OECD REVIEWS OF HEALTH SYSTEMS LATVIA Francesca Colombo

OECD REVIEWS OF HEALTH SYSTEMS: LATVIA Francesca Colombo Head of OECD Health Division Riga, 20 September 2016

Health in Latvia today • Aging, shrinking population • High prevalence of risk factors • Quality and efficiency initiatives underway but room for improvemen • Under-funded system compared to OECD 2

Next steps: • Improve access to care • Build a data-drive health system • Strengthen preventive care • Rise efficiency, strategic contracting 3

1. HEALTH IN LATVIA 4
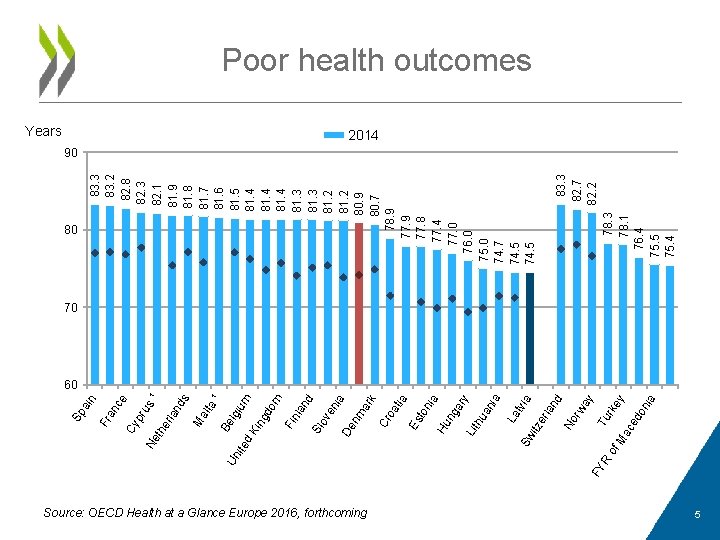
lgi ¹ um d. K ing do m Fin lan d Sl ov en ia De nm ar k Cr oa tia Es ton ia Hu ng ar y Lit hu an ia La tvi Sw a itz er lan d No rw ay FY Tu R rke of y Ma ce do nia Un ite Be lta Ma nd s s¹ ru e nc rla the Ne Cy p Source: OECD Health at a Glance Europe 2016, forthcoming 78. 3 78. 1 76. 4 75. 5 75. 4 Years 83. 3 82. 7 82. 2 83. 3 83. 2 82. 8 82. 3 82. 1 81. 9 81. 8 81. 7 81. 6 81. 5 81. 4 81. 3 81. 2 80. 9 80. 7 78. 9 77. 8 77. 4 77. 0 76. 0 75. 0 74. 7 74. 5 80 Fr a in Sp a Poor health outcomes 2014 90 70 60 5
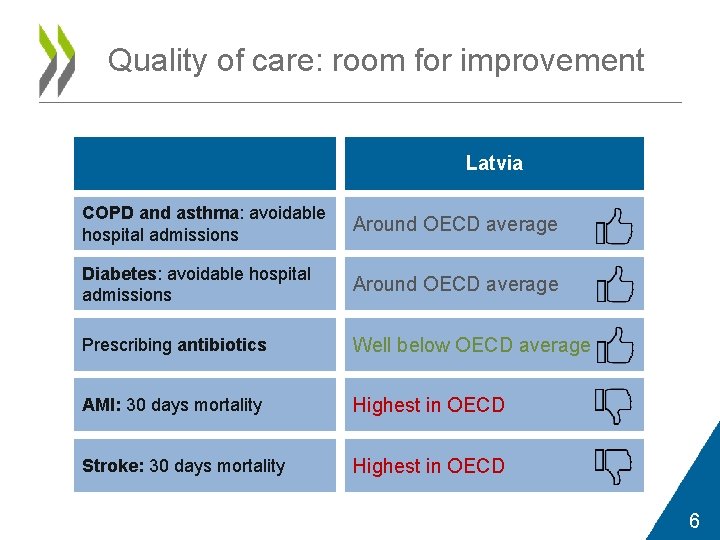
Quality of care: room for improvement Latvia COPD and asthma: avoidable hospital admissions Around OECD average Diabetes: avoidable hospital admissions Around OECD average Prescribing antibiotics Well below OECD average AMI: 30 days mortality Highest in OECD Stroke: 30 days mortality Highest in OECD 6
