Ontwikkelingen op het gebied van integrale zorg een

Ontwikkelingen op het gebied van integrale zorg: een internationaal perspectief Frits Huyse, psychiater Afdeling Algemene Interne Geneeskunde UMCG Deelaanstelling afdeling Psychiatrie VUmc NFZP Utrecht April 2005

Wat doen C-L psychiaters? • Grote variatie tussen praktijken • Consultatieve psychiatrie is: • Reactief • Gebaseerd op de behoeften van dokters en verpleegkundigen • Liaison is theorie maar geen praktijk CONSULTATIEVE ACUTE is gelijk aan PSYCHIATRIE Huyse e. a. Gen Hosp Psychiatry 23(3): 124 -132, 2001 PSYCHIATRIE 11 Europese landen 56 C-L PCD’s 14. 700 patienten


Depression—A Major Cause of Disability Worldwide DALYs— 2000 and 2020 Rank 20001 2020 (Estimated)2 1 Lower respiratory infections Ischemic heart disease 2 3 Perinatal conditions HIV/AIDS Unipolar major depression Road traffic accidents 4 5 Unipolar major depression Diarrheal diseases Cerebrovascular disease Chronic obstructive pulmonary disease 1. World Health Report 2001. Mental Health: New Understanding, New Hope. Geneva, World Health Organization, 2001. 2. Murray CJL, Lopez AD, eds. The Global Burden of Disease. Boston: Harvard University Press; 1996. DALYs=disability-adjusted life-years.

Prevalence of Mental Disorders in Non. Psychiatric Setting Major Depression Community Primary Care General Hospital Setting 5. 1% 5 -14% >15% Panic/GAD 4. 2% 11% 4. 5% Somatization 0. 2% 2. 8%-5% 2%-9% Substance Abuse 6. 0% 10%-30% 20%-50% Any Disorder 18. 5% 21%-26% 30%-60% Carthesian solutions Kathol 2002 2 x


Ontwikkelingen in de gezondheidszorg Somatiek uit GGZ Psychiatrie uit AGZ • 1970 – splitsing neurologie/psychiatrie • Geen systematische somatische opleiding – Deinstitutionalisering • Somatiek verdwijnt uit GGZ • 1990 – MFE vorming • PAAZ verdwijnt uit algemeen ziekenhuis (>50%) – AWBZ • Financiering voor consulten en comorbiditeit verdwijnt

Interdisciplinaire Opleidingen Een kans voor Interne Geneeskunde en Psychiatrie? ROB Gans Hoogleraar Interne UMCG VJC NVv. P Amsterdam, April 4, 2003 Thisbee en ….

INTERNATIONALE VOORBEELDEN • Stepped/shared care modellen • USA/Canada • Psychosomatische model • Duits • The Extended Reattribution Model • Denemarken

HAMILTON MODEL SHARED CARE Nick Kates Models of integrated care APM Frt Myers 2005

The Hamilton Model • • 80 Family physicians 40 practices 1 -6 physicians in each Funded by capitation Each has a counsellor permanently attached 1 full time counsellor / 8, 000 patients Psychiatrist visits each practice ½ day of psychiatrist time per family physician a month

The Hamilton Model : Training Residents • Mc. Master University – 5 year program – 1 st year general medical training – 30 residents in program • Program includes: – Seminars during training – Visits to primary care – Participate in seminars with family medicine residents Somatiek geïntegreerd; interdisciplinaire vorming gegarandeerd

The Hamilton Model : Training Residents • Primary care visits – Residents visit practices with their supervisor – Usually 1 -2 half days a week, during an out-patient rotation - can be child or geriatric – Observe their supervisor seeing cases – Supervisor observes them seeing cases – See collaboration between psychiatrist and family physician being modelled – See a broad range of cases – more than any clinic

Benefits to residents • • Learn about primary care See collaboration modelled Develop specific consultation skills Appreciation of how the rest of the world sees psychiatry • Can follow-up cases after a consultation

Outcomes • Highly rated / popular rotation • Residents highly satisfied with time spent in primary care • Residents also participate in research projects on primary mental health care • Many graduates incorporate this as part of their practice

Kenmerk Hamilton model • Psychiatrie in de huisartsen praktijk • Shared care gebaseerd op effectiviteit van psychiatrische behandelingen

Stepped/shared care modellen Wayne Katon Hackett award lecture APM San Diego 2003 Kurt Kroenke MD Regenstrief Institute Indiana University School of Medicine

