OMH HCBS Waiver Updates Childrens Mental Health Staff

OMH HCBS Waiver Updates Children’s Mental Health Staff Development Training Forum November 29 -30, 2016 Division of Integrated Community Services for Children and Families NYS Office of Mental Health

HCBS Waiver Current State

3 HCBS Waiver Current State • Application Status Updates • CMS Discussions/Temporary Extension • 1915(b)(4) Application • Conflict Free Requirements • CFR - Program Codes and Reporting • Rates - Unbundling • OHCDS – Provider Designation

4 Application Status Updates • Temporary Extension to March 15, 2017; however, ongoing efforts to secure approval of application as soon as possible • OMH/DOH still holding weekly calls with CMS to maintain momentum and keep process moving • Developing interim rates with DOH to transition to MMC and Health Homes • Working on addressing all remaining CMS questions and concerns

5 1915 (b)(4) Application • Recap: The 1915(b)(4) application is to allow OMH to maintain the current ICC structure – ICC Agency designation by county (“Selective Contracting”) • Application was re-submitted to CMS in October 2016 for their review • Anticipating a discussion with CMS in next few weeks

6 Conflict Free • Efforts are underway to address “conflict free” compliance in wake of moving to Health Homes and MMC in 10/2017 • Regardless of decision, ICC Agencies will still be required to: o Create administrative and supervisory firewalls between care coordination and HCBS Wavier services/functions o Discontinue ICC from providing any other HCBS service o Ensure family choice of HCBS service provider and right to change service provider if desired or dissatisfied o Inform child/family of right to file complaint and/or grievance

7 CFR – Program Codes • CMS is requiring providers to complete fiscal cost reporting by each service in the HCBS Wavier • Effective 7/1/2016 (NYC) and 1/1/2017 (ROS) each service will need to be reported separately. • Revised Fiscal Worksheets will be set out shortly • Specific Fiscal questions - reach out to your Field Office Finance

8 New Program Codes • 2230 Children’s HCBS Waiver Individualized Care Coordination • 2240 Children’s HCBS Waiver Respite • 2250 Children’s HCBS Waiver Family Support • 2260 Children’s HCBS Waiver Crisis Response • 2270 Children’s HCBS Waiver Skill Building • 2280 Children’s HCBS Waiver Intensive In-Home • 2350 Children’s HCBS Waiver Supported Employment • 2360 Children’s HCBS Waiver Pre-Vocational Services • 2370 Children’s HCBS Waiver Youth Peer Advocate • 2300 HCBS Waiver will be deleted

9 Rates - Unbundling • Continuing to unbundle rates & separate ICC role from other two waiver services (IIHS & CR) • ICC Rate will continue to be a monthly PMPM; IIHS and CR rates will be billed in units (time intervals) when provided • OMH/DOH working on developing rates to facilitate approval of Waiver renewal by CMS before transition to MMC/HH on 10/2017 • Working on establishing service limitations for all HCBS services

10 OHCDS/Direct Medicaid Billing • The OMH Wavier is unique and has an “OHCDS” billing structure (all services are billed through ICC Agency). This is not consistent with OHCDS guidelines • HCBS Wavier service providers must have the option to either opt into the OHCDS structure OR direct bill Medicaid. • Therefore, to allow for this, if currently subcontracted agencies want to continue to provide services and bill Medicaid directly, they should be sure to apply through the “Provider Designation Application” process outlined in slides below