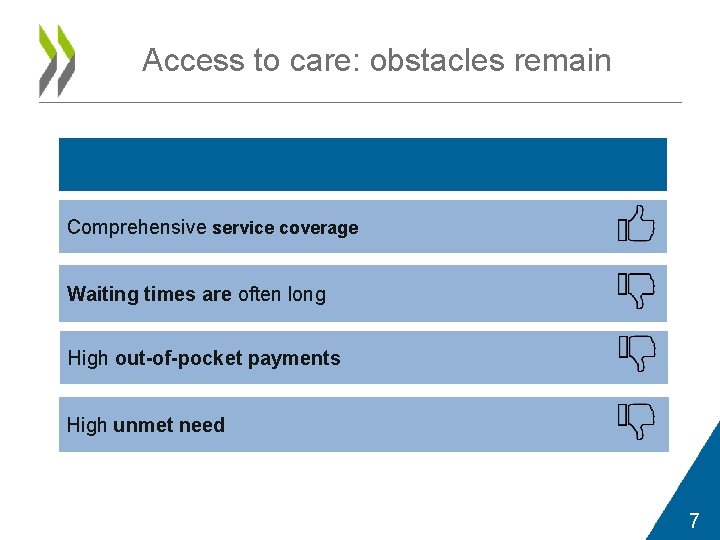
Access to care: obstacles remain Comprehensive service coverage Waiting times are often long High out-of-pocket payments High unmet need 7
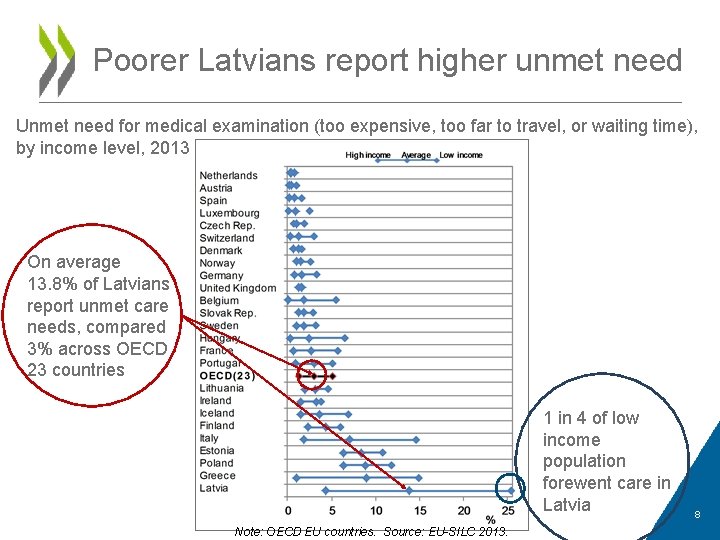
Poorer Latvians report higher unmet need Unmet need for medical examination (too expensive, too far to travel, or waiting time), by income level, 2013 On average 13. 8% of Latvians report unmet care needs, compared 3% across OECD 23 countries 1 in 4 of low income population forewent care in Latvia Note: OECD EU countries. Source: EU-SILC 2013. 8
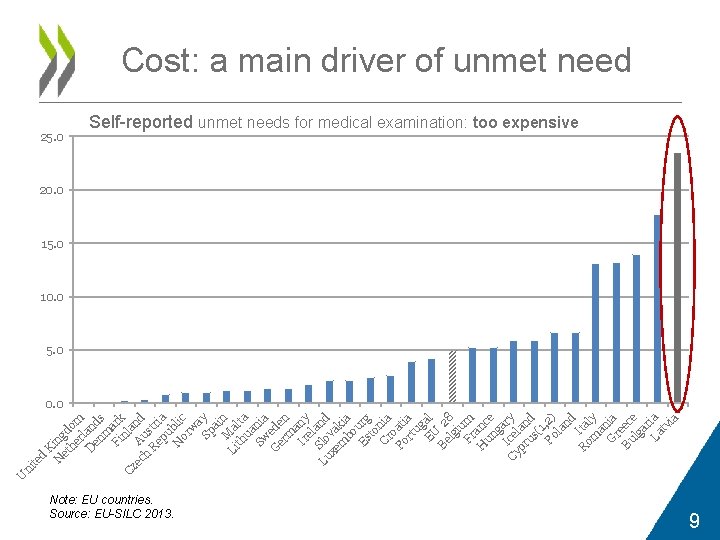
d K N ing et d he om r D lan en ds m Fi ark nl Cz a ec A nd h us Re tr pu ia N blic or w a Sp y ai n M Li a th lta ua Sw nia G ede er n m a Ir ny el a Lu Slo nd v xe a m kia bo Es urg to Cr nia o Po ati rt a ug EU al Be 28 lg iu Fr m H anc un e ga I c Cy e ry pr lan us d (1 Po , 2) la nd Ro Ita m ly an G ia r Bu eec lg e ar La ia tv ia te ni U Cost: a main driver of unmet need 25. 0 Self-reported unmet needs for medical examination: too expensive 20. 0 15. 0 10. 0 5. 0 0. 0 Note: EU countries. Source: EU-SILC 2013. 9
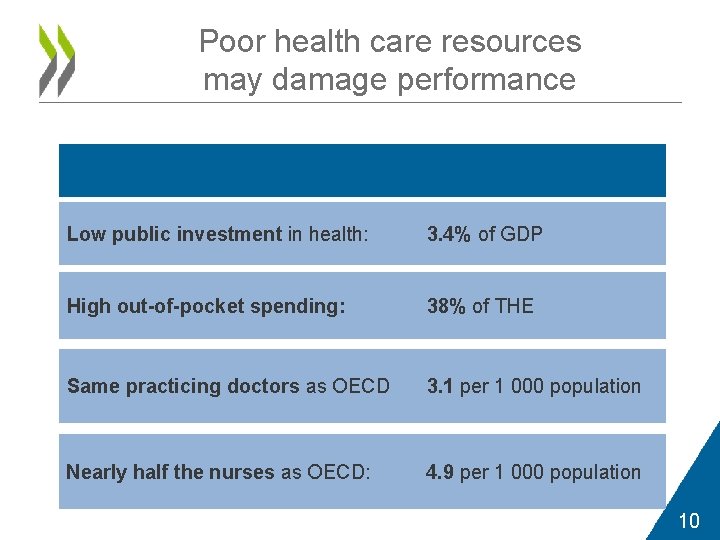