Depression—A Major Cause of Disability Worldwide DALYs— 2000 and 2020 Rank 20001 2020 (Estimated)2 1 Lower respiratory infections Ischemic heart disease 2 3 Perinatal conditions HIV/AIDS Unipolar major depression Road traffic accidents 4 5 Unipolar major depression Diarrheal diseases Cerebrovascular disease Chronic obstructive pulmonary disease 1. World Health Report 2001. Mental Health: New Understanding, New Hope. Geneva, World Health Organization, 2001. 2. Murray CJL, Lopez AD, eds. The Global Burden of Disease. Boston: Harvard University Press; 1996. DALYs=disability-adjusted life-years.

Depression Is Often Underdiagnosed and Inadequately Treated • Less than 1/2 of patients with major depression are explicitly recognized as being depressed 1 • Only about 1/2 of all depressed patients receive some form of therapy for their illness 2 • Only about 1/4 of depressed patients receive an adequate dose and duration of antidepressant treatment 3 1. AHCPR. Rockville, Md: US Dept of Health and Human Services; 1993. Publication 93 -0550. 2. Lepine JP, et al. Int Clin Psychopharmacol. 1997; 12(1): 19 -29. 3. Katon W, et al. Med Care. 1992; 30(1): 67 -76.
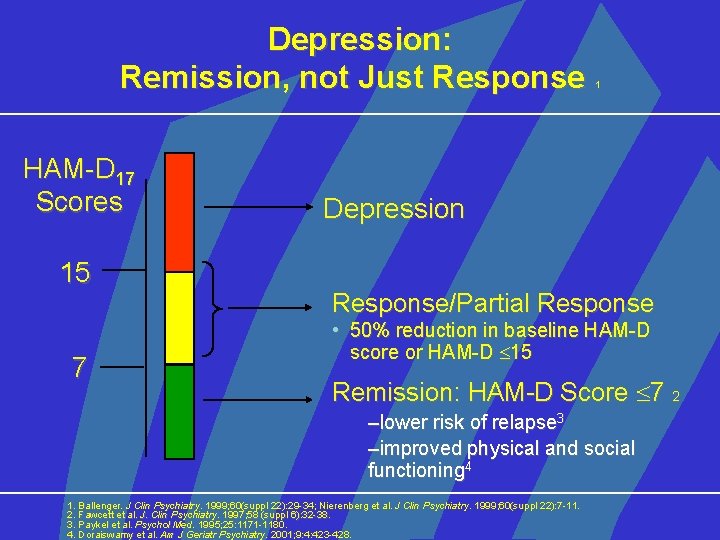
Depression: Remission, not Just Response HAM-D 17 Scores 15 7 1 Depression Response/Partial Response • 50% reduction in baseline HAM-D score or HAM-D 15 Remission: HAM-D Score 7 2 –lower risk of relapse 3 –improved physical and social functioning 4 1. Ballenger. J Clin Psychiatry. 1999; 60(suppl 22): 29 -34; Nierenberg et al. J Clin Psychiatry. 1999; 60(suppl 22): 7 -11. 2. Fawcett et al. J. Clin Psychiatry. 1997; 58 (suppl 6): 32 -38. 3. Paykel et al. Psychol Med. 1995; 25: 1171 -1180. 4. Doraiswamy et al. Am J Geriatr Psychiatry. 2001; 9: 4: 423 -428.

Simon GE

Stepped/shared care modellen: bij patienten met onbegrepen klachten en depressiviteit Kurt Kroenke MD Regenstrief Institute Indiana University School of Medicine

