Ocular allergy Abdulrahman Al Muammar Ocular allergy Allergic

Ocular allergy Abdulrahman Al Muammar

Ocular allergy Allergic eye diseases accounts for up to 3% of all the medical consultations seen in general practice. The milder forms of allergic eye diseases have fluctuating symptoms of itch, tearing, and swelling. Chronic form of the disease give rise, in addition, to more severe symptoms including pain, visual loss from corneal scarring, cataract or glaucoma, and disfiguring skin and lid changes.

Ocular allergy Clinical classifications: l 1) Allergic conjunctivitis (AC): l Acute allergic conjunctivitis: l l l Seasonal or hay fever. Toxic- induced (induced by acute contact with irritant, drugs, preservatives, etc). Chronic allergic conjunctivitis: l l Perennial. Toxic-induced (long standing).

Ocular allergy 2) Contact dermatoblepharitis. l 3) Vernal keratoconjunctivitis (VKC l 4) Giant papillary conjunctivitis (GPC l 5) Atopic keratoconjunctivitis (AKC l 6) Atopic blepharoconjunctivitis (ABC). l

Sensitization Acute and chronic diseases have in common: 1) sensitization to environmental allergens. l 2)Ig E mast cells activation with subsequent mediator cascade. l 3) conjunctival inflammation with prevalence of eosinphils. l 4) the presence of lymphocytes with a Th 2 profile of cytokines production. l

Sensitization The conjunctiva is normally exposed to pictogram quantities of environmental allergens such as pollens, dust mite fecal particles, animal dander and other proteins. l When deposited on the mucosa, these antigens are thought to be processed by lagerhans cells and other antigen presenting cells (APC) in the mucosal epithelium. l

Sensitization l antigen is presented to native Th 0 cells expressing antigen – specific T cell receptors recognize the antigenic peptide. Multiple simultaneous contacts and cytokine exchange between APC and T cells are necessary to trigger antigen specific Th 0 cells to differentiate into Th 2 lymphocyte.
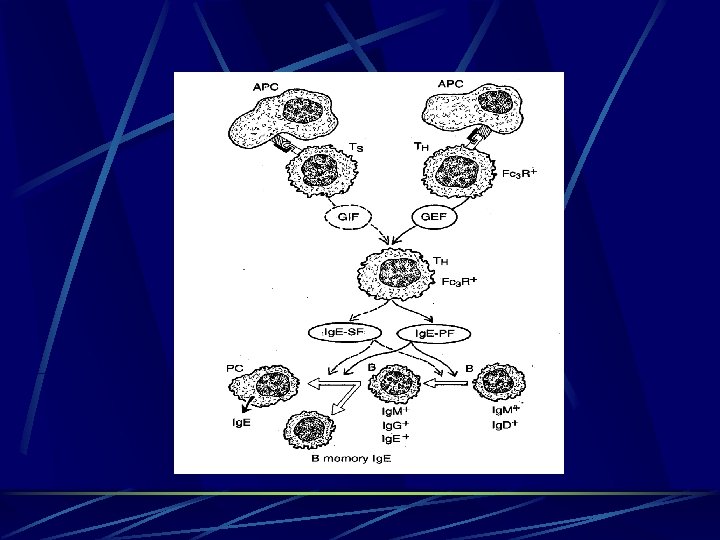
Sensitization. The cytokines released by Th 2 cells ( IL 3, IL 4, IL 5, IL 6, IL 13, GM-CSF) stimulate B cell Ig. E production and inhibit development of Th 1 mediated delayed type hypersensitivity reactions. l B cells which recognize the same allergen that induce Th 2 differentiation, in present of appropriate signals such as IL 4, IL 6 and IL 13 undergo heavy chain switching to produce Ig. E. l
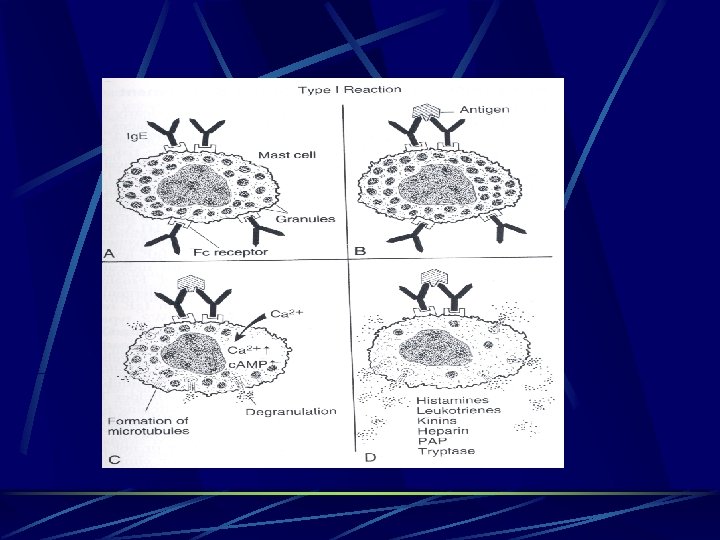

Mast cells l l Mast cells particularly abundant in the conjunctival stroma especially at the limbus. The number of the mast cells in the conjunctiva has been calculated to be 5000/mm 3. conjunctival biopsies from symptomatic allergic patients have shown an increase in subepithelial mast cells with evidence of mast cells degranulation Two different types of mast cells have sown in conjunctiva, differentiated by their content of tryptase alone ( mucosal mast cell or MCT) or both tryptase and chymase ( connective tissue type mast cell or MCTC)

Mast cells Proliferation of these cells in allergic disorders is probably under influence of Th 2 cytokins. l Mast cells and basophils, bearing high affinity surface receptors for Ig E are the most important cells in Ig. E mediated reactions. l

Mast cells mediators: l Histamine. l Vasodilatation…. smooth muscle constriction. l l Heparin. l Prevent blood coagulation. l l Itching. . redness. Anti-inflammatory. Tryptase. l Potentiates histamine. . activates eosinophils and mast cells

Mast cells l Prostaglandins and leukotrienes l Capillary leakage. . smooth muscle contraction. . increase granulocyte action. . platelet aggregation. l Airway hyperresponsiveness…asthma.

Mast cells l Eosinophil chemotactic factor-alpha (ECFalpha). l l Attract eosinophils. Platelet activating factor (PAF). l Platelet aggregation…. neutrophil chemotaxis. Bronchoconstriction…hypotension…hyperemia. . Chemosis. l

Eosinphils l l l Influx of eosinphils is essential in allergic inflammation and profound changes in conjuncatival mucosa. Eosinophils are activated by interaction with other inflammatory cells such as platelet activating factors. Activated eosinophils release very basic highly charged polypeptide including: l l Major basic protein (MBP). Eosinophil cationic protein (ECP). Eosinophil derived neurotoxin (EPX). eosinophil peroxidase (EPO).
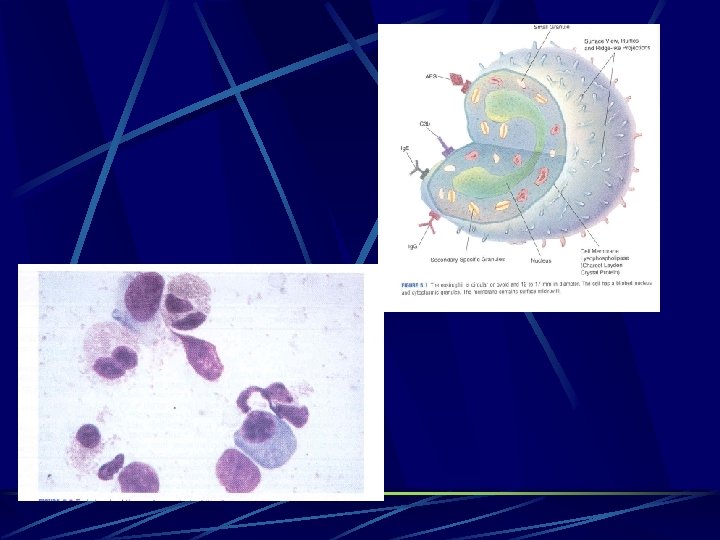