Future of HCBS

12 Future of HCBS • Transformation Timeline • SPA Services • HCBS Services • Difference between SPA & HCBS • Continuum of Care • Provider Designation
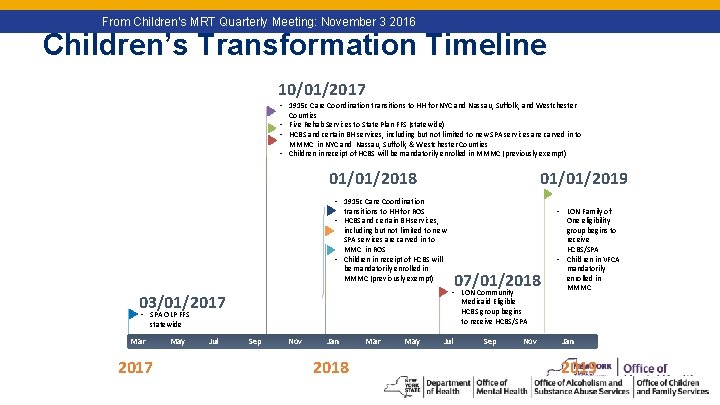
13 From Children’s MRT Quarterly Meeting: November 3 2016 Children’s Transformation Timeline 10/01/2017 • 1915 c Care Coordination transitions to HH for NYC and Nassau, Suffolk, and Westchester Counties • Five Rehab Services to State Plan FFS (statewide) • HCBS and certain BH services, including but not limited to new SPA services are carved in to MMMC in NYC and Nassau, Suffolk, & Westchester Counties • Children in receipt of HCBS will be mandatorily enrolled in MMMC (previously exempt) 01/01/2019 01/01/2018 • 1915 c Care Coordination • LON Family of transitions to HH for ROS • HCBS and certain BH services, including but not limited to new SPA services are carved in to MMC in ROS • Children in receipt of HCBS will be mandatorily enrolled in MMMC (previously exempt) 03/01/2017 Medicaid Eligible HCBS group begins to receive HCBS/SPA • SPA OLP FFS statewide Mar 2017 May Jul 07/01/2018 • LON Community One eligibility group begins to receive HCBS/SPA • Children in VFCA mandatorily enrolled in MMMC Sep Nov Jan 2018 Mar May Jul Sep Nov Jan 2019
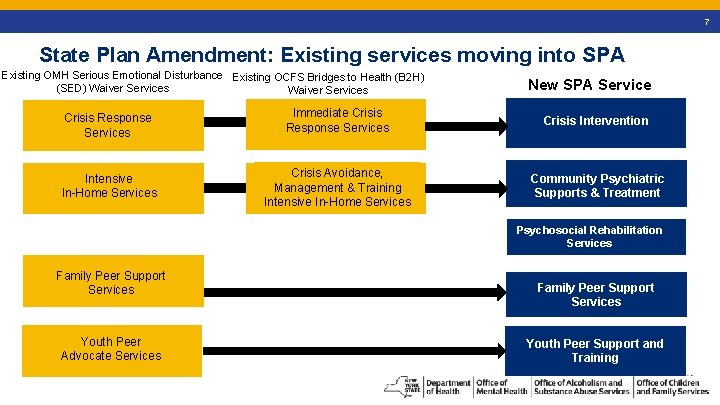
14 State Plan Amendment: Existing services moving into SPA Existing OMH Serious Emotional Disturbance Existing OCFS Bridges to Health (B 2 H) (SED) Waiver Services New SPA Service Crisis Response Services Immediate Crisis Response Services Crisis Intervention Intensive In-Home Services Crisis Avoidance, Management & Training Intensive In-Home Services Community Psychiatric Supports & Treatment Psychosocial Rehabilitation Services Family Peer Support Services Youth Peer Advocate Services Family Peer Support Services Youth Peer Support and Training 7
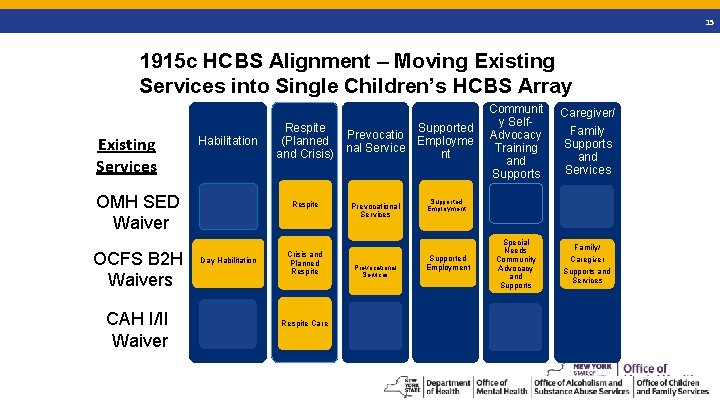