Stepped Care 1. 2. 3. 4. Patient self-management Primary care provider Care manager Collaborative care – Indirect (TCM) – MHS supervises CM – Direct – MHS sees pt in consultation 5. Referral to Mental Health Specialist PC MH
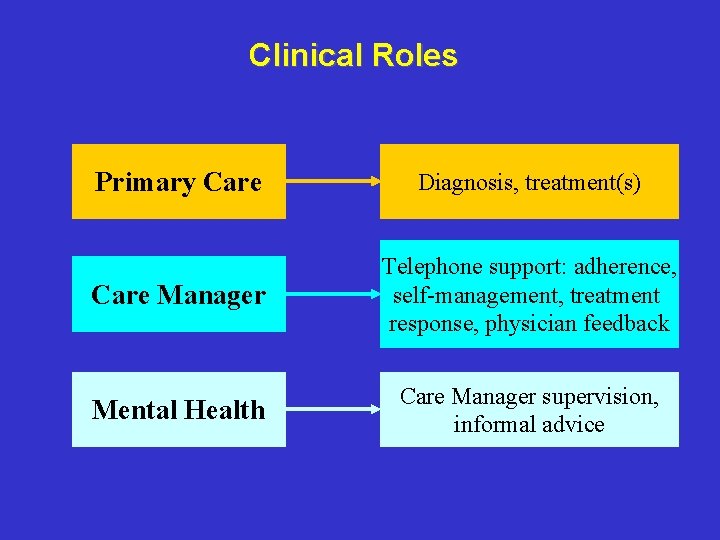
Clinical Roles Primary Care Diagnosis, treatment(s) Care Manager Telephone support: adherence, self-management, treatment response, physician feedback Mental Health Care Manager supervision, informal advice

PHQ-9 A New Depression Tool

Measuring Disease Common Metrics DISEASE MEASURE Hypertension Sphygmomanometer Diabetes Glucometer Asthma Peak flow meter Depression PHQ-9

PHQ-9 Depression Measure • Consists of the 9 DSM-IV depressive symptoms, each scored 0 to 3 • • Validated in 6000 patients (3000 primary care and 3000 ob-gyn) • Diagnostic, severity, & monitoring tool • Widely used in research & clinical care • PHQ-2 version valid for screening Kroenke, JGIM 2001; Kroenke & Spitzer, Psychiatric Annals 2002

Not at all Several days More than half the days 0 1 2 PHQ - 9 1. Over the last 2 weeks, how often have you been bothered by the following problems? Nearly all days 3 a. Little interest or pleasure in doing things b. Feeling down, depressed, or hopeless c. Trouble falling or staying asleep, or sleeping too much d. Feeling tired or having little energy e. Poor appetite or overeating f. Feeling bad about yourself, or that you are a failure. . . g. Trouble concentrating on things, such as reading. . . h. Moving or speaking so slowly. . . i. Thoughts that you would be better off dead. . . Subtotals: 3 4 TOTAL = 16 9

PHQ-9 as Severity Measure • Cutpoints proposed on PHQ-9 for depression severity are: 5 = mild 10 = moderate 15 = moderately severe 20 = severe • Response to therapy = 5 point ↓ • Remission = score < 5
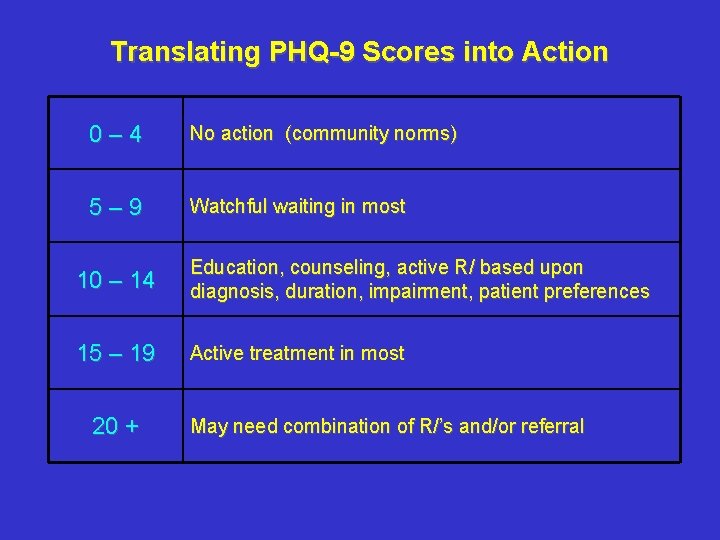
Translating PHQ-9 Scores into Action 0– 4 No action (community norms) 5– 9 Watchful waiting in most 10 – 14 Education, counseling, active R/ based upon diagnosis, duration, impairment, patient preferences 15 – 19 Active treatment in most 20 + May need combination of R/’s and/or referral

Stepped Care 1. 2. 3. 4. Patient self-management Primary care provider Care manager Collaborative care – Indirect (TCM) – MHS supervises CM – Direct – MHS sees pt in consultation 5. Referral to Mental Health Specialist PC MH

Stepped/shared care modellen Wayne Katon Hackett award lecture APM San Diego 2003