Eosinphils l l These proteins may bind to basement membrane protoglycans and hyaluran to cause cellular disaggregation and epithelial desquamation. ECP and MBP are epithelial toxic and are involved in corneal damage that may occur in sever chronic allergy. Eosinphils are also important source of leukotriens, prostaglandins and cytokines such as IL 3, IL 5, and GM CSF, eotaxin and RANTES. ECP and EPX tear level are correlated with clinical signs and symptoms of allergic disease and maybe considered local markers of eosinphil activation.

Neutrophils Following allergen challenge, neutrophils are the first cells to appear in tear fluid and the predominant infiltrating cells in the conjunctive during late phase. l Although the role of neutrophils in allergic disorders is not clear, they can release inflammatory mediators including leukotriens , PAF and cytokines. l Tear level of myeloperoxidase (MPO). a neautrophil activating marker are increased in allergic conjunctivitis. l

Lymphocytes l l l One of the most important process responsible for orchestrating and regulating allergic inflammation is the production of cytokines by T cells lymphocytes. CD 4 -T cells are the predominant population in conjunctival inflamed tissues. T cells have been subdivided into two functionally distinct subset on the basis of their cytokine profile: l l l Th 1 and Th 2. Th 1 is known to produce IL 2 and interferon gamma(INFg). Th 2 is known to produce IL 3, IL 4, IL 5.

Lymphocytes l l T cells in allergic inflamed tissues are mostly CD 4 with cytokine production profile of the Th 2 type. An increase in expression of Th 2 type cytokine (IL 4, IL 5, IL 3) have been demonstrated in SAC, VKC and AKC. Compared to SAC, VKC maybe considered a disease with an over expression of these cytokines in addition to other mechanism involved. Conversely in AKC and GPC in addition to typical Th 2 derived cytokines, increases of IL 2 and INF-g has been shown suggesting that in the most severe atopic conditions a cell medicated hypersensitivity may also occur.

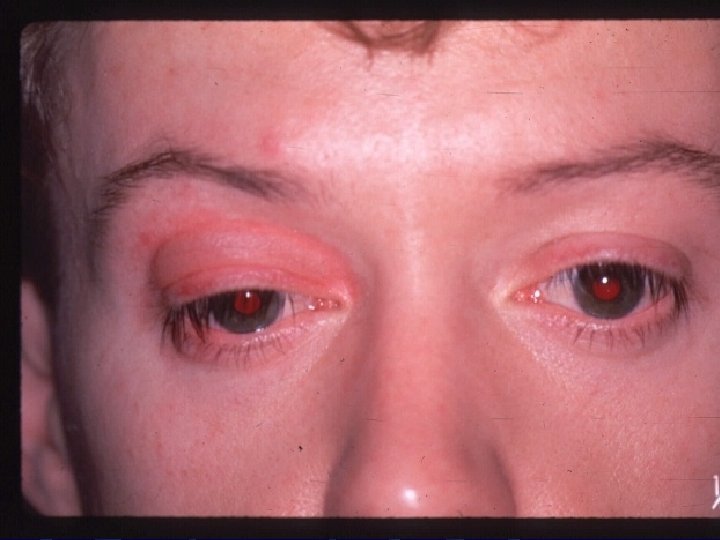
Seasonal allergic conjunctivitis l l Is the commonest and one of the mildest forms of allergic conjunctivitis. It accounts for 25%-50% of all cases of ocular allergy. SAC is often associated by rhinitis and even sinusitis. 70% of patients provide either a personal of familial allergic history. SAC can develop suddenly when patient comes in contact with an appropriate antigen, such as pollens, grasses, or trees.

SAC Symptoms: Itching. l Watery discharge. l Rhinitis. l Sinusitis. l

SAC Signs: Not always present. l Lid swelling. l Ptosis. l Conj hyperemia. l Chemosis (=/- dellen). l Papillary reaction. l Follicular reaction. l
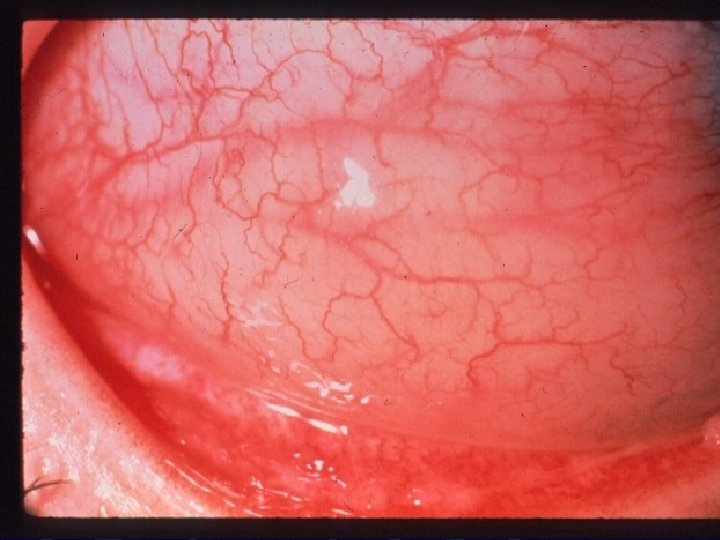

SAC Diagnosis: l l l Clinically. Family history. Conj scrapings for eosinophils. Tear level of Ig. E, serum tear. Radioallergosorbent test measures specific Ig. E levels for a specific antigens. Mast cells activity by measuring tryptase and histamine levels in tear film.

SAC Pathophysiology: Type I hypersenstivity. l Late phase reaction (LPR): l l Clinical, histological, or chemical response to an antigen that occurs 3 to 12 hours after the initial acute (early phase) mast cell-mediated allergic reaction.

SAC Treatment: l Avoidance of allergen: l l l l l Limit outdoor activities. Use air conditioning or air filter system. Drive car with windows closed. Use protective eyegear when outdoor. Washing allergen. Antihistamines. Mast cell stabilizers. NSAIDs. Steroids. Immunotherapy.

