patient safety incident on the patient and any known or likely consequences for the patient going forward as a result. q A sincere and meaningful apology (see section 3. 12). q Factual responses to questions/clarifications sought by the patient/their relevant person.

HSE | Open Disclosure Information to be Provided at Open Disclosure Meeting q The actions/measures taken or planned by the health services provider to manage the incident. q The learning identified and the actions taken or planned by the health services provider to try to prevent a recurrence of the incident. q Agreed next steps to include the planned communication process with the patient and/or their relevant person. q The details of the support services available to the patient and/or their relevant person. q The name and contact details for the designated person whom the patient/relevant person can contact directly should they require further information/clarification of any information provided

HSE | Open Disclosure Documentation: • Essential to ensure continuity and consistency • Imperative that details of the patient safety incident are documented in the clinical record including the details of clinical care provided. • The salient points of the open disclosure meeting must be documented in the patient record including the exact wording and context of any apology given. • Documentation of open disclosure on NIMS • Non-clinical communications to be kept in a separate file i. e. risk reviews, minutes of meetings, CLA forms • Refer to pre-during and post documentation checklist in guidelines and on website

HSE | Open Disclosure Disclosing another clinician’s error Consider ethical duty/responsibility Patients and their relevant persons come first - rights to honest, open and transparent communication - compassion - difficulties in disclosure should not stand in the way - ensuring correct clinical management of the patient’s condition Explore – Do not ignore! - turn towards involved colleague - colleague to colleague discussion - obtain the facts – do not rush to judgement - frame the conversation to minimize defensiveness – curiosity as opposed to accusations – manner – body language – tone - establish what happened - discuss and agree the way forward – clinical management - reporting, disclosure, etc. - seek assistance from the organisation if necessary.

HSE | Open Disclosure Deferring Open Disclosure Only in rare and exceptional circumstances would open disclosure not occur – open disclosure is the expected HSE response to patient safety incidents Circumstances when OD may need to be deferred: • The patient and/or their relevant person cannot be contacted. • The patient and/or relevant person refuses open disclosure. • The patient is extremely ill and is unable to participate in an open disclosure meeting. • The clinician has concerns that initiating open disclosure with the patient may put the patient at risk of causing harm to themselves or to others • Consideration must be given in the above circumstances to initiating open disclosure with the patient’s relevant person, where appropriate, taking into consideration matters relating to patient confidentiality and patient consent. • The escalation processes outlined in the HSE policy must be adhered to.

HSE | Open Disclosure Common Pitfalls

HSE | Open Disclosure 1. Patients have the right to have full knowledge about their healthcare and, in particular, have a right to be informed when things go wrong. 2. Patients must be treated with compassion and empathy. 3. A person whose decision-making capacity is in question is entitled to open disclosure on an equal basis with others. 4. Focus first and foremost on the physical needs of the patient through the provision of appropriate medical treatment or other care to manage any harm that has occurred. 5. All “harm” and “suspected harm” events must be disclosed. “No harm” events should generally be disclosed and “near miss” events must be assessed on a case by case basis. If there is a potential for a “no harm” event or “near miss” event to become a “harm” event in the future the patient must be informed.

HSE | Open Disclosure 6. Initiate OD process as soon as possible and as is practicable (ideally within 24 - 48 hours after the event occurs or becomes known 7. Assess the incident and determine level of response required – low level/high level 8. Adequately prepare for an open disclosure meeting by giving due consideration to what has happened and the facts available. 9. The patient must be informed of all the facts available to the health services provider at the time of the open disclosure meeting in relation to the patient safety incident. 10. Provide a sincere and meaningful apology in a timely manner which is personal to the patient and to the given situation.

HSE | Open Disclosure 11. All additional information obtained must be provided to the patient/relevant person in a timely manner and any clarifications sought in relation to information provided responded to openly and honestly. 12. A designated person must be assigned to maintain communication between the health service and patient/relevant person. 13. The salient points of the OD meeting must be documented in the clinical/care record including the details of any apology provided. 14. Appropriate follow up care and communication must be provided 15. The HSE will provide a safe, supportive and caring environment for staff involved in and/or affected by patient safety incidents and ensure that staff access training on the open disclosure policy relevant to their role

HSE | Open Disclosure 16. The deferral of open disclosure must be managed as per the steps set out in the policy. Only in rare and exceptional circumstances would the deferral of open disclosure occur. 17. Disclosure of information to an adult patient’s relevant person must only be undertaken with the consent of the patient, where possible. 18. Effective governance arrangements are required to support timely and effective open disclosure. Primary responsibility and accountability for the effective management of patient safety incidents, including the open disclosure process, remains at organisational level. 19. The health service provider will develop an implementation plan to support the roll out of the OD policy. 20. The implementation of OD policy must be evaluated and audited.

HSE | Open Disclosure Further information • www. opendisclosure. ie • National documents • Resources for clinicians, organisations and trainers • Open disclosure site leads/group leads/CHO leads/NAS Leads • Yammer. com support forum • National Open Disclosure Office Email: opendisclosure. office@hse. ie

HSE | Open Disclosure Faculty of Radiology: Open disclosure guidelines for radiologists 2016 available at http: //www. radiology. ie/wp-content/uploads/2012/05/Open-Disclosure. Faculty-of-Radiologists-V 1. 2 -April-20161. pdf Open Disclosure of Health Care Acquired Infections (HCAI s) 2018 developed by CPE Expert Group available at http: //www. hpsc. ie/az/microbiologyantimicrobialresistance/strategyforthecontrolofantimicrobia lresistanceinirelandsari/carbapenemresistantenterobacteriaceaecre/guidanc eandpublications/Discussing%20 HCAI_AMROs%20 with%20 patients_fin al_2 July 18. pdf

HSE | Open Disclosure Fact: Things go wrong despite our best efforts Patient safety incidents happen to the best people in the best places – none of us are immune. We must be honest with our patients, our colleagues and with ourselves. Learning is difficult where transparency is absent. Transparency must involve an empathic approach to the patients and families, staff and services involved in/affected by patient safety incidents.

HSE | Open Disclosure Contact Details: Email Opendisclosure. office@hse www. hse. ie/opendisclosure

HSE | Open Disclosure Thank you for your time and attention…. any questions ?

HSE | Open Disclosure For further information Full policy and additional resources (including Staff Support Booklet) www. hse. ie/opendisclosure Contact the National Open Disclosure Office Email: opendisclosure. office@hse. ie