Poor health care resources may damage performance Low public investment in health: 3. 4% of GDP High out-of-pocket spending: 38% of THE Same practicing doctors as OECD 3. 1 per 1 000 population Nearly half the nurses as OECD: 4. 9 per 1 000 population 10
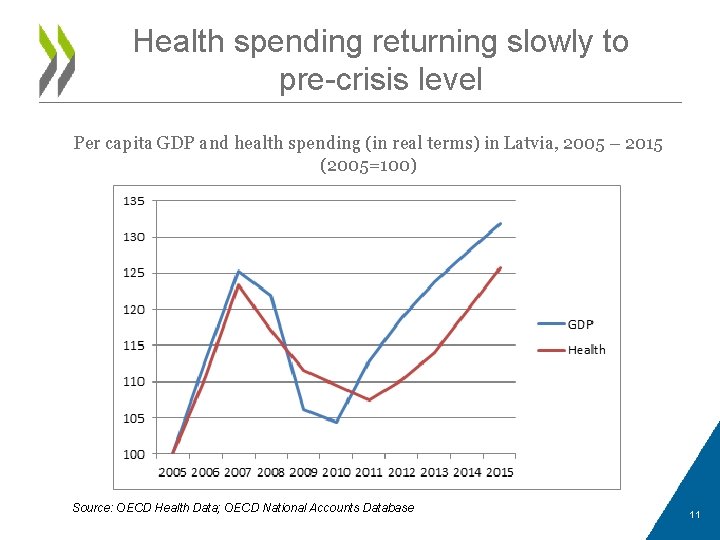
Health spending returning slowly to pre-crisis level Per capita GDP and health spending (in real terms) in Latvia, 2005 – 2015 (2005=100) Source: OECD Health Data; OECD National Accounts Database 11
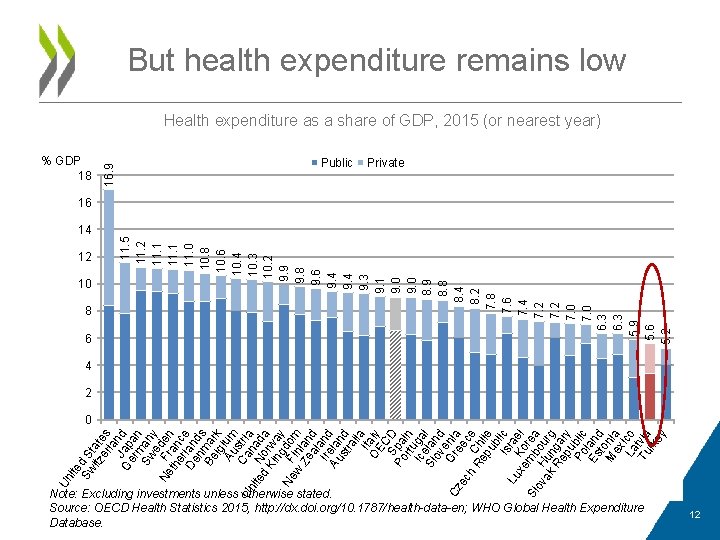
Note: Excluding investments unless otherwise stated. Source: OECD Health Statistics 2015, http: //dx. doi. org/10. 1787/health-data-en; WHO Global Health Expenditure Database. Un ite Sw d S itz tate er s la n Ge Jap d rm an Sw an e y Ne F den th ran e c De rlan e n ds Be mar lg k Au ium Ca stri Un a ite N nad d or a Ki w n ay Ne F gdo w inl m Ze an al d Ire and Au lan str d al i Ita a OE ly C Sp D Po a rtu in Ic ga Sl elan l ov d en G Cz re ia ec e h C ce Re h pu ile b Isr lic Lu a xe Ko el m re Sl ov H bou a ak un rg Re ga pu ry Po blic Es land to M nia ex La ico Tu tvia rk ey 12 10 8 6 11. 5 11. 2 11. 1 11. 0 10. 8 10. 6 10. 4 10. 3 10. 2 9. 9 9. 8 9. 6 9. 4 9. 3 9. 1 9. 0 8. 9 8. 8 8. 4 8. 2 7. 8 7. 6 7. 4 7. 2 7. 0 6. 3 5. 9 5. 6 5. 2 % GDP 18 16. 9 But health expenditure remains low Health expenditure as a share of GDP, 2015 (or nearest year) Public Private 16 14 4 2 0 12