Acute allergic toxic induced conjunctivitis l l l Usually triggered by external non- airborne antigens such as drugs, contact lens solution, irritants, and preservatives. Type I medicated. Symptoms are similar to SAC but no seasonal component. l Itching, tearing, eyelid erythema and swelling, and conjunctival redness and chemosis. Typically occur within minutes after application of an allergen. l l l Bactriacin. . cephalosporins. . sulfacetamide. . tetracycline Atropine…homatropine. Epinephrine. . pilocarpine. . apraclonidine. Antiviral agents. Thimerosal. . chlorhexidine…bezalkonium chloride.
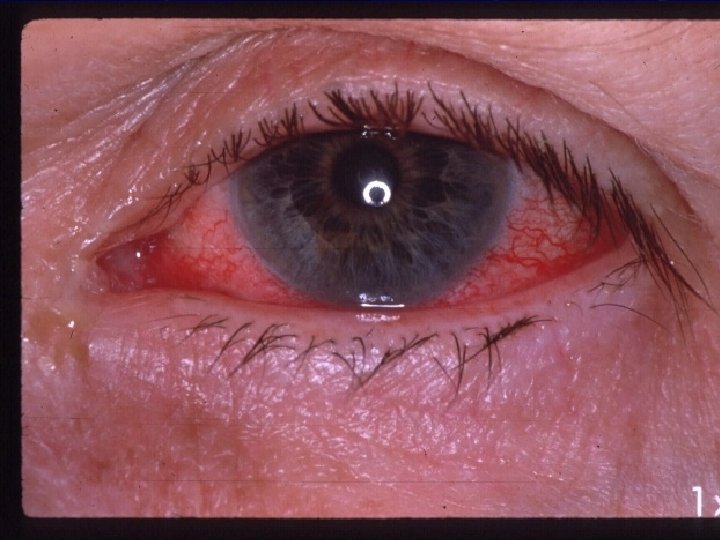
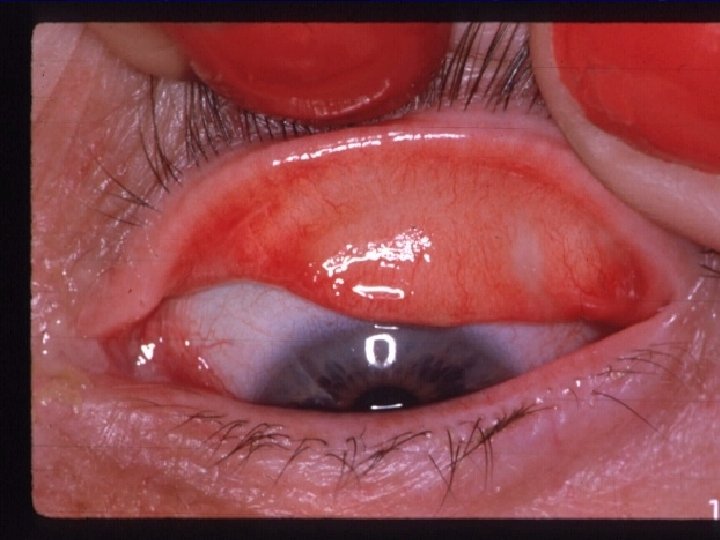
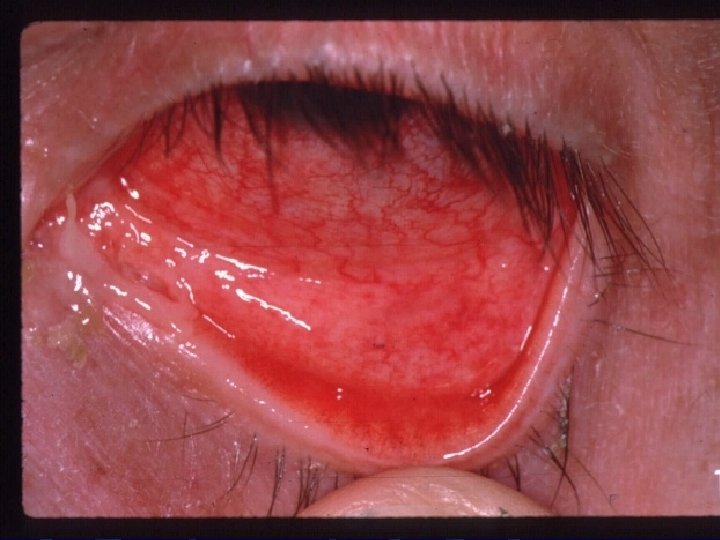

Acute allergic toxic induced conjunctivitis Diagnosis: l l l Clinical presentation. Offending agents. Conj scrapings. Treatment: l l l Discontinue the offending agents. Tears. . Cold compresses. Antihistamines. . NSAIDs. . Steroid

Perennial allergic conjunctivitis PAC Symptoms persist throughout the year, with seasonal variation in up to 87% of patients. The clinical signs and symptoms are similar to SAC, but more persistent. Allergens could be house dust mites, animals, etc. . Type I mediated.

PAC Treatment: l Avoidance of allergen: l l l Cover for mattress and pillows. Washing bedding regularly. Reduce humidity. Vaccum and damp dust. Eliminate animals from house. Washing allergen. Antihistamines. Mast cell stabilizers. NSAIDs. Steroids. Immunotherapy

Contact dermatoblepharitis Reaction that may begin 24 -72 hours following instillation of topical medication. Patients are often sensitized by previous exposure to the offending drugs or preservatives. Acute eczema with erythema, leatherlike thickening, and scaling of the eyelid. Lower eyelid ectropion, and hyperpigmentation. Papillary conjunctivitis and mucoid discharge may develop.
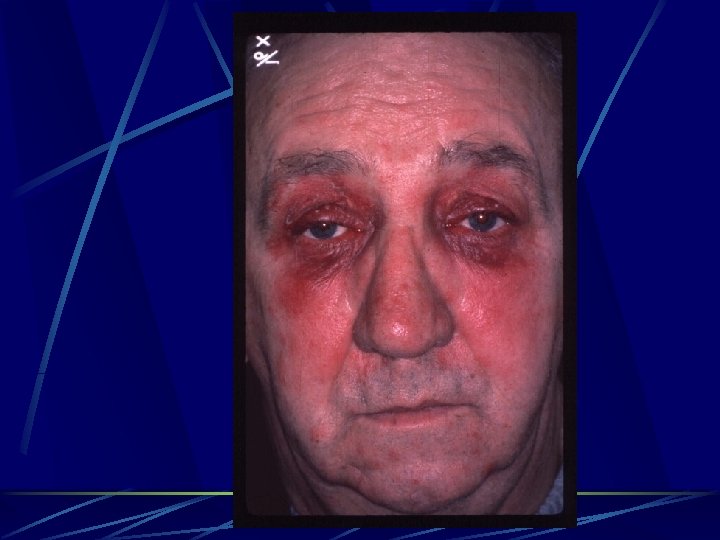

Contact dermatoblepharitis Medications commonly associated with these symptoms: Atropine. . homatropine. l Neomycine. . gentamycine. . tobramycine. l Idoxuridine. . trifluridine. l Thimerosal. l Type IV reaction.

Contact dermatoblepharitis Treatment: Allergen withdrawal. l In severe cases…brief course of topical steroids applied to the eyelids and periocular skin may speed resolution. l

VKC Epidemiology: l l l Rarely appear in patients younger than 3 or older than 25 years of age. M: F is 2: 1. The disease usually lasts 4 to 10 years and resolved after puberty, but also can still be present and even worsened in some adult patients. Occurs more frequently in the Mediterranean area, central Africa, India, and South America. It also occur in cooler climates, such as Great Britain and other northern European countries, which is possibly as a consequences of migratory movements of the susceptible population. Association with atopy is 15 to 60%.

VKC is usually bilateral, although monocular forms and asymmetric symptoms do occur. Three clinical forms can be observed : tarsal, limbal (more common in African and Asian patients), and mixed tarsal/limbal. In majority of the cases, the disease is seasonal, lasting from the beginning of spring until fall. Nevertheless, perennial cases have been observed, especially in warm subtropical or desert climates.