15 1915 c HCBS Alignment – Moving Existing Services into Single Children’s HCBS Array Existing Services Habilitation OMH SED Waiver OCFS B 2 H Waivers CAH I/II Waiver Respite (Planned and Crisis) Respite Day Habilitation Crisis and Planned Respite Care Prevocatio nal Service Prevocational Services Supported Employme nt Communit y Self. Advocacy Training and Supports Caregiver/ Family Supports and Services Supported Employment Special Needs Community Advocacy and Supports Family/ Caregiver Supports and Services 15
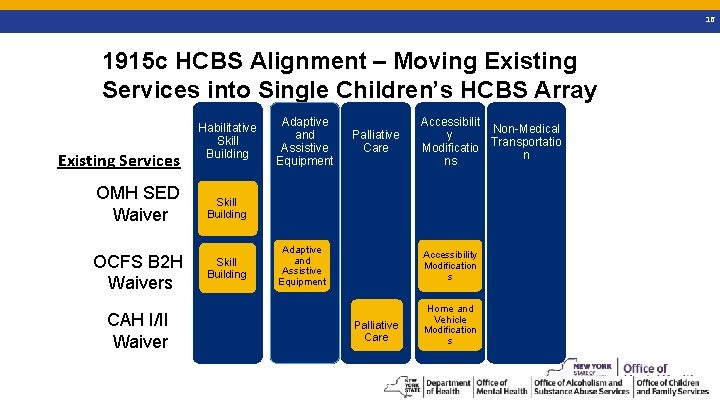
16 1915 c HCBS Alignment – Moving Existing Services into Single Children’s HCBS Array Existing Services Habilitative Skill Building OMH SED Waiver Skill Building OCFS B 2 H Waivers Skill Building CAH I/II Waiver Adaptive and Assistive Equipment Palliative Care Adaptive and Assistive Equipment Accessibilit Non-Medical y Transportatio Modificatio n ns Accessibility Modification s Palliative Care Home and Vehicle Modification s 16
17 Current Continuum of Care
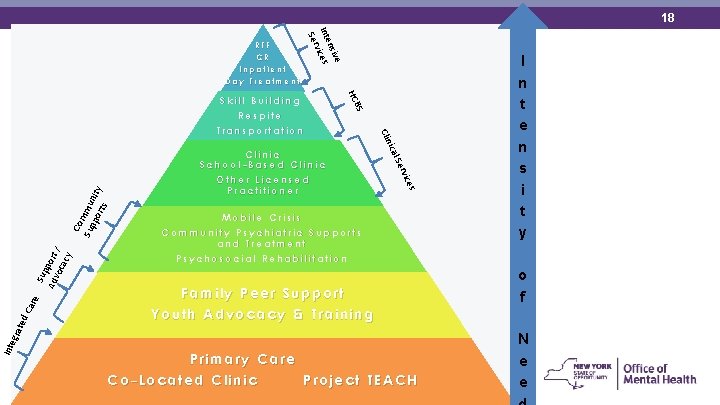
18 ve nsi Inte ices v Ser RTF CR Inpatient Day Treatment Co m Sup mun po i rts ty Sup Ad port voc / acy e es Car rvic l Se ica Clinic School-Based Clinic Other Licensed Practitioner Clin Mobile Crisis Community Psychiatric Supports and Treatment Psychosocial Rehabilitation Family Peer Support Youth Advocacy & Training Int egr a ted BS HC Skill Building Respite Transportation Primary Care Co-Located Clinic Project TEACH I n t e n s i t y o f N e e
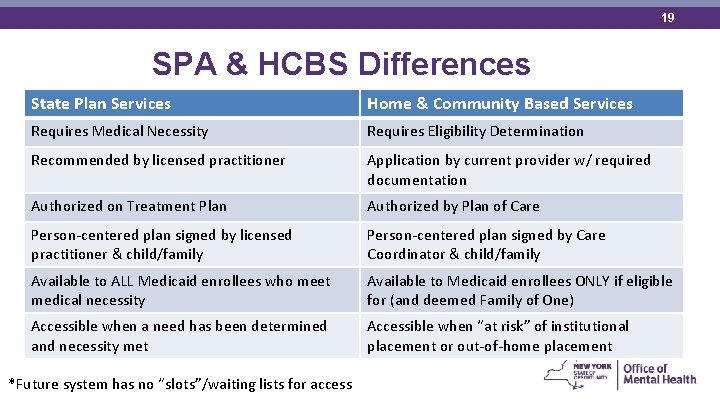
19 SPA & HCBS Differences State Plan Services Home & Community Based Services Requires Medical Necessity Requires Eligibility Determination Recommended by licensed practitioner Application by current provider w/ required documentation Authorized on Treatment Plan Authorized by Plan of Care Person-centered plan signed by licensed practitioner & child/family Person-centered plan signed by Care Coordinator & child/family Available to ALL Medicaid enrollees who meet medical necessity Available to Medicaid enrollees ONLY if eligible for (and deemed Family of One) Accessible when a need has been determined and necessity met Accessible when “at risk” of institutional placement or out-of-home placement *Future system has no “slots”/waiting lists for access