Depression: Impact in Patients with Medical Illness Wayne Katon, M. D.
Major Depression Prevalence: Chronic Medical Illness • Heart Disease 15 to 23% • Diabetes 11 to 12% • COPD 10 to 20%

Prevalence of Major and Minor Depression in Patients with Diabetes • 14. 2% major depression, 8. 7% minor depression (2059 females) • 9. 2% major depression, 8. 3% minor depression (2166 men) • Totals: – 12% major depression – 8. 5% minor depression

Depression and Chronic Medical Illness • Increased prevalence of major depression in the medically ill • Depression amplifies physical symptoms associated with medical illness • Comorbidity increases impairment in functioning • Depression decreases adherence to prescribed regimens • Depression is associated with adverse health behaviors (diet, exercise, smoking) • Depression increases mortality
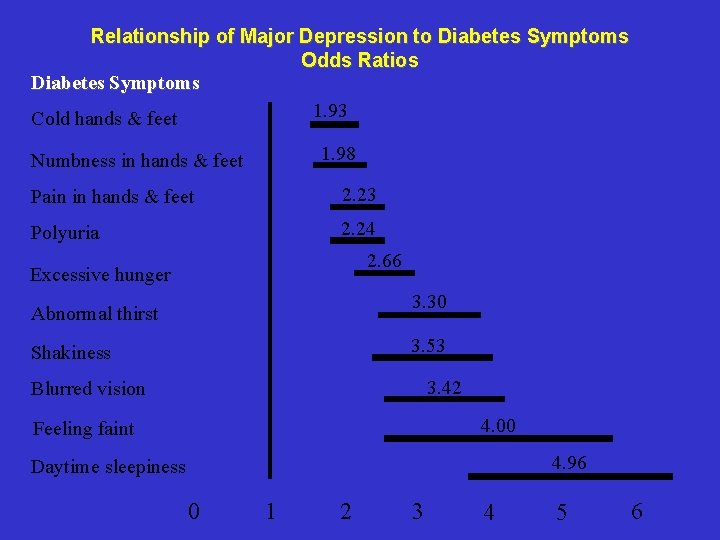
Relationship of Major Depression to Diabetes Symptoms Odds Ratios Diabetes Symptoms 1. 93 Cold hands & feet 1. 98 Numbness in hands & feet Pain in hands & feet 2. 23 Polyuria 2. 24 2. 66 Excessive hunger 3. 30 Abnormal thirst 3. 53 Shakiness 3. 42 Blurred vision 4. 00 Feeling faint 4. 96 Daytime sleepiness 0 1 2 3 4 5 6