VKC Symptoms: Itching. l Tearing. l Mucus secretion. l Photophobia. l Pain. l Blepharospasm. l Decreased visual acuity. l
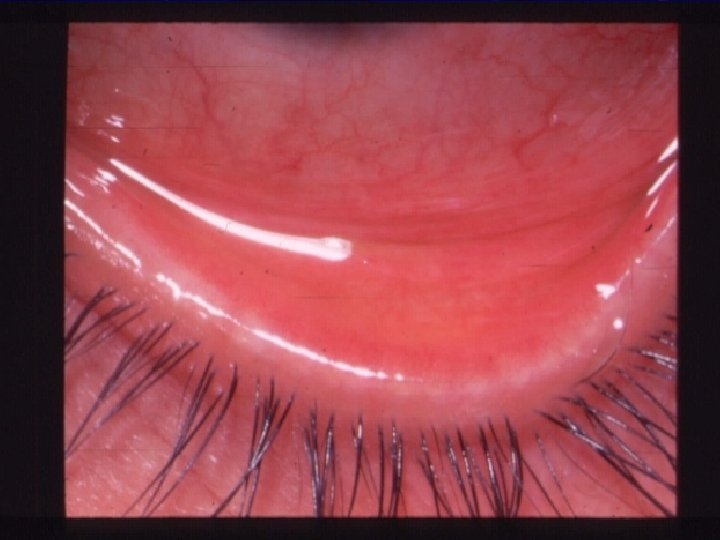
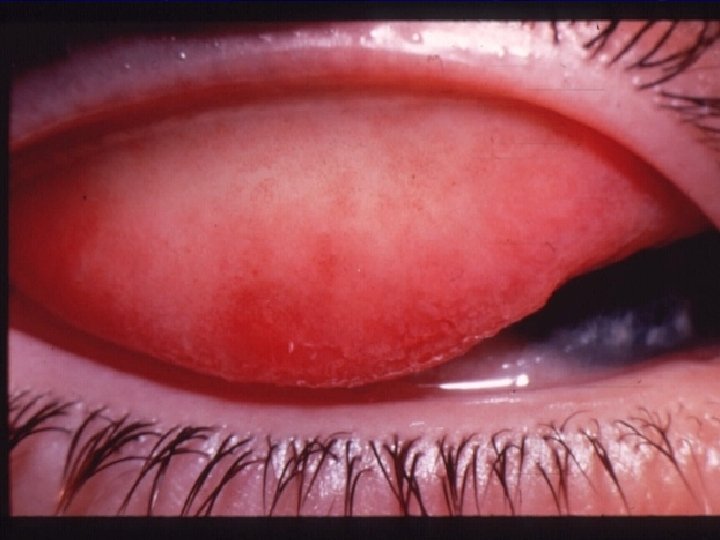
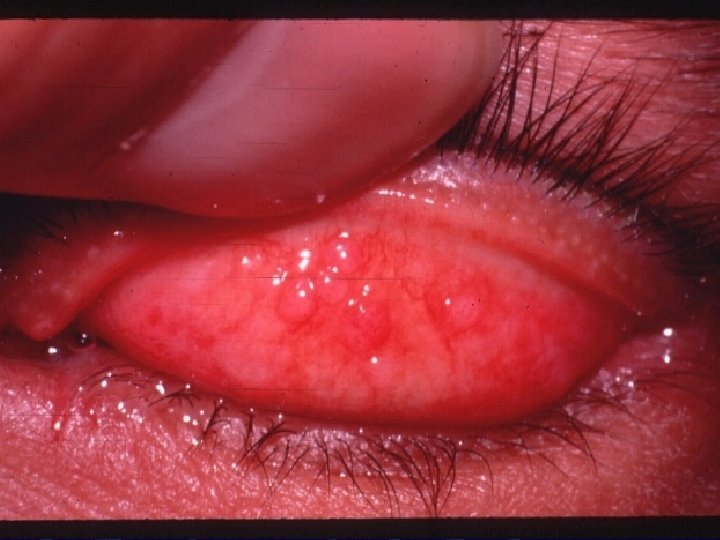
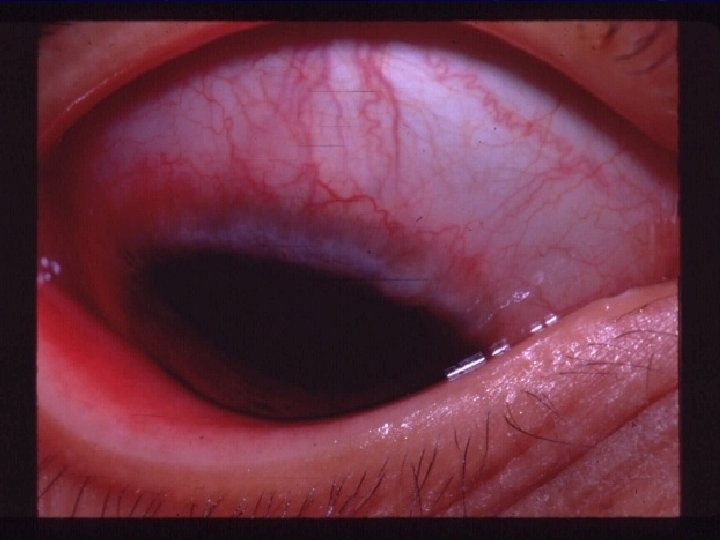
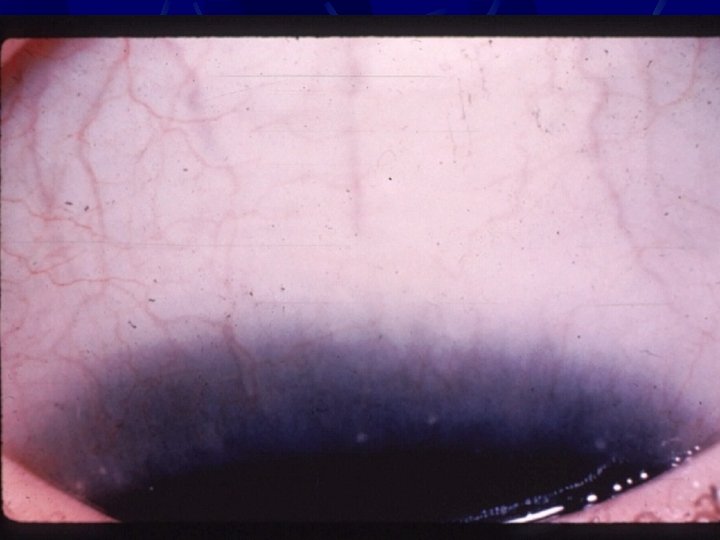
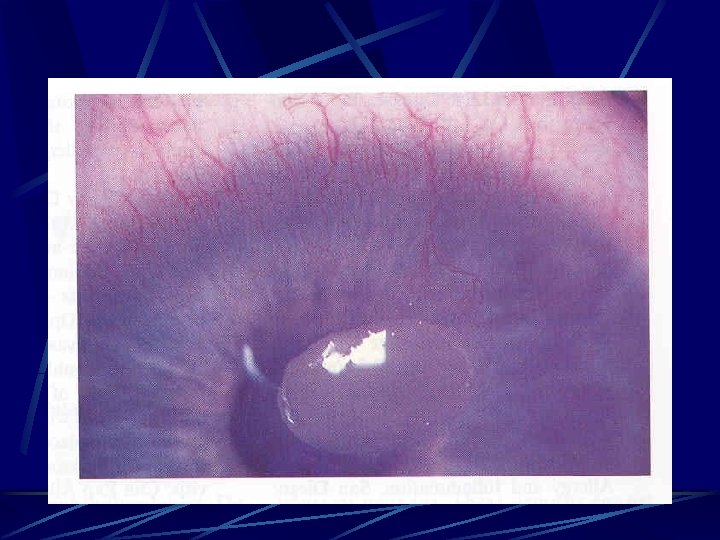
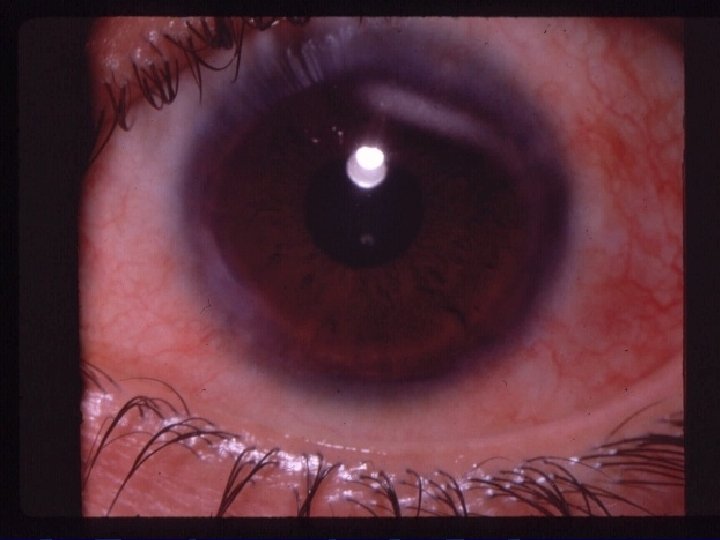
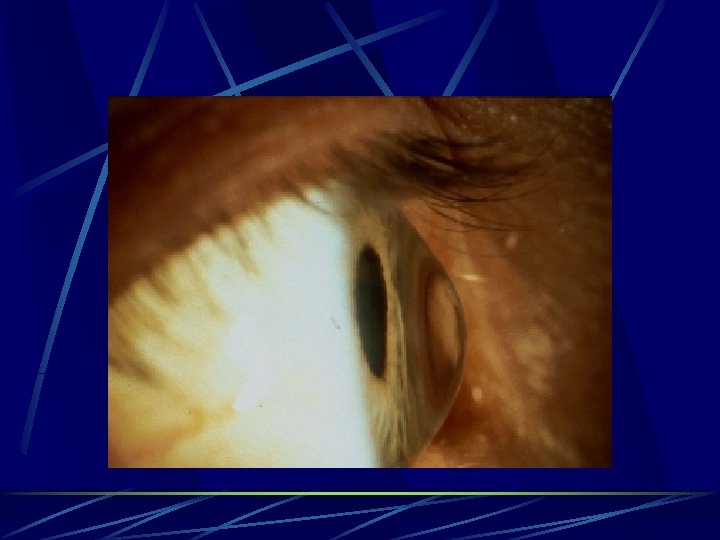