20 Preparing for New Service Structure • Moving from “programs” to services – available array of services for children who have varied needs • Still MUST apply for designation to be able to provide SPA and HCBS services even if a HCBS Wavier provider today • SPA/HCBS will be available to various “populations” of children; substance use, foster care, medically fragile, mental health – what populations are you qualified to serve? Need to indicate capacity/preference on Provider Designation application.

21 Preparing for New Service Structure • When providing SPA services to a MH population, will need an authorization or licensure from OMH; may need the same from other State agencies for other populations (e. g. OASAS for SUD) • For HCBS services, since many are moving to SPA, there will be no “grandfathering, ” but “preference” given to providers doing services today • Should review NEW SPA and HCBS Manuals* to review service definitions, provider qualifications and staffing qualifications for each service *Manuals will be available when Provider Designation Application becomes available

22 Provider Designation Process • Qualifying Provider Agencies: “Any practitioner providing behavioral health services must operate within a child serving agency or agency with children’s behavioral health and health experience that is licensed, certified or designated by DOH, OASAS, OCFS, or OMH in settings permissible by that designation” • Individual practitioners are not eligible to be designated as a SPA or HCBS provider; must be employed by a qualifying child-serving agency • Agencies who are currently NOT licensed, certified or designated by OMH; will need to apply for a User ID to complete a Provider Designation Application (on-line)

23 Provider Designation Process • Current HCBS subcontractors will also need to apply to be able to provide SPA and/or HCBS services • If there are subcontractors who are not currently Medicaid enrolled providers, they will also have to follow steps for Medicaid provider enrollment • As is required today, under MMC, all Family Peers (and Youth Peers in the future) will need to be credentialed to allow for billing of Medicaid for the services they provide

24 Provider Designation • Provider ID for Non-OMH providers and pending application to be available soon. • In anticipation of the release of the Children’s SPA/HCBS Provider Designation Application in the near future, we are alerting all New York State (NYS) providers who may wish to apply for designation to undertake a preparatory step to obtain a user ID. The user ID, granted through the NYS Office of Mental Health (OMH), will enable the electronic application, once released, to be accessed and completed. http: //www. health. ny. gov/health_care/medicaid/redesign/behavioral_health/children/provider_de sign. htm • When the Provider Designation Application becomes available – it will be accessible at the link provided above

25 Questions? ?

26 Contact Information • For answers to your questions, contact: – The OMH HCBS Wavier Unit Ø Joyce Billetts Ø Shannon Fortran Ø Steve Vroman – Email: dcfs@omh. ny. gov – Phone: 518 -474 -8394
- Slides: 26