Depression and Hb. A 1 C • Meta-analysis of 24 studies showed a significant association between depression and Hb. A 1 c • Effect sizes were in the small to moderate range (0. 17, 95% CI 0. 13 – 0. 21) Lustman et al, Diabetes Care, 2000
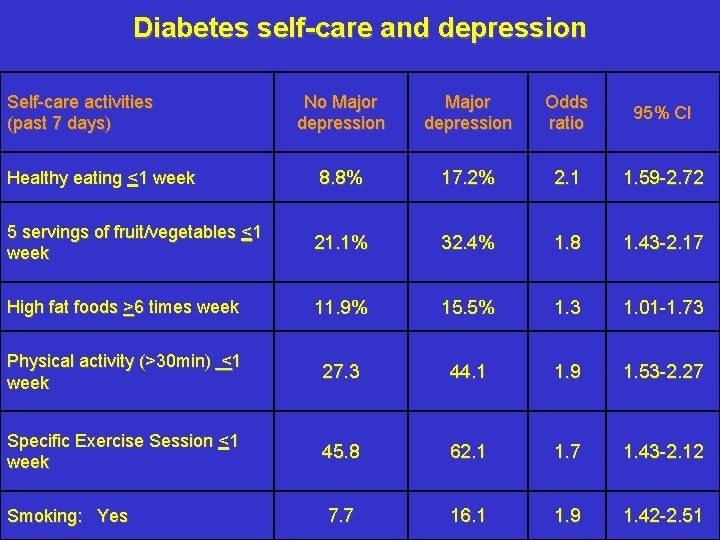
Diabetes self-care and depression Self-care activities (past 7 days) No Major depression Odds ratio 95% CI Healthy eating <1 week 8. 8% 17. 2% 2. 1 1. 59 -2. 72 5 servings of fruit/vegetables <1 week 21. 1% 32. 4% 1. 8 1. 43 -2. 17 High fat foods >6 times week 11. 9% 15. 5% 1. 3 1. 01 -1. 73 Physical activity (>30 min) <1 week 27. 3 44. 1 1. 9 1. 53 -2. 27 Specific Exercise Session <1 week 45. 8 62. 1 1. 7 1. 43 -2. 12 Smoking: Yes 7. 7 16. 1 1. 9 1. 42 -2. 51
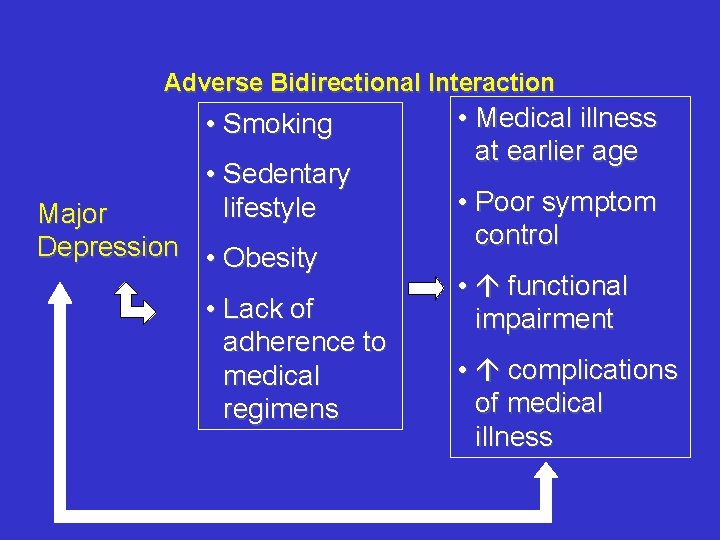
Adverse Bidirectional Interaction • Smoking • Sedentary lifestyle Major Depression • Obesity • Lack of adherence to medical regimens • Medical illness at earlier age • Poor symptom control • functional impairment • complications of medical illness

Stepped Care Models: 3 Assumptions Von Korff et al. , 1999 1) Different people require different levels of care 2) Finding the best level of care depends on monitoring outcomes 3) Moving from lower to higher levels of care based on observed outcomes can increase effectiveness while lowering overall costs Caveats: Patient preferences and initial clinical complexity need to be taken into account Wayne Katon Hackett award lecture APM San Diego 2003

Modellen Katon “Seattle group” • Shared en stepped care gestuurd door behandel uitkomsten • Focus naast depressie op compliance met therapie voor somatische ziekte • “The Pathways Study”Katon ea Arch Gen Psychiatry 2004; 61: 1042 -1049

Psychosomatische model

EACLPP Successful models of integrated care: the psychosomatic model in the German speaking countries EACLPP Wolfgang Söllner (Nuremberg/Germany), Thomas Herzog (Göppingen/Germany) Academy of Psychosomatic Medicine November 2003, San Diego

Special development in Germany • Own specialization „Psychosomatic medicine and psychotherapy“ • Special health care units • Special training for students, doctors with other specializations and nurses • Research focus on the interface between physiology and psychology Why Germany? • Theoretical foundation (paradigm) • Historical and socioeconomic development • Empirical research

1 Counter-movements against the biotechnological paradigm • The biotechnological paradigm: „Machine-model of the body“ • Holostic countermovement in internal medicine (Krehl, Siebeck, v. Bergmann, v. Weizsäcker); „introduction of the subject“ • Psychogenic countermovement: Psychoanalysis introduced the subject of the physician • Ψ meets anthropological medicine; psychiatry stood aside
2 The legacy of national socialism • Necessity to cope with terrible crimes and inhuman practices in medicine during NS. • Intellectual isolation and paralysis after 1945. • Alexander Mitscherlich: „Medicine without humanity“ • „Loss of empathy“ should be compensated. Holistic approaches supported.