VKC Signs: l l l l Papillary reaction. Conjunctival redness and edema GPC. Limbal gelatinous infiltrate. Trantas dots. Mucus discharge. Pseudoptosis. Tarsal conjunctival fibrosis.

VKC Corneal involvement: l l l l SPK (Togby – Dusting of flour…uppper 1/3) PEE. Pannus. Filamentary keratitis. Shield ulcer. Pseudogerontoxon. Keratoconus.

VKC Diagnostic approaches: l l Clinically. Specific Ig. E maybe assayed in serum and tears. CBC for eosinophilia. Conj scraping and tear cytology: l l Eosinophils. Basophils. Neutrophils. Tears tryptase level.

VKC Pathogenesis: Type I hypersensitivity. l Type IV hypersensitivity. l

Histopathology: l Proliferative and degenerative changes in the epithelium: l l Occur early with marked acanthosis, and intraepithelial pseudocysts. Prominent cellular infiltration in the substantia propria: l l Eosinophils, neutrophils, basophils, lymphocytes, and plasma cells. Resident plasma cells and fibroblasts are also increased. Hyperplasia of the connective tissues: l l l VKC Mainly type III collagen, they run parallel to the surface forming the fibrous structure for giant papillae. Trantas dots. Shield ulcer.

VKC Therapy: l Preventive measures: l l l Mucolytic agents 10% Acetylcysteine Tears/vasoconstrictors/ cold compresses. Mast cells stabilizers: l l l Change of climate. Avoid exposure to nonspecific triggering factors such as sun, wind, and salt water. Should be used continuously throughout the season. Antihistamines. NSAIDS: either locally or systemically. Steroids. Short pulses, topical/ tarsal injection. Cyclosporine.

VKC l Corneal ulcers…. Steroids-antibiotic/eye patching. l Superficial keratectomy. l PTK. l l GPC…. . Local steroid injection. l papillae excision/cryotherapy/mucosal graft. l

AKC Atopy is hereditary condition that manifests in ocular diseases, skin abnormalities, and respiratory tract dysfunction. Atopy occurs in 5 to 20% of the general population. The term AKC is misleading, although ocular surface disease is most prominent, the disease usually involve the lid also.

AKC Epidemiology: l l l AKC occur in up to 25% of patients with atopic dermatitis. A review of family history frequently reveals the presence of other diseases such as asthma, hay fever, and urticaria. AKC occurs more frequently in men. Typically begin in the late teens or early twenties, and they persist until the fourth or fifth decade of life. The peak incidence occurs between the ages of 30 and 50 years.

AKC Clinical signs of the disease generally improve with age and may totally regress. l Patients with severe cases don't follow this trend. l AKC is often worse in the winter, but it usually has a perennial pattern of occurrence. l

AKC Clinical features: l Symptoms: Bilateral itching l Tearing l Watery discharge l Burning l Photophobia l Blurred vision. l

AKC Signs: l Lid: l l l l Thickening of the eyelid margins (tylosis) Eyelid swelling. Scaly, indurated, and wrinkled appearance of the periocular skin With profound swelling, a dennie-morgan folds or Dennie line is seen. Chronic inflammation can give upper lid ptosis. Fissures can occur at the lateral canthus owing to excessive skin rubbing. An absence of lateral eyebrows, or Hertoghe’s sign can be seen in severe form. Marginal belpharitis caused by staphylococcal infection is common.
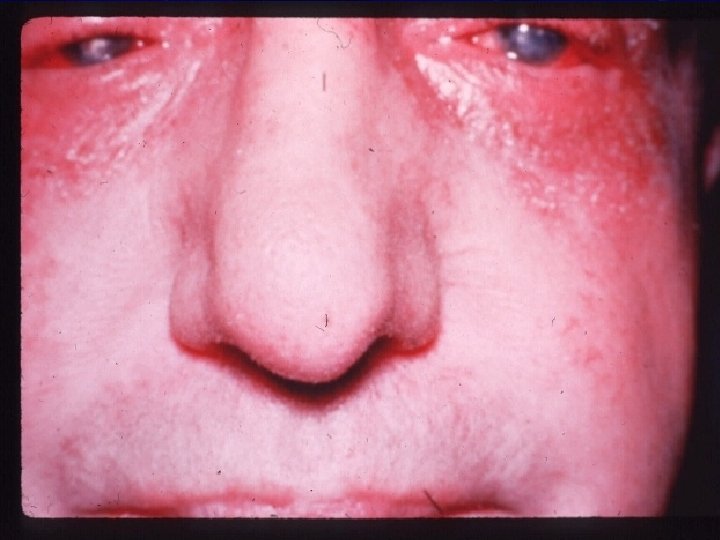

AKC l Conjunctiva: l l l The conjunctive can be hyperemic to milky edematous. Tarsal conjunctival papillary reaction is a common finding usually in small to medium size, both upper and lower conjunctive. Limbal papillae. Trantas dots. Rarely GPC in lower conjunctive. Conjunctival cicatrization and symblepharon most commonly in the inferior fornix.

