ONCOLOGY NURSE COMPASSION FATIGUE INTERVENTION EVIDENCEBASED BENCHMARK PROJECT

ONCOLOGY NURSE COMPASSION FATIGUE INTERVENTION EVIDENCE-BASED BENCHMARK PROJECT FALL 2020

RATIONALE • Compassion fatigue, burnout, and stress are prominent among oncology nurses. • Without appropriate resources hospitals will have high rates of turnover and nurses will experience long-lasting side effects. • Mindfulness-based interventions teach nurses techniques for managing difficult emotions in stressful situations. , burnout, and stress are common in oncology nurses.

GOAL To develop a structured compassion fatigue program for oncology nurses. This course will provide nurses with the skills and resources to manage compassion fatigue, burnout, and stress. This will be required for all the organization’s oncology nurse hires and current staff will be strongly encouraged to attend.

LITERATURE REVIEW After completion of a six-week mindfulness-based intervention 80. 4% of participants felt that their relationship with their emotions improved for the better (Duarte & Pinto-Gouveia, 2016). There was a significant difference in compassion fatigue between the intervention and comparison groups. Potter and others (2013) conducted a five-week compassion fatigue resiliency program that resulted in decreased nurse avoidance and increased enjoyment. Nurses felt like they were not alone with these difficult feelings. Hospital leaders must foster a culture that prioritizes the emotional wellbeing of their staff (Pfaff et al. , 2017). Yilmaz, Ustun, and Gunusen (2018) held a five-week nurse led course that had a significant improvement in all three of the Pro. QOL sub-scales: compassion fatigue, burnout, and compassion satisfaction.

STAKEHOLDERS Hospital administration Oncology nurse managers Oncology clinical educators Oncology nurses Patients

OUTCOMES Describe compassion fatigue and the signs of it Describe the impact of compassion fatigue, burnout, and stress Provide education on available resources Provide mindfulness-based course Evaluate the success of the course and education provided

EVALUATION DESIGN Evaluation of the course will involve the Pro. QOL version 5 being administered before and after the six-week intervention. A survey will also be administered at completion of the course to obtain staff opinions regarding the intervention. The intervention will be considered a success if there is an improvement in any of the Pro. QOL sub-scale scores or if greater than 50% of the participant surveys indicate that staff were able to make positive changes in the way they handle stressful emotions due to participation in the course.
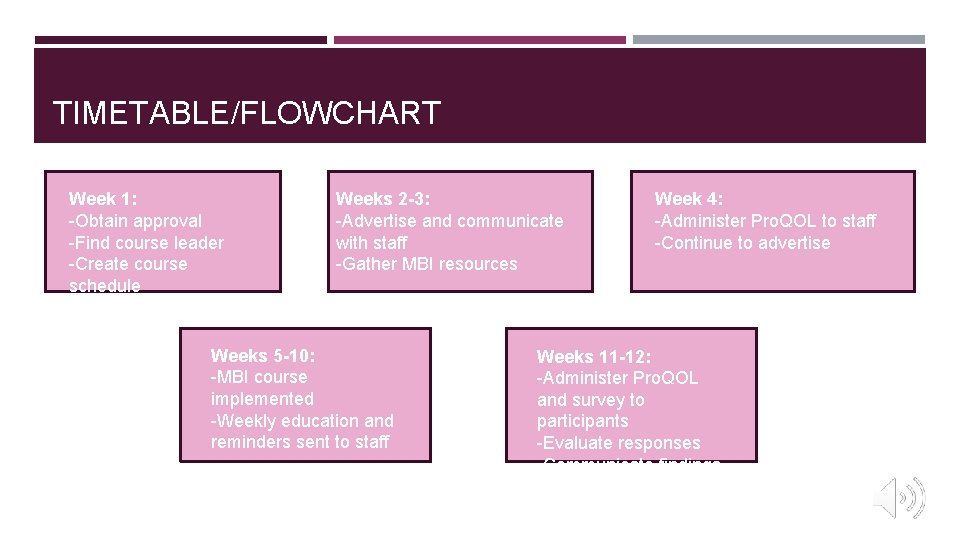
TIMETABLE/FLOWCHART Week 1: -Obtain approval -Find course leader -Create course schedule Weeks 2 -3: -Advertise and communicate with staff -Gather MBI resources Weeks 5 -10: -MBI course implemented -Weekly education and reminders sent to staff Week 4: -Administer Pro. QOL to staff -Continue to advertise Weeks 11 -12: -Administer Pro. QOL and survey to participants -Evaluate responses -Communicate findings