2. TACKLING KEY CHALLENGES… 13

Improving access to care § Commendable efforts to improve access: § § Opening rural practices More nurses in primary care Free hotel-accommodation for some groups Physician assistant or “feldsher” role: § Next steps § Cost-sharing exemptions for vulnerable patients § Assess if “quota” system is fit for purpose § Focus on prevention 14

Improve quality and data use § Quality initiatives are underway: § § P 4 P in primary care Incentives for early cancer detection Coordination in emergency and primary care Electronic health record launch imminent § Next steps: § From minimum standards to quality improvement § Build a data-driven system § Open data publication and benchmarking 15

Improve efficiency § Certain efficiency gains: § Reduction in hospital use, shift to outpatient § Recent introduction of DRG system § Centralised emergency triage system § Next steps: § More strategic contracting § Better targeting of waste 16

More resources may be needed • To see health outcomes closer to the OECD average • To tackle problems with access and quality • For sustainable long-term performance § Initial steps: § § A spending review A comprehensive five or ten-year plan A workforce plan to assess and project need Developing long-term care 17

TO CONCLUDE… 18

Key policy recommendations Improve access to care Focus on improving quality Drive efficiency gains Consider carefully increasing health spending 19

Thank you Contact: Francesca. Colombo@oecd. org Read more about our work Follow us on Twitter: @OECD_Social Website: www. oecd. org/health Newsletter: http: //www. oecd. org/health/update 20
- Slides: 20