AKC l Cornea: PEE/PEK. l Intraepithelial microcyst. l Infecious and noninfecious corneal ulcer. l Peripheral micropannus. l Neovascularization extending to the central cornea. l Keratoconus in 16% of patients with AKC. l Pellucidal marginal degeneration, and keratoglobus. l
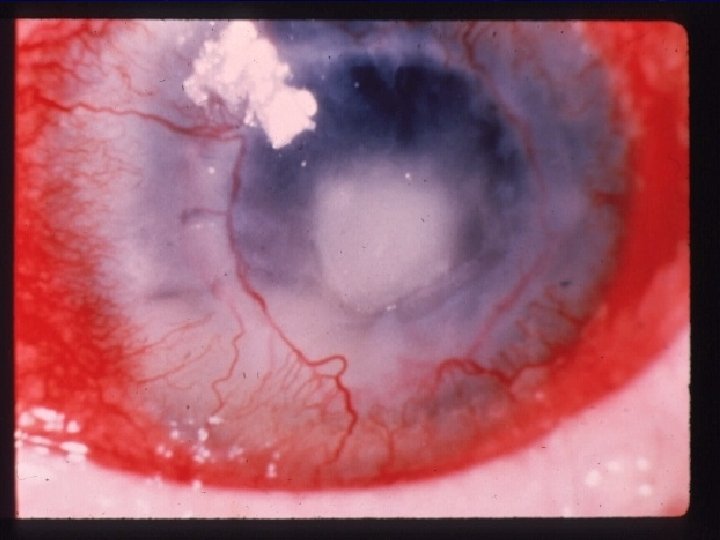

AKC l Lens: ? In 5 to 25% l l l Retina: l l Anterior subcapsular cataract (shield cataract). Posterior subcapsular cataract ( related to steroid ) Retinal detachment. Systemic disorders: l l l Hay fever. Asthma (? in 87%). Atopic dermatitis ( ? In 95%)- chronic pruritic inflammation of the skin mainly forehead, cheeks, and flexor surfaces of the arms and legs, atopic dermatitis usually begin in childhood.
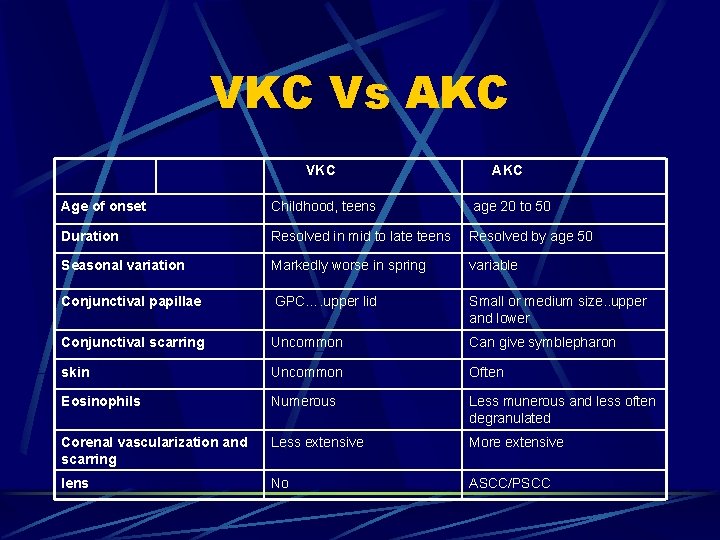
VKC Vs AKC VKC Age of onset Childhood, teens age 20 to 50 Duration Resolved in mid to late teens Resolved by age 50 Seasonal variation Markedly worse in spring variable Conjunctival papillae GPC…. upper lid Small or medium size. . upper and lower Conjunctival scarring Uncommon Can give symblepharon skin Uncommon Often Eosinophils Numerous Less munerous and less often degranulated Corenal vascularization and scarring Less extensive More extensive lens No ASCC/PSCC

AKC Etiology and histopathology: l Type I hypersenstivity reaction. l l Elevated levels of tear and serum Ig. E are charactristic of exacerbated AKC. Conj scraping showed approximately 50 million mast cells, also an excess of eosinophils ( less than VKC) Type IV hypersenstivity Diminished cell medicated immunity is common. l Staph aureus…. . HSV……response to PPD.

AKC Diagnosis: l l l l Family history. Some level of disease activity is always present with variable exacerbations. Atopic dermatitis. Papillary reaction more inferiorly than superiorly. Rarely GPC inferiorly. Usually begin in late teenage or more commonly later. Most severe type of ocular allergy.

AKC In Vivo Tests: Positive intradermal skin tests Conjunctival challenge Prausnitz-Kustner test In Vitro Tests: Basophil histamine release Radioallergosorbent test (RAST)

AKC l l Conjunctival cytology - eosinophils Tear histamine level – 10 ng/ml normal Tear Ig. E, Serum Ig. E Eosinophilia > 500 cells/ml

AKC Managemant: l l l l l Tears. Vasoconstrictors. Cold compresses Antihistamines NSAID. Mast cell stabilizers. Steroid. Cyclosporine. Antibiotics. Surgical: lid procedures/ PKP.

GPC Characterized by the presence of abnormally large papillae ( more than 0. 3 mm in diameter) on the upper tarsal conjunctiva, conjunctival hyperemia, excess mucus secretion, foreign body sensation, and itching. First reported in 1970 in patients wearing contact lenses.

GPC Epidemiology: Incidence among RCL user with average period of 10 months is 10. 5%. l History of atopy plays a major role in predisposition of GPC. l Patients with GPC report higher incidence of allergy to pollens as well as to medications. l

GPC Etiology: l Contact lenses: l l l l l Soft. . any time between 3 weeks to 31/2 yrs after wearing CL. Rigid…may appear even after 11 ys. Sutures. . nylon/prolene. Prosthesis. Cyanoacrylate glue. Scleral buckle. Bleb/valve. . Vernal. Atopy. Epibulbar dermolipoma.