DATA COLLECTION METHODS Pre- and post-course Pro. QOL scores Participant survey
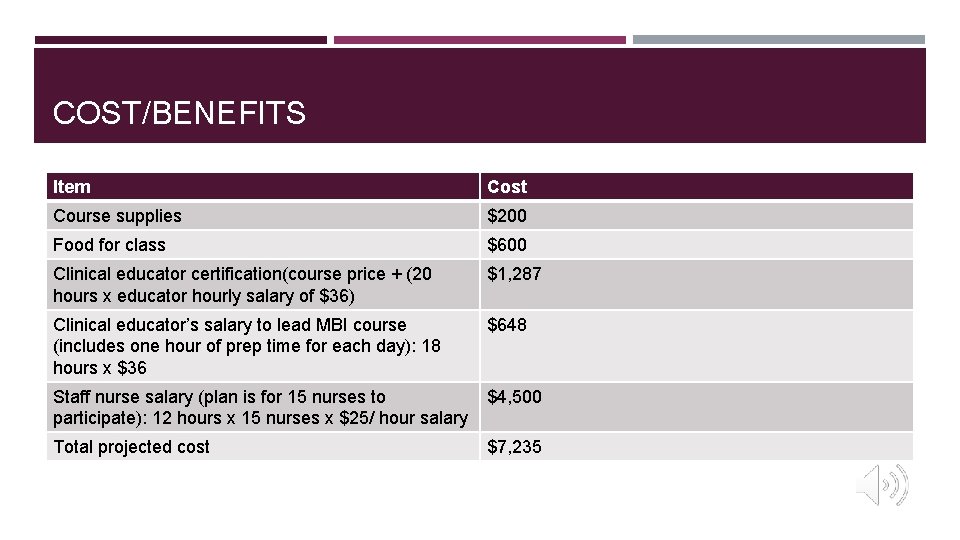
COST/BENEFITS Item Cost Course supplies $200 Food for class $600 Clinical educator certification(course price + (20 hours x educator hourly salary of $36) $1, 287 Clinical educator’s salary to lead MBI course (includes one hour of prep time for each day): 18 hours x $36 $648 Staff nurse salary (plan is for 15 nurses to participate): 12 hours x 15 nurses x $25/ hour salary $4, 500 Total projected cost $7, 235

CONCLUSION/RECOMMENDATIONS Oncology nurse stress levels, burnout, compassion fatigue, and retention are serious issues healthcare organizations are facing today. Mindfulness-based interventions are effective at reducing burnout, compassion fatigue and other psychological symptoms in oncology nurses (Duarte & Pinto-Gouveia, 2016).

REFERENCES Duarte, J. , & Pinto-Gouveia, J. (2016). Effectiveness of a mindfulness-based intervention on oncology nurses’ burnout and compassion fatigue symptoms: A non-randomized study. International Journal of Nursing Studies, 64, 98 -107. doi: 10. 1016/ijnurstu. 2016. 10. 002 Kurnat-Thoma, E. , Ganger, M. , Peterson, K. , & Channell, L. (2017). Reducing annual hospital registered nurse staff turnover-A 10 -element onboarding program intervention. SAGE and Open Nursing, 3, 1 -13 Pfaff, K. A. , Freeman-Gibb, L. , Patrick, L. J. , Di. Biase, R. , & Moretti, O. (2017). Reducing the “cost of caring” in cancer care: Evaluation of a pilot interprofessional compassion fatigue resiliency programme. Journal of Interprofessional Care, 31(4), 512 -519. doi: 10. 1080/13561820. 2017. 1309364 Potter, P. , Deshields, T. , Berger, J. A. , Clarke, M. , Olsen, S. , & Chen, L. (2013). Evaluation of a fatigue resiliency program for oncology nurses. Oncology Nursing Forum, doi: 10. 1188/13. ONF. 180 -187 40(2), 180 -187. Yilmaz, G. , Ustun, B. , & Gunusen, N. P. (2017). Effect of a nurse-led intervention programme compassion on professional quality of life and post-traumatic growth in oncology nurses. International Journal of Nursing Practice. doi: 10. 1111/ijn. 12687

APPENDIX A

APPENDIX B

QUESTIONS AND DISCUSSION
- Slides: 15