Development of psychosomatic medicine in the 60 -ies • The holistic paradigm of psychosomatic medicine (Thure von Uexküll) • The bio-psycho-social paradigm (George Engel) • Paradigm of object relations in medicine: the key-role of the doctorpatient-relationship in medicine (Michael Balint) • The Dührssen study: Implementation of C-L services & psychosomatic wards in the GH
Aims of psychosomatic medicine Patient care C-L Research Education Patient care: • bio-psycho-social diagnosis • Detect and treat psych. comorbidity • emphasis on psychotherapeutic treatment for the medically ill Research: • focus on the interface between physiology and psychology Education: • enhance the psycho-social attitudes and skills of medical students, physicians and nurses (holistic approach)
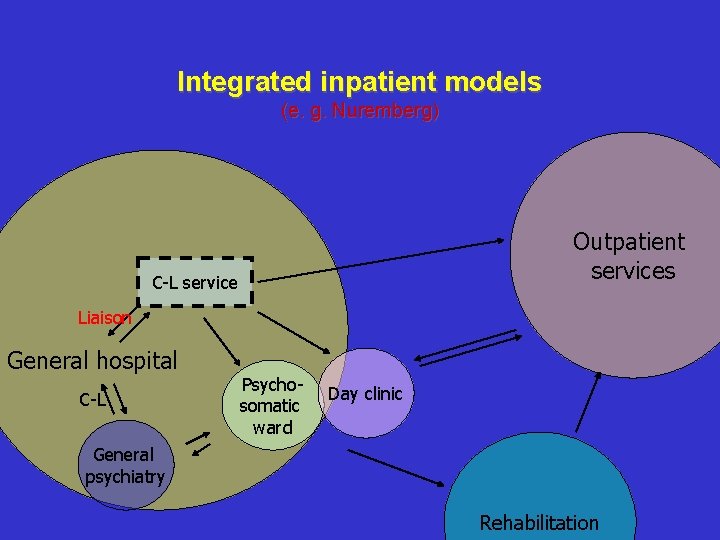
Integrated inpatient models (e. g. Nuremberg) Outpatient services C-L service Liaison General hospital C-L Psychosomatic ward Day clinic General psychiatry Rehabilitation

Inpatient models type A: Integrated psychosomatic ward Two models: • A 1: Head representing both disciplines (e. g. Heidelberg, Stuttgart) • A 2: Interdisciplinary ward, 2 heads (Nuremberg) Physicians: specialists and residents in internal medicine and in PSO Common nursing staff (special training) Additional staff: physiotherapist, art therapist, social worker • Case conferences: common treatment plan • Balint group • Common further education

Education of physicians: „Basic psychosomatic care“ 80 -hour courses • 30 hrs communication skills training and relaxation techniques • 20 hrs psychosomatic theory • 30 hrs Balint group • mandatory for residents in general/internal medicine and obstet/gynecol • Supportive verbal interactions and relaxation techniques are payed by insurances additionally if physicians performed such training (maximum of 12 sessions of 20 minutes duration)
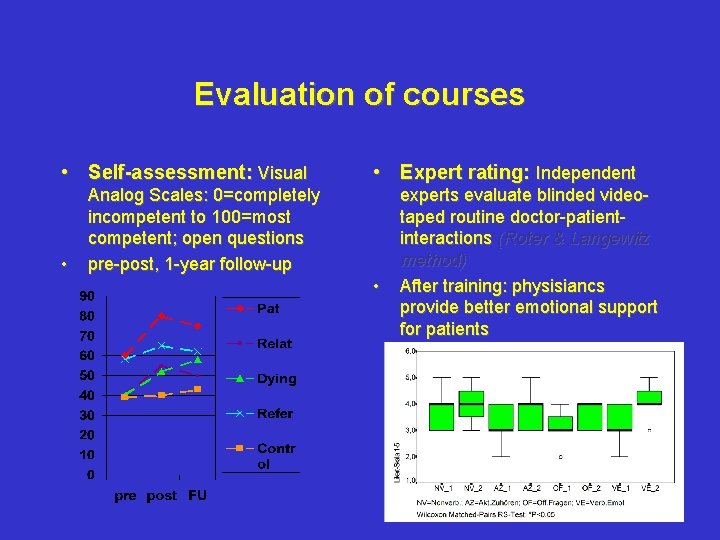
Evaluation of courses • Self-assessment: Visual • • Expert rating: Independent Analog Scales: 0=completely incompetent to 100=most competent; open questions pre-post, 1 -year follow-up • experts evaluate blinded videotaped routine doctor-patientinteractions (Roter & Langewitz method) After training: physisiancs provide better emotional support for patients

The Extended Reattribution Model (TERM) Per Fink, MD, Ph. D, Dr. Med. Sc. The Research Unit for. Functional Disorders Psychosomatics and CL psychiatry Arhus Univerity Hospital Danmark
- Slides: 54