GPC Symptoms: Foreign body sensation. l Intolerance to CLW. l Itching. l Irritation. l Mucus secretion. l

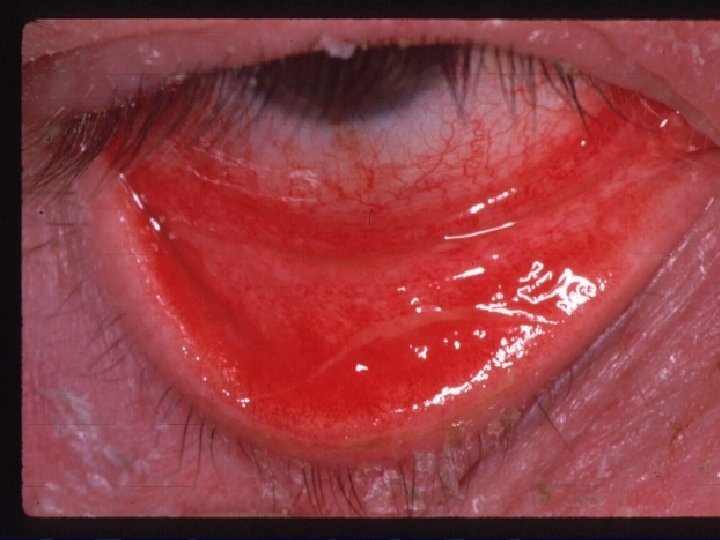
GPC Signs: Enlarged papillae ( > 0. 3 mm in diameter), variable in numbers, and almost always in the upper tarsal conjunctive. l Mucus strands. l Mild to severe hyperemia. l Trantas dots and limbal inflammation. . l Ptosis. l
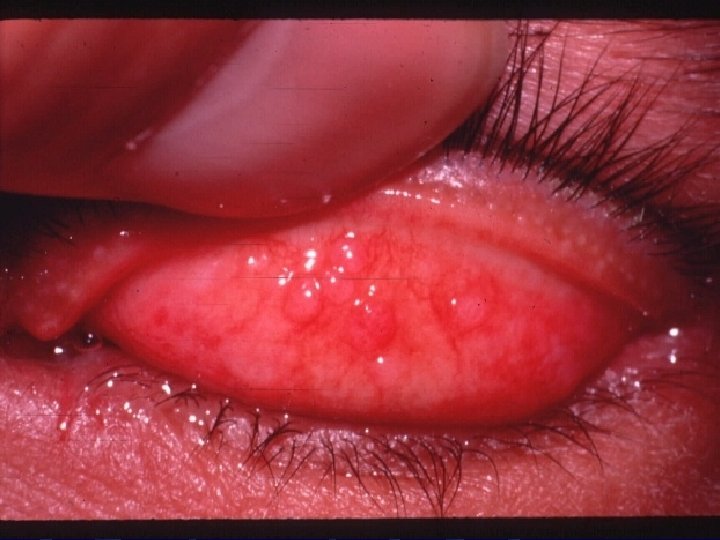

GPC Stages: l Stage I: l l Initial symptoms including mucus in the nasal corner of the eye after sleep and mild itching after lens removal. No papillae detected usually. Stage II: l l Increased severity of mucus and itching and mild blurring of the vision, which occur toward the end of the usual lens wearing time. Small, round papillae, conj is thickened, edematous and hyperemic.

GPC l Stage III: l l Increased severity of mucus and itching, accompanied by excessive lens movement associated with blinking. CL surface become coated with mucus and debris. GPC. . increased in numbers and size. Stage IV: l l l Exacerbation of stage III. CL intolerance. CL are coated and cloudy soon after insertion.

GPC Pathogenesis: l Mechanical trauma…result in degranulation of mast cells and disruption of the epithelial surface. l l l Stimulate production of neutrophil chemotactic factors and inflammatory mediators. Immunological response consisting of both humoral and cell mediated immunity. Mediators in tear fluid: l l l Increase tryptase. increase Ig G, M, E. Increase eosinophil. . MBP. . ECP. Increase histamine. Decrease lactoferin.

GPC treatment; l Prevention: l l l Lens design/hygiene. Burying sutur knots. Relieving the symptoms: l Removal of the CL, prosthesis, suture. l l Symptoms usually dissipate within 48 hrs after d/c CL. Change CL design. . wearing times…hygiene. Mast cell stabilizers…mainly in mild cases. Steroid…. . for moderate to severe cases. l It may take months or even years for GPC to disappear, in some patients, the papillae have not disappeared in more than 20 years, yet these patients remain a symptomatic CLW.

Microbial Allergic Conjunctivitis l • • Staphylococcal blepharoconjunctivitis. Phlyctenular keratoconjunctivitis. Splendore-Hoeppli phenomena Allergic granulomatous nodules
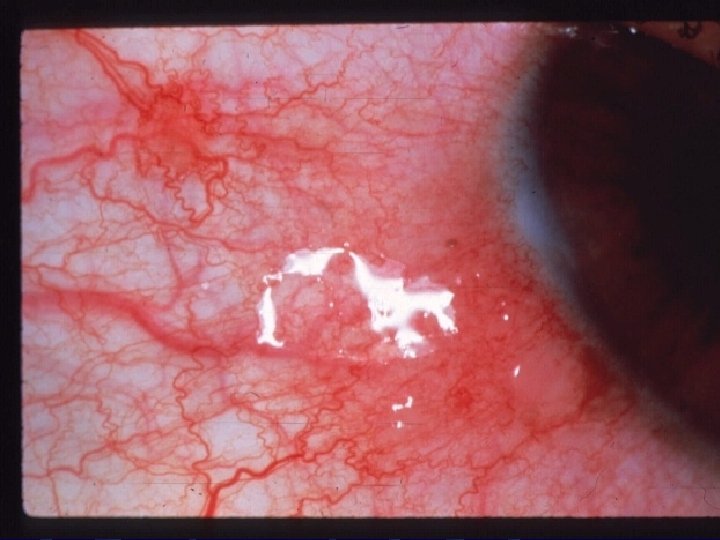
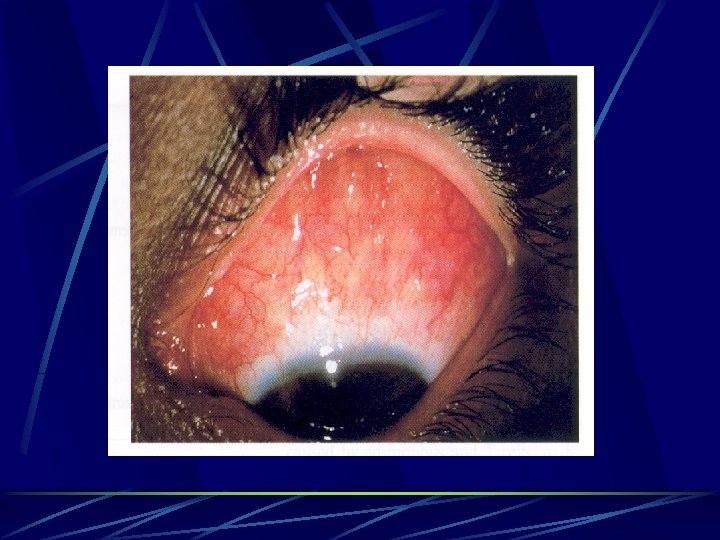

Ocular allergy treatment approach Elimination of allergen. Eliminate eye rubbing. Cool compresses/ tears/ vasoconstrictors. Anithistamines for acute attack. Mast cell stabilizer as prophylactic. NSAIDs fro acute attack Steroid mainly for AKC/ VKC / GPC in short pulses. . Cyclosporine in VKC / AKC. Immunotherapy.

Drug therapy Antihistamines. l Vasoconstrictors. l Mast cell stabilizers. l NSAIDs. l Steroids. l Cyclosporine. l
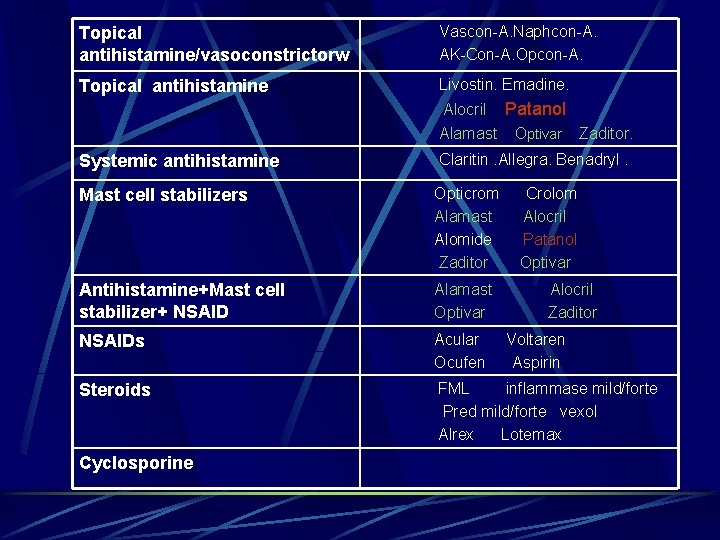
Topical antihistamine/vasoconstrictorw Vascon-A. Naphcon-A. AK-Con-A. Opcon-A. Topical antihistamine Livostin. Emadine. Alocril Patanol. Alamast Optivar Zaditor. Systemic antihistamine Claritin. Allegra. Benadryl. Mast cell stabilizers Opticrom Crolom Alamast Alocril Alomide Patanol Zaditor Optivar Antihistamine+Mast cell stabilizer+ NSAID Alamast Alocril Optivar Zaditor NSAIDs Acular Voltaren Ocufen Aspirin Steroids Cyclosporine FML inflammase mild/forte Pred mild/forte vexol Alrex Lotemax

Antihistamines H 1 receptor H 2 receptor -Found throughout the body. -Vasodilation / increase capillary permeability. -Smooth muscle contraction. -Selective H 1 stimulation in conj…. . produce itching without vasodilation. -Predominantly gut. -Found on ocular surface. -Vasodilation. -Smooth muscle relaxation. -Systemic H 2 antagonist produce decrease in gastric acid production -Selective H 2 stimulation in conj…produce vasodilation (redness). H 3 receptor -Responsible for negative feedback regulation of anaphylactic histamine release. -located on histaminergic terminals of nerves. -Not been identified on ocular tissue. -no selective therapeutic agent yet.

Antihistamines Topical antihistamine: l l All H 1 antagonist. Antihistamine/vasoconstrictor. l l Vascon-A (antazoline 0. 5/naphazoline HCl 0. 05). $10. 99 Naphcon-A ( pheniramine maleate 0. 3/ naphazoline 0. 025). US $10. 69 AK-Con-A ( pheniramine maleate 0. 3/ naphazoline HCl 0. 025). Opcon-A (pheniramine maleate 0. 315/ naphazoline HCl 0. 027). US $14. 49

l l Antihistamines Livostin (CIBA Visio, n) (levocabastine HCl 0. 05%). $53. 47 15000 x more potent than pheniramine. l l Emadine (Alcon), (emedastine difumarate 0. 05%). $53. 84 l l l 4 x/day. Patanol (Alcon), (Olopatadine HCl 0. 1%). $42. 12 l l Onst approx 10 mins. last 4 hours. Has dual action. . antihistamine + mast cell stabilizer. 1 to 2 drops twice a day. Alocril Zaditor Alamast Optivar

Antihistamines Systemic antihistamines: l l Rarely prescribed by ophthalmologist. Useful in patients with rhinitis. Peak action within 1 to 2 hours. Last 4 to 6 hours. l l Claritin (loratadine) 10 mg daily. $26. 99 Allegra (fexofentadine) 60 mg twice daily. $21. 19 Benadryl (diphenhydramine). Zytrec (cetirizine). $1/pill

Antihistamines Side effect: l Topical: Irritation. l PEE due to preservatives. l Dry eye symptoms. l Vasoconstrictors should be used with caution in patient with narrow angle/ HTN/ CVD/ arrhythmias. l

Antihistamines l Systemic: Sedation. l Dizziness. l Fatigue. l Nausea. l Vomiting. l Diarrhea. l Constipation. l Dry eye. l

Mast cell stabilizer l l Opticrom (Akron) (Cromolyn sodium 4%). $15. 79 Crolom (Bausch and Lomb) (cromolyn sodium 4%). US $59. 59 l l Alomide (Alcon), (Lodoxamide 0. 1%). $23. 54 l l l l QID. Found to be superior to cromolyn in VKC. Patanol Alocril Zaditor Alamast Optivar

H 1 anatagonists+ mast cell stabilizer+NSAID l Alocril (Allergan) , (Nedocromil sodium 2%). $41. 59 l l Zaditor (CIBA Vision), (ketotifen fumarate 0. 025%). $36. 70 l l TID to QID doses. Alamast (Santen), (Pemirolast potassium 0. 1%). US $65. 59 l l BID Optivar (azelastine HCI) US $61. 59 l BID

NSAIDs Topical: l l Acular ( Allergan), (ketorolac tromethamine 0. 5%). $50. 15 Voltaren (CIBA), (diclofenac sodium 0. 1%) Ocufen (Allergan), ( flurbiprofen sodium 0. 03%) All act by: l l l Block the cyclo-oxygenase pathway, limiting production of prostaglandins and thromboxanes. Analgesic. S/E: l l l PEE. Persistent epithelial defect. Stromal infiltration. Ulceration. Thinning. Perforation.

NSAIDs Systemic NSAIDs: l Aspirin: l 1 g /day for 6 weeks found to be useful in treating VKC.

Steroids(topical) FML (Allergan), (fluorometholone 0. 1%). $ 35. 74 l FML-F (Allergan), (fluorometholone 0. 25%). l Vexol (Alcon), (rimexolone 1%). $52. 01 l Pred Mild (Allergan), (prednisolone acetate 0. 12%). $ 29 l Pred Forte (Allergan), (prednisolone acetate 1%), $ 54 l Ophtho-Tate (Kenral), (prednisone acetate 1%). $ 18 l Inflamase Mild (CIBA), (prednisone phosphate 1/8%). $ 30 l Inflamase Forte (CIBA), (prednisone phosphate 1%). l $ 28 l Alrex (Bausch and Lomb), (loteprednol etabonate 0. 2%). US $38. 09. l Lotemax (Bausch and Lomb) , (loteprednol etabonate 0. 5%). US $33. 69. l S/E: l l l l Ocular descomfort. Delayed epithelial healing. HSV flare up. Increase IOP. PSCC. Ptosis Mydriasis.

Steroids Local injection. VKC. l AKC. l Oral. l For severe cases as in AKC.

Cyclosporine • • • Cyclosporine (cyclosporine A, Cs. A) is a selective immunosuppressant that inhibits IL 2 and T-cell activation. It also has an inhibitory effect on eosinophils activation. Topical Cs. A 2% was effective as steroid sparing drug in severe VKC and AKC. Its effect is usually transient. l S/E: • • • Intense stinging. Keratitis. Systemic Cs. A has been used in patients with AKC.

Immunotherapy (also called Desensitization or hyposensitization). Long term administration of low but progressively increasing doses of the offending allergen until the evoked clinical reaction is reduced or eliminated. It has been attempted sublingually, nasally, bronchially, ocularly, and subcutaneously (usual route). It takes 3 to 5 years. Recent meta-analysis showed that it is useful for allergic rhinitis and conjunctivitis.
- Slides: 106